Abstract
Since the outbreak of coronavirus disease 2019 (COVID-19), clinicians have tried every effort to understand the disease, and a brief portrait of its clinical features have been identified. In clinical practice, we noticed that many severe or critically ill COVID-19 patients developed typical clinical manifestations of shock, including cold extremities and weak peripheral pulses, even in the absence of overt hypotension. Understanding the mechanism of viral sepsis in COVID-19 is warranted for exploring better clinical care for these patients. With evidence collected from autopsy studies on COVID-19 and basic science research on severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and SARS-CoV, we have put forward several hypotheses about SARS-CoV-2 pathogenesis after multiple rounds of discussion among basic science researchers, pathologists, and clinicians working on COVID-19. We hypothesise that a process called viral sepsis is crucial to the disease mechanism of COVID-19. Although these ideas might be proven imperfect or even wrong later, we believe they can provide inputs and guide directions for basic research at this moment.
Introduction
The severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) outbreak, which was first reported in Wuhan, China, in December, 2019, has had an enormous impact on China and the whole world. The disease caused by SARS-CoV-2 is named coronavirus disease 2019 (COVID-19). By March 19, 2020, the number of confirmed cases had increased to over 200 000. Although most patients infected with SARS-CoV-2 had a mild illness, about 5% of patients had severe lung injury or even multiorgan dysfunction, resulting in a 1·4% case fatality ratio.1
In clinical practice, we noticed that many severe or critically ill COVID-19 patients developed typical clinical manifestations of shock, including cold extremities and weak peripheral pulses, even in the absence of overt hypotension. Many of these patients showed severe metabolic acidosis, indicating possible microcirculation dysfunction. Moreover, some patients had impaired liver2 and kidney function in addition to severe lung injury. These patients met the diagnostic criteria for sepsis and septic shock according to the Sepsis-3 International Consensus,3 but SARS-CoV-2 infection appeared to be the sole cause in most of them.1 Blood and lower respiratory tract specimen cultures turned out to be negative for bacteria and fungus in 76% sepsis patients in a COVID-19 cohort.4 Therefore, viral sepsis would be more accurate to describe the clinical manifestations of severe or critically ill COVID-19 patients.5 Understanding the mechanism of viral sepsis in COVID-19 is warranted for exploring better clinical care for these patients.
Virus infection and COVID-19 pathogenesis in organs
In biopsy or autopsy studies, pulmonary pathology for both early6 and late phase7 COVID-19 patients showed diffuse alveolar damage with the formation of hyaline membranes, mononuclear cells, and macrophages infiltrating air spaces, and a diffuse thickening of the alveolar wall. Viral particles were observed in the bronchial and type 2 alveolar epithelial cells by electron microscopy.8, 9 In addition, spleen atrophy, hilar lymph node necrosis, focal haemorrhage in the kidney, enlarged liver with inflammatory cell infiltration, oedema, and scattered degeneration of the neurons in the brain were present in some patients.8, 9 SARS-CoV-2 infectious virus particles have been isolated from respiratory samples,10 as well as from faecal11 and urine (Zhao J, Guangzhou Medical University, personal communication) specimens from COVID-19 patients, suggesting that multiple organ dysfunction in severe COVID-19 patients is at least partially caused by a direct attack from the virus. However, there are no reports about the post-mortem observations of the broad dissemination of the viral particles by autopsy right now. Whether SARS-CoV-2 can directly target organs other than the lung, especially those organs with high expression of angiotensin-converting enzyme 2 (ACE2)12, 13 and organs with L-SIGN14 as possible alternative cell receptors for SARS-CoV-2, has to be further investigated. In addition, the question of how the SARS-CoV-2 spreads to extrapulmonary organs remains an enigma. Genomic variation of the circulating SARS-CoV-2 has been observed, and the difference in the virulence needs further investigation.15
Immune response to SARS-CoV-2 and viral sepsis
