Dear Editor,
Recently, Wang and colleagues reported in this journal the new threat of novel SARS-like coronavirus in China.1 During the last several decades, humans had been affected by six human coronaviruses (HCoV)—HCoV-NL63, HCoV-HKU1, HCoV-229E, HCoV-OC43, severe acute respiratory syndrome coronavirus (SARS-CoV), and Middle East respiratory syndrome coronavirus (MERS-CoV)—the last two of which caused severe respiratory symptoms and human death on a globe scale.2 On December 2019, a human case in Wuhan, China infected with novel human coronavirus (HCoV) was first reported, who exhibited fever, difficulty with breathing, and invasive lesions in the lungs. This novel HCoV was subsequently designated as 2019-nCoV by World Health Organization (WHO). As of 4, February 2020, a total of 20,520 human cases (of which 426 fatal) of pneumonia infected with the 2019-nCoV had been demonstrated in all of the provinces of China (Fig. 1 ), with fatality rate of ∼5% in Wuhan and ∼0.8% in the rest of cities of China, respectively. Strikingly, the 2019-nCoV had caused family case clusters and sustained human-to-human transmission.3 , 4 On January 30, 2020, WHO declared the 2019-nCoV epidemic as a Public Health Emergency of International Concern (https://www.who.int), posing a new public health concern.
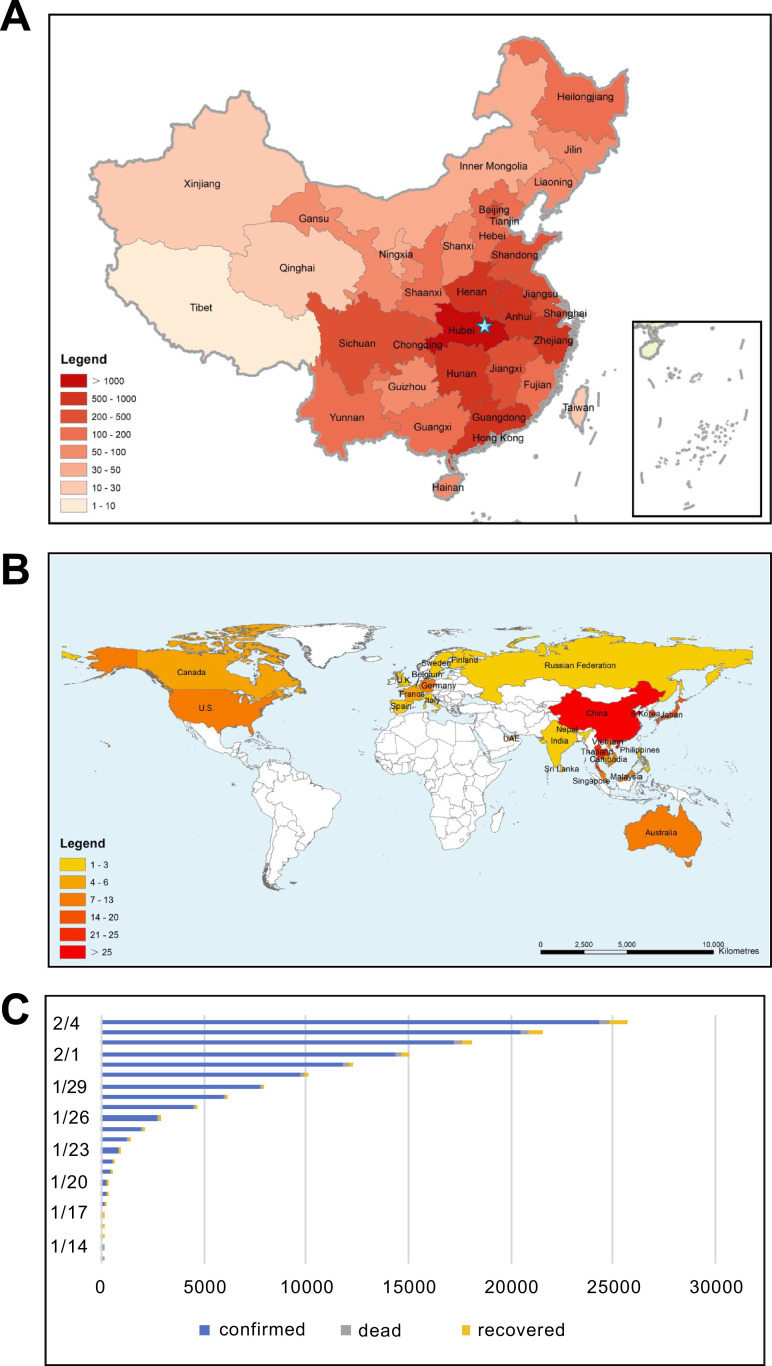
Fig. 1.
