Abstract
Background: Thrombocytopenia has been implicated in patients infected with severe acute respiratory syndrome coronavirus 2, while the association of platelet count and changes with subsequent mortality remains unclear.
Methods: The clinical and laboratory data of 383 patients with the definite outcome by March 1, 2020 in the Central Hospital of Wuhan were reviewed. The association between platelet parameters and mortality risk was estimated by utilizing Cox proportional hazard regression models.
Results: Among the 383 patients, 334 (87.2%) were discharged and survived, and 49 (12.8%) died. Thrombocytopenia at admission was associated with mortality of almost three times as high as that for those without thrombocytopenia (P < 0.05). Cox regression analyses revealed that platelet count was an independent risk factor associated with in-hospital mortality in a dose-dependent manner. An increment of per 50 × 109/L in platelets was associated with a 40% decrease in mortality (hazard ratio: 0.60, 95%CI: 0.43, 0.84). Dynamic changes of platelets were also closely related to death during hospitalization.
Conclusions: Baseline platelet levels and changes were associated with subsequent mortality. Monitoring platelets during hospitalization may be important in the prognosis of patients with coronavirus disease in 2019.
Keywords: Cohort study, coronavirus disease 2019, mortality, platelet count, severe acute respiratory syndrome coronavirus 2
Introduction
In December 2019, a series of pneumonia cases of unknown etiology emerged in Wuhan, Central China with a population of 11 million people and was thought to be related to an exposure from Huanan Seafood Wholesale Market [1,2]. This condition was later confirmed to be the coronavirus disease 2019 (COVID-19) caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Different from normal pathogens, this virus is powerful and has extended rapidly to other Chinese cities and countries, thus leading to the widespread of pneumonia [3–5]. The number of COVID-19 cases has sharply increased in China and by 13 times outside China, and the number of affected countries tripled. Consideration its alarming levels of spread and severity, the World Health Organization characterized COVID-19 as a pandemic on March 11, 2020. COVID-19 poses a great public health and clinical burden worldwide.
The epidemiological and clinical characteristics of patients with COVID-19 have been reported. SARS-CoV-2 infection has a wide clinical spectrum, including asymptomatic infection, mild respiratory disease, and severe pneumonia with acute respiratory failure and even death. Hematological changes, including lymphopenia and thrombocytopenia, have been reported in patients with COVID-19 similar to SARS in 2003 [6,7]. Abnormal coagulation is a common complication of COVID-19 and is manifested by pulmonary vascular leakage, intravascular thrombosis, and disseminated intravascular coagulation. Thrombocytopenia is also a common clinical manifestation associated with poor outcome in patients with community-acquired pneumonia [8]. Platelets not only contribute to hemostasis, but also participate in inflammation and host defense response. The latter is especially important when the lungs are infected. Although many cases of thrombocytopenia have been reported in patients with severe viral pneumonia and thus is a suggestive clinical characteristic of COVID-19, the association of baseline platelets and changes with adverse COVID-19 outcome remains unclear.
Here, a hospital-based cohort study was conducted in all patients with laboratory-confirmed COVID-19 to evaluate the association between platelets at admission and mortality, particularly the dynamic changes of circulating platelets and its role in the disease progression.
Methods
Participants
A retrospective cohort study was conducted on 383 patients with COVID-19 in the Central Hospital of Wuhan from January 2, 2020 and followed to March 1, 2020. COVID-19 was diagnosed according to the World Health Organization interim guidance [9]. Only patients with laboratory-confirmed human infection from throat swab specimens were enrolled, and those with malignant tumors, post craniocerebral operation, died on admission, treatment with anti-platelet drugs, and transferred to other medical institutions were excluded. All enrolled patients were followed up until discharge or death. The requirement for informed consent was waived due to the urgency to collect data on the emerging SARS-CoV-2. This study was approved by the Ethics Committees of the Central Hospital of Wuhan.
Data Collection
Case report forms, nursing records, laboratory findings, and radiological characteristics were reviewed by a team of physicians who treat patients with COVID-19. Demographic characteristics (gender and age), comorbidities (chronic obstructive pulmonary disease, hypertension, diabetes, cardiovascular disease, cerebrovascular disease, and chronic kidney disease), clinical manifestations, laboratory findings, treatment, and outcomes (discharge/death) were extracted from electronic medical records. Laboratory data, including white blood cell count, neutrophil count, lymphocyte count, hemoglobin, platelet count, C-reactive protein, procalcitonin, blood urea nitrogen, creatinine, total bilirubin, alanine aminotransferase, aspartate aminotransferase, fibrinogen, D-dimer, lactate dehydrogenase, creatine kinase, and arterial blood gases (lactate and PaO2/FiO2 ratio), were collected at admission. Additional platelet parameters, including plateletcrit (PCT, %), mean platelet volume (MPV, fL), platelet distribution width (%), and platelet larger cell ratio (P-LCR, %) were also gathered. According to the test projectmanual and reagent instructions of the Central Hospital of Wuhan, the normal reference interval of platelet count was 125–350 × 109/L. Therefore, thrombocytopenia was defined as a blood platelet <125 × 109/L, and non-thrombocytopenia was defined as a blood platelet 125 × 109/L. Acute Physiology and Chronic Health Evaluation II scores (APACHE II), sequential organ failure assessment, and CURB-65 criteria were determined within 24 h after admission. Data on all treatment measures, including antibiotic, antivirus, glucocorticoid, and intravenous immunoglobulin therapy and respiratory support, were acquired during hospitalization. Throat swab samples were collected from all suspected patients at admission, and the laboratory confirmation of SARS-CoV-2 was performed using real-time reverse transcription-polymerase chain reaction according to the manufacturer’s protocol (Beijing Genomics Institution and Geneodx biotechnology Co., Ltd.). Repeated tests for SARS-CoV-2 were performed in confirmed patients to verify viral clearance before hospital discharge.
