Abstract
Background
Presatovir significantly reduced nasal viral load, signs, and symptoms of respiratory syncytial virus (RSV) infection in a human challenge study. We evaluated presatovir in hematopoietic-cell transplant (HCT) recipients with RSV lower respiratory tract infection (LRTI).
Methods
Patients with confirmed RSV in upper and lower respiratory tract and new chest X-ray abnormalities were randomized (1:1), stratified by supplemental oxygen and ribavirin use, to receive oral presatovir 200 mg or placebo every 4 days for 5 doses. The primary endpoint was time-weighted average change in nasal RSV viral load through day 9. Secondary endpoints included supplemental oxygen-free days, incident respiratory failure requiring mechanical ventilation, and all-cause mortality.
Results
From January 31, 2015, to March 20, 2017, 60 patients from 17 centers were randomized (31 presatovir, 29 placebo); 59 received study treatment (50 allogeneic, 9 autologous HCT). In the efficacy population (29 presatovir, 28 placebo), presatovir treatment did not significantly reduce time-weighted average change in viral load (−1.12 vs −1.09 log10 copies/mL; treatment difference −0.02 log10 copies/mL, 95% confidence interval: −.62, .57; P = .94), median supplemental oxygen-free days (26 vs 28 days, P = .84), incident respiratory failure (10.3 vs 10.7%, P = .98), or all-cause mortality (0 vs 7.1%, P = .19) versus placebo. Adverse events were similar between arms (presatovir 80%, placebo 79%). Resistance-associated substitutions in RSV fusion protein emerged in 6/29 presatovir-treated patients.
Conclusions
Presatovir treatment was well tolerated in HCT patients with RSV LRTI but did not improve virologic or clinical outcomes versus placebo.
Clinical Trials Registration
www.clinicaltrials.gov, NCT02254421; EudraCT, #2014-002475-29
Keywords: Presatovir, respiratory syncytial virus, hematopoietic cell transplant, lower respiratory tract infection
Presatovir treatment was safe but did not improve viral or clinical outcomes in hematopoietic-cell transplant recipients with respiratory syncytial virus lower respiratory tract infection. Future studies in this population should incorporate novel methods to evaluate virus-related injury and treatment effects.
Respiratory syncytial virus (RSV) infection is usually associated with respiratory diseases of infants and young children, but RSV lower respiratory tract infection (LRTI) can cause significant morbidity and mortality in adults with predisposing conditions [1]. In recent studies, 16%–27% of hematopoietic-cell transplantation (HCT) recipients initially diagnosed with RSV upper respiratory tract infection (URTI) had LRTI events [2–4]. Mortality rates of up to 60% are reported for RSV LRTI in HCT recipients but appear to be declining [3–7]; however, observed burden of RSV LRTI depends on diagnostic criteria. In cases from 2003 to 2015, no patients with radiographic abnormalities consistent with LRTI but with RSV detected in upper respiratory tract samples only (“possible” RSV LRTI) died, but 28-day mortality was 26% in HCT recipients with probable or proven RSV LRTI [3].
Despite RSV disease burden in HCT recipients and other high-risk adults, options for RSV prophylaxis or treatment in adults are limited. Aerosolized ribavirin is not indicated for RSV treatment in adults and is associated with concerns regarding difficulty of administration, adverse effects, and high cost [8, 9]. Although some centers report using aerosolized or oral ribavirin to treat RSV LRTI in adult HCT recipients, efficacy has not been demonstrated in a randomized controlled clinical trial [10, 11]. Palivizumab is used for prevention of severe RSV disease in high-risk children ≤24 months of age but is not effective as treatment for established infection in children or adult HCT recipients [12–14]. Thus, there is an unmet need for specific treatment for adults at risk for severe RSV infection.
Presatovir is a novel, orally available RSV fusion inhibitor under investigation for treatment of RSV [15]. Presatovir has a favorable safety profile in adult volunteers, and presatovir treatment reduced viral load and respiratory symptoms in healthy adults challenged with RSV [16–18]. Here the safety, tolerability, and efficacy of presatovir in naturally infected HCT recipients with RSV LRTI were evaluated.
METHODS
Patients and Study Design
This phase 2, randomized, double-blind, placebo-controlled, 2-group parallel study recruited HCT recipients 18–75 years of age from 17 centers in 5 countries (Supplemental material, Appendix). Patients presenting any time post-HCT with upper and lower respiratory tract RSV infection documented ≤6 days before start of study treatment and evidence of new abnormalities on chest X-ray obtained ≤48 hours from screening were eligible for inclusion. Lower respiratory tract involvement could be documented from induced sputum, bronchoalveolar lavage, or lung biopsy, but not spontaneous sputum. Patients with documented concurrent LRTI with other respiratory viruses were excluded. Full eligibility criteria are provided in Supplemental methods.
The study followed the International Conference on Harmonisation Good Clinical Practice guidelines and the principles of the Declaration of Helsinki and was approved by local ethics committees. Written informed consent was obtained from patients or legally responsible representatives. Data Monitoring Committee activities and changes to the study protocol are described in Supplemental methods. This trial was registered with ClinicalTrials.gov (NCT02254421) and EudraCT (2014-002475-29) before enrollment began.
Randomization and Masking
Patients were randomly assigned (1:1) to receive presatovir or placebo, stratified centrally by supplemental oxygen use (none to ≤2 L/min vs >2 L/min) and ribavirin use (prescribed at randomization, any route of administration) during the current RSV infection. The randomization schedule used permuted blocks of 2. Allocation was concealed by use of presatovir and placebo tablets with identical appearance. Study treatment assignment information was provided by an interactive web response system (Bracket Global, Wayne, PA, USA). Patients, all study staff, and sponsor were masked to study treatment.
Procedures
Patients received presatovir 200 mg (4 × 50 mg tablets) or placebo orally or via nasogastric tube every 4 days (±24 hours) during study visits on days 1, 5, 9, 13, and 17, and were followed through study day 28. Patients RSV-positive by local molecular testing on day 22 could participate in an optional extended weekly follow-up through day 56. A detailed schedule of study assessments and procedures is provided in Supplemental Table 1.
