Abstract
There are an increasing number of children who are dependent on medical technology to sustain their lives. Although significant research on this issue is taking place, the terminology used is variable and the concept of technology dependence is ill-defined. A systematic concept analysis was conducted examining the attributes, antecedents, and consequences of the concept of technology dependent, as portrayed in the literature. We found that this concept refers to a wide range of clinical technology to support biological functioning across a dependency continuum, for a range of clinical conditions. It is commonly initiated within a complex biopsychosocial context and has wide ranging sequelae for the child and family, and health and social care delivery.
Conclusion: The term technology dependent is increasingly redundant. It objectifies a heterogenous group of children who are assisted by a myriad of technology and who adapt to, and function with, this assistance in numerous ways.
|
What is Known: • There are an increasing number of children who require medical technology to sustain their life, commonly referred to as technology dependent. This concept analysis critically analyses the relevance of the term technology dependent which is in use for over 30 years. | |
|
What is New: • Technology dependency refers to a wide range of clinical technology to support biological functioning across a dependency continuum, for a range of clinical conditions. It is commonly initiated within a complex biopsychosocial context and has wide-ranging sequelae for the child and family, and health and social care delivery. • The paper shows that the term technology dependent is generally portrayed in the literature in a problem-focused manner. • This term is increasingly redundant and does not serve the heterogenous group of children who are assisted by a myriad of technology and who adapt to, and function with, this assistance in numerous ways. More appropriate child-centred terminology will be determined within the TechChild project. |
Keywords: Child, Complex needs, Concept analysis, Family, Technology dependence
Introduction
There are an increasing number of children who require medical technology to sustain their life [1–4] and, in response, an expanding array of medical technology available. This paper analyses the concept of ‘technology dependent’, the term commonly used to refer to these children. The current prevalence and rate of increase in the number of children who are technology dependent is difficult to determine as they depend on a number of interrelated factors including: the prevalence of particular conditions; medical and surgical interventions chosen; and finance and policies for care delivery across and within countries [5–7]. The term technology dependent stems primarily from the phrase ‘technology dependence’ which was coined 30 years ago by the Office of Technology Assessment (US) [8], describing ‘a medical device to compensate for the loss of a vital body function and substantial ongoing nursing care to avert death or further disability’. To the best of our knowledge, this is the first systematic concept analysis to examine the contemporary relevance and utility of this terminology as it is currently portrayed in the literature. This is important for two key reasons: the array of medical technology now available means that the broad term of ‘technology dependent’ has the potential to conjure up a multitude of clinical scenarios; and the objectifying nomenclature does not reflect a child-centric approach. This paper is part of a larger body of research, the TechChild project, funded by the European Research Council. The purpose of this research is to explore influences on the initiation of technology dependence required to sustain a child’s life and to identify more appropriate child-centred terminology in an evidenced-based manner.
An evolutionary concept analysis was employed as it seeks to examine the cluster of key characteristics that through common use, collectively form the real definition of a concept [9]. According to Rodgers [9], it is necessary to understand the antecedents (phenomena usually found prior to concept occurrence), the attributes of the concept, and the consequences that follow as a result. Without a clear conceptual foundation, there is an ambiguity which in turn can compromise the quality of research or theory construction as the area develops [10].
Methods
Rodgers’ evolutionary method [9] was used to systematically analyse the concept of technology dependence in the scientific literature. This method is particularly well suited to this issue given the changing and dynamic nature of advances in medical technology. Alternative approaches to concept analysis are founded in a realist paradigm, in which a reductionist approach focuses on defining a concept as a static entity. Rodgers’ relativist stance, in comparison, seeks to identify how a concept is portrayed in the literature using an inductive approach, while acknowledging that any understanding of a concept is evolutionary as it is influenced by dynamic contextual factors, which may be disciplinary, cultural, or theoretical [9]. Rodgers’ approach to concept analysis includes a set of core activities, which can be carried out simultaneously and not necessarily in a linear manner (Table 1). Analysis seeks to identify what is common, the purpose of which is to identify data that is relevant to the attributes of the concept and its contextual features. Thematic analysis identifies major themes presented in the literature.
Table 1.
Rodgers’ approach to concept analysis
| Activities | |
|---|---|
| 1. | Identify the concept of interest and associated expressions (including surrogate terms) |
| 2. | Identify and select an appropriate realm for data collection |
| 3. | Collect relevant data |
| 4. | Analyse the data |
| 5. | Identify an exemplar of the concept, if appropriate |
| 6. | Identify implications, hypotheses, and implications for further development of the concept |
Data sources and search strategy
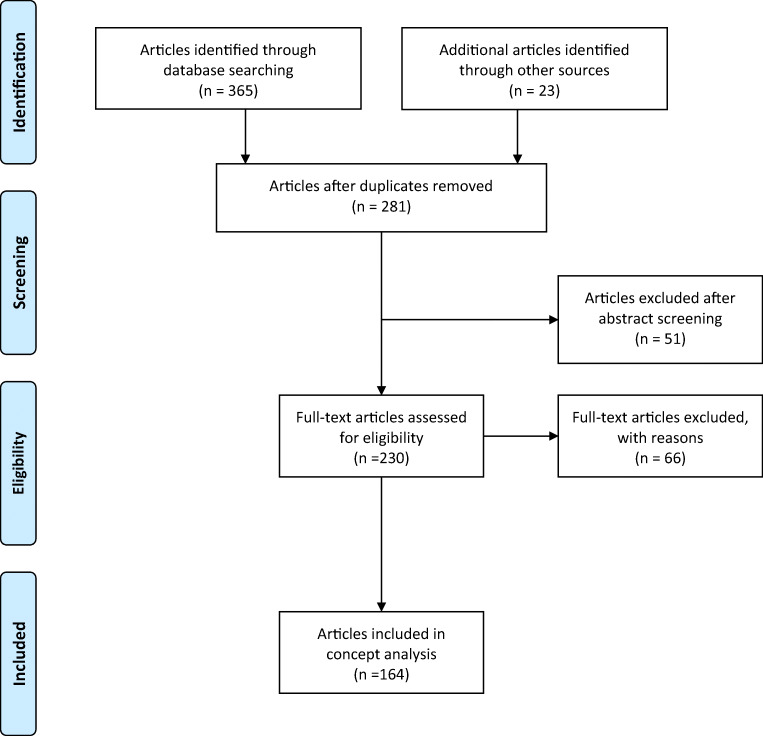
A three-strand approach was used to create a systematic search. An initial scoping search was run in PubMed and CINAHL to identify appropriate control language using MeSH and CINAHL headings. Control language is the language of the topic established at the start of a systematic search, against which other terms which emerge are mapped against. This includes developing a list of synonyms and consideration of reference and non-reference words for the search. A secondary scoping search was then conducted identifying appropriate keywords related to the following: technology dependence, technology dependent, complex care needs, complex medical care needs, complex healthcare needs, children with special healthcare needs, medically fragile, and medically complex children. The final search was run in PubMed, CINAHL, and PsycINFO using a combination of the keywords and control language. The search was limited to English-language literature published over the last 30 years up to the 31st of December 2019. The reference lists of the resulting articles were reviewed to identify any other pertinent articles. An additional hand search was conducted and a grey literature search was completed using OpenGrey, the Systems for Information on Grey literature in Europe (SIGLE), World Health Organization (WHO), National Technical Information Service USA (NTIS), and the National Academies Press. (Fig. 1) Duplicate articles were removed from the search and the remaining abstracts and full texts were reviewed to ensure they included reference to technology dependence. Those that did not meet these criteria were not included in the concept analysis.
Fig. 1.
Data search and selection process
Data extraction and analysis
The majority of the 164 articles identified were from North America and Europe and the majority of papers are from the last 10 years, reflecting the growing population of children requiring technology to sustain their lives. Each of the articles was analysed for data relevant to the (1) attributes, (2) antecedents, and (3) consequences of a child’s dependence on medical technology to sustain life using a coding framework based on Rodgers’ evolutionary method (Table 2). To guide the data analysis process, a set of specific questions were formulated for each category of data set out by Rodgers (Table 3) [9]. It was important to develop a framework specific to the topic of this concept analysis to ensure a clear focus on the specific areas of interest in the review of the literature. The framework was reviewed by MBr and DA, who then organised recurring themes into each category (attributes, antecedents, and consequences) (Fig. 2). In this way, the structure of the findings below is based on these three categories set out by Rodgers [9].