Statistical analysis
Baseline characteristics as continuous and categorical variables were presented as median (interquartile range) and n (%), respectively, and examined by Mann–Whitney U test, χ2 test, or Fisher’s exact test where appropriate. The association between baseline platelet parameters and mortality risk was estimated by Cox proportional hazards regression models in terms of the following confounders: age, sex, baseline comorbidities (including chronic obstructive pulmonary disease, hypertension, diabetes, chronic kidney disease, cardiovascular disease, and cerebrovascular disease). Glucocorticoid and immunoglobulin might affect the hematopoietic system, and these treatments are common in clinical practice. In addition, decreased lymphocyte count represents the progression of the disease, C-reactive protein represents the overall inflammation, and augment blood lactate represents acute lung injury, tissue hypoxia and/or oxygen debt and associated mortality critical patients [10]. Therefore, we also considered these in regression models. Smoothing spline presenting the association of baseline platelet levels and platelets change with subsequent mortality was generated by utilizing the generalized additive model. Survival curve was plotted using the Kaplan–Meier method and examined using the log-rank test. All statistical analyses were performed using R software (The R Foundation, http://www.r-project.org, version 3.6.1) and EmpowerStats (http://www.empowerstats.com, X&Y Solutions, Inc., Boston, MA) unless otherwise indicated. A two-sided significance level of P = 0.05 was used to evaluate statistical significance.
Results
Patients characteristics
Among the 383 COVID-19 patients with median 18 days (range 4 to 50 days) follow-up period, 334 (87.2%) were discharged and survived, and 49 (12.8%) died. The clinical characteristics of all patients stratified by admission platelets are presented in Table I. The median age was 46 years, and 162 (42.3%) patients were male. No significant differences in comorbidities were observed between patients with thrombocytopenia and non-thrombocytopenia. Patients with thrombocytopenia at admission were likely older and had a higher APACHE II score than those with non-thrombocytopenia. Most patients were administered with antibiotics, and some were treated with ribavirin (88.3%), oseltamivir (25.6%), and arbidol (20.9%). Empiric systemic glucocorticoid therapy (58.2%) and intravenous immunoglobulin (56.1%) were used for anti-inflammatory treatment. Noninvasive ventilation was used on 51 patients (13.3%). The thrombocytopenia group had a higher proportion of noninvasive ventilation therapy (26.5% vs. 10.5%) and mortality rate (30.9% vs. 8.9%) than those without thrombocytopenia. The dynamic changes in platelet count from day 1 to day 14 after the onset of the disease were tracked to determine the major clinical features observed during COVID-19 progression. Compared with that for non-survivors, the level of platelets showed an increasing trend for survivors after admission (P < 0.05, Figure 1). Additionally, platelets were negatively associated with APACHE II score, higher of which indicates the higher disease severity at admission (Figure 2).
Table I.
Baseline characteristics of COVID-19 patients with thrombocytopenia and without thrombocytopenia.
| Total (n = 383) | Thrombocytopenia (n = 68) | Non-thrombocytopenia (n = 315) | P-valuea | |
|---|---|---|---|---|
| Age, median (IQR), y | 46 (34–61) | 52 (38–65) | 43 (33–60) | 0.004 |
