Abstract
Being rich in growth factors platelet rich fibrin (PRF) has been used for decades for its healing properties in cosmetic surgeries but its use in transcanal myringoplasty is a novel approach that remains unexplored. In todays era of minimally invasive surgery not only does it provide as a great alternative to conventional myringoplasty but also outshines it. It reduces post operative pain, hospital stay and unlike the conventional technique that uses termporalis fascia as a graft material, PRF myringoplasty if required can be reperformed on the same patient multiple times with minimal risk. This procedure comes as a boon for patients with recurrent graft defects because after multiple revision surgeries, temporalis fascia can be deficient and other graft materials like cartilage/perichondrium or fascia lata etc. have to be harvested surgically for myringoplasty. In PRF myringoplasty there is no upper limit in the number of times the PRF membrane can be made and also it does not entail any surgical incision for graft harvest. A prospective study involving 41 patients was conducted at Netaji Subhash Chandra Bose Medical College, Jabalpur where in the tympanic membrane perforations were repaired using PRF membrane with a successful outcome in 85.4% of the patients included in this study.
Keywords: Platelet rich fibrin, Chronic perforation, Myringoplasty
Introduction
Tympanic membrane (TM) perforations are amongst the common reasons, for which the patients attend ENT Clinics [1]. These perforations may be caused by middle ear infection (acute or chronic) or trauma in the form of instrumentation, slap, blast, accident, and sports injury or cut as a sequelae of tympanostomy tube insertion [2, 3]. Although 88% of traumatic perforations of any size heal without intervention, the remainders become chronic and require treatment [4]. If not treated surgically, then it may result in hearing loss, chronic otorrhea and cholesteatoma formation [5].
The most effective technique for surgical repair of tympanic membrane perforation include myringoplasty. Myringoplasty has been tried with various grafting materials to reconstruct the perforated tympanic membrane. Such grafting materials include skin, fascia, cartilage, vein, fat, perichondrium and duramater. Myringoplasty with temporalis fascia is considered the gold standard method for tympanic membrane closure. Though this method has > 90% closure rate but it is more time consuming and comparatively more complicated [6]. Thus some alternative techniques have been proposed to overcome the problems associated with myringoplasty with temporalis fascia.
The fat plug technique which consists of freshening the perforation edges and filling the perforation using fat plug obtained from ear lobule or from behind the ear, has been accepted as a good alternative for smaller perforations, with a closure rate of 80% to 90% [7–9]. Other alternative techniques include use of paper patches [10, 11] as an OPD procedure; plugging the ear drum with gel-foam after removal of ventilation tubes etc. [12]. Certain autogenous materials have positive effects on both the quantity and quality of wound healing i.e. they are cheaper, less invasive, and readily obtained [13, 14].
Use of platelet-rich fibrin (PRF) was first described by Choukroun et al. [15] in 2001. They were used in oral and maxillofacial surgery to improve bone healing in implant dentistry [15]. Platelet rich fibrin is composed of an assembly of a cytokines, glycemic chains, and structural glycoproteins enmeshed within a slowly polymerised fibrin network [16, 17]. These biochemical components aid in healing through synergistic mechanisms. PRF accelerates the cell proliferation and also offers inflammatory protection to grafts. Moreover, the advantage of PRF include ease of formation and manipulation during the surgical procedure [17]. As PRF membrane has a strong, elastic fibrin structure containing growth factors, it may be an ideal patching material in the treatment of tympanic membrane perforations.
Data regarding effect of PRF in repair of chronic tympanic membrane perforations is sparse and therefore the present study was conducted to evaluate the usage of PRF in repair of chronic tympanic membrane perforations.
Materials and Methods
The present study was conducted as a prospective observational study on 41 patients diagnosed with chronic tympanic membrane perforation at department of ENT, Netaji Subhash Chandra Bose Medical College & Hospital, Jabalpur (M.P.). The objectives of our study were as follows:-
To evaluate the success rate of the platelet rich fibrin membrane usage as a graft material in combination with surgical refreshening of the perforation margins for the repair of chronic tympanic membrane perforations of various sizes.