For virology assessments, bilateral intranasal samples were obtained using midturbinate adult flocked swabs (Copan Diagnostics, Murrieta, CA, USA) at each study visit [19, 20]. Samples were analyzed using reverse transcription quantitative polymerase chain reaction (RT-qPCR) to determine RSV viral load, RSV sequencing of the F gene to evaluate development of resistance, and a multiplex assay to identify coinfections. All nasal samples were analyzed at central laboratories; further details are provided in Supplemental methods. Antibody titer and pharmacokinetic methods are described in Supplemental methods.
Clinical assessments included vital signs, weight, and oxygen saturation by pulse oximetry; laboratory safety assessments included complete blood counts and serum electrolyte and liver enzyme measurements. Patients were observed without oxygen supplementation at each study visit, and the lowest oxygen saturation during observation was recorded. Cardiac safety was assessed via local electrocardiograms and troponin testing on days 1, 17, and 28. Additional safety assessments included evaluation of adverse events (AEs) and documentation of all concomitant medications, hospitalizations, rehospitalizations, intensive care unit care, invasive and noninvasive mechanical ventilation, and supplemental oxygen use (≥2 L/min).
Outcomes
The primary endpoint was time-weighted average change in nasal RSV viral load measured by RT-qPCR (log10 copies/mL) from day 1 to day 9. Key secondary endpoints were number of supplemental oxygen-free days [3], proportion of patients developing respiratory failure requiring invasive or noninvasive mechanical ventilation, and all-cause mortality through day 28. Prespecified exploratory endpoints are described in Supplemental methods. Safety was assessed from AEs and clinical and laboratory parameters.
Statistical Analysis
Assuming time-weighted average change (standard deviation) in RSV log10 viral load from day 1 to day 9 of –1.5 (1.75) log10 copies/mL in placebo-treated patients, 25 patients per treatment group were planned to provide approximately 85% power to detect a ≥1.5 log10 decrease in the primary endpoint in patients receiving presatovir relative to placebo using a 2-sided α of 0.05. We estimated 85% of patients would be evaluable and planned to enroll 60 patients.
The safety population included patients who received ≥1 dose of study drug. The efficacy population included safety population patients with quantifiable RSV viral load on day 1. Primary and secondary efficacy endpoints were analyzed in the efficacy population and post hoc in subgroups defined by supplemental oxygen use, ribavirin use, duration of RSV symptoms, graft-vs-host disease (GVHD), lymphocyte count, and time from HCT to RSV infection on day 1.
The primary analysis tested superiority of presatovir vs placebo using parametric analysis of covariance using baseline viral load and randomization stratification factors as covariates with a 2-sided α of 0.05 (Supplemental methods). Number of supplemental oxygen-free days was analyzed using a negative binomial model with stratification factors as covariates and an offset parameter to account for on-study duration. Patients who died prior to day 28 or received supplemental oxygen on all days of the study period were assigned a value of 0 supplemental oxygen-free days. The proportion of patients developing respiratory failure of any cause requiring invasive or noninvasive mechanical ventilation through day 28 and all-cause mortality through day 28 were analyzed using Cochran-Mantel-Haenszel tests adjusting for the stratification factors at the 2-sided 0.05-level, with 2-sided 95% exact confidence interval (CI) based on the Clopper-Pearson method for each treatment group. Where number of events was small, Fisher exact test was used.
A sequential testing procedure was used to control the Type I error rate of 0.05 across the primary and secondary endpoints [21].
RESULTS
Patients
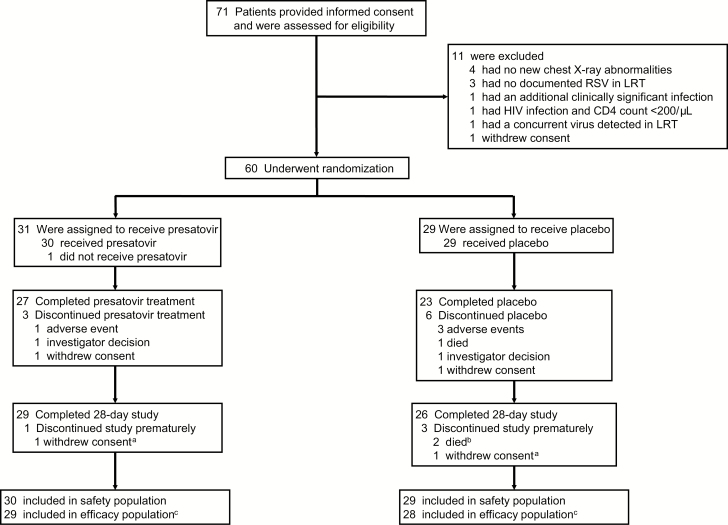
From January 31, 2015, to March 20, 2017, 71 patients were screened for eligibility and 11 were excluded, mostly due to lack of new radiographical abnormalities or inability to confirm lower respiratory tract RSV infection (Figure 1). Sixty patients were randomized, of whom 31 were assigned to presatovir and 29 to placebo; 1 patient randomized to presatovir withdrew consent before receiving study drug. Notable protocol deviations are described in Supplemental results.
Figure 1.
Patient disposition from screening through analysis. The adverse events leading to discontinuation of study drug were acute liver injury with cholestasis in 1 presatovir-treated patient; and sepsis and respiratory failure, bacterial infection and pancytopenia, and leukopenia in 1 placebo-treated patient each. aIncludes the patient who withdrew consent without completing study treatment. bIncludes the patient who died before completing study treatment. c1 patient in each group did not have detectable RSV RNA on day 1. Abbreviations: LRT, lower respiratory tract; RSV, respiratory syncytial virus.
Patient demographics and baseline characteristics were generally balanced between study groups (Table 1). Overall, the majority of patients (50/59; 84.7%) underwent allogeneic HCT and had chronic or acute GVHD (34/59, 57.6%). At start of study treatment, 53 (89.8%) patients were hospitalized for a median of 3 days (range, 0–133 days). Twenty-one (35.6%) patients required >2 L/min of oxygen supplementation, and 23 (39.0%) patients were prescribed ribavirin (any formulation). RSV LRTI was confirmed from induced sputum in 41 (69.5%) patients and by bronchoalveolar lavage in 18 (30.5%) patients. Median time from onset of RSV infection symptoms to start of study treatment was 5 days (range, 1–26 days). Infection was due to RSV A in 29 (49.2%) patients and RSV B in 28 (47.5%) patients; 2 (3.4%) patients (1 presatovir, 1 placebo) had missing day 1 RSV viral load data and were excluded from the efficacy population (N = 57). Median intranasal RSV viral load on day 1 was 6.36 log10 copies/mL (range, 2.5–8.23 log10 copies/mL).
