Fungal peritonitis, a relatively uncommon but serious complication of peritoneal dialysis (PD), is associated with high rates of technique failure (40%) and mortality (15%–50%).1,2 Therefore, immediate PD catheter removal followed by antifungal agent administration for a minimum period of 2 weeks is strongly recommended by the International Society for Peritoneal Dialysis 2016 peritonitis guideline.3 Despite treatment according to this guideline, only one-third of patients with fungal peritonitis are able to resume PD.4 The poor treatment outcomes of fungal peritonitis are hampered by the lack of a sensitive biomarker that can facilitate timely diagnosis and treatment. Serum levels of the fungal cell wall component galactomannan (GM), which is shed by fungi during their growth and death,5 may help address this gap in clinical care. This biomarker has been used to aid in the diagnosis of systemic and invasive fungal infections, as well as in monitoring the treatment response and relapse of fungal infections, particularly of the respiratory system.5 A serum GM index (GMI) of ≥0.5 has previously been used to diagnose suspected fungal pulmonary infections.6,7 As a proof of concept, the potential value of serum and PD effluent GMI in diagnosing and risk-stratifying patients with fungal peritonitis on PD was assessed in the present study.
Results
Patient Demographics and Characteristics
Participant flow is shown in Figure 1. There were no significant differences among patients with fungal peritonitis (n = 23), bacterial peritonitis (n = 21), and no peritonitis (n = 19) with respect to age, sex, PD vintage, residual kidney function, and comorbidities (Table 1, Supplementary Table S1). As expected, controls without peritonitis had no peritonitis symptoms, higher serum albumin concentrations, and lower PD effluent cell counts than did the other groups. The most common fungal pathogen was Candida spp. followed by Trichosporon spp., Aspergillus spp., and Fusarium spp. (Table 2).
Figure 1.
Patient enrollment and randomization flow diagram. GMI, galactomannan index; PD, peritoneal dialysis.
Table 1.
Clinical characteristics of patients on PD in this study
| Characteristic | Fungal peritonitis (n = 23) | Bacterial peritonitis (n = 21) | Nonperitonitis (n = 19) |
|---|---|---|---|
| Male sex | 10 (43) | 10 (48) | 11 (58) |
| Age (yr) | 51.3 ± 13.3 | 55.4 ± 16.0 | 68.1 ± 7.1 |
| Diabetes mellitus | 12 (52) | 9 (43) | 10 (53) |
| Hypertension | 18 (78) | 17 (81) | 14 (74) |
| Serum hemoglobin level (g/dl) | 10.2 ± 3.2 | 10.7 ± 2.7 | 11.9 ± 1.3 |
| Serum albumin level (g/dl) | 2.7 ± 0.9 | 2.8 ± 0.5 | 3.4 ± 0.4 |
| Serum potassium level (mEq/l) | 3.4 ± 0.9 | 3.1 ± 0.9 | 3.5 ± 0.7 |
| Urine volume (ml) | 458.3 ± 264.4 | 283.3 ± 132.9 | 615.5 ± 418.4 |
| Presentation | |||
| Fever | 1 (4) | 2 (10) | 0 |
| Abdominal pain | 5 (22) | 12 (57) | 0 |
| Cloudy dialysate | 18 (78) | 15 (71) | 0 |
| PDE cell count (cells/μl) | 2400 ± 4801 | 4732 ± 6783 | 7 ± 2 |
| PDE neutrophil (%) | 77 ± 18 | 85 ± 12 | 67 ± 11 |
PD, peritoneal dialysis; PDE, peritoneal dialysis effluent.
Data are mean ± SD or n (%).
Table 2.
Organisms cultured in cases of bacterial and fungal peritonitis in this study
| Identified bacteria (21) | Identified fungi (23) |
|---|---|
| Pseudomonas aeruginosa (6) | Candida spp. (6)a |
| Escherichia coli (5) | Trichosporon spp. (3)a |
| CoNS (3) | Aspergillus spp. (3) |
| Streptococcus mitis (2) | Fusarium spp. (2) |
| Staphylococcus aureus (1) | Unidentified mold (2) |
| Enterobacter asburiae (1) | Exophiala spp. (1)a |
| Proteus mirabilis (1) | Acremonium spp. (1) |
| Stenotrophomonas maltophilia (1) | Alternaria spp. (1) |
| Bacillus spp. (1)b | Paecilomyces spp. (1) |
| Penicillium spp. (1) | |
| Scedosporium spp. (1) | |
| Scopulariopsis spp. (1) |
CoNS, coagulase-negative Staphylococcus.
