Abstract
Background and aims
The coronavirus disease 2019 (COVID-19) number of death cases is still increasing. One of the comorbidities associated with severe outcome and mortality of COVID-19 is dyslipidemia. Statin is one of the drugs which is most commonly used for the treatment of dyslipidemic patients. This study aims to analyze the association between statin use and in-hospital outcomes of COVID-19 infection.
Methods
We systematically searched the Google Scholar database using specific keywords related to our aims until August 1st, 2020. All articles published on COVID-19 and statin were retrieved. Statistical analysis was done using Review Manager 5.4 software.
Results
A total of 9 studies with a total of 3449 patients were included in our analysis. Our meta-analysis showed that statin use did not improve severity outcome [OR 1.64 (95% CI 0.51–5.23), p = 0.41, I2 = 93%, random-effect modelling] nor mortality rate from COVID-19 infection [OR 0.78 (95% CI 0.50–1.21), p = 0.26, I2 = 0%, fixed-effect modelling].
Conclusion
Statin use did not improve in-hospital outcomes of COVID-19 infections. Patients with dyslipidemia should continue taking statin drugs despite COVID-19 infection status, given its beneficial effects on cardiovascular outcomes.
Keywords: Coronavirus disease 2019, COVID-19, Statin, Dyslipidemia, Treatment
Highlights
-
•
Currently, evidence regarding benefit of statin in COVID-19 is not supported by sufficient human studies.
-
•
Our meta-analysis showed that statin use did not improve in-hospital outcomes of patients with COVID-19 infections.
-
•
Patients with dyslipidemia should continue taking statin if they develop COVID-19.
1. Introduction
Four months have passed since the World Health Organization (WHO) declares the coronavirus disease 2019 (COVID-19) as global pandemic disease. The number of positive and death cases from COVID-19 is still increasing. The manifestation of COVID-19 range from mild respiratory symptoms such as fever and cough to severe and potentially lethal symptoms such as sepsis, arrhythmia, heart failure, and loss of consciousness [1]. Several comorbid conditions, including dyslipidemia, have been identified to be associated with the development of severe outcomes from COVID-19 [2]. One of the drugs most commonly taken by patients with dyslipidemia is a statin. Statin is an HMG-CoA reductase inhibitor that has been long known as an effective cholesterol-lowering agent. Several articles have proposed that statin may be beneficial in improving the outcome of COVID-19 [3,4]. The beneficial effects of statin may be related to its pleiotropic properties. This pleiotropic property of statin is believed to reduce the burden of obesity, cardiovascular disease, and dyslipidemia which are associated with poor outcomes of COVID-19. The pleiotropic effect of statin can down-regulate the CD147 in human cells, including pulmonary cells, therefore can impair the virus’s ability to infect cells and reducing its infectivity [3]. Statin can also prevent or reverse host cell lipid raft alterations induced by COVID-19 infection, which can reduce both cell infection and viral replication. Moreover, pleiotropic properties of statin can exert anti-inflammatory effects by inhibiting NLRP3 inflammasome through the TLR4/MyD88/NF-κB pathway, therefore restraining the uncontrolled inflammation which can be fatal in COVID-19 patients [3]. In silico study by Reiner et al. [4] showed that statin may be an effective SARS-CoV-2 Mpro inhibitors based on its binding energy which is higher than protease or polymerase inhibitors. However, all of these arguments are not yet supported by sufficient in human studies. This study aims to analyze the association between statin use and in-hospital outcomes from COVID-19 infection.
2. Methods
We conducted a systematic search of the literature on Google scholar using the keywords "statin" OR "lipid-lowering drugs" OR "lipid-lowering agents" AND "coronavirus disease 2019" OR "COVID-19", until the present time (August 1st, 2020) with language restricted to English only. The title, abstract, and full text of all articles identified that matched the search criteria were assessed, and those reporting the rate of metformin use in COVID-19 patients with a clinically validated definition of “severe disease” and "mortality" were included in this meta-analysis. The references of all identified studies were also analyzed (forward and backward citation tracking) to identify other potentially eligible articles.