Table 2.
Coding framework based on Rodgers’ evolutionary method
| Number | Question |
|---|---|
| 1. | What are the key attributes of a child’s dependence on medical technology? |
| 2. | Which factors (antecedents) are proposed to precede technology dependence? |
| 3. | What are the consequences of a child’s dependence on medical technology? |
Table 3.
Guiding questions used during the data analysis phase
| Category | Guiding question |
|---|---|
| Surrogate terms |
What other words say the same thing? Is this word/term referring to technology dependence? |
| Related concepts | Does this term bear any relationship to technology dependence? |
| Attributes |
What are the characteristics of technology dependence, as outlined in this paper? What is the author discussing/describing? |
| Antecedents |
What is happening when technology dependence is initiated? What happens before technology dependence is initiated? |
| Consequences |
What happens after technology dependence is initiated? What happens as a result of technology dependence? |
Fig. 2.
Key characteristics of the attributes, antecedents, and consequences of technology dependence required to sustain a child’s life
Findings
Key attributes of technology dependence required to sustain a child’s life
Synthesis of themes from the literature identified key attributes of technology dependence in children to sustain their lives as heterogenous with a dependency continuum.
Heterogenous
Clinical technological dependence in children spanned a wide range of support for multiple human systems. They included oxygen support, invasive and non-invasive mechanical ventilation, pacemaker, implantable cardioverter defibrillators (ICD), ventricular drains, intravenous drugs, intravenous nutrition, gastrostomy or jejunostomy, ileostomy, colostomy, urethral catheterisation, and dialysis [7, 11–17]. We found that the majority of papers referred to children who were technology dependent as children who predominantly required respiratory or cardiac support in addition to requiring additional technological supports to support their wider clinical care needs including nutrition and gastrointestinal function.
Dependency continuum
The length of time a child may be dependent on clinical technology to sustain their life can vary, depending on the range and severity of their illness. Children may be dependent on a single device or multiple devices for a defined period, or they may be dependent on clinical technology for a longer period of time, depending on the complexity of their clinical presentation [12, 18]. Some children have the potential of being increasingly technology dependent as their illness progresses, depending on their comorbidities [19–25]. This often emerged in the literature related to specific care transitions including from hospital to home [26–33] and moving from children’s services to adult services [32, 34–37].
Antecedents of technology dependence required to sustain a child’s life
The conceptual analysis identified four domains regarding antecedents of technology dependence: clinical characteristics of the child, physician perspectives, the developing autonomy of the child, and parental engagement.
Clinical characteristics of the child
Specific foreground clinical characteristics which may lead to the initiation of technology dependence are identified in the literature. This includes genetic disorders, congenital disorders, issues related to prematurity or perinatal trauma, acquired external causes such as neoplasia, near drowning or trauma, following prolonged resuscitation, perisurgical anoxia, accidental suffocation, renal failure, and degenerative neurological conditions [11, 13, 24, 38–40].
Physician perspectives
The impact of different physician perspectives on care delivery is evident in the literature [38]. Some suggestions for varieties in perspectives include prognostic uncertainty and varying perspectives on the meaning of death of a child in their care [41, 42]. The estimation of prognosis is a significant factor when technology dependence is initiated [43–46]. Where there is prognostic uncertainty, this may be compounded by consideration of the potential opportunities that may emerge with future medical technological advances [17]. On the other hand, physicians who are over pessimistic in their prognostication may not offer hope for survival [47]. It has been suggested that varying perspectives on the initiation of technology dependence may be related to physicians’ views of death; for example, one study review showed that 68% of physicians regarded their patients’ deaths as a personal failure [48].
Developing autonomy of the child
Care delivery to children is unique in that those receiving care are developmentally dynamic and the autonomy of those receiving care must be considered [49–57]. A predominant paternalistic stance is evident in that much of the literature in this area focuses on the perspectives of the clinical team or the parents and there is evidence that children are often excluded from the decision-making process [58, 59]. This may be explained by a priori beliefs of the value of a child’s opinion or on limited belief of the importance of the chronological age or developing abilities of children as they age [60, 61]. Literature that espouses increased autonomy of the child in decision-making argues that it can increase the child’s trust and enhance the child-physician relationship [54, 55, 57, 62–66].
Parental engagement
The concept analysis found multiple concurrent issues that affect parents when technology dependence is initiated for their child. Parents may be influenced by previous experiences, for example if they have another child with a similar condition, how they experienced the care of that child and whether that child is still alive or has died [39]. They may also be so consumed by their immediate concerns for the child’s survival that they may not fully understand the options available for their child’s care [39, 67, 68]. The literature is replete with stressors of the parents at such critical junctures in care delivery including a feeling of lack of control over the ongoing instability of the child, insomnia, poor diet, and exhaustion [69].
A number of potential organisational challenges were also identified, including the potential for miscommunication of information to parents when more than one clinical team is involved [70, 71]; influences of organisational culture on the degree of choice parents can exercise and the power dynamic between the parent/child and physician in decision making [72]; and coercion or pressure put on parents to make quick decisions when decisions are time-sensitive, which can limit the level of communication and engagement to support parents [39]. Supportive measures identified for parents during this time include having a dedicated coordinator to manage the various care communications; this could facilitate more thorough communication of decisions around care delivery and lead to more informed conversations engendering greater trust with families [17, 73].
Consequences of technology dependence required to sustain a child’s life
Finally, the consequences of the concept were identified. These are the factors (consequences) that provide biopsychosocial context beyond the initiation of technology dependence to sustain a child’s life and the phenomena that occur consequently. The conceptual analysis identified four domains of consequence of the initiation of technology dependence: clinical care of the child; psychosocial sequelae for the child; family adaptation; and ongoing impact for health and social care.
Clinical care of the child
A literature review identified multiple issues specific to the clinical care of a child who is dependent on technology to sustain their life. They can have frequent clinic visits, are frequently hospitalised, and have a high risk of critical illness [5–7, 74–76]. These children also have more visits to the Emergency Department than a well child [14, 75, 77–79]. This rate of attendance is often higher than the rates of attendance of elderly patients over 85 years of age [75]. Higher rates of visits are associated with greater distance from the hospital and being a younger child and having a large number of medications [24, 80–82]. Children who are technology dependent may have longer stays in PICU, they are more likely to be readmitted to a PICU during a hospital stay, new morbidities often emerge following admission and readmission to PICU, and they are more likely to die after a prolonged stay in PICU than a child with an acute illness [5, 6, 83–85]. Other clinical issues can include device-related complications; for example, for a child who has an ICD, this may include lead dysfunction, risk of infection, and/or battery depletion [86].
Psychosocial sequelae for the child
There was limited attention paid in the literature to the psychological sequelae for a child who is technology dependent. Protective factors against negative psychological sequelae for children assisted by technology include higher cognitive functioning of the child and greater social functioning of the parents [87, 88]. Some-illness specific issues were found. For example, where low health-related quality of life (HRQoL) was found for children who were technology dependent, the lowest scores were found for children who were technology dependent and also had a neurological impairment [88]. In addition, children who had ICDs were found to have a high potential for anxiety, depression, and post-traumatic stress disorder [16, 89, 90] and overall children with pacemakers were found to have lower HRQoL scores than other children with chronic cardiac disease who were not dependent on a rhythm device [91]. It was also found that females and non-Caucasian children living with an ICD had higher prevalence of anxiety and depressive disorders than other children living with the same device [89, 92].
