Abstract
A 41-year-old male with a history of well controlled HIV presented with confusion and was found to have COVID-19. Lumbar puncture was negative. He had worsening encephalopathy with tonic-clonic seizure requiring intubation. He was treated with hydroxychloroquine and azithromycin with improvement in mental status back to baseline after 6 days.
Keywords: COVID-19, Encephalopathy, Seizures, HIV
Introduction
Coronavirus disease 2019 (COVID-19) was characterized by the World Health Organization (WHO) as a pandemic on March 11, 2020 [1]. This novel coronavirus emerged from Wuhan, China in December 2019 and has been causing respiratory infections with fever, dry cough, dyspnea, and myalgias as the most common signs and symptoms [2,3]. As of April 2, 2020, there have been over 1 million cases reported worldwide with 53,000 deaths. More severe respiratory illnesses and deaths from COVID-19 have been reported in elderly patients, who are also at greater risk of developing altered mental status. A few studies have reported neurologic manifestations in this age group including acute cerebrovascular diseases (CVA), impaired consciousness, and skeletal muscle injury [4]. We report a case of a middle-aged man with COVID-19 who developed acute encephalopathy and tonic-clonic seizure activity.
Case report
A 41-year-old male with a past medical history of well controlled HIV, maintained on dolutegravir-lamivudine with last CD4 count of 604 cells/cu mm and an undetectable viral load two months prior to presentation and recurrent HSV on chronic suppressive therapy presented with abdominal pain, intractable vomiting, and confusion. He became ill six days prior to presentation when the patient started experiencing a dry cough and intermittent fever relieved by antipyretics. On day of presentation, he was only oriented to self. Remainder of symptoms and their development are outlined in Fig. 1. His epidemiologic risk factors for COVID-19 included indirect exposure to a COVID-19 positive patient. Full lab work on day of presentation including COVID-19 testing was performed. Results on day 1 (Table 1) were pertinent for leukopenia. EKG showed sinus tachycardia with first degree AV block and a QTc interval of 424 ms. No respiratory distress was noted. CT chest revealed diffuse patchy nodular ground glass infiltrates (Fig. 2). The remainder of imaging studies including CT head were unremarkable.
Fig. 1.
Development of symptoms throughout the course of the illness.
Table 1.
Laboratory Workup.
| Metabolic Panel | Ref Range & Units | Day of Admission (03/18/2020) | 3/25/2020 | Day of Discharge 03/27/2020 |
|---|---|---|---|---|
| Creatinine | 0.8–1.3 mg/dL | 0.9 mg/dL | 1.0 mg/dL | 1.0 mg/dL |
| AST | 15–41 IU/L | 24 IU/L | 35 IU/L | 46 IU/L |
| ALT | 16–63 IU/L | 22 IU/L | 27 IU/L | 49 IU/L |
| Alkaline Phosphatase | 35–126 IU/L | 42 IU/L | 32 IU/L | 39 IU/L |
| Bilirubin, Total | 0.3–1.2 mg/dL | 0.7 mg/dL | 0.7 mg/dL | 0.4 mg/dL |
| Lactate | 0.4–2.0 mmol/L | 1.2 mmol/L | 1.0 mmol/L | 1.7 mmol/L |
| CBC with differential | Ref Range & Units | Day of Admission (03/18/2020) | 3/25/2020 | Day of Discharge 03/27/2020 |
|---|---|---|---|---|
| WBC | 3.80–10.50 K/μL | 4.57 K/μL | 4.75 K/μL | 5.57 K/μL |
| Hemoglobin | 13.7–17.5 g/dL | 15 g/dL | 14 g/dL | 15.3 g/dL |