Number of cases is given in parentheses.
Yeast-form fungi (others are mold-form).
Gram-positive bacteria (others are gram negative).
Serum GMI Values
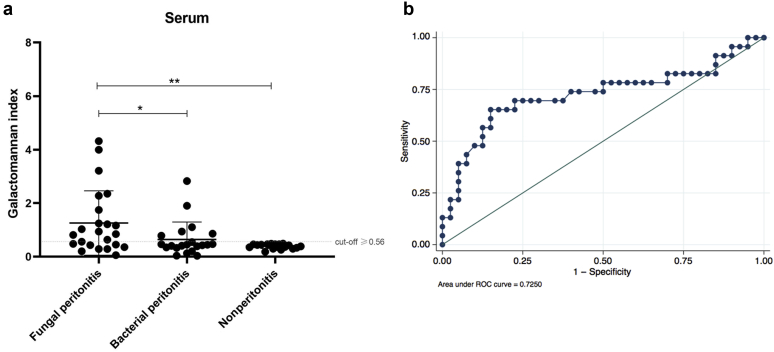
Serum GMI in patients with fungal peritonitis was significantly higher than that in patients with bacterial peritonitis and controls without peritonitis (median, 0.85 [interquartile range, 0.43–1.75] vs 0.45 [interquartile range, 0.35–0.79] vs. 0.43 [interquartile range, 0.34–0.47], respectively; P = 0.036) (Figure 2a). To differentiate fungal peritonitis from non–fungal peritonitis (including bacterial peritonitis and nonperitonitis), a serum GMI cutoff value of ≥0.56 (Supplementary Table S2) provided the best diagnostic accuracy with 65.2% sensitivity, 85.0% specificity, 4.35 positive likelihood ratio, and 0.41 negative likelihood ratio. At this cutoff point, the calculated area under the curve from receiver operating characteristic curve analysis for serum GMI was 0.73 (95% confidence interval, 0.58–0.87) (Table 3 and Figure 2b).
Figure 2.
Serum galactomannan index measurements in patients with fungal peritonitis on peritoneal dialysis (study cases), patients with bacterial peritonitis on peritoneal dialysis (active controls), and controls without peritonitis (a). Receiver operating characteristic (ROC) curves of serum galactomannan assays for the diagnosis of fungal peritonitis (b). *P < 0.01, **P < 0.001.
Table 3.
Performance of serum GMI for differentiating fungal peritonitis from nonfungal peritonitis (bacterial peritonitis and nonperitonitis)
| GM testing | Fungal culture |
LR+ | 4.35 | ||
|---|---|---|---|---|---|
| Positive | Negative | LR− | 0.41 | ||
| GMI cutoff value ≥0.56 in serum | Positive | 15 | 6 | Sensitivity | 65.2% |
| Negative | 8 | 34 | Specificity | 85.0% | |
| PPV, 71.4%; NPV, 81.0% | Accuracy | 77.8% | |||
GM, galactomannan; LR+, positive likelihood ratio; LR−, negative likelihood ratio; NPV, negative predictive value; PPV, positive predictive value.
Six patients with bacterial peritonitis (patients 2, 7, 13, 16, 19, and 20) had a positive GMI result. On the basis of polymerase chain reaction–based diagnosis of fungal infections, 2 patients (patients 16 and 19) had a positive polymerase chain reaction result, indicating a true-positive GMI result. In other words, an occult infection with fungus likely explained the positive GMI result in these 2 cases of bacterial peritonitis. The results of the polymerase chain reaction of the remaining cases were negative, although 2 cases (patients 2 and 13) had positive serum dipstick test results for heme, suggesting a possible explanation for a false-positive GMI result. Of note, there were 2 cases (patients 7 and 20) in which the isolated organism, Pseudomonas aeruginosa (1 case) and Escherichia coli (1 case), was known to cause a false-positive GMI result.
In contrast, 8 patients with fungal peritonitis had a negative serum GMI, including patient 25 (Candida parapsilosis), patient 29 (Exserohilum rostratum), patient 30 (Fusarium solani), patient 31 (Candida guilliermondii), patient 33 (Trichosporon spp.), patient 38 (Aspergillus flavus), patient 42 (Alternaria spp.), and patient 43 (Exophiala spp.). Possible reasons for these false-negative serum GMI results were the presence of a serum inhibitor or a lack of peripheral blood translocation in either the fungal whole cell or the cell wall. Of note, the follow-up serum titer of patient 29 increased to a level above the cutoff value at 1.88 during amphotericin B treatment.
