Abstract
First described by Green in 1832, persistent sciatic artery (PSA) is a rare anomaly classified into 2 types, namely complete and incomplete. We report the case of bilateral PSAs diagnosed by computed tomography angiography (CTA) in a 45-year-old female who presented with a 2-week history of pain and numbness in the left lower limb. Specifically, the CTA showed an incomplete PSA of the right lower limb and a complete PSA of the left lower limb complicated by an aneurysm. Complications of PSA, including aneurysmal rupture, occlusive thrombosis, and distal embolization, are critical as they impose serious hazards to the viability of the lower limbs. Asymptomatic patients with PSA require close surveillance for early detection and proper management of PSA-related complications, as they are prone to early atheromatous degeneration and aneurysm formation.
Keywords: Persistent Sciatic Artery, Bilateral Persistent Sciatic Artery, Vascular Anomaly, Complications, Aneurysm
Introduction
Persistent sciatic artery (PSA) is a rare, but potentially serious vascular anomaly resulting from the lack of regression of an embryonic artery to the lower extremity [1]. The first report of PSA was published in The Lancet by Green in 1832 [2]. The incidence of PSA is estimated to range from 0.025% to 0.06% based on angiographic series; almost 30% of the cases were bilateral, 79% were complete, and gender predilection does not exist [1,3]. The majority of PSA cases are asymptomatic; however, symptoms develop when complications occur [4]. The most frequently reported complications are aneurysm, occlusion of the PSA, and stenosis, occurring in 48%, 9%, and 7% of cases, respectively [3]. Despite its rarity, it is critical for physicians to be mindful of the clinical presentation, diagnosis, and management of PSA. This is because PSA can develop serious complications, such as aneurysmal/atherosclerotic formation, distal thrombo-embolization, and limb-threatening ischemia [5,6].
We describe the case of a 45-year-old patient diagnosed with bilateral PSAs. Moreover, we review the literature about the diagnosis and management of PSA [7].
Case report
A 45-year-old female, otherwise healthy, presented to the emergency department with a 2-week history of left lower limb pain and numbness. Physical examination revealed mild swelling as well as weak femoral and popliteal pulses in the left lower limb. No tenderness, decreased sensation or discoloration were noted. All laboratory investigations were normal.
Computed tomography angiography (CTA), starting from the abdominal aorta to the feet, was performed using a multidetector Toshiba scanner (Aquilion One, Toshiba Medical Systems, Japan) with the following parameters: 120 KvP, 350 mA, 5 mm slice thickness, and 1.0 mm reconstruction. 3D volume-rendered images showed an abnormal artery continuous with the left internal iliac artery. Following its path, this abnormal artery entered the gluteal region, descended downward and joined the popliteal artery at the popliteal fossa (Fig. 1). It was associated with saccular outpouching seen posteriorly at the level of the left femoral head (Fig. 1, 2). The saccular outpouching measured 2.5 × 1.8 cm in its transverse and anteroposterior diameters. The final radiological findings were consistent with a complete PSA, complicated by aneurysmal formation.