A meta-analysis was performed using Review Manager 5.4 (Cochrane Collaboration) software. Dichotomous variables were calculated using the Mantel-Haenszel formula with fixed-effects models, but we would switch to random-effects models if significant heterogeneity was found. We used the I2 statistic to assess the heterogeneity, value of <25%, 26–50%, and >50% considered as low, moderate, and high degrees of heterogeneity, respectively. The effect estimate was reported as odds ratio (OR) along with its 95% confidence intervals (CIs) for dichotomous variables, respectively. P-value was two-tailed, and the statistical significance set at ≤0.05.
3. Results
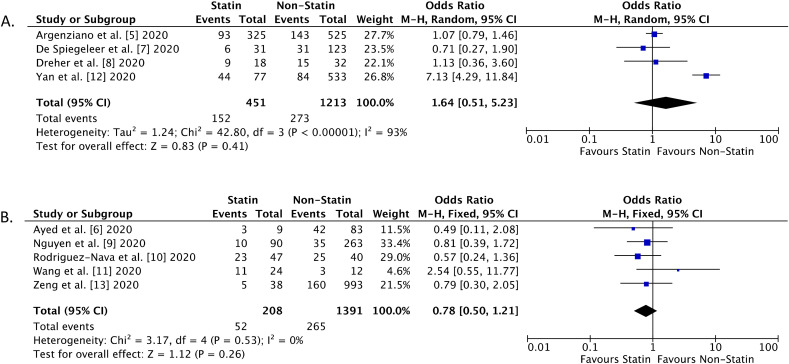
A total of 8350 records were obtained through systematic electronic searches and other ways. After screening titles, abstracts, and full texts, 9 studies [[5], [6], [7], [8], [9], [10], [11], [12], [13]] with a total of 3449 COVID-19 patients were included in the meta-analysis. The essential characteristics of the included studies are summarized in Table 1 . The individual and pooled ORs for the association between statin use and severe outcome of COVID-19 is shown in Fig. 1 A, while the association between statin use and mortality rate from COVID-19 is shown in Fig. 1B. Our pooled analysis showed that statin use did not improve severity outcome [OR 1.64 (95% CI 0.51–5.23), p = 0.41, I 2 = 93%, random-effect modelling] nor mortality rate from COVID-19 infection [OR 0.78 (95% CI 0.50–1.21), p = 0.26, I 2 = 0%, fixed-effect modelling].
Table 1.
Characteristics of included studies.
| Study | Sample size | Design | Age (years) | Outcome | Statin medication |
|
|---|---|---|---|---|---|---|
| Taking (n) | Not taking (n) | |||||
| Argenziano et al. [5] 2020 | 1000 | Case-series | 62.6 ± 18.5 | Severity | 361 (36.1%) | 639 (63.9%) |
| Ayed et al. [6] 2020 | 103 | Retrospective cohort | 53.3 ± 14.1 | Mortality | 10 (9.7%) | 93 (90.3%) |
| De Spiegeller et al. [7] 2020 | 154 | Retrospective cohort | 85.9 ± 7.2 | Severity | 31 (20.1%) | 123 (79.9%) |
| Dreher et al. [8] 2020 | 50 | Retrospective cohort | 66.3 ± 13.3 | Severity | 18 (36%) | 32 (64%) |
| Nguyen et al. [9] 2020 | 356 | Retrospective cohort | 61.3 ± 17 | Mortality | 90 (25.2%) | 266 (74.8%) |
| Rodriguez-Nava et al. [10] 2020 | 87 | Retrospective cohort | 67 ± 12.5 | Mortality | 47 (54%) | 40 (46%) |
| Wang et al. [11] 2020 | 58 | Retrospective cohort | 67 ± 12.5 | Mortality | 27 (46.5%) | 31 (53.5%) |
| Yan et al. [12] 2020 | 610 | Case-control | 48.7 ± 14.1 | Severity | 77 (12.6%) | 533 (87.4%) |
| Zeng et al. [13] 2020 | 1031 | Retrospective cohort | 60.3 ± 14.3 | Mortality | 38 (3.6%) | 993 (96.4%) |
Fig. 1.