Table 1.
Baseline Characteristics and Demographics in the Safety Population
| Patients Given Presatovir (n = 30) | Patients Given Placebo (n = 29) | Total (N = 59) | |
|---|---|---|---|
| Age, years, median (min, max) | 57 (20, 70) | 55 (21, 74) | 56 (20, 74) |
| Male sex at birth | 21 (70.0) | 23 (79.3) | 44 (74.6) |
| Ethnic origin | |||
| White | 23 (76.7) | 18 (62.1) | 41 (69.5) |
| Asian | 4 (13.3) | 3 (10.3) | 7 (11.9) |
| African American or African | 1 (3.3) | 2 (6.9) | 3 (5.1) |
| American Indian or Alaskan | 1 (3.3) | 1 (3.4) | 2 (3.4) |
| Not documented | 1 (3.3) | 5 (17.2) | 6 (10.2) |
| Hispanic or Latino ethnicity | 5 (16.7) | 6 (20.7) | 11 (18.6) |
| Body mass index, kg/m2, median (min, max) | 25.3 (17.8, 36.5) | 23.0 (13.7, 46.0) | 24.1 (13.7, 46.0) |
| Supplemental oxygen at randomization | |||
| None to ≤2 L/min (nasal cannula) | 19 (63.3) | 19 (65.5) | 38 (64.4) |
| No oxygen supplementation | 15 (50.0) | 16 (55.2) | 31 (52.5) |
| >2 L/min (any delivery system) | 11 (36.7) | 10 (34.5) | 21 (35.6) |
| Ribavirin prescribed at randomization | 12 (40.0) | 11 (37.9) | 23 (39.0) |
| Route of administrationa | |||
| Aerosolized | 7 (23.3) | 5 (17.2) | 12 (20.3) |
| Oral | 3 (10.0) | 5 (17.2) | 8 (13.6) |
| Intravenous | 1 (3.3) | 0 | 1 (1.7) |
| RSV LRT involvement confirmation sample | |||
| Induced sputum | 22 (73.3) | 19 (65.5) | 41 (69.5) |
| Bronchoalveolar lavage fluid | 8 (26.7) | 10 (34.5) | 18 (30.5) |
| RSV type | |||
| RSV A | 15 (50.0) | 14 (48.3) | 29 (49.2) |
| RSV B | 14 (46.7) | 14 (48.3) | 28 (47.5) |
| Missingb | 1 (3.3) | 1 (3.4) | 2 (3.4) |
| Nasal RSV RNA, log10 copies/mL, median (min, max)c | 6.73 (2.9, 8.23) | 6.29 (2.50, 7.89) | 6.36 (2.50, 8.23) |
| Respiratory symptom duration before day 1, days, median (min, max) | 6 (1, 26) | 5 (1, 20) | 5 (1, 26) |
| Respiratory rate, breaths/min, median (min, max)d | 19 (14, 38) | 19 (14, 30) | 19 (14, 38) |
| Oxygen saturation, %, median (min, max)e | 94 (82, 100) | 93 (75, 99) | 94 (75, 100) |
| Smoking history | |||
| Never | 14 (46.7) | 18 (62.1) | 32 (54.2) |
| Former | 16 (53.3) | 11 (37.9) | 27 (45.8) |
| Current | 0 | 0 | 0 |
| Other respiratory viruses detectedf | |||
| Rhinovirus or enterovirus | 1 (3.3) | 1 (3.4) | 2 (3.4) |
| Adenovirus | 1 (3.3) | 0 | 1 (1.7) |
| Coronavirus HKU1 | 1 (3.3) | 0 | 1 (1.7) |
| Coronavirus OC43 | 0 | 1 (3.4) | 1 (1.7) |
| Hospitalized on day 1 | 26 (86.7) | 27 (93.1) | 53 (89.8) |
| Unplanned hospitalization | 23 (76.7) | 24 (82.8) | 47 (79.7) |
| Planned hospitalization | 3 (10.0) | 3 (10.3) | 6 (10.2) |
| Hospitalization related to RSV infection | 22 (73.3) | 23 (79.3) | 45 (76.3) |
| Hospitalization days before day 1, median (min, max) | 3 (0, 49) | 3 (0, 133) | 3 (0, 133) |
| HCT type | |||
| Allogeneic HCT | 26 (86.7) | 24 (82.8) | 50 (84.7) |
| Autologous HCT | 4 (13.3) | 5 (17.2) | 9 (15.3) |
| Time from HCT to study day 1, days, median (min, max) | 451 (10, 3125) | 517 (9, 2501) | 485 (169, 863) |
| Underlying hematological disease | |||
| Acute leukemia | 13 (43.3) | 11 (37.9) | 24 (40.7) |
| Multiple myeloma | 5 (16.7) | 6 (20.7) | 11 (18.6) |
| Lymphoma | 5 (16.7) | 5 (17.2) | 10 (16.9) |
| Myelodysplastic syndrome | 3 (10.0) | 3 (10.3) | 6 (10.2) |
| Chronic lymphocytic leukemia | 0 | 2 (6.9) | 2 (3.4) |
| Otherg | 4 (13.3) | 3 (10.3) | 7 (11.9) |
| Chronic or acute GVHD | |||
| Yes | 17 (56.7) | 17 (58.6) | 34 (57.6) |
| No | 9 (30.0) | 7 (24.1) | 16 (27.1) |
| Not applicable, autologous HCT | 4 (13.3) | 5 (17.2) | 9 (15.3) |
| HCT donor type | |||
| Unrelated | 18 (60.0) | 15 (51.7) | 33 (55.9) |
| Matched-related | 5 (16.7) | 9 (31.0) | 14 (23.7) |
| Mismatched-related | 3 (10.0) | 0 | 3 (5.1) |
| Autologous | 4 (13.3) | 5 (17.2) | 9 (15.3) |
| Stem cell source | |||
| Peripheral blood | 25 (83.3) | 25 (86.2) | 50 (84.7) |
| Bone marrow | 4 (13.3) | 2 (6.9) | 6 (10.2) |
| Cord blood | 1 (3.3) | 2 (6.9) | 3 (5.1) |
| Recipient CMV seropositive | 19 (63.3) | 18 (62.1) | 37 (62.7) |
Data are n (%) unless otherwise specified.
