Abstract
Background
The COVID-19 pandemic impacts the whole world. So far, nothing is known about the course of psychological disturbances, such as fear, anxiety, and sleep disturbances of this pandemic over time in Europe.
Methods
Aim of this web-based survey was to assess the mental health burden of the German public over a period of 50 days after the COVID-19 outbreak. 16,245 individuals responded regarding sleep disturbances, COVID-19-fear, and generalized anxiety disorder (GAD-7). Data were put in relation to infection rates, number of deaths and the German stock index.
Results
The specific fear increased rapidly in concordance with infection numbers. However, no relation to the number of deaths was found, COVID-19-fear developed reversed to the stock index. Initially, 13.5% of the respondents reported a reduced sleep quality, and 7.2% a moderate generalized anxiety; proceeding simultaneously with high peaks. Finally, more than twice as many respondents showed psychological burdens.
Conclusion
The COVID-19-fear decreased within six weeks to the level before the shutdown, indicating a habituation to the threatening situation. However, generalized anxiety remained elevated over time. Sleep disturbances, generalized anxiety as well as economical stock alterations develop in advance to infectiological trends which demands consequent and comprehensible information policies.
Keywords: Sleep disturbances, Fear, Generalized anxiety, COVID-19 virus, SARS-CoV-2, Stock index
Graphical abstract
Highlights
-
•
Highly topical issue of mental health aspects of COVID-19 pandemic.
-
•
During pandemic, sleep disturbances are related to generalized anxiety (GAD).
-
•
High peaks of GAD and sleep disturbances when political landmarks occur.
-
•
COVID-19-fear is inversely related to German stock index DAX in time curse.
-
•
Sleep complaints are not associated with reported new COVID-19 cases or deaths.
1. Introduction
Since the outbreak of the COVID-19 pandemic (SARS-CoV-2 virus) in China, a large number of political initiatives have been internationally taken to bring the pandemic under control [1]. On April 30th, 2020, a total of 162,123 COVID-19 cases in Germany have been confirmed, and 6518 German have died from the disease [2]. The population was confronted abruptly and unpredictably with new restrictions or regulations to everyday life on a daily basis. These rapid changes in the current situation created fear [3]. This showed impact on the stock market. While sleep is assumed to be involved in the pathological process of COVID-19 [4], studies on the psychological effects of other viral diseases and pandemics [[5], [6], [7]], and of COVID-19 in China [8], showed increased anxiety, depression and sleep disturbances. These can be only partly transferred to the current situation in Europe. The political effects of the COVID-19 pandemic are unprecedented, as are the psychological effects. The influence of the restrictions on fear for the first few days during COVID-19 has already been pointed out by Teufel et al. (2020): People were profoundly disconceted by the outbreak, and this might even reach a critical threshold in the early phase [9]. Establishing infrastructure for people suffering from withdrawal and psychological disconcertion is crucial [10]. In the absence of references or precedents, it is important to examine the psychological impact - inter alia of policy, infection rates and the number of deaths, as well as the economic impact in the course of such a scenario.
Therefore, in this study, the mental health burden of the German public was assessed and linked with infectiological and economical data.
2. Method
The online-survey period covers different levels of governmental restrictions and loosening of public life in Germany: From the early beginning on March 10th 2020, – before, and during the shutdown, to the successive withdrawal of restrictions. Over the course of 50 days, up until April 30th, 2020, we collected data from 16,245 individuals assessing COVID-19-related fear, generalized anxiety disorder, and sleep quality, in a cross-sectional online survey via online channels (e.g. online newspapers), social media, and print media. Participation was anonymous, in accordance with the Declaration of Helsinki.
