Abstract:
Recent research suggests that SARS-CoV-2-infected individuals can be highly infectious while asymptomatic or pre-symptomatic, and that an infected person may infect 5.6 other individuals on average. This situation highlights the need for rapid, sensitive SARS-CoV-2 diagnostic assays capable of high-throughput operation that can preferably utilize existing equipment to facilitate broad, large-scale screening efforts. We have developed a CRISPR-based assay that can meet all these criteria. This assay utilizes a custom CRISPR Cas12a/gRNA complex and a fluorescent probe to detect target amplicons produced by standard RT-PCR or isothermal recombinase polymerase amplification (RPA), to allow sensitive detection at sites not equipped with real-time PCR systems required for qPCR diagnostics. We found this approach allowed sensitive and robust detection of SARS-CoV-2 positive samples, with a sample-to-answer time of ~50 min, and a limit of detection of 2 copies per sample. CRISPR assay diagnostic results obtained nasal swab samples of individuals with suspected COVID-19 cases were comparable to paired results from a CDC-approved quantitative RT-PCR (RT-qPCR) assay performed in a state testing lab, and superior to those produced by same assay in a clinical lab, where the RT-qPCR assay exhibited multiple invalid or inconclusive results. Our assay also demonstrated greater analytical sensitivity and more robust diagnostic performance than other recently reported CRISPR-based assays. Based on these findings, we believe that a CRISPR-based fluorescent application has potential to improve current COVID-19 screening efforts.
Keywords: CRISPR, COVID-19, Molecular diagnosis, SARS-CoV-2, Highly sensitive, Fluorescent detection
Highlights
-
•
Integrated CRISPR for COVID-19 clinical diagnosis.
-
•
Rapidly identify SARS-CoV-2-specific RNA signatures at an ultra-low concentration.
-
•
Detection environment friendly and compatible for high throughput COVID-19 screening in hospital.
-
•
Successful development and validation with swab samples from patients.
-
•
Improve diagnosis of individuals with suspected COVID-19 infections.
1. Introduction
SARS-CoV-2, first detected in China's Hubei province late in 2019, rapidly spread from its initial outbreak site to produce a pandemic (Zhou et al., 2020), and has to date been detected in more than 200 countries, where it has infected more than 1.9 million people and caused more than 116,000 deaths (Liu et al., 2020). However, disease control efforts are hindered by multiple factors, including difficulty in rapidly producing the number diagnostic tests required for such efforts, the apparent limited diagnostic sensitivity of current tests, and the technical expertise required to obtain valid results with them. Large scale testing is essential, but estimates indicate that large numbers of mild, asymptomatic or pre-symptomatic COVID-19 cases are not detected by current testing efforts (Kobayashi et al., 2020). In the U.S., one estimate suggest that only 1.6% of COVID-19 cases have been detected (Vollmer, 2020), while another study estimates that about 17.9% of individuals infected with SARS-CoV-2 are asymptomatic at their first positive test and may not develop symptoms for up to two weeks (Mizumoto et al., 2020). These are alarming statistics, since one estimate suggests that an infected individual may infect 5.6 additional people on average (Steven et al., 2020), and that individuals with asymptomatic or pre-symptomatic SARS-CoV-2 infections may be as infectious as individuals who are symptomatic (Ai et al., 2020; Liu et al., 2020; Lu et al., 2020; Mizumoto et al., 2020; Zou et al., 2020). Ultra-sensitive, inexpensive and high-throughput testing methods are thus required for effective large-scale screening efforts required to allow identification, isolation, and contact tracing of individuals without apparent disease, to improve local containment and to inform regional disease control efforts. Due to limited testing capacity, most countries and regions have prioritized testing for symptomatic and at-risk individuals. However, most symptoms associated with COVID-19, such as fever and cough, are non-specific and do not distinguish COVID-19 cases from individuals with other respiratory infections (Guan et al., 2020).
Nucleic acid tests employing RT-PCR, are the primary means employed to diagnose COVID-19 using respiratory samples (CDC, 2020; Udugama et al., 2020). Reverse transcription and PCR amplification can be consolidated into a single reaction to allow one-step assays that provide rapid, reproducible and high-throughput results, and this approach is used by the US CDC in its one-step real-time RT-PCR SARS-CoV-2 assay (CDC, 2020). Standard, quantitative real-time RT-PCR (RT-qPCR) assays require well-trained personnel and expensive laboratory instruments to obtain accurate and robust results, which can limit their practical application outside well-equipped facilities (Bachman, 2013; Wong and Medrano, 2005). A recently deployed isothermal assays for COVID-19 that uses the Abbott ID Now system requires less expensive equipment and less training, but also produces less definitive results. In this system, signals detected by 5 min and after 15 min indicate positive and negative results, respectively, but signals between these cut-offs are open to interpretation (Van Ness et al., 2003). Reports also indicate that the positive agreement rate of this assay is only 73.9%–80.4% (Harrington et al., 2020; Hogan et al., 2020; Smithgall et al., 2020). Thus, RT-qPCR assays are still the gold-standard for COVID-19 diagnosis.
Rapid and ultrasensitive COVID-19 diagnostic assays that are capable of high-throughput analyses and which do not require a high degree of technical expertise or sophisticated equipment are required to expand COVID-19 testing capacity. CRISPR-Cas/gRNA complexes have recently been used to sensitively detect nucleic acids, including in those derived from human pathogens (Bruch et al. 2019a, 2019b; Chen et al., 2018; Gootenberg et al., 2017; Hajian et al., 2019; Li et al. 2018, 2019; Lucia et al., 2020; Pardee et al., 2016). For example, one group employed a CRISPR-Cas12a approach (DNA endonuclease-targeted CRISPR trans reporter; DETECTR) to distinguish clinical specimens containing human papillomavirus 16 (HPV16) and HPV18, correctly identifying of 25/25 and 23/25 samples, respectively (Chen et al., 2018).
