Abstract
Foreign body (FB) aspiration is potentially life-threatening in children. A variety of sources and objects have been noted in aspiration events with possible complications ranging from mild to life-threatening. While rare, barium aspiration can cause severe complications, and removal is particularly challenging. Complications of retained barium include acute respiratory distress syndrome, pneumonitis, sepsis, even death. Regardless of the foreign body's identity, substance removal is critical in management. Resourcefulness of removal techniques and an interdisciplinary approach may allow for maximally effective management. We present a case of a pediatric barium aspiration from an unknown source and review evaluation and management strategies.
Keywords: Foreign body, Aspiration, Barium, Bronchoscopy, Microlaryngoscopy, Pneumonia
1. Introduction
Foreign body (FB) aspiration is a potentially life-threatening event in children with a peak incidence between 1 and 3 years old [[1], [2], [3], [4]]. In the pediatric population, the most commonly aspirated items include food items, hardware, and toys [4,5]. While the presentation of most aspirated FBs in children includes a history of an aspiration or possible aspiration event, some FB aspirations are unwitnessed. One study reported a witnessed choking episode in 75% of pediatric patients referred for bronchoscopy for suspected FB aspiration [6]. Regardless of the item aspirated, removal is key to treatment but can be very challenging. In this report, we describe the clinical presentation of aspirated barium from an unknown source. This case was uniquely challenging in its presentation. Our patient was outside of the age of peak incidence and did not have a witnessed episode concerning for aspiration. In part due to the delayed presentation and unknown characterization of the aspirated material, various techniques had to be devised by an interdisciplinary team, including the pediatric otolaryngology and pulmonary teams, to facilitate its removal over multiple operative trips and the child's recovery. This case was exempt from the Institutional Review Board review since this is a report of a single patient without any identifiable information.
2. Case presentation
An otherwise healthy 5-year-old male presented to the emergency department (ED) with 1 day of acute onset left-sided chest pain. He had initially presented to a local urgent care clinic, where a chest x-ray demonstrated a radiopaque lesion in the left lower lobe bronchus, concerning for an aspirated FB (Fig. 1 ). Therefore, he was referred to the pediatric ED, where the pediatric otolaryngology team was consulted. The child described the chest pain as intermittent, worse with inspiration, worse at night, and associated with a nonproductive cough. He also had a history of intermittent fever, clear rhinorrhea, and anorexia for the past 4 days. His neurologic status was completely normal. There was no history of a witnessed cough/choke episode, and the child and his family denied symptoms of noisy breathing, difficulty breathing, apnea, snoring, voice changes, or impaired swallow at any point. He had undergone dental work approximately 4 months prior, but parents denied any other procedural or surgical history. The only remarkable finding on examination in the ED was mildly diminished left lower lobe lung sounds. Given the concern for an airway FB, the patient was taken for emergent rigid laryngoscopy and bronchoscopy.
Fig. 1.
Chest x-ray images initially demonstrating radiopaque foreign body in left inferior lobar bronchus.
Intraoperative evaluation with a 4.0 rigid ventilating bronchoscope demonstrated a metallic-appearing FB in the left inferior lobar bronchus (Fig. 2 ) with surrounding granulation tissue and distal purulent drainage. The trachea, right mainstem bronchus, right upper takeoff, and left bronchus upper divisions were unremarkable. The FB was initially attempted to be extracted with optical forceps. Re-examination demonstrated significant granulation tissue at the site of the extracted FB, erosion of the left inferior lobar bronchial wall, and bloody purulent drainage distally. Small metallic flecks of the FB material were visualized along the tract but were unable to be extracted with instrumentation. An intraoperative chest x-ray was performed, which demonstrated significant residual FB. Given the findings, the pediatric pulmonology team was consulted intraoperatively. Flexible bronchoscopy with lavage was performed, and evidence of an abscess with purulent drainage was identified distal to the granulation tissue. Following this, the otolaryngology team performed repeat rigid bronchoscopy with further saline lavages and suctioning of small pieces of a foreign body as well as purulent material. The FB was found to be metallic, black, oxidized, carbonaceous, and particularly friable. No further foreign body amenable to extraction was visualized. Samples were sent for culture and Metals/Metalloids Acute Poisoning Panel analysis. The patient was administered a dose of intravenous piperacillin-tazobactam and dexamethasone intraoperatively and admitted for further management.
Fig. 2.
