Abstract
High-frequency oscillatory ventilation (HFOV) is characterized by the rapid delivery of small tidal volumes (Vts) of gas and the application of high mean airway pressures (mPaws). These characteristics make HFOV conceptually attractive as an ideal lung-protective ventilatory mode for the management of ARDS, as the high mPaws prevent cyclical derecruitment of the lung and the small Vts limit alveolar overdistension. In this review, we will summarize the literature describing the use of HFOV in adult patients with ARDS. In addition, we will discuss recent experimental studies of HFOV that have advanced our understanding of its mechanical properties. We identified 2 randomized controlled trials (RCTs) and 12 case series evaluating HFOV in adults with ARDS. In these studies, HFOV appears to be safe and consistently improves oxygenation when used as a rescue mode of ventilation in patients with severe ARDS. The two RCTs comparing HFOV to conventional ventilation revealed encouraging results but failed to show a mortality benefit of HFOV over conventional ventilation. Further research is needed to identify optimal patient selection, technique, the actual Vt delivered, and the role of combining HFOV with other interventions, such as recruitment maneuvers, prone positioning, and nitric oxide.
Key words: acute lung injury, ARDS, high-frequency oscillatory ventilation, high-frequency ventilation, mechanical ventilation, respiratory failure, ventilator-induced lung injury
Abbreviations: ALI, acute lung injury; APACHE, acute physiology and chronic health evaluation; CMV, conventional mechanical ventilation; CO, cardiac output; CVP, central venous pressure; Fio2, fraction of inspired oxygen; ETT, endotracheal tube; HFJV, high-frequency jet ventilation; HFOV, high-frequency oscillatory ventilation; HFV, high-frequency ventilation; IL, interleukin; iNO, inhaled nitric oxide; mPaw, mean airway pressure; OI, oxygenation index; ΔP, pressure amplitude; PAOP, pulmonary artery occlusion pressure; PCV, pressure-controlled ventilation; PEEP, positive end-expiratory pressure; RCT, randomized controlled trial; RM, recruitment maneuver; VILI, ventilator-induced lung injury; Vt, tidal volume
In patients with acute lung injury (ALI) or ARDS, conventional mechanical ventilation (CMV) may occasionally lead to injurious airway pressures.1 High-frequency ventilation (HFV) was introduced in the 1960s as a novel ventilatory mode, which was designed to improve oxygenation and ventilation, and to avoid some of the complications associated with CMV.2 The major characteristics of HFV include a respiratory rate in the range of 60 to 900 breaths/min and low tidal volumes (Vts), often below the volume of anatomic dead space.3 Compared to CMV, mean airway pressure (mPaw) is usually higher (Fig 1 ). Thus, while the rapid ventilatory rate can provide adequate gas exchange, the higher mPaw and lower Vts limit alveolar derecruitment and overdistension, respectively. These characteristics make HFV conceptually attractive as a lung-protective ventilatory mode.
Figure 1.
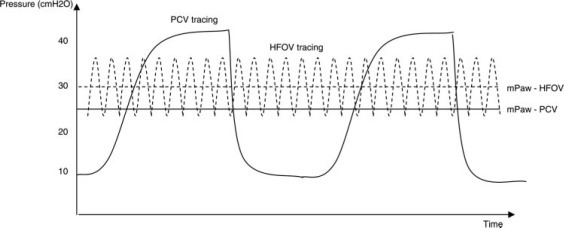
Schematic representation of the purported waveforms of HFOV and conventional pressure-controlled ventilation in the distal airways. The large pressure swings present in the proximal circuit during HFOV (perhaps up to twice the mean airway pressure, depending on the set ΔP) are significantly attenuated in the distal airways. The degree of attenuation is dependent on frequency, ETT size, and inspiratory/expiratory time ratio.
Despite these potential physiologic advantages, the early experience with the high-frequency modes was disappointing. High-frequency jet ventilation (HFJV) was shown to be no better than CMV in maintaining oxygenation and ventilation in adult patients with hypoxemic respiratory failure.4 In premature neonates with respiratory distress syndrome, there was an excess of adverse events in two trials,5 6 with one using HFJV and one using high-frequency oscillatory ventilation (HFOV). These early studies were criticized because of issues with trial design and the inconsistent use of lung recruitment strategies.7 Many lessons were learned from these early studies, including problems with the introduction of a new technology before adequately understanding the physiologic principles and its optimal application.8
Over the past few years, perhaps as a result of the understanding that conventional ventilatory approaches to lung protection can save lives,9 there has been renewed interest in HFV. Most of the more recent advances have been in the utilization of HFOV in adult patients with ALI and ARDS. This article will focus on animal studies from the past few years, which have advanced our understanding of HFOV as it is applied to models of ALI/ARDS, and on more recent clinical studies in adult patients with ALI/ARDS.
Technique of HFOV
Currently, there are three modes of HFV in clinical use, as follows: HFJV; high-frequency percussive ventilation; and HFOV. We will limit this review to HFOV. Detailed descriptions of the other high-frequency modes can be found elsewhere.3 10
During HFOV in adults, a piston pump oscillates at frequencies between 180 and 600 breaths/min (3 to 10 Hz) [Fig 2 ].10 An inspiratory bias flow of fresh gas (30 to 60 L/min) and a resistance valve in the circuit are used to control the mPaw within the circuit. HFOV is unique compared to other modes of HFV, as the return stroke of the piston during expiration leads to the active expiration of gas.11 Arguably, this active expiration allows for less gas trapping. Humidification during HFOV is achieved by passing the bias flow of gas through a humidifier.
Figure 2.