Abbreviations: CMV, cytomegalovirus; GVHD, graft-vs-host disease; HCT, hematopoietic cell transplant; LRT, lower respiratory tract; max, maximum; min, minimum; RSV, respiratory syncytial virus.
aOn the day of the first dose of study drug, 11 patients receiving presatovir and 10 patients receiving placebo were being treated with ribavirin. Current or intended use of ribavirin on day of randomization was used to stratify randomization.
bThese patients were excluded from the efficacy population.
cFor these values, n = 29 for the presatovir arm and n = 28 for the placebo arm.
dFor these values, n = 28 for the placebo arm.
eFor these values, n = 29 for the presatovir arm and n = 27 for the placebo arm.
fTesting was performed at a central laboratory.
gOther comprises 1 patient each with chronic myeloid leukemia, hemophagocytic lymphohistiocytosis, myelofibrosis, and Waldenstrom macroglobulinemia in the presatovir group and 1 patient each with plasma cell leukemia and sickle cell disease in the placebo group.
Nine patients (3 presatovir, 6 placebo) prematurely discontinued study treatment, and 4 patients discontinued study participation before day 28 (1 presatovir, 3 placebo) (Figure 1). Twenty-seven (90.0%) of 30 patients in the presatovir group and 23/29 (79.3%) patients in the placebo group completed treatment to day 17 (Figure 1).
Efficacy
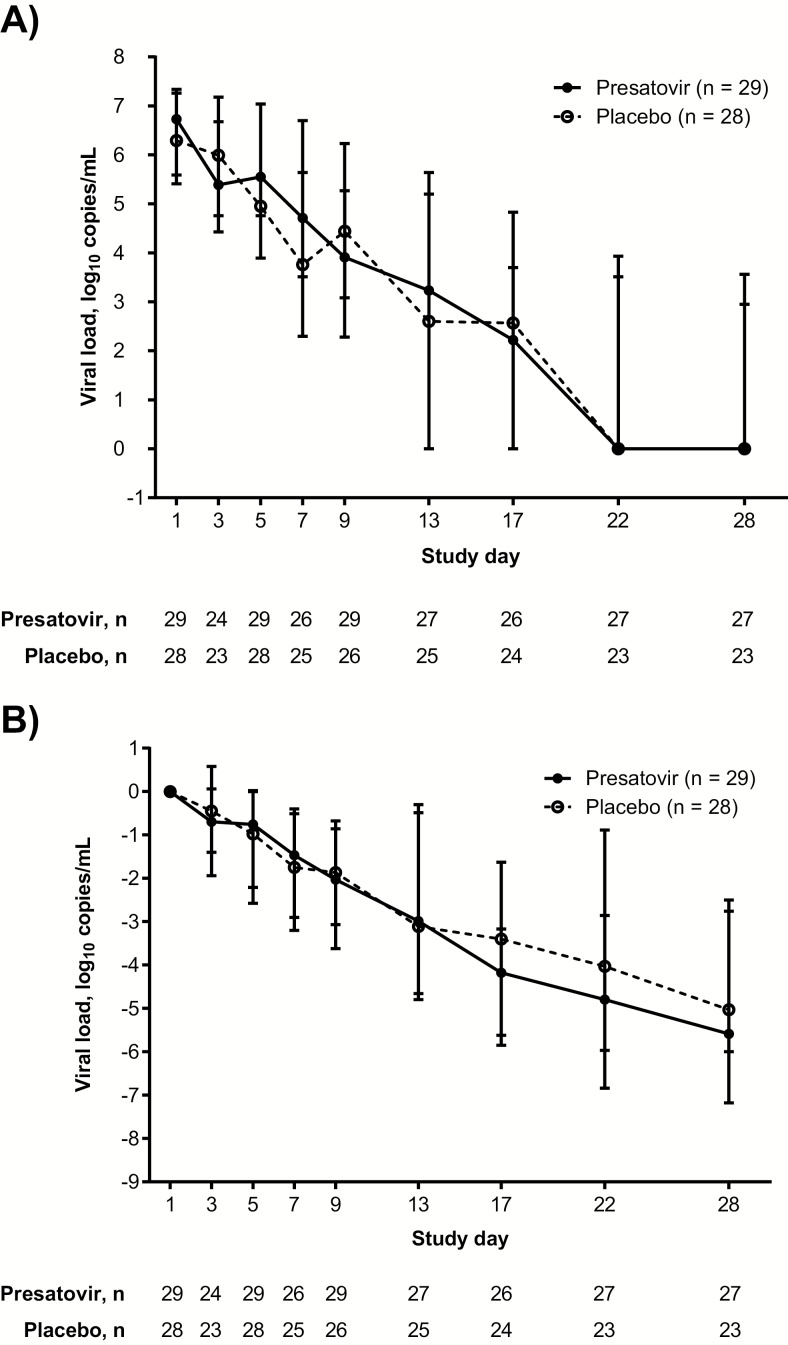
Figure 2A–B shows median absolute RSV viral load and change from baseline at each study visit. Despite adequate plasma concentrations (Supplemental results and Supplemental Table 3), presatovir treatment did not significantly reduce time-weighted average change in log10 RSV viral load from day 1 to day 9 (−1.12 [1.226] log10 copies/mL versus −1.09 [1.028] log10 copies/mL; treatment difference, −0.02 log10 copies/mL; 95% CI, −.62, .57; P = .94) compared with placebo (Table 2).
Figure 2.
Presatovir treatment did not significantly reduce respiratory syncytial virus (RSV) RNA relative to placebo. Panel (A) shows median nasal RSV RNA and panel (B) shows median change from baseline in nasal RSV RNA at each study visit in patients treated with presatovir (solid circles and lines) vs placebo (open circles, dashed lines) in the efficacy population. Error bars represent the interquartile range. Numbers below the graph are n at each time point.