Forest plot that demonstrates the association of statin use with the severe outcome (A) and mortality rate (B) from COVID-19 infection.
4. Discussion
Based on our meta-analysis of available data, statin use did not improve severity outcomes and mortality from COVID-19 infection. Several reasons can be proposed to explain this result. First, apart from its beneficial effects through pleiotropic properties, the action of statin on TLR and NF-κB signaling also carry the potential risk of exacerbating compensatory immune signals and poor disease outcome [14]. This theory is supported by a retrospective analysis of the findings from a multicenter clinical trial on the efficacy of rosuvastatin against infection-induced ARDS that showed higher IL-18 levels and mortality in statin-treated patients [15]. Second, statin may cause myotoxicity in some patients that can cause acute kidney injury. Moreover, this adverse effect of statin may be exacerbated when given concomitantly with antiviral agents for COVID-19 such as lopinavir and darunavir. Statins are a substrate for cytochrome P450 (CYP) system, especially 3A isoenzymes and P-glycoproteins (P-gp), while protease inhibitors, such as lopinavir and darunavir are potent inhibitors of both CYP3A and P-gp, so their concomitant administration will result in markedly statin exposure and adverse effects [14]. Therefore, the beneficial effects of statin may be counter-balanced by its potentially harmful effects and causing a neutral effect toward COVID-19. Finally, the anti-inflammatory effects of statin are relatively lower than corticosteroids [16], making statin cannot make a significant alteration in the inflammation or cytokine storm that happened in COVID-19, thus the in-hospital outcome of COVID-19 was not altered by statin administration.
Patients with dyslipidemia should hence be advised to continue taking statin during the COVID-19 pandemic given its potential benefit in reducing the cardiovascular outcomes and its neutral effects toward COVID-19 outcomes. Physicians should also still giving statin into the regime of their dyslipidemic patients’ treatment if the patients have not been given it yet.
This study has several limitations. First, the presence of confounding factors such as age, other comorbid conditions of patients, and other medications that are taken by patients that can affect the relationship between statin and in-hospital outcomes of COVID-19 shall still be considered. Second, no study states the information regarding dosage and duration of statin treatment in their studied samples that can give rise to bias in this study, given that statin must be given at the right dose and sufficient duration of treatment to exert its pleiotropic effects. We hope that this study can give further insight into statin therapy in COVID-19 patients.
Funding
None.
Declaration of competing interest
The authors declare no conflict of interest regarding this article.
Acknowledgment
None.