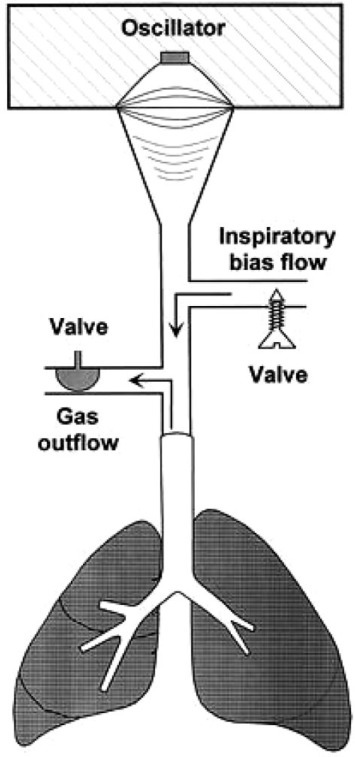
Schematic representation of the high-frequency oscillator. Blended gas is passed through a bias flow circuit. The oscillator pump then actively pushes gas into the airway and subsequently draws it out again. Reproduced with permission from Krishnan and Brower.10
The other unique feature of HFOV is the ability to, for the most part, separate the control of oxygenation and ventilation. Oxygenation is primarily a function of the fraction of inspired oxygen (Fio 2) and mPaw (or lung volume). Ventilation is inversely related to the respiratory frequency and is directly related to the excursion of the diaphragm of the ventilator, with the latter expressed as the pressure amplitude (ΔP) of oscillation.12
Mechanisms of Gas Transport During HFOV
During CMV, gas transport occurs by bulk delivery of gas due to convection through the airways to the alveolar zones. Since a certain proportion of the delivered Vt remains in the proximal airways as dead space volume, the Vt must be more than the dead space volume for gas exchange to occur. Because Vts delivered with HFV are usually less than the anatomic dead space, this traditional concept of gas transport does not apply. Gas transport is thought to occur via a number of convective and diffusive mechanisms (Fig 3 ).13 These include the bulk flow of gas to alveolar units close to the proximal airways, asymmetric velocity profiles, and Taylor dispersion. The latter two mechanisms are related to augmented mixing of gas within the airways because of the high energies involved during HFV. In addition, there is asynchronous filling of adjacent alveolar spaces (termed pendelluft) due to different alveolar-emptying times, collateral ventilation through nonairway connections between neighboring alveoli, and cardiogenic mixing. To further understand these mechanisms, the reader is encouraged to refer to several excellent reviews.3 10 14 15
Figure 3.
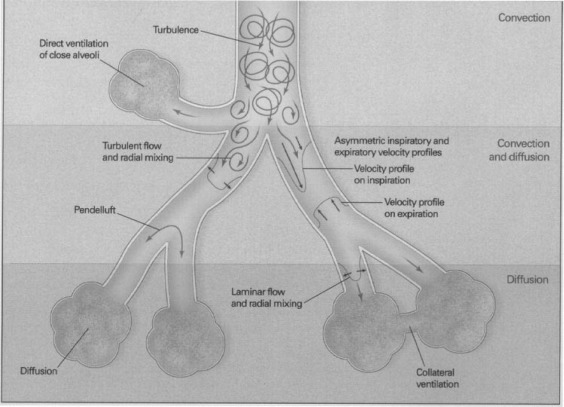
Mechanisms of gas exchange during HFOV. Reproduced with permission from Slutsky and Drazen.13 Copyright 2002 Massachusetts Medical Society. All rights reserved.
Experimental Studies of HFOV in ALI /ARDS
It is now known that CMV can be injurious to the lung through mechanisms such as barotrauma, volutrauma, and atelectrauma,16 Collectively, these mechanisms are called ventilator-induced lung injury (VILI). A lung-protective ventilator strategy that reduces alveolar overdistension (ie, volutrauma) has been shown to reduce mortality in ALI/ARDS patients.9 HFOV may be an ideal lung-protective ventilatory mode by virtue of the comparatively higher mPaws achieved, thus allowing for better lung recruitment and very low Vts.
Low Vts During HFOV
HFOV utilizes an oscillating diaphragm at high frequencies to create pressure swings within the airway, which leads to CO2 elimination. Vts generated during HFOV are proportional to the ΔP and the inspiratory/expiratory ratio, and are inversely proportional to respiratory frequency. The use of high flows of gas, coupled with the resistance of the endotracheal tube (ETT), leads to significant attenuation of these pressure oscillations in the distal airway.17 18 Consequently, it was assumed that the alveolar Vts generated are lower than those on CMV and, hence, are associated with less alveolar overdistension. However, a few recent studies have challenged this assumption.
First, this assumption was based on small animal models and the neonatal literature, in which very high frequencies (ie, > 10Hz) and lower ΔPs are employed. In adult patients, relatively lower frequencies (ie, 3 to 6 Hz) and higher ΔPs (ie, 60 to 90 cm H2O) are often needed to achieve CO2 elimination. In a 2003 study19 of lung injury in an adult sheep model, HFOV at settings similar to those applied in adults delivered Vts that were much higher than originally thought. For example, Sedeek et al19 applied HFOV with an inspiratory/expiratory ratio of 1:1, 60 cm H2O ΔP, and a frequency of 4 Hz, and observed actual Vts of 4.4 mL/kilogram.
Second, as the inner diameter of the ETT increases, so does the inspiratory Vt. In a preterm lamb-based computer model,18 reducing the internal diameter of the ETT from 4.0 to 2.5 mm halved the transmission of the pressure waveform to both the carina and the alveolar compartment. These findings have significant implications as adult patients have larger ETTs and require lower frequencies compared to neonates. Hence, if larger Vts are generated, this mode of ventilation may not be as safe as originally thought. A recent preliminary clinical study of seven adults with ARDS by Hager et al,20 published in abstract form, was reassuring in that measured Vts while patients received HFOV ranged from 44 to 209 mL, which was substantially lower than the Vts commonly used in CMV.
Lung Recruitment During HFOV
The small pressure swings produced during HFOV allow for higher mPaws without injurious levels of peak airway pressure. This leads to better lung recruitment and a higher end-expiratory lung volume. The combined effects of higher mPaws and very small pressure oscillations lead to less cyclical recruitment-derecruitment of the lung.21 Conversely, the much larger pressure swings seen during CMV, despite similar levels of mPaw, may lead to cyclical alveolar collapse at end-expiration.22
Setting the mPaw for optimal lung recruitment, however, remains challenging. Typically, it has been recommended that clinicians initiate HFOV with an mPaw that is 3 to 5 cm H2O higher than the mPaw used during CMV. Using a sheep model of lung injury and calculating the static pressure-volume curves while using CMV, Goddon et al23 found that an mPaw 6 cm H2O above the lower inflection point yielded the best Pao 2/Fio 2 ratio. It was notable that this pressure correlated with the point of maximum curvature on the deflation limb of the pressure-volume curve. In a similar experiment utilizing CT scans to estimate lung recruitment and lung volumes, Luecke et al24 found that the ideal mPaw was 1.5 times the lower inflection point, which also corresponded to the ideal mPaw in the study by Goddon et al.23 At this level of mPaw, the best gas exchange was achieved without compromising cardiac output (CO). Unfortunately, neither of these strategies is practical or clinically applicable for most intensivists.