| Platelets | 150–350 K/μL | 175 K/μL | 211 K/μL | 268 K/μL |
| Neutrophils, Absolute | 1.70–7.00 K/μL | 3.17 K/μL | 3.21 K/μL | 3.17 K/μL |
| Lymphocytes, Absolute | 1.20–3.50 K/μL | 0.99 K/μL | 0.90 K/μL | 1.39 K/μL |
| Monocytes, Absolute | 0.30–1.00 K/μL | 0.37 K/μL | 0.53 K/μL | 0.67 K/μL |
| Eosinophils, Absolute | 0.04–0.54 K/μL | 0 K/μL | 0.04 K/μL | 0.17 K/μL |
| Basophils, Absolute | 0.01–0.10 K/μL | 0.01 K/μL | 0.02 K/μL | 0.06 K/μL |
| Prognostic Markers | Ref Range & Units | Day of Admission (03/18/2020) | 3/25/2020 | Day of Discharge 03/27/2020 |
|---|---|---|---|---|
| LDH | 98−192 IU/L | 169 IU/L | 244 IU/L | 260 IU/L |
| Ferritin | 24−250 ng/mL | |||
| D-Dimer | 0.00 – 0.50 ug/mL | 6.66 ug/mL | ||
| Troponin | <0.05 ng/mL | <0.03 ng/mL | 0.06 ng/mL | |
| CRP | < = 7.48 mg/L | 11.3 mg/L | 63.08 mg/L | 14.05 mg/L |
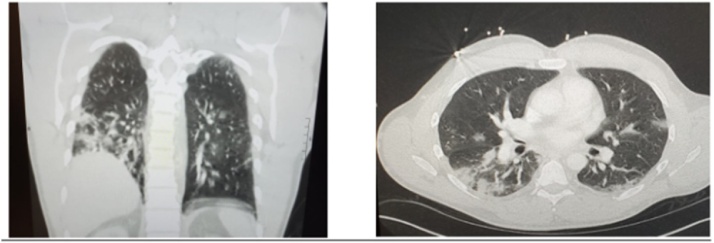
Fig. 2.
CT scan of the chest with coronal (left) and cross sectional (right) views showing diffuse patchy peripheral ground glass infiltrates most consolidative within the right lower lobe.
Because the patient presented with acute encephalopathy in the setting of HIV, he underwent a lumbar puncture (Table 2) with no white cells noted in the cerebrospinal fluid. He was started on cefepime, ampicillin, vancomycin, and acyclovir for empiric bacterial meningitis and herpes encephalitis coverage.
Table 2.
CSF and Infectious Workup.
| CSF Analysis | Ref Range Units | Day of Admission (03/18/20) |
|---|---|---|
| Color, CSF | Colorless | Colorless |
| Appearance, CSF | Clear | Clear |
| RBC, CSF | <1 /μL | 5 |
| WBC, CSF | 0 – 5 /μL | 0 |
| Glucose, CSF | 40−70 mg/dL | 81 |
| Protein, CSF | 15−45 mg/dL | 102 |
| Culture, CSF | No growth | No Growth at 96 h |
| Gram Stain, CSF | No organism seen | 3+ WBC seen, no organisms seen |
| HSV1 DNA, CSF | Not detected | Not detected |
| HSV2 DNA, CSF | Not detected | Not detected |
| West Nile Virus Ab IgG, CSF | <1.30 index | <1.30 |
| West Nile Virus Ab IgM, CSF | <0.90 index | <0.90 |
| Crypto Ag, CSF | Negative | Negative |
| Infectious Panel | Ref Range & Units | Day Of Admission (03/18/20) |
|---|---|---|
| COVID-19 (Pennsylvania DOH) | Not detected | Positive |
| T-helper cells (CD4) count | 443-1,705 cells/cu mm | 247 cells/cu mm |
| Influenza A/B PCR | Negative | Negative |
| Respiratory Viral Panel, PCR | Negative | Negative |
| Blood Cultures | Negative | Negative |
| RPR | Non- reactive | Non- reactive |
On day two of hospitalization, the patient was found to have worsening encephalopathy, agitation, and new-onset left sided ptosis. He subsequently developed witnessed tonic-clonic seizure complicated by a tongue laceration leading to respiratory arrest requiring intubation and sedation. MRI performed at that time was unremarkable. An EEG showed evidence of diffuse slowing but no epileptiform activity.
COVID-19 testing was noted to be positive and he was started on hydroxychloroquine 400 mg twice a day for one day followed by 200 mg twice a day for four days in addition to azithromycin 500 mg once followed by 250 mg daily for four days. Cefepime, ampicillin, and vancomycin were discontinued. Hospital course was further complicated by acute kidney injury which resolved after discontinuation of acyclovir on day 6 of presentation when HSV PCR was negative.
