Abstract
Bovine coronaviruses are spread all over the world. They cause two types of clinical manifestations in cattle either an enteric, calf diarrhoea and winter dysentery in adult cattle, or respiratory in all age groups of cattle. The role of coronaviruses in respiratory infections is still a hot topic of discussion since they have been isolated from sick as well as healthy animals and replication of disease is rarely successful. Bovine coronavirus infection is characterised by high morbidity but low mortality. The laboratory diagnosis is typically based on serological or molecular methods. There is no registered drug for the treatment of virus infections in cattle and we are limited to supportive therapy and preventative measures. The prevention of infection is based on vaccination, biosecurity, management and hygiene. This paper will cover epidemiology, taxonomy, pathogenesis, clinical signs, diagnosis, therapy, economic impact and prevention of coronavirus infections in cattle.
Keywords: Bovine coronavirus, Calf diarrhoea, Winter dysentery, Bovine respiratory disease complex, Betacoronavirus
Introduction
Coronaviruses are a very relevant topic, especially at this time when we are facing a severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) pandemic, which has elucidated how little we still know about these microorganisms and their spread from animals to humans (Bojkova et al. 2020). This review paper provides a complete overview of the essential current information on bovine coronaviruses’ epidemiology, taxonomy, pathogenesis, clinical signs, diagnosis, therapy and prevention. It also provides information on the economic relevance of bovine coronavirus infections and a description of Norway’s control programme for the limitation of their spread.
The virus and taxonomy
Bovine coronaviruses (BCoV) are single-stranded positive-sense RNA viruses with a lipid envelope. Coronaviruses are spherical and got their name from the spike glycoproteins protruding from their envelope resembling a solar corona (Bárcena et al. 2009). They have five major structural proteins: hemagglutinin-esterase protein (HE), spike glycoprotein (S), small membrane protein (E), membrane protein (M) and nucleocapsid protein (N) (Suzuki et al. 2020), with the S and HE proteins being crucial for the virus to enter host cells and induce an immune response (Saif 2010; Ellis 2019). The N protein is most homologous between different BCoVs and is used for molecular diagnosis (Cho et al. 2001a; Park et al. 2006).
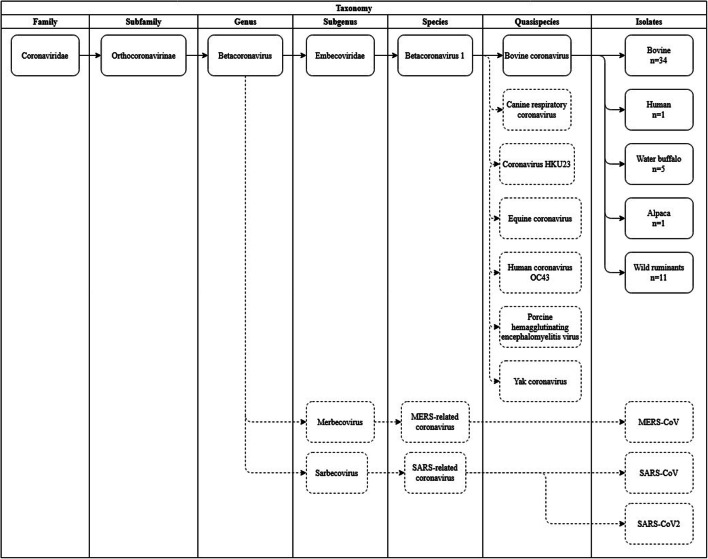
Bovine coronaviruses belong to the order Nidovirales, family Coronaviridae, subfamily Orthocoronavirinae, genus Betacoronavirus and subgenus Embecovirus. The genus Betacoronavirus is important for humans as well, as it contains one of the common cold viruses (human coronavirus OC43) and viruses associated with epidemics of severe acute respiratory syndrome-related coronavirus (HCoV-SARS) and Middle East respiratory syndrome-related coronavirus (MERS-CoV) as well as the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), responsible for the current disastrous pandemic (ICTV 2019). A close relation of different coronaviruses explains the potential for zoonotic infections. Since 2008, bovine coronaviruses are no longer a distinct species. They have been merged into one species called Betacoronavirus 1 together with other human, swine, horse and dog coronaviruses (human enteric coronavirus; human coronavirus OC43; porcine hemagglutinating encephalomyelitis virus; equine coronavirus; canine respiratory coronavirus), and others were added later (Fig. 1). The change was justified because insufficient demarcation in the replicase 1ab domains is present (at least 10%) to warrant a separate species (de Groot et al. 2008). Thus, BCoVs are now regarded as host-range variant or quasispecies. Scientists have also identified a group of bovines like coronaviruses that cause similar clinical signs in other domestic and wild ruminants, which could serve as a reservoir for cattle infection and vice versa (Amer 2018).
Fig. 1.
Taxonomy of bovine coronavirus and its relation to SARS and MERS coronavirus
Epidemiology
BCoVs are widespread all over the world (Boileau and Kapil 2010; Toftaker et al. 2017). Winter dysentery was typically reported in colder regions but new reports have documented episodes in warmer seasons (summer in Korea) or in tropical countries like Thailand, Brazil and Cuba (Barrera Valle et al. 2006; Park et al. 2006; Takiuchi et al. 2009; Ribeiro et al. 2016; Singasa et al. 2017). They can be divided into two groups based on clinical signs. The coronaviruses that were isolated from calves and cattle with diarrhoea are referred to as enteric BCoV (EBCoV) and those that were isolated from animals with respiratory clinical signs as respiratory BCoV (RBCoV). Enteric BCoV can be further subdivided into EBCoV that cause diarrhoea in calves (EBCoV-CD) and those that cause winter dysentery in adult cattle (EBCoV-WD) (Boileau and Kapil 2010).
