Abstract
Background
Since October, 2017 (and until October, 2020), pre-exposure prophylaxis (PrEP) has only been available in England, UK, through the PrEP Impact Trial, by purchasing it from some genitourinary medicine clinics, or via online sources. Here we report changes from 2013 to 2018 in PrEP and postexposure prophylaxis (PEP) awareness and use among HIV-negative gay, bisexual, and other men who have sex with men (MSM) and assess predictors of PrEP initiation.
Methods
In the prospective cohort study Attitudes to, and Understanding of Risk of Acquisition of HIV 2 (AURAH2), MSM were recruited from three sexual health clinics in England: two in London and one in Brighton, UK. Men were eligible if they were aged 18 years or older and HIV-negative or of unknown HIV status. Participants self-completed a baseline paper questionnaire at one of the three clinics between July 30, 2013, and April 30, 2016, and were subsequently able to complete 4-monthly and annual online questionnaires, which were available between March 1, 2015, and March 31, 2018, and collected information on sociodemographics, health and wellbeing, HIV status, and sexual behaviours. PrEP and PEP use in the previous 12 months was obtained at baseline and in annual questionnaires. We assessed trends over calendar time in 3-month periods from first enrolment to the end of the study period (July–December, 2013, was counted as one period) in use of PrEP and PEP using generalised estimating equation logistic models. We used age-adjusted Poisson models to assess factors associated with PrEP initiation among participants who reported never having used PrEP at baseline.
Findings
1162 men completed a baseline questionnaire, among whom the mean age was 34 years (SD 10·4), and of those with available data, 942 (82%) of 1150 were white, 1076 (94%) of 1150 were gay, and 857 (74%) of 1159 were university educated. 622 (54%) of 1162 men completed at least one follow-up online questionnaire, of whom 483 (78%) completed at least one annual questionnaire. Overall, PrEP use in the past year increased from 0% (none of 28 respondents) in July to December, 2013, to 43% (23 of 53) in January to March, 2018. The corresponding increase in PrEP use among men who reported condomless sex with two or more partners was from 0% (none of 13 respondents) to 78% (21 of 27). PEP use peaked in April to June, 2016, at 28% (41 of 147 respondents), but decreased thereafter to 8% (four of 53) in January to March, 2018. Among 460 men who had never used PrEP at baseline, predictors of initiating PrEP included age 40–44 years (incidence rate ratio [IRR] 4·25, 95% CI 1·14–15·79) and 45 years and older (3·59, 1·08–11·97) versus younger than 25 years; and after adjustment for age, recent HIV test (5·17, 1·89–14·08), condomless sex (5·01, 2·16–11·63), condomless sex with two or more partners (5·43, 2·99–9·86), group sex (1·69, 1·01–2·84), and non-injection chemsex-related drugs use (2·86, 1·67–4·91) in the past 3 months, PEP use (4·69, 2·83–7·79) in the past 12 months, and calendar year (Jan 1, 2017, to March 31, 2018 vs July 30, 2013, to Dec 31, 2015: 21·19, 9·48–47·35). Non-employment (0·35, 0·14–0·91) and unstable or no housing (vs homeowner 0·13, 0·02–0·95) were associated with reduced rates of PrEP initiation after adjustment for age. About half of PrEP was obtained via the internet, even after the PrEP Impact trial had started (11 [48%] of 23 respondents in January to March, 2018).
Interpretation
PrEP awareness and use increased substantially from 2013 to 2018 among a cohort of MSM in England. Improving access to PrEP by routine commissioning by National Health Service England could increase PrEP use among all eligible MSM, but should include public health strategies to target socioeconomic and demographic disparities in knowledge and use of PrEP.
Funding
National Institute for Health Research.
Introduction
The PROUD study, an open-label randomised controlled trial carried out at 13 sites in England, UK, in 2015, reported that daily oral pre-exposure prophylaxis (PrEP) with tenofovir–emtricitabine resulted in an 86% reduction in HIV infection in gay, bisexual, and other men who have sex with men (hereafter referred to as men who have sex with men [MSM]).1 A subsequent modelling study has shown that the introduction of a PrEP programme for MSM in the UK would be cost-effective and possibly cost-saving in the long term.2 In England, PrEP is freely available to people at risk of HIV only in the context of the PrEP Impact trial by Public Health England that launched across England in October, 2017. All trial participants will get National Health Service (NHS) England funded PrEP until at least October, 2020 (the end of the trial). Otherwise, people can legally purchase PrEP for their own use via the internet or from some genitourinary medicine clinics. A nationally commissioned PrEP programme for England has been agreed and should be operational by the end of the PrEP Impact trial.
Research in context.
Evidence before this study
Pre-exposure prophylaxis (PrEP) taken daily or on-demand has been shown to be highly effective for prevention of HIV infection among men who have sex with men (MSM) in clinical trials and open-label studies. PrEP is recommended by WHO for HIV-negative individuals at substantial risk of sexually acquired HIV, including MSM. We searched PubMed for longitudinal cohort studies in English that included MSM in England, UK, published from database inception up to Jan 31, 2020, using key search terms including “pre-exposure prophylaxis”, “PrEP”, “HIV”, “MSM”, “homosexual”, “men who have sex with men”, “gay”, “bisexual men”, “longitudinal”, “cohort”, and “prospective”. We identified 83 articles, which included articles of clinical trials, demonstration projects, and cohort studies mostly done in high-income countries. Apart from reports on PrEP uptake and associated factors, among these articles were studies about sexual behaviours, sexually transmitted infections, and HIV incidence among PrEP users; PrEP awareness, acceptability, and willingness to use; PrEP retention, engagement, adherence, and discontinuation; and characteristics of PrEP users. We identified two studies run in England, two articles from the PROUD trial, and one article from our research group (the Attitudes to, and Understanding of Risk of Acquisition of HIV [AURAH] and AURAH2 study) that measured changes in the prevalence of sexual behaviours and PrEP use, by comparing data from the AURAH cross-sectional study with baseline data from the AURAH2 prospective cohort. To our knowledge, no data have been published from longitudinal cohort studies in England, excluding those from clinical trials or PrEP demonstration projects.
Added value of this study
This study provides the first estimates of trends in PrEP use and predictors of PrEP initiation among HIV-negative MSM in England, using data from a prospective cohort, at a critical time in planning the roll-out of PrEP in England. We found that, despite free PrEP availability in England being only through the PrEP Impact trial, both awareness and use of PrEP increased substantially from 2013 to 2018 among MSM attending three sexual health clinics in south-east England. In 2018, PrEP use was almost 80% among men with multiple condomless sex partners. A substantial proportion of men accessing PrEP obtained it via the internet. PrEP use was lower among those with lower socioeconomic status than among those of higher socioeconomic status.
Implications of all the available evidence
The available evidence highly supports the addition of PrEP to the standard of care for MSM who would benefit from the preventive prophylaxis. Sociodemographic and economic barriers associated with PrEP use should be promptly addressed via routine commissioning of PrEP.