Metallic-appearing foreign body in left inferior lobar bronchus visualized on rigid bronchoscopy prior to manipulation or extraction.
Because of the metallic nature of the aspirated substance (Fig. 3 ), computed tomography (CT) of the chest was selected over magnetic resonance imaging (MRI) as the follow-up imaging of choice. Chest CT performed the day after initial removal demonstrated residual foreign body in the left lower lobe bronchus measuring 1.95 centimeters (cm) in the longest dimension and abscesses distal to the obstruction (Fig. 4 ). The largest discrete abscess cavity measured 1.8 cm × 1.1 cm. Repeat operative evaluation was performed the next day to extract further retained FB. As the material was known to be radiopaque and metallic, numerous methods were used to attempt extraction. Different sizes of Fogarty catheters were passed distal to the intraoperatively visualized foreign body pieces, inflated, and withdrawn with the balloon inflated. Endoscopic baskets were passed distal to the foreign body to attempt removal (Fig. 5 ). A range of endoscopic forceps for airway surgery were attempted to grasp the foreign body pieces for removal. A nasal bridle magnet was secured to optical forceps to attempt securing and removing the metallic foreign body pieces. Ultimately, the foreign body was extracted in pieces using optical peanut-grasping forceps with repeated irrigations over a series of twenty to thirty passes of the rigid endoscope due to the material's friability.
Fig. 3.
The metallic foreign body obtained from operative bronchoscopy responding to a magnet placed beside specimen cup.
Fig. 4.
Computer tomography (CT) chest imaging performed following initial operative procedure demonstrating residual foreign body, lung parenchyma damage, and post-obstructive abscess.
Fig. 5.
Residual carbonaceous metallic-appearing foreign body in left inferior lobar bronchus attempting to be extracted with use of endoscopic basket.
Then, the pediatric pulmonology team passed a flexible bronchoscope through the rigid bronchoscope and visualized some small residual foreign body debris not amenable to continued extraction attempts (Fig. 6, Fig. 7 ). A peripherally inserted central catheter (PICC) was also placed intraoperatively for anticipated prolonged intravenous antibiotic regimen.
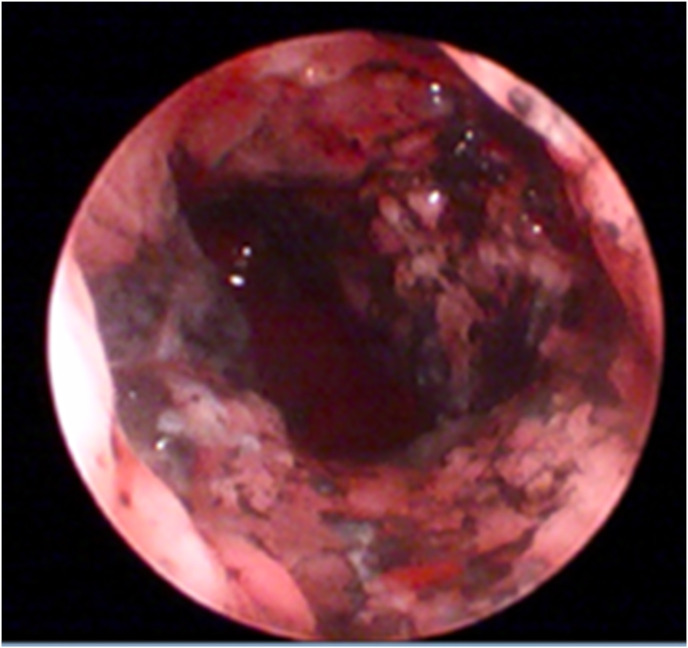
Fig. 6.
Residual carbonaceous metallic-appearing foreign body in the left inferior lobar bronchus visualized with flexible bronchoscopy following extraction and lavages.
Fig. 7.
Residual carbonaceous metallic-appearing foreign body in the left inferior lobar bronchus visualized with flexible bronchoscopy following extraction and lavages.
Following the procedure, the patient remained admitted for continuous positive airway pressure until tolerating room air, intravenous steroids, scheduled albuterol and chest physiotherapy, and piperacillin-tazobactam for broad spectrum coverage of the pneumonia. A follow-up chest CT was obtained three days later, which demonstrated near complete removal of the foreign body, improvement in the left lower lobe pulmonary abscess cavity and consolidation, and residual dilation of the left lower lobe segmental bronchus (Fig. 8 ). Culture from initial operative evaluation grew Haemophilus influenza. The pediatric infectious disease team was consulted for intravenous antibiotic selection and management, and the patient was discharged seven days after admission with a prolonged course of piperacillin-tazobactam through his PICC line and plans to follow-up as an outpatient with the pediatric infectious disease, pulmonary, and otolaryngology teams.