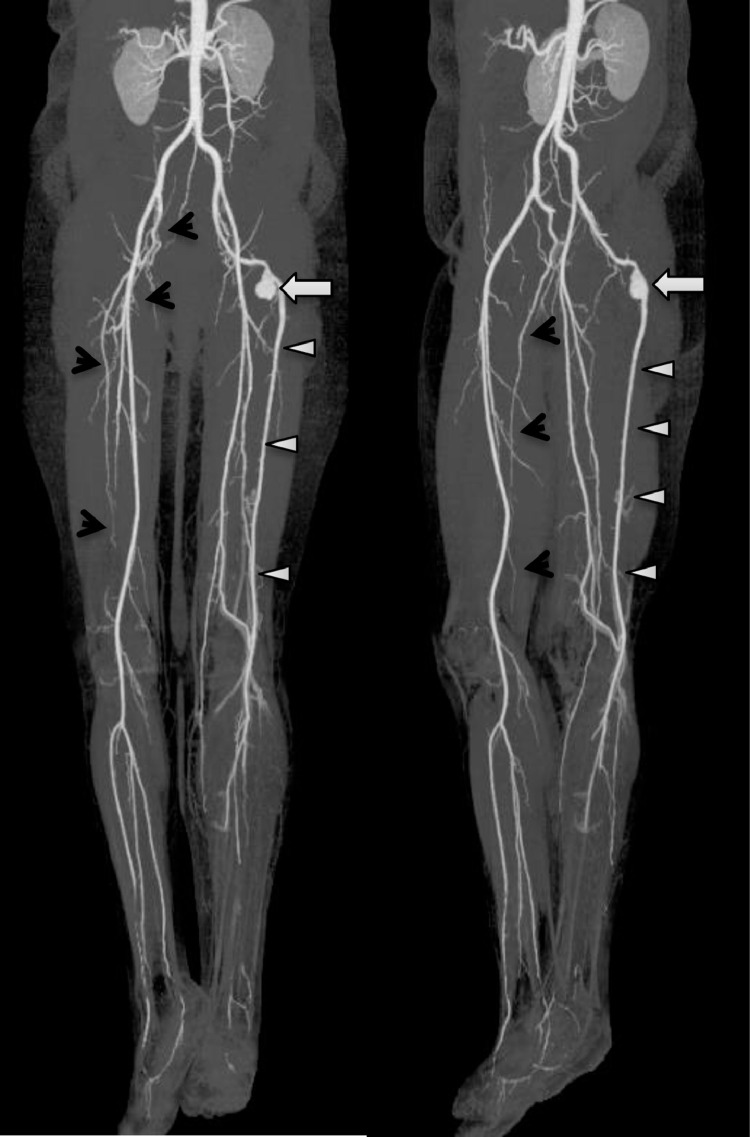
Fig. 1.
Digital subtraction angiography of the lower limbs. Axial coronal and oblique reformatted images showing the left complete persistent sciatic artery (PSA, arrow head) running into the posterior thigh and joining the popliteal artery. The PSA is complicated by a saccular aneurysm (arrow).The right incomplete PSA terminates just above the popliteal fossa with no communication (black short arrow).
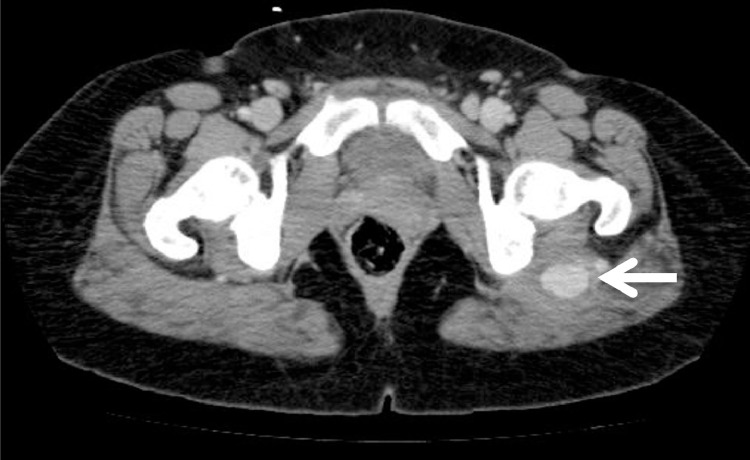
Fig. 2.
Computed tomography angiography. An axial scan of the gluteal region showing a saccular dilatation (aneurysm) of the left persistent sciatic artery (white arrow).
Although this vascular abnormality has led to the patient's chief presenting complaint, the CTA also showed a right-sided persistent posterior circulation in the thigh which terminated just above the popliteal fossa without communication to the popliteal artery. The radiological findings were consistent with an incomplete PSA (Fig. 1). The right and left femoral arteries were well-opacified and small in caliber. On the other hand, the anterior and posterior tibial arteries, as well as the peroneal arteries, were well-opacified with normal anatomy and course. The patient was admitted for embolization; however, the patient asked to be discharged against medical advice.