Among gay and bisexual men in the UK, modelling of available data suggests that the estimated annual number of new HIV infections has decreased by 71%, from 2800 in 2012, to 800 in 2018.3 The annual number of HIV diagnoses recorded among gay and bisexual men in the UK has also decreased by 35%, from 3480 in 2014, to 2250 in 2018.3 Based on a CD4 cell count back-calculation model, the modelled number of incident infections among gay and bisexual in England has decreased by 65% since 2014, with the most rapid decrease occurring after 2016.3 A combination of PrEP scale-up, a large increase in ever and repeat HIV testing, and rapid antiretroviral therapy initiation at diagnosis are most likely responsible for these steep decreases in new infections, largely among MSM.4 Similar decreases in HIV diagnoses among MSM have also been reported in San Francisco, CA, and New York City, NY, in the USA,5, 6 and New South Wales, Australia.7
To date, little information exists on trends in PrEP awareness and uptake and predictors of PrEP initiation in England. Such data would be helpful to further inform the unrestricted PrEP implementation programme in England in 2020, in which PrEP will be made routinely available after completion of the PrEP Impact trial.8
The Attitudes to, and Understanding of Risk of Acquisition of HIV 2 (AURAH2) study is among the first prospective cohort studies of MSM in England. We assessed changes in awareness of, and use of, PrEP and postexposure prophylaxis (PEP), predictors of PrEP initiation, and factors associated with reporting the recent use of PrEP among initially HIV-negative MSM between 2013 and 2018.
Methods
Study design and participants
The AURAH2 study was a prospective cohort study that recruited MSM who were HIV negative or of unknown HIV status from two large sexual health clinics in London (56 Dean Street and Mortimer Market Centre) and one in Brighton (Claude Nicol clinic), between July 30, 2013, and April 30, 2016.9 Additionally, participants were eligible if they were aged 18 years or older and attending or had attended the study clinics for routine sexually transmitted infection (STI) or HIV testing. Individuals who consented to participation in the study completed a confidential baseline paper questionnaire in the clinic. During the follow-up period, participants self-completed subsequent 4-monthly and annual questionnaires that were available online from March, 2015, until March, 2018; hence, maximum follow-up was 3 years. The baseline and follow-up questionnaires gathered information on demographic and socioeconomic factors, health and wellbeing, knowledge and understanding of HIV, lifestyle, sexual health, recent sexual behaviour, and PrEP and PEP use. The study protocol has been described previously.9
All participants provided written informed consent before taking part. The AURAH2 study was approved by the designated research ethics committee, The National Research Ethics Service committee London-Hampstead (14/LO/1881), in November, 2014. Based on the research protocol and all versions of study documents, the AURAH2 study subsequently received permission for clinical research at three participating NHS sites: Chelsea and Westminster NHS Foundation Trust, Central and North West London NHS Foundation Trust, and the Brighton and Sussex University Hospitals NHS Trust.
Measures
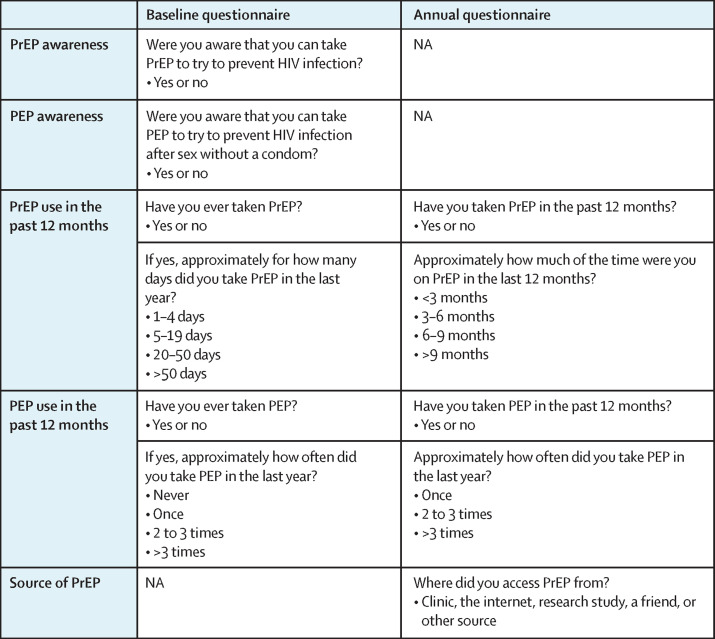
All measures were self-reported from participant questionnaires. Information on PrEP and PEP use was collected in the baseline and annual questionnaires, with information on PrEP and PEP awareness collected at baseline only. The main outcomes of interest were PrEP and PEP awareness and reported PrEP and PEP use in the previous 12 months. Study definitions and questions are shown in figure 1 . To be classified as positive for having taken PrEP or PEP in the past 12 months, at baseline or at the annual questionnaire, participants were required to have answered “yes” to the question on having ever taken PrEP or PEP, and subsequently indicated use in the past year on the question on frequency of use. Missing answers to PrEP and PEP use questions were classified as no use.
Figure 1.
PrEP and PEP measures in the AURAH2 study*
AURAH2=Attitudes to and Understanding of Risk of Acquisition of HIV 2. NA=not applicable. PrEP=pre-exposure prophylaxis. PEP=postexposure prophylaxis. *PrEP data were not collected in the 4-monthly online questionnaire.
Sociodemographic variables of interest included age group (<25, 25–29, 30–34, 35–39, 40–44, ≥45 years), country of birth and ethnicity (white UK born, other ethnicity UK born, white non-UK born, other ethnicity non-UK born), sexual identity (gay, bisexual or other), university education (yes, no), ongoing relationship (yes, no), employment status (employed, not employed), sufficient money for basic needs (all of the time, most of the time, sometimes or no), and housing status (homeowner, renting, unstable or other). We considered the following seven measures of HIV risk and related behaviours and activities (in the past 3 months, unless otherwise stated): condomless anal sex (condomless sex), condomless sex with two or more partners, group sex (sex involving more than two participants on the same occasion), recreational drug use classified into four groups (none; drug use but not injection or chemsex-related; use of at least one chemsex-related drug [crystal methamphetamine, γ-hydroxybutyrate (GHB), γ-butyrolactone (GBL), or mephedrone] but no injection drug use; injection drug use), STI diagnosis (in the past 12 months at the baseline questionnaire, and in the past 3 months at the annual questionnaire), PrEP or PEP use in the past 12 months, and having had a recent HIV test (in the past 6 months at the baseline questionnaire, and in the past 3 months at the annual questionnaire). Mental health and lifestyle factors of interest included depressive symptoms (a score of ≥10 on the Patient Health Questionnaire-9),10 anxiety symptoms (a score of ≥10 on the Generalised Anxiety Disorder-7 test),11 and higher alcohol consumption (a score of ≥6 on the WHO alcohol screening tool audit, Alcohol Use Disorders Identification Test-consumption [AUDIT-C], questionnaire; first two questions only).12 Ethnicity, sexual identity, education, employment, financial status, and housing status were fixed variables derived from the baseline questionnaire, whereas age, depressive symptoms, anxiety symptoms, alcohol consumption, and HIV risk and related behaviours were time-varying variables derived from baseline and annual questionnaires. We treated missing values as “no” answers (these accounted for <5% for each variable), except for the few individuals with missing values for the variables of age, country of birth and ethnicity, sexual identity, financial status, and housing status, who were excluded from analyses for those variables.
Statistical analysis
In preparation for the analyses, we considered calendar year 3-month periods from the first enrolment (July, 2013) to the end of the study period (March, 2018). Information from each participant's questionnaires was ascribed to the 3-month period in which the questionnaire was completed. We combined data for the last two quarters of 2013 as one calendar period (July–December, 2013) because recruitment started on July 30, 2013, and so the third quarter of 2013 was less than 3 months; the number recruited by September, 2013, was too small to have a separate period. To describe the prevalence of PrEP and PEP awareness at baseline, we used data from all available baseline questionnaires. We assessed trends over calendar time in the proportion of participants who indicated PrEP and PEP awareness at baseline over the period from July, 2013, to April, 2016 (enrolment stage), and did a χ2 test for linear trends in proportions.