BCoVs belong to one serotype (Takahashi et al. 1983; Saif 2010) but can be differentiated using molecular and antigenic methods; however, no distinct separating marker between clinical syndromes was identified (Zhang et al. 1994; Tsunemitsu and Saif 1995; Fukutomi et al. 1999; Hasoksuz et al. 2002; Kanno et al. 2007). The genetic sequences tend to cluster according to the geographical region of detection rather than the clinical picture (Park et al. 2006; Bidokhti et al. 2012; Beuttemmuller et al. 2017). A bigger difference was also observed between older and newer isolates than between isolates from different clinical syndromes (Zhang et al. 2007; Saif 2010). Furthermore, the same clinical picture was observed in calves experimentally infected with isolates from all three clinical syndromes of BCoV (Cho et al. 2001a; Bidokhti et al. 2012). They also provide some degree of cross-immunity, with no clinical signs and only virus shedding detected upon reinfection (El-Kanawati et al. 1996; Cho et al. 2001a). Therefore, it is speculated that clinical signs are not the result of infection with specific BCoV strain but of other circumstances at the time of infection such as stress, temperature and host health (Bidokhti et al. 2012; Suzuki et al. 2020).
Pathogenesis
Animals become infected with BCoV through the faecal-oral route or inhalation of aerosol (Thomas et al. 2006; Saif 2010; Oma et al. 2016). BCoVs enter the cell by binding to its membrane receptors (N-acetyl-9-O-acetylneuraminic acid) with the S protein, more specifically the S1 part, which forms the bulb. The virus gains entry into the cell by cleavage of the S protein by cellular trypsin-like proteases. The S2 part, which forms the stem of the protein, mediates the fusion of the virus with the host cell membrane (Popova and Zhang 2002). Whether the initial replication takes place in the respiratory (nasal turbinates, trachea and lungs) or the gastrointestinal tract (enterocytes) is still a matter of debate. With one side, claiming that the initial replication takes place in the respiratory tract and large quantities of virus protected by mucus are then swallowed to infect the intestine (Saif 2010; Oma et al. 2016), while the other side claims that the gastrointestinal tract is infected first and the virus reaches the respiratory tract with viraemia (Park et al. 2007; Boileau and Kapil 2010). Whatever the primary site of replication is, BCoVs are shed both in faeces and in nasal secretions (Cho et al. 2001a; Park et al. 2007). The duration of virus shedding can be quite extensive, up to 932 days post-infection detected with nested PCR in nasal discharge and 1058 days in faeces, as shown by Kanno et al. (2018). The role of chronically/subclinically infected animals is still debated because detection of the virus is common in clinically healthy adults and calves (Crouch et al. 1985; Cho et al. 2001a; Bartels et al. 2010; Coura et al. 2015). The most common route of disease transmission is from dam to calf or between calves. Between herds, infections occur with the purchase of new animals or with contaminated fomites (Oma et al. 2016; Oma et al. 2018). Dogs have also been suggested as carriers (Erles et al. 2003; Boileau and Kapil 2010). BCoV affects the whole gastrointestinal tract starting in the duodenum then spreading to the large intestine causing villous atrophy and other mucosal lesions (Mebus et al. 1973; Langpap et al. 1979; Park et al. 2007). In the respiratory tract, it causes interstitial pneumonia and epithelial damage on nasal turbinates, trachea and lungs (Park et al. 2007; Oma et al. 2016; Kalkanov et al. 2019).
Clinical signs
Calf diarrhoea
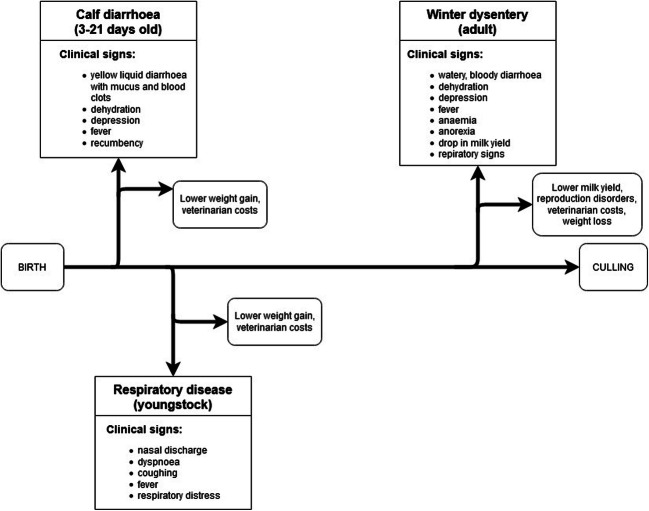
BCoV causes necrotic enterocolitis with loss of villous length, which results in malabsorption diarrhoea (Mebus et al. 1973; Langpap et al. 1979; Park et al. 2007). Morbidity is high while mortality can vary depending on age and immunity (Alfieri et al. 2018). The virus can cause haemorrhagic diarrhoea in calves. Most calves have yellow liquid diarrhoea with mucus and blood clots, dehydration, hypothermia and depression (Fig. 2). Reduced feed intake and electrolyte loss can result in metabolic acidosis and hypoglycaemia (Gomez and Weese 2017). In severe cases, fever, recumbence and death can also occur. Some calves may have additional respiratory signs (Mebus et al. 1973; Boileau and Kapil 2010). Most are affected between 3 and 21 days of age (Saif and Heckert 1990). The incubation period is 1–7 days (Mebus et al. 1973; Cho et al. 2001a). Clinical signs last for 3–6 days (Gomez and Weese 2017). Calves spread the virus with both faeces and nasal secretions (Cho et al. 2001a). The disease is self-limiting (Alfieri et al. 2018). BCoV can be found in both healthy and sick calves (Bartels et al. 2010; Coura et al. 2015). In a Uruguayan study, they found a seasonal pattern, with the winter months (average temperature < 13 °C) having a higher frequency of detection of BCoV in calves (odds ratio: 9.05; 95% CI: 2.77–29.53) (Castells et al. 2019).
Fig. 2.
