Abstract
Gastric bezoars are foreign bodies that occur when certain drugs or foods aggregate in the stomach. They cannot be digested and most are unable to pass through the pylorus. Here, we describe a giant hard gastric bezoar that was removed by using combined dual knife–electric snare treatment. This strategy has rarely been reported and can eliminate the need for surgery. The patient exhibited a giant hard gastric bezoar and reported a habit of eating persimmons. A giant persimmon bezoar was treated using a combined dual knife–electric snare approach, without any complications. Follow-up endoscopy revealed that the bezoar had been successfully removed. This report also provides a summary of the diagnostic and therapeutic courses of gastric bezoars.
Keywords: dual knife, electric snare, gastroscopy, giant gastric bezoar, case report, diospyros, digestive system, endoscopy
Introduction
Bezoars are foreign bodies formed by aggregates of matter that cannot be digested; although they can exist in any part of the digestive tract, most occur in the stomach.1 Gastric bezoars formed after consumption of persimmons are the most common bezoar type in China.2 Persimmon bezoars have hard surfaces and can be diagnosed through abdominal ultrasonography, computed tomography, and upper endoscopy. Currently, treatments for gastric bezoars include endoscopy, medications, and surgical procedures.3,4 Small bezoars can freely pass through the gastrointestinal tract. Medical treatments include inhibition of gastric acid secretion or neutralization of secreted acids; these approaches are effective for the treatment of recent, small, or soft gastric bezoars, whereas they are often ineffective for old, large, or hard bezoars. In contrast, surgical intervention is the optimal treatment method for giant hard gastric bezoars with bleeding ulcers; this approach is characterized by considerable trauma, slow postoperative recovery, and risks of complications (e.g., intestinal adhesion).3,4 Endoscopic treatments include the use of alligator forceps, lithotripters, needle cutters, snares, and holmium:yttrium aluminum garnet (YAG) laser lithotripsy.5,6 Notably, holmium:YAG laser lithotripsy treatment was reported to provide a promising outcome for a patient with a giant gastric bezoar.6 Endoscopic lithotripsy is a potential treatment for gastric bezoars; this approach is characterized by minor trauma, more rapid recovery, fewer complications, and low cost. Here, we describe a patient with a giant hard gastric bezoar that was successfully removed by combined dual knife–electric snare treatment, without any complications.
Case presentation
A 57-year-old woman presented to our department with the complaint of epigastric pain that had been present for 1 month. The patient reported a long-term habit of eating persimmons. Her physical and systemic examination findings were unremarkable; no abnormal physical findings or laboratory data were observed. Gastroscopy revealed a giant hard bezoar in the stomach cavity, with an approximate size of 6.0 × 8.0 cm (Figure 1a). On the second day after admission, an Olympus 260 gastroscope with a transparent cap was inserted into the stomach cavity with the patient under intravenous anesthesia (GIFH260; Olympus, Tokyo, Japan). Food residue was removed from the stomach. Then, a dual knife (MK-T-2-195, Nanjing Minimally Invasive Gold Knife; Nanjing Minimally Invasive Medical Technology Co., Ltd., Nanjing, China) with peak power 100 W was used to create two grooves in the surface of gastric bezoar along its longitudinal axis (Figure 1b). The gastric bezoar was then rotated 90° and two grooves were created along its horizontal axis using the dual knife (Figure 1c). Next, the gastric bezoar was fixed along the longitudinal grooves with an Olympus electric snare (SD-230U-20; Olympus Corporation, Tokyo, Japan) and lifted upwards. The electric snare was confirmed to not contact the stomach mucosa. The gastric bezoar was fragmented along its longitudinal axis by using the electric snare at power setting 40 to 50 W. The electric snare was then used to grasp the gastric bezoar along the transverse grooves and fragment it with power setting 40 to 50 W. This process yielded fragments of approximately 4.0 × 5.0 cm. The grooves of larger diameter gastric bezoar fragments were excavated with the dual knife and further fragmented using the electric snare (Figure 1d). Finally, the small fragments were removed from the stomach with Dormia basket (FG-24SX-1; Olympus Corporation) (Figure 1e). Some fragments were able to spontaneously pass through the pylorus. Subsequently, the patient experienced relief of epigastric pain and did not exhibit complications (e.g., bleeding, perforation, or throat lesions). One week later, endoscopic examination revealed multiple gastric ulcers, but showed no remaining bezoar fragments (Figure 1f). The detailed process of giant gastric bezoar removal using combined dual knife–electric snare treatment is shown in Figure 2. The patient’s information was deidentified to preserve their privacy; thus, informed consent was not required for publication of this report.
Figure 1.