Isothermal amplification methods (e.g., recombinase polymerase amplification (RPA) and loop-mediated isothermal amplification (LAMP) ), that can provide analytical sensitivities similar to PCR without a thermocycler (Craw and Balachandran, 2012; Notomi et al., 2000; Zaghloul and El-Shahat, 2014) are being utilized in SARS-CoV-2 diagnostics currently under development (Yinhua et al., 2020; Zaghloul and El-Shahat, 2014). One recently published report, incorporated RT-LAMP with CRISPR-Cas12a to allow detection of SARS-CoV-2 in respiratory swab RNA extracts in a colorimetric lateral flow assay (Broughton et al., 2020). This assay was reported to rapidly and accurately detect SARS-CoV-2 positive samples, albeit with moderately reduced sensitivity when compare to qPCR assay performance in the same samples.
In this work, we describe a rapid and accurate RT-PCR CRISPR-Cas12a fluorescent reporter assay that demonstrates comparable diagnostic performance to a CDC-approved test performed in a state testing lab, without inconclusive or invalid results that were observed when the same samples were analyzed by qPCR in a clinical laboratory. Notably, this assay detected samples estimated to contain two copies of its RNA target, while the qPCR assay did not produce detectable target signal in samples containing less than five copies of its amplified DNA target.
2. Material and methods
2.1. Materials
The QIAamp DSP Viral RNA Mini Kit (#61904) for RNA extraction was purchased from QIAGEN (Hilden, Germany). The SuperScript™ IV One-Step RT-PCR System (#1235820), TaqPath™ 1-Step RT-qPCR Master Mix (4X) (#A15299), nuclease-free water (#4387936), and carrier RNA (#4382878) work as negative control was purchased from Thermo Fisher Scientific Inc. (Waltham, USA). The TwistAmp® Basic kit (#TABAS03KIT) for recombinase polymerase amplification (RPA) was purchased from TwistDx Limited (Maidenhead, UK). EnGen® Lba Cas12a (#M0653T) and NEBuffer™ 2.1 (#B7202S), ProtoScript® II Reverse Transcriptase (#M0368S) were purchased from New England Biolabs (Ipswich, USA). Primers, gRNA, probes (Table S1), including those for the 2019-nCoV CDC qPCR Probe Assay (CDC Emergency Use Authorization Kits, #10006606), and the 2019-nCoV_N_Positive Control (#10006625), Hs_RPP30 Control (#10006626), MERS-CoV Control (#10006624), and SARS-CoV Control (#10006623) were synthesized by Integrated DNA Technologies, Inc. (Coralville, USA).
2.2. Specimen collection and nucleic acid extraction
A total of 29 nasal swab specimens were collected based on clinical indications and current CDC guidance from Tulane Hospitals in New Orleans, LA from April 1 to April 10, 2020. Subsequently, 100 μL of RNA were extracted from equal volumes of clinical sample using the QIAamp DSP Viral RNA Mini Kit, and extracted RNA was stored at −80 °C until analysis.
2.3. Amplification of target fragments
For RT-PCR reactions, 5 μL isolated RNA sample was mixed with 15 μL of one-step RT-PCR mix containing 10 μL of 2× Platinum™ SuperFi™ RT-PCR Master Mix, 1 μL of forward primer (10 μM), 1 μL of reverse primer (10 μM), 0.2 μL of SuperScript™ IV RT Mix, and 2.8 μL of nuclease-free water. Samples were then incubated in a T100 thermocycler (Bio-Rad, California, USA) using a cDNA synthesis protocol (1 cycle at 55 °C for 10 min) immediately followed by a DNA amplification protocol (98 °C for 2 min; 35 cycles at 98 °C for 10 s, 60 °C for 10 s, and 72 °C for 15 s, followed by a final elongation step at 72 °C for 5 min). For RPA reactions, RPA pellets were resuspended in 29.5 μL of the supplied Rehydration Buffer, and 11.8 μL of this RPA solution, 0.5 μL of ProtoScript® II Reverse Transcriptase, 0.5 μL of forward primer (10 μM), 0.5 μL of reverse primer (10 μM), 0.2 μL of nuclease-free water, 2 μL of MgOAC solution (280 mM), and 5 μL of the isolated RNA sample were mixed and incubated at 42 °C for 20 min.
2.4. Optimization of the CRISPR-based fluorescent detection system (CRISPR-FDS)
CRISPR-FDS reactions were performed as fellow: 20 μL of RT-PCR or RPA reaction product was transferred to a 96-well half-area plate and mixed with 10 μL of a CRISPR reaction mixture containing 3 μL of 10× NEBuffer™ 2.1, 3 μL of gRNA (300 nM), 1 μL of EnGen® Lba Cas12a (1 μM), 1.5 μL of fluorescent probe (10 μM), and 1.5 μL of nuclease-free water. After incubation at 37 °C for 20 min in the dark, fluorescence signal was detected using SpectraMax i3x Multi-Mode Microplate Reader (Molecular Devices, LLC., San Jose, USA).