It has been shown that proinflammatory cytokines and chemokines including tumour necrosis factor (TNF) α, interleukin 1β (IL-1β), IL-6, granulocyte-colony stimulating factor, interferon gamma-induced protein-10, monocyte chemoattractant protein-1, and macrophage inflammatory proteins 1-α were significantly elevated in COVID-19 patients.16, 17 Like in a severe influenza infection, the cytokine storm might play an important role in the immunopathology of COVID-19. Previous studies revealed that lung epithelial cells, macrophages, and dendritic cells all express cytokines to some extent during influenza infection via the activation of pattern recognition receptors (including the Toll-like receptors TLR3, TLR7, and TLR8), retinoic acid-inducible gene I, and the NOD-like receptor family members.18 However, little is known about the situation in COVID-19 at this moment. It is crucial to identify the primary source of the cytokine storm in response to SARS-CoV-2 infection and the virological mechanisms behind the cytokine storm. It would also be relevant to elucidate the kinetics of cytokine activation during SARS-CoV-2 infection: when were the first cytokines released and what were they? Also, whether direct virus-induced tissue damage, systemic cytokine storm, or the synergistic effects of both, contributes to the multiple organ dysfunction of severe COVID-19 patients remains to be addressed. Furthermore, it is worth keeping track of whether blocking one of these proinflammatory mediators would affect the clinical outcome. The anti-IL-6R monoclonal antibody or corticosteroids have been proposed to alleviate the inflammatory response. However, IL-6 might play an important role in initiating a preliminary response against virus infection by promoting neutrophil-mediated viral clearance, as one study revealed that IL-6 or IL-6R deficiency led to persistence of influenza infection and ultimately death in mice.19 And the use of corticosteroids is still controversial.20, 21
Yet the dysregulated immune response also has an immune suppression stage following the proinflammatory phase. It is characterised by sustained and substantial reduction of the peripheral lymphocyte counts, mainly CD4 T and CD8 T cells in COVID-19 patients, and is associated with a high risk of developing secondary bacterial infection.4 This condition, known as lymphopenia, was also found in severe influenza and other respiratory viral infections. The degree of lymphopenia has been shown to correlate with the severity of COVID-19.17 The mechanism underlying lymphopenia remains unknown. Previous studies have shown that SARS-like viral particles and SARS-CoV RNA were detected in T lymphocytes isolated from peripheral blood sample, spleen, lymph nodes, and lymphoid tissue of various organs,22, 23 suggesting that SARS-CoV might be able to infect T cells directly. The receptor-binding domains of the spike proteins between SARS-CoV-2 and SARS-CoV show a high degree of consistency,24, 25 and SARS-CoV-2 RNA was also detected in blood samples.16 Therefore, it is reasonable to hypothesise that, in addition to the activation-induced cell death induced by Fas and Fas ligand interaction as well as TNF-related apoptosis-inducing ligand axis,26 SARS-CoV-2 could directly infect lymphocytes, particularly T cells, and initiate or promote the cell death of lymphocytes, which eventually lead to lymphopenia and impaired antiviral responses. However, such a hypothesis needs to be further investigated. It also needs to be identified what types of cell death are happening in the lymphocytes after SARS-CoV-2 infection. In addition, it is intriguing that the lymphocytes lack ACE2 expression, suggesting an alternative mechanism by which SARS-CoV-2 compromises T lymphocytes.13 Whether or not alveolar macrophages can phagocytise the viral particles and then transfer to lymphocytes is an open question in the field.
COVID-19 and abnormal coagulation
Studies have revealed that 71·4% of non-survivors of COVID-19 matched the grade of overt disseminated intravascular coagulation (≥5 points according to the International Society on Thrombosis and Haemostasis criteria)27 and showed abnormal coagulation results during later stages of the disease; particularly increased concentrations of D-dimer and other fibrin degradation products were significantly associated with poor prognosis.4 However, the concrete mechanisms for coagulopathy are not identified yet. Whether SARS-CoV-2 is able to directly attack vascular endothelial cells expressing high levels of ACE2,13 and then lead to abnormal coagulation and sepsis, still needs to be explored. Meanwhile, ACE2 is also an important regulator of blood pressure. High expression of ACE2 in the circulatory system after infection of SARS-CoV-2 might partially contribute to septic hypotension.28 Questions have been raised about using inhibitor therapy with angiotensin II receptor blockers (ARB) and ACE inhibitors for COVID-19 patients with hypertension. Some researchers suggested that ACE inhibitors might benefit these patients by reducing pulmonary inflammation,29 although others argued that ACE inhibitors might enhance viral entry by regulating ACE2 levels.30 However, there has been little clinical evidence on the risk of treating COVID-19 patients with ARB or ACE inhibitors. Further research is needed to explore whether these drugs inhibit or aid viral entry.