Family adaptation
The adaptation of a child’s family to their technology dependence is well documented for children living assisted with respiratory support, though much less so for other technology. The stress of moving out of PICU and the realignment of care expectations has been identified as a period of significant stress for parents [71]. General concerns when planning to move to home includes parents’ stress about becoming a clinician in the home and stress about the potential for equipment malfunction [24, 68, 71, 93–107]. Specific challenges identified include grieving for a well child [71]; learning to master care delivery in a variety of settings [108]; guilt over having less time with the other children at home or relying on them for assistance in care giving [109]; causing pain to their child when carrying out clinical procedures [109–112]; concern over sleep disturbance [108, 113]; and difficulty accessing and delivering a large number of medications [24].
A number of papers highlight how parents obtain a sense of control as they adapt their role as primary care givers of a child who is technology dependent. This includes focusing on becoming an expert carer, focusing on the child’s achievements, and the importance of their spirituality or religion to help them cope [102, 114]. Resilience training has been found to have a positive effect on parents’ ability to cope [115]. However, while parents often become very good clinical problem solvers [112], they have identified specific areas for greater support when planning for discharge. This includes support for ongoing self-directed learning once they are at home, greater support to deal with the myriad of financial concerns, and greater flexibility in the level and amount of care delivery made available to them [71, 101, 105–107, 116]. The impact on siblings adapting to living with a child who is technology dependent is increasingly being documented in the literature. This includes a focus on the positive aspects of adaption such as the development of a strong attachment and having protective tendencies towards their sibling [117]. Negative aspects have also been identified, including a risk of isolation, missing out on social and family events, and risk of psychological distress as the family adapts to a new way of being [117–119]. Earlier papers on this topic urged caution over placing extraordinary burdens on parents and families by the introduction of life-sustaining technology in the home [120]. More recently, there is a very clear impetus internationally to encourage care of the child as close to home as possible and preferably in the home [121, 122].
Ongoing impact for health and social care
The variety of challenges for health and social care delivery, related to the increasing number of children who require technology to sustain their lives, are well documented in the literature. This includes challenges in the development of integrated care for this cohort of children and co-creation of integrated care with children and their families [106, 107, 113, 123]. Care delivery across acute and community care services can be complicated by inconsistent standards for discharge to home [107, 124–127]. Specific areas that could enhance care delivery include enhanced access to specialist care, including same-day appointments to appropriately trained physicians in the community [80, 128, 129]; increased use of telehealth, electronic records, and patient summaries [130, 131]; specialist home care visits in the initial week following discharge to home [81]; and increased access to respite care in and out of the home [103, 113, 130–136]. Access to, and governance of, appropriately trained nurses is identified as an ongoing challenge as this population of children grows [5, 35]. Specifically, there is an increasing call for advanced practice nurses across various healthcare sectors to care for children who are technology dependent [88, 103, 135–137] and the need for an increased number of school nurses to support access to education for these children [138–141]. Children dependent on technology are living longer and this impacts on their transition to adult services and onward care in adult healthcare; there is a need for enhanced models of transition to adult services with established and standardised protocols [106, 125].
Discussion
This concept analysis shows that the term technology dependent continues to be widely used as an umbrella term for a large group of children, without much evidence of any critical consideration of its use. The most commonly referenced definition is now 33 years old [8]. We found that literature on technology dependence to sustain a child’s life refers to a wide range of clinical technology to support biological functioning across a dependency continuum, for a range of clinical conditions. This assistance is initiated within a complex biopsychosocial context and has wide ranging sequelae for the child and family and health and social care delivery. This highlighted the heterogenous nature of technology dependence, the fact that children could be assisted by one or more devices and the fact that the length of time for this assistance can vary. We also found that the language around technology dependence in the literature to date is very problem focused. The majority of work focuses on the negative sequelae of using technology to assist a child. This includes challenges with decision-making, organisational culture, frequency of hospitalisation, psychological challenges and concerns around family adaptation, and ongoing access to health and social care [6, 59, 90, 96, 113].
Twenty years ago, Nelson [142], in a chapter titled ‘The Ventilator/Baby as Cyborg: a Case Study in Technology and Medical Ethics’, suggested that technology dependence would eventually be viewed as routine care. The question of how we understand this coexistence of human beings with the opportunities posed by advancing technological augmentations is a significant issue [143–145]. An important step is critically reviewing the use of the term technology dependent. There is a need for more contemporary language that is more solution focused and child-centric. Our findings point to the redundancy of the term technology dependent, a mechanical term that continues to be used to group together a growing population of children who are assisted by technology in a myriad of ways, who adapt to, and function with, this assistance very differently. This is essential for research that is required to illuminate coping strategies and adaptation of children and their families to assistance from technology. The use of such a mechanical phrase can also detract from seeking to understand more about the phenomena happening when the use of technology is initiated, the absence of which can lead to the potential for more anecdote and personal opinion to influence actions, than empirical evidence. This is the focus of TechChild, a programme of research funded by the European Research Council which asks Just because we can, should we? An anthropological perspective on the initiation of technology dependence to sustain a child’s life. The overarching aim of this project is to specifically explore influences on the initiation of technological assistance and to develop a theory to explain the initiation of this technology in the context of contrasting health, legal, and socio-political systems. Within this 5-year programme, the terminology in use will be examined further and the current paper provides a foundation to this work.
Limitations
No specific international guidelines emerged from our search of the literature on the use of the term technology dependent. This is likely to be due to the fact that clinical guidelines predominantly focus on specific clinical presentations instead of using more broad terminology. We found that the term technology dependent encompasses a broad span of clinical areas and specialties, though the majority of papers referred to children who require predominantly respiratory or cardiac support. It is possible that some specific characteristics of other groups of children assisted by technology were not identified in this concept analysis, though the final definition may still be pertinent to the wider group of children who are assisted by technology.
Conclusion
In an era where interventionist medicine is increasingly available for ever more medically fragile children, this concept analysis is timely. We found that the term technology dependent refers to a wide range of clinical technology to support biological functioning across a dependency continuum, for a range of clinical conditions. They are initiated within a complex biopsychosocial context and have wide ranging sequelae for the child and family and health and social care delivery. The concept analysis highlighted that this term is predominantly portrayed in the literature as a very problem-focused issue. We suggest that the term is increasingly redundant and objectifies a heterogenous group of children who are assisted by a myriad of technology and who adapt to, and function with, this assistance in numerous ways.
Abbreviations
- ICD
Implantable cardioverter defibrillators
- HRQoL
Health-related quality of life
- PICU
Paediatric intensive care unit
Authors’ contribution
MB, DA and MQ made a substantial contribution to conception and design of the concept analysis and MB, DA and MQ screened the data gathered. MB, DA, MQ, JEC, PL and JB were involved in the acquisition of the data. All authors were involved in the interpretation of data, in drafting the article and revising it critically for important intellectual content. All authors agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Funding information
The project is funded by the European Research Council 803051.
Compliance with ethical standards
Conflict of interest
The authors declare that they have no conflict of interest and have no financial relationship with the organisation that sponsored the research.
Ethical approval
The article does not contain any studies with human participants or animals performed by any of the authors.
Footnotes
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Contributor Information
Maria Brenner, Email: brennerm@tcd.ie.
Denise Alexander, Email: ALEXANPD@tcd.ie.
Mary Brigid Quirke, Email: quirkemb@tcd.ie.
Jessica Eustace-Cook, Email: Jessica.Eustace-Cook@tcd.ie.
Piet Leroy, Email: p.leroy@mumc.nl.
Jay Berry, Email: Jay.Berry@childrens.harvard.edu.
Martina Healy, Email: martina.healy@olchc.ie.
Carmel Doyle, Email: doylec5@tcd.ie.
Kate Masterson, Email: kmasters@tcd.ie.