For the Cas12a substrate-dependent kinetics study, assays were conducted with molar ratios of Cas12a/gRNA to fluorescent probe set at 1:5, 1:10, 1:15, 1:20, and 1:25. For the temperature-dependent kinetics study, reactions were performed using a 1:20 Cas12a/gRNA to fluorescent probe ratio and incubated at 27 °C, 37 °C, and 42 °C. For the target-dependent kinetics study, the system was conducted with reactions that were performed using a 1:20 Cas12a/gRNA to fluorescent probe ratio and 106,107, 108, 109 and 1010 copies of the target fragments.
2.5. Clinical sample analysis
RT-qPCR was performed with the CDC 2019-Novel Coronavirus (2019-nCoV) Real Time RT-qPCR Diagnosis Panel. In these reactions, 5 μL of RNA sample was mixed with 1.5 μL of Combined Primer/Probe Mix, 5 μL of TaqPath™ 1-Step RT-qPCR Master Mix (4×), and 8.5 μL of nuclease-free water. RT-qPCR reactions were performed using a QuantStudio 6 Flex Real-Time PCR System (Thermo Fisher Scientific Inc., Waltham, USA) using the reaction conditions specified for this assay. For CRISPR-FDS assays, samples were processed as described in Section 2.4, using a 1:20 molar ratio of Cas12a/gRNA to fluorescent reporter, and analyzed after incubation at 37 °C for 20 min.
3. Results
3.1. CRISPR-based Fluorescent Diagnosis System for COVID-19 (COVID-19 CRISPR-FDS)
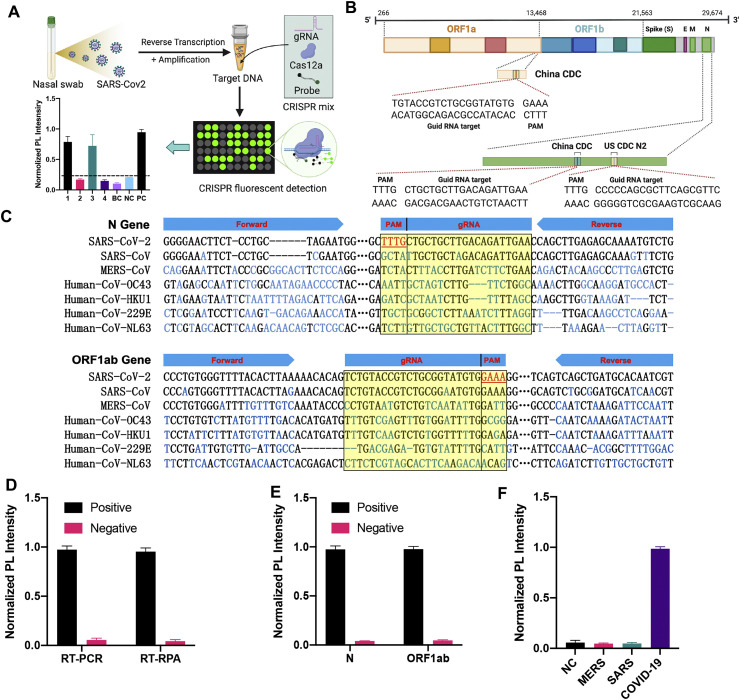
RT-qPCR is the most popular method employed for SARS-CoV-2 detection, but requires significant technical expertise, as well as equipment that is not available in all clinical laboratories. The COVID-19 CRISPR-FDS assay we describe uses a streamlined approach that does not require any special equipment beyond that found in most clinical and research laboratories. CRISPR-FDS employs three closely linked steps: RNA extraction, target amplification, and fluorescent signal detection (Fig. 1 A). In CRISPR-FDS, one-step RT-PCR or RT-RPA methods are used to amplify target regions from viral RNA extracted from nasal swabs, and the resulting amplicons are transferred in their entirety to the gRNA/Cas12a-based CRISPR system for fluorescence detection. Recognition of the target amplicon by the gRNA/Cas12a complex, which is regulated by a target-specific synthetic gRNA, induces the gRNA/Cas12a complex to specifically cleaves the target amplicon and non-specifically cleave a reporter oligo modified with fluorescein and a quencher molecule at each terminus to produce a fluorescent signal. Notably, this method has a ~50 min sample to answer time, employs easily obtained reagents and equipment available in most clinical laboratories, can be readily automated to meet a demand for high-throughput testing, and has the potential for use in point-of-care settings if assay results are analyzed with a portable fluorescence reader.
Fig. 1.
A CRISPR-based Fluorescent Diagnosis System for COVID-19 (COVID-19 CRISPR-FDS). (A) Schematic illustration of a CRISPR-FDS assay for detection of SARS-CoV-2 RNA in clinical samples. (B) SARS-CoV-2 genome map of COVID-19 CRISPR-FDS target sequences, and (C) sites in ORF1ab gene and the N protein gene that are detected COVID-19 CRISPR-FDS. Normalized CRISPR-FDS photoluminescent (PL) signal from SARS-CoV-2 RNA positive (109 copies/sample) and negative control (polyA carrier RNA) samples following (D) target amplification by RT-PCR or RPA, (E) by RT-PCR for each assay target, and (F) by RT-PCR for related beta coronavirus species (109 copies/sample). Bar graph data represents the mean ± SD, of three experimental replicates.
