Since the outbreak of COVID-19 caused by SARS-CoV-2, we tested 5 different blood specimens that were confirmed positive for SARS-CoV-2 IgG and IgM antibodies [1]. The measurements were for anti-nuclear antibody (ANA), anti-extractable nuclear antigen (ENA), anti-double-stranded DNA (dsDNA), actin antibody, mitochondrial antibody, rheumatoid factor (RF), and C1q immune complexes. We were surprised to find out that 3 of the 5 specimens had significant elevations in ANA, ENA, actin and mitochondrial antibodies, but not against dsDNA or RF. This prompted us to investigate patterns of cross-reactivity between SARS-CoV-2 and autoimmune target proteins.
Vaccine-induced autoimmunity from autoimmune cross-reactivity is associated with narcolepsy, Guillain-Barré syndrome, multiple sclerosis, demyelinating neuropathies, systemic lupus erythematosus, and postural orthostatic tachycardia syndrome in susceptible subgroups as reported by Segal and Shoenfeld [2]. Due to the significant red flags for the potential cross-reactive interactions with the current COVID-19 pandemic, we studied the relationships between spike and nuclear proteins of SARS-CoV-2 and autoimmune target proteins.
Commercially available mouse monoclonal antibody made against recombinant SARS coronavirus spike protein and rabbit monoclonal antibody made against SARS coronavirus nucleoprotein were applied at optimal dilution to the SARS-CoV-2 proteins and to 50 different tissue antigens using enzyme-linked immunosorbent assay (ELISA). Recombinant SARS-CoV-2 spike protein S1 and recombinant SARS-CoV-2 nucleocapsid protein were purchased from RayBiotech. ELISA wells were coated with nuclear antigens, dsDNA, F-actin, and mitochondria (M2) antigen purchased from different companies. An additional 45 tissue antigens used in this study have been previously described [9]. Each SARS-CoV-2 antibody was applied to quadruplicate wells. After the completion of all ELISA steps, the developed color was measured at 405 nm.
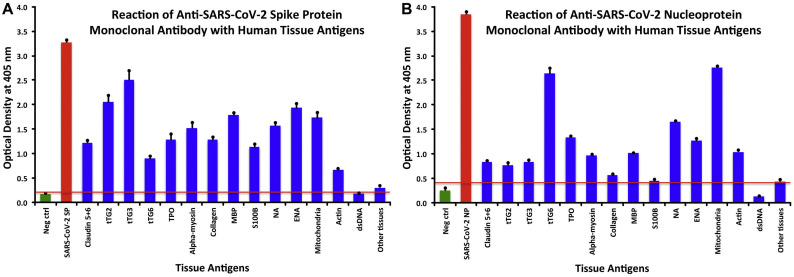
Looking at the reaction between SARS-CoV-2 spike protein antibody and tissue proteins (Fig. 1A), we found that the strongest reactions were with transglutaminase 3 (tTG3), transglutaminase 2 (tTG2), ENA, myelin basic protein (MBP), mitochondria, nuclear antigen (NA), α-myosin, thyroid peroxidase (TPO), collagen, claudin 5+6, and S100B. The reaction of this antibody was not as strong with several other antigens (Fig. 1A).
Fig. 1.
(A) Reaction of anti-SARS-CoV-2 spike protein monoclonal antibody with human tissue antigens. (B) Reaction of anti-SARS-CoV-2 nucleoprotein monoclonal antibody with human tissue antigens.
The nucleoprotein antibody showed some overlap in immune cross-reactivity with anti-spike protein antibody. As shown in Fig. 1B, nucleoprotein antibody reacted strongly with mitochondria, tTG6, NA, TPO, ENA, TG, actin, and MBP. Similar to spike protein, the nucleoprotein antibody reaction was not as strong with several other antigens as shown in Fig. 1A and B.
As the number of SARS-CoV-2 infections increase from day to day, scientists are learning that the damage caused by this virus can extend well beyond the lungs, where infection can lead to pneumonia and the often fatal condition called acute respiratory distress syndrome [3]. The virus can in fact affect the body from head to toe, including the nervous [4], cardiovascular [5], immune [6], and digestive systems [7].
Is it possible that some of the extensive organ, tissue, and cellular damage done by SARS-CoV-2 is due to viral antigenic mimicry with human tissue?
If the answer is yes, then we may face an increase in the rates of autoimmune disease in the future, because any factor that causes chronic inflammation in the body can potentially induce autoimmune disease.