Fig. 8.
CT chest obtained three days after second operative event demonstrating near complete removal of the foreign body, abscess cavity and consolidation improvement, and residual dilation of the left lower lobe segmental bronchus.
During the coming weeks, the COVID-19 pandemic escalated, somewhat complicating follow-up. As such, the patient's planned follow-ups were performed via telemedicine as able. Six days prior to scheduled follow-up for potential PICC line removal, he presented to the ED for accidental dislodgement of the PICC line. Therefore, the line was removed, and he was instructed to complete two additional weeks of amoxicillin-clavulanic acid therapy. In the interim, the Associated Regional and University Pathologists, Inc. Metals/Metalloids Acute Poisoning Panel resulted, identifying the foreign body as being made of barium. Neither the patient nor his parents were able to identify a potential source of barium. Most recent follow-up occurred about 4 months after initial presentation. At that visit, the patient was doing very well without any respiratory symptoms. Repeat chest CT at that time did not show any residual foreign body or abscesses, but it did demonstrate some residual bronchiectasis. This raised concern that he may be at increased risk for developing bacterial pneumonia or bronchitis in the future. Therefore, it was recommended that the patient be evaluated in a prompt manner with a low threshold to start antibiotics if he developed fever or respiratory symptoms in the future. In addition, it was recommended that the patient be encouraged to be physically active to promote airway clearance with a plan to start regular airway clearance therapy, such as chest physiotherapy or high-frequency chest wall oscillation, if he developed pneumonia again.
3. Discussion
Foreign body aspiration is a potentially life-threatening occurrence. Children under the age of 3 years old comprise 80% of aspiration events [7]. We report a unique case of unwitnessed aspirated barium, unknown at time of attempted extractions, in an older child and describe its challenging, but successful, removal and treatment. To our knowledge, this is the first report of an unwitnessed barium FB aspiration. Our patient only had undergone a dental procedure prior to presentation, and dental instruments and implants are not reported to have barium content. Therefore, our patient's source and date of barium exposure remains unknown.
Barium is a highly toxic earth metal that occurs as a divalent cation associated with other elements in nature. Depending on which elements are associated, it has variable levels of water solubility [8]. Barium can be toxic in a state of higher water/acidic solubility, but it is benign when insoluble. Therefore, the highly insoluble barium sulfate is safely and widely used in medical imaging [[9], [10], [11], [12]].
Electronic database review of current literature resulted in few articles describing pediatric barium aspiration. Jackson et al. identified significant aspiration of liquid barium sulfate during a diagnostic barium esophagram with minor resultant clinical consequences, despite identifying a large tracheo-esophageal cleft [13]. The consequences of aspiration vary by patient age, comorbidities, concentration and volume aspirated, and if gastric contents were also aspirated [[14], [15], [16]]. Significant aspirations are often clinically symptomatic at the time of aspiration, unlike our patient, who did not demonstrate acute symptoms or signs of aspiration. Other case reports, mainly in adults, describe barium aspiration with clinically significant outcomes; however, it is difficult to differentiate the effect of aspirated barium from that of aspirated gastric content [17,18]. Once aspirated, barium particles are either removed via cough or mucociliary clearance, and remaining particles accumulate in the alveolar space [19]. Yan et al. describes large quantity barium sulfate aspiration leading to severe complications due to the compromise of the lungs’ endurance capacity. These complications can include dyspnea, hypoxemia, acute respiratory distress syndrome, respiratory failure, and even death with high quantities of barium aspiration. In addition, deposition of barium sulfate into the lungs can lead to structural complications, including bronchial granuloma, pneumonia, and pulmonary fibrosis [20]. Currently, there is no consensus in the literature on management of barium aspiration nor the long-term effects on the lungs. Certain occupations, such as mining, ceramics, and metalworking, are at highest risk for accidental barium ingestion. Other commercially available materials containing barium include shaving powder, fireworks, and rodenticide [[21], [22], [23], [24], [25], [26]]. This case demonstrates that aspirated solid barium has the potential to lead to bronchiectasis, even if it is successfully removed. Overall, barium exposure is rare outside of the medical setting.