3.2. Target mapping and primer design
Numerous assays have now been developed to detect SARS-CoV-2, most of which employ strategies to that amplify species-specific regions of the SARS-CoV-2 RNA genome, including sites in the viral nucleocapsid (N) and envelope (E) genes, and open reading frame 1 ab (ORF1ab). The assay developed by the Chinese CDC targets sites with ORF1ab and the N gene, while a test from the US CDC targets two sites within the N gene, and one developed by the World Health Organization targets a region within the E gene, each of which contains a potential CRISPR recognition site (Fig. 1B). To permit direct comparison of the results from our proposed CRISPR-FDS approach with those from an establish test in clinical use, we designed primers and gRNAs (Table S1) to target the SARS-CoV-2 ORF1ab and N regions analyzed by the Chinese CDC assay (Fig. 1B). Bioinformatic analysis of these primers and gRNAs against common respiratory flora and other viral pathogens revealed that these sequences exhibited strong specificity for the SARS-CoV-2 genome (Table S2). Sequence alignment of these SARS-CoV-2 target regions with corresponding sites in related beta coronaviruses that cause middle east respiratory syndrome (MERS-CoV), severe acute respiratory syndrome (SARS-CoV), and human coronaviruses (Human-CoV) OC43/HKU1/229E/NL63, detected differing amounts of sequence variation between these species (Fig. 1C). The target region within the N gene exhibited the greatest degree of variation in this analysis, with multiple nucleotide differences detected along the aligned sequences. More differences were detected between SARS-CoV-2 and MERS-CoV than SARS-CoV in this region, in agreement with their relative phylogenetic distance. However, SARS-CoV still exhibited two or more variations with each N gene primer, while differed at three of four positions of the gRNA protospacer adjacent motif (PAM) required for CAS12a cleavage activity. The SARS-CoV ORF1ab region differed from the matching gRNA at a single position outside its PAM, but both primer regions used to produce the target for this gRNA exhibited at least nucleotide variant, decreasing the likelihood for false positive SARS-CoV recognition events. Analysis of RT-PCR-amplified and RT-RPA-amplified ORF1ab target sequence from a SARS-CoV-2 RNA positive control sample demonstrated that both approaches produced strong signal relative to the background present in their matching negative control samples (Fig. 1D). This difference was observed for both assay targets (Fig. 1E), and signal detected with MERS-CoV and SARS-CoV samples did not differ from negative control signal (Fig. 1F).
3.3. COVID-19 CRISPR-FDS assay optimization
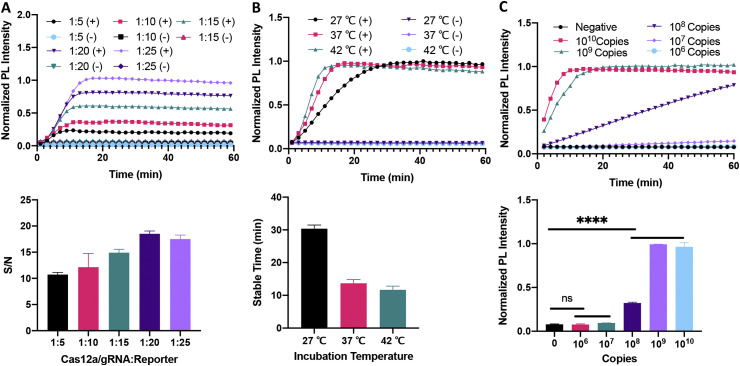
Since CRISPR activity determines the sensitivity of this assay, we conducted systematic studies of its reaction kinetics to optimize assay performance. CRISPR-mediated photoluminescence (PL) signal progressively increased with input fluorescent reporter substrate concentration when CRISPR-FPR assays containing a constant amount of target RNA were incubated with increasing amounts of substrate (Fig. 2 A). The signal-to-noise ratio increased with the ratio of reporter substrate to CRISPR/gRNA complex in this analysis, demonstrating the greatest signal-to-noise ratio at a 1:20 M ratio of Cas12a/gRNA to reporter and plateauing or modestly decreasing at a 1:25 ratio, the highest analyzed in this study. A potential decrease detected at the highest reporter concentration could be due to the background fluorescent signal of un-cleaved reporter. Given the benefits of high signal-to-noise ratio for assay sensitivity, we elected to use the 1:20 ratio for subsequent experiments. The final CRISPR-FDS signal intensity did not differ with temperature in assays incubated at 27 °C–42 °C, but incubation temperature significantly altered the rate of substrate conversion, with reaction completion times decreasing from 30 min at 27 °C, to 14 and 12 min at 37 °C and 42 °C, respectively (Fig. 2B). CRISPR-FDS reactions can thus be performed at ambient temperature, or at elevated temperature using isothermal water baths or heat blocks, without influencing the final assay outcome. Cas12a/gRNA complex cleavage activity is dependent upon the concentration of amplified target present during the final assay incubation period, so that substrate conversion rates vary with the target amplicon concentration during the assay readout. Significant CRISPR-FDS signal was observed within a 20 min readout period only in assays spiked with 108 copies of the target amplicon, while complete substrate conversion was detected only in samples spiked with ≥109 copies (Fig. 2C). The observed limit of detection (LOD) of 108 amplicons per CRISPR-FDS readout sample implies this assay should be very tolerant of RT-RPA or RT-PCR pre-amplification efficiency, since single copy RNAs should be detected when amplification efficiencies are >0.69 (See supplementary information). COVID-19 CRISPR-FDS assays performed with RT-PCR and RT-RPA amplified samples, detected samples spiked with ≥2 copies of the target RNA sequence, regardless of the method used in the pre-amplification step (Fig. 3 A and B), in good agreement with our calculated estimate for its LOD. This result compared favorably with the LOD of the qPCR gold-standard method, which was 5 copies/test (Fig. 3C). Signals of complete CRISPR-FDS reactions were also found to be stable for ≤1 h at ambient temperature, reducing the need to read signal quickly when testing large sample batches.
Fig. 2.