HFOV and VILI
Many investigators have thus hypothesized that the mechanical advantages of HFOV should lead to a lower incidence of VILI. Experiments in small animals21 seem to support this hypothesis, demonstrating less histologic damage and lung inflammation. In saline solution-lavaged rabbit models of lung injury,21 25 26 27 HFOV has been found to reduce the morphologic findings of VILI, including hyaline membrane formation, alveolar leukocyte infiltration, and airway epithelial damage when compared to CMV. In addition, the expression of messenger RNA for tumor necrosis factor, several interleukins (ILs) [ie, IL-1β, IL-6, IL-8, and IL-10], transforming growth factor, and adhesion molecules were all reduced in animals receiving HFOV.
Most of the earlier animal studies comparing HFOV and CMV utilized relatively high peak inspiratory pressures and Vts. Whether or not HFOV compares favorably to CMV applied with a “lung-protective” strategy (ie, low Vt and high levels of positive end-expiratory pressure [PEEP]) has been the subject of several investigations.25 28 29 30 Imai et al25 compared pathophysiologic and biochemical markers in a saline solution-lavaged rabbit model of ARDS treated with the following four different ventilatory strategies: (1) CMV with moderate Vts (10 to 12 mL/kg); (2) CMV with low Vts (5 to 6 mL/kg) and PEEPs 2 to 3 cm H2O higher than the lower inflection point; (3) CMV with low Vts and PEEPs of 8 to 10 cm H2O; and (4) HFOV. Rabbits treated with HFOV had less neutrophil infiltration, lower levels of tumor necrosis factor, and decreased pathologic changes in the alveolar spaces when compared to the other groups of rabbits. In contrast, Vasquez de Anda et al28 found no difference in lung mechanics and protein concentration in BAL fluid samples when comparing HFOV to pressure-controlled ventilation (PCV) applied with high levels of PEEP in a rat model of ARDS. Compared with small animals, HFOV applied to adults with larger ETTs may lead to larger pressure swings and greater Vts. Unfortunately, there are currently few large animal studies of HFOV and ALI.31 32 33 34 One study from 200333 compared PCV, HFOV, and intratracheal percussive ventilation in a sheep model of lung injury. The investigators found greater histologic damage in the PCV group, which was ventilated with relatively high Vts (8 mL/kg). Overall, more large animal studies are needed to compare HFOV and lung-protective CMV.
Clinical Application of HFOV in Adult Patients With ARDS
Table 1 presents a summary of case series and randomized trials evaluating HFOV in adults.35 36 37 38 39 40 45 46 47 48 50 51 63 64 The first study of HFOV in adults with ARDS was published in 1997.35 This single-center study described the use of HFOV in 17 adult patients with ARDS, mainly due to sepsis and pneumonia, who were not responding to CMV. The patients had a mean Pao 2/Fio 2 ratio of 68 mm Hg, an oxygenation index (OI) [Fio 2 × mPaw × 100/Pao 2] of 48, and an APACHE (acute physiology and chronic health evaluation) II score of 23. All of the patients showed improvement in the OI with HFOV, and the overall survival rate was 47%. Of note, these authors observed that nonsurvivors had received CMV for a significantly longer duration prior to receiving HFOV than survivors. This finding suggests that HFOV may be more effective when initiated earlier in the course of ARDS. An alternate point of view is that patients in whom ARDS develops later in their ICU stay (and thus are candidates for an HFOV trial at a later time point) may have a poorer outcome, regardless of whether HFOV is used or not.
Table 1.
Comparison of Published Clinical Studies Evaluating the Use of HFOV in Adult Patients With ARDS*
| Study/Year | Study Design | Patients, No. | Baseline Characteristics | Mortality Rate | Comments |
|---|---|---|---|---|---|
| Fort et al35/1997 | Prospective | 17 | Mean age, 38 yr; Pao2/Fio2 ratio, 68.6; OI, 48.6; APACHE II score, 23.3 | 30-d, 53% | Greater number of days receiving CMV (p < 0.009) and OI > 47 were associated with mortality; 3 patients (17.6%) were withdrawn from HFOV because of hypotension |
| Claridge et al36/1999 | Prospective | 5 | Trauma patients; mean age, 36.6 yr; Pao2/Fio2 ratio, 52.2; APACHE II score, 28.5 | 20% | No complications reported |
| Mehta et al37/2001 | Prospective | 24 | Mean age, 48.5 yr; Pao2/Fio2 ratio, 98.8; OI, 32.5; APACHE II score, 21.5 | 30-d, 66% | Small increases in PAOP and CVP and a small decrease in CO were documented during HFOV, with no significant change in systemic BP; two patients (8.3%) had a pneumothorax |
| Cartotto et al38/2001 | Retrospective | 6 | Burn patients; mean age, 48.5 yr; Pao2/Fio2 ratio; 98.8; OI, 32.5; APACHE II score, 21.5 | 30-d, 83.3% | No complications reported |
| Derdak et al45/2002 | RCT | 48 | Mean age, 49.5 yr; Pao2/Fio2 ratio, 112.5; OI, 25.2; APACHE II score, 22 | 30-d: while receiving HFOV, −37%; while receiving CMV, 52% (p = 0.102) | First RCT comparing HFOV to CMV; similar complication rate in both groups |
| Andersen et al39/2002 | Retrospective | 16 | Mean age, 38.2; Pao2/Fio2 ratio, 92; OI, 28.1; SAPS II score, 40.3 | 3-mo, 31% | One patient (6.3%) had a pneumothorax |
| Mehta et al48/2003 | Prospective | 23 | Mean age, 44.9 yr; Pao2/Fio2 ratio, 75; APACHE II score, 28.6 | ICU, 61% | This study demonstrated that iNO can be used successfully as rescue therapy in patients with severe ARDS and high O2 requirements (mean increase in Pao2/Fio2 ratio at 30 min, 38%); five patients (21.7%) had a pneumothorax |
| David et al40/2003 | Prospective | 42 | Median age, 49 yr; Pao2/Fio2 ratio, 94; OI, 23; APACHE II score, 28 | 30-d, 43% | One patient (2.4%) had a pneumothorax |
| Mehta et al51/2004 | Retrospective | 156 | Median age, 47.8 yr; Pao2/Fio2 ratio, 91; OI, 31.2; APACHE II score, 23.8 | 30-d, 62% | 34 patients (21.8%) had a pneumothorax |
| Ferguson et al47/2005 | Prospective | 25 | Median age, 50 yr; Pao2/Fio2 ratio, 92; APACHE II score, 24 | ICU, 44% | This pilot study demonstrated the safety and efficacy of combining early RMs with HFOV for rapid and sustained improvements in oxygenation; 8% of patients had a chest tube inserted for barotraumas; 3.3% of RMs were aborted because of hypotension |
| Papazian et al50/2005 | RCT | 39 | Mean age, 52 yr; Pao2/Fio2 ratio, 103; SOFA score, 9.5 | ICU: supine HFOV, 38.4%; prone CV, 30.8%; prone HFOV, 23.1% | This randomized study compared HFOV, prone positioning, or their combination in patients with severe ARDS (13 patients in each arm); patients in the supine HFOV group had no improvement in oxygenation; 1 patient (2.5%) had mucus plugging necessitating a change of ETT |
| Bollen et al46/2005 | RCT | 61 | Mean age, 81 yr; HFOV, 37 patients; CMV, 24 patients; study prematurely stopped; OI, 22; APACHE II score, 21 | 30-d: with HFOV, 43%; with CMV, 33% (p = 0.59) | HFOV group: four patients (10.8%) had hypotension and one patient (2.7%) had an air leak; CMV group: one patient (4.2%) had hypotension and one patient (4.2%) had an air leak; baseline OI was higher in HFOV group (25 vs 18, respectively); 19% of HFOV group crossed over to CMV, and 17% of CMV group crossed over to HFOV |
| Pachl et al63/2006 | Prospective | 30 | Mean age, 55 yr; Pao2/Fio2 ratio, 121; SOFA score, 9.6 | 46% | This study showed that HFOV might be more effective in extrapulmonary forms of ARDS, compared to pulmonary forms of ARDS; complications were not reported |
| Finkielman et al64/2006 | Retrospective | 14 | Mean age, 56 yr; APACHE II score, 35; SOFA score, 11.5 | ICU, 57% | HFOV was discontinued in one patient for refractory hypotension |
SAPS = simplified acute physiology score; SOFA = sequential organ failure assessment.