References
- 1.Wallis C, Paton JY, Beaton S, Jardine E. Children on long-term ventilatory support: 10 years of progress. Arch Dis Child. 2011;96:998–1002. doi: 10.1136/adc.2010.192864. [DOI] [PubMed] [Google Scholar]
- 2.Racca F, Berta G, Sequi M, Bignamini E, Capello E, Cutrera R, Ottonello G, Ranieri VM, Salvo I, Testa R, Wolfler A, Bonati M, on behalf of the “LTV Pediatric Italian Network” Long-term home ventilation of children in Italy: a national survey. Pediatr Pulmonol. 2011;46:566–572. doi: 10.1002/ppul.21401. [DOI] [PubMed] [Google Scholar]
- 3.Weiss S, Van Egmond-Fröhlich A, Hofer N, et al. Long-term respiratory support for children and adolescents in Austria: a national survey. Klin Padiatr. 2016;228(1):42–46. doi: 10.1055/s-0035-1565240. [DOI] [PubMed] [Google Scholar]
- 4.Amin R, Sayal P, Syed F, Chaves A, Moraes TJ, MacLusky I. Pediatric long-term home mechanical ventilation: twenty years of follow-up from one Canadian center. Pediatr Pulmonol. 2014;49(8):816–824. doi: 10.1002/ppul.22868. [DOI] [PubMed] [Google Scholar]
- 5.Denis-Larocque G, Williams K, St-Sauveur I, Ruddy M, Rennick J. Nurses’ perceptions of caring for parents of children with chronic medical complexity in the pediatric intensive care unit. Intensive Crit Care Nurs. 2017;43:149–155. doi: 10.1016/j.iccn.2017.01.010. [DOI] [PubMed] [Google Scholar]
- 6.Heneghan JA, Reeder RW, Dean JM, et al. Characteristics and outcomes of critical illness in children with feeding and respiratory technology dependence. Pediatr Crit Care Med. 2019;20:417–425. doi: 10.1097/PCC.0000000000001868. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Pyngottu A, Werner H, Lehmann P, Balmer C. Health-related quality of life and psychological adjustment of children and adolescents with pacemakers and implantable cardioverter defibrillators: a systematic review. Pediatr Cardiol. 2019;40(1):1–16. doi: 10.1007/s00246-018-2038-x. [DOI] [PubMed] [Google Scholar]
- 8.U.S. Congress Office of Technology Assessment . Technology-dependent children: hospital v. home care—a technical memorandum. Washington: U.S. Government Printing Office; 1987. [Google Scholar]
- 9.Rodgers BL, editor. Concept analysis: an evolutionary view. Philadelphia: Saunders; 2000. [Google Scholar]
- 10.Weaver K, Mitcham C. Nursing concept analysis in North America: state of the art. Nurs Philos. 2008;9(3):180–194. doi: 10.1111/j.1466-769X.2008.00359.x. [DOI] [PubMed] [Google Scholar]
- 11.Crain LS, Mangravite DN, Allport R, et al. Health care needs and services for technology-dependent children in developmental centers. Western J Med. 1990;152(4):434–438. [PMC free article] [PubMed] [Google Scholar]
- 12.Palfrey JS, Haynie M, Porter S, Bierle T, Cooperman P, Lowcock J. Project school care: integrating children assisted by medical technology into educational settings. J Sch Health. 1992;62(2):50–54. doi: 10.1111/j.1746-1561.1992.tb07883.x. [DOI] [PubMed] [Google Scholar]
- 13.Goldberg AI. Technology assessment and support of life-sustaining devices in home care: the home care physician perspective. Chest. 1994;105(5):1448–1453. doi: 10.1378/chest.105.5.1448. [DOI] [PubMed] [Google Scholar]
- 14.Russell CJ, Simon TD. Care of children with medical complexity in the hospital setting. Pediatr Ann. 2014;43(7):e157–e162. doi: 10.3928/00904481-20140619-09. [DOI] [PubMed] [Google Scholar]
- 15.Cancelinha C, Madureira N, Macao P, et al. Long-term ventilation in children: ten years later. Rev Port Pneumol. 2015;21(1):16–21. doi: 10.1016/j.rppnen.2014.03.017. [DOI] [PubMed] [Google Scholar]
- 16.Looman WS, Hullsiek RL, Pryor L, Mathiason MA, Finkelstein SM. Health-related quality of life outcomes of a telehealth care coordination intervention for children with medical complexity: a randomized controlled trial. J Pediatr Health Care. 2018;32(1):63–75. doi: 10.1016/j.pedhc.2017.07.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Nageswaran S, Hurst A, Radulovic A. Unexpected survivors: children with life-limiting conditions of uncertain prognosis. Am J Hosp Palliat Care. 2018;35(4):690–696. doi: 10.1177/1049909117739852. [DOI] [PubMed] [Google Scholar]
- 18.Giambra BK, Broome ME, Sabourin T, Buelow J, Stiffler D. Integration of parent and nurse perspectives of communication to plan care for technology dependent children: the theory of shared communication. J Pediatr Nurs. 2017;34:29–35. doi: 10.1016/j.pedn.2017.01.014. [DOI] [PubMed] [Google Scholar]
- 19.Serwint JR, Nellis ME. Deaths of pediatric patients: relevance to their medical home, an urban primary care clinic. Pediatrics. 2005;115:57–63. doi: 10.1542/peds.2004-0445. [DOI] [PubMed] [Google Scholar]
- 20.Berry JG, Graham DA, Graham RJ, Zhou J, Putney HL, O'Brien JE, Roberson DW, Goldmann DA. Predictors of clinical outcomes and hospital resource use of children after tracheotomy. Pediatrics. 2009;124:563–572. doi: 10.1542/peds.2008-3491. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Odetola FO, Gebremariam A, Davis MM. Comorbid illnesses among critically ill hospitalized children: impact on hospital resource use and mortality, 1997-2006. Pediatr Crit Care Med. 2010;1:457–463. doi: 10.1097/PCC.0b013e3181c514fa. [DOI] [PubMed] [Google Scholar]
- 22.Spratling R. Defining technology dependence in children and adolescents. West J Nurs Res. 2015;37(5):634–651. doi: 10.1177/0193945914526002. [DOI] [PubMed] [Google Scholar]
- 23.Graham RJ, Rodday AM, Weidner RA, Parsons SK. The impact on family of pediatric chronic respiratory failure in the home. J Pediatr. 2016;175:40–46. doi: 10.1016/j.jpeds.2016.05.009. [DOI] [PubMed] [Google Scholar]
- 24.Okido ACC, Pina JC, Lima RAG. Factors associated with involuntary hospital admissions in technology-dependent children. Rev Esc Enferm USP. 2016;50(1):29–35. doi: 10.1590/S0080-623420160000100004. [DOI] [PubMed] [Google Scholar]
- 25.Bezerra Goes FG, Cabral IE. Discourses on discharge care for children with special healthcare needs. Rev Bras Enferm. 2017;70(1):154–161. doi: 10.1590/0034-7167-2016-0248. [DOI] [PubMed] [Google Scholar]
- 26.Alexander E, Rennick JE, Carnevale F, Davis M. Daily struggles: living with long-term childhood technology dependence. Can J Nurs Res. 2002;34:7–14. [PubMed] [Google Scholar]
- 27.Howard L, Hunt K, Slade M, O'Keane V, Senevirante T, Leese M, Thornicroft G. Assessing the needs of pregnant women and mothers with severe mental illness: the psychometric properties of the Camberwell Assessment of Need - Mothers (CAN-M) Int J Methods Psychiatr Res. 2007;16:177–185. doi: 10.1002/mpr.227. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Samwell B. From hospital to home: journey of a child with complex care needs. Nurs Child Young People. 2012;24:14–19. doi: 10.7748/ncyp2012.11.24.9.14.c9389. [DOI] [PubMed] [Google Scholar]
- 29.Berry JG, Hall M, Cohen E, O’Neill M, Feudtner C. Ways to identify children with medical complexity and the importance of why. J Pediatr. 2015;67:229–237. doi: 10.1016/j.jpeds.2015.04.068. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Glader L, Plews-Ogan J, Agrawal R. Children with medical complexity: creating a framework for care based on the international classification of functioning, Disability and Health. Dev Med Child Neurol. 2016;258:1116–1123. doi: 10.1111/dmcn.13201. [DOI] [PubMed] [Google Scholar]