Clinical signs and economic impact of bovine coronaviruses on cattle through their lifetime
Winter dysentery
In adult cattle, BCoV infection is characterised by epizootic outbreaks of self-limiting watery diarrhoea with the presence of blood, fever, depression, dehydration, anorexia, colic and drop in milk yield (Fig. 2) (Takahashi et al. 1983; Jactel et al. 1990; Natsuaki et al. 2007; Boileau and Kapil 2010; Akgül et al. 2013; Abuelo and Perez-Santos 2016). In severe cases, anaemia may occur because of blood loss (Natsuaki et al. 2007). The virus can be detected in both faeces and nasal secretions (Abuelo and Perez-Santos 2016). Naïve, dairy cows in the postpartum period are the most affected (Natsuaki et al. 2007). Incidentally, Ribeiro et al. (2016) have diagnosed a case of winter dysentery in pasture steers in Brazil. Concurrent respiratory signs have also been observed (Jactel et al. 1990; Akgül et al. 2013; Abuelo and Perez-Santos 2016). The incubation period is 2–8 days (Boileau and Kapil 2010). Morbidity is very high, up to 100%, but mortality is low, less than 2% (Jactel et al. 1990; Gagea et al. 2006; Takiuchi et al. 2009). Animals respond well to supportive treatment and usually recover in 2–3 days (Akgül et al. 2013). The episode will usually pass in 1–2 weeks depending on herd size and previous exposure to BCoV. Episodes of winter dysentery were historically associated with colder regions and the onset of cold weather (cold stress), but new reports suggest that this is not the case with episodes in warmer seasons or in tropical countries (Barrera Valle et al. 2006; Park et al. 2006; Takiuchi et al. 2009; Ribeiro et al. 2016; Singasa et al. 2017). Park et al. (2006) speculate that this could be attributed to the absence of receptor-destroying enzyme (RDE) which they observed in the warmer season isolates and could lead to enhanced virulence or survivability in warmer environments. Lesions are similar to those seen in calf diarrhoea, mainly localised to the colon (Natsuaki et al. 2007). It is suspected that adult cattle are carriers of BCoV and that clinical signs emerge due to environmental stressors (Jactel et al. 1990; Abuelo and Perez-Santos 2016).
Respiratory BCoV
BCoV has been isolated and detected in many outbreaks of respiratory disease in cattle of all ages (Heckert et al. 1990; Saif 2010; Decaro et al. 2008). Clinical signs include nasal discharge, dyspnoea, coughing, fever and respiratory distress (Fig. 2) (Saif 2010). However, controversy exists whether BCoV is also associated with bovine respiratory disease complex (BRDC). The controversy is based on the fact that many studies have isolated BCoV from feedlot cattle with clinical signs of BRDC and no or limited co-infection with other respiratory pathogens (Storz et al. 2000a; Lin et al. 2000; Lathrop et al. 2000; Cho et al. 2001b; Thomas et al. 2006; Paller et al. 2017), while others have achieved the same in clinically healthy cattle (Crouch et al. 1985; Heckert et al. 1990; Hasoksuz et al. 1999; Workman et al. 2019). However, most of the first studies have also identified seroconversion. Seroconversion protected animals from severe BRDC clinical signs and treatment in subsequent infections (Martin et al. 1998; Lin et al. 2000; Cho et al. 2001b; Plummer et al. 2004). Some studies did not confirm this association (Heckert et al. 1990; Workman et al. 2019). Few studies have confirmed BCoV in the lungs (McNulty et al. 1984; Storz et al. 2000a; Park et al. 2007; Paller 2019). Still, BCoV could be the factor that opens the floodgates for secondary bacterial infection. Storz et al. (2000b) have confirmed infections with BCoV and Pasteurella using Evan’s criteria for causation. Ellis (2019), however, argues that the presence of BCoV in sick animals is not enough and a connection between virus load and clinical symptoms should be further investigated to confirm causality. Additionally, the evidence demonstrating Koch’s postulates is scant and unsystematic (Ellis 2019). However, BCoVs should not be dismissed as a respiratory pathogen but should rather still be considered as a piece of the puzzle in the multifactorial aetiology of BRDC until proven otherwise.
Diagnosis
Infection with BCoVs can be suspected based on history, clinical presentation and age of the animal in enteric cases. Differential diagnoses include BVDV, Schmallenberg virus infection, Salmonella spp., Clostridium perfringens infection (enterotoxaemia), fasciolosis, nematodiasis and some intoxications in adult cattle and BVDV, rotavirus, enterotoxigenic Escherichia coli, Cryptosporidium parvum, coccidiosis, Salmonella spp., Clostridium perfringens infection (enterotoxaemia), giardiasis, nematodiasis and some intoxications in calves (Boileau and Kapil 2010; Sedda and Rogers 2013; Heller and Chigerwe 2018). For the definitive diagnosis, BCoV infection must be confirmed using laboratory assays like electron microscopy, virus isolation, serological or molecular methods. Rapid lateral flow immunoassay tests are also useful for cow-/calf-side testing (Kleina et al. 2008; Icen et al. 2013). Nasal swabs, tracheobronchial lavage, probang cups and faecal samples are used in live animals. It must be noted that the shedding of BCoVs is high at the time of initial infection and then stops or shifts to an intermittent shedding pattern (Coura et al. 2015; Oma et al. 2016). At necropsy trachea, nasal turbinates, lungs and the spiral colon are the samples of choice (Boileau and Kapil 2010). Oma et al. (2016) also detected virus RNA in mesenteric lymph nodes. Electron microscopy is hindered by low sensitivity (Saif 2010). For the isolation of BCoV either from enteric or respiratory samples, a cloned line of human rectal tumour (HRT)-18 cell cultures are used; however, the process is fastidious (Saif 2010; Ellis 2019). For the detection of virus antigens in tissues, immunofluorescent or immunohistochemical staining has proven to be effective (Boileau and Kapil 2010). To judge the serologic response of animals, virus neutralisation, hemagglutination inhibition (HI) tests and enzyme-linked immunosorbent assay (ELISA) are performed. Because seroconversion in cattle is common, paired-samples are preferred (Saif 2010; Workman et al. 2019). Antigens in faeces and nasal swabs are detected using antigen-capture ELISA. However, molecular methods are more sensitive and have become widely used. They include RT-PCR, nested RT-PCR, real-time RT quantitative (q) PCR assays and genome sequencing (Saif 2010; Bidokhti et al. 2012; Kanno et al. 2018; Paller et al. 2017; Workman et al. 2019). The N protein gene is used for BCoV detection and S glycoprotein sequence for epidemiologic investigation and virus differentiation (Cho et al. 2001a; Park et al. 2006; Bidokhti et al. 2012). The sensitivity of molecular methods could lead to false-positive results in biologically insignificant cases (Oma et al. 2016; Ellis 2019). Oma et al. (2016) have detected the shedding of the virus with RT-qPCR 5 weeks post-inoculation, but at 3 weeks post-challenge, none of the comingled naïve calves became infected. They were also unable to isolate the virus at this point.