| Male | 162 (42.3%) | 38 (55.9%) | 124 (39.4%) | 0.01 |
| Comorbidities | ||||
| COPD | 17 (4.4%) | 6 (8.8%) | 11 (3.5%) | 0.09 |
| Hypertension | 81 (21.1%) | 18 (26.5%) | 63 (20.0%) | 0.24 |
| Diabetes | 36 (9.4%) | 8 (11.8%) | 28 (8.9%) | 0.49 |
| Cardiovascular disease | 14 (3.7%) | 2 (2.9%) | 12 (3.8%) | >0.99 |
| Cerebrovascular disease | 14 (3.7%) | 3 (4.4%) | 11 (3.5%) | 0.72 |
| Chronic kidney disease | 19 (5.0%) | 6 (8.8%) | 13 (4.1%) | 0.12 |
| Baseline severity of illness | ||||
| CURB65 | 0.005 | |||
| 1 | 273 (71.3%) | 39 (57.4%) | 234 (74.3%) | |
| 1 | 110 (28.7%) | 29 (42.6%) | 81 (25.7%) | |
| APACHEII, median (IQR) | 2 (1–4) | 4 (2–8) | 2 (0–4) | <0.001 |
| Laboratory findings, median (IQR) | ||||
| White blood cell count, ×109/L | 4.8 (3.6–6.3) | 3.9 (2.7–5.1) | 5.0 (3.8–6.5) | <0.001 |
| Neutrophil count, ×109/L | 3.2 (2.0–4.5) | 2.8 (1.5–3.8) | 3.3 (2.2–4.7) | 0.005 |
| Lymphocyte count, ×109/L | 1.0 (0.7–1.4) | 0.8 (0.5–1.1) | 1.1 (0.8–1.5) | <0.001 |
| Hemoglobin, g/L | 131 (122–141) | 131 (120–141) | 131 (122–141) | 0.80 |
| Procalcitonin, ng/mL | 0.05 (0.04–0.08) | 0.06 (0.05–0.17) | 0.05 (0.04–0.07) | <0.001 |
| C-reactive protein, mg/dL | 1.2 (0.3–3.9) | 2.5 (0.8–4.5) | 1.0 (0.2–3.6) | 0.002 |
| Total bilirubin, mmol/L | 8 (6–12) | 9 (7–13) | 8 (6–11) | 0.023 |
| Alanine aminotransferase, U/L | 19 (13–30) | 24 (14–31) | 18 (13–30) | 0.12 |
| Aspartate aminotransferase, U/L | 21 (17–33) | 29 (20–41) | 21 (17–30) | <0.001 |
| Blood urea nitrogen, mmol/L | 4.0 (3.2–5.2) | 4.6 (3.5–6.0) | 4.0 (3.2–4.9) | 0.004 |
| Creatinine, μmol/L | 64 (52–78) | 69 (59–83) | 63 (50–76) | 0.006 |
| Fibrinogen, g/L | 2.9 (2.4–3.4) | 2.9 (2.5–3.2) | 2.8 (2.4–3.5) | 0.75 |
| D-dimer, mg/L | 0.4 (0.2–0.8) | 0.5 (0.3–1.0) | 0.4 (0.2–0.8) | 0.033 |
| Lactate, mmol/L | 1.2 (0.8–1.6) | 1.2 (0.8–1.8) | 1.2 (0.7–1.6) | 0.19 |
| PaO2:FIO2, mm Hg | 420 (270–528) | 337 (208–520) | 424 (280–540) | 0.008 |
| Platelet parameters, median (IQR) | ||||
| Platelet count, ×109/L | 174 (137–213) | 105 (92–116) | 186 (160–227) | <0.001 |
| Plateletcrit, % | 0.18 (0.14–0.22) | 0.11 (0.09–0.12) | 0.19 (0.16–0.23) | <0.001 |
| The mean platelet volume, fL | 10.0 (9.2–10.7) | 10.3 (9.6–10.9) | 9.9 (9.1–10.6) | 0.001 |
| The platelet distribution width, % | 15.5 (10.9–16.4) | 12.9 (11.0–16.5) | 15.8 (10.9–16.3) | 0.81 |
| The platelet larger cell ratio, % | 25.2 (20.1–31.1) | 28.5 (22.6–33.7) | 24.3 (19.8–30.2) | 0.003 |
| Treatment | ||||
| Quinolones | 254 (66.3%) | 42 (61.8%) | 212 (67.3%) | 0.38 |
| Cephalosporins | 191 (49.9%) | 41 (60.3%) | 150 (47.6%) | 0.06 |
| Ribavirin | 338 (88.3%) | 60 (88.2%) | 278 (88.3%) | >0.99 |
| Oseltamivir | 98 (25.6%) | 17 (25.0%) | 81 (25.7%) | 0.90 |
| Arbidol | 80 (20.9%) | 12 (17.6%) | 68 (21.6%) | 0.45 |
| Glucocorticoid therapy | 223 (58.2%) | 45 (66.2%) | 178 (56.5%) | 0.14 |
| Intravenous immunoglobulin | 215 (56.1%) | 39 (57.4%) | 176 (55.9%) | 0.82 |
| noninvasive ventilation | 51 (13.3%) | 18 (26.5%) | 33 (10.5%) | 0.001 |
| Clinical outcomes | <0.001 | |||
| Hospital discharge | 334 (87.2%) | 47 (69.1%) | 287 (91.1%) | |
| Death | 49 (12.8%) | 21 (30.9%) | 28 (8.9%) |
Abbreviations: APACHE II, Acute Physiology and Chronic Health Evaluation II; COPD, chronic obstructive pulmonary disease; FiO2, a fraction of inspired oxygen; IQR, interquartile range; PaO2, partial pressure of oxygen
ap values indicate differences between thrombocytopenia and non-thrombocytopenia patients.
Figure 1.