2.1. Assessment instruments
Self-reported generalized anxiety was assessed by use of Generalized-Anxiety-Disorder-7 (GAD-7) with seven items on a four-point Likert-scale (“not at all” to “nearly every day”) [11]. Sleep quality was assessed by the respective item of the Patient-Health-Questionnaire-9 (PHQ-9) [12], on a four-point Likert-scale (0 = “never” to 3 = “nearly every day”), reporting the frequency of both insomnia and hypersomnia [13]. A mean sum score of ≥3 correspond to severe sleep disturbances. COVID-19-fear was assessed using the item (“I worry about Covid-19”) on a seven-point Likert-scale (“I do not agree at all” to “I totally agree”).
Infectiological data (number of cases and deaths) was obtained from the German government's central scientific institution in the field of biomedicine Robert-Koch-Institute (RKI) [14]. Additionally, the daily German stock index (DAX) was imported from the “Deutsche Börse” [15]. Approximation curves for the variables of psychological burdens were laid over the exact data curves.
2.2. Time course of political events
In Germany, the government announced the closure of educational institutions on Friday, March 13th, 2020. This was the first measure to slow down the spread of the virus. It affected a large part of the population. The following day, politicians called for solidarity and compliance with medical recommendations. Subsequently, on March 22nd, the government announced a contact ban, which largely banned gatherings of more than two people in public places. It was announced at the end of March that the restrictions would be retained. Over the Easter holidays a significant decrease in new infections was observed. On April 20th, an easing of measures in the retail sector was announced. It was once again possible to buy goods beyond the basic supply in smaller shops. On April 27th wearing a facemask became mandatory in public places and in contact with other people in supermarkets for instance.
3. Results
The survey sample size (N = 16,245) varied over the 50 days between 45 (day 41) and 2225 (day 3). Demographics are shown in Table 1 .
Table 1.
Demographics.
| N | Percent (%) | |
|---|---|---|
| Gender | 16,245 | |
| Female | 11,500 | 70.8 |
| Male | 4695 | 28.9 |
| Other | 50 | 0.3 |
| Age Category (years) | 15,359a | |
| <18 | 384 | 2.5 |
| 18-24 | 2091 | 13.6 |
| 25-34 | 3734 | 24.3 |
| 35-44 | 3423 | 22.3 |
| 45-54 | 2833 | 18.5 |
| 55-64 | 2123 | 13.8 |
| 65-74 | 652 | 4.3 |
| 75-84 | 109 | 0.7 |
| >85 | 10 | 0.1 |
| Education | 16,245 | |
| university degree | 6756 | 41.6 |
| high school diploma | 5271 | 32.4 |
| secondary school degree (“Realschule”) | 3010 | 18.5 |
| secondary school degree (“Hauptschule”) | 728 | 4.5 |
| no secondary school degree | 130 | 0.8 |
| other form of education | 350 | 2.2 |
| Size of district | 16,245 | |
| large city (>100,000) | 9281 | 55.2 |
| medium-sized city (20,000–100,000) | 3882 | 22.9 |
| small town (5000–20,000) | 1923 | 11.1 |
| rural district (<5000) | 1897 | 10.8 |
Technical difficulties, not missing values (n = 886).
3.1. COVID-19-fear
The COVID-19-fear increases during the first three weeks of measurement and reaches a climax around March 22nd, when a contact prohibition was announced. Following this, anxiety declines. Approximately from April 20th, 2020, the COVID-19-fear is at its initial level - at the point when the restrictions were also released from the political side.