Treatment
Because there is currently no effective treatment for viral diseases, we are limited to supportive therapy. In calf diarrhoea, this consists of fluid, glucose and electrolyte supplementation to counter dehydration, hypoglycaemia, electrolyte imbalance and acidosis. Calves also benefit from a warm and dry stall (Boileau and Kapil 2010).
Winter dysentery is usually a self-limiting disease. However, in advanced cases, oral or intravenous fluid therapy or in cases of severe dysentery blood transfusion are indicated. The use of non-steroidal anti-inflammatory drugs (NSAID) and anti-haemorrhagic agents is also described (Natsuaki et al. 2007; Abuelo and Perez-Santos 2016; Chigerwe and Heller 2018).
In the case of BRDC, antimicrobial treatment is still advised because the secondary bacterial infection is common. The administration of non-steroidal anti-inflammatory drugs has also proven beneficial (Boileau and Kapil 2010).
Economic impact
The economic impact of winter dysentery is substantial, especially in dairy herds. The drop in milk production can vary from 0 to 70% per outbreak compared with the daily milk yield before infection according to different studies (Takahashi et al. 1983; Jactel et al. 1990; Takiuchi et al. 2009; Akgül et al. 2013; Abuelo and Perez-Santos 2016; Toftaker et al. 2017). In a Swedish study, the loss was calculated to be 51 L per cow in the period from 7 days before and 19 days after a reported outbreak compared with an uninfected cow. Additional costs can be attributed to veterinary treatment, additional labour, weight loss and reproduction disorders (Fig. 2) (Toftaker et al. 2017). Feedlot calves that shed BECoV had 8.17 kg lower weight gain compared with non-shedding herd mates (Cho et al. 2001b). Despite the role BRCoV in BRDC not being defined, we can still assume that economic losses also occur in respiratory infections with BRCoV (Martin et al. 1998).
Prevention
The prevention of BCoV diseases is important to limit the use of antimicrobials and subsequently reduce the occurrence of antimicrobial resistance, increase the quality of animal products and animal welfare. The prevention of BCoV was historically based on vaccination, management and hygiene. There are registered multivalent vaccines for dams to limit the shedding of the virus and provide hyperimmune colostrum that provides passive protection of calves, which both can protect from or lessen the severity of BCoV diarrhoea in calves. Vaccination of dams has proven to be fairly effective in a Uruguayan study, with calves from unvaccinated dams having a 4.02 (95% CI: 1.18–8.9) higher odds of shedding BCoV (Castells et al. 2019). The importance of adequate passive immunity cannot be overstated (Boileau and Kapil 2010). A modified live vaccine for oral vaccination of calves also exists for the prevention of diarrhoea (Boileau and Kapil 2010). There were also studies using an intranasal vaccine for BCoV in feedlot calves to limit the effect of BRDC (Plummer et al. 2004) and a vaccine against winter dysentery (Takamura et al. 2002). Metaphylactic antimicrobials are also used in the prevention of bacterial co-infections in BRDC (McVey 2009). Management, housing and biosecurity also play a crucial role (Boileau and Kapil 2010). BCoVs are susceptible to heat, detergents and disinfectants like sodium hypochlorite, chloramine T, povidone iodine, 70% ethanol, glutaraldehyde, quaternary ammonium compounds, phenolic compounds and formaldehyde (Sattar et al. 1989; Sattar and Springthorpe 1996). However, coronaviruses have been reported to survive well at low temperatures and high relative humidity. Their survival on surfaces is also long, up to 120 h (Duan et al. 2003) and even longer in organic medium (Geller et al. 2012).
Norway is to the authors’ best knowledge the only country in the world that has implemented a control programme for BCoVs. It has a joined Bovine Respiratory Syncytial Virus and BCoV national, industry run control programme based on serological surveillance and the classification of herds (positive/negative) in place since 2016. The programme aims to reduce the occurrence of BCoV on herd level by protecting herds from infection through biosecurity measures. Herds with negative status and additional biosecurity measures are reworded financially (10% increase in price for young stock and breeding animals). The cost of the control programme is sheared between the producers and the industry. Eligible samples are bulk tank milk, pooled first lactation cow milk and pooled serum samples from young stock older than 180 days to avoid maternal antibody interference. Beef herds test only young stock. The negative status is valid for 1 year. If a producer buys an animal from a positive herd, the status is automatically switched to positive. The biosecurity measures include separation of animals of different statuses, different transport vehicles, the building of loading areas, the provision of a sluice and clean clothes and footwear for visitors. They have also provided a hotline to report outbreaks of disease to limit further spread (Stokstad et al. 2020).