Discussion
Our case-cohort study demonstrated that serum GMI may be useful for the timely diagnosis of fungal peritonitis. Because GMI measurement is less time-consuming than the conventional culture method (6 hours vs. 3–6 days), the more rapid diagnosis of fungal peritonitis by GMI offers a potential clinical advantage to patients on PD. The International Society for Peritoneal Dialysis 2016 peritonitis guideline recommended that an immediate catheter removal should be considered when fungi are identified in PD effluent. Earlier catheter removal is associated with improved outcomes, including mortality.3
Optimal serum GMI cutoff values ≥0.5 have been used for the diagnosis of invasive fungal infections.8,9,S1 However, in the present study, a slight increase in the cutoff to ≥0.56 provided the most optimal diagnostic accuracy for fungal peritonitis. This finding implies that there is a translocation of GM from the peritoneal fluid into the circulation in patients with fungal peritonitis. We demonstrated that serum GMI could be used for the diagnosis of fungal peritonitis with >65% sensitivity and 83% specificity. After excluding false positive from hemolytic serum (2 cases) and true positive from occult fungal infection (2 cases), there were 2 cases (10%) with bacterial peritonitis and false-positive serum GMI above the 0.56 cutoff. These cases involved specific bacterial pathogens known to produce false-positive GMI results, namely, Pseudomonas aeruginosa (1 case) and Escherichia coli (1 case). The false positivity in these cases possibly occurred because of (i) the high concentration of these organisms in the blood, causing a cross-reactivity in the Platelia Aspergillus enzyme immunoassay (Bio-Rad, Marnes-la-Coquette, France),9 and (ii) transient fungal antigenemia from cow’s milk productsS2 or fungal overgrowth in the compromised gut during the episode of severe gram-negative peritonitis and prolonged antibiotic treatment.S3 Dietary factors must therefore be taken into account when interpreting the cause of false-positive results in young children and patients with an impaired intestinal barrier.
In contrast, the false-negative GMI in 4 patients with Candida parapsilosis, Candida guilliermondii, Trichosporon spp., and Alternaria spp. might be related to fungal burden or the cell wall GM compositions of these fungi, leading to decreased sensitivity. GM detection is not possible in patients with Pneumocystis jiroveci, Candida spp. (some strains), and Acremonium spp. because of the absence of GM content in the cell walls of these fungi.S4 Meanwhile, the false-negative GMI occurred only in the serum of 4 patients who were infected with Aspergillus flavus, Exophiala spp., Exserohilum rostratum, and Fusarium solani. It is possible that fungal pathogens in all these cases did not invade into the bloodstream.
This study has some limitations. First, the number of patients in our proof-of-concept study was relatively small, such that a much larger study would be required to confidently establish the utility of serum GMI as a diagnostic biomarker for fungal peritonitis. Second, the results of this study may not generalize to populations on PD outside Thailand in whom the incidence of fungal peritonitis is appreciably lower.
In conclusion, serum GMI is a promising biomarker for the diagnosis of fungal peritonitis in patients on PD, particularly in conjunction with other parameters such as potassium hydroxide stain, culture, and polymerase chain reaction.
Disclosure
DWJ received lecture fees from Baxter Healthcare and Fresenius Medical Care and grant support from Baxter Healthcare. All the other authors declared no competing interests.
Acknowledgments
We acknowledge the contributions of the staffs, nurses, and all investigators who work at participating Thailand PD Outcomes and Practice Patterns Study (PDOPPS) centers, including King Chulalongkorn Memorial Hospital Sunpasitthiprasong Hospital, Phayao Hospital, Pranangklao Hospital, Siriraj Hospital, Nakhon Pathom Hospital, Bangkok Metropolitan Administration General Hospital, Chaoprayayomraj Hospital, Taksin Hospital, Udon Thani Hospital, Chaiyaphum Hospital, Mukdahan Hospital, Sukhothai Hospital, Nakornping Hospital, Sawanpracharak Hospital, Trang Hospital, Pong Hospital, Chaophraya Abhaibhubejhr Hospital, Trat Hospital, KhueangNai hospital, Amnatcharoen Hospital, and Songkhla Hospital. This study was supported by the Kidney Foundation of Thailand, Ratchadaphiseksomphot Endowment Fund (CU_GRS_61_06_30_01), Chulalongkorn University, the National Research Council of Thailand (156/2560), Thailand Research Foundation (IRG5780017), and the 90th Anniversary of Chulalongkorn University Fund (GCUGR1125594013D).