Table 2.
Time-Weighted Average Change in Nasal RSV RNA to Day 9, Supplemental Oxygen-Free Days Through Day 28, Respiratory Failure Requiring Mechanical Ventilation, and All-Cause Mortality in the Efficacy Population
| Presatovir (n = 29) | Placebo (n = 28) | |
|---|---|---|
| Time-weighted average change in nasal RSV RNA (log10 copies/mL) from baseline to day 9 | ||
| Mean (SD) | −1.12 (1.23) | −1.09 (1.03) |
| Adjusted meana (95% CI) | −1.00 (−1.43, −.56) | −0.97 (−1.41, −.53) |
| P valuea | .94 | |
| Number of supplemental oxygen-free days through day 28 | ||
| Median (min, max) | 26 (0, 33) | 28 (0, 30) |
| P valueb | .84 | |
| Patients who developed respiratory failure requiring mechanical ventilation through day 28 | ||
| n (%) | 3 (10.3) | 3 (10.7) |
| P valuec | 1.00 | |
| All-cause mortality through day 28 | ||
| n (%) | 0 | 2 (7.1) |
| P valuec | .24 |
Abbreviations: CI, confidence interval; max, maximum; min, minimum; RSV, respiratory syncytial virus; SD, standard deviation.
aResults were calculated from the analysis of covariance model including baseline values and stratification factors.
bResults were calculated from the negative binomial model with stratification factors as covariates.
c P-value was calculated using Fisher exact test.
During the 28-day study period, 14/29 (48.3%) presatovir-treated patients and 12/28 (42.9%) placebo-treated patients required supplemental oxygen. Median (range) number of supplemental oxygen-free days was similar between presatovir-treated (26 [0–33] days) and placebo-treated (28 [0–30] days) patients (P = .84) (Table 2). Three presatovir-treated patients (10.3%) and 3 placebo-treated patients (10.7%) developed respiratory failure requiring mechanical ventilation through study day 28 (P = 1.0). No presatovir-treated patients and 2 placebo-treated patients (7.1%) died through day 28 (P = .24) (Table 2); 1 death was due to respiratory failure. Exploratory efficacy outcomes are described in Supplemental results.
Primary and secondary efficacy endpoints did not differ appreciably between patients treated with presatovir relative to placebo in subgroups defined by absolute lymphocyte count on day 1, presence of GVHD, time from onset of RSV symptoms to study treatment, and timing of RSV infection after HCT (Supplemental Tables 6–9). Optional extended viral monitoring and serologic responses to RSV infection are presented in the Supplemental Results.
Sequencing of RSV F gene detected postbaseline amino acid substitutions at resistance-associated positions in 6/29 (20.7%) of presatovir-treated patients and 0/28 placebo-treated patients. These substitutions were detected a median of 25 (range, 7–56) days after start of treatment (Supplemental Table 10).
Safety
Twenty-four presatovir-treated patients (80.0%) and 23 placebo-treated patients (79.3%) experienced ≥1 AE, whereas 7 presatovir-treated patients (23.3%) and 7 placebo-treated patients (24.1%) experienced serious AEs (SAEs). Adverse events ≥grade 3 occurred in 7 presatovir-treated patients (23.3%) and 9 placebo-treated patients (31.0%). Individual AEs occurred in ≤10% of presatovir-treated patients (Table 3). Numerically more frequent AEs in patients treated with presatovir versus placebo were pneumonia, increased alanine aminotransferase, hypokalemia, nausea, acute sinusitis, and epistaxis (3 patients each, 10%), and increased aspartate aminotransferase, dry mouth, and increased alkaline phosphatase (2 patients each, 6.7%; Table 3). Except for SAE pneumonia in 3 presatovir-treated patients (10%), grade 3 or 4 AEs and SAEs occurred in 1 patient each and were numerically less frequent overall in patients treated with presatovir versus placebo (Supplemental Tables 11–12). There were no significant imbalances in electrocardiogram and troponin results during the study. No patients treated with presatovir and 2 patients treated with placebo (6.9%) died during the 28-day study period; 1 death was due to respiratory failure and 1 to progressive acute leukemia. Another 2 patients (6.9%) who received placebo died after day 28, 1 of respiratory failure, and 1 of invasive fusariosis.
Table 3.
Adverse Events and Laboratory Abnormalities Reported for at Least 2 Patients in the Safety Population
| Adverse Event | Presatovir (n = 30) | Placebo (n = 29) |
|---|---|---|
| Any adverse event | 24 (80.0) | 23 (79.3) |
| Diarrhea | 3 (10.0) | 3 (10.3) |
| Anemia | 1 (3.3) | 4 (13.8) |
| Headache | 2 (6.7) | 3 (10.3) |
| Pneumonia | 3 (10.0) | 2 (6.9) |
| Pyrexia | 2 (6.7) | 3 (10.3) |
| Alanine aminotransferase increased | 3 (10.0) | 1 (3.4) |
| Hypokalemia | 3 (10.0) | 1 (3.4) |
| Hypotension | 2 (6.7) | 2 (6.9) |
| Nausea | 3 (10.0) | 1 (3.4) |
| Thrombocytopenia | 1 (3.3) | 3 (10.3) |
| Acute sinusitis | 3 (10.0) | 0 |
| Anxiety | 1 (3.3) | 2 (6.9) |
| Aspartate aminotransferase increased | 2 (6.7) | 1 (3.4) |
| Cough | 0 | 3 (10.3) |
| Dry mouth | 2 (6.7) | 1 (3.4) |
| Epistaxis | 3 (10.0) | 0 |
| Lymphopenia | 1 (3.3) | 2 (6.9) |
| Edema, peripheral | 1 (3.3) | 2 (6.9) |
| Rash | 1 (3.3) | 2 (6.9) |
| Respiratory failure | 1 (3.3) | 2 (6.9) |
| Acute kidney injury | 0 | 2 (6.9) |
| Atrial fibrillation | 0 | 2 (6.9) |
| Alkaline phosphatase increased | 2 (6.7) | 0 |
| Dizziness | 0 | 2 (6.9) |
| Fatigue | 0 | 2 (6.9) |
| Neutropenia | 0 | 2 (6.9) |
Data are shown as n (%).