Clinical findings and surgical procedure in a patient with a giant gastric bezoar. (a) Gastroscopy revealed a giant hard bezoar in the stomach cavity. (b) Two grooves were created along the longitudinal axis on the bezoar surface using a dual knife. (c) Two grooves were created along the horizontal axis on the bezoar surface using a dual knife. (d) Giant gastric bezoar was fragmented by an electric snare. (e) Giant gastric bezoar fragments were removed from the stomach using a Dormia basket. (f) No bezoar fragments remained in the stomach.
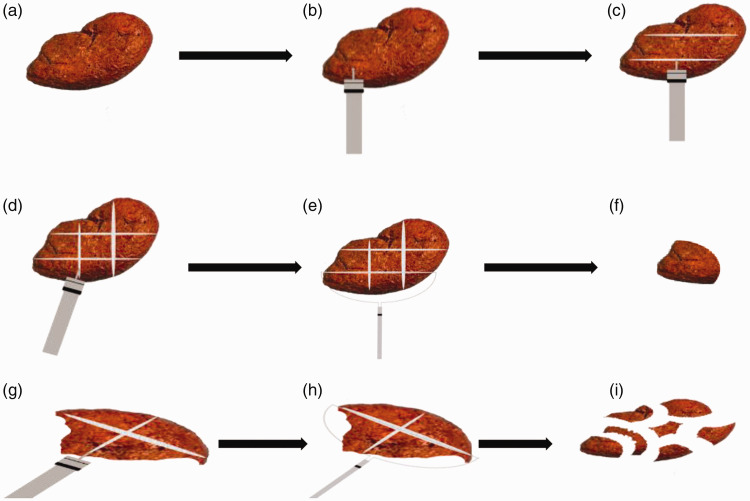
Figure 2.
Schematic of giant gastric bezoar removal using combined dual knife–electric snare treatment. (a) Giant bezoar present in the stomach. (b) Giant gastric bezoar cut by a dual knife. (c) Two grooves created along the longitudinal axis on the bezoar surface using a dual knife. (d) Two grooves created along the horizontal axis on the bezoar surface using a dual knife. (e) Giant gastric bezoar fragmented by an electric snare. (f) Giant gastric bezoar fragments. (g–i) Grooves of gastric bezoar fragments excavated using a dual knife and removed using a Dormia basket.
Discussion
In recent decades, the incidence of gastric bezoars has gradually increased.4,7 Factors that contribute to gastric bezoar formation are complex and differ according to location; notably, changes in diet have greatly increased their incidence. Gastric bezoars occur when foods aggregate in the stomach, forming a coagulum or lump that cannot be digested.4,7 Common clinical manifestations in patients with gastric bezoars include nausea, vomiting, epigastric pain, dyspepsia, and weight loss; common complications include bleeding ulcers, obstruction, and perforation.8,9 Classifications of bezoars according to their compositions include diospyrobezoars, trichobezoars, lactobezoars, and pharmacobezoars; notably, the components of gastric bezoars are similar to the components of gallstones.10 Diospyrobezoars are composed of indigestible fruit or vegetable content, such as persimmons, orange piths, eggplants, grapefruits, and mangos. Gastric bezoar hardness is related to its composition.7 Because Chinese individuals have a habit of eating persimmons, bezoars containing persimmons (especially giant bezoars) are common in China; persimmon bezoars exhibit hard surfaces and cannot readily pass through the gastrointestinal tract. Gastric giant bezoars are defined as those with diameter >4 cm. Current clinical management approaches for gastric bezoars include medication, surgery, and endoscopy.3,4,11 For giant gastric bezoars, medication is the simplest therapy. The treatments used in western medicine mainly consist of inhibiting gastric acid secretion or neutralizing secreted acids, but they are often ineffective for old, massive, or hard bezoars. In recent years, traditional Chinese medicine has developed some new approaches for treatment of gastric bezoars.3,4,11 These treatments are inexpensive and effective for neutralization of gastric acids, dissolution of bezoars, promotion of gastrointestinal emptying, and protection of mucosal function. Furthermore, they are noninvasive. Surgical treatment is another important treatment option for giant gastric bezoars; as noted in the Introduction, this approach is characterized by considerable trauma and slow postoperative recovery.6,12 Specialized lithotripters and miniature explosive lithotripsy require expensive equipment, which increases the financial burden for patients. Some studies have shown that holmium:YAG laser lithotripsy is effective for treatment of giant bezoars; the optical fiber diameter, energy, frequency, power, and other parameters of the laser are important considerations for the safety and outcome of the procedure.6,12
To the best of our knowledge, this is the first complete and detailed report regarding the removal of a giant gastric bezoar from the stomach by using combined dual knife–electric snare treatment. Here, we used a dual knife to create grooves on the surface of the hard gastric bezoar; we then firmly fixed the electric snare to the surface of the bezoar, which facilitated fragmentation of the bezoar by the electric snare. After repeated electric fragmentation steps, the gastric bezoar was removed through the esophagus. The Nanjing Minimally Invasive Gold Knife was used in this surgical procedure; this equipment is inexpensive and can greatly reduce the financial burden for patients. Moreover, this knife has a cutter wire length of 15 mm; the cutter head is small and round, such that it exhibits considerable resistance during cutting, as well as high cutting efficiency and easy directional control. We successfully removed the giant hard gastric bezoar from our patient by using combined dual knife–electric snare treatment. We encountered no adverse events and our patient demonstrated rapid recovery; follow-up endoscopy revealed the absence of bezoar fragments. Thus, this therapy is effective, safe, inexpensive, and widely applicable.