To examine trends in past 12-month PrEP and PEP use over the entire study period, we used pooled data from all available baseline and annual questionnaires. We used univariate generalised estimation equation (GEE) models with a logit link and robust SEs to assess trends over calendar time during the period July, 2013, to March, 2018, in the proportion of questionnaires for which PrEP and PEP use were reported, accounting for multiple questionnaire responses from individual participants. Calendar year was fitted as a continuous variable to obtain a test for linear trend. Similarly, we investigated trends over calendar time in the proportion of men who reported condomless sex with two or more partners, and trends in PrEP use among these men specifically. We also assessed trends over time (in 6-month calendar periods) in source of PrEP, using questionnaires in which PrEP use was reported.
We assessed, in a longitudinal analysis, factors associated with PrEP initiation during follow-up among those who reported not using PrEP at baseline and who had completed at least one annual questionnaire. PrEP initiation was defined as the first report of PrEP use in the past 12 months from an annual questionnaire; time to initiation was the time from baseline to the date of completion of the questionnaire in which PrEP was first reported, or from baseline to the end of follow-up if PrEP was not initiated. We considered each factor separately in age-adjusted Poisson models (using age as a continuous variable) with robust SEs. The predictors considered included sociodemographic factors, mental health, lifestyle factors, and sexual health and behaviours reported in past questionnaires associated with subsequent PrEP initiation. We present these results as age-adjusted incidence rate ratios (IRRs) with their corresponding 95% CIs.
We did an additional cross-sectional analysis to examine factors associated with being on PrEP, using all available baseline and annual questionnaires. We used GEE models with a logit link function, adjusted for age (as a continuous variable). Also, separately among PrEP users, we analysed factors associated with reporting non-prescribed PrEP (ie, PrEP obtained via the internet, friends, or others sources) using all available annual questionnaires in which PrEP use was reported. We present these results as age-adjusted odds ratios (ORs) with their corresponding 95% CIs.
p values below 0·05 were considered to be significant. We did all analyses using STATA (version 15.1).
Role of the funding source
The funder had no role in study design, data collection, data analysis, data interpretation, or writing of the report. The corresponding author had full access to all the data in the study and had final responsibility for the decision to submit for publication.
Results
1162 men enrolled in the study between July 30, 2013, and April 30, 2016 (table 1 ). The mean age at baseline was 34 years (SD 10·4). Of those with available data, participants were predominantly of white ethnicity (942 [82%] of 1150), self-reported being gay (1076 [94%] of 1150), had a university degree (857 [74%] of 1159), reported being employed (1053 [91%] of 1159), and always had money to cover basic needs (896 [77%] of 1158). Regarding sexual behaviour in the past 3 months, 741 (64%) of 1159 men reported condomless sex, 410 (35%) of 1159 reported condomless sex with two or more partners, 500 (43%) of 1159 reported group sex, and 695 (60%) of 1159 reported the use of at least one recreational drug; including 38 (3%) who reported injection drug use. In the previous 12 months, 440 (38%) of 1159 men reported they had been diagnosed with an STI, 240 (21%) reported taking PEP, and 58 (5%) reported taking PrEP.
Table 1.
Baseline sociodemographic, health and lifestyle characteristics, sexual behaviour, and PrEP and PEP use among participants who completed the baseline, follow-up, and annual questionnaires in the AURAH2 study, 2013–18
| Completed baseline questionnaire (n=1162) | Completed at least one follow-up questionnaire (n=622) | Completed at least one annual questionnaire (n=483) | ||
|---|---|---|---|---|
| Sociodemographics | ||||
| Age, years | ||||
| Mean | 34 (10·4) | 34 (11·3) | 35 (11·2) | |
| Median | 31 (26–39) | 33 (26–41) | 33 (26–42) | |
| <25 | 275/1153 (23·9%) | 132/613 (21·5%) | 103/479 (21·5%) | |
| 25–29 | 207/1153 (17·9%) | 86/613 (14·0%) | 69/479 (14·4%) | |
| 30–34 | 226/1153 (19·6%) | 121/613 (19·8%) | 87/479 (18·2%) | |
| 35–39 | 157/1153 (13·6%) | 89/613 (14·5%) | 68/479 (14·2%) | |
| 40–44 | 121/1153 (10·5%) | 70/613 (11·4%) | 55/479 (11·5%) | |
| ≥45 | 167/1153 (14·5%) | 114/613 (18·6%) | 97/479 (20·2%) | |
| Country of birth and ethnicity | ||||
| Born in the UK, white | 568/1150 (49·4%) | 317/611 (51·9%) | 262/479 (54·7%) | |
| Born in the UK, other ethnicity* | 60/1150 (5·2%) | 29/611 (4·7%) | 20/479 (4·2%) | |
| Non-UK born, white | 374/1150 (32·5%) | 195/611 (31·9%) | 149/479 (31·1%) | |
| Non-UK born, other ethnicity* | 148/1150 (12·9%) | 70/611 (11·5%) | 48/479 (10·0%) | |
| Sexual identity | ||||
| Gay | 1076/1150 (93·6%) | 581/614 (94·6%) | 455/480 (94·8%) | |
| Bisexual or other | 74/1150 (6·4%) | 33/614 (5·4%) | 25/480 (5·2%) | |
| University education | ||||
| Yes | 857/1159 (73·9%) | 471/619 (76·1%) | 365/483 (75·6%) | |
| No | 302/1159 (26·1%) | 148/619 (23·9%) | 118/483 (24·4%) | |
| Employed | ||||
| Yes | 1053/1159 (90·9%) | 548/619 (88·5%) | 431/483 (89·2%) | |
| No | 106/1159 (9·1%) | 71/619 (11·5%) | 52/483 (10·8%) | |
| Money to cover basic needs | ||||
| All of the time | 896/1158 (77·4%) | 509/618 (82·4%) | 404/481 (84·0%) | |
| Most of the time | 194/1158 (16·8%) | 81/618 (13·1%) | 58/481 (12·1%) | |
| Sometimes or no | 68/1158 (5·8%) | 28/618 (4·5%) | 19/481 (3·9%) | |
| Housing status† | ||||
| Homeowner | 314/1147 (27·4%) | 200/607 (33·0%) | 168/475 (35·4%) | |
| Renting | 680/1147 (59·3%) | 328/607 (54·0%) | 250/475 (52·6%) | |
| Unstable or other | 153/1147 (13·3%) | 79/607 (13·0%) | 57/475 (12·0%) | |
| HIV risk and behaviours | ||||
| Ongoing relationship | ||||
| Yes | 465/1159 (40·1%) | 257/619 (41·5%) | 202/481 (42·0%) | |
| No | 694/1159 (59·9%) | 362/619 (58·5%) | 279/481 (58·0%) | |
| Recent HIV test | ||||
| No | 322/1159 (27·8%) | 155/619 (25·0%) | 123/481 (25·6%) | |
| Yes | 837/1159 (72·2%) | 464/619 (75·0%) | 358/481 (74·4%) | |
| Condomless sex in the past 3 months | ||||
| No | 418/1159 (36·1%) | 224/619 (36·2%) | 172/480 (35·8%) | |