COVID-19 CRISPR-FDS assay optimization. (A) Substrate-dependent, (B) temperature-dependent, and (C) target-dependent effects on CRISPR-FDS signal. An aliquot containing 109 target amplicon copies, or an equivalent amount of poly A carrier RNA were analyzed as positive (+) and negative (−) control samples, respectively. Data presented in the top rows of each panel and the bottom row of (C) are normalized to the highest signal intensity detected in the corresponding experiment. Bar graph data represents the mean ± SD, of three experimental replicates. (ns, P > 0.05; ****,P < 0.0001).
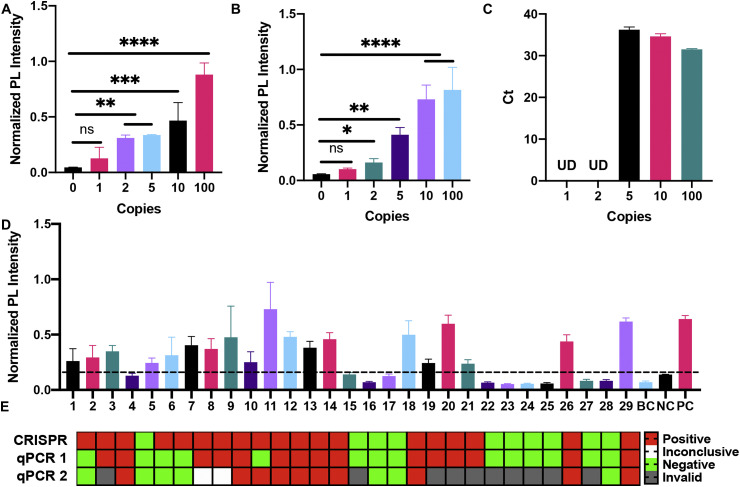
Fig. 3.
COVID-19 CRISPR-FDS analytical and diagnostic performance. Limit of detection (LOD) samples containing the indicated number of viral genomes after amplification by (A) RT-PCR and (B) RT-RPA for COVID-19 CRISPR-FDS analysis or by (C) RT-qPCR, indicated significant differences and undetermined (UD) results. (D) RT-PCR COVID-19 CRISPR-FDS results for a cohort of 29 individuals with suspected COVID-19 cases, run in parallel with blank (BC; nuclease free water), negative (NC; carrier RNA) and positive (PC; 109 target amplicon copies) control samples, where the dashed line indicates the threshold for a positive result. Results depict the mean ± SD of three experimental replicates. (E) Comparison of SARS-CoV-2 test results for matching patient samples analyzed by CRISPR-FDS, or by RT-qPCR by a state (qPCR 1) and a clinical testing laboratory (qPCR 2). (ns, P > 0.05; *, P < 0.05; **, P < 0.01; ***, P < 0.001; ****,P < 0.0001).
3.4. COVID-19 CRISPR-FDS diagnostic performance
For the analysis of clinical samples, a COVID-19 CRISPR-FDS assay result was considered positive if it was equal or greater than a cut-off threshold equal to the mean signal of the negative control samples plus three times its standard deviation (Kim et al., 2016). Using this criterion, 19 of 29 nasal swab samples were found to be SARS-CoV-2 positive (Fig. 3D). These results demonstrated good overall agreement with valid and conclusive test results generated by state and hospital laboratories using a CDC-authorized qPCR method (Fig. 3E). These patients were diagnosed based on the results from the state testing laboratory (qPCR 1), considering the poor quality of the hospital laboratories results. CRISPR-FDS exhibited complete concordance with the positive results obtained by the state testing laboratory (100% sensitivity), but detected SARS-CoV-2 signal in three samples (1, 5 and 6) that were judged to be negative by the state testing laboratory (71.4% specificity). In the absence of serology data or other information, it is not clear if these three samples represent false positive CRISPR-FDS assay results, or if they represent positive samples that were missed by the RT-qPCR method. Notably, 10 of the samples analyzed by the hospital produced invalid results and two others had inconclusive results, which compared poorly with the result rate from the state laboratory, and suggest the difficulty of introducing this assay in a hospital setting, particularly during an emerging epidemic.
4. Discussion
Although RT-qPCR is the most widely used diagnostic method for COVID-19, its sensitivity has not proven satisfactory, resulting in a relatively high number of false-negative results, so that a substantial number of infected individuals do not receive proper diagnoses and treatment. In a study of more than 1000 patients, 75% of COVID-19 suspects had negative RT-qPCR test results but positive chest computerized tomograph results, and 48% of these patients were considered highly likely to have had COVID-19, with an additional 33% considered probable cases (Ai et al., 2020). Notably, we observed a high frequency of invalid or inconclusive test results from samples analyzed in a clinical laboratory, all of which gave valid results when analyzed by RT-PCR in the state testing laboratory or by our CRISPR-FDS assay.
CRISPR applications are popular in detection assays due to the ability of Cas13 (Gootenberg et al., 2018) and Cas12a (Chen et al., 2018), respectively, to bind RNA or DNA targets specified by an input gRNA sequence to induce probe cleavage and thereby amplify the detection signal from nucleic acid amplification assays. Various isothermal amplification methods, such as RPA and LAMP, have been reported for the detection of COVID-19 (Ding et al., 2020; Lucia et al., 2020; Yu et al., 2020), but many problems were identified upon detailed analysis of these methods, including low sensitivity and low throughput. Our attempt to replicate results from one of the LAMP studies found that the described N gene and E gene LAMP reactions exhibited strong non-specific amplification, and that it was not possible to distinguish between positive and negative samples, even after titrating the amount input template or varying the reaction time or temperature (Fig. S1). We therefore did not pursue RT-LAMP as a potential means for template amplification in our CRISPR-FDS assay. Further, while we found that RPA worked well, we did not employ it in our final assay, since the necessary reagents are currently available from a single company, limiting its potential for immediate widespread application.