To compare the outcomes of technique of placement of PRF membrane for the closure of perforation i.e. overlay/underlay + overlay combined.
To compare the clinical factors influencing the successful closure of perforation between the successful and failure group of PRF myringoplasty
Inclusion and Exclusion Criteria
All patients with tympanic membrane perforations which were present for at least 6 months; without evidence of active chronic otitis media, cholesteatoma or retraction pocket formation (unsafe CSOM); without suspected ossicular pathology on microscopic examination were included in the study. Patients with history of previous middle ear surgery; nasopharyngeal or skull base pathology resulting in obvious eustachian tube dysfunction; history of radiation to head and neck region; or refusing platelet rich fibrin membrane grafting and choosing alternative treatment options were excluded from the study.
After obtaining ethical clearance from our Institute’s ethical committee, proper informed consent was obtained from all the participants. All the patients fulfilling the inclusion criteria were selected using purposive sampling during the study period of 6 months i.e. from 1st June 2019 to 31st November 2019. Detailed history regarding socio-demographic variables along with presenting complaints was obtained from all the study participants and entered in a pro-forma. Following this each patient was subjected to clinical examination and an otological examination. This was followed by an audiological assessment and then a microscopic examination. The size of the perforation was observed under an operating microscope and was classified into one of the four groups as per the SALIBA’s classification (Table 1).
Table 1.
Perforation size division according to SALIBA’S Classification
| Group | Perforation | Size in percent | TM quadrant affected | Image |
|---|---|---|---|---|
| I | Small | Less than 25% | Less than 1 Quadrant (Q) in size of TM |  |
| II | Medium | More than 25% but less than 50% | More than 1 Q size but less than 2 Q size | 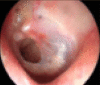 |
| III | Large | More than 50% but not total | More than 2 Q size but not total | 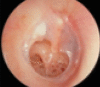 |
| IV | Total | 100% or total | Completely 4 Q size |  |
Preparation of Platelet Rich Fibrin
For preparation of Platelet rich fibrin, 10 ml blood sample was withdrawn from each patient using a sterile glass vacutainer just before the surgery. The sample was then centrifuged using a table top centrifuge at 3000 rpm for 15 min. Centrifugation thus resulted in the formation of a fibrin clot (platelet-rich fibrin) in the middle of the tube (between the RBC layer at the bottom and plasma at the top) (Fig. 1).
Fig. 1.
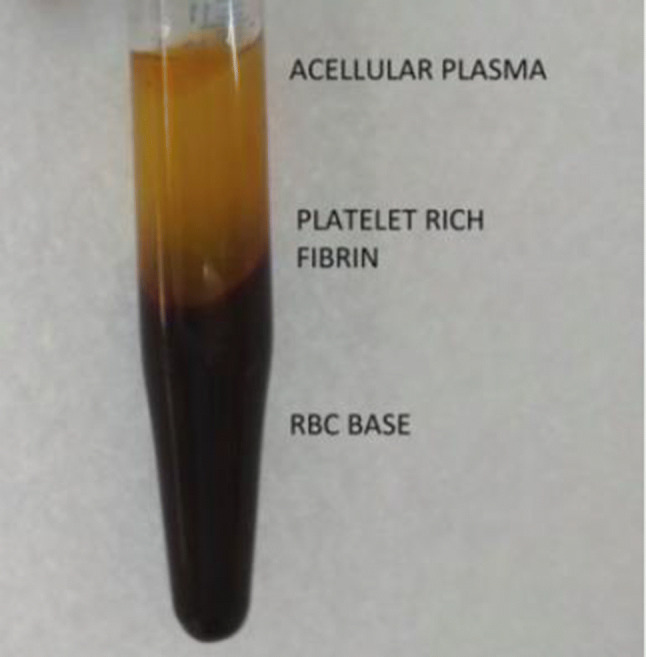
Post centrifugation separation of blood into its components
The plasma layer is deficient in platelets. Platelet rich fibrin was removed with sterile forceps from the sterile container and stripped from the adjacent red blood cell layer (Fig. 2). The blob of PRF was then placed between two glass slides and gently pressed for about three minutes (Figs. 3, 4). The exudate (PRF Serum) was carefully collected in another container for further usage in the soaking of ab-gels. Thus a thin membrane about the thickness of 1 mm, rich in fibrin from the matrix and with good tensile strength was obtained. The membrane was then cut according to the size of the perforation. Figure 5 shows comparison of PRF membrane before and after pressing whereas Fig. 6 shows final PRF membrane formed for usage during the procedure.
