Abstract
Purpose
Total knee arthroplasty (TKA) rates have increased substantially in the recent decades worldwide, with Germany being one of the leading countries in the prevalence of TKA. The aim of this study was to provide an overview of treatment changes during the last decade and to project the expected burden of primary and revision TKA (rTKA) for the next 30 years.
Methods
Comprehensive nationwide data from Germany was used to quantify primary and revision TKA rates as a function of age and gender. Projections were performed with use of a Poisson regression models and a combination of exponential smoothing and autoregressive integrated moving average models on historical procedure rates in relation to official population projections from 2020 to 2050.
Results
The incidence rate of primary TKAs is projected to increase by around 43% to 299 per 100,000 inhabitants [95% CI 231–368], leading to a projected total number of 225,957 primary TKAs in 2050 (95% CI 178,804–276,442). This increase has been related to a growing number of TKA performed in male patients, with the highest increase modelled in patients between 50 and 65 years of age.
At the same time, the annual total number of revision procedures is forecast to increase even more rapidly by almost 90%, accounting for 47,313 (95% CI 15,741–78,885; IR = 62.7 per 100,000, 95% CI 20.8–104.5) procedures by 2050. Those numbers are primarily associated with a rising number of rTKAs secondary to periprosthetic joint infection (PJI).
Conclusions
Using this country- specific forecast approach, a rising number of primary TKA and an even more rapidly growing number of rTKA, especially for PJI, has been projected until 2050, which will inevitably provide a huge challenge for the future health care system. As many other industrialized nations will face similar demographic and procedure-specific developments, these forecasts should be alarming for many health care systems worldwide and emphasize the tremendous need for an appropriate financial and human resource management in the future.
Level of evidence
Level III, prognostic study, economic and decision analysis.
Keywords: Arthroplasty, Total knee replacement, Revision knee arthroplasty, Projection model, Germany
Introduction
Over the last decades total knee arthroplasty (TKA) has been widely established as a highly successful treatment for advanced osteoarthritis of the knee in terms of pain relief and improvements in function and health-related quality of life [5, 17, 28, 41]. Based on these experiences and supported by constant advancements in long-term patient-oriented outcomes [7, 15, 16], this has led to an increasing number of surgeons offering total knee arthroplasty to younger and higher-demanding patients more frequently nowadays. Although perioperative mortality rates remain low (∼0.5%), about 3–5% of all TKA fail each year due to septic or aseptic loosening or component failure [33]. This is of particular concern as the financial and economic impact of revision knee arthroplasty is substantially greater compared with primary TKA [1, 8], due to longer times of surgery, more expensive prostheses, longer length of stay and higher rates of complications [42]. In this context, revisions due to periprosthetic joint infection (PJI) are one of the most severe complications after arthroplasty that affect the quality of a patient's life and also place the highest (financial) burden on the health care system [29, 30].
Prior studies from countries all over the world [40, 47, 49, 52] have almost exclusively focused on the projections of the future demand of primary TKA and reported a further rise in the near future, mainly driven by a constantly aging population and an increase of unfavorable risk factors, including obesity and osteoarthritis [11]. However, studies providing an outlook on the future burden revision knee arthroplasty are almost completely missing. Based on the rising number of primary TKA, it was hypothesized that the volume of revision procedures, especially due to PJI, will rapidly increase in the future, which will place an immense burden on future health care systems and also raises the question, if current clinical standards and treatment strategies have to be reconsidered.
Methods
An analysis of data from the national inpatient statistics of Germany was conducted. This database includes all annual inpatient treatment reports from all German hospitals and medical institutions, making this study a nationwide survey (except military and psychiatric facilities). The data is based on the International Statistical Classification of Diseases and Related Health Problems, Tenth Edition (ICD-10) and the German procedure classification system (OPS), which is the official classification system for encoding surgical procedures in Germany. These statistics contain anonymized data from the Federal Bureau of Statistics, sustaining plausibility checks, and data validation on a medical and economic level. All cases reported between 2005 and 2018 were analyzed based on the corresponding OPS codes in its most recent version [6]. All patients with knee arthroplasty, including either bicondylar or unicompartmental arthroplasty and all revision knee arthroplasties and explantations, were identified, although data regarding different types of primary arthroplasties were not available prior to 2008. Age was categorized in the following groups: < 50, 50–55, 55–59, 60–64, 65–69, 70–74, 75–79, 80–84, and older than 85 years.
Population data was available from official population projection statistics until 2050 [45]. These population projections consider the future mortality and increased life expectancy for the oldest population groups, and the immigration rate.
Data from 2005 to 2018 (baseline years) and population forecasts up to the year 2050 were then used to project the annual incidence of primary and revision arthroplasty in Germany. A linear (Poisson, “classic approach”) regression analysis was performed to estimate the expected incidence with calendar year, sex, and patient age as covariates, as recently reported by Schwartz et al. [50]. The incidence was calculated by dividing the estimated number of arthroplasties for the national total and for each age subgroup by the corresponding official population forecast. Expected mean incidence was adjusted for population size using the age-specific logged population numbers as off-set. To overcome overdispersion problems that could result in an underestimation of variance, a robust sandwich covariance matrix estimator for variance calculation was used. To minimize the error of variance underestimation of the estimated parameter because of overdispersion, a quasi-Poisson regression to the data in accordance with the theory of quasi-likelihood was applied.