Conclusion
Coronaviruses are involved in the aetiology of three clinical syndromes in cattle. However, its role in BRDC still needs to be proven beyond a reasonable doubt. Future research should aim to further investigate the reasons for the occurrence of different clinical syndromes in animals infected with the same BCoV and the role of cattle in coronavirus transmission to humans. In the light of the recent coronavirus pandemic, it would also be crucial to know if cattle can become infected and transmit the new SARS-CoV-2.
Funding information
The research programme group P4-0092 of the Veterinary Faculty, University of Ljubljana, funded by the Slovenian Research Agency supported this work.
Compliance with ethical standards
Conflict of interest
The authors declare that they have no conflict of interest.
Footnotes
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- Abuelo A, Perez-Santos M. A winter dysentery (coronavirus infection) outbreak in a dairy herd in Galicia (northwestern Spain) Veterinary Record Case Reports. 2016;4:e000328. doi: 10.1136/vetreccr-2016-000328. [DOI] [Google Scholar]
- Akgül G, Mecitoğlu Z, Ertürk A, Çatik S, Temizel EM, Gülyaz V, Gülaçti I, Özdemir S, Onat K, Şenlik B, Şentürk S. Isolation of First Local Coranavirus from Cattle with Winter Dysentery in Turkey. Uludag University Journal Of The Faculty Of Veterinary Medicine. 2013;32(2):63–69. [Google Scholar]
- Alfieri AA, Ribeiro J, de Carvalho Balbo L, Lorenzetti E, Alfieri AF. Dairy calf rearing unit and infectious diseases: diarrhea outbreak by bovine coronavirus as a model for the dispersion of pathogenic microorganisms. Tropical Animal Health and Production. 2018;50(8):1937–1940. doi: 10.1007/s11250-018-1592-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Amer HM. Bovine-like coronaviruses in domestic and wild ruminants. Animal Health Research Reviews. 2018;19:113–124. doi: 10.1017/S1466252318000117. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bárcena M, Oostergetel GT, Bartelink W, Faas FG, Verkleij A, Rottier PJ, Koster AJ, Bosch BJ. Cryo-electron tomography of mouse hepatitis virus: Insights into the structure of the coronavirion. Proceedings of the National Academy of Sciences of the United States of America. 2009;106(2):582–587. doi: 10.1073/pnas.0805270106. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Barrera VM, Rodríguez BE, Betancourt MA, Frías Lepuroux MT, Brandão P. Short communication: First report in Cuba of bovine coronavirus detection in a winter dysentery outbreak. Spanish Journal of Agricultural Research. 2006;4(3):221–224. [Google Scholar]
- Bartels CJ, Holzhauer M, Jorritsma R, Swart WA, Lam TJ. Prevalence, prediction and risk factors of enteropathogens in normal and non-normal faeces of young Dutch dairy calves. Preventive Veterinary Medicine. 2010;93(2-3):162–169. doi: 10.1016/j.prevetmed.2009.09.020. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Beuttemmuller EA, Alfieri AF, Headley SA, Alfieri AA. Brazilian strain of bovine respiratory coronavirus is derived from dual enteric and respiratory tropism. Genetics and Molecular Research. 2017;16:2. doi: 10.4238/gmr16029580. [DOI] [PubMed] [Google Scholar]
- Bidokhti MR, Tråvén M, Ohlson A, Baule C, Hakhverdyan M, Belák S, Liu L, Alenius S. Tracing the transmission of bovine coronavirus infections in cattle herds based on S gene diversity. The Veterinary Journal. 2012;193(2):386–390. doi: 10.1016/j.tvjl.2011.12.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Boileau MJ, Kapil S. Bovine Coronavirus Associated Syndromes. Veterinary Clinics of North America: Food Animal Practice. 2010;26(1):123–146. doi: 10.1016/j.cvfa.2009.10.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bojkova D., Klann K., Koch B. Widera M., Krause D., Ciesek S., Cinatl J. and Münch C., 2020. Proteomics of SARS-CoV-2-infected host cells reveals therapy targets, Nature, 10.1038/s41586-020-2332-7 [DOI] [PMC free article] [PubMed]
- Castells M, Giannitti F, Caffarena RD, Casaux ML, Schild C, Castells D, Riet-Correa F, Victoria M, Parreño V, Colina R. Bovine coronavirus in Uruguay: genetic diversity, risk factors and transboundary introductions from neighboring countries. Archives of Virology. 2019;164(11):2715–2724. doi: 10.1007/s00705-019-04384-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Chigerwe M, Heller MC. Diagnosis and Treatment of Infectious Enteritis in Adult Ruminants. Veterinary Clinics of North America.Food Animal Practise. 2018;34(1):119–131. doi: 10.1016/j.cvfa.2017.10.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cho KO, Hasoksuz M, Nielsen PR, Chang KO, Lathrop S, Saif LJ. Cross-protection studies between respiratory and calf diarrhea and winter dysentery coronavirus strains in calves and RT-PCR and nested PCR for their detection. Archives of Virology. 2001;146(12):2401–2419. doi: 10.1007/s007050170011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cho KO, Hoet AE, Loerch SC, Wittum TE, Saif LJ. Evaluation of concurrent shedding of bovine coronavirus via the respiratory tract and enteric route in feedlot cattle. America Journal of Veterinary Research. 2001;62(9):1436–1441. doi: 10.2460/ajvr.2001.62.1436. [DOI] [PubMed] [Google Scholar]