3.2. Generalized anxiety and sleep disturbance
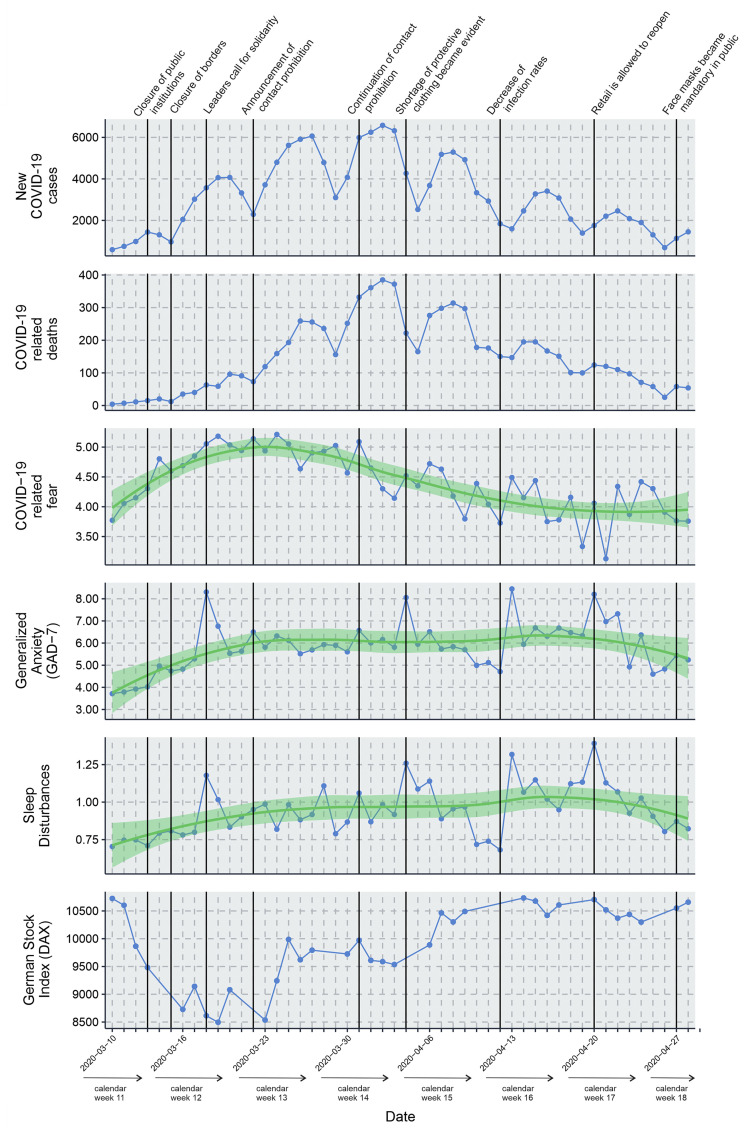
At the beginning of the survey (March 10th) 7.2% of the respondents reached the cut-off for a moderate generalized anxiety (cut-off ≥ 10), measured using the GAD-7. Almost 13.5% of the participants reported severe reduced sleep quality [12,13]. The two curves of generalized anxiety and sleep (see Fig. 1 , panel d and e) proceed simultaneously, and show peaks at nearly the same time points. High peaks appear on March 18th before leaders’ calls for solidarity (37% over cut-off of GAD-7, 33.5% of sleep disturbances), and April 4th associated with evident lack of protective clothing in hospitals and community (40.7% over cut-off of GAD-7, 33.5% of sleep disturbances), and April 20th 2020, associated with successive withdrawal of restrictions (32% over cut-off of GAD-7, 30.1% of sleep disturbances). A minimum appears around April 13th 2020, when media reported a decline in new COVID-19 infections. At the end of the survey period, 22.1% of the respondents reached the cut-off for moderate generalized anxiety; 26.3% for severe sleep disturbances.
Fig. 1.
Time course of psychological burden, the rates of infection and deaths, and the daily DAX during the spread of COVID-19 from March 10th to April 24th 2020. From top down: Severe course and death from COVID-19, self-reported levels (means) of COVID-19-related fear, generalized anxiety, and sleep difficulties (sleep item of PHQ-9), and the DAX daily performance index. Overall, 16,245 (range 45 to 2225 daily) respondents participated. Vertical lines indicate dates of significant political landmarks in Germany: Closure of public institutions (The government announced the closure of educational institutions on Friday, March 13th, 2020), Closure of borders (The government announced the closure of borders to other states.), Leaders call for solidarity (German Chancellor Angela Merkel, appealed for solidarity and compliance with medical recommendations by a long awaited public speech.), Announcement of contact prohibition (The government announced a contact ban, which largely banned gatherings of more than two people in public places, and e.g. shops with the exception of the food trade, restaurants, and cinemas were closed.), Continuation of contact prohibition, Shortage of protective clothing became evident (by media reports), Decrease of infection rates (reported by the Robert-Koch-Institute), Retail is allowed to reopen (It was once again possible to buy goods beyond the basic supply in smaller shops.), Face masks became mandatory in public (in public places and in contact with other people in supermarkets for instance). Green lines show approximated curves.
