Highlights
-
•
Surgical training during the COVID-19 Pandemic required restructuring.
-
•
Surgical Services can meet hospital needs as an access and procedure team.
-
•
Videoconferencing platforms can be utilized for continued communication and education.
Early 2020, coronavirus disease 2019 (COVID-19) became prevalent in New York City.1 The New York State Governor designated University Hospital of Brooklyn (UHB) as a COVID-19 hospital. The faculty, residents, and students that serve it reflect the diverse cultures and nationalities of Brooklyn. State University New York (SUNY) Downstate Health Sciences University is the sole academic medical center in Brooklyn, training 59 General Surgery residents. Residents rotate at five hospitals: UHB (the primary teaching hospital), Kings County Hospital, Brooklyn Campus of the Veterans Affairs NY Harbour Healthcare System, Coney Island Hospital, and Richmond University Medical Center. We are also responsible for the surgical education of SUNY Downstate Health Sciences University College of Medicine.
The COVID-19 pandemic dramatically changed the daily activities of the Department of Surgery. All elective surgeries and clinics were canceled per the American College of Surgeons guidelines.2 The number of emergency surgeries also decreased. Consequently, we saw a rapid decline in the surgical service census. As NYC became a COVID-19 epicenter, our Department of Surgery was challenged with how to ensure resident and faculty safety while mitigating supply shortages and providing care for the surplus of critically ill patients.
Residents were told to remain at their current clinical assignments because of familiarity with that hospital’s safety protocols and prevent potential COVID-19 contamination across the residency. The Graduate Medical Education (GME) Office declared Pandemic Emergency Status with the Accreditation Council for Graduate Medical Education (ACGME),3 which allowed flexibility for residents’ redeployment. In response to the pandemic, all vacation requests for its faculty and residents rescinded. The UHB research resident was redeployed to active clinical duties. Residents received a refresher course on resuscitation and ventilator management. Appropriate use of personal protective equipment (PPE) was emphasized, and the GME Office provided additional training on PPE donning and duffing.
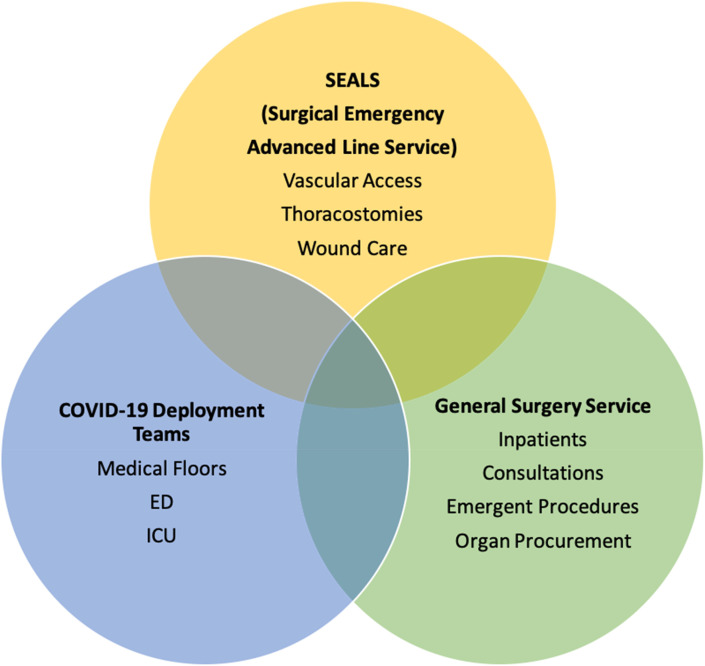
UHB filled quickly with hundreds of patients with COVID-19. Many had a complicated course requiring interventions, including intubation, pressor support, and hemodialysis. The residents rotating at UHB were restructured into three teams (Fig. 1 .). (1) A Call team with responsibilities including routine floor work, support of medical services by assisting in proning patients and performing emergency resuscitations and covering the Transplant Surgery service. (2) A Surgical Emergency Advanced Line Service (SEALS) team, composed of residents and a supervising attending, was assigned to assist with procedural solutions for all inpatients, including placement of arterial, central venous, dialysis, and midline catheters. The SEALS team was also responsible for thoracostomy, pigtail catheter insertion, and wound management. (3) The remaining surgical residents were redeployed to the medical floors, emergency department and ICUs. Throughout redeployment, residents adhered to the ACGME Big Four governance under the Stage 3 Pandemic Emergency status: duty hour regulations, having faculty supervision, and adequate resources including PPE. All other common program and specialty-specific requirements were suspended.3
Fig. 1.
General surgery resident groups during COVID-19 pandemic.
Additionally, program-wide phone message group to discuss issues, announce changes and help create a cohesive community despite physical distances. We had a Rapid Response Leadership Team consisting of chief residents and site directors, which met via teleconferencing regularly to address ongoing concerns. Direct patient contact was ideally limited to one person during rounds. Every morning, PPE was distributed from a carefully controlled inventory. We used an N95 respirator when at risk for aerosolization it is covered by a surgical mask that is changed according to CDC guidance.4 Face shields were reused after cleaning.5 Gowns were issued daily and not changed between patients with COVID-19 in the same unit, unless soiled. We were instructed to report immediately if experiencing any symptoms with isolation at home for 7 days if symptomatic. Residents had to be asymptomatic for three days before medical clearance for return to duty.6 , 7 From mid-April, eleven residents were isolated due to COVID-19-like symptoms, and two tested positive. Additionally, free mental health services were offered by the GME Office and UHB.