Subsequent to this study, a number of other groups published their experience with HFOV.36 37 38 39 40 41 These were generally small case series (range, 5 to 42 cases), in which patients had severe ARDS and HFOV was employed as rescue therapy.9 42 43 While all of these studies showed that the application of HFOV was associated with improvements in oxygenation compared with baseline during CMV, survival was generally poor. As with other studies in patients with ARDS,44 only a minority of patients treated with HFOV died due to respiratory failure.
In adult patients with ARDS, only two prospective, randomized trials45 46 have been published comparing HFOV with CMV. In a study by Derdak et al,45148 adults in 13 centers were randomized to receive either HFOV or CMV. At baseline, patients in both groups were well-matched, with a mean age of 49.5 years, an APACHE II score of 22, and similar Pao 2/Fio 2 ratios (approximately 110). The main findings of this study were as follows: (1) an earlier improvement in the Pao 2/Fio 2 ratio (< 16 h) in the HFOV group, which did not persist beyond 24 h; and (2) a similar but low incidence of adverse events in both groups (intractable hypotension, 0 to 3%; air leak, 9 to 12%; mucus-plugging of ETT, 4 to 5%). The study was also notable for a nonsignificant trend toward a lower 30-day mortality rate in the HFOV group compared to that in the group receiving conventional ventilation (37% vs 52%, respectively; p = 0.102). As this study was performed before the publication of the first ARDS Network trial,9 relatively large Vts (10 mL/kg) with high peak inspiratory pressures were used, which has been a major criticism of this study.
The second randomized controlled trial (RCT) was stopped prematurely for slow enrollment after randomizing 61 patients to HFOV or CMV.46 A trend toward a higher ICU mortality rate in the HFOV group (43% vs 33%, respectively; p = 0.59) was found. However, interpretation of this study is limited because of the small number of patients enrolled, the baseline differences in the two groups (including a higher OI in the HFOV group), the lack of explicit ventilation protocols, and the crossover of 18% of patients to the alternate arm.
Role of Adjunctive Therapies
Improvement in oxygenation in patients receiving HFOV can be slow, taking up to 8 h in one study.37 This is a consequence of the small Vts that are used, leading to very little tidal recruitment. The use of recruitment maneuvers (RMs) may increase or hasten alveolar recruitment. A multicenter, observational pilot study47 has demonstrated the safety and efficacy of repeated RMs applied in a strict, protocolized fashion. In this study of 25 patients with early ARDS, RMs applied at the commencement of HFOV resulted in early and significant improvements in Pao 2/Fio 2 ratio compared to standardized CMV (200 vs 92 mm Hg, respectively, within 1.5 h). The improvement in oxygenation occurred more rapidly than has been reported in other HFOV studies.35 37 45 The RMs were relatively safe, and only 8 of 244 RMs (3.3%) were aborted, mainly because of hypotension.
If adults with ARDS remain hypoxemic during HFOV, prone positioning and inhaled nitric oxide (iNO) may further improve gas exchange.48 49 In a study of 23 adults with ARDS, Mehta et al48 administered iNO at 5 to 20 ppm during HFOV and observed that the mean Pao 2/Fio 2 ratio increased by 38% at 30 min. In addition, 83% of patients had a significant improvement in oxygenation in response to iNO, which is greater than the response observed in most studies applying iNO during CMV.48
Papazian and colleagues compared the impact of supine HFOV, prone HFOV, and prone CMV on 12-h oxygenation in 39 patients with ARDS.50 While both groups of prone patients (ie, CMV and HFOV groups) had similar and significant improvements in oxygenation, the supine HFOV group showed no improvement. This was a surprising finding given that all previous studies35 37 51 have shown improvements in oxygenation with HFOV. The most likely explanation for this difference is that insufficient airway pressures (average mPaw, 25 cm H2O) were applied during HFOV in this study. Thus, the improvement in oxygenation in the prone HFOV group likely reflects the effect of the change in position only, and not the combined effect of the two modalities. Furthermore, the 12-h observation period may have been insufficient for maximal HFOV-induced lung recruitment, as other studies35 45 have shown that the maximal improvement in oxygenation occurs beyond 12 h.
HFOV and Mortality of Patients With ARDS
Many of the clinical studies35 37 40 51 have demonstrated that the delayed initiation of HFOV is an independent predictor of death. In addition, an RCT comparing HFOV and CMV demonstrated a trend toward lower mortality in the HFOV group.45 These observations are consistent with findings in animal models of ALI, which have shown that prolonged exposure to excessive Vts and insufficient PEEP can further exacerbate the lung injury,52 53 54 can increase the levels of proinflammatory cytokines, and potentially can promote the development of multiorgan failure and death.43 55 A recent systematic review56 of the determinants of mortality with the use of HFOV in adults with ARDS also found a 20% higher mortality rate for every additional day CMV was received. However, this association was confounded by differences in pH (pH adjusted: relative risk, 1.03; 95% confidence interval, 0.73 to 1.46).