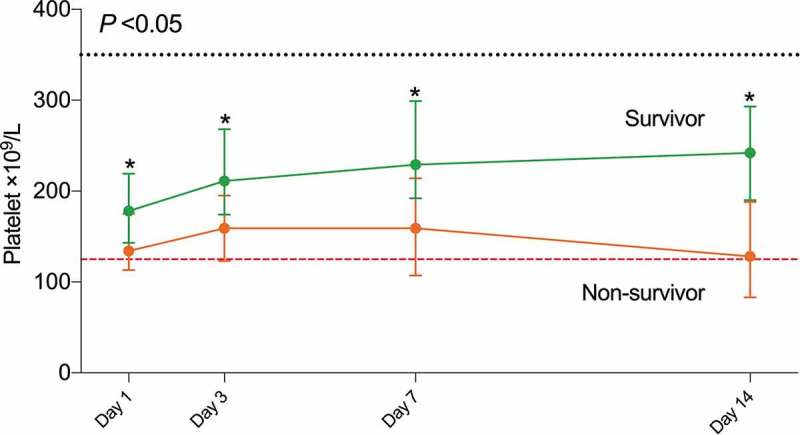
Timeline charts illustrate the platelet levels in 383 patients with COVID-19 (49 non-survivors and 334 survivors) on day 1, day 3, day 7, and day 14 after admission
Data are represented as median and 95% confidence interval. The dash lines in black show the upper normal limit of platelets, and the dash line in red shows the lower normal limit of platelets. Generalized linear-mixed models examined the differences in the platelets between non-survivor and survivor groups over time.* P < .05 for non-survivor vs. survivor.
Figure 2.
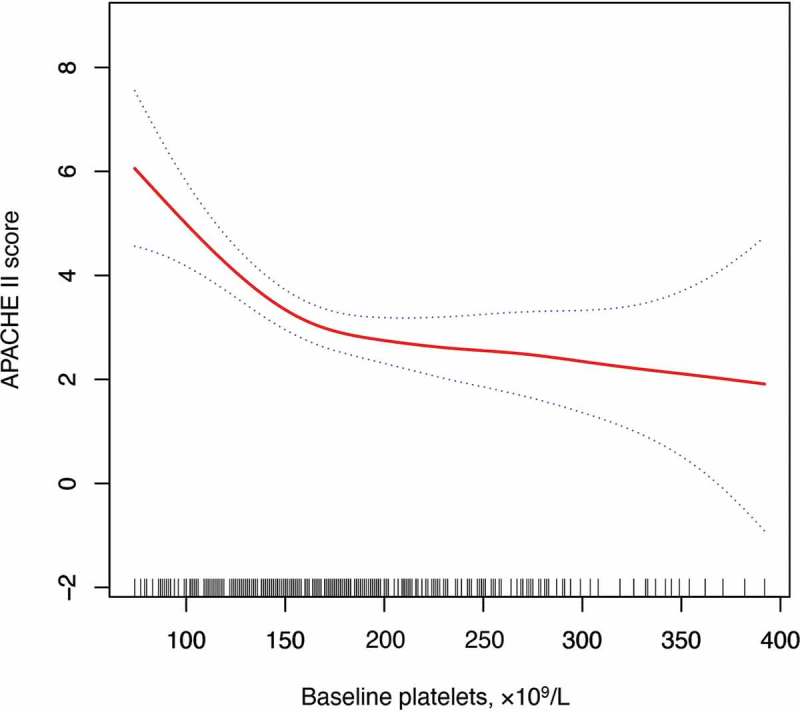
The smoothing spline presenting the association between baseline platelet count and APACHE II score was generated by utilizing the generalized additive model.
Laboratory findings
At admission, patients with thrombocytopenia had lower white blood cell, neutrophil, and lymphocyte count and higher levels of procalcitonin and C-reactive protein compared with those without thrombocytopenia (Table I). Remarkable differences were found in the levels of total bilirubin, aspartate aminotransferase, blood urea nitrogen, creatinine, and D-dimer. These indicators were significantly higher in patients with thrombocytopenia than in those without thrombocytopenia. Decreased levels of PaO2:FIO2 were observed in the thrombocytopenia group compared with those in the non-thrombocytopenia group. Analysis of platelet parameters revealed that patients with thrombocytopenia had lower levels of platelets and PCT and higher levels of MPV and P-LCR than those without thrombocytopenia.
Association between platelets and mortality
Cox proportional hazard regression models adjusted for several death-related risk factors at admission, including age, sex, baseline comorbidities, lymphocyte count, blood lactate, C-reactive protein, glucocorticoid therapy, and intravenous immunoglobulin. The results revealed that after adjustment for potential confounders, platelets and PCT were independent risks for mortality (Table II). In dose–response analyses, per 50 × 109/L increment in platelet count were significantly associated with 40% decreased mortality (HR 0.60, 95%CI: 0.43, 0.84) in all patients (Table III). In the analysis of 261 patients with a platelet count below 200 × 109/L, the association was still robust. A smoothing spline was further plotted to visually present the non-linear relationship between platelets at admission and mortality. We observed the mortality decreased with elevating platelet count, and the curve gradually tends to be gentle when platelet count >200 × 109/L (Figure 3a). Continuous tracking of the changes in platelets within the first 7 days after admission revealed that when platelets increased, the risk of death decreased during the treatment and vice-versa (Figure 3b). Further analysis showed that the worst outcome was noted in the subgroup of patients with a platelet level <200 × 109/L at admission and decrease in 7 days, followed by patients with a platelet level <200 × 109/L at admission and increase in 7 days, patients with a platelet level 200 × 109/L at admission and decrease in 7 days, and patients with a platelet level 200 × 109/L at admission and increase in 7 days (Figure 4).
Table II.