Fig. 2.

Separation of RBC layer from PRF blob
Fig. 3.
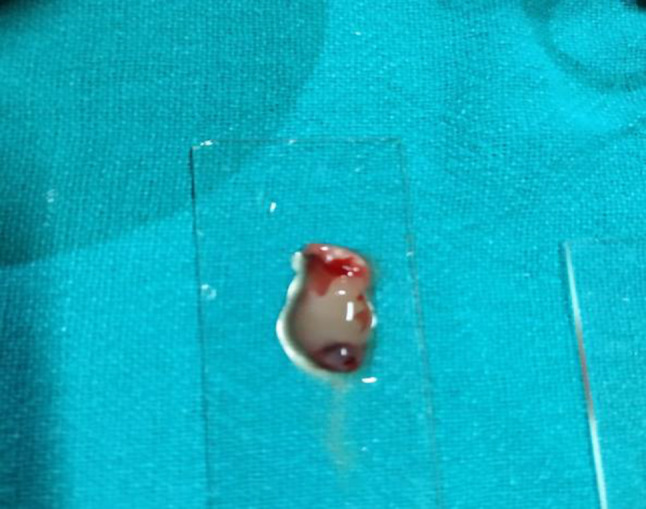
PRF blob retrieved and placed on a glass slide
Fig. 4.

PRF blob placed between two glass slides and compressed gently for 3 min
Fig. 5.

Comparison of PRF membrane before and after compression
Fig. 6.

Final PRF membrane formed as graft material for the procedure
All patients underwent surgery under an operating microscope. The external auditory canal was cleaned of cerumen, and local anaesthetic was applied to the four quadrants of the external ear canal using a 26 gauge syringe with 2% lidocaine with 1:100,000 epinephrine. A thin rim of the perforation was then carefully excised, de-epithelialised circumferentially and freshened using an angled pick or sickle knife and alligator micro ear forceps. Following this, gel-foam pieces soaked with antibiotic ciprofloxacin and PRF exudate (rich in growth factors) were placed into the middle ear through the perforation to support the PRF membrane in the cases of medium and large perforation. Two techniques were used for the repair of the perforations.
In technique-1, the underlay + overlay combination technique, the PRF membrane of adequate size is cut over a glass slide by a 15 number blade and carefully maneuvered microscopically to be placed just medial to the perforation and over the ab-gel bed. Care is taken to ensure that the margins of the perforation is in intimate contact with the underlay PRF membrane. Another PRF membrane approximately 2 mm larger in size than the size of the perforation is placed over the newly freshened perforation margins. The PRF membrane was overlapped carefully over all the intact epithelium edges around the perforation.
In technique-2, the overlay technique, all the steps were kept same except instead of placing a PRF membrane medial to the tympanic membrane perforation, only one PRF membrane of size about 1.5 times the size of perforation was placed laterally over the newly freshened perforation.
The PRF membrane was then covered with pieces of gel-foams soaked with antibiotic ciprofloxacin drops and the PRF exudate and the ear canal was filled with bacitracin ointment. A small pack soaked in bacitracin is placed over the lateral aspect of EAC. Patients were given instructions for its removal on the very next day. No other ear dressing was required. These gel-foam pieces were used to prevent the displacement of the PRF membrane and to support it from both sides. Patients were discharged immediately after the procedure and were instructed to keep their ears dry, avoid straining at stool, lifting heavy weights, to avoid air travel and to prevent nose-blowing for 1 month.