There is a need to compare HFOV and the best available lung-protective CMV with adequate power and with mortality as the primary outcome. With better understanding of VILI, and the use of lung-protective ventilatory strategies, mortality from ARDS has been decreasing over the past decade.9 44 57 As a result, the choice of a conventional strategy is important. In a recently published trial57 conducted by the ARDS Network, two fluid management strategies (liberal and conservative) were compared in the management of established ALI. In both study arms, a lung-protective ventilation protocol with low Vts and limited plateau pressures were used. The 60-day mortality rates were 28.4% and 25.5%, respectively, which is one of the lowest mortality rates in large, published trials of ALI/ARDS. Whether or not HFOV as a lung-protective ventilatory mode would be able to reduce mortality beyond what has already been achieved with CMV is uncertain.
Complications of HFOV
Because of the higher mPaws that are applied during HFOV, potential concerns include barotrauma and hemodynamic compromise. In a retrospective study by Mehta et al,51 26% of 156 patients had HFOV discontinued because of difficulties with oxygenation, ventilation, or hemodynamics, and the incidence of pneumothorax was 21.8%. However, in the two RCTs12 46 of HFOV vs CMV that have been published so far, the incidence of pneumothorax and hypotension were comparable between the two groups. In the Treatment with Oscillation and an Open Lung Strategy pilot study,47 which applied repeated RMs as part of an aggressive lung recruitment strategy, only 1 patient (of 25) required withdrawal from HFOV for barotrauma. Two patients (8%) required a chest tube insertion for barotrauma, and eight RMs (of 244; 3.3%) were aborted because of hypotension. Recognition of a pneumothorax is a particular challenge in patients receiving HFOV. The background noise of the ventilator, coupled with the lack of true breath sounds due to minimal bulk flow, makes the detection of a pneumothorax by auscultation difficult. Often, reduction or asymmetry in the body wiggle, in response to the pressure waves, or a rise in ΔP are clues that such an event has occurred.
The application of HFOV has been associated with increases in central venous pressure (CVP) and pulmonary artery occlusion pressure (PAOP), and with a small, clinically insignificant decrease in CO.37 45 51 58 In the randomized trial by Derdak et al,45 the CVP increased from 14 mm Hg at baseline to 16 mm Hg at 2 h. The corresponding values for the PAOP were 16 and 18 mm Hg, respectively; and for the CO, 7.4 and 7.0 L/min, respectively. In another study by David et al,58 similar findings were obtained. In addition, the stroke volume index, and the end-systolic and diastolic area indexes decreased. The increases in CVP and PAOP likely reflected the increased mPaw, while the decreased CO and cross-sectional area of the left ventricle were likely due to a decrease in venous return.
Therefore, it is important that patients transitioning from CMV to HFOV are adequately volume repleted; judicious fluid challenges may be necessary to prevent or ameliorate the hemodynamic effects of higher mPaws. The extent to which this additional fluid may be detrimental is uncertain. However, given the recent data57 implicating more aggressive fluid strategies in longer ICU stays and ventilator times, this needs to be done with caution and evaluated carefully.
Adequate humidification is important, because of the high gas flows and minute ventilation. With HFOV, the desiccation of secretions could potentially lead to mucus inspissation and ETT obstruction,12 although the incidence of this complication is relatively low (4 to 5%).35 37
Very heavy sedation to induce apnea is often needed, as most patients are intolerant of the technique. The continuous use of IV sedation has been associated with prolonged duration of mechanical ventilation, and ICU and hospital length of stays.59 60 In addition, neuromuscular blocking agents, medications that have been implicated in the development of critical illness polyneuropathy,61 are usually necessary.51
One other concern with HFOV is the lack of an approved expiratory filter for the device, potentially leading to aerosolization of infectious droplets. During the outbreak of severe acute respiratory syndrome in Toronto, HFOV was grouped as a high-risk respiratory procedure (together with noninvasive ventilation, intubation, and nebulized therapies) precisely because of this issue.62
In summary, HFOV has been shown to lead to improvements in oxygenation in adult patients with ARDS, particularly in those not responding to CMV, with complication rates that are similar to those patients receiving CMV. Previous studies have suggested that the earlier application of HFOV in adult patients with ARDS may lead to lower mortality when compared to CMV. Currently, the practice in our institution is to consider using HFOV once lung-protective ventilation with CMV is no longer possible (ie, an inability to adequately oxygenate or ventilate the patient while maintaining a plateau pressure of < 30 cm H2O and an Fio 2 of < 0.6). These thresholds may be lower than what most clinicians would consider to be the “failure” of CMV. Table 2 shows the initiation settings for HFOV at our institution. We also favor RMs during the initiation of HFOV to accelerate lung recruitment. The reader should be aware that RMs are relatively contraindicated if there is significant barotrauma. In addition, because of the high mPaws used and the need for rapid alveolar emptying, HFOV is relatively contraindicated in patients with severe obstructive lung disease or asthma. Currently, a well-validated and standardized algorithm does not exist, and there are variations between institutions on many aspects, including mPaw titration protocol, the routine use of ETT cuff leaks to enhance CO2 clearance, RMs, weaning, transition back to CMV, and the use of other adjuncts (such as prone positioning and iNO).
Table 2.
Suggested Settings for Initiating HFOV
| Oxygenation | Ventilation |
|---|---|
| Fio2, 0.9–1.0 | Frequency, 5 Hz |
| mPaw, 5 cm H2O above last measured mPaw while on conventional ventilation | Power set to give a ΔP that causes a “wiggle from shoulder to mid-thigh”; usually between 60 and 90 cm H2O initially |
| Inspiratory time, 33% | |
| Bias flow, 40 L/min | |
| Consider RMs (eg, 40 cm H2O for 40 s with the piston off) |
Future Research Directions
Over the past decade, our understanding of HFOV and how it relates to VILI has increased substantially. Small animal studies have indeed shown that HFOV may attenuate VILI. However, in order to extrapolate these results to adult patients with ARDS, studies using large animal models of lung injury are needed.
Although it is emerging in mainstream clinical use in adult patients, HFOV remains a unique mode of ventilation with different gas exchange principles compared to those for CMV. As with other new technologies in the ICU, clinicians and administrators of individual institutions need to study the added cost of training staff and the safety issues surrounding a mode of mechanical ventilation that may be infrequently utilized. In addition, more clinical studies of HFOV are needed to address the many unanswered questions regarding the use of HFOV in adult patients with ARDS. What are the optimal timing, patient selection, and technique to be used? How do we optimally recruit the lung and measure this at the bedside? And finally, given the substantial mortality reductions with current CMV-based lung-protective strategies, HFOV needs to be compared directly with CMV in a large RCT with mortality as the primary outcome measure.