Discussion
The sciatic artery is an embryonic vascular structure. It originates from the continuation of the internal iliac artery and develops as the dorsal root of the umbilical artery to supply the lower limb [8,9]. During normal embryonic development, the femoral artery develops when the sciatic artery regresses between the 22-25 mm embryonic stage [9]. If this process fails to take place, the elastic components of the primitive arterial wall remain hypoplastic. PSA is particularly prone to undergo aneurysm formation, atherosclerosis, distal thrombo-embolization, and rupture. Thus, it poses substantial risks to the viability of the lower extremity [1,4,8,10]. These risks are exaggerated in patients undergoing hip replacement or renal transplantation procedures. If this anomaly is present in the recipient internal iliac artery, division of the PSA during renal artery anastomosis can lead to limb ischemia [1,3].
PSA is classified into 2 types based on the relationship between the sciatic artery and femoral artery; complete and incomplete PSAs [4,11]. In the vast majority of cases, the PSA is complete; there is no discontinuation in its vascular course from the internal iliac to the popliteal artery [1]. Thus, the complete PSA represents the dominant blood supply for the lower limb, whereas the superficial femoral artery is hypoplastic and provides only collateral vessels to the lower limb [1,4]. In such cases, the superficial femoral artery, rather than the PSA, is the main blood supply for the lower limb [1,4]. PSA can present unilaterally or bilaterally, with approximately 30% of cases being bilateral [3].
The Pillet classification of 1980, further modified by Gauffre in 1994, integrates the aforementioned PSA variations into a classification system of five types [12,13]. Additionally, a more recent classification of PSA was proposed by Ahn et al in 2016 [14]. This new classification not only accounts for concomitant incomplete persistent sciatic and superficial femoral arteries (classes I-IV), but also takes note of the presence of aneurysms (Table 1). Hence, it has a crucial rule in selecting an appropriate management option [14]. And our case is classified as class Ia, indicating having both complete superficial femoral artery and complete PSA that is associated with an aneurysm.
Table 1.
Ahn-Min's classification of persistent sciatic artery (PSA).
| Class | SFA | PSA | Aneurysm | Pillet-Gauffre classification | |
|---|---|---|---|---|---|
| (ScPc) | Class I | Complete | Complete | − | Type 1, 5a |
| Class Ia | + | ||||
| (ScPi) | Class II | Complete | Incomplete | − | Type 3, 4 |
| Class IIa | + | ||||
| (SiPc) | Class III | Incomplete | Complete | − | Type 2a, 2b, 5b |
| Class IIIa | + | ||||
| (SiPi) | Class IV | Incomplete | Incomplete | − | None |
| Class IVa | + | ||||
PSA: persistent sciatic artery; SFA: superficial femoral artery; ScPi: complete superficial femoral artery and incomplete persistent sciatic artery; ScPc: complete superficial femoral artery and complete persistent sciatic artery; SiPc: incomplete superficial femoral artery and complete persistent sciatic artery; SiPi: incomplete superficial femoral artery and incomplete persistent sciatic artery.
“a” indicates accompanying PSA
The clinical diagnosis of PSA is largely incidental [4,15]. It is usually identified during arteriography indicated for other causes or suspected in cases of pulsatile gluteal masses. It may also present with neurological signs and symptoms of a sciatic compression due to a dilated aneurysm [1,8]. Also, in rare cases whereby the patent sciatic artery occludes both the external iliac and femoral arteries, PSA can produce a pathognomonic clinical sign (Cowie's sign) characterized by an absent femoral pulse associated with palpable popliteal and/or pedal pulses [16].