| Yes | 741/1159 (63·9%) | 395/619 (63·8%) | 308/480 (64·2%) | |
| Condomless sex with ≥2 partners in past 3 months | ||||
| No | 749/1159 (64·6%) | 385/619 (62·2%) | 299/480 (62·3%) | |
| Yes | 410/1159 (35·4%) | 234/619 (37·8%) | 181/480 (37·7%) | |
| Group sex in the past 3 months | ||||
| No | 659/1159 (56·9%) | 327/619 (52·8%) | 247/480 (51·5%) | |
| Yes | 500/1159 (43·1%) | 292/619 (47·2%) | 233/480 (48·5%) | |
| Recreational drug use | ||||
| None | 464/1159 (40·0%) | 229/619 (37·0%) | 181/480 (37·7%) | |
| Drug use, non-injection, non-chemsex-related | 336/1159 (29·0%) | 179/619 (28·9%) | 145/480 (30·2%) | |
| Use of ≥1 chemsex-related drug, non-injection | 321/1159 (27·7%) | 192/619 (31·0%) | 139/480 (29·0%) | |
| Injection drug use | 38/1159 (3·3%) | 19/619 (3·1%) | 15/480 (3·1%) | |
| STI diagnoses‡ | ||||
| No | 719/1159 (62·0%) | 384/619 (62·0%) | 297/480 (61·9%) | |
| Yes | 440/1159 (38·0%) | 235/619 (38·0%) | 183/480 (38·1%) | |
| PEP use in the past 12 months | ||||
| No | 919/1159 (79·3%) | 496/619 (80·1%) | 387/481 (80·5%) | |
| Yes | 240/1159 (20·7%) | 123/619 (19·9%) | 94/481 (19·5%) | |
| PrEP use in the past 12 months | ||||
| No | 1101/1159 (95·0%) | 589/619 (95·2%) | 460/481 (95·6%) | |
| Yes | 58/1159 (5·0%) | 30/619 (4·8%) | 21/481 (4·4%) | |
| Mental health and lifestyle | ||||
| Higher risk alcohol consumption§ | ||||
| No | 1008/1159 (87·0%) | 537/619 (86·8%) | 418/483 (86·5%) | |
| Yes | 151/1159 (13·0%) | 82/619 (13·2%) | 65/483 (13·5%) | |
| Depressive symptoms¶ | ||||
| No | 1018/1159 (87·8%) | 544/619 (87·9%) | 424/483 (87·8%) | |
| Yes | 141/1159 (12·2%) | 75/619 (12·1%) | 59/483 (12·2%) | |
| Anxiety symptoms‖ | ||||
| No | 1033/1159 (89·1%) | 562/619 (90·8%) | 440/483 (91·1%) | |
| Yes | 126/1159 (10·9%) | 57/619 (9·2%) | 43/483 (8·9 %) | |
Data are n/N (%), mean (SD), or median (IQR). Data are from baseline paper questionnaire. Condomless sex refers to condomless anal sex. Data are missing from the baseline questionnaire as follows: age (n=9), money status (n=4), housing status (n=15); country of birth and ethnicity (n=12), sexual identity (n=12), university education (n=3), employment (n=3), relationship (n=3), HIV test (n=3), condomless sex in the past 3 months (n=3), condomless sex with ≥2 partners in the past 3 months (n=3), group sex in the past 3 months (n=3), PEP use (n=3), PrEP use (n=3), recreational drug use (n=3), STI diagnoses (n=3), alcohol consumption (n=3), depressive symptoms (n=3), and anxiety symptoms (n=3). AURAH2=Attitudes to and Understanding of Risk of Acquisition of HIV 2. PrEP=pre-exposure prophylaxis. PEP=postexposure prophylaxis. STI=sexually transmitted infection.
Other ethnicity includes Black, Asian, Mixed, and other ethnic groups.
Renting housing includes private renting and renting from council or housing association; unstable or other housing includes temporary accommodation, staying with friends or family, other accommodation, and homeless.
In the past 12 months at the baseline questionnaire and in the past 3 months at the annual questionnaire.
Higher risk defined as a score of ≥6 on the WHO modified alcohol screening tool audit, Alcohol Use Disorders Identification Test-consumption, questionnaire.
Defined as a score of ≥10 on the Patient Health Questionnaire-9.
Defined as a score of ≥10 on the Generalised Anxiety Disorder-7.
622 (54%) of 1162 men completed at least one online follow-up questionnaire, of whom 483 (78%) completed at least one annual questionnaire. A higher proportion of participants who were older, had greater financial security, and with more stable housing status continued on the study than did those who were younger, who only sometimes or did not have money to cover basic needs and who had unstable or no housing (table 1). The number of follow-up questionnaires (4-monthly and annual) completed by the end of the study period was 3277.
To describe PrEP and PEP awareness at enrolment by calendar period of baseline questionnaire, we used data from 1161 of 1162 participants who completed a baseline questionnaire (one questionnaire was excluded from the analysis due to missing data). Overall, at baseline, 838 (72%) of 1161 participants were aware of PrEP and 1074 (93%) were aware of PEP. The proportion of men who at baseline reported PrEP awareness increased significantly over calendar time of recruitment, from 12 (43%) of 28 men recruited in July to December, 2013, to 58 (92%) of 63 men recruited in April to June, 2016 (ptrend<0·0001; breakdown by quarters not shown). The awareness of PEP was already high in the first period of recruitment (26 [93%] of 28 men recruited in July to December, 2013) and remained so over the recruitment period (61 [97%] of 63 recruited in April to June, 2016; ptrend=0·69).
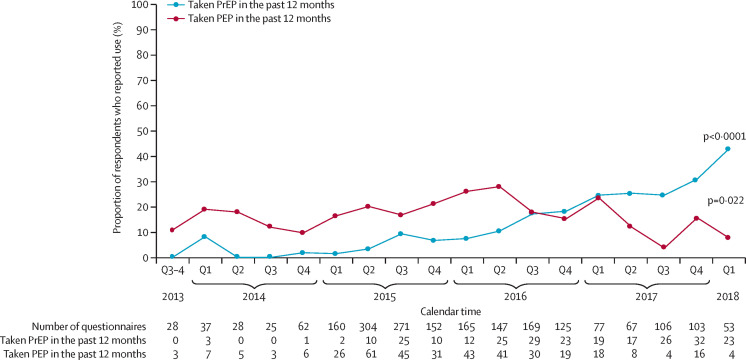
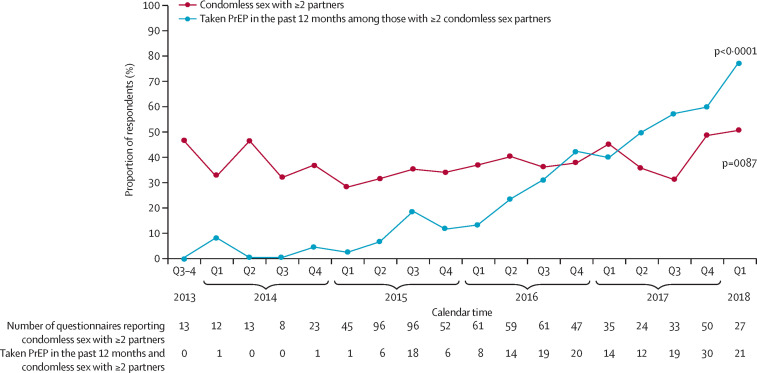
To describe changes in past 12 month PrEP and PEP use over calendar time, we used data from 2079 questionnaires (baseline and annual follow-up) from 1161 participants. Overall, PrEP use in the past 12 months was reported in 248 (12%) questionnaires. PrEP use increased significantly from 0% (none of 28 respondents) in the last two quarters of 2013 to 43% (23 of 53) by January to March, 2018 (p value for linear trend from GEE-logistic model <0·0001; figure 2 ). By contrast, some fluctuation was seen in the trend of past 12-month use of PEP. PEP use was reported in 371 (18%) questionnaires. PEP use was consistently higher than PrEP use until the period July to September, 2016, but after reaching a peak of 28% (41 of 147 respondents) in April to June, 2016, the proportion of men who reported PEP use began to decrease significantly to a low of 8% (four of 53 respondents) by January to March, 2018 (p value for linear trend from GEE = 0·022). From the 2079 questionnaires (of which one questionnaire was excluded from analysis due to missing data on year of enrolment), 755 (36%) reported condomless sex with two or more partners; we observed a slight increase in this prevalence from 46% (13 of 28 respondents) in the period July to December, 2013, to 51% (27 of 53) in January to March, 2018 (p value for linear trend from GEE = 0·087). Of 755 questionnaires, 190 (25%) reported having taken PrEP in the past 12 months. PrEP use increased significantly among men who reported condomless sex with two or more partners, from 0% (none of 13 respondents) in July to December, 2013, to 78% (21 of 27) in January to March, 2018 (p value for linear trend from GEE <0·0001; figure 3 ).
