Abstract
Lisfranc injuries are relatively uncommon but carry devastating consequences if left untreated. Although many surgical techniques have been proposed for best operative management, there is an ongoing debate over which procedure is superior. We performed a systematic review and meta-analysis comparing the outcomes of transarticular screw fixation and dorsal bridge plating in management of Lisfranc injuries. Ovid MEDLINE, Ovid Embase and Cochrane Central Register of Controlled Trials (CENTRAL) were searched to identify randomised controlled trials (RCTs) and cohort studies comparing the outcomes between screw and dorsal plate fixation. The pooled outcome data were calculated by random and fixed effect models. One prospective cohort and three retrospective studies were identified with a total of 210 patients with mean follow up of 40.6 months. All papers were analysed for quality using the modified Newcastle Ottawa score. The results show that dorsal bridge plating is associated with better American Orthopaedic Foot and Ankle Society score (AOFAS) compared with transarticular screw fixation (OR – 0.71, 95% CI -1.31 to −0.10, p = 0.02). Dorsal plating may also be associated with fewer cases of arthritis, although this was not significant (OR 2.46, 95% CI 0.89 to 6.80, p = 0.08). We found no significant differences between the groups in terms of Foot Function Index (FFI), post traumatic arthritis and failure of hardware material. Although our results suggest dorsal bridge plating may provide superior functional outcomes, there is a scarcity of literature with little robustness to make definitive conclusions. High quality randomised trials are required.
Keywords: Transarticular screw, Dorsal bridge plating, Lisfranc, Infection, Arthritis, Post-operative function
1. Introduction
Lisfranc injuries (tarsometatarsal dislocations or fracture dislocations) are relatively uncommon. The goals of treatment are to achieve a painless, plantigrade stable foot with return to premorbid function.1 Suboptimal treatment can lead to chronic pain, arthritis, flat foot deformity, residual ligament instability and associated soft tissue injuries.2 Transarticular screw fixation in the midfoot has been the traditional surgical technique in the management of Lisfranc injuries.3, 4, 5 Their rigid fixation should theoretically maintain anatomical reduction until ligamentous stability is restored. However, studies have reported complications of screw fixation such as articular disruption, metal work breakage, failure of fracture compression and re-fracture through screw hole upon its removal.6,7 Cadaveric studies have promoted the use of dorsal bridge plates, shown to be a more favourable biomechanical construct compared to transarticular screws in rigid fixation of Lisfranc injuries.6,8 This comes with the added benefit of avoiding penetration of the articular surface, extra-articular placement and bypassing comminuted fractures, thereby allowing better reduction.7,9 However, unlike transarticular screws, dorsal bridge plates cannot be placed percutaneously, increasing the risk of soft tissue injury, neurovascular damage and wound leakage. Controversy exists on which surgical technique results in better surgical outcomes. Our objective was to perform a systematic review and meta-analysis to investigate the outcomes between dorsal bridge plating (the intervention) and transarticular screw fixation (the comparator).
2. Methods
A systematic review and meta-analysis was carried out and reporting according to the standards in the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA).10
2.1. Eligibility criteria
We included all studies that were randomised controlled trials (RCTs) and cohort studies that compared outcomes of transarticular screw fixation and dorsal bridge plating of Lisfranc injuries. Patients less than 18 years of age were excluded.
2.2. Outcome measures
Outcome measures were post-operative infection rate, American Orthopaedic Foot and Ankle Society (AOFAS) functional score, Foot Function Index (FFI) score, post-traumatic arthritis and failure of hardware material.
2.3. Literature search strategy
The following databases were searched: Ovid MEDLINE (Ovid MEDLINE(R) ALL 1946 to March 06, 2020), Ovid Embase (Embase 1974–2020 Week 10), and Cochrane Central Register of Controlled Trials (CENTRAL). The search strategies for Ovid MEDLINE and Ovid Embase incorporated two search concepts – Lisfranc/tarsometatarsal fracture and injury terms, and plate and bridging terms, with the two search concepts being combined using the Boolean operator AND. These two search concepts represent the P and the I of the PICO question. The relatively small number of results meant there was no need to include the comparator C, screw fixation, in the search strategies. Both free text terms and relevant subject headings were used. The search strategy for Ovid MEDLINE is given in Appendix 1. The search strategy for Cochrane CENTRAL used just a single search concept for Lisfranc and tarsometatarsal terms, as the number of results was relatively small and no additional search concept was necessary, thus ensuring maximum sensitivity. The searches were carried out on 9th March 2020. The literature search was not restricted to the English language or publication date. All relevant articles and reviews were examined for further relevant citations.