Association between platelet parameters and subsequent mortality estimated by Cox proportional hazards regression models.
| Quartile 1 | Quartile 2 | Quartile 3 | Quartile 4 | P trend | |
|---|---|---|---|---|---|
| Platelet levels, ×109/L | <138 | 138-174 | 174-213 | 213 | |
| No. of death/total | 25/96 | 10/94 | 10/95 | 4/98 | |
| Crude model | 5.42 (1.89, 15.60) | 2.20 (0.69, 7.02) | 2.29 (0.72, 7.31) | 1.00 (ref.) | <0.001 |
| Model 1 | 3.86 (1.27, 11.79) | 2.88 (0.86, 9.67) | 2.77 (0.84, 9.10) | 1.00 (ref.) | 0.02 |
| Model 2 | 4.24 (1.32, 13.61) | 3.74 (1.06, 13.18) | 3.72 (1.10, 12.53) | 1.00 (ref.) | 0.03 |
| Plateletcrit, % | <0.14 | 0.14–0.18 | 0.18–0.22 | 0.22 | |
| No. of death/total | 23/86 | 12/103 | 10/91 | 4/103 | |
| Crude model | 6.24 (2.16, 18.04) | 2.51 (0.81, 7.79) | 2.46 (0.77, 7.84) | 1.00 (ref.) | <0.001 |
| Model 1 | 4.82 (1.59, 14.57) | 2.49 (0.76, 8.17) | 2.51 (0.77, 8.17) | 1.00 (ref.) | 0.003 |
| Model 2 | 6.46 (2.03, 20.56) | 2.64 (0.76, 9.11) | 3.00 (0.90, 10.05) | 1.00 (ref.) | 0.001 |
| The mean platelet volume, fL | <9.2 | 9.2–10.0 | 10.0–10.7 | 10.7 | |
| No. of death/total | 8/87 | 10/101 | 11/93 | 20/102 | |
| Crude model | 0.54 (0.24, 1.23) | 0.57 (0.27, 1.21) | 0.56 (0.27, 1.18) | 1.00 (ref.) | 0.11 |
| Model 1 | 0.84 (0.36, 1.96) | 0.53 (0.24, 1.18) | 0.66 (0.30, 1.44) | 1.00 (ref.) | 0.35 |
| Model 2 | 0.67 (0.27, 1.65) | 0.49 (0.22, 1.12) | 0.46 (0.19, 1.09) | 1.00 (ref.) | 0.22 |
| The platelet distribution width, % | <11.0 | 11.0–15.5 | 15.5–16.4 | 16.4 | |
| No. of death/total | 11/96 | 16/95 | 9/93 | 13/99 | |
| Crude model | 0.87 (0.39, 1.95) | 1.13 (0.55, 2.36) | 0.84 (0.36, 1.97) | 1.00 (ref.) | 0.94 |
| Model 1 | 1.40 (0.61, 3.23) | 2.04 (0.93, 4.50) | 1.07 (0.44, 2.62) | 1.00 (ref.) | 0.19 |
| Model 2 | 1.46 (0.62, 3.45) | 2.78 (1.19, 6.45) | 0.94 (0.37, 2.42) | 1.00 (ref.) | 0.12 |
| The platelet larger cell ratio, % | <20 | 20-25 | 25-31 | 31 | |
| No. of death/total | 7/94 | 11/96 | 12/96 | 19/97 | |
| Crude model | 0.41 (0.17, 0.97) | 0.67 (0.32, 1.41) | 0.58 (0.28, 1.20) | 1.00 (ref.) | 0.06 |
| Model 1 | 0.74 (0.30, 1.82) | 0.74 (0.34, 1.62) | 0.62 (0.29, 1.30) | 1.00 (ref.) | 0.45 |
| Model 2 | 0.69 (0.27, 1.78) | 0.90 (0.39, 2.08) | 0.48 (0.20, 1.14) | 1.00 (ref.) | 0.58 |
Data are presented as hazard ratios (HR) and 95% confidence intervals.
P trend was estimated using the median value of each quartile.
Model 1 adjusted for age, sex, and baseline comorbidities (including chronic obstructive pulmonary disease, hypertension, diabetes, chronic
kidney disease, cardiovascular disease, and cerebrovascular disease);
Model 2 adjusted for model 1, plus glucocorticoid therapy, intravenous immunoglobulin, blood lactate, C-reactive protein, and lymphocyte count
Table III.
Association between the increase of platelet per 50 × 109/L and mortality risk.
| Increase per 50 × 109/L over the whole range of platelet count | P value | Increase per 50 × 109/L
when platelets below 200 × 109/L |
P value | |
|---|---|---|---|---|
| No. of death/total | 49/383 | 44/261 | ||
| Crude model | 0.51 (0.38, 0.69) | <0.001 | 0.50 (0.33, 0.76) | 0.001 |
| Model 1 | 0.63 (0.46, 0.85) | 0.003 | 0.62 (0.40, 0.95) | 0.03 |
| Model 2 | 0.60 (0.43, 0.84) | 0.003 | 0.62 (0.39, 0.98) | 0.04 |
Data are presented as hazard ratios (HR) and 95% confidence intervals
Model 1 adjusted for age, sex, and baseline comorbidities (including chronic obstructive pulmonary disease, hypertension, diabetes, chronic kidney disease, cardiovascular disease, and cerebrovascular disease);
Model 2 adjusted for model 1, plus glucocorticoid therapy, intravenous immunoglobulin, blood lactate, C-reactive protein, and lymphocyte count.