Footnotes
Supplementary References.
Supplementary Methods.
Table S1. Patient characteristics, previous peritonitis, laboratories, and outcome.
Table S2. Accuracy of serum galactomannan index for differentiating fungal peritonitis at different cutoff points.
Contributor Information
Talerngsak Kanjanabuch, Email: golfnephro@hotmail.com.
Thailand PD Outcomes and Practice Patterns Study (PDOPPS) Steering Committee:
Talerngsak Kanjanabuch, Piyaporn Towannang, Pichet Lorvinitnun, Nisa Thongbor, Suchai Sritippayawan, Nipa Aiyasanon, Guttiga Halue, Donkum Kaewboonsert, Pensri Uttayotha, Wichai Sopassathit, Kittisak Tangjittrong, Salakjit Pitakmongkol, Ussanee Poonvivatchaikarn, Bunpring Jaroenpattrawut, Somphon Buranaosot, Sukit Nilvarangkul, Warakoan Satitkan, Wanida Somboonsilp, Pimpong Wongtrakul, Ampai Tongpliw, Anocha Pullboon, Chanchana Boonyakrai, Montha Jankramol, Surapong Narenpitak, Apinya Wechpradit, Sajja Tatiyanupanwong, Chadarat Kleebchaiyaphum, Wadsamon Saikong, Worauma Panya, Siriwan Thaweekote, Sriphrae Uppamai, Jarubut Phisutrattanaporn, Sirirat Sirinual, Setthapon Panyatong, Puntapong Taruangsri, Boontita Prasertkul, Thanchanok Buanet, Rutchanee Chieochanthanakij, Panthira Passorn, Niwat Lounseng, Rujira Luksanaprom, Angsuwarin Wongpiang, Metinee Chaiwut, Worapot Treamtrakanpon, Ruchdaporn Phaichan, Peerapach Rattanasoonton, Wanlaya Thongsiw, Narumon Lukrat, Sayumporn Thaitrng, Phichit Songviriyavithaya, Yupha Laoong, Niparat Pikul, Uraiwan Parinyasiri, Navarat Rukchart, Korawee Sukmee, and Wandee Chantarungsri
Appendix
Members of the Thailand PD Outcomes and Practice Patterns Study (PDOPPS) Steering Committee are as follows: Talerngsak Kanjanabuch and Piyaporn Towannang, Department of Medicine, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand; Pichet Lorvinitnun and Nisa Thongbor, Department of Medicine, Sunpasitthiprasong Hospital, Ubon Ratchathani, Thailand; Suchai Sritippayawan and Nipa Aiyasanon, Division of Nephrology, Department of Internal Medicine, Siriraj Hospital, Bangkok, Thailand; Guttiga Halue, Donkum Kaewboonsert, and Pensri Uttayotha, Department of Medicine, Phayao Hospital, Phayao, Thailand; Wichai Sopassathit, Kittisak Tangjittrong, and Salakjit Pitakmongkol, Division of Nephrology, Department of Internal Medicine, Pranangklao Hospital, Nonthaburi, Thailand; Ussanee Poonvivatchaikarn and Bunpring Jaroenpattrawut, Nephrology Clinic, Nakhon Pathom Hospital, Nakhon Pathom, Thailand; Somphon Buranaosot, Sukit Nilvarangkul, and Warakoan Satitkan, Bangkok Metropolitan Administration General Hospital, Bangkok, Thailand; Wanida Somboonsilp, Pimpong Wongtrakul, Ampai Tongpliw, and Anocha Pullboon, CAPD Clinic, Chaoprayayomraj Hospital, Suphanburi, Thailand; Chanchana Boonyakrai and Montha Jankramol, Division of Nephrology, Department of Internal Medicine, Taksin Hospital, Bangkok, Thailand; Surapong Narenpitak and Apinya Wechpradit, Renal Unit, Department of Internal Medicine, Udonthani Hospital, Udon Thani, Thailand; Sajja Tatiyanupanwong and Chadarat Kleebchaiyaphum, Nephrology Division, Department of Internal Medicine, Chaiyaphum Hospital, Chaiyaphum, Thailand; Wadsamon Saikong, Worauma Panya, and Siriwan Thaweekote, CAPD Clinic, Mukdahan Hospital, Mukdahan, Thailand; Sriphrae Uppamai, Jarubut Phisutrattanaporn, and Sirirat Sirinual, Department