- Coura FM, Freitas MD, Ribeiro J, de Leme RA, de Souza C, Alfieri AA, Facury Filho EJ, de Carvalho AÚ, Silva MX, Lage AP, Heinemann MB. Longitudinal study of Salmonella spp., diarrheagenic Escherichia coli, Rotavirus, and Coronavirus isolated from healthy and diarrheic calves in a Brazilian dairy herd. Tropical Animal Health and Production. 2015;47(1):3–11. doi: 10.1007/s11250-014-0675-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Crouch CF, Bielefeldt OH, Watts TC, Babiuk LA. Chronic shedding of bovine enteric coronavirus antigen-antibody complexes by clinically normal cows. Journal of General Virology. 1985;66(7):1489–1500. doi: 10.1099/0022-1317-66-7-1489. [DOI] [PubMed] [Google Scholar]
- de Groot R.J., Ziebuhr J., Poon L.L., Woo P.C., Talbot P., Rottier P.J.M., Holmes K.V., Baric R., Perlman S. and Enjuanes L., 2008. Revision of the Family Coronaviridae. Taxonomic Proposal of the Coronavirus Study Group to the ICTV Executive Committee. Available athttps://data.ictvonline.org/proposals/2008.085-122V.v4.Coronaviridae.pdf. Accessed on 6 Apr 2020
- Decaro N, Campolo M, Desario C, Cirone F, D’Abramo M, Lorusso E, Greco G, Mari V, Colaianni ML, Elia G, Martella V, Buonavoglia C. Respiratory disease associated with bovine coronavirus infection in cattle herds in Southern Italy. Journal of Veterinary Diagnostic Investigation. 2008;20(1):28–32. doi: 10.1177/104063870802000105. [DOI] [PubMed] [Google Scholar]
- Duan SM, Zhao XS, Wen RF, Huang JJ, Pi GH, Zhang SX, Han J, Bi SL, Ruan L, Dong XP, Research Team SARS. Stability of SARS coronavirus in human specimens and environment and its sensitivity to heating and UV irradiation. Biomedical and Environmental Sciences. 2003;16(3):246–255. [PubMed] [Google Scholar]
- El-Kanawati ZR, Tsunemitsu H, Smith DR, Saif LJ. Infection and cross-protection studies of winter dysentery and calf diarrhea bovine coronavirus strains in colostrum-deprived and gnotobiotic calves. American Journal of Veterinary Research. 1996;57:48–53. [PubMed] [Google Scholar]
- Ellis J. What is the evidence that bovine coronavirus is a biologically significant respiratory pathogen in cattle? Canadian Veterinary Journal. 2019;60(2):147–152. [PMC free article] [PubMed] [Google Scholar]
- Erles K, Toomey C, Brooks HW, Brownlie J. Detection of a group 2 coronavirus in dogs with canine infectious respiratory disease. Virology. 2003;310(2):216–223. doi: 10.1016/S0042-6822(03)00160-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Fukutomi T, Tsunemitsu H, Akashi H. Detection of bovine coronaviruses from adult cows with epizootic diarrhea and their antigenic and biological diversities. Archives of Virology. 1999;144:997–1006. doi: 10.1007/s007050050562. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gagea MI, Bateman KG, van Dreumel T, McEwen BJ, Carman S, Archambault M, Shanahan RA, Caswell JL. Diseases and pathogens associated with mortality in Ontario beef feedlots. Journal of Veterinary Diagnostic Investigation. 2006;18(1):18–28. doi: 10.1177/104063870601800104. [DOI] [PubMed] [Google Scholar]
- Geller C, Varbanov M, Duval RE. Human coronaviruses: insights into environmental resistance and its influence on the development of new antiseptic strategies. Viruses. 2012;4(11):3044–3068. doi: 10.3390/v4113044. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gomez DE, Weese JS. Viral enteritis in calves. Canadian Veterinary Journal. 2017;58(12):1267–1274. [PMC free article] [PubMed] [Google Scholar]
- Hasoksuz M, Lathrop SL, Gadfield KL, Saif LJ. Isolation of bovine respiratory coronaviruses from feedlot cattle and comparison of their biological and antigenic properties with bovine enteric coronaviruses. American Journal of Veterinary Research. 1999;60(10):1227–1233. [PubMed] [Google Scholar]
- Hasoksuz M, Sreevatsan S, Cho KO, Hoet AE, Saif LJ. Molecular analysis of the S1 subunit of the spike glycoprotein of respiratory and enteric bovine coronavirus isolates. Virus Research. 2002;84(1-2):101–109. doi: 10.1016/S0168-1702(02)00004-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Heckert RA, Saif LJ, Hoblet KH, Agnes AG. A longitudinal study of bovine coronavirus enteric and respiratory infections in dairy calves in two herds in Ohio. Veterinary Microbiology. 1990;22(2-3):187–201. doi: 10.1016/0378-1135(90)90106-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Heller MC, Chigerwe M. Diagnosis and Treatment of Infectious Enteritis in Neonatal and Juvenile Ruminants. Veterinary Clinics of North America.Food Animal Practise. 2018;34(1):101–117. doi: 10.1016/j.cvfa.2017.08.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Icen H, Arserim NB, Isik N, Özkan C, Kaya A. Prevalence of Four Enteropathogens with Immunochromatographic Rapid Test in the Feces of Diarrheic Calves in East and Southeast of Turkey. Pakistan Veterinary Journal. 2013;33(4):496–499. [Google Scholar]
- ICTV Master Species List 2019.v1. https://talk.ictvonline.org/files/master-species-lists/m/msl/9601/download Accessed on 6 Apr 2020
- Jactel B, Espinasse J, Viso M, Valiergue H. An Epidemiological Study Of Winter Dysentery In Fifteen Herds In France. Veterinary Research Communications. 1990;14(5):367–379. doi: 10.1007/BF00343215. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kalkanov I, Dinev I, Zarkov I. Etiological and pathomorphological investigations in calves with coronaviral pneumoenteritis. Macedonian Veterinary Review. 2019;42(1):43–49. [Google Scholar]
- Kanno T, Hatama S, Ishihara R, Uchida I. Molecular analysis of the S glycoprotein gene of bovine coronaviruses isolated in Japan from 1999 to 2006. Journal of General Virology. 2007;88:1218–1224. doi: 10.1099/vir.0.82635-0. [DOI] [PubMed] [Google Scholar]