The patients were followed up between 1–3 months postoperatively. Hearing improvement was assessed using the audiogram results obtained preoperatively and at least 1–3 months postoperatively. Hearing parameters used were change in air–bone gap. Air–bone gap was calculated as the average difference between air conduction and bone conduction at 0.5, 1, 2 and 4 kHz. The first post-operative appointment was scheduled at 1 month or before in case of any complication.
Statistical Analysis
Data was compiled using MS Excel and analysed using SPSS 20. Data was grouped and expressed as frequency and percentage whereas numerical data was expressed as mean ± standard deviation. Appropriate statistical tests were applied and p < 0.05 were considered as statistically significant.
Results
The present study included a total of 41 patients with chronic tympanic membrane perforations fulfilling the inclusion criteria. Mean age of patients in the present study was 34.85 ± 10.91 years and maximum patients belonged to 21 to 30 and 31 to 40 years of age (29.3% each). About 51.2% patients in present study were females. The most common size of perforation was (MCP) medium central perforation observed in 56.1% cases followed by 26.9% cases with (SCP) small central perforation of unilateral side. Central followed by antero-inferior quadrant were the most commonly involved in 39% and 14.6% cases respectively. Mean duration of ear discharge in present study was 3.5 ± 2.2 years.
All the patients underwent surgical repair of tympanic membrane by closure of perforation using platelet rich fibrin membrane (Figs. 7, 8 and Table 2).
Fig. 7.

Image showing pre-operative tympanic membrane status with a central perforation
Fig. 8.

Image showing post-operative healed tympanic membrane status with graft uptake
Table 2.
Post-operative status of patients after 2 weeks of the procedure
| Post op findings | Frequency (n = 41) | Percentage |
|---|---|---|
| Post op membrane status | ||
| Intact | 35 | 85.4 |
| Perforation exists with discharge | 6 | 14.6 |
| Complications | ||
| None | 35 | 85.4 |
| Came back with discharge | 5 | 12.2 |
| Came back with otomycosis | 1 | 2.4 |
In present study, successful outcome was observed in 85.4% cases, whereas in 14.6% cases, perforation with discharge persisted post-operatively. Among them, 12.2% cases presented with discharge and 2.4% cases presented with otomycosis.
In present study, (Table 3) most common technique used was overlay and underlay and outcome were significantly better in cases in whom overlay and underlay technique was used (p < 0.05).
Table 3.
Association of successful outcome with intraoperative technique
| Intra op technique | Outcome | |||
|---|---|---|---|---|
| Success | Failure | |||
| Frequency | Percentage | Frequency | Percentage | |
| Overlay | 11 | 26.8 | 5 | 12.2 |
| Overlay and underlay | 24 | 58.5 | 1 | 2.4 |
p = 0.02
Table 4 presents findings of PTA pre-operatively and post-operatively, it was observed that post-operatively hearing loss significantly improved in both the ears (p < 0.001), however, post-operatively PTA could not be done in 14.6% cases.
Table 4.
Post-operative improvement in hearing status
| PTA | Right ear | Left ear | ||
|---|---|---|---|---|
| Pre Op | Post Op | Pre Op | Post Op | |
| Mild HL | 3 (7.3) | 3 (7.3) | 2 (4.9) | 0 (0) |
| Mild CHL | 9 (22) | 5 (12.2) | 11 (26.8) | 10 (24.4) |
| Minimal HL | 11 (26.8) | 13 (31.7) | 4 (9.8) | 9 (22) |
| Minimal CHL | 0 (0) | 0 (0) | 1 (2.4) | 1 (2.4) |
| Moderate HL | 1 (2.4) | 1 (2.4) | 0 (0) | 0 (0) |
| Moderate CHL | 8 (19.5) | 5 (12.2) | 3 (7.3) | 1 (2.4) |
| Moderate mixed HL | 0 (0) | 2 (4.9) | 3 (7.3) | 3 (7.3) |
| Moderate severe mixed HL | 1 (2.4) | 1 (2.4) | 1 (2.4) | 2 (4.9) |
| Moderate severe SNHL | 0 (0) | 0 (0) | 1 (2.4) | 0 (0) |
| WNL | 5 (12.2) | 5 (12.2) | 15 (36.6) | 9 (22) |
| Could not be done | 0 (0) | 6 (14.6) | 0 (0) | 6 (14.6) |
| p value | 0.001 | 0.001 | ||
The present study documented unsuccessful outcome in 6 cases, and no statistically significant association was observed for baseline variables such as age, gender, size and location of perforation with outcome (p > 0.05). Ossicular involvement was observed in none of the patients in the present study. However, the present study observed no statistical association of outcome with clinical features (p > 0.05).