Figure 3.

The nonlinear relationship of (a) platelets at admission and (b) platelet changes with mortality.
The smoothing splines were generated utilizing generalized additive model and adjusted for age, sex, baseline comorbidities (including chronic obstructive pulmonary disease, hypertension, diabetes, chronic kidney disease, cardiovascular disease, and cerebrovascular disease), glucocorticoid therapy, intravenous immunoglobulin, blood lactate, C-reactive protein, and lymphocyte count. The red line indicates the risk of mortality and the blue dot line indicates 95% confidence intervals.
Figure 4.

Kaplan–Meier curves stratified by platelet count at admission and platelet changes in 7 days.
Discussion
Patients with COVID-19 usually have a rapid progression of pneumonitis and even develop ARDS and death. Among the 383 COVID-19 patients enrolled, most were admitted with platelets in the normal range, and a few had thrombocytopenia. Although the majority of current studies revealed a decreased number of platelets in groups with severe COVID-19 [6,7], no research has investigated the dynamic changes of platelets and estimated the association of baseline platelets and platelets change with subsequent mortality in patients infected with SARS-CoV-2. In the present study, clinical characteristics were compared between patients with and without thrombocytopenia. Cox proportional hazard regression analysis was used to adjust for several death-related risk factors at admission. Our study highlights the following: (a) thrombocytopenia at admission was associated with mortality that is almost three times higher than that in patients without thrombocytopenia; (b) platelet count was an independent risk factor for COVID-19 mortality; and (c) the dynamic changes of platelets were closely related to death during treatment. Our study highlights that platelet monitoring might be important for COVID-19 prognosis.
Enhanced platelet activation leading to platelet deposition in damaged pulmonary blood vessels has been supported by various clinical studies, and thrombocytopenia is an important feature of SARS [11,12]. Thrombocytopenia has exceeded 50% incidence rate in patients with SARS and is an important indicator of poor prognosis [13–15]. A meta-analysis with 1779 COVID-19 patients reported that thrombocytopenia was associated with threefold-enhanced risk of severe COVID-19 and an lower platelet count was observed with mortality [16]. Similar to this study, the current work confirmed that thrombocytopenia at admission is associated with death in patients with COVID-19. Platelets in patients with SARS are negatively correlated with their sVCAM-1 levels. sVCAM-1 is involved in adhesion and chemotaxis and contributes to early vascular injury and suppression of T cell function. Vascular injury or immunosuppression may explain the poor outcome [17]. By using the Cox regression model for multivariate analysis, we found that platelets and PCT are independent risk factors that predict death. Although platelets were routinely measured daily, the role of platelets and PCT in predicting the outcome of patients with COVID-19 has not been previously reported, and the correlation between platelet dynamics and disease prognosis has not been studied. Different platelet thresholds have been used in epidemiological studies for the incidence, risk factors, and consequences of thrombocytopenia among critically ill patients [18,19]. In our cohort, a non-linear relationship between platelets at admission and mortality was observed, and the trend tends to be gentle when platelet count >200 × 109/L (Figure 3a). Further analysis showed that patients with a platelet level <200 × 109/L at admission and decrease in 7 days had the highest mortality rate, whereas those with a platelet level 200 × 109/L at admission and increase in 7 days had the lowest mortality rate. Moreover, thrombocytopenia had a close relationship with prognosis even within the normal reference range. The dynamic changes of platelets within the first 7 days after admission were negatively correlated with the prognosis. Cox proportional hazards regression models displayed a 40% decrease in mortality risk for every 50 × 109/L increase in platelets. In summary, platelet count is an important prognostic marker for patients with COVID-19, and the dynamic levels of platelets during treatment are closely associated with death. PCT was calculated from platelet count, and its levels at admission still retained a detrimental effect on clinical outcome [20].
The mechanism of SARS-CoV-2 on thrombocytopenia is poorly understood, but several potential explanations are considered [21]. Histological examinations of lung necropsy from patients with COVID-19 revealed bilateral diffuse alveolar damage with cellular fibromyxoid exudates and interstitial mononuclear inflammatory infiltrates as dominated by lymphocytes; this finding has raised the possibility of immunopathological damage for lung tissues [22]. Damaged lung tissues would cause platelet activation and aggregation in the lungs, and thrombi formation at the site of the injury may lead to the consumption of platelets and megakaryocytes. In addition, SARS-CoV-2 induces a low-grade disseminated intravascular coagulopathy state characterized by the elevation of D-dimers and fibrinogen and further increases the consumption of platelets in damaged lungs. The lungs may be the sites of platelet release from mature megakaryocytes [23]. Inflammation and long-term oxygen treatment also result in extensive alveolar damage and other pulmonary pathological changes. The pulmonary capillary bed is morphologically altered, thus further affecting the lung megakaryocyte fragmentation and megakaryocytopoiesis. The increased consumption and decreased production of platelet may affect thrombocytopenia. Similar to SARS coronavirus, SARS-CoV-2 thrombocytopenia may involve other mechanisms. This new condition may directly infect hematopoietic precursor cells and inhibit their growth. CD 13 and CD66a are expressed on human bone marrow CD34+ cells. SARS-CoV-2 may induce growth inhibition by binding to the CD13 or CD66a of hematopoietic cells and bone marrow stromal cells, resulting in abnormal hematopoiesis and immunodeficiency [21]. The body undergoes immune-mediated hematopoietic stem cell damage, thereby further leading to thrombocytopenia.