Due to the fact, that Poisson regression can theoretically provide exponential growth to infinity, some authors have tried alternative estimation models of future projections, e.g., using asymptotic or logarithmic regressions [40, 47]. These models seem to be more economic-logically than knowledge-driven, as regressions based on logarithm or an exponent will only fit optimally, if this is the exact nature of the true relationship. To overcome this issue, time series forecasting has become more and more popular in recent years, especially in the context of economic issues. Exponential smoothing and autoregressive integrated moving average (ARIMA) models are the two most widely used approaches [18, 39], and provide complementary approaches to the problem. While exponential smoothing models are based on a description of the trend and seasonality in the data and weigh averages of past observations, with the weights decaying exponentially as the observations get older, ARIMA models aim to describe the autocorrelation in the data. In both cases, future values are constrained to be linear functions of past observations. In this study, a grouped time series analysis for modelling time effects and accounting for respective gender and age groups was used. These models contained a combination of ARIMA and exponential smoothening models (ETS) as introduced by Hyndman et al. [13]. Based on the stepwise Hyndman–Khandakar algorithm, the best model was selected using a combination of Kwiatkowski–Phillips–Schmidt–Shin (KPSS) unit root test, minimization of the Akaike’s Information Criterion for small samples (cAIC) [3] and maximum likelihood method algorithm. After forecasting [14], the prediction accuracy of each model was verified by splitting the dataset into training (years 2005–2015) and testing subsets (years 2016–2018) and comparing the mean absolute percentage error (MAPE) of the prediction, which was defined as follows:
where XI denotes the observed ED visits at month I, and denotes the predicted ED visits at year I. The MAPE is a percentage error that measures the relative difference between the actual and forecast values of a given model. The lower the MAPE, the more accurate is the model’s forecast. Based on the validation dataset, the Poisson model for primary TKA and the ARIMA model for revision TKA appeared to fit the historical data best, although all models did not show highly significant differences (Table 1). Therefore, this investigation ultimately opted for a data-driven model-averaging strategy (by minimizing model errors) that considers all models, which has been considered the golden standard in the economic literature, assuming that a combination of forecasts will surpass individual forecasts [38].
Table 1.
Accuracy of the different prediction models used in this study
| Type | Model | RMSE | MAPE |
|---|---|---|---|
| TKA | arima | 581.24 | 2.52% |
| ets | 744.87 | 3.54% | |
| poisson | 324.75 | 1.77% | |
| rev TKA | arima | 61.09 | 2.00% |
| ets | 131.34 | 3.95% | |
| poisson | 236.27 | 11.17% |
RMSE root mean squared error, MAPE mean absolute percentage error
Because of the anonymization of the diagnosis-related group DRG data, arthroplasty patients who underwent a revision (replacement or explantation) could not be individually followed, and therefore, actual revision rates could not be calculated. Instead, the revision burden (RB) was estimated by dividing the number of revisions in the form of replacements or extractions by the number of all primary and revision arthroplasties, which is a concept previously introduced by Malchau et al. [36]
All statistical analyses were performed using R Version 3.6.3 (R Development Core Team, The R Foundation for Statistical Computing, Vienna, Austria).
Results
From 2005 to 2018 a total of 2,151,448 primary TKAs were recorded in Germany. During that time, the annual number of procedures rose from 128,932 in 2005 to 170,494 in 2018, representing an increase of 32.4%. Respecting the population growth, the annual overall incidence changed substantially from 157 per 100,000 to 209 per 100,000 inhabitants (P < 0.001). Overall, almost two third of all TKA were performed in women, although the proportion of male patients rose steadily from 31.0% (2005) to 38.5% (2018). 41% of all TKAs were performed in patients between 70 and 80 years of age, with a substantial increase in younger patients during the course of the study.
Regarding different types of implants, a significant increase in utilization of unicompartmental knee arthroplasty (UKA) (5.6% → 10.7%) has been reported, particularly in younger (55–65 years), male patients (48%).
During the same period, 326,019 revision procedures were performed, with a significant increase in the annual total number and incidence (19.6 per 100,000 inhabitants in 2005 and 30.8 per 100,000 in 2018) over time (P < 0.01). Most revisions were performed in female patients aged 75 years and older (~ 67.1%). Gender ratio was almost even in younger patients.
In this context, revision burden (~ 10%) for TKA showed no significant change during the study period despite a rise in total number. At the same period, however, the number of revisions for UKA significantly increased about 42.6%. However, due to a simultaneously higher increase in primary unicompartmental procedures, the revision burden for these implants has also decreased (22.0 → 13.7%).
Most common indications for rTKA were mechanical complications (~ 55%), like aseptic loosening, prosthetic joint infection (PJI) (~ 21%) and fracture (~ 2–3%). Male patients had a substantially higher relative revision burden (RR = 1.6) for PJI, whereas the RR for periprosthetic fracture was higher in women (RR = 2.2). Although mechanical complications have remained the most common indications for revision at every time point of the study, there was little change in total number during the study period. In contrast, both an increase in PJI (+ 47.6%) and periprosthetic fractures (+ 320.1%) was documented.
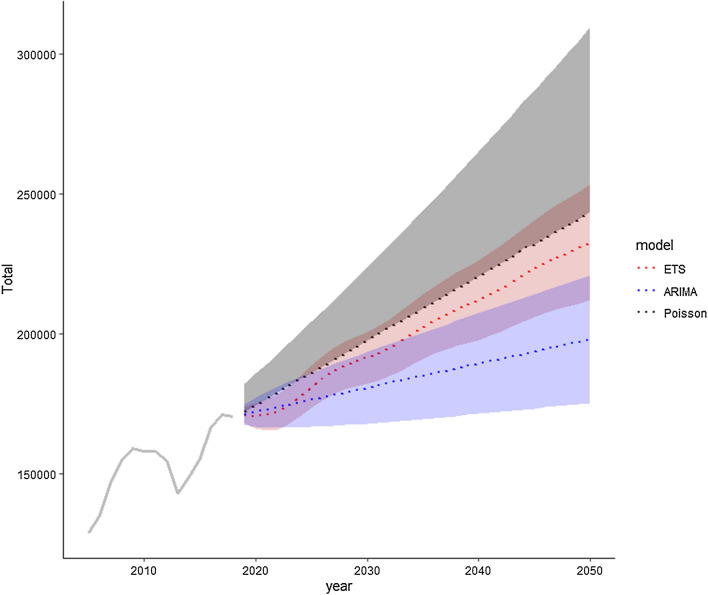
Based on the projection models used, an average increase of 43% in the incidence rate of primary TKAs to 299 per 100,000 inhabitants [95% CI 231–368] is projected, leading to a mean projected total number of 225.957 primary TKAs in 2050 (95% CI 178,804–276,442) (Figs. 1 and 2). This increase has been mainly related to a growing number of TKA performed in male patients, with the highest increase modelled in patients between 50 and 65 years of age, whose numbers more than tripled until 2050 (Fig. 3a, b].