References
- 1.Kwenandar F., Japar K.V., Damay V., Hariyanto T.I., Tanaka M., Lugito N.P.H. Coronavirus disease 2019 and cardiovascular system: a narrative review. Int J Cardiol Heart Vasc. 2020;29:100557. doi: 10.1016/j.ijcha.2020.100557. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Hariyanto T.I., Kurniawan A. Dyslipidemia is associated with severe coronavirus disease 2019 (COVID-19) infection. Diabetes Metab Syndr. 2020 doi: 10.1016/j.dsx.2020.07.054. 10.1016/j.dsx.2020.07.054. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Rodrigues-Diez R.R., Tejera-Muñoz A., Marquez-Exposito L., Rayego-Mateos S., Santos Sanchez L., Marchant V. Statins: could an old friend help in the fight against COVID-19? Br J Pharmacol. 2020 doi: 10.1111/bph.15166. 10.1111/bph.15166. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Reiner Ž., Hatamipour M., Banach M., Pirro M., Al-Rasadi K., Jamialahmadi T. Statins and the COVID-19 main protease: in silico evidence on direct interaction. Arch Med Sci. 2020;16(3):490–496. doi: 10.5114/aoms.2020.94655. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Argenziano M.G., Bruce S.L., Slater C.L., Tiao J.R., Baldwin M.R., Barr R.G. Characterization and clinical course of 1000 patients with coronavirus disease 2019 in New York: retrospective case series. BMJ. 2020;369:m1996. doi: 10.1136/bmj.m1996. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Ayed M., Borahmah A.A., Yazdani A., Sultan A., Mossad A., Rawdhan H. Assessment of clinical characteristics and mortality-associated factors in COVID-19 critical cases in Kuwait. medRxiv. 2020 doi: 10.1101/2020.06.17.20134007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.De Spiegeleer A., Bronselaer A., Teo J.T., Byttebier G., De Tré G., Belmans L. The effects of ARBs, ACEis, and statins on clinical outcomes of COVID-19 infection among nursing home residents. J Am Med Dir Assoc. 2020;21(7):909–914. doi: 10.1016/j.jamda.2020.06.018. e2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Dreher M., Kersten A., Bickenbach J., Balfanz P., Hartmann B., Cornelissen C. The characteristics of 50 hospitalized COVID-19 patients with and without ARDS. Dtsch Arztebl Int. 2020;117(16):271–278. doi: 10.3238/arztebl.2020.0271. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Nguyen A.B., Upadhyay G.A., Chung B., Smith B., Besser S.A., Johnson J.A. Outcomes and cardiovascular comorbidities in a predominantly Afrian-American population with COVID-19. medRxiv. 2020 doi: 10.1101/2020.06.28.20141929. [DOI] [Google Scholar]
- 10.Rodriguez-Nava G., Trelles-Garcia D.P., Yanez-Bello M.A., Chung C.W., Trelles-Garcia V.P., Friedman H.J. Atorvastatin associated with decreased hazard for death in COVID-19 patients admitted to an ICU: a retrospective cohort study. Crit Care. 2020;24(1):429. doi: 10.1186/s13054-020-03154-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Wang B., Van Oekelen O., Mouhieddine T.H., Del Valle D.M., Richter J., Cho H.J. A tertiary center experience of multiple myeloma patients with COVID-19: lessons learned and the path forward. medRxiv. 2020 doi: 10.1101/2020.06.04.20122846. 2020.06.04.20122846. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Yan H., Valdes A.M., Vijay A., Wang S., Liang L., Yang S. Role of drugs affecting the renin-angiotensin-aldosterone system on susceptibility and severity of COVID-19: a large case-control study from Zheijang Province, China. medRxiv. 2020 doi: 10.1101/2020.04.24.20077875. [DOI] [Google Scholar]
- 13.Zeng H., Zhang T., He X., Du Y., Tong Y., Wang X. Impact of hypertension on progression and prognosis in patients with COVID-19: a retrospective cohort study in 1031 hospitalized cases in Wuhan, China. medRxiv. 2020 doi: 10.1101/2020.06.14.20125997. [DOI] [Google Scholar]
- 14.Dashti-Khavidaki S., Khalili H. Considerations for statin therapy in patients with COVID-19. Pharmacotherapy. 2020;40(5):484–486. doi: 10.1002/phar.2397. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Rogers A.J., Guan J., Trtchounian A., Hunninghake G.M., Kaimal R., Desai M. Association of elevated plasma interleukin-18 level with increased mortality in a clinical trial of statin treatment for acute respiratory distress syndrome. Crit Care Med. 2019;47(8):1089–1096. doi: 10.1097/CCM.0000000000003816. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Vukovic P.M., Maravic-Stojkovic V.R., Peric M.S., Jovic MDj, Cirkovic M.V., Gradinac SDj. Steroids and statins: an old and a new anti-inflammatory strategy compared. Perfusion. 2011;26(1):31–37. doi: 10.1177/0267659110385607. [DOI] [PubMed] [Google Scholar]