Influenza A H1N1 (swine flu) has spread around the world with what has, at times, felt like horrifying speed, but there is a feeling that many of us have dodged a bullet. Of the 2384 laboratory-confirmed cases reported in 24 countries, as TLID went to press, there had been 44 deaths, 42 of which were in Mexico. These numbers are far lower than the annual toll from seasonal influenza, which kills hundreds of people every day in the peak season.
But epidemiologists are still largely in the dark about how the virus will continue to spread and, ultimately, how severe the disease it causes will be. Since the first cases were identified in Mexico in late April, WHO has upped its pandemic alert level from three to five, and seems to be on the brink of moving to level six—the highest possible—which would mean the virus had reached pandemic status. But have countries prepared effective strategies to cope with this?
The threats of severe acute respiratory syndrome (SARS) and H5N1 a few years ago prompted the world to set up plans to deal with the possibility that these viruses would, by developing sustained human-to-human transmission, trigger a pandemic. The chaos caused by the outbreaks revealed just how badly countries around the world—increasingly linked by frequent international travel and growing globalisation—were prepared to deal with a worldwide infectious disease pandemic. Pandemic preparedness has come a long way since those two viruses caused worldwide alarm, says Sandra Mounier-Jack (London School of Hygiene and Tropical Medicine, London, UK) but there are holes in many countries' plans.
In 2006, with her colleague Richard Coker, Mounier-Jack compared the strategies of Asia-Pacific countries with those in Europe. Many of the Asia-Pacific plans, had a stronger focus on early containment of disease and “social distancing”. Developing countries are likely to need this strategy more than developed ones, Mounier-Jack told TLID, because of chronic shortages of antiviral drugs and vaccines. But the problem with focusing on surveillance and monitoring, she says, is that poor countries, especially those in Asia, “don't have a plan B if the virus becomes pandemic”.
Coker agrees. He told TLID that developing countries are “severely underprepared” for a pandemic. Furthermore, many existing plans focus, somewhat short-sightedly, “on avian influenza in poultry”.
The duo's analyses showed that countries, including those in Europe, “did not adequately address organisational responsibility at the local level”. Even now, these plans have only really been tested through desk-based exercises, says Mounier-Jack. Whether strategic plans are operational is the key question, says Coker. In southeast Asia, for example, only Thailand has evaluated its preparedness. “Despite being a relatively affluent country in the region, it would have substantial resource shortages if a pandemic is anything but mild”, he says. “Without this sort of analysis”, Coker adds, “policy makers risk making knee-jerk decisions in their allocation of resources that may be ineffective, inefficient, and inequitable”.
A 2007 survey of 30 countries by the European Centre for Disease Prevention and Control revealed that European preparedness was patchy too. Many plans included only half of the WHO recommendations for dealing with pandemics.
The challenges Mounier-Jack foresees are implementational—how responsibility is divided between primary and secondary care, for example—rather than in technical or medical problems. She also advocates a cohesive multisectoral approach between the food industry, the health-care sector, and government.
Quarantine and travel bans might seem an intuitive way to curb the spread, but the reality is more complicated. For one thing, health officials have been at odds over the advice the public should follow. In late April, the European Union's health commissioner Androulla Vassiliou said Europeans “should avoid travelling to Mexico or the USA unless it's very urgent”. Almost immediately, Richard Besser, the acting director for the US Centers for Disease Control and Prevention, and Michael Bloomberg, New York City's mayor, disagreed.
Apart from the fact that “travel restrictions would have very little effect on stopping the virus from spreading”, says Alessandro Vespignani (Indiana University, Bloomington, IN, USA), “it would be highly disruptive to the global community”. Vespignani is modelling the spread of H1N1 with travel data, high-definition geographical population data, and disease dynamics, including the number of people each infected person passes it on to (reproductive rate). Estimates for H1N1's reproductive rates are 1·0–1·4, which is fairly low given that seasonal influenza has a rate of 1·5–3·0.
Vespignani's predictions for the rest of May “point to a steady increase in the number of observed cases”. More worryingly, he told TLID that “just in the USA, we could hit several thousand cases”. He hopes, however, that he will soon see discrepancies between his model and the reality on the ground. Although this is not a scenario scientists usually wish for, in this case it would mean that containment and mitigation measures had been successful.
A stadium worker watches a football match from which the public have been excluded in Mexico City
© 2009 Claudio Cruz/AP/Press Association Images
H1N1's seemingly low reproductive rate does not mean we should be complacent: a 2006 study of the rate of the 1918 pandemic influenza suggests that the rate of the first wave of the virus was about 1·5, but that of the second wave was 3·5. Coker points out that H5N1 is still present in many countries and is endemic in southeast Asia. One concern at the back of many virologists' minds is the prospect, however remote, that the H1N1 might recombine with the virulent H5N1 to form a so-called Armageddon virus. If that happened, says Coker, antivirals would need to be rapidly distributed; the problem is that those drugs are currently being allocated to deal with the existing H1N1 virus.