Fig. 1.
Projected total number of TKA until 2050 depending on the model used (confidence intervals in shades)
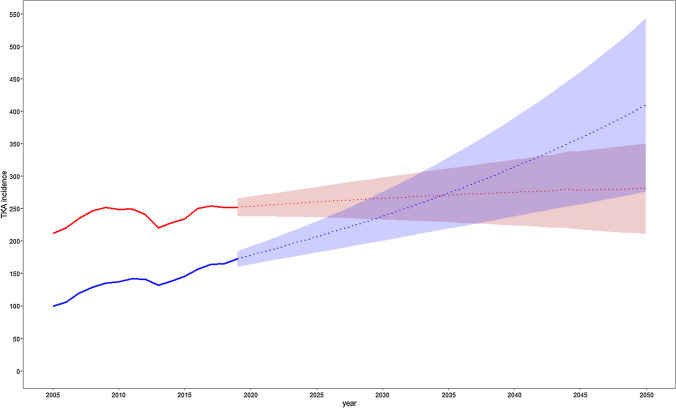
Fig. 2.
Projected incidence rate of TKA for men (blue) and women (red) until 2050 (per 100,000 inhabitants, Poisson modelling)
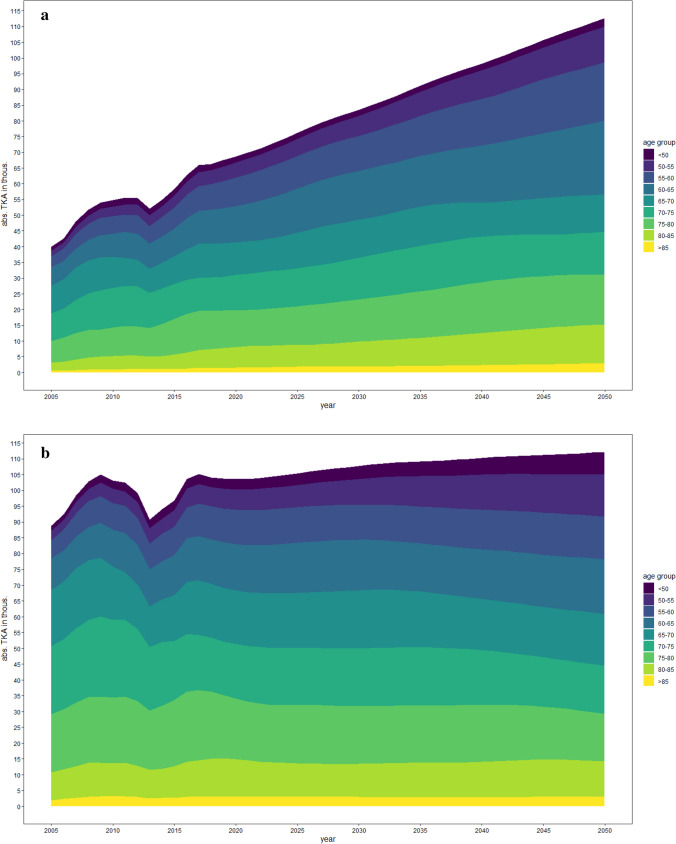
Fig. 3.
Projected total number of TKA (in thousands) for men (a) and women (b) per age age group until 2050
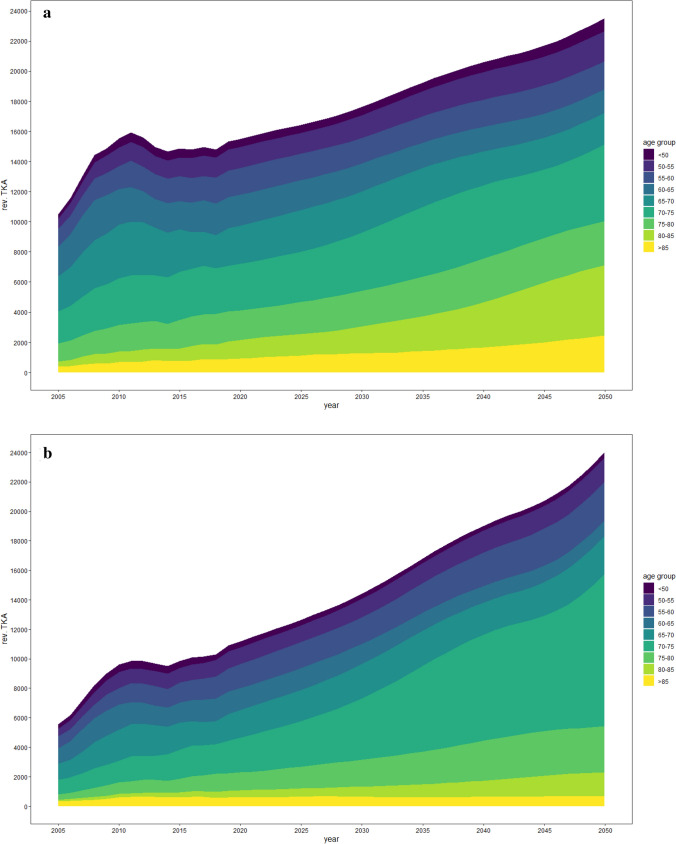
With the number of primary TKAs rising, an enormous increase in the total number of revision procedures by an average of 88% is also projected, accounting for 47,313 per year (95% CI 15,741–78,885; IR = 62.7 per 100,000, 95% CI 20.8–104.5) procedures by 2050 (Fig. 4). Although this increase can be mainly attributed to a rising number in patients 70 years and older, younger patients (aged 55–64) showed a significant upward trend in revision procedures during the study period, as well (Fig. 5a, b).