Figure 2.
Prevalence of PrEP and PEP use in the past 12 months over time among MSM, 2013–18
Data are from baseline and annual questionnaires, missing values on use of PrEP and PEP questions were treated as “no” answers. 1161 participants provided 2079 questionnaires; one questionnaire was excluded from the analysis due to missing data on year of enrolment. p values are for linear trends. MSM=men who have sex with men. PrEP=pre-exposure prophylaxis. PEP=postexposure prophylaxis. Q=quarter.
Figure 3.
Prevalence of condomless sex with two or more partners and prevalence of PrEP use among these men, 2013–18
Data for condomless sex with ≥2 partners are from all baseline and annual questionnaires (ie, 1161 participants provided 2079 questionnaires; one questionnaire was excluded from the analysis due to missing data on year of enrolment). Data on PrEP use in the past 12 months is from those with ≥2 condomless sex partners at baseline and in the annual questionnaires (n=755 questionnaires; one questionnaire was excluded from the analysis due to missing data on year of enrolment). Condomless sex is condomless anal sex. p values are for linear trends. PrEP=pre-exposure prophylaxis. Q=quarter.
Of all available annual questionnaires that reported PrEP sources (n=190), 112 (59%) indicated PrEP had been obtained from the internet, 65 (34%) from clinics, and 13 (7%) from friends or other sources. In October, 2017, to March, 2018, (after the PrEP Impact trial started), the proportion of respondents who reported sourcing PrEP from the internet was 65% (36 of 55), from a clinic was 25% (14 of 55), and from friends or other sources was 9% (five of 55). The proportion of respondents who reported PrEP use who also reported sourcing their PrEP from the internet increased over time. This proportion was 0% (none of 12) in the period of July to December, 2015, 67% (six of nine) in January to June, 2016, 58% (30 of 52) in July to December, 2016, 67% (24 of 36) in January to June, 2017, 71% (41 of 58) in July to December, 2017 (the period in which the Impact Trial started), and 48% (11 of 23) in January to March, 2018.
To examine factors associated with initiating PrEP, we restricted our analysis to the 460 participants who reported no previous PrEP use in the baseline questionnaire and who completed at least one annual follow-up questionnaire (data from 875 questionnaires). Age-adjusted IRRs for factors associated with initiating PrEP are shown in table 2 . The PrEP initiation rate increased substantially from 2013 to 2018. When considering year as a continuous variable, the age-adjusted IRR per calendar year was 5·91 (3·68–9·49; p<0·0001). Compared with the category of younger than 25 years, rate of PrEP initiation was increased in the age categories of 40–44 years and age 45 years and older. In age-adjusted models, non-employment and unstable housing were significantly associated with a reduced rate of PrEP initiation compared with being a homeowner. Behavioural factors associated with higher rates of PrEP initiation within the past 12 months were having a recent HIV test; reporting condomless sex; condomless sex with two or more partners, group sex, use of non-injected chemsex-related drugs, and use of PEP in the past 12 months (table 2).
Table 2.
Longitudinal analysis of factors associated with initiating PrEP and cross-sectional analysis of factors associated with being on PrEP in the previous 12 months
|
Predictors of initiating PrEP (n=460)* |
Factors associated with past 12-month use of PrEP (n=1162)† |
||||
|---|---|---|---|---|---|
| Age-adjusted IRR (95% CI) | p value | Age-adjusted OR (95% CI) | p value | ||
| Age (time-updated) per year‡ | 1·02 (1·01–1·04) | 0·0010 | 1·04 (1·03–1·05) | <0·0001 | |
| Age (time-updated) category, years‡ | |||||
| <25 | 1 (ref) | 0·0050 | 1 (ref) | <0·0001 | |
| 25–29 | 1·76 (0·47–6·56) | .. | 1·13 (0·49–2·57) | .. | |
| 30–34 | 2·42 (0·69–8·45) | .. | 2·86 (1·44–5·68) | .. | |
| 35–39 | 1·93 (0·49–7·59) | .. | 3·04 (1·47–6·29) | .. | |
| 40–44 | 4·25 (1·14–15·79) | .. | 3·89 (1·80–8·36) | .. | |
| ≥45 | 3·59 (1·08–11·97) | .. | 3·54 (1·77–7·09) | .. | |
| Country of birth and ethnicity | |||||
| Born in the UK, white | 1 (ref) | 0·42 | 1 (ref) | 0·52 | |
| Born in the UK, other ethnicity§ | 1·52 (0·46–5·03) | .. | 1·74 (0·84–3·59) | .. | |
| Non-UK born, white | 1·19 (0·68–2·11) | .. | 1·17 (0·79–1·71) | .. | |
| Non-UK born, other ethnicity§ | 1·34 (0·56–3·24) | .. | 1·08 (0·63–1·87) | .. | |
| Sexual identity | |||||
| Bisexual or other | 1 (ref) | 0·79 | 1 (ref) | 0·29 | |
| Gay | 1·21 (0·29–4·95) | .. | 1·53 (0·69–3·38) | .. | |
| University education | |||||
| Yes | 1 (ref) | 0·24 | 1 (ref) | 0·63 | |
| No | 0·67 (0·34–1·31) | .. | 0·91 (0·63–1·32) | .. | |
| Employed | |||||
| Yes | 1 (ref) | 0·032 | 1 (ref) | 0·078 | |
| No | 0·35 (0·14–0·91) | .. | 0·58 (0·32–1·06) | .. | |
| Money to cover basic needs | |||||
| All of the time | 1 (ref) | 0·070¶ | 1 (ref) | 0·12‖ | |
| Most of the time | 1·04 (0·45–2·37) | .. | 0·83 (0·52–1·32) | .. | |
| Sometimes or no | 0·57 (0·08–3·86) | .. | 0·52 (0·21–1·31) | .. | |
| Housing status | |||||
| Homeowner | 1 (ref) | 0·025 | 1 (ref) | 0·031 | |
| Renting | 0·56 (0·29–1·07) | .. | 0·71 (0·47–1·06) | .. | |
| Unstable or other | 0·13 (0·02–0·95) | .. | 0·36 (0·18–0·73) | .. | |
| Ongoing relationship | |||||
| Yes | 1 (ref) | 0·88 | 1 (ref) | 0·48 | |
| No | 0·96 (0·57–1·61) | .. | 0·88 (0·63–1·24) | .. | |
| Recent HIV test | |||||
| No | 1 (ref) | 0·0010 | 1 (ref) | <0·0001 | |
| Yes | 5·17 (1·89-14·08)** | .. | 2·73 (1·93–3·87)†† | .. | |
| Condomless sex in the past 3 months | |||||
| No | 1 (ref) | <0·0001 | 1 (ref) | <0·0001 | |
| Yes | 5·01 (2·16–11·63) | .. | 4·57 (2·91–7·17) | .. | |
| Condomless sex with ≥2 partners in the past 3 months | |||||
| 0 or 1 | 1 (ref) | <0·001 | 1 (ref) | <0·0001 | |
| ≥2 | 5·43 (2·99–9·86) | .. | 5·64 (3·97–8·01) | .. | |
| Group sex in the past 3 months | |||||
| No | 1 (ref) | 0·045 | 1 (ref) | 0·0010 | |
| Yes | 1·69 (1·01–2·84) | .. | 1·77 (1·26–2·47) | .. | |
| PEP use in the previous 12 months | |||||
| No | 1 (ref) | <0·0001 | 1 (ref) | 0·0070 | |
| Yes | 4·69 (2·83–7·79) | .. | 1·78 (1·17–2·71) | .. | |
| Recreational drug use | |||||
| None | 1 (ref) | 0·0020 | 1 (ref) | <0·0001 | |
| Drug use, non-injection, non-chemsex-related | 0·39 (0·05–2·83) | .. | 0·82 (0·29–2·27) | .. | |
| Use of ≥1 chemsex-related drug, non-injection | 2·86 (1·67–4·91) | .. | 2·70 (1·91–3·81) | ||