Footnotes
Dr. Mehta has received honoraria from Viasys for speaking at conferences. Drs. Chan and Stewart have reported to the ACCP that no significant conflicts of interest exist with any companies/organizations whose products or services may be discussed in this article.
References
- 1.American Thoracic Society The European Society of Intensive Care Medicine, The Societe de Reanimation de Langue Francaise. International consensus conferences in intensive care medicine: ventilator-associated lung injury in ARDS; this official conference report was cosponsored by the American Thoracic Society, The European Society of Intensive Care Medicine, and The Societe de Reanimation de Langue Francaise, and was approved by the ATS Board of Directors, July 1999. Am J Respir Crit Care Med. 1999;160:2118–2124. doi: 10.1164/ajrccm.160.6.ats16060. [DOI] [PubMed] [Google Scholar]
- 2.Slutsky AS. Nonconventional methods of ventilation. Am Rev Respir Dis. 1988;138:175–183. doi: 10.1164/ajrccm/138.1.175. [DOI] [PubMed] [Google Scholar]
- 3.dos Santos CC, Slutsky AS. Overview of high-frequency ventilation modes, clinical rationale, and gas transport mechanisms. Respir Care Clin N Am. 2001;7:549–575. doi: 10.1016/s1078-5337(05)70006-x. [DOI] [PubMed] [Google Scholar]
- 4.Hurst JM, Branson RD, Davis K, Jr et. al Comparison of conventional mechanical ventilation and high-frequency ventilation: a prospective, randomized trial in patients with respiratory failure. Ann Surg. 1990;211:486–491. doi: 10.1097/00000658-199004000-00017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.HIFI Study Group High-frequency oscillatory ventilation compared with conventional mechanical ventilation in the treatment of respiratory failure in preterm infants. N Engl J Med. 1989;320:88–93. doi: 10.1056/NEJM198901123200204. [DOI] [PubMed] [Google Scholar]
- 6.Wiswell TE, Graziani LJ, Kornhauser MS. High-frequency jet ventilation in the early management of respiratory distress syndrome is associated with a greater risk for adverse outcomes. Pediatrics. 1996;98:1035–1043. [PubMed] [Google Scholar]
- 7.Bryan AC, Froese AB. Reflections on the HIFI trial. Pediatrics. 1991;87:565–567. [PubMed] [Google Scholar]
- 8.Bohn D. The history of high-frequency ventilation. Respir Care Clin N Am. 2001;7:535–548. doi: 10.1016/s1078-5337(05)70005-8. [DOI] [PubMed] [Google Scholar]
- 9.Acute Respiratory Distress Syndrome Network Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Engl J Med. 2000;342:1301–1308. doi: 10.1056/NEJM200005043421801. [DOI] [PubMed] [Google Scholar]
- 10.Krishnan JA, Brower RG. High-frequency ventilation for acute lung injury and ARDS. Chest. 2000;118:795–807. doi: 10.1378/chest.118.3.795. [DOI] [PubMed] [Google Scholar]
- 11.Slutsky AS, Brown R, Lehr J. High-frequency ventilation: a promising new approach to mechanical ventilation. Medical Instrumentation. 1981;15:229–233. [PubMed] [Google Scholar]
- 12.Derdak S. High-frequency oscillatory ventilation for acute respiratory distress syndrome in adult patients. Crit Care Med. 2003;31:S317–S323. doi: 10.1097/01.CCM.0000057910.50618.EB. [DOI] [PubMed] [Google Scholar]
- 13.Slutsky AS, Drazen JM. Ventilation with small tidal volumes. N Engl J Med. 2002;347:630–631. doi: 10.1056/NEJMp020082. [DOI] [PubMed] [Google Scholar]
- 14.Chang HK. Mechanisms of gas transport during ventilation by high-frequency oscillation. J Appl Physiol. 1984;56:553–563. doi: 10.1152/jappl.1984.56.3.553. [DOI] [PubMed] [Google Scholar]
- 15.Pillow JJ. High-frequency oscillatory ventilation: mechanisms of gas exchange and lung mechanics. Crit Care Med. 2005;33:S135–S141. doi: 10.1097/01.ccm.0000155789.52984.b7. [DOI] [PubMed] [Google Scholar]
- 16.Frank JA, Matthay MA. Science review: mechanisms of ventilator-induced injury. Crit Care. 2003;7:233–241. doi: 10.1186/cc1829. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Slutsky AS, Kamm RD, Rossing TH. Effects of frequency, tidal volume, and lung volume on CO2 elimination in dogs by high frequency (2–30 Hz), low tidal volume ventilation. J Clin Invest. 1981;68:1475–1484. doi: 10.1172/JCI110400. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Pillow JJ, Sly PD, Hantos Z. Dependence of intrapulmonary pressure amplitudes on respiratory mechanics during high-frequency oscillatory ventilation in preterm lambs. Pediatr Res. 2002;52:538–544. doi: 10.1203/00006450-200210000-00013. [DOI] [PubMed] [Google Scholar]
- 19.Sedeek KA, Takeuchi M, Suchodolski K. Determinants of tidal volume during high-frequency oscillation. Crit Care Med. 2003;31:227–231. doi: 10.1097/00003246-200301000-00035. [DOI] [PubMed] [Google Scholar]
- 20.Hager DN, Fessler MH, Fuld MK. Effects of frequency (f) and pressure amplitude (P) on tidal volumes (Vt) in adults with ARDS during high-frequency oscillatory ventilation (HFOV) [abstract] Proc Am Thorac Soc. 2006;3:A376. [Google Scholar]
- 21.Hamilton PP, Onayemi A, Smyth JA. Comparison of conventional and high-frequency ventilation: oxygenation and lung pathology. J Appl Physiol. 1983;55:131–138. doi: 10.1152/jappl.1983.55.1.131. [DOI] [PubMed] [Google Scholar]
- 22.Luecke T, Herrmann P, Kraincuk P. Computed tomography scan assessment of lung volume and recruitment during high-frequency oscillatory ventilation. Crit Care Med. 2005;33:S155–S162. doi: 10.1097/01.ccm.0000155916.47455.df. [DOI] [PubMed] [Google Scholar]
- 23.Goddon S, Fujino Y, Hromi JM. Optimal mean airway pressure during high-frequency oscillation: predicted by the pressure-volume curve. Anesthesiology. 2001;94:862–869. doi: 10.1097/00000542-200105000-00026. [DOI] [PubMed] [Google Scholar]