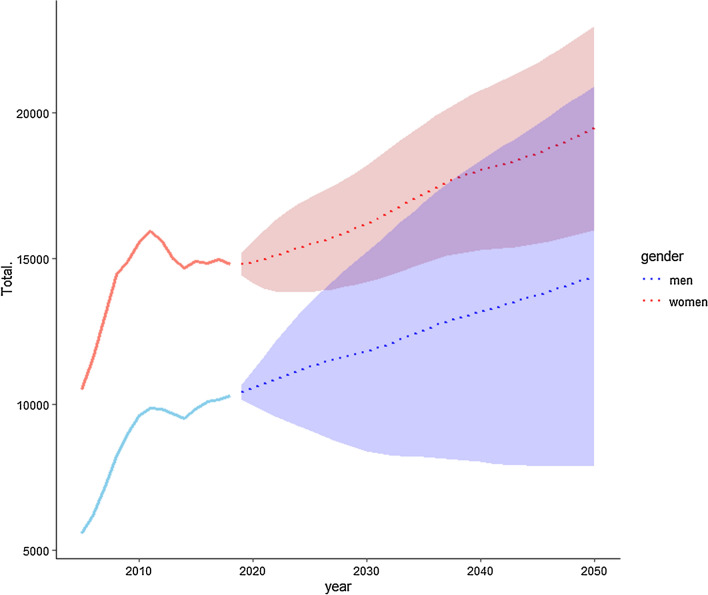
Fig. 4.
Projected total number of revision TKA for men (blue) and women (red) until 2050 (per 100,000 inhabitants, ARIMA modelling)
Fig. 5.
Projected total number of revision TKA (in thousands) for women (a) and men (b) per age age group until 2050
These trends have been mainly associated with a rising number of rTKAs secondary to PJI (Fig. 6) and periprosthetic fracture, while revisions due to mechanical complications, such as aseptic loosening, only showed little change over time.
Fig. 6.
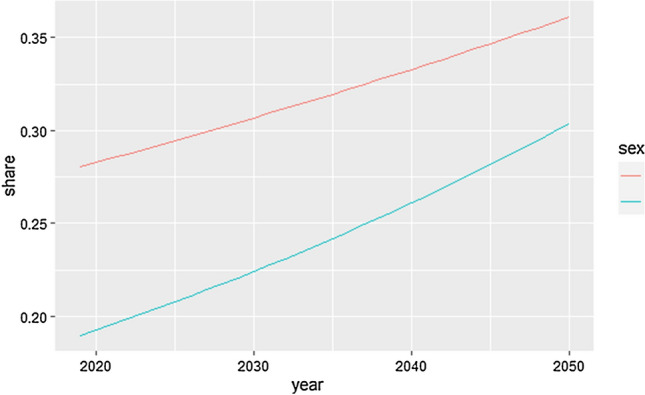
Projections of the proportional share of periprosthetic joint infections (PJI) for men (blue) and women (red) until 2050
Discussion
Based on the present analysis, the most important findings of this study were the substantial increase in incidence of primary TKA and an even higher rise in revision TKA over the next three decades, which will inevitable place an immense burden on the future health care system. It also draws attention to the important problem of rapidly growing rates of PJI and its associated challenges, which will certainly affect the clinical care. In combination with an expected population decline due to further aging and lower birth rates in the upcoming decades, this raises the question, if an already financially strained healthcare system will be able to cover this demand in the future [44]. At the same time, it emphasizes the need for qualified surgeons and for future research to improve the reliability and survivorship of TKA [28, 31].
Just recently, Rupp et al. published their projections of primary TKA and total hip arthroplasty in Germany from 2016 through 2040 based on the same database. Using a Poisson approach with general health expenditures as additional covariate, they projected the total number of TKAs to rise by 45% until 2040, with the greatest increase being predicted to occur in patients aged 40–49 years (269%) [48]. These findings are strongly supported by the projections of the present investigation, with an average increase of 43% of primary TKA between 2018 and 2050. Similar trends and rates have also been reported for other European countries [5, 40, 47]. For the U.S. an even higher increase has been projected (+ 673% between 2005 and 2030) [28]. However, different population structures and methodologies may be responsible for observed differences and also other nondemographic factors (e.g., access and reimbursement costs) have to be considered, when discussing potential differences in use. In Germany, unrestricted access to all official medical treatment is guaranteed, which is certainly not the case for all countries. Still, a worldwide trend towards a higher future TKA volume is evident. In this context, a large part of the projected increase will be associated with a higher utilization of TKA in younger patients, indicating, that its potential benefits may have transferred to a higher operation volume over the last decades.
As indications further expand to a younger, more active population, revision rates have also been shown to markedly increase in those patients in recent investigations [37, 43]. This raises the fear of an uncontrolled further growth of these revision procedures in the future, if the rise in volume of TKA cannot be slowed down by new advancements (like prevention of or non-operative strategies for osteoarthritis) or, if survivorship of the implants cannot be sufficiently prolonged.