2.4. Study selection
Two authors (K.B and A.S) independently reviewed the titles and abstracts from the search results, after which potentially suitable papers were reviewed in full paper format by each author independently. Those that met the eligibility criteria were chosen and any discrepancies highlighted and resolved (J.M).
2.5. Data collection
The data collected included study-related data (authors, country of origin, year of publication, published journal and study design) and demographics and clinical information (age, sex and duration of follow up). All outcome measures were recorded by the selecting author independently (K.B and A.S.).
2.6. Data synthesis and statistical analysis
Review Manager 5.3 software was used for data synthesis and analysis. Odds ratios (OR) were used for all dichotomous variables (post-operative infection, post-traumatic arthritis and failure of hardware material). An odds ratio >1 favoured the transarticular screw group regarding each complication. The standard mean differences (SMD) between transarticular screw fixation and plating were assessed for the continuous parameters, FFI and AOFAS. Statistical heterogeneity was assessed using the value I2 and result of chi-squared. A P-value of <0.1 and an I2 greater than 50% were considered suggestive of statistical heterogeneity, prompting a random-effects modelling estimate. Otherwise a fixed effect model was used. Articles in which standard deviation were not measured to pool the data were assigned elementary inequalities and approximations to estimate the variance as per Hozo et al.11
2.7. Methodological quality
Methodological quality of included articles were evaluated by two co-authors (K.B. and A.S.) to assess the risk of bias. Cochrane Risk of Bias tool was intended to be used in analysing bias in RCTs to include selection, attrition and reporting bias.12 Cohort studies were assessed using the modified Newcastle-Ottawa scale which assessed each study in terms of comparability of study groups, selection of study groups and the ascertainment of outcome of interest.13
3. Results
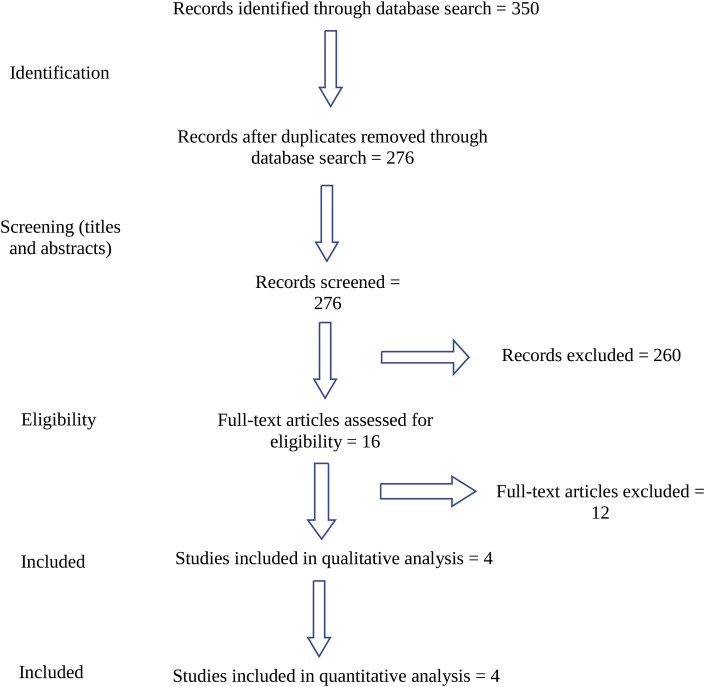
A total of 350 primary studies were identified, with 276 after deduplication. 260 papers were excluded upon abstract review, leaving 16 studies for full text review. 12 full text articles were excluded based on the eligibility criteria: 4 were identified in the full text to be case studies and 8 did not have an appropriate comparison arm (whether dorsal bridge plating or transarticular screw fixation). This left 4 studies for final quantitative and qualitative analysis. Fig. 1 shows the study selection flow according to PRISMA guidelines. One study was a prospective cohort,14 with the other three retrospective cohort studies.15, 16, 17
Fig. 1.