DISCUSSION
This is the first placebo-controlled clinical trial, to our knowledge, evaluating treatment of RSV LRTI with a new antiviral agent in HCT recipients. Presatovir had a favorable safety profile and was well tolerated but did not decrease time-weighted average change in nasal RSV viral load from day 1 to day 9, number of days with supplemental oxygen use, or frequency of respiratory failure or mortality relative to placebo. In contrast, presatovir treatment significantly reduced viral load, clinical signs, and symptoms of experimental RSV infection in healthy volunteers treated upon detection of RSV replication [16]. Potential explanations for this discrepancy have important implications for design of clinical trials evaluating antiviral treatments for RSV infection in HCT recipients and other patient populations.
In the past 5 years, treatment with a fusion inhibitor or nucleoside polymerase inhibitor significantly reduced RSV viral load, signs, and symptoms in 3 challenge studies in healthy human volunteers [16, 22, 23]. However, clinical trials of presatovir conducted in multiple different patient populations, including this study and a companion URTI study (Chemaly et al [24], this issue), indicate difficulties remain in translating challenge study results to successful clinical trials in patients with natural infection [25, 26]. One partial explanation is the challenge model’s inconsistent representation of the natural infection setting. Challenge study volunteers were inoculated intranasally with RSV, then monitored for nasal RSV replication with twice-daily nasal washes that were immediately evaluated with molecular assays for RSV [16, 22, 23]. Antiviral treatment was initiated 6–24 hours after RSV detection, generally several days before peak viral load and prior to manifestation of significant clinical signs and symptoms [16, 22, 23]. In the present study, patients with naturally acquired RSV LRTI received presatovir later in the disease course compared with challenge study subjects (median [range], 5 [1–26] days after symptom onset); delay was also observed in the URTI trial (median [range], 4 [1–10] days) and other studies of presatovir in natural RSV infection [25, 26]. Because clinical signs and symptoms tend to correlate with nasal viral load [16, 22], these patients presumably presented near or more likely after peak nasal viral load, potentially beyond the therapeutic window for presatovir even in immunocompromised patients. Host immune-mediated clearance of the virus at this stage may also mask treatment-induced reduction in viral load. Thus, treatment delay may explain lack of presatovir efficacy in the current study.
The mechanism of action of presatovir may also have limited efficacy in this study. Because RSV is capable of cell-to-cell spread, inhibition of viral fusion may not halt propagation of established infection along the respiratory tract. Therefore, fusion inhibitors, such as presatovir, may need to be administered, whereas virus-cell fusion still represents the main mode of viral spread to appreciably reduce nasal viral load. Emergence of F gene protein amino acid substitutions associated with fusion inhibitor resistance was also relatively frequent (21%) in this immunocompromised population. Polymerase inhibitors can terminate intracellular RSV replication and may have wider therapeutic windows compared with fusion inhibitors [27]. However, no polymerase inhibitor has demonstrated clinical efficacy in a natural infection setting to date. Furthermore, nasal viral load is questionable as a primary endpoint for proof-of-concept studies in naturally infected patients with LRTI because upper respiratory tract samples, although more convenient to obtain, may not reflect viral activity in the lower respiratory tract, particularly in immunocompromised patients. Alternative approaches are needed for noninvasive measurement of viral disease dynamics and antiviral activity in lower airway and alveolar tissue.
The findings of this trial call into question whether appearance of new radiological opacities with documentation of RSV in the upper or lower respiratory tract accurately classifies patients with RSV infection. This approach may be satisfactory for retrospective studies but inadequate as an enrollment criterion for prospective clinical trials. Radiographic findings in adults with RSV LRTI confirmed from a lower respiratory tract specimen are not well characterized, and radiographic abnormalities in these patients may be caused by other viruses, bacteria, or fungi—particularly in immunocompromised patients—or even noninfectious processes. As RSV chiefly affects airway epithelium [28], RSV LRTI could manifest without radiographic findings, and present only as lower airway symptoms (eg, wheezing or obstructive spirometry pattern). Furthermore, the degree of lung injury in patients with RSV LRTI may not be reversible by antiviral treatment alone. These issues will need to be considered in future clinical trials.
The lack of clinical benefit in this study may also relate to the selected clinical endpoints, which occurred at lower-than-anticipated rates that decreased power to detect a treatment effect. Although all subjects enrolled in the current study met Waghmare et al’s criteria for proven or probable LRTI, median number of supplemental oxygen-free days through day 28 was much higher (26 and 28 days for presatovir-treated and placebo-treated patients, respectively, vs 17 days), and fewer patients required >2 L/min supplemental oxygen at baseline (35.6% versus 57%) relative to patients who presented with or developed LRTI in the Waghmare study [3]. Furthermore, lymphopenia is a major risk factor for RSV infection and subsequent poor outcomes in HCT recipients [2, 4, 29], but only 4/47 patients with available data in the current study were lymphopenic (<200 cells/mm3) at baseline, possibly because RSV infection occurred relatively late after HCT (median, 485 vs 129 days in the Waghmare study). These differences could be due to limited enrollment of patients perceived as fragile because of the requirement for lower respiratory sampling to confirm RSV LRTI. Enrichment of the study population for immunosuppressed patients should be considered in future clinical trials of therapies for RSV infection in HCT recipients.
In summary, presatovir treatment was generally well tolerated in HCT recipients with naturally acquired RSV LRTI but did not achieve virologic or clinical endpoints. The tendency of adults with naturally acquired RSV infection to seek treatment only after several days of symptoms, when the treatment window may have closed for fusion inhibitors in particular, is a challenge for clinical trials of RSV-specific antiviral therapies. The numerically lower rate of pulmonary complications in the presatovir URTI trial suggests that early treatment, before LRTI develops, is key for success in future studies.
Supplementary Data
Supplementary materials are available at Clinical Infectious Diseases online. Consisting of data provided by the authors to benefit the reader, the posted materials are not copyedited and are the sole responsibility of the authors, so questions or comments should be addressed to the corresponding author.