Many CRISPR protocols use paper strips to detect the signal output. This is a good solution for single sample testing since it does not require any equipment to read the results, but its LOD is much lower than fluorescence-based detection methods (Table S3). Our CRISPR-FDS assay can be readily performed in 96-well microtiter plates and read with fluorescent plate readers found in most well-equipped clinical laboratories to allow sensitive and high-throughput SARS-CoV-2 detection. Finally, our results indicate that our CRISPR-FDS asssay demonstrates results comparable to those obtained with a CDC-approved RT-qPCR assay in a state testing lab, but produced more valid results than were obtained when the same RT-qPCR assay was employed in a clinical setting. Notably, CRISPR-FDS produced positive results for a fraction of the samples that produced negative results with the RT-qPCR assay, although it was not possible to determine if these results represented false positive CRISPR-FDS results or false negative RT-qPCR results due to the lack of associated follow up data. CRISPR-FDS thus produces sensitive and robust results using readily available equipment and streamlined, high-throughput workflow suitable for use in clinical laboratories, and potentially applicable to point of care settings with the appropriate equipment. One potential drawback to our CRISPR-FDS approach is that it is designed to provide clear positive or negative results, not to quantify viral load, as can be determined by RT-qPCR assays using real-time PCR systems. We do not see this as a major drawback given the clear need for rapid, sensitive, and robust assays to diagnose COVID-19.
5. Conclusions
RT-PCR or RT-RPA-based CRISPR-FDS assays provide a sensitive and robust means for high-throughput COVID-19 diagnosis suitable for use in clinical laboratories, and exhibit the potential to enable reliable COVID-19 diagnosis at remote testing sites with minimal equipment, to improve large scale diagnosis efforts required to reduce the SARS-CoV-2 transmission and COVID-19 disease. However, further efforts need to be made to overcome the current bottleneck in point of care testing to permit self-testing or increase the testing capacity of small clinics that lack the resources to perform current assays. We are currently investigating the potential to integrate the RT-RPA-based CRISPR-FDS onto a microfluidic chip that can be read by a smart phone in attempt to meet this need.
CRediT authorship contribution statement
Zhen Huang: Methodology, Data curation, Validation, Writing - original draft. Di Tian: Resources, Validation. Yang Liu: Writing - original draft. Zhen Lin: Resources. Christopher J. Lyon: Writing - review & editing. Weihua Lai: Supervision. Dahlene Fusco: Resources. Arnaud Drouin: Resources. Xiaoming Yin: Resources, Investigation, Supervision. Tony Hu: Resources, Funding acquisition, Supervision. Bo Ning: Conceptualization, Validation, Writing - review & editing, Supervision.
Declaration of competing interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Acknowledgements
This work was supported by the startup fund of Dr. Tony Hu at Tulane University; Zhen Huang acknowledges support from the China Scholarship Council. The following reagent was obtained through BEI Resources, NIAID, NIH: Quantitative Synthetic RNA from SARS-Related Coronavirus 2, NR-52358.
Footnotes
Supplementary data to this article can be found online at https://doi.org/10.1016/j.bios.2020.112316.
Contributor Information
Tony Hu, Email: tonyhu@tulane.edu.
Bo Ning, Email: bning1@tulane.edu.
Appendix A. Supplementary data
The following is the Supplementary data to this article:
References
- Ai T., Yang Z., Hou H., Zhan C., Chen C., Lv W., Tao Q., Sun Z., Xia L. Radiology; 2020. Correlation of Chest CT and RT-PCR Testing in Coronavirus Disease 2019 (COVID-19) in China: A Report of 1014 Cases. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bachman J. Reverse-transcription PCR (RT-PCR) Methods Enzymol. 2013;530:67–74. doi: 10.1016/B978-0-12-420037-1.00002-6. [DOI] [PubMed] [Google Scholar]
- Broughton J.P., Deng X., Yu G., Fasching C.L., Servellita V., Singh J., Miao X., Streithorst J.A., Granados A., Sotomayor-Gonzalez A., Zorn K., Gopez A., Hsu E., Gu W., Miller S., Pan C.-Y., Guevara H., Wadford D.A., Chen J.S., Chiu C.Y. CRISPR–Cas12-based detection of SARS-CoV-2. Nat. Biotechnol. 2020:1–5. doi: 10.1038/s41587-020-0513-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bruch R., Baaske J., Chatelle C., Meirich M., Madlener S., Weber W., Dincer C., Urban G.A. CRISPR/Cas13a-Powered electrochemical microfluidic biosensor for nucleic acid amplification-free miRNA diagnostics. Adv. Mater. 2019;31(51):1905311. doi: 10.1002/adma.201905311. [DOI] [PubMed] [Google Scholar]