PRISMA flow diagram for study selection.
In total in the four included studies there were 210 subjects with acute Lisfranc injuries with a mean follow up of 40.6 months. Of these, 93 patients underwent transarticular screw fixation, with 117 receiving dorsal bridge plating. The basic characteristics of all included studies are presented in Table 1.
Table 1.
Baseline characteristics of included studies.
| Paper | Author | Year | Study Design | Sample size | Transarticular screw fixation | Dorsal bridge plating | Mean age | Gender | Follow up (months) |
|---|---|---|---|---|---|---|---|---|---|
| Outcome comparison of Lisfranc injuries treated through dorsal plate fixation versus screw fixation | Hu et al.14 | 2014 | Prospective cohort | 60 | 28 | 32 | 46 | N/A | 31 |
| Functional outcomes after temporary bridging with locking plates in Lisfranc injuries | Van Koperen et a l15 | 2016 | Retrospective cohort | 34 | 13 | 21 | 43.8 | 19 M, 15F | 56.9 |
| Functional outcomes Post Lisfranc injury – Transarticular screws, Dorsal Bridge or Combination treatment | Lau et al.16 | 2017 | Retrospective cohort | 33 | 14 | 19 | n/a | 26 M, 7F | 57.7 |
| Dorsal bridge plating or transarticular screws for Lisfranc fracture dislocations | Kirzner et al.17 | 2018 | Retrospective cohort | 83 | 38 | 45 | 36.8 | 62 M, 21F | 34 |
3.1. Methodological quality of studies
Using the Modified Newcastle-Ottawa Scale, one study was rated of good quality,14 two fair quality,16,17 and one poor (Table 2).18 Both fair quality studies had the possibility of selection bias regarding the allocation of patients in the differing treatment groups. The poor-quality study did not comment on the comparability of patient demographics between both groups.
Table 2.
Risk of bias summary showing authors’ judgement about each risk of bias judgement. ∗: no risk of bias. –: high risk of bias.
| Modified Newcastle-Ottawa Scale | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Study | Selection | Comparability | Outcome | Quality of study as per AHRQ standards | ||||||
| Representativeness of exposed cohort | Selection of non-exposed cohort | Ascertainment of exposure | Outcome of interest not present at start of study | Study controls for age/sex | Study controls for ≥3 risk factors | Assessment of outcome | Follow up > 1 year | Adequacy of follow up of cohorts | ||
| Hu 2014 | ∗ | ∗ | ∗ | ∗ | – | ∗ | ∗ | ∗ | ∗ | Good |
| Van Koperen 2016 | ∗ | ∗ | ∗ | ∗ | – | – | ∗ | ∗ | ∗ | Poor |
| Lau 2017 | – | – | ∗ | ∗ | ∗ | ∗ | ∗ | ∗ | ∗ | Fair |
| Kirzner 2018 | – | – | ∗ | ∗ | ∗ | ∗ | ∗ | ∗ | ∗ | Fair |
3.2. Outcome: post-operative infection
Post-operative infection was reported in all four studies.14, 15, 16, 17 There were no significant differences between the transarticular screw and dorsal bridge plating group in infection rates (OR 1.04, 95% confidence interval 0.43 to 2.53, p = 0.92) Fig. 2. There was a low level of heterogeneity amongst the studies (I2 = 0, p = 0.75).
Fig. 2.
Forest plots of the comparison for a) post-operative infection, b) post-traumatic arthritis, c) Implant failure, d) AOFAS score and e) FFI score.
3.3. Outcome: post traumatic arthritis
Post traumatic arthritis was reported in two studies.14,15 This included 94 patients. There were no significant differences between transarticular screw and dorsal bridge plating group in arthritis (OR 2.46, 95% CI 0.89 to 6.80, p = 0.08) Fig. 2. There was a low level of heterogeneity amongst the studies (I2 = 0, p = 0.78).