Conclusion
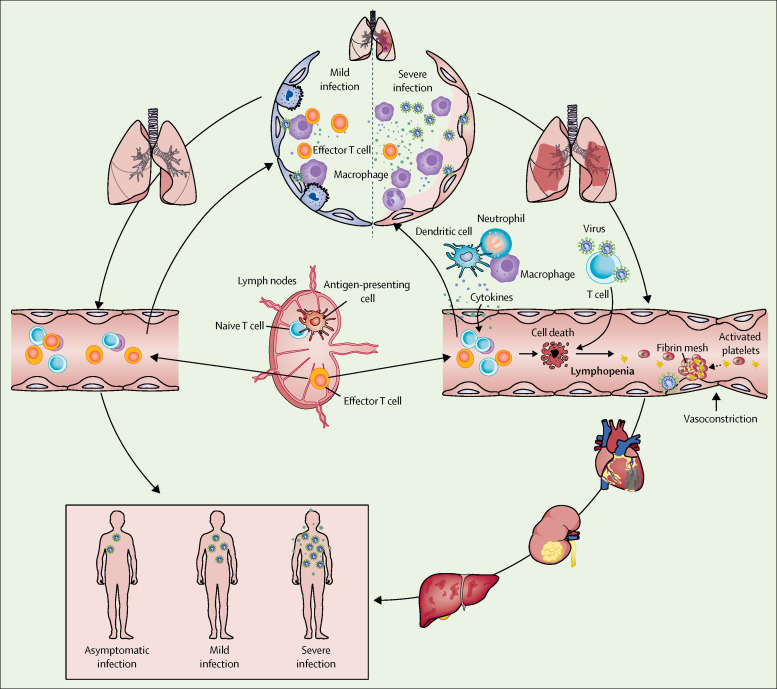
On the basis of observations from COVID-19 patients, we hypothesise that in mild cases, resident macrophages initiating lung inflammatory responses were able to contain the virus after SARS-CoV-2 infection; both innate and adaptive immune responses were efficiently established to curb the viral replication so that the patient would recover quickly. However, in severe or critical COVID-19 cases, the integrity of the epithelial–endothelial (air–blood) barrier was severely interrupted. In addition to epithelial cells, SARS-CoV-2 can also attack lung capillary endothelial cells, which leads to a large amount of plasma component exudate in the alveolar cavity. In response to the infection of SARS-CoV-2, alveolar macrophages or epithelial cells could produce various proinflammatory cytokines and chemokines. Upon this change, monocytes and neutrophils were then chemotactic to the infection site to clear these exudates with virus particles and infected cells, resulting in uncontrolled inflammation. In this process, because of the substantial reduction and dysfunction of lymphocytes, the adaptive immune response cannot be effectively initiated. The uncontrolled virus infection leads to more macrophage infiltration and a further worsening of lung injury. Meanwhile, the direct attack on other organs by disseminated SARS-CoV-2, the immune pathogenesis caused by the systemic cytokine storm, and the microcirculation dysfunctions together lead to viral sepsis (figure ). Therefore, effective antiviral therapy and measures to modulate the innate immune response and restore the adaptive immune response are essential for breaking the vicious cycle and improving the outcome of the patients.
Figure.
Occurrence and outcome of severe acute respiratory syndrome coronavirus 2 viral sepsis
Since the outbreak of COVID-19, clinicians have tried every effort to understand the disease, and a brief portrait of its clinical features have been identified. However, there are still open questions about the mechanisms of the observations. With evidence collected from autopsy studies on COVID-19 and basic science research on SARS-CoV-2 and SARS-CoV, we have put forward several hypotheses about SARS-CoV-2 pathogenesis after multiple rounds of discussion among basic science researchers, pathologists, and clinicians working on COVID-19. We hypothesise that a process called viral sepsis is crucial to the disease mechanism of COVID-19. Although these ideas might be proven imperfect or even wrong later on, we believe that they raise questions for future research.