| Injection drug use | 1·00 (0·12–7·42) | .. | 1·76 (0·79–3·91) | ||
| STI diagnoses | |||||
| No | 1 (ref) | 0·81 | 1 (ref) | 0·73 | |
| Yes | 1·07 (0·59–1·98) | .. | 1·07 (0·75–1·53) | .. | |
| Higher risk alcohol consumption | |||||
| No | 1 (ref) | 0·97 | 1 (ref) | 0·12 | |
| Yes | 1·01 (0·49–2·09) | .. | 0·63 (0·35–1·13) | .. | |
| Depressive symptoms | |||||
| No | 1 (ref) | 0·76 | 1 (ref) | 0·11 | |
| Yes | 0·87 (0·35–2·15) | .. | 0·62 (0·35–1·11) | .. | |
| Anxiety symptoms | |||||
| No | 1 (ref) | .. | 1 (ref) | .. | |
| Yes | 1·30 (0·52–3·24) | 0·57 | 0·75 (0·39–1·41) | 0·35 | |
| Calendar year | 5·91 (3·68–9·49) | <0·0001 | 2·43 (2·12–2·79) | <0·0001 | |
| Calendar year category | |||||
| July 30, 2013–Dec 31, 2015 | 1 (ref) | <0·0001 | 1 (ref) | <0·0001 | |
| 2016 | 6·69 (3·28–13·68) | .. | 2·80 (2·04–3·84) | .. | |
| Jan 1, 2017–March 31, 2018 | 21·19 (9·48–47·35) | .. | 7·44 (5·39–10·26) | .. | |
Ethnicity, sexual identity, education, employment, money status, and housing status are fixed variables; age, lifestyle characteristics, and HIV-risk behaviour are time-varying variables. Condomless sex is condomless anal sex. IRR=incidence rate ratio. OR=odds ratio. PrEP=pre-exposure prophylaxis. PEP=postexposure prophylaxis. STI=sexually transmitted infection.
Total observations are from 875 questionnaires; total observations used: for age, country of birth and ethnicity, sexual identity, university education, employment status, relationship status, money status, recent HIV test, condomless sex in the past 3 months, condomless sex with ≥2 partners in the past 3 months, group sex in the past 3 months, STI diagnosis, recreational drug use, PEP use, alcohol use, depression, anxiety symptoms, and calendar year were from 868 questionnaires done by 457 men; and for housing status were from 860 questionnaires done by 453 men.
Total observations are from 2080 questionnaires; total observations used: for age, university education, employment status, money status, relationship status, recent HIV test, condomless sex in the past 3 months, condomless sex with ≥2 partners in the past 3 months, group sex in the past 3 months, STI diagnosis, recreational drug use, PEP use, alcohol use, depression, and anxiety symptoms were from 2062 questionnaires done by 1153 men; for country of birth and ethnicity were from 2061 questionnaires from 1152 men; for sexual identity were from 2050 questionnaires done by 1143 men; for housing status were from 2050 questionnaires done by 1149 men; and for calendar year were from 2061 questionnaires done by 1153 men.
IRRs and ORs for age are unadjusted, age is included as a continuous variable when adjusting effects of other variables for age.
Other ethnicity includes Black, Asian, Mixed, and other ethnic groups.
ptrend=0·54.
ptrend=0·037.
Within the past 6 months.
Within the past 3 months.
To assess factors associated with reporting PrEP use in the previous year, we used data from 2080 questionnaires representing 1162 respondents (baseline and follow-up; table 2). The predictors for PrEP use in the previous year were similar to those associated with initiating PrEP. In particular, older age and later calendar year were strongly associated with increased use of PrEP, while unstable or other housing was associated with less use of PrEP than being a homeowner. We found some evidence of a trend between money status and reporting PrEP use (ptrend=0·037). Behavioural factors associated with reporting the use of PrEP were a recent HIV test, reporting condomless sex, condomless sex with two or more partners, group sex, non-injection chemsex-related drugs use, and PEP use. Country of birth and ethnicity, sexual identity, education, ongoing relationship, higher alcohol use, STI diagnosis, and symptoms of depression and anxiety were not associated with initiation of PrEP or use of PrEP (table 2).
In an additional analysis we looked at the association between health and behavioural factors and source of PrEP amongst those reporting use (190 questionnaires from 128 participants). We found that past 3-month STI diagnosis (unadjusted OR from GEE-logistic model 2·00, 95% CI 1·09–3·69; p=0·025), condomless sex (unadjusted OR 3·55, 95% CI 1·14–11·09; p=0·029), condomless sex with two or more partners (2·22, 1·01–4·85; p=0·045), group sex (2·32, 1·23–4·39; p=0·0090), use of non-injection chemsex-related drugs (3·69, 1·80–7·56; p<0·0001), and calendar year as a continuous variable (2·12, 1·43–3·15; p=0·028) were all associated with reported use of non-prescribed PrEP (data for other variables are not shown).
Discussion
To our knowledge, this Article is the first prospective study of PrEP use among MSM in England. In this study of MSM attending sexual health clinics in London and Brighton, UK, between 2013 and 2018, we found that use of PrEP increased substantially over the study period. The internet was the preferred source for obtaining PrEP, and online PrEP purchasing still continued even after the PrEP Impact trial started. Between January and March, 2018, about 48% of men who reported PrEP use obtained it from the internet, and paid for it using their own money. A substantial increase in PrEP use was also seen among men who self-reported engaging in condomless sex with two or more partners; in the period of January to March, 2018, the proportion was 78% compared with 0% in 2013.
The increased level of awareness, use, and rates of initiation of PrEP in this study coincided first with the PROUD study (Nov 29, 2012, to April 30, 2014),1 and then the initiation of the PrEP Impact implementation trial in England, and the availability of PrEP through NHS sexual health clinics in Scotland and Wales, and through a pilot in Northern Ireland. The PrEP Impact trial started recruitment in 2017 and the rate of PrEP initiation among the men in our study, who at least at baseline had attended these study sites, increased by more than twenty times in 2017–18 compared with before 2015. The high proportion of men accessing PrEP online despite the PrEP Impact trial opening for enrolment might have been because available places were rapidly filled and recruitment was closed temporarily.13 As a result, men in need of PrEP were being turned away and had no choice but to purchase it via the internet (Clarke A and Nwokolo N, unpublished). Substantial advocacy efforts from community-based organisations have also contributed to some men accessing PrEP online.
