Emerging studies suggest that the novel coronavirus (nCoV) severe acute respiratory syndrome coronavirus 2 and the disease it causes, COVID-19, selectively afflicts the elderly, particularly those with chronic comorbidities.1 , 2 Here, we report on 2 heart transplant recipients with COVID-19, one a severe presentation and another mild.
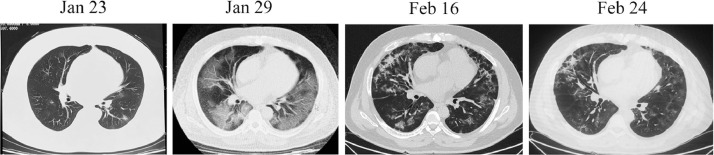
The first was a 51-year-old man with a heart transplant on November 8, 2003. His immunosuppression was tacrolimus 1 mg twice daily plus mycophenolate mofetil 0.5 g twice daily. The last known blood concentration of tacrolimus was 6.5 ng/ml, and cardiac allograft function was normal with a history of well-controlled hypertension. On January 23, 2020, he complained of intermittent fever, chills, fatigue, poor appetite, and diarrhea. On examination, his temperature was 38.5°C, oxygen saturation was 99% on room air, and respiratory rate was 20 breaths per minute without distress. Laboratory tests showed a white blood cell count of 4.87 × 109 cells/liter (normal range, 4.0–10.0 × 109 cells/liter) and C-reactive protein levels of 18.6 mg/liter (normal range, 0–10 mg/liter). Chest computed tomography (CT) scan showed bilateral ground-glass opacities (Figure 1 ). He was initially treated with intravenous levofloxacin and ribavirin but remained febrile. He was admitted to Wuhan Fifth Hospital on January 26, 2020, and a throat swab nucleic acid test was positive for 2019-nCoV. Moxifloxacin 0.4 g and ganciclovir 0.25 g were then given intravenously daily and continued until February 5, 2020. Initially, his temperature rose to 39°C with a dry cough on January 27, 2020, and oxygen saturation decreased gradually, requiring nasal oxygen supplementation. Body temperature dropped to normal on January 29; however, oxygen saturation deteriorated (75% without supplemental oxygen after slight activity). CT scan revealed worsening of lung lesions (Figure 1), and oxygen was given through a face mask, with improvement of oxygen saturation to 95%. Intravenous human gamma globulin 10 g/day and methylprednisolone 80 mg/day were initiated for 5 consecutive days, and other immunosuppressive drugs were held from January 30 to February 5, 2020. After treatment, the patient's symptoms improved, and oxygen saturation was maintained above 96% with nasal cannula oxygen. Intravenous medications were then stopped, and oral administration of moxifloxacin 0.4 g/day and arbidol (a non-nucleoside antiviral and immunomodulating drug given for influenza) 0.2 g 3 times a day was administered for 5 days. Immunosuppressive and anti-hypertensive drugs were resumed on February 12, 2020. The patient's temperature normalized for more than 20 days without cough for 10 days and preserved oxygen saturation. Two consecutive reverse transcriptase–polymerase chain reaction throat swabs for 2019-nCoV on February 14 and 18, 2020 were negative. A CT scan on February 24 showed significant resolution of lung lesions (Figure 1). The patient was discharged on February 27, 2020. Typical imaging demonstrated dynamic progress of the disease (Figure 1). However, resolution of lung lesions lagged behind symptom relief.
Figure 1.
Dynamic chest computed tomographic manifestations of severe COVID-19 in a heart transplant recipient.
A second male heart transplant recipient aged 43 years old presented to the outpatient clinic with fever for 2 days on January 25, 2020 and exhibited mild lung lesions on CT scan, but a nucleic acid test for 2019-nCoV was positive. The patient was quarantined at home and then admitted to the hospital on February 6, 2020, following which he was discharged on February 11 when 2 nucleic acid tests for 2019-nCoV tested negative. Detailed information on this patient is in Table 1 .
Table 1.
Clinical Characteristics of the Second Patient
| Characteristic | Description |
|---|---|
| Date of transplant | May 17, 2017 |
| Immunosuppression | Tacrolimus 1.5 mg in the morning, 2 mg in the evening |
| Mycophenolate mofetil 0.5 g twice daily | |
| Blood concentration of tacrolimus | 8.3 ng/ml |
| Allograft function | Left ventricular ejection fraction 64% |
| Comorbidities | Hyperlipidemia and impaired glucose tolerance |
| Lab test | January 25, 2020: WBC 8.2 × 109 cells/liter, lymphocyte 0.8 × 109 cells/liter, CRP 13.4 mg/liter February 7, 2020: WBC 8.4 × 109 cells/liter, lymphocyte 1.5 × 109 cells/liter, CRP 1.0 mg/liter |
| RT-PCR of 2019-nCoV (Throat swab) |
Positive on January 28, negative on February 8 and 10 |
| Treatment | Ceftriaxone sodium 2.0 g and ganciclovir 0.25 g intravenously (January 25–31); oral moxifloxacin 0.4 g/day and arbidol 0.2 g 3 times a day (February 1–10) |
| Symptoms evolution | Fever for 2 days, up to 38.5°C Fatigue and poor appetite from January 28 to February 5 |
| Rejection during or after COVID-19 | None |
| Other complications | None |
Abbreviations: CRP, C-reactive protein; nCoV, novel coronavirus; RT-PCR, reverse transcriptase–polymerase chain reaction; WBC, white blood cell.
These cases may represent the first descriptions of COVID-19 in heart transplant recipients and suggest that presentations appear to be similar to those observed in non-transplant recipients. We have also followed 200 heart transplant patients in the Hubei area by telephone and found a third confirmed patient who is currently under treatment in another hospital, but the case details are not available to us, and therefore, are not included in our report. Whether organ transplant recipients are more susceptible to COVID-19 requires further large-scale epidemiologic investigation, but the presentation pattern and resolution of the disease using the described supportive measures may serve to inform direction of care if such patients are encountered elsewhere.
Editor's Note: The article published from China may include patients transplanted at a time when concerns existed with unethical procurement of organ donors, and therefore, may represent a violation of the publication policy. However, the editors have chosen to override this aspect because of the critical importance of the information provided in such a paper for the benefit and help of our patients while recognizing the dignity of those from whom the unethical organs were most probably obtained.
Footnotes
Editor's Note: The article published from China may include patients transplanted at a time when concerns existed with unethical procurement of organ donors, and therefore may represent a violation of the publication policy. However, the editors have chosen to override this aspect, due to the critical importance of the information provided in such a paper for the benefit and help of our patients while recognizing the dignity of those from whom the unethical organs were most probably obtained.
Contributor Information
Jie Cai, Email: cjdoctor@163.com.
Nianguo Dong, Email: dongnianguo@hotmail.com.
References
- 1.Wang D, Hu B, Hu C. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. JAMA. 2020;323:1061–1069. doi: 10.1001/jama.2020.1585. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Yang X, Yu Y, Xu J, et al. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study [e-pub ahead of print]. Lancet Respir Publ. doi: 10.1016/S2213-2600(20)30079-5. Accessed February 24, 2020. [DOI] [PMC free article] [PubMed]