Future basic science research is needed to explore whether SARS-CoV-2 directly attacks vascular endothelial cells, and to examine the effect of SARS-CoV-2 on coagulation and virus dissemination. Clinical trials and animal experiments should be done to assess the effect of ARB and ACE inhibitors on the outcome of SARS-CoV-2 infection in vivo. Efforts should be made to confirm whether SARS-CoV-2 directly infects lymphocytes, and how it influences the adaptive immune response. The kinetics of the cytokine response during SARS-CoV-2 infection also need further investigation. The efficacy of immunomodulatory therapies should be assessed in randomised clinical trials.
Acknowledgments
Acknowledgments
We appreciate the advice and editing of this Hypothesis by Xuetao Cao in Nankai University.
Contributors
HL did the literature search and drafted the paper. JX helped with the literature search and revised the manuscript. BC put forward the hypothesis and revised the manuscript. LL, DZ, JX, HD, NT, and XS provided ideas about the mechanism of viral sepsis and revised the paper.
Declaration of interests
We declare no competing interests.
Supplementary Material
References
- 1.Guan WJ, Ni ZY, Hu Y, et al. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med. 2020 doi: 10.1056/NEJMoa2002032. published online Feb 28. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Zhang C, Shi L, Wang FS. Liver injury in COVID-19: management and challenges. Lancet Gastroenterol Hepatol. 2020 doi: 10.1016/S2468-1253(20)30057-1. published online March 4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Singer M, Deutschman CS, Seymour CW, et al. The third international consensus definitions for sepsis and septic shock (Sepsis-3) JAMA. 2016;315:801–810. doi: 10.1001/jama.2016.0287. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Zhou F, Yu T, Du R, et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet. 2020;395:1054–1062. doi: 10.1016/S0140-6736(20)30566-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Lin GL, McGinley JP, Drysdale SB, Pollard AJ. Epidemiology and immune pathogenesis of viral sepsis. Front Immunol. 2018;9 doi: 10.3389/fimmu.2018.02147. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Tian S, Hu W, Niu L, Liu H, Xu H, Xiao S-Y. Pulmonary pathology of early phase 2019 novel coronavirus (COVID-19) pneumonia in two patients with lung cancer. J Thorac Oncol. 2020 doi: 10.1016/j.jtho.2020.02.010. published online Feb 28. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Xu Z, Shi L, Wang Y, et al. Pathological findings of COVID-19 associated with acute respiratory distress syndrome. Lancet Respir Med. 2020;8:420–422. doi: 10.1016/S2213-2600(20)30076-X. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.China National Health Commision Diagnosis and treatment of novel coronavirus pneumonia in China (trial version 7) https://www.who.int/docs/default-source/wpro---documents/countries/china/covid-19-briefing-nhc/1-clinical-protocols-for-the-diagnosis-and-treatment-of-covid-19-v7.pdf?sfvrsn=c6cbfba4_2
- 9.Yao XH, Li TY, He ZC, et al. A pathological report of three COVID-19 cases by minimally invasive autopsies. Zhonghua Bing Li Xue Za Zhi. 2020;49:E009. doi: 10.3760/cma.j.cn112151-20200312-00193. (in Chinese). [DOI] [PubMed] [Google Scholar]
- 10.Zhu N, Zhang D, Wang W, Li X, et al. A novel coronavirus from patients with pneumonia in China, 2019. N Engl J Med. 2020;382:727–733. doi: 10.1056/NEJMoa2001017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Wang W, Xu Y, Gao R, et al. Detection of SARS-CoV-2 in different types of clinical specimens. JAMA. 2020 doi: 10.1001/jama.2020.3786. published online March 11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Zhou P, Yang X-L, Wang X-G, et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature. 2020;579:270–273. doi: 10.1038/s41586-020-2012-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Hamming I, Timens W, Bulthuis MLC, Lely AT, Navis G, van Goor H. Tissue distribution of ACE2 protein, the functional receptor for SARS coronavirus. A first step in understanding SARS pathogenesis. J Pathol. 2004;203:631–637. doi: 10.1002/path.1570. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Jeffers SA, Tusell SM, Gillim-Ross L, et al. CD209L (L-SIGN) is a receptor for severe acute respiratory syndrome coronavirus. Proc Natl Acad Sci USA. 2004;101:15748–15753. doi: 10.1073/pnas.0403812101. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Yu WB, Tang GD, Zhang L, Corlett RT. Decoding evolution and transmissions of novel pneumonia coronavirus using the whole genomic data. http://www.chinaxiv.org/abs/202002.00033 [DOI] [PMC free article] [PubMed]