Discussion
Myringoplasty involves repair of tympanic membrane perforation with an autologous graft. Platelet rich fibrin membrane was used in the present study during transcanal myringoplasty to close the perforations. The platelet rich fibrin membrane acts by releasing multiple growth factors. These growth factors include connective tissue growth factor (CTGF), fibroblast growth factor-2 (FGF-2), bone morphogenetic protein (BMP-2), and transforming growth factor-beta 2 (TGF-β2). These factors once released play an important role in cell proliferation and thus aid in healing [18]. Of course, it also acts as a scaffolding for the epithelial layers to grow on both sides of the PRF graft. Platelet rich fibrin has been used with good success rate and minimal complications in cases of traumatic and acute perforations, however, in this study we tried to assess the role of PRF membrane in closure of chronic tympanic membrane perforations. The present study included 41 patients with mean age of 34.85 ± 10.91 years. Majority of patients belonged to 21 to 40 years of age and male to female sex ratio was 0.95.
Successful closure with intact tympanic membrane was observed in 85.4% cases in the present study, however, post-operative discharge persisted in 12.2% of cases in this study. Gür et al. in their comparative study compared the closure rate, speed of healing, and hearing gain in patients of traumatic tympanic membrane. They randomly allocated the patients in two groups i.e. patients of group 1 were managed using PRF whereas that of group 2 were managed using paper patch. They documented closure of perforation in 93% cases using PRF whereas in another group using paper patch, the closure rate obtained was 83%. On day 10, full closure of the TM was observed in 24 (80%) patients in PRF Group and 16 (53%) patients in paper patch group (p < 0.05) [19].
Kumar [2] reported relatively higher success rate of 92% as compared to present study (85.4%). The observed difference could be due to the difference in cause of perforations i.e. in reference study PRF was conducted for traumatic perforations whereas in present study, PRF was used for chronic perforations.
The present study documented statistically significant association of outcome with intraoperative technique, whereas no such association was observed with size as well as location of perforation. Sengupta et al. in their study compared the outcome of overlay, underlay and combined techniques in myringoplasty and documented overall success rates among underlay, overlay and combined to be 81.25, 85.71 and 90% [20].
Failure rates in present study were significantly higher in patients with deviated nasal septum and grade 2 and 3 tonsillar hypertrophy (p < 0.05). This could depend on exaggerated antigenic stimulation and tonsils may be the reservoirs of pathogenic organisms, maintaining chronic hyper-stimulation of immune response. However Nair et al. documented 100% graft uptake using platelet rich fibrin even in presence of middle ear inflammation. Also they concluded that platelet rich fibrin increased the chances of graft uptake even in larger perforations [21].
Habesoglu et al. [22] in their study on closure of acute tympanic perforations concluded that the use of platelet-rich fibrin accelerates the tympanic membrane closure.
Garin et al. [23] also observed good safety of platelet rich fibrin without any adverse effect in middle ear packing.
The advantages of platelet rich fibrin include its easy preparation; as platelet rich fibrin is autologous, the chances of immunogenic reaction, disease transmission and graft failure are minimal. As PRF can be prepared any number of times so there is virtually unlimited graft material available for repeat surgeries and even in the surgeries which failed after the usage of temporalis fascia. It is inexpensive and can be used as an OPD procedure [23, 24]. PRF myringoplasty doesn’t require any incision and therefore patient morbidity is minimum. It can be taken as the first procedure for the closure of tympanic membrane perforation before any more invasive tympanoplasty procedure is attempted. Growth factors released by PRF acts for extended duration i.e. up to 7 days or more. Also slow polymerisation and remodeling of the fibrin matrix within PRF effectively sustains growth factors and other critical cells and thus aids in healing [25].