Because SARS-CoV-2 attacks the respiratory system first, in a very interesting letter [8] Kanduc and Shoenfeld suggested that because the SARS-CoV-2 spike glycoprotein and lung surfactant proteins shared 13 out of 24 pentapeptides, the immune response following infection with SARS-CoV-2 may lead to cross-reactions with pulmonary surfactant proteins, followed by SARS-CoV-2-associated lung disease [8]. Based on their findings, they warned against the use of the entire SARS-CoV-2 antigens in the vaccines and cautioned that perhaps the use of only unique peptides would be the most effective way to fight the SARS-CoV-2 infection. Very similar suggestions were made by Razim et al., in designing a vaccine against Clostridium difficile [9]. Two sequences, peptide 9 and peptide 10, of C. difficile were recognized not only by the sera of patients with C. difficile infections but also by the sera of patients with autoimmune disease. Razim et al. concluded that before considering a protein as a vaccine antigen, special care should be taken in analyzing the sequence of tissue cross-reactive epitopes in order to avoid possible future side effects [9].
We agree with Razim et al., and we feel that our own findings that 21 out of 50 tissue antigens had moderate to strong reactions with the SARS-CoV-2 antibodies are a sufficiently strong indication of cross-reaction between SARS-CoV-2 proteins and a variety of tissue antigens beyond just pulmonary tissue, which could lead to autoimmunity against connective tissue and the cardiovascular, gastrointestinal, and nervous systems.
We live in critical times when the world may be veering towards the very real possibility of requiring immunity certification “passports” earned by prior infection with SARS-CoV-2 or vaccination before being allowed to travel, or perhaps even to work [10].
At the moment, scientists are frantically trying to develop either a definitive cure, neutralizing antibodies, or a vaccine to protect us from contracting the disease in the first place, and they want it right now. We must consider that finding a vaccine for a disease may normally take years. There are reasons for all the precautions involved in developing a vaccine, not the least of which are unwanted side-effects. In light of the information discussed above about the cross-reactivity of the SARS-CoV-2 proteins with human tissues and the possibility of either inducing autoimmunity, exacerbating already unhealthy conditions, or otherwise resulting in unforeseen consequences, it would only be prudent to do more extensive research regarding the autoimmune-inducing capacity of the SARS-CoV-2 antigens. The promotion and implementation of such an aggressive “immune passport” program worldwide in the absence of thorough and meticulous safety studies may exact a monumental cost on humanity in the form of another epidemic, this time a rising tide of increased autoimmune diseases and the years of suffering that come with them.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Declaration of Competing Interest
None.
Contributor Information
Aristo Vojdani, Email: drari@msn.com.
Datis Kharrazian, Email: datis56@gmail.com.
References
- 1.Whitman J.D., Hiatt J., Mowery C.T., Shy B.R., Yu R., Yamamoto T.N. Test performance evaluation of SARS-CoV-2 serological assay. MedRxiv. 2020 doi: 10.1101/2020.04.25.20074856. (preprint) [DOI] [Google Scholar]
- 2.Segal Y., Shoenfeld Y. Vaccine-induced autoimmunity: the role of molecular mimicry and immune crossreaction. Cell Mol. Immunol. 2018;15(6):586–594. doi: 10.1038/cmi.2017.151. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Zhou P., Yang X.-L., Wang X.-G., Hu B., Zhang L., Zhang W. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature. 2020;579(7798):270–273. doi: 10.1038/s41586-020-2012-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Nath A. Neurologic complications of coronavirus infections. Neurology. 2020;94(19):809–810. doi: 10.1212/WNL.0000000000009455. [DOI] [PubMed] [Google Scholar]
- 5.Zheng Y.-Y., Ma Y.-T., Zhang J.-Y., Xie X. COVID-19 and the cardiovascular system. Nat. Rev. Cardiol. 2020;17(5):259–260. doi: 10.1038/s41569-020-0360-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Shi Y., Wang Y., Shao C., Huang J., Gan J., Huang X. COVID-19 infection: the perspectives on immune responses. Cell Death Different. 2020;27:1451–1454. doi: 10.1038/s41418-020-0530-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Lin L., Jiang X., Zhang Z., Huang S., Zhang Z., Fang Z. Gastrointestinal symptoms of 95 cases with SARS-CoV-2 infection. Gut. 2020;69(6):997–1001. doi: 10.1136/gutjnl-2020-321013. [DOI] [PubMed] [Google Scholar]
- 8.Kanduc D., Shoenfeld Y. On the molecular determinants of the SARS-CoV-2 attack. Clin. Immunol. 2020;215:108426. doi: 10.1016/j.clim.2020.108426. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Razim A., Pacyga K., Aptekorz M., Martirosian G., Szuba A., Pawlak-Adamska E. Epitopes identified in GADPH from Clostridium difficile recognized as common antigens with potential autoimmunizing properties. Sci. Rep. 2018;8(1):13946. doi: 10.1038/s41598-018-32193-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Hall M.A., Studdert D.M. Privileges and immunity certification during the COVID-19 pandemic. JAMA. 2020 May 6 doi: 10.1001/jama.2020.7712. [DOI] [PubMed] [Google Scholar]