Notes
Author Contributions. F. M. M. wrote the first draft of the manuscript with input from J. W. C. F. M. M., R. F. C., M. B., J. W. C., and S. S. D. contributed to study design. Y. G. performed statistical analysis. P. G. performed pharmacokinetics analysis. D. P. P. performed virology analysis. All authors critically reviewed the manuscript and approved the final version for submission.
Acknowledgements. The authors extend their thanks to the patients and their families for their participation. Editorial support was provided by Judith M. Phillips, DVM, PhD, of AlphaBioCom, LLC, and funded by Gilead Sciences, Inc.
Financial support. This work was supported by Gilead Sciences, Inc.
Potential conflicts of interest. F. M. M. reports research grants paid to his institution and consulting fees for clinical trial design from Gilead Sciences, Inc., during the conduct of the study; and research support paid to his institution and consulting fees for clinical trial design from Chimerix and GlaxoSmithKline, research grant support paid to his institution from Ansun, and personal fees from Roche Molecular Diagnostics and Visterra outside the current study. R. F. C. reports research grants paid to his institution and personal fees from Gilead Sciences, Inc., during the conduct of the study; research grants paid to his institution from Ablynx, AiCuris, Ansun, Chimerix, Merck, Oxford Immunotec, Novartis, Pulmotec, Shire, and Xenex; and consultant fees/honoraria from Ablynx, Achaogen, ADMA Biologics, Ansun, Astellas, Chimerix, Clinigen, Janssen, Oxford Immunotec, Merck/Merck Sharp and Dohme (MSD), Pulmotect, Shionogi, Shire, and Xenex outside the current study. K. M. M. reports grants as a clinical trial investigator from Gilead Sciences, Inc., during the conduct of the study; clinical research grants from Ansun, Astellas, Merck, Rebiotix, Scynexis, and Shire; and consultant fees/honoraria from Chimerix, GlaxoSmithKline, Merck, and Scynexis outside the current study. D. G. L. reports research grants and consultant fees or speaker honoraria from Astellas, MSD, and Pfizer outside the current study. H. H. H. reports nothing to disclose. C. B. S. reports grants paid to her institution from Gilead Sciences, Inc., during the conduct of the study and from Abbott, Ablynx, Chimerix, GlaxoSmithKline, Merck, Schering, Shire, and ViiV outside the current study. A. B. reports funding to her institution from Gilead Sciences, Inc., during the conduct of the study; and research grants from Pfizer and SOS Oxygène and consultant/speaker fees from Ablynx; Gilead Sciences, Inc.; Merck; Pfizer; Shire; Therakos; and Zambon outside the current study. S. S. reports grants paid to his institution from Gilead Sciences, Inc., during the conduct of the study; grants paid to his institution from Astellas, Ansun, Cidara, Emergent BioSolutions, Merck, Scynexis, Shiongi, Shire, and T2 Microsystems outside the current study; and direct payments as a member of a data safety monitoring board from Merck outside the current study. P. L. reports research grants or fees/honoraria paid to his institution from Astellas; Gilead Sciences, Inc.; Merck; Oxford Immunotec; and Shire; and consultant fees/honoraria from Ablynx and AiCuris outside the current study. A. W. reports clinical trial support from Gilead Sciences, Inc., during the conduct of the study. E. B. reports speaker fees from Boehringer Ingelheim; Gilead Sciences, Inc.; Novartis; Pfizer; and Roche outside the current study. Y. J. K. reports grants from Gilead Sciences, Inc., during the conduct of the study. M. M., D. P. P., Y. G., P. G., and T. R. W. are employees of Gilead Sciences, Inc., and may hold stock. R. J. is a former employee of and holds stock in Gilead Sciences, Inc. M. B. reports clinical trial support and consulting fees from Gilead Sciences, Inc., during the conduct of the study; and grants and personal fees from Ablynx; Ansun; Chimerix; GlaxoSmithKline; Merck; Shire; and Vir Bio; and personal fees from Bavarian Nordic; Humabs, Inc.; Janssen; Modema Therapeutics; Pulmocide; and Pulmotect outside the current study. J. W. C. is an employee and stockholder of Janssen BioPharma and a former employee and current stockholder of Gilead Sciences, Inc. S. S. D. reports grants paid to his institution from Gilead Sciences, Inc., during the conduct of the study; and grants to his institution and personal fees for consulting, advisory board, and speaker bureau participation from Merck; personal fees for advisory board participation from Clinigen and Janssen; and grants paid to his institution from Ablynx, AiCuris, Ansun, GlaxoSmithKline, Oxford Immunotec, and Shire outside the current study. All authors have submitted the ICMJE Form for Disclosure of Potential Conflicts of Interest. Conflicts that the editors consider relevant to the content of the manuscript have been disclosed.