Conclusions
Transcanal Myringoplasty with platelet rich fibrin can be used as an effective day care procedure for patients presenting with chronic perforations of tympanic membrane. Management of chronic perforations with platelet rich fibrin is associated with significant improvement in hearing, good success rate (85.4%) and minimal complications.
Further studies are required to assess efficacy of PRF in cases of chronic large and subtotal perforations of the tympanic membrane.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Contributor Information
Anirudh Shukla, Email: anirudhshukla@outlook.com.
Yogesh Singh Kaurav, Email: yskaurav@gmail.com.
References
- 1.Seddik Abd El-Gelil A, Mohamed Dawod Y. Effect of platelet rich plasma-enriched gelfoam on chronic tympanic membrane perforation. Al-Azhar Med J. 2020;49(1):173–180. [Google Scholar]
- 2.Kumar RD. Application of platelet rich fibrin matrix to repair traumatic tympanic membrane perforations: a pilot study. Indian J Otolaryngol Head Neck Surg. 2019;71(2):1126–1134. doi: 10.1007/s12070-017-1239-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Sinkkonen ST, Jero J, Aarnisalo AA. Tympanic membrane perforation. Duodecim; laaketieteellinen aikakauskirja. 2014;130(8):810–818. [PubMed] [Google Scholar]
- 4.Amoils CP, Jackler RK, Lustig LR. Repair of chronic tympanic membrane perforations using epidermal growth factor. Otolaryngol Head Neck Surg. 1992;107(5):669–683. doi: 10.1177/019459989210700509. [DOI] [PubMed] [Google Scholar]
- 5.Imamoglu M, Isik AU, Acuner O, Harova G, Bahadir O. Fat-plug and paper-patch myringoplasty in rats. J Otolaryngol Head Neck Surg. 1998;27(6):318. [PubMed] [Google Scholar]
- 6.Zaman A, Omar S. Myringoplasty using temporalis fascia and its clinical outcome. Int J Otorhinolaryngol Head Neck Surg. 2019;5(6):1539. doi: 10.18203/issn.2454-5929.ijohns20194162. [DOI] [Google Scholar]
- 7.Ringenberg JC. Fat graft tympanoplasty. Laryngoscope. 1962;72(2):188–192. doi: 10.1288/00005537-196202000-00005. [DOI] [PubMed] [Google Scholar]
- 8.Mitchell RB, Pereira KD, Lazar RH. Fat graft myringoplasty in children—a safe and successful day-stay procedure. J Laryngol Otol. 1997;111(2):106–108. doi: 10.1017/S002221510013659X. [DOI] [PubMed] [Google Scholar]
- 9.Landsberg R, Fishman G, DeRowe A, Berco E, Berger G. Fat graft myringoplasty: results of a long-term follow-up. J Otolaryngol. 2006;35(1):44–47. doi: 10.2310/7070.2005.4124. [DOI] [PubMed] [Google Scholar]
- 10.Golz A, Goldenberg D, Netzer A, Fradis M, Westerman ST, Westerman LM, Joachims HZ. Paper patching for chronic tympanic membrane perforations. Otolaryngol Head Neck Surg. 2003;128(4):565–570. doi: 10.1016/S0194-5998(03)00124-4. [DOI] [PubMed] [Google Scholar]
- 11.Dursun E, Dogru S, Gungor A, Cincik H, Poyrazoglu E, Ozdemir T. Comparison of paper-patch, fat, and perichondrium myringoplasty in repair of small tympanic membrane perforations. Otolaryngol Head Neck Surg. 2008;138(3):353–356. doi: 10.1016/j.otohns.2008.01.003. [DOI] [PubMed] [Google Scholar]
- 12.Puterman M, Leiberman A. Gelfoam plug tympanostomy concomitant with removal of retained ventilation tubes. Int J Pediatr Otorhinolaryngol. 2005;69:57–60. doi: 10.1016/j.ijporl.2004.08.001. [DOI] [PubMed] [Google Scholar]