In our analysis, older age was independently associated with being more likely to initiate PrEP, with the rate of initiation among men aged 40 years and older being four times higher than among those younger than 25 years. This finding was similar to that in a cohort in Amsterdam in which the median age among men initiating PrEP was 40 years,14 and a cohort in Australia in which rates of PrEP initiation were highest among men aged 40 years and older.15 We also found that indicators of socioeconomic disadvantage (eg, not being employed, having unstable housing status, and having less or no money for basic needs), were associated with a reduced rate of initiating PrEP or being on PrEP. Previous research in the UK has shown that lower socioeconomic situation is associated with worse HIV treatment outcomes among individuals living with HIV.16 Efforts need to be made to ensure that socioeconomically disadvantaged individuals have equitable access to all effective HIV prevention strategies, including PrEP.
High-risk sexual behaviours such as condomless sex, condomless sex with two or more partners, group sex, and using non-injection chemsex-related drugs were also associated with PrEP use, indicating appropriate use of PrEP by these men. Similar to our findings, a recent national online prospective study in Australia reported that younger age, less use of illicit party or sex drugs, and lower engagement in HIV sexual risk behaviours such as group sex or any condomless sex, were independently associated with non-uptake of PrEP.15 The study also reported an increase in the uptake of PrEP from baseline (2014–15) to 24 months of follow-up.
Qualitative data from the PROUD study17 showed that MSM who were already having frequent condomless sex added PrEP as a prevention tool. MSM with a high risk of contracting HIV through condomless sex should be offered PrEP as a matter of urgency. In our study, more than 22% of respondents in 2018 were not using PrEP when having condomless sex with multiple partners and so were still at risk. These data would support the national roll-out of PrEP in England.
We did not find an association between STI diagnoses and taking PrEP, except among men who reported past 12-month non-prescribed PrEP use. A 2019 meta-analysis of 20 PrEP studies and trials among MSM found high incidences of STIs among MSM taking PrEP, ranging from 33·0 per 100 person-years to 99·8 per 100 person-years.18 However, whether PrEP use leads to increased rates of STIs remains unknown. The meta-analysis generated estimates of STI incidence among MSM who engaged in high-risk sexual behaviours, rather than comparing the rates among MSM taking PrEP versus not taking PrEP. The PROUD study found extremely high levels of STI diagnoses, but detected no difference in the occurrence of STIs between the immediate and deferred PrEP groups;1 while, the PrEPX study in Australia found the incidence of STIs increased during PrEP use, but that this finding was partly explained by increased testing frequency.19 Additionally, in the PrEPX study, half of the participants were not diagnosed with an STI during follow-up and STIs were highly concentrated among PrEP users with repeat STIs, and associated with number of partners and group sex. Regular STI testing should continue alongside PrEP use to ensure patients' good sexual health.
Although in our study we found no significant association between anxiety or depression and reporting recent PrEP use or PrEP, in a 2020 Australian study, PrEP use was independently associated with lower levels of HIV-related anxiety among PrEP-eligible men (MSM at high risk of HIV infection) than among PrEP ineligible men (MSM at low risk).20
Alongside the increase in PrEP use, we found a substantial decreasing trend in PEP use between 2013 and 2018, and that the use of PEP was a predictor of future PrEP initiation. This finding suggests that transition from PEP use to PrEP use occurred in these men. Guidelines recommend transitioning MSM who are at continuous risk of HIV from use of PEP towards use of PrEP.21 PrEP taken daily or on-demand before possible exposure is a highly effective strategy for reducing the risk of HIV acquisition among MSM who are at high and ongoing risk of infection.21 PEP, on the other hand, is a short-term treatment and is to be used in emergency circumstances after recent HIV exposure (within 72 h).22 Both PrEP and PEP should be a part of combination HIV prevention strategy.
Our study has some limitations. Men in this cohort were recruited from three sexual health clinics where the PROUD study was run and might have been better informed about PrEP than the general MSM population in England. Therefore, prevalence of PrEP and PEP use in this study might overestimate use in the MSM population nationwide. Men in this cohort were recruited from three sexual health clinics in urban areas in southeast England, and so the sample size was relatively small and these men might not be representative of the broader MSM population in England and the UK. Trends in use and predictors of PrEP initiation might also differ among MSM who are not engaged with sexual health clinics. Additionally, the sample comprised predominantly men who were highly educated, employed, in a stable economic situation, of white ethnicity, and with access to the internet (follow-up questionnaires were only available online, therefore to complete the questionnaires participants needed an internet connection), which might not allow generalisability to all MSM living in England. However, the Australian prospective cohort study that used a more diverse sample of MSM reached similar findings as were observed in our study.15 Further research is needed to investigate PrEP use among MSM who are more socioeconomically disadvantaged in England and the UK. Recall bias and social desirability bias might be evident in these self-reported data; however, the study collected sensitive and personal data through an online follow-up questionnaire, which might have reduced such bias.23 Finally, the online retention of participants who initially registered in the study was lower than we hoped; however, more than 60% of participants who completed at least one online questionnaire (n=622) were followed-up until the end of the study (n=400).24
In summary, this study provides important data for PrEP implementation in England. PrEP use has increased substantially over the past 5 years, with a high proportion of PrEP being obtained via the internet. Our data suggest that men engaging in sexual behaviour related to high HIV risk, who are older, and those of higher socioeconomic status are significantly more likely to use PrEP. A fully commissioned programme for PrEP in England has been agreed; however, implementation has been delayed (Rodger AJ, unpublished). Due to the COVID-19 pandemic, the programme might not be fully operational across England by the end of the PrEP Impact trial in October, 2020. To transition participants of the PrEP Impact trial onto the nationally commissioned programme, an interim supply of PrEP will be made available by the trial for participants with an ongoing need for PrEP and who attend services where the national programme has not yet commenced. The results of our study can inform the implementation of the national programme by highlighted patient groups who might be at increased risk of HIV infection but less likely to be aware of or using PrEP and who could benefit most from public health outreach and advice. Improving access to PrEP via routine commissioning by NHS England could increase PrEP use among all eligible MSM and reduce socioeconomic disparities, if it is accompanied by an understanding of these disparities and tailoring of public health message and services to address them.
Data sharing
Any personally identifiable data cannot be made publicly available to protect participants privacy. All other relevant data are available upon request to the corresponding author.
Acknowledgments
Acknowledgments
The AURAH2 study was funded by the NIHR under its Programme Grants for Applied Research Programme (RP-PG1212-20006). The AURAH2 Study Group thank the NIHR for their support through the Comprehensive Clinical Research Network. The AURAH2 study was also sponsored by the Joint Research Office at University College London (London, UK). NH received funding from the Indonesian Endowment Fund for Education (LPDP Indonesia Scholarship) during the conduct of this study. The views expressed in this Article are those of the authors and are not necessarily those of the NIHR, or the Department of Health and Social Care.
Contributors
AJR, ANP, FCL, JS, AS, NN, DA, RG, and AC conceived, designed, and managed the data collection in the AURAH2 study. NH, VC, JS, and ARM conducted data cleaning and variable derivation. SC contributed to the conception of the analysis, interpretation of data, and final approval of the manuscript. NH did all analyses and drafted the manuscript. All authors contributed to the conception of this analysis and participated in interpretation of data, revising, and final approval of the manuscript.