3.3. Trends in comparison to infection and death rates, and economic index
The climax of infection cases was reached on April 4th, 2020 (Nnew cases = 6559) [14]. The death rate shows a slight delay of about two weeks to the illness rate. In comparison to the curves of the reported rates of new cases and deaths, the climax of COVID-19-fear appears about ten days earlier. COVID-19-fear shows a rapid increase before infection and death rates rise, and then an equally rapid decline to the baseline level. The approximated curve can be interpreted as an inverse of the German stock market index. This falls synchronously with the rise of the Covid-19-fear and then rises as rapid as the COVID-19-fear. Generalized anxiety and sleep disturbances increase slightly. They do not reach the baseline level after the period of 50 days.
4. Discussion
To date, this is the first study to access detailed information of the course of psychological burdens in Germany over a time before the COVID-19-related shutdown to the first relaxation of restrictions. This report shows trends of COVID-19-fear, anxiety and sleep disturbances from the beginning during these phases of government-imposed measures. In addition, psychological burdens were linked to infectiological trends and economical indices.
A rapidly increasing COVID-19-fear and decreasing stock market in comparison with a more sedate reaction of generalized fear and sleep disturbances show few connections to real new cases and death rates. No correlations can be drawn out of these findings. Since the COVID-19-fear increased rapidly and then levelled off despite reports of further cases and deaths, it may be comparable to a more functional fear of an unknown enemy which needs to first be assessed. Its association with the trend of the DAX could be illustrated. It is noteworthy, that a bidirectional effect can be imagined: As a rising fear influences the buying behaviour on the market or that a suffering stock market even adds to the COVID-19-fear in the population. The fear and the stock market recover and return to the initial level. Even before the infectiological changes, COVID-19-fear seems to increase preliminarily. This can be interpreted in the sense of a warning function and may be used for behavioural preparation - in the sense of adherence preparation. Following this alert action, the affect habituates. The behavioural preparation seems to be complete.
Meanwhile, generalized anxiety and sleep disturbances in general seem to decrease only slightly. This represents the distinct psychological burden on the population in this pandemic situation. However, characteristics of this situation are the high peaks in these variables, which in the chronological overview can be interpreted as a reaction to media reports. The current data show much higher percentages in the population exposed to COVID-19 compared to the normative population [11]. At peak stages, this is up to 8 times higher. The media coverage indicates as having an immense influence on the mental health. This is an important fact, which was previously revealed [9], but is now being confirmed for various aspects, such as the implementation and relief of constraints. A sufficient level of information is therefore mandatory. Apart from this, individuals with high levels of burden should have access to interventions [4,[16], [17], [18]].
The current study has some limitations, e.g., the varying sample size over time curse due to the study design. Furthermore, information on burden was given by self-report and cannot be compared with information on mental state or potential mental disorders. However, this study shows a highly topical issue to address neglected aspects of mental health in the COVID-19 pandemic.
The accompanying psychological burdens - especially high peaks of anxiety and sleep disturbances - of today's world should be considered in political reporting and also in possible psychological and psychosocial interventions.
Credit authorship contribution statement
Madeleine Hetkamp; Adam Schweda: Conceptualization, evaluation of the study. Madeleine Hetkamp: Prepared the manuscript. Adam Schweda: Visualized the data. Alexander Bäuerle; Benjamin Weismüller; Hannah Kohler; Venja Musche; Nora Dörrie; Christoph Schöbel: Supported in the preparation of the manuscript, reviewing and editing. Martin Teufel; Eva-Maria Skoda: Supervised the conceptualization, collection and evaluation of the study.