Even in the setting of an unknown foreign body, various maneuvers can be utilized intraoperatively to extract the foreign body utilizing the available knowledge regarding its composition. Imaging demonstrated a radiopaque foreign body and initial intraoperative evaluation revealed it to be metallic in nature. Further investigation postoperatively also revealed the foreign body to have magnetic properties. Therefore, we attempted extraction with a magnet on return to the operating theater. We also utilized extraction methods from other specialties, including Urologic baskets and Fogarty embolectomy catheters. The extraction was further complicated by the friable nature of the foreign body, which prompted use of lavage as well. Resourcefulness and perseverance were important in extracting the unknown, friable substance. Also, even previously unreported materials, including earth metals like barium, should remain on the differential for foreign body material. Our multidisciplinary approach to this patient's treatment provided more methods for evaluation, extraction, and management of complications over a prolonged period. Our case required expertise from various disciplines for management of the foreign body itself, post-obstructive infection, lung parenchymal scarring, and respiratory compromise. While successful removal of a foreign body that has been present in the airway for an unknown period of time is critical for treatment, it is also important to consider initiating broad-spectrum antibiotics, consider repeating chest imaging after foreign body removal, and follow closely for possible sequelae, such as bronchiectasis.
4. Conclusion
We present the diagnostic approach and treatment of the rare occurrence involving a barium foreign body aspiration in a pediatric patient without preceding medical imaging, occupational exposure, or other known source. In this case, the high level of suspicion, the use of multiple removal techniques, and joint efforts of multiple specialties resulted in an overall good outcome for our patient. This case further demonstrates the importance of long-term follow-up of patients who have had a foreign body aspiration, even after successful removal.
Author disclosure statement
The authors have no conflicts of interest or funding sources associated with this research study. No competing financial interests exist.
Acknowledgements
Mark Sharafinski, University of Wisconsin-Madison Department of Radiology; Huifang Xu, University of Wisconsin-Madison Department of Geoscience.
References
- 1.Behrman R., Kliegman R., Jenson H. eighteenth ed. Elsevier Science; Philadelphia, Pa: 2007. Nelson Textbook of Pediatrics; pp. 1769–1770. [Google Scholar]
- 2.Dikensoy O., Usalan C., Filiz A. Foreign body aspiration: clinical utility of flexible bronchoscopy. Postgrad. Med. 2002;78:399–403. doi: 10.1136/pmj.78.921.399. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Karakoç F., Karadaǧ B., Akbenlioǧlu C. Foreign body aspiration: what is the outcome? Pediatr. Pulmonol. 2002;34:30–36. doi: 10.1002/ppul.10094. [DOI] [PubMed] [Google Scholar]
- 4.Schmidt H., Manegold B.C. Foreign body aspiration in children. Surg. Endosc. 2000;14:644–648. doi: 10.1007/s004640000142. [DOI] [PubMed] [Google Scholar]
- 5.Mu L., He P., Sun D. Inhalation of foreign bodies in Chinese children: a review of 400 cases. Laryngoscope. 1991;101:657–660. doi: 10.1288/00005537-199106000-00014. [DOI] [PubMed] [Google Scholar]
- 6.Cohen S., Avital A., Godfrey S., Gross M., Kerem E., Springer C. Suspected foreign body inhalation in children: what are the indications for bronchoscopy? J. Pediatr. 2009;155(2):276–280. doi: 10.1016/j.jpeds.2009.02.040. [DOI] [PubMed] [Google Scholar]
- 7.Chapin M.M., Rochette L.M., Annest J.L., Haileyesus T., Conner K.A., Smith G.A. Nonfatal choking on food among children 14 Years or younger in the United States, 2001–2009. Pediatrics. 2013;132(2):275–281. doi: 10.1542/peds.2013-0260. [DOI] [PubMed] [Google Scholar]