- Bruch R., Urban G.A., Dincer C. CRISPR/Cas powered multiplexed biosensing. Trends Biotechnol. 2019;37(8):791–792. doi: 10.1016/j.tibtech.2019.04.005. [DOI] [PubMed] [Google Scholar]
- CDC . U.S. Centers for Disease Control and Prevention Division of Viral Diseases; 2020. CDC 2019-Novel Coronavirus (2019-nCoV) Real-Time RT-PCR Diagnostic Panel. [Google Scholar]
- Chen J.S., Ma E., Harrington L.B., Da Costa M., Tian X., Palefsky J.M., Doudna J.A. CRISPR-Cas12a target binding unleashes indiscriminate single-stranded DNase activity. Science. 2018;360(6387):436–439. doi: 10.1126/science.aar6245. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Craw P., Balachandran W. Isothermal nucleic acid amplification technologies for point-of-care diagnostics: a critical review. Lab Chip. 2012;12(14):2469–2486. doi: 10.1039/c2lc40100b. [DOI] [PubMed] [Google Scholar]
- Ding X., Yin K., Li Z., Liu C. All-in-One dual CRISPR-cas12a (AIOD-CRISPR) assay: a case for rapid, ultrasensitive and visual detection of novel coronavirus SARS-CoV-2 and HIV virus. bioRxiv. 2020 doi: 10.1101/2020.03.19.998724. In preparation. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gootenberg J.S., Abudayyeh O.O., Kellner M.J., Joung J., Collins J.J., Zhang F. Multiplexed and portable nucleic acid detection platform with Cas13, Cas12a, and Csm6. Science. 2018;360(6387):439–444. doi: 10.1126/science.aaq0179. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gootenberg J.S., Abudayyeh O.O., Lee J.W., Essletzbichler P., Dy A.J., Joung J., Verdine V., Donghia N., Daringer N.M., Freije C.A., Myhrvold C., Bhattacharyya R.P., Livny J., Regev A., Koonin E.V., Hung D.T., Sabeti P.C., Collins J.J., Zhang F. Nucleic acid detection with CRISPR-Cas13a/C2c2. Science. 2017;356(6336):438–442. doi: 10.1126/science.aam9321. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Guan W.J., Ni Z.Y., Hu Y., Liang W.H., Ou C.Q., He J.X., Liu L., Shan H., Lei C.L., Hui D.S.C., Du B., Li L.J., Zeng G., Yuen K.Y., Chen R.C., Tang C.L., Wang T., Chen P.Y., Xiang J., Li S.Y., Wang J.L., Liang Z.J., Peng Y.X., Wei L., Liu Y., Hu Y.H., Peng P., Wang J.M., Liu J.Y., Chen Z., Li G., Zheng Z.J., Qiu S.Q., Luo J., Ye C.J., Zhu S.Y., Zhong N.S., China Medical Treatment Expert Group for, C Clinical characteristics of coronavirus disease 2019 in China. N. Engl. J. Med. 2020;328(18):1708–1720. doi: 10.1056/NEJMoa2002032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hajian R., Balderston S., Tran T., deBoer T., Etienne J., Sandhu M., Wauford N.A., Chung J.-Y., Nokes J., Athaiya M., Paredes J., Peytavi R., Goldsmith B., Murthy N., Conboy I.M., Aran K. Detection of unamplified target genes via CRISPR–Cas9 immobilized on a graphene field-effect transistor. Nature Biomedical Engineering. 2019;3(6):427–437. doi: 10.1038/s41551-019-0371-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Harrington A., Cox B., Snowdon J., Bakst J., Ley E., Grajales P., Maggiore J., Kahn S. Comparison of Abbott ID Now and Abbott m2000 methods for the detection of SARS-CoV-2 from nasopharyngeal and nasal swabs from symptomatic patients. J. Clin. Microbiol. 2020 doi: 10.1128/JCM.00798-20. JCM.00798-00720. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hogan C.A., Sahoo M.K., Huang C., Garamani N., Stevens B., Zehnder J., Pinsky B.A. Five-minute point-of-care testing for SARS-CoV-2: not there yet. J. Clin. Virol. 2020;128 doi: 10.1016/j.jcv.2020.104410. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kim D., Garner O.B., Ozcan A., Di Carlo D. Homogeneous entropy-driven amplified detection of biomolecular interactions. ACS Nano. 2016;10(8):7467–7475. doi: 10.1021/acsnano.6b02060. [DOI] [PubMed] [Google Scholar]
- Kobayashi T., Jung S.M., Linton N.M., Kinoshita R., Hayashi K., Miyama T., Anzai A., Yang Y., Yuan B., Akhmetzhanov A.R., Suzuki A., Nishiura H. Communicating the risk of death from novel coronavirus disease (COVID-19) J. Clin. Med. 2020;9(2) doi: 10.3390/jcm9020580. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Li S.Y., Cheng Q.X., Wang J.M., Li X.Y., Zhang Z.L., Gao S., Cao R.B., Zhao G.P., Wang J. CRISPR-Cas12a-assisted nucleic acid detection. Cell Discov. 2018;4(1):1–4. doi: 10.1038/s41421-018-0028-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Li Y., Li S., Wang J., Liu G. CRISPR/Cas systems towards next-generation biosensing. Trends Biotechnol. 2019;37(7):730–743. doi: 10.1016/j.tibtech.2018.12.005. [DOI] [PubMed] [Google Scholar]
- Liu Y., Gayle A.A., Wilder-Smith A., Rocklov J. The reproductive number of COVID-19 is higher compared to SARS coronavirus. J. Trav. Med. 2020;27(2) doi: 10.1093/jtm/taaa021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Liu Q., Liu Z., Zhu J., Zhu Y., Li D., Gao Z., Zhou L., Tang Y., Zhang X., Yang J., Wang Q. Assessing the Global Tendency of COVID-19 Outbreak. medRxiv. 2020 doi: 10.1101/2020.03.18.20038224. Submitted for publication. [DOI] [Google Scholar]