of Internal Medicine, Sukhothai Hospital, Sukhothai, Thailand; Setthapon Panyatong, Puntapong Taruangsri, Boontita Prasertkul, and Thanchanok Buanet, Kidney Center, Department of Internal Medicine, Nakornping Hospital, Chiang Mai, Thailand; Rutchanee Chieochanthanakij and Panthira Passorn, Dialysis Unit, Sawanpracharak Hospital, Nakhon Sawan, Thailand; Niwat Lounseng and Rujira Luksanaprom, Department of Medicine, Trang Hospital, Trang, Thailand; Angsuwarin Wongpiang and Metinee Chaiwut, CAPD, Pong Hospital, Phayao, Thailand; Worapot Treamtrakanpon and Ruchdaporn Phaichan, Department of Medicine, Chaophya Abhaiphubejhr Hospital, Prachin Buri, Thailand; Peerapach Rattanasoonton and Wanlaya Thongsiw, Department of Medicine, Trat Hospital, Trat, Thailand; Narumon Lukrat and Sayumporn Thaitrng, CAPD Unit, KhueangNai Hospital, Ubon Ratchatani, Thailand; Phichit Songviriyavithaya, Yupha Laoong, and Niparat Pikul, Division of Nephrology, Department of Medicine, Amnatcharoen Hospital, Amnatcharoen, Thailand; and Uraiwan Parinyasiri, Navarat Rukchart, Korawee Sukmee, and Wandee Chantarungsri, Kidney Diseases Clinic, Department of Internal Medicines, Songkhla Hospital, Songkhla, Thailand.
Supplementary Material
References
- 1.Miles R., Hawley C.M., McDonald S.P. Predictors and outcomes of fungal peritonitis in peritoneal dialysis patients. Kidney Int. 2009;76:622–628. doi: 10.1038/ki.2009.202. [DOI] [PubMed] [Google Scholar]
- 2.Matuszkiewicz-Rowinska J. Update on fungal peritonitis and its treatment. Perit Dial Int. 2009;29(suppl 2):S161–S165. [PubMed] [Google Scholar]
- 3.Li P.K.-T., Szeto C.C., Piraino B. ISPD peritonitis recommendations: 2016 update on prevention and treatment. Perit Dial Int. 2016;36:481–508. doi: 10.3747/pdi.2016.00078. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Nadeau-Fredette A.C., Bargman J.M. Characteristics and outcomes of fungal peritonitis in a modern North American cohort. Perit Dial Int. 2015;35:78–84. doi: 10.3747/pdi.2013.00179. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Wingard J.R. Have novel serum markers supplanted tissue diagnosis for invasive fungal infections in acute leukemia and transplantation? Best Pract Res Clin Haematol. 2012;25:487–491. doi: 10.1016/j.beha.2012.10.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Marr K.A., Balajee S.A., McLaughlin L. Detection of galactomannan antigenemia by enzyme immunoassay for the diagnosis of invasive aspergillosis: variables that affect performance. J Infect Dis. 2004;190:641–649. doi: 10.1086/422009. [DOI] [PubMed] [Google Scholar]
- 7.Shin B., Koh W.J., Jeong B.H. Serum galactomannan antigen test for the diagnosis of chronic pulmonary aspergillosis. J Infect. 2014;68:494–499. doi: 10.1016/j.jinf.2014.01.005. [DOI] [PubMed] [Google Scholar]
- 8.Vaziri N.D., Yuan J., Rahimi A. Disintegration of colonic epithelial tight junction in uremia: a likely cause of CKD-associated inflammation. Nephrol Dial Transplant. 2012;27:2686–2693. doi: 10.1093/ndt/gfr624. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Swanink C.M.A., Meis J.F.G.M., Rijs A.J.M.M. Specificity of a sandwich enzyme-linked immunosorbent assay for detecting Aspergillus galactomannan. J Clin Microbiol. 1997;35:257–260. doi: 10.1128/jcm.35.1.257-260.1997. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.