3.4. Outcome: implant failure
Two studies of 143 patients reported on this outcome.14,17 There were no significant differences between both groups in implant failure post-operatively (OR 0.46, 95% CI 0.09 to 2.39, p = 0.35) Fig. 2. There was a moderate level of heterogeneity amongst studies (I2 = 57%, p = 0.13).
3.5. Outcome: AOFAS
All four studies reported on this outcome.14, 15, 16, 17 The dorsal bridge plating patients had significantly favourable functional outcomes based on their AOFAS score compared to the transarticular group (OR – 0.71, 95% CI -1.31 to −0.10, p = 0.02) Fig. 2. There was however a high level of heterogeneity amongst the studies (I2 = 76%, p = 0.006).
3.6. Outcome: Foot Function Index
Foot function index (FFI) scores were reported in two studies of 67 patients.15,16 There was no significant difference in the FFI score between both groups (OR -0.04, 95% CI -0.53 to 0.45, p = 0.87) Fig. 2. There was a low level of heterogeneity amongst the studies (I2 = 0, p = 0.87).
4. Discussion
We performed a systematic review and meta-analysis on reported outcomes between dorsal bridge plating (the intervention) and transarticular screw fixation (the comparator).
Our analysis suggests dorsal bridge plating is associated with better AOFAS score compared with transarticular screw fixation (OR – 0.71, 95% CI -1.31 to −0.10, p = 0.02). We also found dorsal plating may be associated with fewer cases of arthritis although this was not significant (OR 2.46, 95% CI 0.89 to 6.80, p = 0.08). We found no difference in FFI, rates of infection and implant failure. The quality of evidence available ranged from low to adequate.
The superiority of dorsal bridge plating in AOFAS scores can be attributed to its biomechanical construct. It bypasses the articular surface, limiting arthrosis, thereby improving functional outcome. Furthermore, if the plate breaks at the joint normal joint motion may occur without need for subsequent hardware material. Contrast this with transarticular screw breakage through the joint which limits tarsometatarsal joint motion thereby delaying time to functional recovery. If screws through the dorsal plate break, the distal threads can be left in the metatarsals or cuneiforms without further joint damage or soft tissue irritation.6 With dorsal bridge plating, early postoperative range of motion is feasible, limiting joint stiffness, muscle atrophy and disuse osteopenia - all factors influencing AOFAS scoring. The poor AOFAS score in transarticular fixation in Van Koperen et al. study may have resulted from this cohort having more polytrauma, open fractures and higher energy trauma compared to the plating group.15 Furthermore, differences in AOFAS scores between the treatment groups may have been due to weight bearing status. However, this was minimised as 3 of the 4 studies were consistent with weight bearing status, with both dorsal bridge plating and transarticular screw fixation groups undergoing non-weight bearing for 6 weeks with progressive full weight bearing up to 3 months.14,16,17 Post-operative rehabilitation was not commented upon in the remaining study.15 Kirzner et al. found a trend of better anatomical reduction in the plating group, suggesting the improved functional outcome may be a result of the improved maintenance of anatomical reduction rather than plating.17
Although not statistically significant in this review, lower rates of arthritis are observed in bridge plating due to its extra-articular surface properties. Hu et al. reported nearly twice as many screw fixations to have arthritic changes (46.4%) compared to dorsal plating (25%). Good quality studies are required to compare such expected effects.14
A proposed drawback of plate fixation is the potential need for greater dissection, which is thought to increase risks of infection.6,8 However, our systematic review showed no evidence of this. Open reduction increases possibility of removing intra-articular debris or an interposed capsule, allowing for improved reduction by direct inspection.18, 19, 20
The main limitation in all the studies appears to be a small number of patients. This may lead to a type 2 statistical error (i.e. a false positive due to random error), even when determining the pooled effect of the included studies. An appropriately powered randomised controlled trial (RCT) is required to determine whether the lack of significance difference for some outcomes is true. All our studies were non-RCTs which have the greatest potential of selection bias. However, a recently registered RCT is aiming to compare such clinical outcomes between the two treatment modalities over a one-year period. Such results, currently awaiting, may help in defining the desired treatment option.21 Furthermore despite the superior functional outcomes in dorsal bridge plating, there was a high level of heterogeneity amongst the studies. Such could be explained by subgroup analyses of variables including smoking and diabetes, both of which were unfortunately lacking in data. For example, in the case of diabetes: one study only mentioned patient population with diabetes,17 one excluded diabetics,14 and two did not mention the condition.15,16
In conclusion, our systematic review and meta-analysis suggests that dorsal bridge plating for acute Lisfranc injuries may be associated with better functional outcomes compared to transarticular screw fixation. The available evidence is limited and inadequate to make definitive conclusions. The current literature requires high-quality randomised controlled trial to investigate this, with one already under way.21
5. Learning points
-
1.