Radiological investigations are beneficial in identifying, classifying and selecting the best treatment option. Noninvasive procedures such as Doppler ultrasound (US), CTA, and magnetic resonance angiography (MRA) represent useful tools for diagnosis [4,17]. Doppler US is the first line, noninvasive diagnostic modality used to confirm the presence of PSA [4,17,18]. CTA and MRA are superior to Doppler US in various aspects, including the assessment of the whole course and bilateral peripheral circulation, PSA classification, and evaluation of potential coexisting complications [1,18,19]. Additionally, MRA can provide valuable information about the relation between the sciatic artery and sciatic nerve. Although conventional angiography is considered the gold standard for PSA diagnosis, it has a disadvantage of giving false impressions of occluded distal circulation (namely popliteal and tibial vasculature). This may be ascribed to the slow flow in the dilated arteries or the failure to place the catheter tip proximal to the internal iliac orifice [17], [18], [19], [20].
Management of PSA depends on the clinical presentation of the patient, type of PSA, and radiological findings. Management may vary from a simple “watch and wait” approach, to various surgical procedures, such as bypass, other revascularization techniques or major/minor amputation. If the patient is diagnosed incidentally with no complications, then routine follow-up is recommended [4]. On the other hand, if an aneurysm or vascular occlusive disease is present, the appropriate treatment will be either surgical or endovascular. Generally, there are 4 methods to obliterate PSA aneurysms: ligation, resection, embolization, or endovascular stent grafting [18,20]. Aneurysm embolization using push-able coils has been reported to be successful, although undesirable due to the discomfort it causes [3,19,20]. In cases of vascular occlusion, vascular reconstruction can be achieved in three methods. These include performing the standard femoral-popliteal bypass (if the common femoral artery is sufficiently developed to provide adequate inflow), ilio-popliteal trans-obturator bypass, or interposition bypass [18,21]. Additionally, in cases of thrombosis and extensive distal arterial embolization, intra-arterial thrombolytic therapy may be beneficial prior to definitive surgical revascularization [22].
PSA is a rare vascular anomaly with many variations. It is best assessed by CTA to delineate its course and rule out complications. Asymptomatic patients with PSA require close surveillance for early detection and prompt management of PSA-related complications, such as aneurysm formation or vascular occlusion. Conversely, symptomatic patients with complications should be carefully evaluated by angiography to reduce the hazard of adverse events that may arise during surgical or interventional manipulations.
Acknowledgments
Role of the funding source
Non applicable.
Consent for publication
Consent for publication of the manuscript and the related patient information has been obtained.
Ethical approval and consent to participate
Case reports are exempted from ethical approval according to policies of our hospital (King Fahad University Hospital). Maximum effort was made to keep the identity of our patient private. The figures do not display any indentifying information.
Footnotes
Authors contributions: Aljawhara Alsaadoun wrote the original manuscript. Radiology image reporting was performed and interpreted by Eman A. Almomen, and Obaid M. Aldhafeeri. The revision of the final manuscript was performed by Wafa F. Al-Dhafeeri. All authors read and approved the final manuscript.
Competing Interests: None.
Acknowledgments: None.