Based on our clinical experience, we make the following recommendations: (1) Grooves should be created along the longitudinal and transverse axes of the gastric bezoar; to facilitate fragmentation of a gastric bezoar into smaller pieces, the peak power of the dual knife should be set at 100 W. (2) The bezoar should be prepared with a dual knife; for ease of fragmentation, the groove should penetrate the surface of the bezoar as much as possible. (3) To avoid gastric mucosal injury, the bezoar should be lifted and the electric snare wire should not touch the stomach mucosa. (4) An electric snare with power 40 to 50 W is ideal for fragmentation of the hard surface of the gastric bezoar; an ordinary mechanical snare is often ineffective. (5) The electric snare may be damaged due to high temperatures when the operative time exceeds 30 minutes; thus, we recommend that experienced doctors perform the procedure. (6) To avoid damage to the esophagus, the gastric bezoar should be fragmented into pieces with maximum diameter less than 2 cm.
In conclusion, our findings in this case highlight the safety and effectiveness of combined dual knife–electric snare treatment for removal of a giant gastric bezoar, which involves minimal pain, lower risk, and reduced financial burden.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
ORCID iD
Fang Cheng https://orcid.org/0000-0003-2121-2013
References
- 1.Iwamuro M, Okada H, Matsueda K, et al. Review of the diagnosis and management of gastrointestinal bezoars. World J Gastrointest Endosc 2015; 7: 336–345. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Gao F, Gao R, Hao JY, Jia JD. Gastric bezoar: a case of a patient treated with traditional Chinese medicine. J Altern Complement Med 2012; 18(1): 93–95. doi;10.1089/acm.2010.0794 [DOI] [PubMed] [Google Scholar]
- 3.Jin S, Xu Y. Progress in diagnosis and treatment of gastrolithiasis and type. Chin J Clin 2012; 6: 153–155. [Google Scholar]
- 4.Dai Q, Jiang F. A huge gastric bezoar treated by traditional Chinese medicine purgative: a case report. Medicine (Baltimore) 2018; 97: e13712. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Ugenti I, Travaglio E, Lagouvardou E, et al. Successful endoscopic treatment of gastric phytobezoar: a case report. Int J Surg Case Rep 2017; 37: 45–47. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Grande G, Manno M, Zulli C, et al. An alternative endoscopic treatment for massive gastric bezoars: Ho:YAG laser fragmentation. Endoscopy 2016; 48: E217. [DOI] [PubMed] [Google Scholar]
- 7.Khan S, Jiang K, Zhu LP, et al. Upper gastrointestinal manifestation of bezoars and the etiological factors: a literature review. Gastroenterol Res Pract 2019; 2019: 5698532. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Khan S, Khan IA, Ullah K, et al. Etiological aspects of intragastric bezoars and its associations to the gastric function implications: a case report and a literature review. Medicine (Baltimore) 2018; 97: e11320. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Parakh JS, McAvoy A, Corless DJ. Rapunzel syndrome resulting in gastric perforation. Ann R Coll Surg Engl 2016; 98: e6–e7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Iwamuro M, Urata H, Hirata S, et al. A bezoar composed of bilirubin calcium, calcium carbonate, and fatty acid calcium. Case Rep Gastrointest Med 2019; 23: 5742672. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Qin X, Chen J, Liang M, et al. Overview of TCM treatment of gastric bezoars. Asia-Pac Trad Med 2017; 13: 61–64. [Google Scholar]
- 12.Kronenberg P, Traxer O. Update on lasers in urology 2014: current assessment on holmium:yttrium-aluminum-garnet (Ho:YAG) laser lithotripter settings and laser fibers. World J Urol 2015; 33: 463–469. [DOI] [PubMed] [Google Scholar]