- 13.Lou ZC, He JG. A randomised controlled trial comparing spon- taneous healing, gelfoam patching and edge-approximation plus gelfoam patching in traumatic tympanic membrane perforation with inverted or everted edges. Clin Otolaryngol. 2011;36:221–226. doi: 10.1111/j.1749-4486.2011.02319.x. [DOI] [PubMed] [Google Scholar]
- 14.Park MK, Kim KH, Lee JD, Lee BD. Repair of large traumatic tympanic membrane perforation with a Steri-strips patch. Otolaryngol Head Neck Surg. 2011;145:581–585. doi: 10.1177/0194599811409836. [DOI] [PubMed] [Google Scholar]
- 15.Choukroun J, Adda F, Schoeffler C, Vervelle A. Une opportunité en paro-implantologie: le PRF. Implantodontie. 2001;42:55–62. [Google Scholar]
- 16.Dohan DM, Choukroun J, Diss A, Dohan SL, Dohan AJ, Mouhyi J, et al. Platelet-rich fibrin (PRF): a second-generation platelet concentrate. Part II: Platelet-related biologic features. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101:e45–e50. doi: 10.1016/j.tripleo.2005.07.009. [DOI] [PubMed] [Google Scholar]
- 17.Dohan DM, Rasmusson L, Albrektsson T. Classification of plate- let concentrates from pure platelet-rich plasma (P-PRP) to leucocyte and platelet-rich fibrin (L-PRF) Trends Biotechnol. 2009;27:158–167. doi: 10.1016/j.tibtech.2008.11.009. [DOI] [PubMed] [Google Scholar]
- 18.Tang XB, Dong PL, Wang J, Zhou HY, Zhang HX, Wang SZ. Effect of autologous platelet-rich plasma on the chondrogenic differentiation of rabbit adipose-derived stem cells in vitro. Exp Therap Med. 2015;10(2):477–483. doi: 10.3892/etm.2015.2528. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Gür ÖE, Ensari N, Öztürk MT, Boztepe OF, Gün T, Selçuk ÖT, Renda L. Use of a platelet-rich fibrin membrane to repair traumatic tympanic membrane perforations: a comparative study. Acta Oto-laryngol. 2016;136(10):1017–1023. doi: 10.1080/00016489.2016.1183042. [DOI] [PubMed] [Google Scholar]
- 20.Sengupta A, Basak B, Ghosh D, Basu D, Adhikari D, Maity K. A study on outcome of underlay, overlay and combined techniques of myringoplasty. Indian J Otolaryngol Head Neck Surg. 2012;64(1):63–66. doi: 10.1007/s12070-011-0257-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Nair NP, Alexander A, Abhishekh B, Hegde JS, Ganesan S, Saxena SK. Safety and efficacy of autologous platelet-rich fibrin on graft uptake in myringoplasty: a randomized controlled trial. Int Arch Otorhinolaryngol. 2019;23(01):077–082. doi: 10.1055/s-0038-1649495. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Habesoglu M, Oysu C, Sahin S, Sahin-Yilmaz A, Korkmaz D, Tosun A, Karaaslan A. Platelet-rich fibrin plays a role on healing of acute-traumatic ear drum perforation. J Craniofac Surg. 2014;25(6):2056–2058. doi: 10.1097/SCS.0000000000001140. [DOI] [PubMed] [Google Scholar]
- 23.Garin P, Mullier F, Gheldof D, Dogne JM, Putz L, Van Damme JP. Platelet-rich fibrin (PRF): an autologous packing material for middle ear microsurgery. B-ENT. 2014;10(01):27–34. [PubMed] [Google Scholar]
- 24.Sharma D, Mohindroo S, Azad RK. Efficacy of platelet rich fibrin in myringoplasty. Int J Otorhinolaryngol Head Neck Surg. 2018;4:677–681. doi: 10.18203/issn.2454-5929.ijohns20181670. [DOI] [Google Scholar]
- 25.Karimi K, Rockwell H. The benefits of platelet-rich fibrin. Facial Plast Surg Clin. 2019;27(3):331–340. doi: 10.1016/j.fsc.2019.03.005. [DOI] [PubMed] [Google Scholar]