Funding: This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
References
- 1.Mayschak DT, Flye MW. Treatment of the persistent sciatic artery. Ann Surg. 1984;199(January (1)):69–74. doi: 10.1097/00000658-198401000-00012. http://www.ncbi.nlm.nih.gov/pubmed/6691734 [cited 2019 Sep 6]Available from: [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.GREEN, PH.On a new variety of femoral artery. Lancet. 1832 [cited 2019 Sep 6];1:730–1. Available from:https://ci.nii.ac.jp/naid/10026515451/
- 3.van Hooft IM, Zeebregts CJ, van Sterkenburg SMM, de Vries WR, Reijnen MMPJ. The persistent sciatic artery [Internet]. Vol. 37. Eur J Vascul Endovasc Surg. 2009:585–591. doi: 10.1016/j.ejvs.2009.01.014. http://www.ncbi.nlm.nih.gov/pubmed/19231248 [cited 2019 Sep 6]Available from: [DOI] [PubMed] [Google Scholar]
- 4.Cavallo Marincola B, Napoli A, Anzidei M, Marotta E, Boni F, Cartocci G. Persistence of the sciatic artery: a case report of a combined (complete and incomplete) type causing leg ischemia. Case Rep Vasc Med. 2012;2012:1–5. doi: 10.1155/2012/196798. http://www.ncbi.nlm.nih.gov/pubmed/22973532 [cited 2019 Sep 6]Available from: [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Tanaka M, Okamoto M, Okamoto K, Fukui T. A case of persistent sciatic artery aneurysm with recurrent embolism. Int J Surg Case Rep. 2019;60(January):156–160. doi: 10.1016/j.ijscr.2019.06.017. https://www.sciencedirect.com/science/article/pii/S2210261219303281 [cited 2019 Sep 12]Available from: [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Shehzad KN, Monib S, Mensa M, Halawa MO. Bilateral persistent sciatic arteries complicated by unilateral acute lower limb ischaemia. J Surg Case Rep. 2019;2019(April (4)) doi: 10.1093/jscr/rjz119. https://academic.oup.com/jscr/article/doi/10.1093/jscr/rjz119/5477446 [cited 2019 Sep 12]Available from: [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Agha RA, Fowler AJ, Saeta A, Barai I, Rajmohan S, Orgill DP. The SCARE statement: consensus-based surgical case report guidelines. Int J Surg. 2016;34(October):180–186. doi: 10.1016/j.ijsu.2016.08.014. http://www.ncbi.nlm.nih.gov/pubmed/27613565 [cited 2019 Sep 12]Available from: [DOI] [PubMed] [Google Scholar]
- 8.Freeman MP, Tisnado J, Cho SR. Persistent sciatic artery. Report of three cases and literature review. Brit J Radiol. 1986;59:217–223. doi: 10.1259/0007-1285-59-699-217. http://www.ncbi.nlm.nih.gov/pubmed/3512010 [cited 2019 Sep 6]Available from: [DOI] [PubMed] [Google Scholar]
- 9.Paraskevas G, Papaziogas B, Gigis J, Mylonas A, Gigis P. The persistence of the sciatic artery. Folia Morphol (Warsz) 2004;63(4):515–518. https://www.semanticscholar.org/paper/The-persistence-of-the-sciatic-artery.-Paraskevas-Papaziogas/b690a34596a9c014920c2601083602fc51d223fc [cited 2019 Sep 6]Available from: [PubMed] [Google Scholar]
- 10.Brantley SK, Rigdon EE, Raju S. Persistent sciatic artery: embryology, pathology, and treatment. J Vasc Surg. 1993;18(August (2)):242–248. http://www.ncbi.nlm.nih.gov/pubmed/8350433 [cited 2019 Sep 6]Available from: [PubMed] [Google Scholar]
- 11.Bower EB, Smullens SN, Parke WW. Clinical aspects of persistent sciatic artery: report of two cases and review of the literature. Surgery. 1977;81(May (5)):588–595. http://www.ncbi.nlm.nih.gov/pubmed/850875 [cited 2019 Sep 6]Available from: [PubMed] [Google Scholar]