- 8.Oskarsson A. Barium. In: Nordberg G.F., Fowler B.A., Nordberg M., editors. Handbook on the Toxicology of Metals. fourth ed. Academic Press; London, UK: 2014. pp. 625–634. [Google Scholar]
- 9.Downs J.C. Suicidal ingestion of barium-sulfide-containing shaving powder. Am. J. Forensic Med. Pathol. 1995;16:56–61. doi: 10.1097/00000433-199503000-00013. [DOI] [PubMed] [Google Scholar]
- 10.Gould D.B., Sorrell M.R., Lupariello A.D. Barium sulfide poisoning. Some factors contributing to survival. Arch. Intern. Med. 1973;132:891–894. doi: 10.1001/archinte.132.6.891. [DOI] [PubMed] [Google Scholar]
- 11.Jacobs I.A., Taddeo J., Kelly K., Valenziano C. Poisoning as a result of barium styphnate explosion. Am. J. Ind. Med. 2002;41:285–288. doi: 10.1002/ajim.10056. 2002. [DOI] [PubMed] [Google Scholar]
- 12.Johnson C.H., VanTassell V.J. Acute barium poisoning with respiratory failure and rhabdomyolysis. Ann. Emerg. Med. 1991;20:1138–1142. doi: 10.1016/s0196-0644(05)81393-9. [DOI] [PubMed] [Google Scholar]
- 13.Jackson M., Kapur N., Goyal V., Choo K., Sarikwal A., Masters I.B., Isles A.F. Barium aspiration in an infant: a case report and review of management. Frontiers in Pediatrics. 2014;2(37):1–4. doi: 10.3389/fped.2014.00037. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Lopez-Castilla J., Cano M., Munoz M., Soult J.A., Andrés A., Montilla M. Massive bronchoalveolar aspiration of barium sulphate during a radiologic study of the upper digestive tract. Pediatr. Pulmonol. 1997;24(2):126–127. [PubMed] [Google Scholar]
- 15.Taman I., Kortsik C. Severe barium sulphate aspiration in the lung: clinical presentation, prognosis and therapy. Respiration. 1999;66:81–410. doi: 10.1159/000029344. 1159/000029344. [DOI] [PubMed] [Google Scholar]
- 16.Whiting J. Aspiration of barium. N. Engl. J. Med. 2003;348(25):2582–2583. doi: 10.1056/NEJM200306193482522. [DOI] [PubMed] [Google Scholar]
- 17.Fruchter O., Dragu R. A deadly examination. N. Engl. J. Med. 2003;348(11):1016. doi: 10.1056/NEJMicm020803. [DOI] [PubMed] [Google Scholar]
- 18.Gray C., Sivaloganathan S., Simpkins K. Aspiration of high-density barium contrast medium causing acute pulmonary inflammation – report of two fatal cases in elderly women with disordered swallowing. Clin. Radiol. 1989;40(4):3970400. doi: 10.1016/s0009-9260(89)80135-7. [DOI] [PubMed] [Google Scholar]
- 19.Roggli V., Shelburne J. Mineral pneumoconiosis. In: Dahl D.H., Hammar S.P., editors. Pulmonary Pathology. second ed. Springer-Verlag; New York: 1998. pp. 589–618. [Google Scholar]
- 20.Yan G.W., Deng J.F., Bhetuwal A. A case report and literature review of barium sulphate aspiration during upper gastrointestinal examination. Medicine (Baltim.) 2017;96(47) doi: 10.1097/MD.0000000000008821. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Schorn T.F., Olbricht C., Schüler A. Barium carbonate intoxication. Intensive Care Med. 1991;17:60–62. doi: 10.1007/BF01708412. [DOI] [PubMed] [Google Scholar]
- 22.Lewi Z., Warsaw D.M., Bar-Khayim Y. Food-poisoning from barium carbonate. Lancet. 1964;284:342–343. doi: 10.1016/s0140-6736(64)90281-8. [DOI] [PubMed] [Google Scholar]
- 23.Shankle R., Keane J.R. Acute paralysis from inhaled barium carbonate. Arch. Neurol. 1988;45:579–580. doi: 10.1001/archneur.1988.00520290119024. [DOI] [PubMed] [Google Scholar]
- 24.Thomas M., Bowie D., Walker R. Acute barium intoxication following ingestion of ceramic glaze. Postgrad. Med. 1998;74:545–546. doi: 10.1136/pgmj.74.875.545. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Silva R.F., Santi L.Q., Santos A.A. Barium toxicity after exposure to contaminated contrast solution–Goias State, Brazil, 2003. MMWR Morb. Mortal. Wkly. Rep. 2003;52:1047–1048. [PubMed] [Google Scholar]
- 26.Deepthiraju B., Varma P.R.K. Barium toxicity: a rare presentation of fire-works ingestion. Indian Pediatr. 2012;49:762. doi: 10.1007/s13312-012-0144-z. [DOI] [PubMed] [Google Scholar]