Geographic distribution of the 2019-nCoV and the number of human cases. Geographic distribution of the 2019-nCoV in(A)China and(B)the world, respectively. The color of bar chart represents the number of human infection. The blue star represents the location of Wuhan, China. Data are available from the World Health Organization (https://www.who.int) and National Health and Family Planning Commission of the People's Republic of China (http://www.nhfpc.gov.cn). The map in the inset indicates islands in the South China Sea. The map was designed using ArcGIS Desktop 10.4 software (http://www.esri.com/software/arcgis/arcgis-for-desktop/). (C) The number of human cases by date are plotted, which shows a gradual increase over time. The blue bar chart represents the numbers of confirmed cases, and the gray bar chart represents the death toll, and the yellow bar chart represents the numbers of recovered cases.
The emergence of novel 2019-nCoV highlights the necessity of tracing the origin of virus and the updated prevention and control systems in order to avert outbreaks. We found that the genomes of the novel 2019-nCoV were genetically closely related to beta SARS-related CoV (SARSr-CoV) circulating in China and had undergone genetic recombination with SARSr-CoV (Fig. 2 and Supplementary Figure S1-S3). The overall genome identity of the 2019-nCoV and SARSr-CoV was ranging from 82% to 89%. With rapid dissemination of the 2019-nCoV, the viruses had been transmitted rapidly in more than 25 countries, and a steep increase in human infection with the 2019-nCoV occurred in China (Fig. 1). To further explore the genetic evolution of the 2019-nCoV, phylogenic relationships of 31 isolates examined in this study were explored and divided into four genotypes, including G1, G2, G3, and G4. We found that 25 isolates clustered together and had been circulating in Thailand and multiple provinces (e.g. Taiwan, Guangdong, Zhejiang, and Hubei) of China, suggestive of the ongoing co-circulation of the viruses. The 2019-nCoV circulating in USA and Wuhan, China clustered into an independent cluster. However, interestingly, the SZTH-002, 20SF013, and SZTH-001 strains in Guangdong province were located at basal branch of the 2019-nCoV (Fig. 2), indicative of a single origin. The genetic diversity of RNA-dependent RNA polymerase of the 2019-nCoV was very small (Supplementary Figure S1). By contrast, the Spike (S) genes of some 2019-nCoV prevailing in Guangdong province were found at the root of the 2019-nCoV in Wuhan (Supplementary Figure S2). These findings indicated that the 2019-nCoV were infected from different regions in Wuhan and had been undergoing continuous evolution and dissemination in different regions. Compared with the rapid mutation of the influenza A viruses, the degree of diversification of the 2019-nCoV was much smaller. Nevertheless, we cannot rule out if the 2019-nCoV continue evolving to become more transmissible and virulent in humans in the near future.