- Kanno T, Ishihara R, Hatama S, Uchida I. A long-term animal experiment indicating persistent infection of bovine coronavirus in cattle. Journal of Veterinary Medical Science. 2018;80(7):1134–1137. doi: 10.1292/jvms.18-0050. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kleina D, Kernb A., Lapanc G., Benetkad V., Möstld K., Hassle A., and Baumgartner W., 2008. Evaluation of rapid assays for the detection of bovine coronavirus, rotavirus A and Cryptosporidium parvum in faecal samples of calves. The Veterinary Journal, 10.1016/j.tvjl.2008.07.016 [DOI] [PMC free article] [PubMed]
- Langpap TJ, Bergeland ME, Reed DE. Coronaviral enteritis of young calves: virologic and pathologic findings in naturally occurring infections. American Journal of Veterinary Research. 1979;40(10):1476–1478. [PubMed] [Google Scholar]
- Lathrop SL, Wittum TE, Brock KV, Loerch SC, Perino LJ, Bingham HR, McCollum FT, Saif LJ. Association between infection of the respiratory tract attributable to bovine coronavirus and health and growth performance of cattle in feedlots. American Journal of Veterinary Research. 2000;61(9):1062–1066. doi: 10.2460/ajvr.2000.61.1062. [DOI] [PubMed] [Google Scholar]
- Lin XQ, O’Reilly KL, Storz J, Purdy CW, Loan RW. Antibody responses to respiratory coronavirus infections of cattle during shipping fever pathogenesis. Archives of Virology. 2000;145:2335–2349. doi: 10.1007/s007050070024. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Martin SW, Nagy E, Shewen PE, Harland RJ. The association of titers to bovine coronavirus with treatment for bovine respiratory disease and weight gain in feedlot calves. Canadian Journal of Veterinary Research. 1998;62(4):257–261. [PMC free article] [PubMed] [Google Scholar]
- McNulty MS, Bryson DG, Allan GM, Logan EF. Coronavirus infection of the bovine respiratory tract. Veterinary Microbiology. 1984;9:425–434. doi: 10.1016/0378-1135(84)90063-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McVey DS. BRD research needs in the next 10-20 years. Animal Health Research Review. 2009;10(2):165–167. doi: 10.1017/S1466252309990247. [DOI] [PubMed] [Google Scholar]
- Mebus CA, Stair EL, Rhodes MB, Twiehaus MJ. Pathology of neonatal calf diarrhea induced by a coronavirus-like agent. Veterinary Pathology. 1973;10(1):45–64. doi: 10.1177/030098587301000105. [DOI] [PubMed] [Google Scholar]
- Natsuaki S, Goto K, Nakamura K, Yamada M, Ueo H, Komori T, Shirakawa H, Uchinuno Y. Fatal Winter Dysentery with Severe Anemia in An Adult Cow. Journal of Veterinary Medical Science. 2007;69(9):957–960. doi: 10.1292/jvms.69.957. [DOI] [PubMed] [Google Scholar]
- Oma VS, Tråvén M, Alenius S, Myrmel M, Stokstad M. Bovine coronavirus in naturally and experimentally exposed calves; viral shedding and the potential for transmission. Virology Journal. 2016;13:100. doi: 10.1186/s12985-016-0555-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Oma VS, Klem T, Traven M, Alenius S, Gjerset B, Myrmel M, Stokstad M. Temporary carriage of bovine coronavirus and bovine respiratory syncytial virus by fomites and human nasal mucosa after exposure to infected calves. BMC Veterinary Research. 2018;14(1):22. doi: 10.1186/s12917-018-1335-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Paller T., 2019. Aetiology of bovine respiratory disease complex in calves and young cattle, (PhD thesis, University of Ljubljana), http://knjiznica.vf.uni-lj.si/PortalGenerator/Document.aspx?id=250. Accessed 20 Apr 2020
- Paller T, Hostnik P, Pogačnik M, Toplak I. The prevalence of ten pathogens detected by a real-time PCR method in nasal swab samples collected from live cattle with respiratory disease. Slovenia veterinary research. 2017;54(3):101–107. [Google Scholar]
- Park SJ, Jeong C, Yoon SS, Choy HE, Saif LJ, Park SH, Kim YJ, Jeong JH, Park SI, Kim HH, Lee BJ, Cho HS, Kim SK, Kang MI, Cho KO. Detection and Characterization of Bovine Coronaviruses in Fecal Specimens of Adult Cattle with Diarrhea during the Warmer Seasons. Journal Of Clinical Microbiology. 2006;44(9):3178–3188. doi: 10.1128/JCM.02667-05. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Park SJ, Kim GY, Choy HE, Hong YJ, Saif LJ, Jeong JH, Park SI, Kim HH, Kim SK, Shin SS, Kang MI, Cho KO. Dual enteric and respiratory tropisms of winter dysentery bovine coronavirus in calves. Archives of Virology. 2007;152(10):1885–900. doi: 10.1007/s00705-007-1005-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Plummer PJ, Rohrbach BW, Daugherty RA, Daugherty RA, Thomas KV, Wilkes RP, Duggan FE, Kennedy MA. Effect of intranasal vaccination against bovine enteric coronavirus on the occurrence of respiratory tract disease in a commercial backgrounding feedlot. Journal of the American Veterinary Medical Association. 2004;225(5):726–731. doi: 10.2460/javma.2004.225.726. [DOI] [PubMed] [Google Scholar]
- Popova R, Zhang X. The Spike but Not the Hemagglutinin/Esterase Protein of Bovine Coronavirus Is Necessary and Sufficient for Viral Infection. Virology. 2002;294:222–236. doi: 10.1006/viro.2001.1307. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ribeiro J, Lorenzetti E, Alfieri AF, Alfieri AA. Molecular detection of bovine coronavirus in a diarrhea outbreak in pasture-feeding Nellore steers in southern Brazil. Tropical Animal Health and Production. 2016;48:649–653. doi: 10.1007/s11250-015-0975-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Saif LJ. Bovine Respiratory Coronavirus. Veterinary Clinics of North America: Food Animal Practice. 2010;26(2):349–364. doi: 10.1016/j.cvfa.2010.04.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Saif LJ, Heckert RA. Enteric coronaviruses. In: Saif LJ, Theft KW, editors. Viral diarrheas of man and animals. Boca Raton, Florida: CRC Press; 1990. pp. 185–252. [Google Scholar]