In this context, Schwartz et al. have recently tried to forecast the numbers of revision knee arthroplasty in the U.S., projecting the incidence of rTKA to increase between 78 and 182% by the year 2030 [50]. Patients aged between 55 and 74 showed the highest increase in revision incidence, whereas incidence in the 75–84 age group decreased. These findings can also be supported by the present study, as an 88% increase of rTKA has been projected by 2050, with a rising number of patients requiring revision surgery earlier in their lifetime. As the longevity of rTKAs is far inferior to primary TKA, a growing population of multiple-revised patients has to be expected in the future [22]. The combination of a considerably aging population and an increasingly younger rTKA population [24] is an alarming trend, especially considering the impairment many patients are suffering following (multiple) rTKA. According to a study from the UK 93% of all patients were still working before rTKA, while afterwards patients rarely (7%) return to work [51]. In addition to an already shrinking working population, due to the constantly aging population, this will inevitably add up to the already enormous economic challenge for healthcare and social systems [42].
Furthermore, a significant increase in utilization of UKA was observed, especially in young, male patients. Although usually good outcomes can be achieved [21, 23, 35], revision rates of UKA have been shown to be significantly higher compared to TKA [4, 10, 34]. If the current trend continues, this will probably result in an even further increase in the demand of revision surgeries in future decades.
Although perioperative mortality rates remain low (∼0.5%), about 3–5% of all TKA and up to 10% of UKA fail each year due to septic or aseptic loosening or component failure [25, 33]. However, many problems associated with TKA in the past, such as mechanical complications like implant breakage and wear, might have been successfully addressed over the years. This is supported by the presented results, as revision due to mechanical complications showed a decreasing incidence over the last decade. In contrast, the problems associated with PJI and periprosthetic fractures remain unsolved and will lead to an even greater challenge in the future, as their incidence is rising to worrisome rates [26, 32]. As the number of revisions secondary to PJI is increasing, its share is also projected to rise to over one third of all revision procedures by 2050, with male patients having the highest risk, as previously described [24, 27]. This is of utmost interest, as the clinical and economic burden of rTKA for PJI is eminent [19] and also provides a major risk for uncontrolled growth in cost for future generations [20].
Besides PJI, periprosthetic fractures have a similarly negative impact on cost and morbidity for the patient and the health care system [46, 50], albeit their incidence is way lower than PJI. Based on the tremendous rise in the incidence of periprosthetic fractures observed during the last decade, the future challenge of these complications is evident. For this reason, key strategies, such as prevention programs and the use of non-operative treatment options to delay primary TKA, if possible, should be a main focus of current research and healthcare providers [48]. Furthermore, stake-holders in the healthcare systems should be encouraged to provide additional capacity in geriatric treatment and care, to satisfy the requirements associated with the higher demand of rTKA in a more vulnerable patient cohort [2].
This study has several limitations, mainly due to the design of the database. First, the analysis and projections are mainly related to one country with a certain population structure and may, therefore, potentially vary for other countries. While Germany and others (such as Italy, Russia or most Eastern European countries) face working population declines in the near future due to lower birth and immigration rates, that are unable to make up for the aging of the population, the working population in other countries is still growing due to high immigration and fertility rates. However, most industrialized nations will face similar demographic and procedure-specific developments in the near future, which is why these forecasts should be alarming for many health care systems worldwide.
Secondly, the use of a database in general carries the inherent weaknesses of unverifiable accuracy of coding and data input. Furthermore, since the calculations were based on the historical growth of (revision) TKA numbers as well as the population projection of the Federal Bureau of Statistics of Germany, they might be biased from past trends that could change in the future.
Although the official forecast on population developments was included in the projections, this study could not take changes of lifestyle (such as increasing rates of obesity, and subsequent osteoarthritis) into account. This might directly affect the upcoming need for primary and revision knee arthroplasty surgery, as a higher BMI has been associated with a higher rate for revision [9]. Furthermore, index case complexity or pertinent comorbidities could not be included. At the same time, implant designs and materials may further improve, potentially being associated with a greater implant survival rate, which would inevitably affect the number of future revision procedures. Additionally, potential limitations in the availability of surgeons or the limited economic resources of private and public payers and hospitals, as well as changes in indication or access to medical care could not be taken into consideration. Therefore, these projections may be interpreted as a conservative estimation for the future socio-economic health community, if primary implant survival cannot be improved in the upcoming years.
Despite these limitations, this regression framework offers an economically acceptable model and its applicability in forecasting total joint replacement makes this study especially relevant to other countries with a high incidence and volume of TKA, particularly in view of current economic difficulties (due to COVID-19 [12, 53] or future pandemic).
It also raises the globally-important question, if societies will be able and willing to shoulder the additional burden associated with the growing number of these procedures, or, if it may happen, that new coping strategies will arise (e.g., restricting access to TKA for certain patients or even rationing them), to maintain cost coverage. This certainly holds the danger of restricting therapeutic freedom by government (cost-) control in the future. Ultimately, this study emphasizes the importance of critically assessing each patient´s need for knee arthroplasty by every single surgeon and maybe serves as a dynamo to reflect on possible alternative treatment options.
Conclusion
Using this country- specific forecast approach, a rising number of primary TKA and an even more rapidly growing number of rTKA, especially for periprosthetic joint infection, has been projected until 2050, which will inevitably provide a huge challenge for the future health care system. As many other industrialized nations will face similar demographic and procedure-specific developments, these forecasts should be alarming for many health care systems worldwide, and emphasize the tremendous need for an appropriate financial and human resource management in the future.
Acknowledgements
We thank Kristina Klug, MSc., Goethe-Universität Frankfurt Frankfurt am Main, Institut für Psychologie, for supporting the authors with the statistical analysis.
Author contributions
AK, Orthopedic Surgeon: Conception and design, Analysis and interpretation of data, Writing the manuscript, Statistical analysis. MW, Orthopedic Surgeon: Proofreading the manuscript, Statistical analysis, Data analysis, Critically revising the article. YG, Orthopaedic Surgeon: Proofreading the manuscript, Statistical analysis, Data analysis. PD, Professor, Orthopedic Surgeon: Proofreading the manuscript, Administrative/technical/material support. MR, Professor, Orthopedic Surgeon: Proofreading the manuscript, Administrative/technical/material support. RH, Professor, Orthopedic Surgeon: Proofreading the manuscript, Conception and design, Administrative/technical/material support. KK, Orthopedic Surgeon: Proofreading the manuscript, Literature review, Data analysis, Administrative/technical/material support.