- 12.Gauffre S, Lasjaunias P, Zerah M. Sciatic artery: a case, review of literature and attempt of systemization. Surg Radiol Anat. 1994;16(1):105–109. doi: 10.1007/BF01627932. http://www.ncbi.nlm.nih.gov/pubmed/8047957 [cited 2019 Sep 6]Available from: [DOI] [PubMed] [Google Scholar]
- 13.Pillet J, Albaret P, Toulemonde JL, Cronier P, Raimbeau G, Chevalier JM. Ischio-popliteal artery trunk, persistence of the axial artery. Bull Assoc Anat (Nancy) 1980;64(March (184)):97–110. http://www.ncbi.nlm.nih.gov/pubmed/7459444 [cited 2019 Sep 6]Available from: [PubMed] [Google Scholar]
- 14.Ahn S, Min S-K, Min S-I, Ha J, Jung IM, Kim SJ. Treatment strategy for persistent sciatic artery and novel classification reflecting anatomic status. Eur J Vasc Endovasc Surg. 2016;52(September (3)):360–369. doi: 10.1016/j.ejvs.2016.05.007. http://www.ncbi.nlm.nih.gov/pubmed/27369291 [cited 2019 Sep 6]Available from: [DOI] [PubMed] [Google Scholar]
- 15.Papon X, Picquet J, Fournier HD, Enon B, Mercier P. Persistent sciatic artery: report of an original aneurysm-associated case. Surg Radiol Anat. 1999;21(2):151–153. doi: 10.1007/s00276-999-0151-5. http://www.ncbi.nlm.nih.gov/pubmed/10399218 [cited 2019 Sep 6]Available from: [DOI] [PubMed] [Google Scholar]
- 16.Brancaccio G, Falco E, Pera M, Celoria G, Stefanini T, Puccianti F. Symptomatic persistent sciatic artery. J Am Coll Surg. 2004;198(January (1)):158. doi: 10.1016/j.jamcollsurg.2003.06.008. https://linkinghub.elsevier.com/retrieve/pii/S1072751503010627 [cited 2019 Sep 6]Available from: [DOI] [PubMed] [Google Scholar]
- 17.Williams LR, Flanigan DP, O'Connor RJA, Schuler JJ. Persistent sciatic artery. Am J Surg. 1983;145(May (5)):687–693. doi: 10.1016/0002-9610(83)90122-8. http://www.ncbi.nlm.nih.gov/pubmed/6846710 [cited 2019 Sep 6]Available from: [DOI] [PubMed] [Google Scholar]
- 18.Wang B, Liu Z, Shen L. Bilateral persistent sciatic arteries complicated with chronic lower limb ischemia. Int J Surg Case Rep. 2011;2(8):309–312. doi: 10.1016/j.ijscr.2011.07.010. http://www.ncbi.nlm.nih.gov/pubmed/22096762 [cited 2019 Sep 6]Available from: [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Sindel T, Yilmaz S, Onur R, Sindel M. Persistent sciatic artery. Radiologic features and patient management. Saudi Med J. 2006;27(May (5)):721–724. http://www.ncbi.nlm.nih.gov/pubmed/16680268 [cited 2019 Sep 6]Available from: [PubMed] [Google Scholar]
- 20.McEnaney RM, Baril DT, Gupta N, Marone LK, Makaroun MS, Chaer RA. Persistent sciatic artery aneurysm treated with concomitant tibial bypass and vascular plug embolization. J Vasc Surg. 2009;50(October (4)):915–918. doi: 10.1016/j.jvs.2009.04.072. https://linkinghub.elsevier.com/retrieve/pii/S0741521409010209 [cited 2019 Sep 6]Available from: [DOI] [PubMed] [Google Scholar]
- 21.Dehiyan A, Singla RK, Sharma RK, Agnihotri G. Persistent sciatic artery. Int J Med Dent Sci. 2014;3(January (1)):352. http://www.informaticsjournals.com/index.php/ijmds/article/view/19416 [cited 2019 Sep 6]Available from: [Google Scholar]
- 22.Ahmad W, Majd P, Luebke T, Gawenda M, Brunkwall JS. Clinical outcome after surgical and endovascular treatment of symptomatic persistent sciatic artery with review of the literature and reporting of three cases. Vascular. 2016;24(October (5)):469–480. doi: 10.1177/1708538115611791. http://journals.sagepub.com/doi/10.1177/1708538115611791 [cited 2019 Sep 6]Available from: [DOI] [PubMed] [Google Scholar]