- 31.Seear M, Kapur A, Wensley D, Morrison K, Behroozi A. The quality of life of home-ventilated children and their primary caregivers plus the associated social and economic burdens: a prospective study. Arch Dis Child. 2016;101:620–627. doi: 10.1136/archdischild-2015-309796. [DOI] [PubMed] [Google Scholar]
- 32.Brenner M, Connolly M, Larkin P, et al. Adaptation of a voice-centered relational framework to explore the perspective of parents who have transitioned to home with a child with complex care needs. Compr Child Adolesc Nurs. 2017;40(4):285–293. doi: 10.1080/24694193.2017.1373159. [DOI] [PubMed] [Google Scholar]
- 33.Coller RJ, Nelson BB, Klitzner TS, Saenz AA, Shekelle PG, Lerner CF, Chung PJ. Strategies to reduce hospitalizations of children with medical complexity through complex care: expert perspectives. Acad Pediatr. 2017;17(4):381–338. doi: 10.1016/j.acap.2017.01.006. [DOI] [PubMed] [Google Scholar]
- 34.Hewitt-Taylor J. Caring for children with complex and continuing health needs. Nurs Stand. 2005;19:41–47. doi: 10.7748/ns2005.06.19.42.41.c3900. [DOI] [PubMed] [Google Scholar]
- 35.Brenner M, Larkin P, Hilliard C, Cawley D, Howlin F, Connolly M (2015) Parents’ perspectives of the transition to home when a child has complex technological health care needs. Int J Integr Care 15. 10.5334/ijic.1852 [DOI] [PMC free article] [PubMed]
- 36.Lindsay S, Hoffman A. A complex transition: lessons learned as three young adults with complex care needs transition from an inpatient paediatric hospital to adult community residences. Child Care Health Dev. 2015;41:397–407. doi: 10.1111/cch.12203. [DOI] [PubMed] [Google Scholar]
- 37.Woodgate RL, Zurba M, Edwards M, Ripat J, Rempel G. The embodied spaces of children with complex care needs: effects on the social realities and power negotiations of families. Health Place. 2017;46:6–12. doi: 10.1016/j.healthplace.2017.04.001. [DOI] [PubMed] [Google Scholar]
- 38.Carter B, Miller-Smith L, Verhagen E, Janvier A. The lure of technology: considerations in newborns with technology-dependence. In: Verhagen E, Janvier A, editors. Ethical dilemmas for critically ill babies. 2016. pp. 81–91. [Google Scholar]
- 39.Murrell DV, Lotze TE, Farber HJ, Crawford CA, Wiemann CM. The experience of families with children with spinal muscular atrophy type 1 across health care systems. J Child Neurol. 2017;32(11):917–923. doi: 10.1177/0883073817716853. [DOI] [PubMed] [Google Scholar]
- 40.Spratling R. Understanding the health care utilization of children who require medical technology: a descriptive study of children who require tracheostomies. Appl Nurs Res. 2017;34:62–65. doi: 10.1016/j.apnr.2017.02.017. [DOI] [PubMed] [Google Scholar]
- 41.Yates A, Hoffman T, Shepherd E, Boettner B, McBride K. Pediatric sub-specialist controversies in the treatment of congenital heart disease in trisomy 13 or 18. J Gent Couns. 2011;20:495–509. doi: 10.1007/s10897-011-9373-x. [DOI] [PubMed] [Google Scholar]
- 42.Haug S, Goldstein M, Cummins D, Fayard E, Merritt T (2017) Using patient-centered care after a prenatal diagnosis of trisomy 18 or trisomy 13: a review. JAMA Pediatr 171. 10.1001/jamapediatrics.2016.4798 [DOI] [PubMed]
- 43.Wilkinson D. “We don’t have a crystal ball ... ” neonatologists’ views on prognosis, magnetic resonance imaging and treatment withdrawal for infants with birth asphyxia. Monash Bioeth Rev. 2010;29(1):05.01–05.19. [PubMed] [Google Scholar]
- 44.Rasmussen LA, Bell E, Racine E. A qualitative study of physician perspectives on prognostication in neonatal hypoxic ischemic encephalopathy. J Child Neurol. 2016;31(11):1312–1319. doi: 10.1177/0883073816656400. [DOI] [PubMed] [Google Scholar]
- 45.Kukora S, Gollehon N, Weiner G, Laventhal N. Prognostic accuracy of antenatal neonatology consultation. J Perinatol. 2017;37(1):27–31. doi: 10.1038/jp.2016.171. [DOI] [PubMed] [Google Scholar]
- 46.Davies J, Slade P, Wright I, Stewart P. Posttraumatic stress symptoms following childbirth and mothers’ perceptions of their infants. Infant Ment Health J. 2008;29:537–554. doi: 10.1002/imhj.20197. [DOI] [PubMed] [Google Scholar]
- 47.Janvier A, Mercurio M. Saving vs. creating: perceptions of intensive care at different ages and the potential for injustice. J Perinatol. 2013;33:333–335. doi: 10.1038/jp.2012.134. [DOI] [PubMed] [Google Scholar]
- 48.Fadadu PP, Liu JC, Schiltz BM, Xoay TD, Phuc PH, Kumbamu A, Ouellette Y (2019) A mixed-methods exploration of pediatric intensivists' attitudes toward end-of-life care in Vietnam. J Palliat Med 22(8). 10.1089/jpm.2018.0496 [DOI] [PubMed]
- 49.Weithorn LA, Campbell SB. The competency of children and adolescents to make informed treatment decisions. Child Dev. 1982;53(6):1589–1598. [PubMed] [Google Scholar]
- 50.McCabe MA. Involving children and adolescents in medical decision making: developmental and clinical considerations. J Pediatr Psychol. 1996;21(4):505–516. doi: 10.1093/jpepsy/21.4.505. [DOI] [PubMed] [Google Scholar]
- 51.Alderson P. Competent children? Minors’ consent to health care treatment and research. Soc Sci Med. 2007;65(11):2272–2283. doi: 10.1016/j.socscimed.2007.08.005. [DOI] [PubMed] [Google Scholar]
- 52.Pousset G, Bilsen J, De Wilde J, Benoit Y, Verlooy J, Bomans A, Deliens L, Mortier F. Attitudes of adolescent cancer survivors toward end-of-life decisions for minors. Pediatrics. 2009;124(6):e1142–e1148. doi: 10.1542/peds.2009-0621. [DOI] [PubMed] [Google Scholar]
- 53.Duncan RE, Sawyer SM. Respecting adolescents’ autonomy (as long as they make the right choice) J Adolesc Health. 2010;47(2):113–114. doi: 10.1016/j.jadohealth.2010.05.020. [DOI] [PubMed] [Google Scholar]
- 54.Diekema DS. Adolescent refusal of lifesaving treatment: are we asking the right questions? Adolesc Med State Art Rev. 2011;22(2):213–228. [PubMed] [Google Scholar]
- 55.Katz AL, Webb SA. Informed consent in decision-making in pediatric practice. Pediatrics. 2016;138(2):e20161485. doi: 10.1542/peds.2016-1485. [DOI] [PubMed] [Google Scholar]
- 56.Grootens-Wiegers P, Hein IM, van den Broek JM, de Vries MC. Medical decision-making in children and adolescents: developmental and neuroscientific aspects. BMC Pediatr. 2017;17(1):120. doi: 10.1186/s12887-017-0869-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Sabatello M, Janvier A, Verhagen E, Morrison W, Lantos J. Pediatric participation in medical decision making: optimized or personalized? Am J Bioeth. 2018;18(3):1–3. doi: 10.1080/15265161.2017.1418931. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Carnevale FA, Alexander E, Davis M, Rennick J, Troini R. Daily living with distress and enrichment: the moral experience of families with ventilator-assisted children at home. Pediatrics. 2006;117(1):e48–e60. doi: 10.1542/peds.2005-0789. [DOI] [PubMed] [Google Scholar]
- 59.Rapoport A, Harrison C, Carnevale FA. Section 3: Ethics of initiation of long-term ventilation in children at home. Can J Respir Crit Care Sleep Med. 2018;2(sup1):16–22. [Google Scholar]
- 60.Schapiro T. What is a child? Ethics. 1999;109(4):715–738. [Google Scholar]
- 61.Tristram E. The foundations of bioethics. 2. Oxford: Oxford University Press; 1996. [Google Scholar]
- 62.Committee on Bioethics, American Academy of Pediatrics Informed consent, parental permission, and assent in pediatric practice. Pediatrics. 1995;95:314–317. [PubMed] [Google Scholar]