Funding
There is no funding source.
Compliance with ethical standards
Conflict of interest
None of the authors, their immediate families, and any research foundation with which they are affiliated received any financial payments or other benefits from any commercial entity related to the subject of this article. Alexander Klug or any member of his or her immediate family, has no funding or commercial associations (e.g., consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article. Manuel Weißenberger or any member of his or her immediate family, has no funding or commercial associations (e.g., consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article. Reinhard Hoffmann or any member of his or her immediate family, has no funding or commercial associations (e.g., consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article. Yves Gramlich or any member of his or her immediate family, has no funding or commercial associations (e.g., consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article. Philipp Drees or any member of his or her immediate family, has no funding or commercial associations (e.g., consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article. Maximilian Rudert or any member of his or her immediate family, has no funding or commercial associations (e.g., consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article. KarlPhilipp Kutzner or any member of his or her immediate family, has no funding or commercial associations (e.g., consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article.
Ethical approval
No ethical approval was needed for this study.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Karl Philipp Kutzner and Manuel Weißenberger contributed equally to this publication.
Contributor Information
Alexander Klug, Email: alexander.klug@bgu-frankfurt.de.
Yves Gramlich, Email: yves.gramlich@bgu-frankfurt.de.
Maximilian Rudert, Email: m-rudert.klh@uni-wuerzburg.de.
Philipp Drees, Email: philipp.drees@unimedizin-mainz.de.
Reinhard Hoffmann, Email: reinhard.hoffmann@bgu-frankfurt.de.
Manuel Weißenberger, Email: m-weissenberger.klh@uni-wuerzburg.de.
Karl Philipp Kutzner, Email: kkutzner@joho.de.
References
- 1.Ackerman IN, Bohensky MA, Zomer E, et al. The projected burden of primary total knee and hip replacement for osteoarthritis in Australia to the year 2030. BMC Musculoskelet Disord. 2019;20:90. doi: 10.1186/s12891-019-2411-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Andreozzi V, Conteduca F, Iorio R, et al. Comorbidities rather than age affect medium-term outcome in octogenarian patients after total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2019 doi: 10.1007/s00167-019-05788-6. [DOI] [PubMed] [Google Scholar]
- 3.Bozdogan H. Model selection and Akaike's Information Criterion (AIC): the general theory and its analytical extensions. Psychometrika. 1987;52:345–370. doi: 10.1007/BF02294361. [DOI] [Google Scholar]
- 4.Chawla H, van der List JP, Christ AB, et al. Annual revision rates of partial versus total knee arthroplasty: a comparative meta-analysis. Knee. 2017;24:179–190. doi: 10.1016/j.knee.2016.11.006. [DOI] [PubMed] [Google Scholar]
- 5.Culliford D, Maskell J, Judge A, et al. Future projections of total hip and knee arthroplasty in the UK: results from the UK Clinical Practice Research Datalink. Osteoarthr Cartil. 2015;23:594–600. doi: 10.1016/j.joca.2014.12.022. [DOI] [PubMed] [Google Scholar]
- 6.Deutsches Institut für Medizinische Dokumentation und Information (DIMDI) im Auftrag des Bundesministeriums für Gesundheit (BMG) unter Beteiligung der Arbeitsgruppe OPS des Kuratoriums für Fragen der Klassifikation im Gesundheitswesen (KKG), OPS Version 2019 (Operationen- und Prozedurenschlüssel), Köln. Accessed May 20 2020
- 7.Goudie EB, Robinson C, Walmsley P, et al. Changing trends in total knee replacement. Eur J Orthop Surg Traumatol. 2017;27:539–544. doi: 10.1007/s00590-017-1934-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Guerrero-Ludueña RE, Comas M, Espallargues M, et al. Predicting the burden of revision knee arthroplasty: simulation of a 20-Year horizon. Value Health. 2016;19:680–687. doi: 10.1016/j.jval.2016.02.018. [DOI] [PubMed] [Google Scholar]
- 9.Hamilton DF, Howie CR, Burnett R, et al. Dealing with the predicted increase in demand for revision total knee arthroplasty: challenges, risks and opportunities. Bone Joint J. 2015;97-B:723–728. doi: 10.1302/0301-620X.97B6.35185. [DOI] [PubMed] [Google Scholar]
- 10.Hansen EN, Ong KL, Lau E, et al. Unicondylar knee arthroplasty has fewer complications but higher revision rates than total knee arthroplasty in a study of large United States databases. J Arthroplasty. 2019;34:1617–1625. doi: 10.1016/j.arth.2019.04.004. [DOI] [PubMed] [Google Scholar]
- 11.Heijink A, Gomoll AH, Madry H, et al. Biomechanical considerations in the pathogenesis of osteoarthritis of the knee. Knee Surg Sports Traumatol Arthrosc. 2012;20:423–435. doi: 10.1007/s00167-011-1818-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Hirschmann MT, Hart A, Henckel J, et al. COVID-19 coronavirus: recommended personal protective equipment for the orthopaedic and trauma surgeon. Knee Surg Sports Traumatol Arthrosc. 2020;28:1690–1698. doi: 10.1007/s00167-020-06022-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Hyndman RJ, Koehler AB, Snyder RD, et al. A state space framework for automatic forecasting using exponential smoothing methods. Int J Forecast. 2002;18:439–454. doi: 10.1016/S0169-2070(01)00110-8. [DOI] [Google Scholar]