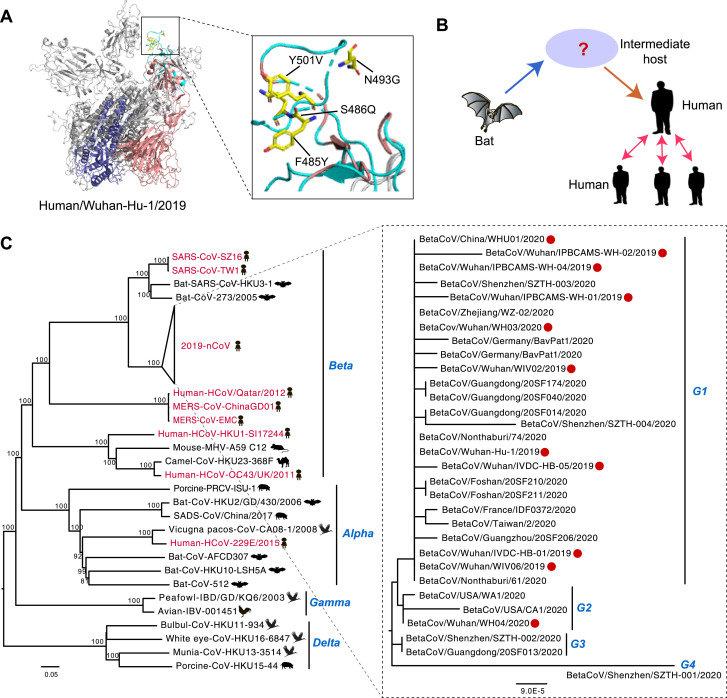
Fig. 2.
Evolutionary history of the 2019-nCoV. (A) Structural analysis of envelope spike (S) protein of novel coronaviruses. The red and blue regions indicate the spike protein 1 and spike protein 2, respectively. The wathet blue region indicates the receptor binding region of 2019-nCoV. The correspondencing amino acids to the three-dimensional (3D) structure of the S protein were mapped using MacPymol (http://www.pymol.org/). (B) A simple model of 2019-nCoV origin inferred from phylogenic tree and clinical feature of humans infected with the 2019-nCoV. (C) Maximum likelihood tree of the full-length genome of coronaviruses using MEGA 7 version. Red color indicates the human-origin coronaviruses, and red dot represents the isolates in Wuhan, China. The scale bar represents the number of nucleotide substitutions per site (subs/site).
The S protein mediates receptor binding and membrane fusion, and of particular note, it is of great importance to determine host tropism and transmission capacity.5 Zhou et al. demonstrated that the 2019-nCoV use the same cell entry receptor, ACE2, as SARS-CoV.6 The receptor binding region of the 2019-nCoV was more similar to that of SARS-CoV; however, we found that four amino acid substitutions in the receptor binding region of the 2019-nCoV, including S486Q, F485Y, N493G, and Y501V substitutions (2019-nCoV numbering), were different from that of SARS-CoV (Fig. 2), which might affect the receptor binding ability.
Bats provide a rich “gene pool” for interspecies exchange of genetic fragments of CoV.7 Continuous surveillance in bats provide us a clue to the correlation between the 2019-nCoV and the animal origin CoV. Despite the shared cluster between the 2019-nCoV and bat SARSr-CoV, we cannot infer that the reservoir of the 2019-nCoV was originated from bats. Most of the patients infected with novel 2019-nCoV had a history to the seafood and live animal markets, and the vendor used to sale wild animal species, including marmot, snake, leopard cat, bamboo rat, badger, and hedgehog in Huanan seafood wholesale market (Supplementary Figure S4), all of which were susceptible to the novel CoV in nature, indicating that it remains likely there was intermediate hosts in the transmission cascade from bats to humans (Fig. 2). However, a question of a public health interest is which intermediate hosts harbor the 2019-nCoV that could infect humans, which should be examined in greater detail. Recently, the continuous interspecies transmission events of CoV occurred, including the emergence of MERS-CoV from camels to humans and swine acute diarrhea syndrome CoV from bat to swine, posing serious threats to public health.8 , 9 With the tradition of feeding wild animals for food or use in traditional medicine in China, wild birds, mammals, and reptiles carrying the novel zoonotic viruses flowed frequently in trading center, which had considerable potential to transmit to humans of emerging viruses.