Transarticular screw fixation has been one of the traditional methods of Lisfranc fracture fixation
-
2.
Cadaveric studies have shown Dorsal bridge plating may be a superior biomechanical construct avoiding the common complications seen in transarticular screw fixation
-
3.
Four low to moderate quality studies in literature comparing the two treatment strategies in regards to the following clinical outcomes: AOFAS, FFI, post-operative infection, post-traumatic arthritis and implant failure
-
4.
Our findings suggest dorsal bridge plating may lead to superior AOFAS scores although high level of heterogeneity amongst studies
-
5.
High-quality randomised controlled trials required to investigate whether lack of significant differences between some outcomes are true
Financial disclosure
None reported.
Funding
No funding was acquired for this project.
CRediT authorship contribution statement
Khalis Boksh: Conceptualization, Methodology, Software, Validation, Formal analysis, Investigation, Resources, Data curation, Writing - original draft, Writing - review & editing, Visualization, Project administration. Ashwini Sharma: Validation, Investigation, Data curation. Douglas Grindlay: Resources, Writing - review & editing. Pip Divall: Resources. Jitendra Mangwani: Validation, Writing - review & editing, Supervision, Project administration.
Declaration of competing interest
None reported.
Appendix 1.
Ovid MEDLINE search strategy.
-
1
((lisfranc∗ OR tarsometatars∗ OR “tars∗ metatars∗" OR midfoot) ADJ3 (fracture∗ OR dislocat∗ OR injur∗ OR trauma∗)).mp.
-
2
Metatarsal Bones/in
-
3
Metatarsus/in
-
4
Tarsal Joints/in
-
5
1 OR 2 OR 3 OR 4
-
6
bridg∗.mp.
-
7
plate∗.mp.
-
8
plating.mp.
-
9
Bone Plates/
-
10
6 OR 7 OR 8 OR 9
-
11
5 AND 10
References
- 1.Watson T.S., Shurnas P.S., Denker J. Treatment of lisfranc joint injury: current concepts. J Am Acad Orthop Surg. 2010;18(12):718–728. doi: 10.5435/00124635-201012000-00002. [DOI] [PubMed] [Google Scholar]
- 2.Saft S.H., RV Franciosi F.C.J. Fracture-dislocation of the tarsometatarsal joints: a case report. J Am Podiatr Med Assoc. 1981;71(3):162–165. doi: 10.7547/87507315-71-3-162. [DOI] [PubMed] [Google Scholar]
- 3.Chiodo C.P., Myerson M.S. Developments and advances in the diagnosis and treatment of injuries to the tarsometatarsal joint. Orthop Clin N Am. 2001;32(1):11–20. doi: 10.1016/s0030-5898(05)70190-5. [DOI] [PubMed] [Google Scholar]
- 4.Arntz C.T., Veith R.G., Hansen S.T. Fractures and fracture-dislocations of the tarsometatarsal joint. J Bone Jt Surg - Ser A. 1988;70(2):173–181. [PubMed] [Google Scholar]
- 5.Kuo R.S., Tejwani N.C., Digiovanni C.W. Outcome after open reduction and internal fixation of Lisfranc joint injuries. J Bone Jt Surg - Ser A. 2000;82(11):1609–1618. doi: 10.2106/00004623-200011000-00015. [DOI] [PubMed] [Google Scholar]
- 6.Alberta F.G., Aronow M.S., Barrero M. Ligamentous Lisfranc joint injuries: a biomechanical comparison of dorsal plate and transarticular screw fixation. Foot Ankle Int. 2005;26(6):462–473. doi: 10.1177/107110070502600607. [DOI] [PubMed] [Google Scholar]