This study is subjected to several limitations. First, as an observational study, we cannot conclude that the reported associations between platelet parameters and mortality are causal. Second, we cannot exclude the possibility of remaining residual confounding or unmeasured potential confounders. Third, the pathological mechanism of platelet parameters in the progression of COVID-19 remains poorly defined, and further clinical and basic research are necessary to clarify this issue. Although this study is the first to identify the association between platelet parameters and mortality risk in patients with COVID-19, a large-scale and multi-center study is warranted to confirm these findings.
Conclusions
This hospital-based cohort study among 383 confirmed patients with COVID-19 revealed an association of baseline platelets and platelets change with subsequent mortality. Hence, monitoring platelets during hospitalization may be important in the prognosis of patients with SARS-CoV-2.
Funding Statement
Health and Family Planning Commission of Wuhan Municipality [WX18A02].
Acknowledgements
We deeply regret and mourn all the lives lost in this disaster of SARS-CoV-2. We wish to express our deepest respect to all the people who are currently fighting against the outbreak of COVID-19.
Author’s contributions
LY and DL had full access to all the data in the study, and took responsibility for the integrity of the data and the accuracy of the data analysis. YL, YG, LC, and LY made substantial contributions to the study concept and design. YL and WS took responsibility for obtaining ethical approval, collecting samples, and confirming data accuracy. LC was in charge of the statistical analysis. YL, LC, and YG were in charge of the manuscript draft. YG, LC, WS, SZ, DL, and LY contributed to critical revision of the report. All authors reviewed and approved the final version.
Competing interests
None of the authors have conflicts of interest.
Consent for publication
Not available.
Ethical approval
The Ethics Committees of the Central Hospital of Wuhan approved this study.
Availability of data and material
The data that support the findings of this study are available from the corresponding authors on reasonable request. We can provide participant data without names and identifiers, but not the study protocol, or statistical analysis plan. After the publication of study findings, the data will be available for others to request. Once the data can be made public, the research team will provide an email address for communication. The corresponding authors have the right to decide whether to share the data or not based on the research objectives and plan provided.
References
- 1.Zhu N, Zhang D, Wang W, Li X, Yang B, Song J, Zhao X, Huang B, Shi W, Lu R, et al. A novel coronavirus from patients with pneumonia in China, 2019. N Engl J Med 2020;382:727–733. doi: 10.1056/NEJMoa2001017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Chen N, Zhou M, Dong X, Qu J, Gong F, Han Y, Qiu Y, Wang J, Liu Y, Wei Y, et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet 2020;395:507–513. doi: 10.1016/S0140-6736(20)30211-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Holshue ML, DeBolt C, Lindquist S, Lofy KH, Wiesman J, Bruce H, Spitters C, Ericson K, Wilkerson S, Tural A, et al. First case of 2019 novel coronavirus in the United States. N Engl J Med 2020;382:929–936. doi: 10.1056/NEJMoa2001191. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Pongpirul WA, Pongpirul K, Ratnarathon AC, Prasithsirikul W.. Journey of a thai taxi driver and novel coronavirus. N Engl J Med 2020;382:1067–1068. doi: 10.1056/NEJMc2001621. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Rothe C, Schunk M, Sothmann P, Bretzel G, Froeschl G, Wallrauch C, Zimmer T, Thiel V, Janke C, Guggemos W, et al. Transmission of 2019-nCoV infection from an asymptomatic contact in Germany. N Engl J Med 2020;382:970–971. doi: 10.1056/NEJMc2001468. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Guan WJ, Ni ZY, Hu Y, Liang WH, Ou CQ, He JX, Liu L, Shan H, Lei CL, Hui D, et al. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med 2020. doi: 10.1056/NEJMoa2002032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Zhou F, Yu T, Du R, Fan G, Liu Y, Liu Z, Xiang J, Wang Y, Song B, Gu X, et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet 2020. doi: 10.1016/S0140-6736(20)30566-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Brogly N, Devos P, Boussekey N, Georges H, Chiche A, Leroy O. Impact of thrombocytopenia on outcome of patients admitted to ICU for severe community-acquired pneumonia. J Infect 2007;55:136–140. doi: 10.1016/j.jinf.2007.01.011. [DOI] [PubMed] [Google Scholar]
- 9.World Health Organization Clinical management of severe acute respiratory infection when novel coronavirus (nCoV) infection is suspected: interim guidance. Published January 28, 2020. Accessed January31,2020https://www.who.int/publications-detail/clinical-management of-severe-acute-respiratory-infection-when-novel coronavirus-(ncov)-infection-is-suspected