The AURAH2 Study Group
Alison J Rodger, Andrew N Phillips, Valentina Cambiano, Janey Sewell, Andrew Speakman, Nadia Hanum, Ada R Miltz, Richard Gilson, Nneka Nwokolo, Amanda Clarke, David Asboe, Simon Collins, Ana Milinkovic, Fabienne Styles, Rosanna Laverick, Marzena Orzol, Emmi Suonpera, Ali Ogilvy, Celia Richardson, Elaney Youssef, Sarah Kirk, Marion Campbell, Lisa Barbour, Fiona C Lampe.
Declaration of interests
AC reports personal fees and other from Gilead Sciences (conference and educational travel bursaries, and consultancy fees), personal fees from ViiV Healthcare (conference travel bursaries and consultancy fees) outside of the submitted work. FCL and RG report grants from National Institute for Health Research (NIHR) during the conduct of the study. All other authors declare no competing interests.
References
- 1.McCormack S, Dunn DT, Desai M. Pre-exposure prophylaxis to prevent the acquisition of HIV-1 infection (PROUD): effectiveness results from the pilot phase of a pragmatic open-label randomised trial. Lancet. 2016;387:53–60. doi: 10.1016/S0140-6736(15)00056-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Cambiano V, Miners A, Dunn D. Cost-effectiveness of pre-exposure prophylaxis for HIV prevention in men who have sex with men in the UK: a modelling study and health economic evaluation. Lancet Infect Dis. 2018;18:85–94. doi: 10.1016/S1473-3099(17)30540-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.O'Halloran C, Sun S, Nash S. Public Health England, December; London: 2019. HIV in the United Kingdom: towards zero HIV transmissions by 2030. 2019 report.https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/858559/HIV_in_the_UK_2019_towards_zero_HIV_transmissions_by_2030.pdf [Google Scholar]
- 4.Nwokolo N, Hill A, McOwan A, Pozniak A. Rapidly declining HIV infection in MSM in central London. Lancet HIV. 2017;4:e482–e483. doi: 10.1016/S2352-3018(17)30181-9. [DOI] [PubMed] [Google Scholar]
- 5.Scheer S, Hsu L, Schwarcz S. Trends in the San Francisco human immunodeficiency virus epidemic in the “getting to zero” era. Clin Infect Dis. 2018;66:1027–1034. doi: 10.1093/cid/cix940. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.New York City Department of Health and Mental Hygiene . HIV Epidemiology Program, November; Queens, NY: 2019. HIV surveillance annual report, 2018.https://www1.nyc.gov/assets/doh/downloads/pdf/dires/hiv-surveillance-annualreport-2018.pdf [Google Scholar]
- 7.Government of New South Wales; 2018. The NSW HIV Strategy 2016 – 2020. Quarter 4 & annual 2018: data report.https://www.health.nsw.gov.au/endinghiv/Publications/q4-2018-and-annual-hiv-data-report.pdf [Google Scholar]
- 8.Department of Health and Social Care . UK Government; London: March 15, 2020. HIV drug PrEP to be available across England.https://www.gov.uk/government/news/hiv-drug-prep-to-be-available-across-england [Google Scholar]
- 9.Sewell J, Speakman A, Phillips AN. Attitudes to and understanding of risk of acquisition of HIV over time: design and methods for an internet-based prospective cohort study among UK men who have sex with men (the AURAH2 study) JMIR Res Protoc. 2016;5:e128. doi: 10.2196/resprot.5582. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med. 2001;16:606–613. doi: 10.1046/j.1525-1497.2001.016009606.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Spitzer RL, Kroenke K, Williams JB, Löwe B. A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med. 2006;166:1092–1097. doi: 10.1001/archinte.166.10.1092. [DOI] [PubMed] [Google Scholar]
- 12.Babor TF, Higgins-Biddle J, Saunders JB, Monteiro MG. second edition. Department of Metal Health and Substance Dependence, World Health Organization; 2001. AUDIT: the Alcohol Use Disorders Identification Test: guidelines for use in primary care. [Google Scholar]
- 13.NHS England . NHS England; 2020. PrEP trial updates.https://www.england.nhs.uk/commissioning/spec-services/npc-crg/blood-and-infection-group-f/f03/prep-trial-updates/#march [Google Scholar]
- 14.Coyer L, van Bilsen W, Bil J. Pre-exposure prophylaxis among men who have sex with men in the Amsterdam Cohort Studies: use, eligibility, and intention to use. PLoS One. 2018;13 doi: 10.1371/journal.pone.0205663. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Hammoud MA, Vaccher S, Jin F. HIV pre-exposure prophylaxis (PrEP) uptake among gay and bisexual men in Australia and factors associated with the nonuse of PrEP among eligible men: results from a prospective cohort study. J Acquir Immune Defic Syndr. 2019;81:e73–e84. doi: 10.1097/QAI.0000000000002047. [DOI] [PubMed] [Google Scholar]
- 16.Burch LS, Smith CJ, Anderson J. Socioeconomic status and treatment outcomes for individuals with HIV on antiretroviral treatment in the UK: cross-sectional and longitudinal analyses. Lancet Public Health. 2016;1:e26–e36. doi: 10.1016/S2468-2667(16)30002-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Gafos M, Horne R, Nutland W. The context of sexual risk behaviour among men who have sex with men seeking PrEP, and the impact of PrEP on sexual behaviour. AIDS Behav. 2019;23:1708–1720. doi: 10.1007/s10461-018-2300-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Werner RN, Gaskins M, Nast A, Dressler C. Incidence of sexually transmitted infections in men who have sex with men and who are at substantial risk of HIV infection - a meta-analysis of data from trials and observational studies of HIV pre-exposure prophylaxis. PLoS One. 2018;13 doi: 10.1371/journal.pone.0208107. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Traeger MW, Cornelisse VJ, Asselin J. Association of HIV preexposure prophylaxis with incidence of sexually transmitted infections among individuals at high risk of HIV infection. JAMA. 2019;321:1380–1390. doi: 10.1001/jama.2019.2947. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Keen P, Hammoud MA, Bourne A. Use of HIV pre-exposure prophylaxis associated with lower HIV anxiety among gay and bisexual men in Australia who are at high risk of HIV infection: results from the Flux study. J Acquir Immune Defic Syndr. 2020;83:119–125. doi: 10.1097/QAI.0000000000002232. [DOI] [PubMed] [Google Scholar]
- 21.Brady M, Rodger A, Asboe D. BHIVA/BASHH guidelines on the use of HIV pre-exposure prophylaxis (PrEP) 2018. HIV Med. 2019;20(suppl 2):s2–s80. doi: 10.1111/hiv.12718. [DOI] [PubMed] [Google Scholar]
- 22.Cresswell F, Waters L, Briggs E. UK guideline for the use of HIV post-exposure prophylaxis following sexual exposure, 2015. Int J STD AIDS. 2016;27:713–738. doi: 10.1177/0956462416641813. [DOI] [PubMed] [Google Scholar]
- 23.DiClemente RJ, Swartzendruber AL, Brown JL. Improving the validity of self-reported sexual behavior: no easy answers. Sex Transm Dis. 2013;40:111–112. doi: 10.1097/OLQ.0b013e3182838474. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Sewell J, Cambiano V, Speakman A. Changes in chemsex and sexual behaviour over time, among a cohort of MSM in London and Brighton: findings from the AURAH2 study. Int J Drug Policy. 2019;68:54–61. doi: 10.1016/j.drugpo.2019.03.021. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
Any personally identifiable data cannot be made publicly available to protect participants privacy. All other relevant data are available upon request to the corresponding author.