- 14.Hyndman RJ, Lee AJ, Wang E. Fast computation of reconciled forecasts for hierarchical and grouped time series. Comput Stat Data Anal. 2016;97:16–32. doi: 10.1016/j.csda.2015.11.007. [DOI] [Google Scholar]
- 15.Inacio MCS, Graves SE, Pratt NL, et al. Increase in total joint arthroplasty projected from 2014 to 2046 in Australia: a conservative local model with international implications. Clin Orthop Relat Res. 2017;475:2130–2137. doi: 10.1007/s11999-017-5377-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Inacio MCS, Paxton EW, Graves SE, et al. Projected increase in total knee arthroplasty in the United States–an alternative projection model. Osteoarthr Cartil. 2017;25:1797–1803. doi: 10.1016/j.joca.2017.07.022. [DOI] [PubMed] [Google Scholar]
- 17.Jenkins PJ, Clement ND, Hamilton DF, et al. Predicting the cost-effectiveness of total hip and knee replacement: a health economic analysis. Bone Joint J. 2013;95-B:115–121. doi: 10.1302/0301-620X.95B1.29835. [DOI] [PubMed] [Google Scholar]
- 18.Juang W-C, Huang S-J, Huang F-D, et al. Application of time series analysis in modelling and forecasting emergency department visits in a medical centre in Southern Taiwan. BMJ Open. 2017;7:e018628. doi: 10.1136/bmjopen-2017-018628. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Kamath AF, Ong KL, Lau E, et al. Quantifying the burden of revision total joint arthroplasty for periprosthetic infection. J Arthroplasty. 2015;30:1492–1497. doi: 10.1016/j.arth.2015.03.035. [DOI] [PubMed] [Google Scholar]
- 20.Kasch R, Assmann G, Merk S, et al. Economic analysis of two-stage septic revision after total hip arthroplasty: what are the relevant costs for the hospital's orthopedic department? BMC Musculoskelet Disord. 2016;17:112. doi: 10.1186/s12891-016-0962-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Kennedy JA, Burn E, Mohammad HR, et al. Lifetime revision risk for medial unicompartmental knee replacement is lower than expected. Knee Surg Sports Traumatol Arthrosc. 2020 doi: 10.1007/s00167-020-05863-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Khan M, Osman K, Green G, et al. The epidemiology of failure in total knee arthroplasty: avoiding your next revision. Bone Joint J. 2016;98-B:105–112. doi: 10.1302/0301-620X.98B1.36293. [DOI] [PubMed] [Google Scholar]
- 23.Kievit AJ, Kuijer PPFM, de Haan LJ, et al. Patients return to work sooner after unicompartmental knee arthroplasty than after total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2019 doi: 10.1007/s00167-019-05667-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Klasan A, Magill P, Frampton C, et al. Factors predicting repeat revision and outcome after aseptic revision total knee arthroplasty: results from the New Zealand Joint Registry. Knee Surg Sports Traumatol Arthrosc. 2020 doi: 10.1007/s00167-020-05985-8. [DOI] [PubMed] [Google Scholar]
- 25.Kleeblad LJ, van der List JP, Zuiderbaan HA, et al. Larger range of motion and increased return to activity, but higher revision rates following unicompartmental versus total knee arthroplasty in patients under 65: a systematic review. Knee Surg Sports Traumatol Arthrosc. 2018;26:1811–1822. doi: 10.1007/s00167-017-4817-y. [DOI] [PubMed] [Google Scholar]
- 26.Kokko MA, Abdel MP, Berry DJ, et al. A retrieval analysis perspective on revision for infection. Arthroplast Today. 2019;5:362–370. doi: 10.1016/j.artd.2019.03.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Kunutsor SK, Whitehouse MR, Blom AW, et al. Patient-related risk factors for periprosthetic joint infection after total joint arthroplasty: a systematic review and meta-analysis. PLoS ONE. 2016;11:e0150866. doi: 10.1371/journal.pone.0150866. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Kurtz S, Ong K, Lau E, et al. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am. 2007;89:780–785. doi: 10.2106/JBJS.F.00222. [DOI] [PubMed] [Google Scholar]
- 29.Kurtz SM, Lau E, Schmier J, et al. Infection burden for hip and knee arthroplasty in the United States. J Arthroplasty. 2008;23:984–991. doi: 10.1016/j.arth.2007.10.017. [DOI] [PubMed] [Google Scholar]
- 30.Kurtz SM, Lau E, Watson H, et al. Economic burden of periprosthetic joint infection in the United States. J Arthroplasty. 2012;27:61–5.e1. doi: 10.1016/j.arth.2012.02.022. [DOI] [PubMed] [Google Scholar]
- 31.Kurtz SM, Ong KL, Lau E, et al. Impact of the economic downturn on total joint replacement demand in the United States: updated projections to 2021. J Bone Joint Surg Am. 2014;96:624–630. doi: 10.2106/JBJS.M.00285. [DOI] [PubMed] [Google Scholar]
- 32.Kurtz SM, Lau EC, Son M-S, et al. Are we winning or losing the battle with periprosthetic joint infection: trends in periprosthetic joint infection and mortality risk for the medicare population. J Arthroplasty. 2018;33:3238–3245. doi: 10.1016/j.arth.2018.05.042. [DOI] [PubMed] [Google Scholar]
- 33.Lavernia C, Lee DJ, Hernandez VH. The increasing financial burden of knee revision surgery in the United States. Clin Orthop Relat Res. 2006;446:221–226. doi: 10.1097/01.blo.0000214424.67453.9a. [DOI] [PubMed] [Google Scholar]