In 2018, China had participated a Global Virome Project to identify unknown viruses from wildlife to better prepare for the epidemics of infectious diseases in humans.10 With multiple species of CoV circulating in different animal species that could be transmitted to humans, no one knows when or where the next outbreak will occur. Nevertheless, decreasing the risk for the spread of novel viruses including reducing contact among humans and wild animal species and stopping novel viruses at their origins is urgently needed. We call upon wildlife biologists, ecologists, doctors, and veterinarians should promote exchange and share data across disciplines as a mean to minimize the potential for pandemics of the 2019-nCoV.
Declaration of Competing Interest
All authors have no potential conflicts of interest to disclose.
Acknowledgement
We sincerely thank the authors of the human 2019 coronavirus from GISAID EpiFlu™ Database. This work was supported by the National Natural Science Foundation of China (31941014, 31830097, 31672586), Key Research and Development Program of Guangdong Province (2019B020218004), Earmarked Fund for China Agriculture Research System (CARS-41-G16), Guangdong Province Universities and Colleges Pearl River Scholar Funded Scheme (2018, Wenbao Qi), and Young Scholars of Yangtze River Scholar Professor Program (2019, Wenbao Qi).
Footnotes
Supplementary material associated with this article can be found, in the online version, at doi: 10.1016/j.jinf.2020.02.001.
Contributor Information
Ming Liao, Email: mliao@scau.edu.cn.
Wenbao Qi, Email: qiwenbao@scau.edu.cn.
Appendix. Supplementary materials
References
- 1.Wang R., Zhang X., Irwin D.M., Shen Y. Emergence of SARS-like Coronavirus poses new challenge in China. J Infect. 2020 doi: 10.1016/j.jinf.2020.01.017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Su S., Wong G., Shi W. Epidemiology, genetic recombination, and pathogenesis of coronaviruses. Trends Microbiol. 2016;24(6):490–502. doi: 10.1016/j.tim.2016.03.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Huang C., Wang Y., Li X., Ren L., Zhao J., Hu Y. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. 2020 doi: 10.1016/S0140-6736(20)30183-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Chan J.F., Yuan S., Kok K.H., To K.K., Chu H., Yang J. A familial cluster of pneumonia associated with the 2019 novel coronavirus indicating person-to-person transmission: a study of a family cluster. Lancet. 2020 doi: 10.1016/S0140-6736(20)30154-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Lu G., Wang Q., Gao G.F. Bat-to-human: spike features determining ‘host jump’ of coronaviruses SARS-CoV, MERS-CoV, and beyond. Trends Microbiol. 2015;23:468–478. doi: 10.1016/j.tim.2015.06.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Zhou P., Yang X., Wang X., Hu B., Zhang L., Zhang W. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature. 2020 doi: 10.1038/s41586-020-2012-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Hu B., Zeng L., Yang X., Ge X., Zhang W., Li B. Discovery of a rich gene pool of bat SARS-related coronaviruses provides new insights into the origin of Sars coronavirus. Plos Pathog. 2017;13(11) doi: 10.1371/journal.ppat.1006698. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Shen X., Sabir J.S.M., Irwin D.M., Shen Y. Vaccine against Middle East respiratory syndrome coronavirus. Lancet Infect Dis. 2019;19(10):1053–1054. doi: 10.1016/S1473-3099(19)30476-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Zhou P., Fan H., Lan T., Yang X., Shi W., Zhang W. Fatal swine acute diarrhoea syndrome caused by an HKU2-related coronavirus of bat origin. Nature. 2018;556(7700):255–258. doi: 10.1038/s41586-018-0010-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Carroll D., Daszak P., Wolfe N.D., Gao G.F., Morzaria S., Pablos-Méndez A. The global virome project. Science. 2018;359(6378):872–874. doi: 10.1126/science.aap7463. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.