- 63.Horridge KA. Advance care planning: practicalities, legalities, complexities and controversies. Arch Dis Child. 2015;100(4):380–385. doi: 10.1136/archdischild-2014-305945. [DOI] [PubMed] [Google Scholar]
- 64.DeCourcey DD, Silverman M, Oladunjoye A, Wolfe J. Advance care planning and parent-reported end-of-life outcomes in children, adolescents, and young adults with complex chronic conditions. Crit Care Med. 2019;47(1):101–108. doi: 10.1097/CCM.0000000000003472. [DOI] [PubMed] [Google Scholar]
- 65.Mitchell S, Spry JL, Hill E, Coad J, Dale J, Plunkett A. Parental experiences of end of life care decision-making for children with life-limiting conditions in the paediatric intensive care unit: a qualitative interview study. BMJ Open. 2019;9:e028548. doi: 10.1136/bmjopen-2018-028548. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Sidgwick P, Fraser J, Fortune P, McCulloch R. Parallel planning and the paediatric critical care patient. Arch Dis Child. 2019;104(10):994–997. doi: 10.1136/archdischild-2018-315222. [DOI] [PubMed] [Google Scholar]
- 67.Eden LM, Callister LC. Parent involvement in end-of-life care and decision making in the newborn intensive care unit: an integrative review. J Perinat Educ. 2010;19(1):29–39. doi: 10.1624/105812410X481546. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.de Souza EJ, da Silva LF, Santos da Conceição D, Dórea Paiva E. Families concerns about the care of children with technology-dependent special health care needs. Investig Educ Enferm. 2015;33(3):547–555. doi: 10.17533/udea.iee.v33n3a19. [DOI] [PubMed] [Google Scholar]
- 69.Minton C, Batten L, Huntington A. A multicase study of prolonged critical illness in the intensive care unit: families’ experiences. Intensive Crit Care Nurs. 2019;50:21–27. doi: 10.1016/j.iccn.2018.08.010. [DOI] [PubMed] [Google Scholar]
- 70.Edwards JD, Kun SS, Graham RJ, Keens TG. End-of-life discussions and advance care planning for children on long-term assisted ventilation with life-limiting conditions. J Palliat Care. 2012;28(1):21–27. [PMC free article] [PubMed] [Google Scholar]
- 71.McFeeters M (2016) The lived experiences of hospital for parents of children commenced on invasive long-term ventilation. Unpublished thesis. DeMonteforte University. http://hdl.handle.net/2086/13059
- 72.Baird HS. Paediatric long term ventilation; the right or wrong move? A critical analysis on case studies in PICU, exploring controversial issues surrounding the initiation of long term ventilation in children with chronic disease. Arch Dis Child. 2011;96(1):A80–A81. [Google Scholar]
- 73.Mims J, Crisham P. Health care management of children with cognitive and physical disabilities: to treat or not to treat. J Neurosurg Nurs. 1996;28(4):238–251. [PubMed] [Google Scholar]
- 74.Dosa NP, Boeing NM, Ms NP, Kanter RK. Excess risk of severe acute illness in children with chronic health conditions. Pediatrics. 2001;107(3):499–504. doi: 10.1542/peds.107.3.499. [DOI] [PubMed] [Google Scholar]
- 75.Berry JG, Wilson KM, Dumas H, et al. Use of post-acute facility care in children hospitalized with acute respiratory illness. J Hosp Med. 2017;12(8):626–631. doi: 10.12788/jhm.2780. [DOI] [PubMed] [Google Scholar]
- 76.Benneyworth BD, Gebremariam A, Clark SJ, Shanley TP, Davis MM. Inpatient health care utilization for children dependent on long-term mechanical ventilation. Pediatrics. 2011;127(6):e1533–e1541. doi: 10.1542/peds.2010-2026. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Cohen E, Kuo DZ, Agrawal R, Berry JG, Bhagat SKM, Simon TD, Srivastava R. Children with medical complexity: an emerging population for clinical and research initiatives. Pediatrics. 2011;127(3):529–538. doi: 10.1542/peds.2010-0910. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Lindahl B, Lindblad BM. Family members’ experiences of everyday life when a child is dependent on a ventilator: a metasynthesis study. J Fam Nurs. 2011;17(2):241–269. doi: 10.1177/1074840711405392. [DOI] [PubMed] [Google Scholar]
- 79.Hudson SM. Hospital readmissions and repeat emergency department visits among children with medical complexity: an integrative review. J Pediatr Nurs. 2013;28(4):316–339. doi: 10.1016/j.pedn.2012.08.009. [DOI] [PubMed] [Google Scholar]
- 80.Peltz A, Wu CL, White ML, Wilson KM, Lorch SA, Thurm C, Hall M, Berry JG. Characteristics of rural children admitted to pediatric hospitals. Pediatrics. 2016;137(5):e20153156. doi: 10.1542/peds.2015-3156. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Wells S, O'Neill M, Rogers J, Blaine K, Hoffman A, McBride S, Tschudy MM, Shumskiy I, Mauskar S, Berry JG. Nursing-led home visits post-hospitalization for children with medical complexity. J Pediatr Nurs. 2017;34:10–16. doi: 10.1016/j.pedn.2017.03.003. [DOI] [PubMed] [Google Scholar]
- 82.De Jesus-Rojas W, Aneji C, Samuels CL, et al. Outcomes of technology dependent nicu infants: a single center 5-year review comparing usual care versus comprehensive medical care. Am J Respir Crit Care Med. 2018;197:A2052. [Google Scholar]
- 83.Burns JP, Sellers DE, Meyer EC, Lewis-Newby M, Truog RD. Epidemiology of death in the PICU at five U.S. teaching hospitals. Crit Care Med. 2014;42(9):2101–2108. doi: 10.1097/CCM.0000000000000498. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84.Truog RD, Hahn E, Seltzer R, et al. The intensive care unit isn't right, but there is nowhere else to go: family experience of recurrent and prolonged pediatric hospitalizations: a systematic review. J Pain Symptom Manag. 2017;53(2):446–447. [Google Scholar]
- 85.Pinto NP, Rhinesmith EW, Kim TY, Ladner PH, Pollack MM. Long-term function after pediatric critical illness: results from the survivor outcomes study. Pediatr Crit Care Med. 2017;18(3):e122–e130. doi: 10.1097/PCC.0000000000001070. [DOI] [PubMed] [Google Scholar]
- 86.Stephenson EA, Berul CI. Temporary and permanent pacemakers and automated internal defibrillators. In: Da Cruz E, Ivy D, Jaggers J, editors. Pediatric and congenital cardiology, cardiac surgery and intensive care. London: Springer; 2014. [Google Scholar]
- 87.Kuo DZ, Cohen E, Agrawal R, Berry JG, Casey PH. A national profile of caregiver challenges among more medically complex children with special health care needs. Arch Pediatr Adolesc Med. 2011;165(11):1020–1026. doi: 10.1001/archpediatrics.2011.172. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88.Eicken A, Kolb C, Lange S, Brodherr-Heberlein S, Zrenner B, Schreiber C, Hess J. Implantable cardioverter defibrillator (ICD) in children. Int J Cardiol. 2006;107(1):30–35. doi: 10.1016/j.ijcard.2005.02.048. [DOI] [PubMed] [Google Scholar]
- 89.Webster G, Panek KA, Labella M, Taylor GA, Gauvreau K, Cecchin F, Martuscello M, Walsh EP, Berul CI, DeMaso DR. Psychiatric functioning and quality of life in young patients with cardiac rhythm devices. Pediatrics. 2014;133(4):e964–e972. doi: 10.1542/peds.2013-1394. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Freedenberg VA, Thomas SA, Friedmann E. A pilot study of a mindfulness based stress reduction program in adolescents with implantable cardioverter defibrillators or pacemakers. Pediatr Cardiol. 2015;36(4):786–795. doi: 10.1007/s00246-014-1081-5. [DOI] [PubMed] [Google Scholar]