- Lu R., Zhao X., Li J., Niu P., Yang B., Wu H., Wang W., Song H., Huang B., Zhu N., Bi Y., Ma X., Zhan F., Wang L., Hu T., Zhou H., Hu Z., Zhou W., Zhao L., Chen J., Meng Y., Wang J., Lin Y., Yuan J., Xie Z., Ma J., Liu W.J., Wang D., Xu W., Holmes E.C., Gao G.F., Wu G., Chen W., Shi W., Tan W. Genomic characterisation and epidemiology of 2019 novel coronavirus: implications for virus origins and receptor binding. Lancet. 2020;395(10224):565–574. doi: 10.1016/S0140-6736(20)30251-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lucia C., Federico P.-B., Alejandra G.C. An Ultrasensitive, Rapid, and Portable Coronavirus SARS-CoV-2 Sequence Detection Method Based on CRISPR-Cas12. bioRxiv. 2020 doi: 10.1101/2020.02.29.971127. Submitted for publication. [DOI] [Google Scholar]
- Mizumoto K., Kagaya K., Zarebski A., Chowell G. Estimating the asymptomatic proportion of coronavirus disease 2019 (COVID-19) cases on board the Diamond Princess cruise ship, Yokohama, Japan, 2020. Euro Surveill. 2020;25(10) doi: 10.2807/1560-7917.ES.2020.25.10.2000180. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Notomi T., Okayama H., Masubuchi H., Yonekawa T., Watanabe K., Amino N., Hase T. Loop-mediated isothermal amplification of DNA. Nucleic Acids Res. 2000;28(12):E63. doi: 10.1093/nar/28.12.e63. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pardee K., Green A.A., Takahashi M.K., Braff D., Lambert G., Lee J.W., Ferrante T., Ma D., Donghia N., Fan M., Daringer N.M., Bosch I., Dudley D.M., O'Connor D.H., Gehrke L., Collins J.J. Rapid, low-cost detection of zika virus using programmable biomolecular components. Cell. 2016;165(5):1255–1266. doi: 10.1016/j.cell.2016.04.059. [DOI] [PubMed] [Google Scholar]
- Smithgall M.C., Scherberkova I., Whittier S., Green D.A. Comparison of Cepheid Xpert Xpress and Abbott ID Now to Roche Cobas for the Rapid Detection of SARS-CoV-2. Journal of Clinical Virology. 2020;128 doi: 10.1016/j.jcv.2020.104428. 104428. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Steven S., Yen Ting L., Chonggang X., Ethan R.-S., Nick H., Ruian K. High contagiousness and rapid spread of severe acute respiratory syndrome coronavirus 2. Emerging Infectious Disease journal. 2020;26(7) doi: 10.3201/eid2607.200282. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Udugama B., Kadhiresan P., Kozlowski H.N., Malekjahani A., Osborne M., Li V.Y.C., Chen H., Mubareka S., Gubbay J., Chan W.C.W. Diagnosing COVID-19: the disease and tools for detection. ACS Nano. 2020;14(4):3822–3835. doi: 10.1021/acsnano.0c02624. [DOI] [PubMed] [Google Scholar]
- Van Ness J., Van Ness L.K., Galas D.J. Isothermal reactions for the amplification of oligonucleotides. Proc. Natl. Acad. Sci. Unit. States Am. 2003;100(8):4504–4509. doi: 10.1073/pnas.0730811100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Vollmer C.B.S. 2020. Average Detection Rate of SARS-CoV-2 Infections Is Estimated Around Six Percent University of Goettingen. [Google Scholar]
- Wong M.L., Medrano J.F. Real-time PCR for mRNA quantitation. Biotechniques. 2005;39(1):75–85. doi: 10.2144/05391RV01. [DOI] [PubMed] [Google Scholar]
- Yinhua Z, Jin X, Sun L., Raphael O.N., Wei H., Tanner N.A. Rapid Molecular Detection of SARS-CoV-2 (COVID-19) Virus RNA Using Colorimetric LAMP. medRxiv. 2020 doi: 10.1101/2020.02.26.20028373. Submitted for publication. [DOI] [Google Scholar]
- Yu L., Wu S., Hao X., Li X., Liu X., Ye S., Han H., Dong X., Li X., Li J. medRxiv; 2020. Rapid Colorimetric Detection of COVID-19 Coronavirus Using a Reverse Tran-Scriptional Loop-Mediated Isothermal Amplification (RT-LAMP) Diagnostic Plat-form: iLACO. Submitted for publication. [DOI] [Google Scholar]
- Zaghloul H., El-Shahat M. Recombinase polymerase amplification as a promising tool in hepatitis C virus diagnosis. World J. Hepatol. 2014;6(12):916–922. doi: 10.4254/wjh.v6.i12.916. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zhou P., Yang X.L., Wang X.G., Hu B., Zhang L., Zhang W., Si H.R., Zhu Y., Li B., Huang C.L., Chen H.D., Chen J., Luo Y., Guo H., Jiang R.D., Liu M.Q., Chen Y., Shen X.R., Wang X., Zheng X.S., Zhao K., Chen Q.J., Deng F., Liu L.L., Yan B., Zhan F.X., Wang Y.Y., Xiao G.F., Shi Z.L. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature. 2020;579(7798):270–273. doi: 10.1038/s41586-020-2012-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zou L., Ruan F., Huang M., Liang L., Huang H., Hong Z., Yu J., Kang M., Song Y., Xia J., Guo Q., Song T., He J., Yen H.L., Peiris M., Wu J. SARS-CoV-2 viral load in upper respiratory specimens of infected patients. N. Engl. J. Med. 2020;382(12):1177–1179. doi: 10.1056/NEJMc2001737. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.