References
- 1. Falsey AR, Walsh EE. Respiratory syncytial virus infection in adults. Clin Microbiol Rev 2000; 13:371–84. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Kim YJ, Guthrie KA, Waghmare A, et al. Respiratory syncytial virus in hematopoietic cell transplant recipients: factors determining progression to lower respiratory tract disease. J Infect Dis 2014; 209:1195–204. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Waghmare A, Xie H, Kimball L, et al. Supplemental oxygen-free days in hematopoietic cell transplant recipients with respiratory syncytial virus. J Infect Dis 2017; 216:1235–44. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Shah DP, Ghantoji SS, Shah JN, et al. Impact of aerosolized ribavirin on mortality in 280 allogeneic haematopoietic stem cell transplant recipients with respiratory syncytial virus infections. J Antimicrob Chemother 2013; 68:1872–80. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Whimbey E, Champlin RE, Couch RB, et al. Community respiratory virus infections among hospitalized adult bone marrow transplant recipients. Clin Infect Dis 1996; 22:778–82. [DOI] [PubMed] [Google Scholar]
- 6. Whimbey E, Champlin RE, Englund JA, et al. Combination therapy with aerosolized ribavirin and intravenous immunoglobulin for respiratory syncytial virus disease in adult bone marrow transplant recipients. Bone Marrow Transplant 1995; 16:393–9. [PubMed] [Google Scholar]
- 7. Shah JN, Chemaly RF. Management of RSV infections in adult recipients of hematopoietic stem cell transplantation. Blood 2011; 117:2755–63. [DOI] [PubMed] [Google Scholar]
- 8. VIRAZOLE®(Ribavirin for Inhalation Solution, USP). Full Prescribing Information. Bridgewater, NJ, USA: Valeant Pharmaceuticals North America LLC, 2016. [Google Scholar]
- 9. Chemaly RF, Aitken SL, Wolfe CR, Jain R, Boeckh MJ. Aerosolized ribavirin: the most expensive drug for pneumonia. Transpl Infect Dis 2016; 18:634–6. [DOI] [PubMed] [Google Scholar]
- 10. Boeckh M, Englund J, Li Y, et al. ; NIAID Collaborative Antiviral Study Group Randomized controlled multicenter trial of aerosolized ribavirin for respiratory syncytial virus upper respiratory tract infection in hematopoietic cell transplant recipients. Clin Infect Dis 2007; 44:245–9. [DOI] [PubMed] [Google Scholar]
- 11. Waghmare A, Englund JA, Boeckh M. How I treat respiratory viral infections in the setting of intensive chemotherapy or hematopoietic cell transplantation. Blood 2016; 127:2682–92. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. SYNAGIS® (palivizumab) injection, for intramuscular use. Full prescribing information. Gaithersburg, MD, USA: MedImmune, LLC, May 2017. Available from https://www.azpicentral.com/synagis/synagis.pdf. Accessed February 27, 2018. [Google Scholar]
- 13. American Academy of Pediatrics Committee on Infectious Diseases, American Academy of Pediatrics Bronchiolitis Guidelines Committee. Updated guidance for palivizumab prophylaxis among infants and young children at increased risk of hospitalization for respiratory syncytial virus infection. Pediatrics 2014; 134:415–20. [DOI] [PubMed] [Google Scholar]
- 14. de Fontbrune FS, Robin M, Porcher R, et al. Palivizumab treatment of respiratory syncytial virus infection after allogeneic hematopoietic stem cell transplantation. Clin Infect Dis 2007; 45:1019–24. [DOI] [PubMed] [Google Scholar]
- 15. Mackman RL, Sangi M, Sperandio D, et al. Discovery of an oral respiratory syncytial virus (RSV) fusion inhibitor (GS-5806) and clinical proof of concept in a human RSV challenge study. J Med Chem 2015; 58:1630–43. [DOI] [PubMed] [Google Scholar]
- 16. DeVincenzo JP, Whitley RJ, Mackman RL, et al. Oral GS-5806 activity in a respiratory syncytial virus challenge study. N Engl J Med 2014; 371:711–22. [DOI] [PubMed] [Google Scholar]
- 17. German P, Xin Y, Chien JW, et al. Phase 1 first-in-human, single- and multiple-ascending dose, and food effect studies to assess the safety, tolerability, and pharmacokinetics of presatovir for the treatment of respiratory syncytial virus infection. J Clin Pharmacol 2018; 58:1025–34. [DOI] [PubMed] [Google Scholar]
- 18. Xin Y, Weng W, Murray BP, et al. The drug-drug interaction profile of presatovir. J Clin Pharmacol 2018; 58:771–80. [DOI] [PubMed] [Google Scholar]
- 19. Frazee BW, Rodriguez-Hoces de la Guardia A, Alter H, et al. Accuracy and discomfort of different types of intranasal specimen collection methods for molecular influenza testing in emergency department patients. Ann Emerg Med 2018; 71:509–17 e1. [DOI] [PubMed] [Google Scholar]
- 20. Smieja M, Castriciano S, Carruthers S, et al. Development and evaluation of a flocked nasal midturbinate swab for self-collection in respiratory virus infection diagnostic testing. J Clin Microbiol 2010; 48:3340–2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Dmitrienko A, Offen WW, Westfall PH. Gatekeeping strategies for clinical trials that do not require all primary effects to be significant. Stat Med 2003; 22:2387–400. [DOI] [PubMed] [Google Scholar]
- 22. DeVincenzo JP, McClure MW, Symons JA, et al. Activity of oral ALS-008176 in a respiratory syncytial virus challenge study. N Engl J Med 2015; 373:2048–58. [DOI] [PubMed] [Google Scholar]
- 23. DeVincenzo J, Tait D, Oluwayi O, et al. Safety and efficacy of oral RV521 in a human respiratory syncytial virus (RSV) phase 2a challenge study. Am J Respir Crit Care Med 2018; 197:A7715. [Google Scholar]
- 24. Chemaly RF, Dadwal SS, Bergeron A, et al. A phase 2, randomized, double-blind, placebo-controlled trial of presatovir for the treatment of respiratory syncytial virus upper respiratory tract infection in hematopoietic-cell transplant recipients. Clin Infect Dis 2019. doi:10.1093/cid/ciz1166 [DOI] [PMC free article] [PubMed]
- 25. Gottlieb J, Torres F, Haddad T, et al. A phase 2b, randomized controlled trial of presatovir, an oral RSV fusion inhibitor, for the treatment of respiratory syncytial virus (RSV) in lung transplant (LT) recipients. J Heart Lung Transplant 2018; 37:S155. [DOI] [PubMed] [Google Scholar]
- 26. Hanfelt-Goade D, Maimon N, Nimer A, et al. A phase 2b, randomized, double-blind, placebo-controlled trial of presatovir (GS-5806), a novel oral RSV fusion inhibitor, for the treatment of respiratory syncytial virus (RSV) in hospitalized adults. Am J Respir Crit Care Med 2018;197: A4457. [Google Scholar]
- 27. Brookes DW, Coates M, Allen H, et al. Late therapeutic intervention with a respiratory syncytial virus L-protein polymerase inhibitor, PC786, on respiratory syncytial virus infection in human airway epithelium. Br J Pharmacol 2018; 175:2520–34. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28. Welliver TP, Garofalo RP, Hosakote Y, et al. Severe human lower respiratory tract illness caused by respiratory syncytial virus and influenza virus is characterized by the absence of pulmonary cytotoxic lymphocyte responses. J Infect Dis 2007; 195:1126–36. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29. Chemaly RF, Ghosh S, Bodey GP, et al. Respiratory viral infections in adults with hematologic malignancies and human stem cell transplantation recipients: a retrospective study at a major cancer center. Medicine (Baltimore) 2006; 85:278–87. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.