To the Editor: On January 7, 2020, a novel coronavirus, severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), was isolated in a patient affected by interstitial pneumonia. As SARS-CoV2 infection has spread worldwide, an increasing number of authors have reported chilblainlike lesions as possible manifestations of SARS-CoV-2 infection.1 , 2
To test this hypothesis, we performed serologic and stool/rectal polymerase chain reaction tests in a cohort of children who developed chilblainlike lesions during the SARS-CoV-2 outbreak in Italy, between March 8 and April 30, 2020.
Enrollment criteria are described in the Supplemental material (available via Mendeley at https://doi.org/10.17632/wzh2tyb46y.2).
During the enrollment period, 35 cases of chilblainlike lesions were eligible for the study. Twenty-four patients agreed to serologic testing (68.6%).
All patients were white, mean age was 13 years (range, 6-17 years), and the female to male ratio was 2:1. Twenty-two patients presented with chilblains on the toes (Fig 1 ) and 2 lesions were located on the heels, 6 patients developed blistering lesions, 83% of lesions lasted more than 14 days, and 8% lasted less than 1 week.
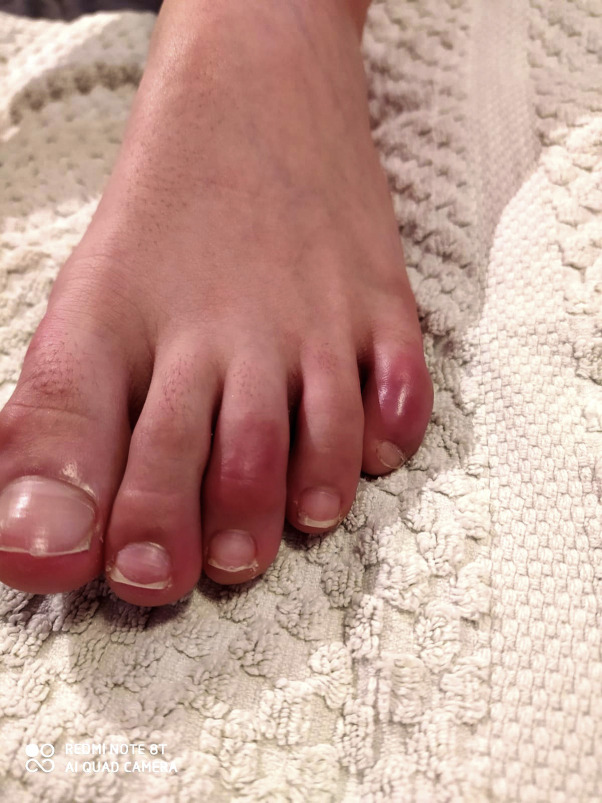
Fig 1.
Typical chilblainlike lesions in a pediatric patient enrolled in the study.
Two patients had known contact with SARS-CoV-2–positive individuals, defined by positive nasal swab result. Seven more patients had close contact with someone who presented symptoms that might be SARS-CoV-2 related such as asthenia, loss of smell (anosmia), cough, and prolonged fever. In 25% of cases, at least 1 parent was a health worker. Further details are available in the Supplemental Results.
Chemiluminescence assay (Liaison SARS-CoV-2 IgG, Diasorin) was performed for all patients; 7 patients were tested with In3diagnostic ERADIKIT COVID19, and the other 17 with EDI Novel Coronavirus COVID-19.
A total of 3 patients (12.5%) tested positive via both enzyme-linked immunosorbent assay and chemiluminescence. In 1 patient (4.1%), enzyme-linked immunosorbent assay test result was positive, whereas chemiluminescence result was negative. None of the 4 patients with positive results presented with fever, 50% had cough, and 25% presented with transient diarrhea up to 14 days before skin lesion appearance. All 4 patients had contact with a relative who had confirmed SARS-CoV-2 infection (2 patients) or anosmia (2 patients). Fecal polymerase chain reaction was tested in 4 patients (16.6%), and no result was positive; rectal swab was performed in 17 patients (70.8%) and was positive in 1, which also was positive at both serologic tests.
Finally, patients with chilblainlike lesions were compared with a cohort of 24 SARS-CoV-2–infected children. Table I shows the comparison between the 2 groups. Chilblain patients were significantly older (13 vs 4 year; P < .001); fever was present in a limited number of cases (16.7% vs 92%; P < .001), and certainty of exposure to SARS-CoV-2 was limited (8% vs 56%; P < .001).
Table I.
Comparison between pediatric cohorts with chilblainlike lesions and severe acute respiratory syndrome coronavirus 2 infection
| Epidemilogical characteristics and symptoms | Chilblains | SARS-CoV-2 infection∗ | P value |
|---|---|---|---|
| No. of patients | 24 | 25 | NA |
| Age, y, (range) | 13 (10.5–14) | 3.8 (0.95–9) | <.001 |
| Female patient, no. (%) | 15 (62.5) | 8 (32) | .04 |
| Skin lesions, no. (%) | 24 (100) | 3 (12) | <.001 |
| Fever, no. (%) | 4 (16.7) | 23 (92) | <.001 |
| Cough, no. (%) | 10 (41.7) | 13 (52) | .5 |
| Conjunctivitis, no. (%) | 3 (12.5) | 0 | .1 |
| GI symptoms, no. (%) | 5 (20.8) | 6 (24) | >.99 |
| Certain exposure to SARS-CoV-2, no. (%) | 2 (8.3) | 14 (56) | <.001 |
The differences between groups were analyzed with Mann-Whitney U test for continuous data and Fisher's exact test for categoric data. All tests were 2 tailed, and the significance was set at P < .05.
GI, Gastrointestinal; NA, not available; SARS-CoV-2, severe acute respiratory syndrome coronavirus 2.
Twenty-two patients hospitalized and 3 evaluated in the emergency department at the Regina Margherita Children's Hospital.
According to our data, the hypothesis of a direct etiologic link between SARS-CoV-2 and chilblain is not confirmed by serologic tests; it is difficult to assess whether in the 4 patients with positive serology SARS-CoV-2 was involved in the pathogenesis of chilblainlike lesions. A limit of our study is the absence of tissue biopsies, so our experimental approach could not rule out the presence of virus in patients' lesions that may induce an interferon-I response.3 As confirmed by other studies,4 the low prevalence (12.5%) of seropositive patients suggests that other pathologic hypotheses should be considered to explain the recent outbreaks of chilblainlike lesions worldwide.
Footnotes
Funding sources: None.
Conflicts of interest: None disclosed.
Reprints not available from the authors.
References
- 1.Piccolo V., Neri I., Filippeschi C., et al. Chilblain-like lesions during COVID-19 epidemic: a preliminary study on 63 patients. J Eur Acad Dermatol Venereol. 2020 doi: 10.1111/jdv.16526. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.de Masson A., Bouaziz J.-D., Sulimovic L., et al. Chilblains are a common cutaneous finding during the COVID-19 pandemic: a retrospective nationwide study from France. J Am Acad Dermatol. 2020;83(2):667–670. doi: 10.1016/j.jaad.2020.04.161. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Kolivras A., Dehavay F., Delplace D., et al. Coronavirus (COVID-19) infection-induced chilblains: a case report with histopathologic findings. JAAD Case Rep. 2020;6(6):489–492. doi: 10.1016/j.jdcr.2020.04.011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Andina D., Noguera-Morel L., Bascuas-Arribas M., et al. Chilblains in children in the setting of COVID-19 pandemic. Pediatr Dermatol. 2020;37(3):406–411. doi: 10.1111/pde.14215. [DOI] [PMC free article] [PubMed] [Google Scholar]