- 34.Lee JK, Kim HJ, Park JO, et al. Inferior outcome of revision of unicompartmental knee arthroplasty to total knee arthroplasty compared with primary total knee arthroplasty: systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc. 2018;26:3403–3418. doi: 10.1007/s00167-018-4909-3. [DOI] [PubMed] [Google Scholar]
- 35.Lizaur-Utrilla A, Martinez-Mendez D, Miralles-Muñoz FA, et al. Comparable outcomes after total knee arthroplasty in patients under 55 years than in older patients: a matched prospective study with minimum follow-up of 10 years. Knee Surg Sports Traumatol Arthrosc. 2017;25:3396–3402. doi: 10.1007/s00167-016-4406-5. [DOI] [PubMed] [Google Scholar]
- 36.Malchau H, Herberts P, Eisler T, et al. The Swedish Total Hip Replacement Register. J Bone Joint Surg Am. 2002;84-A(Suppl 2):2–20. doi: 10.2106/00004623-200200002-00002. [DOI] [PubMed] [Google Scholar]
- 37.McCalden RW, Robert CE, Howard JL, et al. Comparison of outcomes and survivorship between patients of different age groups following TKA. J Arthroplasty. 2013;28:83–86. doi: 10.1016/j.arth.2013.03.034. [DOI] [PubMed] [Google Scholar]
- 38.Moral-Benito E. Model averaging in economics: an overview. J Econ Surv. 2015;29:46–75. doi: 10.1111/joes.12044. [DOI] [Google Scholar]
- 39.Moran JL, Solomon PJ. Conventional and advanced time series estimation: application to the Australian and New Zealand Intensive Care Society (ANZICS) adult patient database, 1993–2006. J Eval Clin Pract. 2011;17:45–60. doi: 10.1111/j.1365-2753.2010.01368.x. [DOI] [PubMed] [Google Scholar]
- 40.Nemes S, Rolfson O, W-Dahl A, et al. Historical view and future demand for knee arthroplasty in Sweden. Acta Orthop. 2015;86:426–431. doi: 10.3109/17453674.2015.1034608. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Nguyen L-CL, Lehil MS, Bozic KJ. Trends in total knee arthroplasty implant utilization. J Arthroplasty. 2015;30:739–742. doi: 10.1016/j.arth.2014.12.009. [DOI] [PubMed] [Google Scholar]
- 42.Oduwole KO, Molony DC, Walls RJ, et al. Increasing financial burden of revision total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2010;18:945–948. doi: 10.1007/s00167-010-1074-8. [DOI] [PubMed] [Google Scholar]
- 43.Paxton EW, Namba RS, Maletis GB, et al. A prospective study of 80,000 total joint and 5000 anterior cruciate ligament reconstruction procedures in a community-based registry in the United States. J Bone Joint Surg Am. 2010;92(Suppl 2):117–132. doi: 10.2106/JBJS.J.00807. [DOI] [PubMed] [Google Scholar]
- 44.Petzold T, Haase E, Niethard FU, et al. Orthopädisch-unfallchirurgische Versorgung bis 2050. Analyse des Inanspruchnahmeverhaltens bei relevanten Erkrankungen und Ableitung der Häufigkeit ärztlicher Leistungserbringer (Orthopaedic and trauma surgical care until 2050. Analysis of the utilization behavior for relevant diseases and derivation of the number of medical service providers) Orthopade. 2016;45:167–173. doi: 10.1007/s00132-015-3176-y. [DOI] [PubMed] [Google Scholar]
- 45.Pötzsch ORF. Demographic analyses, methods and projections, births and deaths: Germany’s population by 2060—Results of the 13th coordinated population projection. Wiesbaden: Federal Statistical Office of Germany; 2015. [Google Scholar]
- 46.Reeves RA, Schairer WW, Jevsevar DS. Costs and risk factors for hospital readmission after periprosthetic knee fractures in the United States. J Arthroplasty. 2018;33:324–330.e1. doi: 10.1016/j.arth.2017.09.024. [DOI] [PubMed] [Google Scholar]
- 47.Romanini E, Decarolis F, Luzi I, et al. Total knee arthroplasty in Italy: reflections from the last fifteen years and projections for the next thirty. Int Orthop. 2019;43:133–138. doi: 10.1007/s00264-018-4165-7. [DOI] [PubMed] [Google Scholar]
- 48.Rupp M, Lau E, Kurtz SM, et al. Projections of primary TKA and THA in Germany from 2016 through 2040. Clin Orthop Relat Res. 2020 doi: 10.1097/CORR.0000000000001214. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Schwartz AJ, Chang Y-HH, Bozic KJ, et al. Evidence of pent-up demand for total hip and total knee arthroplasty at age 65. J Arthroplasty. 2019;34:194–200. doi: 10.1016/j.arth.2018.09.087. [DOI] [PubMed] [Google Scholar]
- 50.Schwartz AM, Farley KX, Guild GN, et al. Projections and epidemiology of revision hip and knee arthroplasty in the United States to 2030. J Arthroplasty. 2020 doi: 10.1016/j.arth.2020.02.030. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Scott CEH, Turnbull GS, MacDonald D, et al. Activity levels and return to work following total knee arthroplasty in patients under 65 years of age. Bone Joint J. 2017;99B-8:1037–1046. doi: 10.1302/0301-620X.99B8.BJJ-2016-1364.R1. [DOI] [PubMed] [Google Scholar]
- 52.Sloan M, Premkumar A, Sheth NP. Projected volume of primary total joint arthroplasty in the U.S., 2014 to 2030. J Bone Joint Surg Am. 2018;100:1455–1460. doi: 10.2106/JBJS.17.01617. [DOI] [PubMed] [Google Scholar]
- 53.Thaler M, Khosravi I, Hirschmann MT, et al. Disruption of joint arthroplasty services in Europe during the COVID-19 pandemic: an online survey within the European Hip Society (EHS) and the European Knee Associates (EKA) Knee Surg Sports Traumatol Arthrosc. 2020;28:1712–1719. doi: 10.1007/s00167-020-06033-1. [DOI] [PMC free article] [PubMed] [Google Scholar]