For now, though, the northern hemisphere is out of its annual influenza season and there is a window for H1N1 vaccine production. An initial idea to incorporate this strain into the vaccine against regular seasonal influenza has been dismissed, and WHO is due to talk with vaccine manufacturers about switching to production of a pandemic H1N1 vaccine. On May 6, Marie-Paule Kieny, director of WHO's vaccine research initiative, said WHO estimated that the world's vaccine production capacity could make 1 billion to 2 billion doses of H1N1 vaccine. During the H5N1 outbreaks, tests indicated that, unlike seasonal influenza, people needed two doses for a vaccine to be effective. Whether people would need two doses of H1N1 vaccine is too early to say, said Kieny.
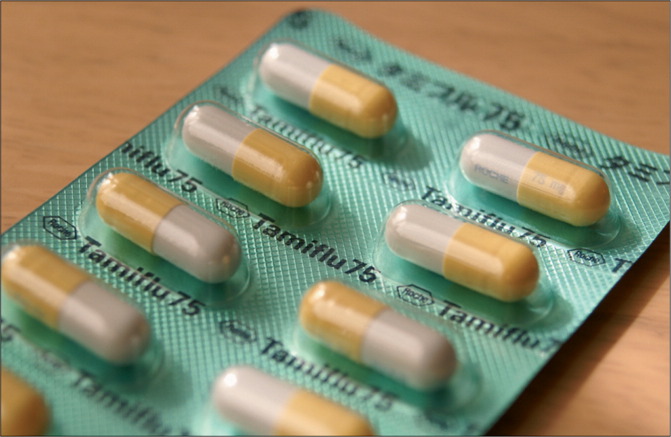
Influenza A H1N1 is susceptible to oseltamivir—but for how long?
© 2009 kanonn
For developing countries, these issues are less pressing than the question of whether they can get their hands on the vaccine at all. So, on May 19, WHO's Director General Margaret Chan and UN Secretary General Ban Ki-Moon are meeting in Geneva with vaccine manufacturers to appeal to “corporate responsibility” and discuss “avenues to ensure equitable access for developing countries to this vaccine”.
If doomsayers are right, and H1N1 does become pandemic, the biggest guns in the drug arsenal are oseltamivir and zanamivir. However, monotherapy is vulnerable to resistance. “N1 genes are more prone to mutations, and oseltamivir-resistance occurrence in N1 genes is not uncommon”, says Alan McNally (Nottingham Trent University, Nottingham, UK). “Indeed the vast majority of seasonal H1N1 isolates this past autumn–winter were oseltamivir resistant. This undoubtedly poses a threat, and is something that reference labs will be monitoring extremely closely”, says McNally.
WHO is at pains to stress that raising the alert to level six would not relate to the severity of the infection. If anything, initial indications are that the virus is no more harmful than seasonal influenza. H1N1 is a hybrid of virus genes originating in viruses of pigs, birds, and human beings. Wendy Barclay (Imperial College, London, UK) has analysed H1N1's genes and says that it has “no genetic features of a highly pathogenic virus at all”. She told TLID that “it looks as though this virus should target the upper respiratory tract and not the lung”. This is important because viruses that bind in the lower respiratory tract, such as H5N1, cause more severe illness. Barclay adds that the virus's NS1 protein “looks normal, so we would not expect a cytokine storm”.
Epidemiologists are also scrabbling to collect as much information as they can about which groups of people are the hardest hit, and to find out why some people develop more severe symptoms than others. On May 5, WHO's assistant director-general for health security and environment, Keiji Fukuda, told reporters that the average age of infection was the mid-20s. But he pointed out that the infections tend to be seen in travellers, so does the age reflect a characteristic of the virus or the fact that young people are most likely to travel? Older people might have an immunity if they have been exposed to components of the virus before.
Countries worldwide will now be figuring out how to prepare for a relatively unknown quantity. Did scientists and health officials take their eye off the ball after the initial fears of a bird flu or SARS pandemic faded? It is understandable that pandemic fatigue set in, says Mounier-Jack, since countries have a range of health-care concerns to deal with. But should scientists have seen this coming? In 2004, Richard Webby and Robert Webster (St Jude Children's Research Hospital, TN, USA) raised a note of concern that in 1998 swine H1N1 had recombined with human and bird viruses. They warned that “the growing complexity of influenza at this animal–human interface and the presence of viruses with a seemingly high affinity for reassortment makes the US swine population an increasingly important reservoir of viruses with human pandemic potential”. Knowing this potential is one thing, but it is not clear “how one would prevent that from happening”, says Barclay.
As Fukuda told reporters on May 4, “there is no timetable for how the virus will spread”. For now, it is going to be a matter of watching and waiting to see what H1N1 does next.