- 24.Luecke T, Meinhardt J, Herrmann P. Setting mean airway pressure during high-frequency oscillatory ventilation according to the static pressure–volume curve in surfactant-deficient lung injury: a computed tomography study. Anesthesiology. 2003;99:1313–1322. doi: 10.1097/00000542-200312000-00012. [DOI] [PubMed] [Google Scholar]
- 25.Imai Y, Nakagawa S, Ito Y. Comparison of lung protection strategies using conventional and high-frequency oscillatory ventilation. J Appl Physiol. 2001;91:1836–1844. doi: 10.1152/jappl.2001.91.4.1836. [DOI] [PubMed] [Google Scholar]
- 26.McCulloch PR, Forkert PG, Froese AB. Lung volume maintenance prevents lung injury during high frequency oscillatory ventilation in surfactant-deficient rabbits. Am Rev Respir Dis. 1988;137:1185–1192. doi: 10.1164/ajrccm/137.5.1185. [DOI] [PubMed] [Google Scholar]
- 27.Rotta AT, Gunnarsson B, Fuhrman BP. Comparison of lung protective ventilation strategies in a rabbit model of acute lung injury. Crit Care Med. 2001;29:2176–2184. doi: 10.1097/00003246-200111000-00021. [DOI] [PubMed] [Google Scholar]
- 28.Vazquez de Anda GF, Hartog A, Verbrugge SJ. The open lung concept: pressure-controlled ventilation is as effective as high-frequency oscillatory ventilation in improving gas exchange and lung mechanics in surfactant-deficient animals. Intensive Care Med. 1999;25:990–996. doi: 10.1007/s001340050994. [DOI] [PubMed] [Google Scholar]
- 29.Gommers D, Hartog A, Schnabel R. High-frequency oscillatory ventilation is not superior to conventional mechanical ventilation in surfactant-treated rabbits with lung injury. Eur Respir J. 1999;14:738–744. doi: 10.1034/j.1399-3003.1999.14d03.x. [DOI] [PubMed] [Google Scholar]
- 30.Vazquez de Anda GF, Gommers D, Verbrugge SJ. Mechanical ventilation with high positive end-expiratory pressure and small driving pressure amplitude is as effective as high-frequency oscillatory ventilation to preserve the function of exogenous surfactant in lung-lavaged rats. Crit Care Med. 2000;28:2921–2925. doi: 10.1097/00003246-200008000-00039. [DOI] [PubMed] [Google Scholar]
- 31.Brederlau J, Muellenbach R, Kredel M. High frequency oscillatory ventilation and prone positioning in a porcine model of lavage-induced acute lung injury. BMC Anesthesiol. 2006;6:4. doi: 10.1186/1471-2253-6-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Krishnan RK, Meyers PA, Worwa C. Standardized lung recruitment during high frequency and conventional ventilation: similar pathophysiologic and inflammatory responses in an animal model of respiratory distress syndrome. Intensive Care Med. 2004;30:1195–1203. doi: 10.1007/s00134-004-2204-x. [DOI] [PubMed] [Google Scholar]
- 33.Sedeek KA, Takeuchi M, Suchodolski K. Open-lung protective ventilation with pressure control ventilation, high-frequency oscillation, and intratracheal pulmonary ventilation results in similar gas exchange, hemodynamics, and lung mechanics. Anesthesiology. 2003;99:1102–1111. doi: 10.1097/00000542-200311000-00016. [DOI] [PubMed] [Google Scholar]
- 34.Muellenbach RM, Kredel M, Zollhoefer B. Sustained inflation and incremental mean airway pressure trial during conventional and high-frequency oscillatory ventilation in a large porcine model of acute respiratory distress syndrome. BMC Anesthesiol. 2006;6:8. doi: 10.1186/1471-2253-6-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Fort P, Farmer C, Westerman J. High-frequency oscillatory ventilation for adult respiratory distress syndrome: a pilot study. Crit Care Med. 1997;25:937–947. doi: 10.1097/00003246-199706000-00008. [DOI] [PubMed] [Google Scholar]
- 36.Claridge JA, Hostetter RG, Lowson SM. High-frequency oscillatory ventilation can be effective as rescue therapy for refractory acute lung dysfunction. Am Surg. 1999;65:1092–1096. [PubMed] [Google Scholar]
- 37.Mehta S, Lapinsky SE, Hallett DC. Prospective trial of high-frequency oscillation in adults with acute respiratory distress syndrome. Crit Care Med. 2001;29:1360–1369. doi: 10.1097/00003246-200107000-00011. [DOI] [PubMed] [Google Scholar]
- 38.Cartotto R, Cooper AB, Esmond JR. Early clinical experience with high-frequency oscillatory ventilation for ARDS in adult burn patients. J Burn Care Rehabil. 2001;22:325–333. doi: 10.1097/00004630-200109000-00006. [DOI] [PubMed] [Google Scholar]
- 39.Andersen FA, Guttormsen AB, Flaatten HK. High frequency oscillatory ventilation in adult patients with acute respiratory distress syndrome: a retrospective study. Acta Anaesthesiol Scand. 2002;46:1082–1088. doi: 10.1034/j.1399-6576.2002.460905.x. [DOI] [PubMed] [Google Scholar]
- 40.David M, Weiler N, Heinrichs W. High-frequency oscillatory ventilation in adult acute respiratory distress syndrome. Intensive Care Med. 2003;29:1656–1665. doi: 10.1007/s00134-003-1897-6. [DOI] [PubMed] [Google Scholar]
- 41.David M, Karmrodt J, Weiler N. High-frequency oscillatory ventilation in adults with traumatic brain injury and acute respiratory distress syndrome. Acta Anaesthesiol Scand. 2005;49:209–214. doi: 10.1111/j.1399-6576.2004.00570.x. [DOI] [PubMed] [Google Scholar]
- 42.Esteban A, Alia I, Gordo F. Prospective randomized trial comparing pressure-controlled ventilation and volume-controlled ventilation in ARDS. Chest. 2000;117:1690–1696. doi: 10.1378/chest.117.6.1690. [DOI] [PubMed] [Google Scholar]