- 91.Czosek RJ, Bonney WJ, Cassedy A, Mah DY, Tanel RE, Imundo JR, Singh AK, Cohen MI, Miyake CY, Fawley K, Marino BS. Impact of cardiac devices on the quality of life in pediatric patients. Circ Arrhythm Electrophysiol. 2012;5(6):1064–1072. doi: 10.1161/CIRCEP.112.973032. [DOI] [PubMed] [Google Scholar]
- 92.Sears SF, Hazelton AG, St Amant J, et al. Quality of life in pediatric patients with implantable cardioverter defibrillators. Am J Cardiol. 2011;107(7):1023–1027. doi: 10.1016/j.amjcard.2010.11.027. [DOI] [PubMed] [Google Scholar]
- 93.O’Brien ME, Wegner CB. Rearing the child who is technology dependent: perceptions of parents and home care nurses. J Spec Pediatr Nurs. 2002;7(1):7e15. doi: 10.1111/j.1744-6155.2002.tb00143.x. [DOI] [PubMed] [Google Scholar]
- 94.Feudtner C, Villareale NL, Morray B, et al. Technology-dependency among patients discharged from a children's hospital: a retrospective cohort study. BMC Pediatr. 2005;5(1):5–8. doi: 10.1186/1471-2431-5-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 95.Kuster PA, Badr LK, Chang BL, Wuerker AK, Benjamin AE. Factors influencing health promoting activities of mothers caring for ventilator-assisted children. J Pediatr Nurs. 2004;19:276e287–276e287. doi: 10.1016/j.pedn.2004.05.009. [DOI] [PubMed] [Google Scholar]
- 96.Spiers G, Parker G, Gridley K, Atkin K. The psychosocial experience of parents receiving care closer to home for their ill child. Health Soc Care Commun. 2011;19(6):653–660. doi: 10.1111/j.1365-2524.2011.01008.x. [DOI] [PubMed] [Google Scholar]
- 97.Halley GC. Getting children home on long term ventilation. Paediatr Child Health. 2012;22(12):541–543. [Google Scholar]
- 98.Manhas KP, Mitchell I. Extremes, uncertainty, and responsibility across boundaries: facets and challenges of the experience of transition to complex, pediatric home care. J Child Health Care. 2012;16(3):224–336. doi: 10.1177/1367493511430677. [DOI] [PubMed] [Google Scholar]
- 99.Toly VB, Musil CM, Carl JC. Families with children who are technology dependent: normalization and family functioning. West J Nurs Res. 2012;34:52e71. doi: 10.1177/0193945910389623. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 100.Toly VB, Musil CM, Carl JC. A longitudinal study of families with technology-dependent children. Res Nurs Health. 2012;35:40e54–40e54. doi: 10.1002/nur.21454. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 101.Coad J (2013) Breathing matters - improving care with a training needs analysis of ventilated children, young people, families and professionals. Final Report. http://www.togetherforshortlives.org.uk/assets/0000/4689/Coad.CCFAR.BreathingMa tters.FINAL_2013_Report_27.08.13.Pdf
- 102.Smith J, Cheater F, Bekker H. Parents’ experiences of living with a child with a long-term condition: a rapid structured review of the literature. Health Expect. 2013;18(4):452–474. doi: 10.1111/hex.12040. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 103.Whiting M. Impact, meaning and need for help and support: the experience of parents caring for children with disabilities, life-limiting/life-threatening illness or technology dependence. J Child Health Care. 2013;17:92–108. doi: 10.1177/1367493512447089. [DOI] [PubMed] [Google Scholar]
- 104.Bowles JD, Jnah AJ, Newberry DM, Hubbard CA, Roberston T. Infants with technology dependence: facilitating the road to home. Adv Neonatal Care. 2016;16(6):424–429. doi: 10.1097/ANC.0000000000000310. [DOI] [PubMed] [Google Scholar]
- 105.Sterni LM, Collaco JM, Baker CD, Carroll JL, Sharma GD, Brozek JL, Finder JD, Ackerman VL, Arens R, Boroughs DS, Carter J, Daigle KL, Dougherty J, Gozal D, Kevill K, Kravitz RM, Kriseman T, MacLusky I, Rivera-Spoljaric K, Tori AJ, Ferkol T, Halbower AC. An official American Thoracic Society clinical practice guideline: pediatric chronic home invasive ventilation. Am J Respir Crit Care Med. 2016;193(8):E16–E35. doi: 10.1164/rccm.201602-0276ST. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 106.Brenner M, O'Shea MP, Larkin P, Luzi D, Pecoraro F, Tamburis O, Berry J, Alexander D, Rigby M, Blair M. Management of a child with complex care needs at the acute community interface in Europe. Lancet Child Adolesc Health. 2018;2:822–831. doi: 10.1016/S2352-4642(18)30272-4. [DOI] [PubMed] [Google Scholar]
- 107.Brenner M, O'Shea MP, McHugh R, Clancy A, Larkin P, Luzi D, Pecoraro F, Olaso EM, Lignou S, Alma M, Satherley RM, Tamburis O, Warters A, Wolfe I, Hilliard C, Berry J, Alexander D, Rigby M, Blair M. Principles for optimising the provision of complex care at the acute community interface in Europe. Lancet Child Adolesc Health. 2018;2:832–838. doi: 10.1016/S2352-4642(18)30270-0. [DOI] [PubMed] [Google Scholar]
- 108.Nishigaki K, Kanamori Y, Ikeda M, Sugiyama M, Minowa H, Kamibeppu K. Changes in mothers' psychosocial perceptions of technology-dependent children and adolescents at home in Japan: acknowledgement of children's autonomy. Asian Nurs Res (Korean Soc Nurs Sci) 2016;10(2):100–105. doi: 10.1016/j.anr.2016.04.001. [DOI] [PubMed] [Google Scholar]
- 109.Spiers G, Beresford B. “It goes against the grain”: a qualitative study of the experiences of parents’ administering distressing health-care procedures for their child at home. Health Expect. 2017;20(5):920–928. doi: 10.1111/hex.12532. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 110.Kirk S, Glendinning C, Callery P. Parent or nurse? The experience of being the parent of a technology-dependent child. J Adv Nurs. 2005;51(5):456–464. doi: 10.1111/j.1365-2648.2005.03522.x. [DOI] [PubMed] [Google Scholar]
- 111.McDonald J, McKinlay E, Keeling S, Levack W. How family carers engage with technical health procedures in the home: a grounded theory study. BMJ Open. 2015;5(7):e007761. doi: 10.1136/bmjopen-2015-007761. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 112.McDonald J, McKinlay E, Keeling S, Levack W. Complex home care: challenges arising from the blurring of boundaries between family and professional care. Kotuitui N Z J Soc Sci Online. 2017;12(2):246–255. [Google Scholar]
- 113.Suzuki S, Sato I, Emoto S, Kamibeppu K. Physio-psychological burdens and social restrictions on parents of children with technology dependency are associated with care coordination by nurses. J Pediatr Nurs. 2017;36:124–131. doi: 10.1016/j.pedn.2017.06.006. [DOI] [PubMed] [Google Scholar]
- 114.Okido ACC, Zago MMF, Lima RAG. Care for technology dependent children and their relationship with the health care systems. Rev Lat Am Enfermagem. 2015;23(2):291–298. doi: 10.1590/0104-1169.0258.2554. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 115.Toly VB, Musil CM. Factors related to depressive symptoms in mothers of technology-dependent children. Issues Ment Health Nurs. 2015;36(7):518–527. doi: 10.3109/01612840.2015.1009662. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 116.Mendes MA. Partnership with parents of technology-dependent children: clarification of the concept. ANS Adv Nurs Sci. 2016;39(1):85–93. doi: 10.1097/ANS.0000000000000106. [DOI] [PubMed] [Google Scholar]
- 117.Toly VB, Blanchette JE, Sikorski S, Musil CM, al-Hamed A. Maternal perspectives of well siblings' adjustment to family life with a technology-dependent child. J Fam Nurs. 2017;23(3):392–417. doi: 10.1177/1074840717721705. [DOI] [PubMed] [Google Scholar]