On day 6 of hospitalization, the patient’s level of consciousness improved off sedation (Fig. 3), and he was successfully extubated. Remdesivir was approved for compassionate use, however was not administered as patient had significant clinical improvement at that point. EKG on the day of discharge showed normal sinus rhythm with QTc interval of 501 ms.
Fig. 3.
Evolution of neurologic symptoms.
Discussion
While the primary signs and symptoms of COVID-19 are fever, cough, and dyspnea, in rare cases, encephalopathy may be the predominant presenting symptom. In terms of neurologic manifestations, retrospective analyses have reported CVA, impaired consciousness, and anosmia, but severe encephalopathy has rarely been reported [4].
The patient’s initial symptomatology included minimal respiratory complaints without oxygen requirements. He then quickly deteriorated, developing encephalopathy which was complicated by a witnessed seizure, as well as a cranial nerve palsy with left sided ptosis. A lumbar puncture did not reveal pleocytosis, indicating that COVID-19 likely did not cause a viral meningitis, although CSF PCR for COVID-19 was not done as it is not currently available in the United States. As this was the first atypical presentation of COVID-19 witnessed by the hospital staff, one of the main difficulties encountered was managing the patient's agitation while maintaining proper isolation precautions required for further imaging. This caused diagnostic delays and limited an expedient workup. Ultimately, MRI brain with and without contrast and EEG studies were obtained after the patient was intubated. Results were unremarkable, but could have been altered by the fact that the patient was sedated at the time of EEG, although benzodiazepines were not among the agents used for his sedation.
A similar case was described in a patient with a prodrome of cough and fever, who subsequently developed altered mental status and became nonverbal. Antiepileptics were initiated prophylactically due to abnormal epileptiform discharges on EEG; however, this patient had preexisting encephalomalacia from a previous CVA [5].
This case presented many challenges as it was one of the first atypical presentations of COVID-19 witnessed by the hospital staff. One of the biggest challenges was the ability to secure a safe setting for further workup, including imaging and EEG, in an encephalopathic and agitated patient who tested positive for COVID–19. In times when agitation prevents safe transport of patients to imaging/testing, intubation and sedation despite the absence of life-threatening respiratory complications should be considered as an option to achieve safer conditions for necessary diagnostic imaging and testing.
Several questions arise from this case. One question involves the patient’s history of well controlled HIV and COVID-19-induced leukopenia. Are patients that are well controlled on antiretroviral therapy inherently at greater risk for being infected with COVID-19? Does COVID-19-induced leukopenia adversely affect this patient population despite having a normal CD4 count? Does this population suffer from more severe symptoms? All of these questions deserve further study.
Another question involves the patient’s neurologic manifestations of this disease. If further cases of seizure activity are reported in COVID-19 positive patients, the usefulness of prophylactic antiepileptics will need to be evaluated especially if they present with significant encephalopathy even in the absence of abnormal brain anatomy. Presently, COVID-19 is a viral entity that is not yet fully understood and its epileptogenic potential is yet unclear, but will hopefully be better elucidated with more studies.
Declaration of Competing Interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
References
- 1.World Health Organization . 2020. WHO characterizes COVID-19 as a pandemic.https://www.who.int/emergencies/diseases/novel-coronavirus-2019/events-as-they-happen March 11, 2020. Accessed March 31, 2020. [Google Scholar]
- 2.Chen N., Zhou M., Dong X., Qu J., Gong F., Han Y. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet. 2020;395:507–513. doi: 10.1016/S0140-6736(20)30211-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Wang D., Hu B., Hu C., Zhu F., Liu X., Zhang J. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. JAMA. 2020 doi: 10.1001/jama.2020.1585]. [Epub] [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Mao L., Wang M., Chen S., Hu Y., Chen S., He Q. JAMA Neurol. 2020. Neurological manifestations of hospitalized patients with COVID-19 in Wuhan, China: a retrospective case series study. medRxiv. 02.22.20026500. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Filatov A., Sharma P., Hindi F., Espinosa P.S. Neurological complications of coronavirus disease (COVID-19): encephalopathy. Cureus. 2020;12(3):e7352. doi: 10.7759/cureus.7352. [DOI] [PMC free article] [PubMed] [Google Scholar]