- 16.Huang C, Wang Y, Li X, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. 2020;395:497–506. doi: 10.1016/S0140-6736(20)30183-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Liu J, Li S, Liu J, et al. Longitudinal characteristics of lymphocyte responses and cytokine profiles in the peripheral blood of SARS-CoV-2 infected patients. medRxiv. 2020 doi: 10.1101/2020.02.16.20023671. published online Feb 22. (preprint). [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Iwasaki A, Pillai PS. Innate immunity to influenza virus infection. Nat Rev Immunol. 2014;14:315–328. doi: 10.1038/nri3665. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Dienz O, Rud JG, Eaton SM, et al. Essential role of IL-6 in protection against H1N1 influenza virus by promoting neutrophil survival in the lung. Mucosal Immunol. 2012;5:258–266. doi: 10.1038/mi.2012.2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Russell CD, Millar JE, Baillie JK. Clinical evidence does not support corticosteroid treatment for 2019-nCoV lung injury. Lancet. 2020;395:473–475. doi: 10.1016/S0140-6736(20)30317-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Shang L, Zhao J, Hu Y, Du R, Cao B. On the use of corticosteroids for 2019-nCoV pneumonia. Lancet. 2020;395:683–684. doi: 10.1016/S0140-6736(20)30361-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Taubenberger JK, Morens DM. The pathology of influenza virus infections. Annu Rev Pathol. 2008;3:499–522. doi: 10.1146/annurev.pathmechdis.3.121806.154316. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Gu J, Gong E, Zhang B, et al. Multiple organ infection and the pathogenesis of SARS. J Exp Med. 2005;202:415–424. doi: 10.1084/jem.20050828. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Xu X, Chen P, Wang J, et al. Evolution of the novel coronavirus from the ongoing Wuhan outbreak and modeling of its spike protein for risk of human transmission. Sci China Life Sci. 2020;63:457–460. doi: 10.1007/s11427-020-1637-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Lu R, Zhao X, Li J, et al. Genomic characterisation and epidemiology of 2019 novel coronavirus: implications for virus origins and receptor binding. Lancet. 2020;395:565–574. doi: 10.1016/S0140-6736(20)30251-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Peteranderl C, Herold S. the impact of the interferon/tnf-related apoptosis-inducing ligand signaling axis on disease progression in respiratory viral infection and beyond. Front Immunol. 2017;8:313. doi: 10.3389/fimmu.2017.00313. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Tang N, Li D, Wang X, Sun Z. Abnormal coagulation parameters are associated with poor prognosis in patients with novel coronavirus pneumonia. J Thromb Haemost. 2020 doi: 10.1111/jth.14768. published online Feb 19. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Wang PH, Cheng Y. Increasing host cellular receptor—angiotensin-converting enzyme 2 (ace2) expression by coronavirus may facilitate 2019-nCoV infection. bioRxiv. 2020 doi: 10.1101/2020.02.24.963348. published online Feb 27. (preprint). [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Sun ML, Yang JM, Sun YP, Su GH. Inhibitors of RAS might be a good choice for the therapy of COVID-19 pneumonia. Zhonghua Jie He He Hu Xi Za Zhi. 2020;43:219–222. doi: 10.3760/cma.j.issn.1001-0939.2020.03.016. [DOI] [PubMed] [Google Scholar]
- 30.Ferrario CM, Jessup J, Chappell MC, et al. Effect of angiotensin-converting enzyme inhibition and angiotensin II receptor blockers on cardiac angiotensin-converting enzyme 2. Circulation. 2005;111:2605–2610. doi: 10.1161/CIRCULATIONAHA.104.510461. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.