- Sattar SA, Springthorpe VS. Transmission of viral infections throughanimate and inanimate surfaces and infection control through chemical disin-fection. In: Hurst C, editor. Modeling Disease Transmission and Its Prevention by Disinfection. Cambridge, UK: Cambridge University Press; 1996. pp. 224–257. [Google Scholar]
- Sattar SA, Springthorpe VS, Karim Y, Loro P. Chemical disinfection of non-porous inanimate surfaces experimentally contaminated with four human pathogenic viruses. Epidemiology and Infection. 1989;102(3):493–505. doi: 10.1017/s0950268800030211. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sedda L, Rogers DJ. The influence of the wind in the Schmallenberg virus outbreak in Europe. Scientific reports. 2013;3:3361. doi: 10.1038/srep03361. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Singasa K, Songserm T, Lertwatcharasarakul P, Arunvipas P. Molecular and phylogenetic characterization of bovine coronavirus virus isolated from dairy cattle in Central Region, Thailand. Tropical Animal Health and Production. 2017;49(7):1523–1529. doi: 10.1007/s11250-017-1358-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Stokstad M., Klem T.B., Myrmel M., Oma V.S., Toftaker I., Østerås O. and Nødtvedt A., 2020. Using Biosecurity Measures to Combat Respiratory Disease in Cattle: The Norwegian Control Program for Bovine Respiratory Syncytial Virus and Bovine Coronavirus, Frontiers in Veterinary Science, 10.3389/fvets.2020.00167. Accessed on 9.4.2020 [DOI] [PMC free article] [PubMed]
- Storz J, Purdy CW, Lin X, Burrell M, Truax RE, Briggs RE, Frank GH, Loan RW. Isolation of respiratory bovine coronavirus, other cytocidal viruses, and Pasteurella spp from cattle involved in two natural outbreaks of shipping fever. Journal of the American Veterinary Medical Association. 2000;216(10):1599–1604. doi: 10.2460/javma.2000.216.1599. [DOI] [PubMed] [Google Scholar]
- Storz J, Lin X, Purdy CW, Chouljenko VN, Kousoulas KG, Enright FM, Gilmore WC, Briggs RE, Loan RW. Coronavirus and Pasteurella Infections in Bovine Shipping Fever Pneumonia and Evans’ Criteria for Causation. Journal of Clinical Microbiology. 2000;38(9):3291–3298. doi: 10.1128/jcm.38.9.3291-3298.2000. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Suzuki T, Otake Y, Uchimoto S, Hasebe A, Goto Y. Genomic Characterization and Phylogenetic Classification of Bovine Coronaviruses Through Whole Genome Sequence Analysis. Viruses. 2020;12(2):183. doi: 10.3390/v12020183. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Takahashi F, Akashi H, Inaba Y. Bovine Epizootic Diarrhea Resembling Winter Dysentery Caused by Bovine Coronavirus. Japan Agricultural Research Quarterly. 1983;17(3):185–190. [Google Scholar]
- Takamura K, Matsumoto Y, Shimizu Y. Field study of bovine coronavirus vaccine enriched with hemagglutinating antigen for winter dysentery in dairy cows. Canadian Journal of Veterinary Research. 2002;66(4):278–281. [PMC free article] [PubMed] [Google Scholar]
- Takiuchi E, Fernandes BA, Alfieri AF, Filippsen P, Alfieri AA. An Outbreak of Winter Dysentery Caused by Bovine Coronavirus in a High-Production Dairy Cattle Herd from a Tropical Country. Brazilian Archives of Biology and Technology. 2009;52:57–61. [Google Scholar]
- Thomas CJ, Hoet AE, Sreevatsan S, Wittum TE, Briggs RE, Duff GC, Saif LJ. Transmission of bovine coronavirus and serologic responses in feedlot calves under field conditions. American Journal of Veterinary Research. 2006;67(8):1412–1420. doi: 10.2460/ajvr.67.8.1412. [DOI] [PubMed] [Google Scholar]
- Toftaker I, Holmøy I, Nødtvedt A, Østerås O, Stokstad M. A cohort study of the effect of winter dysentery on herd-level milk production. Journal of Dairy Science. 2017;100:6483–6493. doi: 10.3168/jds.2017-12605. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tsunemitsu H, Saif LJ. Antigenic and biological comparisons of bovine coronaviruses derived from neonatal calf diarrhea and winter dysentery of adult cattle. Archives of Virology. 1995;140:1303–1311. doi: 10.1007/BF01322757. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Workman AM, Kuehn LA, McDaneld TG, Clawson ML, Loy JD. Longitudinal study of humoral immunity to bovine coronavirus, virus shedding, and treatment for bovine respiratory disease in pre-weaned beef calves. BMC Veterinary Research. 2019;15:161. doi: 10.1186/s12917-019-1887-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zhang X, Herbst W, Kousoulas KG, Storz J. Comparison of the S genes and the biological properties of respiratory and enteropathogenic bovine coronaviruses. Archives of Virology. 1994;134:421–426. doi: 10.1007/BF01310579. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zhang X, Hasoksuz M, Spiro D, Halpin R, Wang S, Vlasova A, Janies D, Jones LR, Ghedin E, Saif LJ. Quasispecies of bovine enteric and respiratory coronaviruses based on complete genome sequences and genetic changes after tissue culture adaptation. Virology. 2007;363(1):1–10. doi: 10.1016/j.virol.2007.03.018. [DOI] [PMC free article] [PubMed] [Google Scholar]