- 10.Smith I, Kumar P, Molloy S, Rhodes A, Newman PJ, Grounds RM, Bennett ED. Base excess and lactate as prognostic indicators for patients admitted to intensive care. Intensive Care Med 2001;27:74–83. doi: 10.1007/s001340051352. [DOI] [PubMed] [Google Scholar]
- 11.Bone RC, Francis PB, Pierce AK. Intravascular coagulation associated with the adult respiratory distress syndrome. Am J Med 1976;61:585–589. doi: 10.1016/0002-9343(76)90135-2. [DOI] [PubMed] [Google Scholar]
- 12.Peiris JS, Yuen KY, Osterhaus AD, Stöhr K. The severe acute respiratory syndrome. N Engl J Med 2003;349:2431–2441. doi: 10.1056/NEJMra032498. [DOI] [PubMed] [Google Scholar]
- 13.Wong RS, Wu A, To KF, Lee N, Lam CW, Wong CK, Chan PK, Ng MH, Yu LM, Hui DS, et al. Haematological manifestations in patients with severe acute respiratory syndrome: retrospective analysis. BMJ 2003;326:1358–1362. doi: 10.1136/bmj.326.7403.1358. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Choi KW, Chau TN, Tsang O, Tso E, Chiu MC, Tong WL, Lee PO, Ng TK, Ng WF, Lee KC, et al. Outcomes and prognostic factors in 267 patients with severe acute respiratory syndrome in Hong Kong. Ann Intern Med 2003;139:715–723. doi: 10.7326/0003-4819-139-9-200311040-00005. [DOI] [PubMed] [Google Scholar]
- 15.Ko JH, Park GE, Lee JY, Lee JY, Cho SY, Ha YE, Kang CI, Kang JM, Kim YJ, Huh HJ, et al. Predictive factors for pneumonia development and progression to respiratory failure in MERS-CoV infected patients. J Infect 2016;73:468–475. doi: 10.1016/j.jinf.2016.08.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Lippi G, Plebani M, Michael Henry B. Thrombocytopenia is associated with severe coronavirus disease 2019 (COVID-19) infections: A meta-analysis. Clin Chim Acta 2020. doi: 10.1016/j.cca.2020.03.022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Chen RF, Chang JC, Yeh WT, Lee CH, Liu JW, Eng HL, Yang KD. Role of vascular cell adhesion molecules and leukocyte apoptosis in the lymphopenia and thrombocytopenia of patients with severe acute respiratory syndrome (SARS). Microbes Infect 2006;8:122–127. doi: 10.1016/j.micinf.2005.06.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Hui P, Cook DJ, Lim W, Fraser GA, Arnold DM. The frequency and clinical significance of thrombocytopenia complicating critical illness: a systematic review. Chest 2011;139:271–278. doi: 10.1378/chest.10-2243. [DOI] [PubMed] [Google Scholar]
- 19.Wang T, Liu Z, Wang Z, Duan M, Li G, Wang S, Li W, Zhu Z, Wei Y, Christiani DC, et al. Thrombocytopenia is associated with acute respiratory distress syndrome mortality: an international study. PLoS One 2014;9:e94124. doi: 10.1371/journal.pone.0094124. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Uğur M, Ayhan E, Bozbay M, Çiçek G, Ergelen M, Işık T, Uyarel H, Ertaş G, Çakıllı Y, Öz A, et al. The independent assocıatıon of plateletcrıt wıth long-term outcomes in patıents undergoıng prımary percutaneous coronary interventıon. J Crit Care 2014;29:978–981. doi: 10.1016/j.jcrc.2014.07.001. [DOI] [PubMed] [Google Scholar]
- 21.Yang M, Ng MH, Li CK. Thrombocytopenia in patients with severe acute respiratory syndrome (review). Hematology 2005;10:101–105. doi: 10.1080/10245330400026170. [DOI] [PubMed] [Google Scholar]
- 22.Xu Z, Shi L, Wang Y, Zhang J, Huang L, Zhang C, Liu S, Zhao P, Liu H, Zhu L, et al. Pathological findings of COVID-19 associated with acute respiratory distress syndrome. Lancet Respir Med 2020. doi: 10.1016/S2213-2600(20)30076-X.0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Lefrançais E, Ortiz-Muñoz G, Caudrillier A, Mallavia B, Liu F, Sayah DM, Thornton EE, Headley MB, David T, Coughlin SR, et al. The lung is a site of platelet biogenesis and a reservoir for haematopoietic progenitors. Nature 2017;544:105–109. doi: 10.1038/nature21706. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Citations
- World Health Organization Clinical management of severe acute respiratory infection when novel coronavirus (nCoV) infection is suspected: interim guidance. Published January 28, 2020. Accessed January31,2020https://www.who.int/publications-detail/clinical-management of-severe-acute-respiratory-infection-when-novel coronavirus-(ncov)-infection-is-suspected
Data Availability Statement
The data that support the findings of this study are available from the corresponding authors on reasonable request. We can provide participant data without names and identifiers, but not the study protocol, or statistical analysis plan. After the publication of study findings, the data will be available for others to request. Once the data can be made public, the research team will provide an email address for communication. The corresponding authors have the right to decide whether to share the data or not based on the research objectives and plan provided.