- 118.Vermaes IPR, van Susante AMJ, van Bakel HJA. Psychological functioning of siblings in families of children with chronic health conditions: a meta-analysis. J Pediatr Psychol. 2012;37:166–184. doi: 10.1093/jpepsy/jsr081. [DOI] [PubMed] [Google Scholar]
- 119.Knafl KA, Deatrick JA, Knafl G, et al. Patterns of family management of childhood chronic conditions and their relationship to child and family functioning. J Pediatr Nurs. 2013;28:523–535. doi: 10.1016/j.pedn.2013.03.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 120.Cohen MH. The triggers of heightened parental uncertainty in chronic, life-threatening childhood illness. Qual Health Res. 1995;5(1):63–77. [Google Scholar]
- 121.Parker G, Spiers G, Gridley K, Atkin K, Birks Y, Lowson K, Light K. Systematic review of international evidence on the effectiveness and costs of paediatric home care for children and young people who are ill. Child Care Health Dev. 2013;39:1–19. doi: 10.1111/j.1365-2214.2011.01350.x. [DOI] [PubMed] [Google Scholar]
- 122.Statile AM, Schondelmeyer AC, Thomson JE, et al. Improving discharge efficiency in medically complex pediatric patients. Pediatrics. 2016;138:e2015383. doi: 10.1542/peds.2015-3832. [DOI] [PubMed] [Google Scholar]
- 123.Van Cleave J. Children with special health care needs: with population-based data, better individual care plans. Pediatrics. 2015;135:e1040–e1041. doi: 10.1542/peds.2015-0319. [DOI] [PubMed] [Google Scholar]
- 124.Morse RB, Hall M, Fieldston ES, McGwire G, Anspacher M, Sills MR, Williams K, Oyemwense N, Mann KJ, Simon HK, Shah SS. Hospital-level compliance with asthma care quality measures at children's hospitals and subsequent asthma-related outcomes. JAMA. 2011;306(13):1454–1460. doi: 10.1001/jama.2011.1385. [DOI] [PubMed] [Google Scholar]
- 125.Berry JG, Blaine K, Rogers J, et al. A framework of pediatric hospital discharge care informed by legislation, research, and practice. JAMA Pediatr. 2014;168(10):955–962. doi: 10.1001/jamapediatrics.2014.891. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 126.Agarwal A, Willis D, Tang X, Bauer M, Berlinski A, Com G, Ward WL, Carroll JL. Transition of respiratory technology dependent patients from pediatric to adult pulmonology care. Pediatr Pulmonol. 2015;50(12):1294–1300. doi: 10.1002/ppul.23155. [DOI] [PubMed] [Google Scholar]
- 127.Berry JG, Ziniel SI, Freeman L, Kaplan W, Antonelli R, Gay J, Coleman EA, Porter S, Goldmann D. Hospital readmission and parent perceptions of their child’s hospital discharge. Int J Qual Health Care. 2013;25(5):573–581. doi: 10.1093/intqhc/mzt051. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 128.Zajicek-Farber ML, Lotrecchiano GR, Long TM, et al. Parental perceptions of family centered care in medical homes of children with neurodevelopmental disabilities. Matern Child Health J. 2015;19:1744–1755. doi: 10.1007/s10995-015-1688-z. [DOI] [PubMed] [Google Scholar]
- 129.De Jesus-Rojas W, Mosquera RA, Samuel C, et al. The effect of comprehensive medical care on the long-term outcomes of children discharged from the NICU with tracheostomy. Open Respir Med J. 2018;12(1):39–49. doi: 10.2174/1874306401812010039. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 130.Abraham G, Fehr J, Ahmad F, Jeffe DB, Copper T, Yu F, White AJ, Auerbach M, Schnadower D. Emergency information forms for children with medical complexity: a simulation study. Pediatrics. 2016;38(2):e20160847. doi: 10.1542/peds.2016-0847. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 131.Larson IA, Hoffman A, Artman M. Maximizing health outcomes in a medical home for children with medical complexity: the Beacon Program. J Pediatr. 2017;183:45–45. doi: 10.1016/j.jpeds.2017.01.024. [DOI] [PubMed] [Google Scholar]
- 132.Dingfield L, Bender L, Harris P, Newport K, Hoover-Regan M, Feudtner C, Clifford S, Casarett D. Comparison of pediatric and adult hospice patients using electronic medical record data from nine hospices in the United States, 2008–2012. J Palliat Med. 2015;18:120–126. doi: 10.1089/jpm.2014.0195. [DOI] [PubMed] [Google Scholar]
- 133.Thienprayoon R, Lee SC, Leonard D, Winick N. Hospice care for children with cancer: where do these children die? J Pediatr Hematol Oncol. 2015;37:373–377. doi: 10.1097/MPH.0000000000000331. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 134.Brenner M, Cote SM, Boivin M, Tremblay RE. Severe congenital malformations, family functioning and parents’ separation/divorce: a longitudinal study. Child Care Health Dev. 2016;42(1):16–24. doi: 10.1111/cch.12269. [DOI] [PubMed] [Google Scholar]
- 135.Thienprayoon R, San Julian Mark M, Grossoehme D. Provider-prioritized domains of quality in pediatric home-based hospice and palliative care: a study of the Ohio pediatric palliative care and end-of-life network. J Palliat Med. 2018;21(3):290–296. doi: 10.1089/jpm.2017.0333. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 136.Farmer JE, Clark MJ, Drewel EH, Swenson TM, Ge B. Consultative care coordination through the medical home for CSHCN: a randomized controlled trial. Matern Child Health J. 2011;15:1110–1118. doi: 10.1007/s10995-010-0658-8. [DOI] [PubMed] [Google Scholar]
- 137.Looman WS, Erickson MM, Garwick AW, et al. Meaningful use of data in care coordination by the advanced practice RN: the telefamilies project. Comput Inform Nurs. 2012;30:649–654. doi: 10.1097/NXN.0b013e318266caf2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 138.Looman WS, Presler E, Erickson MM, Garwick AW, Cady RG, Kelly AM, Finkelstein SM. Care coordination for children with complex special health care needs: the value of the advanced practice nurse’s enhanced scope of knowledge and practice. J Pediatr Health Care. 2013;27:293–303. doi: 10.1016/j.pedhc.2012.03.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 139.Shimizu F, Katsuda H. Teachers' perceptions of the role of nurses: caring for children who are technology-dependent in mainstream schools. Jpn J Nurs Sci. 2015;12(1):35–43. doi: 10.1111/jjns.12046. [DOI] [PubMed] [Google Scholar]
- 140.Shimizu F, Suzuki M. Role development of nurses for technology-dependent children attending mainstream schools in Japan. J Spec Pediatr Nurs. 2015;20(2):87–97. doi: 10.1111/jspn.12105. [DOI] [PubMed] [Google Scholar]
- 141.Ballard SL, Dymond SK. Inclusive education for secondary age students with severe disabilities and complex health care needs. Intellect Dev Disabil. 2018;56(6):427–441. [Google Scholar]
- 142.Nelson RM. The ventilator/baby as cyborg: a case study in technology and medical ethics. In: Brodwin PE, editor. Biotechnology and culture: bodies, anxieties, ethics. Bloomington: Indiana University Press; 2000. pp. 3–23. [Google Scholar]
- 143.Wilkinson D. Death or disability? The ‘Carmentis Machine’ and decision-making for critically ill children. Oxford: Oxford University Press; 2013. [Google Scholar]
- 144.Garrett JR. Two agendas for bioethics: critique and integration. Bioethics. 2015;29(6):440–447. doi: 10.1111/bioe.12116. [DOI] [PubMed] [Google Scholar]
- 145.Ho LY, Tan TK, Goh PSJ. Advocating for the best interests of critically ill newborn infants. Proc Singap Healthc. 2013;22(3):213–224. [Google Scholar]