- 43.Ranieri VM, Suter PM, Tortorella C. Effect of mechanical ventilation on inflammatory mediators in patients with acute respiratory distress syndrome: a randomized controlled trial. JAMA. 1999;282:54–61. doi: 10.1001/jama.282.1.54. [DOI] [PubMed] [Google Scholar]
- 44.Frutos-Vivar F, Nin N, Esteban A. Epidemiology of acute lung injury and acute respiratory distress syndrome. Curr Opin Crit Care. 2004;10:1–6. doi: 10.1097/00075198-200402000-00001. [DOI] [PubMed] [Google Scholar]
- 45.Derdak S, Mehta S, Stewart TE. High-frequency oscillatory ventilation for acute respiratory distress syndrome in adults: a randomized, controlled trial. Am J Respir Crit Care Med. 2002;166:801–808. doi: 10.1164/rccm.2108052. [DOI] [PubMed] [Google Scholar]
- 46.Bollen CW, van Well GT, Sherry T. High frequency oscillatory ventilation compared with conventional mechanical ventilation in adult respiratory distress syndrome: a randomized controlled trial. Crit Care. 2005;9:430–439. doi: 10.1186/cc3737. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Ferguson ND, Chiche J-D, Kacmarek RM. Combining high-frequency oscillatory ventilation and recruitment maneuvers in adults with early acute respiratory distress syndrome: the Treatment with Oscillation and an Open Lung Strategy (TOOLS) Trial pilot study. Crit Care Med. 2005;33:479–486. doi: 10.1097/01.ccm.0000155785.23200.9e. [DOI] [PubMed] [Google Scholar]
- 48.Mehta S, MacDonald R, Hallett DC. Acute oxygenation response to inhaled nitric oxide when combined with high-frequency oscillatory ventilation in adults with acute respiratory distress syndrome. Crit Care Med. 2003;31:383–389. doi: 10.1097/01.CCM.0000049953.86613.02. [DOI] [PubMed] [Google Scholar]
- 49.Varkul MD, Stewart TE, Lapinsky SE. Successful use of combined high-frequency oscillatory ventilation, inhaled nitric oxide, and prone positioning in the acute respiratory distress syndrome. Anesthesiology. 2001;95:797–799. doi: 10.1097/00000542-200109000-00038. [DOI] [PubMed] [Google Scholar]
- 50.Papazian L, Gainnier M, Marin V. Comparison of prone positioning and high-frequency oscillatory ventilation in patients with acute respiratory distress syndrome. Crit Care Med. 2005;33:2162–2171. doi: 10.1097/01.ccm.0000181298.05474.2b. [DOI] [PubMed] [Google Scholar]
- 51.Mehta S, Granton J, MacDonald RJ. High-frequency oscillatory ventilation in adults: the Toronto experience. Chest. 2004;126:518–527. doi: 10.1378/chest.126.2.518. [DOI] [PubMed] [Google Scholar]
- 52.Muscedere J, Mullen J, Gan K. Tidal ventilation at low airway pressures can augment lung injury. Am J Respir Crit Care Med. 1994;149:1327–1334. doi: 10.1164/ajrccm.149.5.8173774. [DOI] [PubMed] [Google Scholar]
- 53.Parker JC, Hernandez LA, Peevy KJ. Mechanisms of ventilator-induced lung injury. Crit Care Med. 1993;21:131–143. doi: 10.1097/00003246-199301000-00024. [DOI] [PubMed] [Google Scholar]
- 54.Tsuno K, Miura K, Takeya M. Histopathologic pulmonary changes from mechanical ventilation at high peak airway pressures. Am Rev Respir Dis. 1991;143:1115–1120. doi: 10.1164/ajrccm/143.5_Pt_1.1115. [DOI] [PubMed] [Google Scholar]
- 55.Slutsky AS, Tremblay LN. Multiple system organ failure: is mechanical ventilation a contributing factor? Am J Respir Crit Care Med. 1998;157:1721–1725. doi: 10.1164/ajrccm.157.6.9709092. [DOI] [PubMed] [Google Scholar]
- 56.Bollen CW, Uiterwaal CS, van Vught AJ. Systematic review of determinants of mortality in high frequency oscillatory ventilation in acute respiratory distress syndrome. Crit Care. 2006;10:R34. doi: 10.1186/cc4824. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Wiedemann HP, Wheeler AP, National Heart, Lung and Blood Institute Acute Respiratory Distress Syndrome (ARDS) Clinical Trials Network Comparison of two fluid-management strategies in acute lung Injury. N Engl J Med. 2006;354:2564–2575. doi: 10.1056/NEJMoa062200. [DOI] [PubMed] [Google Scholar]
- 58.David M, von Bardeleben RS, Weiler N. Cardiac function and haemodynamics during transition to high-frequency oscillatory ventilation. Eur J Anaesthesiol. 2004;21:944–952. doi: 10.1017/s0265021504000328. [DOI] [PubMed] [Google Scholar]
- 59.Kress JP, Pohlman AS, O'Connor MF. Daily interruption of sedative infusions in critically ill patients undergoing mechanical ventilation. N Engl J Med. 2000;342:1471–1477. doi: 10.1056/NEJM200005183422002. [DOI] [PubMed] [Google Scholar]
- 60.Brook AD, Ahrens TS, Schaiff R. Effect of a nursing-implemented sedation protocol on the duration of mechanical ventilation. Crit Care Med. 1999;27:2609–2615. doi: 10.1097/00003246-199912000-00001. [DOI] [PubMed] [Google Scholar]
- 61.Latronico N, Peli E, Botteri M. Critical illness myopathy and neuropathy. Curr Opin Crit Care. 2005;11:126–132. doi: 10.1097/01.ccx.0000155357.24360.89. [DOI] [PubMed] [Google Scholar]
- 62.Sweeney AM, Lyle J, Ferguson ND. Nursing and infection-control issues during high-frequency oscillatory ventilation. Crit Care Med. 2005;33(suppl):S204–S208. doi: 10.1097/01.ccm.0000155918.29268.84. [DOI] [PubMed] [Google Scholar]
- 63.Pachl J, Roubik K, Waldauf P. Normocapnic high-frequency oscillatory ventilation affects differently extrapulmonary and pulmonary forms of acute respiratory distress syndrome in adults. Physiol Res. 2006;55:15–24. doi: 10.33549/physiolres.930775. [DOI] [PubMed] [Google Scholar]
- 64.Finkielman JD, Gajic O, Farmer JC. The initial Mayo Clinic experience using high-frequency oscillatory ventilation for adult patients: a retrospective study. BMC Emerg Med. 2006;6:2. doi: 10.1186/1471-227X-6-2. [DOI] [PMC free article] [PubMed] [Google Scholar]