Despite suspension of the ACGME didactic requirements, our department continued to maintain educational sessions to provide continuity of the curriculum and engage with residents for both wellness and training (Table 1 .). This may have been even more important for residents with families in other states and countries. All of our group educational activities were converted to videoconferencing.8 , 9 Weekly grand rounds, morbidity and mortality conference, guest speakers, and journal club were held during the daytime. Core Curriculum and board exam preparation continued but were moved to evening and recorded, due to the demands of ongoing clinical duties. For continued care of patients without COVID-19 requiring outpatient follow-up and consultation, telemedicine platforms were initiated.
Table 1.
Summary of general surgery residency structure during COVID-19 pandemic.
| Workforce Adjustments |
|---|
| Anticipation of significantly decreased routine workload |
| Optimization of workforce (rescheduling of vacation/research) |
| Contingencies for temporary reduction of residents due to illness |
| Creation of a dedicated access/procedure service (SEALS) |
| Safety |
| Physical separation of resident subgroups |
| Limitation of direct interaction with COVID-19 patients |
| Guidance of conservative PPE use |
| Distribution of PPE to all residents and staff |
| Escalation protocol for PPE shortage |
| Isolation and Return to Duty protocols of symptomatic residents and staff |
| Easy access to mental health support services and wellness activities |
| Abide by ACGME duty hours regulations |
| Academic Activities |
| Refresher course on ventilator management, with emphasis on COVID-19 related lung injury, and resuscitation |
| PPE donning and duffing training |
| Continuation of academic curriculum |
| Use of web-based platforms for education and residency community engagement |
| Flexibility of teaching hours to include evening sessions |
| Recording of academic activities for self-study |
By assigning residents to a multitude of medical services, we risked losing our surgery department’s identity, yet they kept our general surgery residency as a cohesive unit. Our procedure service (SEALS) allowed primary teams to focus on medical care without the burden of procedures and surgical residents to practice their skills and manage critically ill patients with COVID-19.
Caring for patients suffering from COVID-19 infection is as novel as the disease itself. There were no guidelines on how to treat patients, much less ourselves. The trepidation exhibited by both patients and healthcare workers was palpable. We witnessed death on a massive scale. We lost many of our patients, and even some of our colleagues and loved ones. Morale significantly increased because we understood that our department underscored our safety, cohesiveness, physical and mental well-being, as well as maintenance of resident education while meeting the overwhelming needs of UHB. We have endured massive devastation during this crisis. Yet, we remained unified, not despite our different backgrounds and perspectives but precisely because of them. It is paramount that as physicians, we understand the importance of caring for not just our patients and families but also ourselves and each other.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Declaration of competing interest
None of the authors have conflicts to disclose.
References
- 1.World Health Organization Coronavirus disease 2019 (COVID-19). United states. https://www.cdc.gov/coronavirus/2019-nCoV/hcp/index.html Available at. Accessed April 7, 2020.
- 2.American College of Surgeons COVID-19: recommendations for management of elective surgical procedure. United states. https://www.facs.org/covid-19/clinical-guidance/elective-surgery Available at. Accessed April 7, 2020.
- 3.Accreditation Council for Graduate Medical Education Stage 3 pandemic emergency status guidance. United states. Retrieved from ACGME. https://acgme.org/COVID-19/Three-Stages-of-GME-During-the-COVID-19-Pandemic/Stage-3-Pandemic-Emergency-Status-Guidance Accessed April 18, 2020.
- 4.Centers for Disease Control and Prevention Release stockpiled N95. United states. https://www.cdc.gov/coronavirus/2019-ncov/release-stockpiled-N95.html Available at. Accessed April 9, 2020.
- 5.Centers for Disease Control and Prevention PPE strategy. United states. https://www.cdc.gov/coronavirus/2019-ncov/hcp/ppe-strategy/eye-protection.html Available at. Accessed April 9, 2020.
- 6.Surviving Sepsis Campaign Surviving sepsis guidelines for COVID-19. United states. https://www.sccm.org/SurvivingSepsisCampaign/Guidelines/COVID-19 Available at. Accessed April 18, 2020.
- 7.Centers for Disease Control and Prevention Criteria for return to work for healthcare personnel with suspected or confirmed COVID-19. United states. https://www.cdc.gov/coronavirus/2019-ncov/hcp/return-to-work.html Available at. Accessed April 10, 2020.
- 8.Augestad K.M., Lindsetmo R.O. Overcoming distance: video-conferencing as a clinical and educational tool among surgeons. World J Surg. 2009 Jul;33(7):1356–1365. doi: 10.1007/s00268-009-0036-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Marttos A.C., Jr., Fernandes Juca Moscardi M., Fiorelli R.K.A. Use of telemedicine in surgical education: a seven-year experience. Am Surg. 2018 Aug 1;84(8):1252–1260. [PubMed] [Google Scholar]