- 7.Cohen D.A., Parks B.G., Schon L.C. Screw fixation compared to H-locking plate fixation for first metatarsocuneiform arthrodesis: a biomechanical study. Foot Ankle Int. 2005;26(11):984–989. doi: 10.1177/107110070502601114. [DOI] [PubMed] [Google Scholar]
- 8.Marks R.M., Parks B.G., Schon L.C. Midfoot fusion technique for neuroarthropathic feet: biomechanical analysis and rationale. Foot Ankle Int. 1998;19(8):507–510. doi: 10.1177/107110079801900801. [DOI] [PubMed] [Google Scholar]
- 9.Frigg R. Locking compression plate (LCP). An osteosynthesis plate based on the dynamic compression plate and the point contact fixator (PC-fix) Injury. 2001;32(2):63–66. doi: 10.1016/s0020-1383(01)00127-9. [DOI] [PubMed] [Google Scholar]
- 10.Liberati A., Altman D.G., Tetzlaff J. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol. 2009;6(7) doi: 10.1016/j.jclinepi.2009.06.006. [DOI] [PubMed] [Google Scholar]
- 11.Hozo S.P., Djulbegovic B., Hozo I. Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol. 2005;20(5):13. doi: 10.1186/1471-2288-5-13. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Higgins J., Altman D. Cochrane Book Series; 2008. Assessing Risk of Bias in Included Studies. Cochrane Handbook for Systematic Reviews of Interventions. [Google Scholar]
- 13.Wells G., Shea B., O’Connell D. 2000. The Newcastle-Ottawa Scale (NOS) for Assessing the Quality of Nonrandomised Studies in Meta-Analyses. [Google Scholar]
- 14.Hu S.J., Chang S.M., Li X.H. Outcome comparison of Lisfranc injuries treated through dorsal plate fixation versus screw fixation. Acta Ortopédica Bras. 2014;22(6):315–320. doi: 10.1590/1413-78522014220600576. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.van Koperen P.J., de Jong V.M., Luitse J.S.K. Functional outcomes after temporary bridging with locking plates in lisfranc injuries. J Foot Ankle Surg. 2016;55(5):922–926. doi: 10.1053/j.jfas.2016.04.005. el al. [DOI] [PubMed] [Google Scholar]
- 16.Lau S., Guest C., Hall M. Functional outcomes post lisfranc injury - transarticular screws, dorsal bridge plating or combination treatment? J Orthop Trauma. 2017;31(8):447–452. doi: 10.1097/BOT.0000000000000848. [DOI] [PubMed] [Google Scholar]
- 17.Kirzner N., Zotov P., Goldbloom D. Dorsal bridge plating or transarticular screws for Lisfranc fracture dislocations. Bone Joint Lett J. 2018;100(4):468–474. doi: 10.1302/0301-620X.100B4.BJJ-2017-0899.R2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Schepers T., Oprel P.P., Van Lieshout E.M.M. Influence of approach and implant on reduction accuracy and stability in Lisfranc fracture-dislocation at the tarsometatarsal joint. Foot Ankle Int. 2013;34(5):705–710. doi: 10.1177/1071100712468581. [DOI] [PubMed] [Google Scholar]
- 19.Anderson J.G., Bohay D.R. Management of midfoot and metatarsal fractures in the osteopenic patient. Tech Foot Ankle Surg. 2006;5(4):230–238. [Google Scholar]
- 20.Thordarson D.B., Hurvitz G. PLA screw fixation of lisfranc injuries. Foot Ankle Int. 2002;23(11):1003–1007. doi: 10.1177/107110070202301106. [DOI] [PubMed] [Google Scholar]
- 21.Bilenki J. 2019. Midfix RCT – Does Dorsal Plating of Lisfranc Injuries Lead to Better MOxFQ Pain Scores at 1 Year Compared to Transarticular Screw Fixation? – A Prospective Randomized-Controlled Trial. International Clinical Trials Registry Platform. [Google Scholar]