Funding
This study was supported by the Essen University Medicine Foundation. The funder had no role in the design and conduct of the study; management, collection, analysis and interpretation of the data; preparation, review or approval of the manuscript; and decision to submit the manuscript for publication.
Footnotes
We have no competing interests.
The ICMJE Uniform Disclosure Form for Potential Conflicts of Interest associated with this article can be viewed by clicking on the following link: https://doi.org/10.1016/j.sleep.2020.08.033.
Conflict of interest
The following is the supplementary data related to this article:
Multimedia component 1
References
- 1.Fisher D., Wilder-Smith A. The global community needs to swiftly ramp up the response to contain COVID-19. Lancet. 2020;395:1109–1110. doi: 10.1016/S0140-6736(20)30679-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Tägliche Fallzahl des Coronavirus in Deutschland 2020 Statista. 2020. https://de.statista.com/statistik/daten/studie/1100739/umfrage/entwicklung-der-taeglichen-fallzahl-des-coronavirus-in-deutschland/ [Google Scholar]
- 3.Asmundson G.J.G., Taylor S. Coronaphobia: fear and the 2019-nCoV outbreak. J Anxiety Disord. 2020;70:102196. doi: 10.1016/j.janxdis.2020.102196. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Chen Y., Zhao A., Xia Y. In the big picture of COVID-19 pandemic: what can sleep do. Sleep Med. 2020;72:109–110. doi: 10.1016/j.sleep.2020.06.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Lee A.M., Wong J.G., McAlonan G.M. Stress and psychological distress among SARS survivors 1 Year after the outbreak. Can J Psychiatr. 2016;52:233–240. doi: 10.1177/070674370705200405. [DOI] [PubMed] [Google Scholar]
- 6.McAlonan G.M., Lee A.M., Cheung V. Immediate and sustained psychological impact of an emerging infectious disease outbreak on health care workers. Can J Psychiatr. 2016;52:241–247. doi: 10.1177/070674370705200406. [DOI] [PubMed] [Google Scholar]
- 7.Mak I.W.C., Chu C.M., Pan P.C. Long-term psychiatric morbidities among SARS survivors. Gen Hosp Psychiatr. 2009;31:318–326. doi: 10.1016/j.genhosppsych.2009.03.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Huang Y., Zhao N. Generalized anxiety disorder, depressive symptoms and sleep quality during COVID-19 outbreak in China: a web-based cross-sectional survey. Psychiatr Res. 2020;288:112954. doi: 10.1016/j.psychres.2020.112954. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Teufel M., Schweda A., Dörrie N. Not all world leaders use Twitter in response to the COVID-19 pandemic: impact of the way of Angela Merkel on psychological distress, behaviour and risk perception. J Public Health. 2020;35:3085. doi: 10.1093/pubmed/fdaa060. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Brooks S.K., Webster R.K., Smith L.E. The psychological impact of quarantine and how to reduce it: rapid review of the evidence. Lancet. 2020;395:912–920. doi: 10.1016/S0140-6736(20)30460-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Löwe B., Decker O., Müller S. Validation and standardization of the generalized anxiety disorder screener (GAD-7) in the general population. Med Care. 2008;46:266–274. doi: 10.1097/MLR.0b013e318160d093. [DOI] [PubMed] [Google Scholar]
- 12.Kroenke K., Spitzer R.L. The PHQ-9: a new depression diagnostic and severity measure. Psychiatr Ann. 2002;32:509–515. doi: 10.3928/0048-5713-20020901-06. [DOI] [Google Scholar]
- 13.MacGregor K.L., Funderburk J.S., Pigeon W. Evaluation of the PHQ-9 Item 3 as a screen for sleep disturbance in primary care. J Gen Intern Med. 2012;27:339–344. doi: 10.1007/s11606-011-1884-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.RKI COVID19. 2020. https://npgeo-corona-npgeo-de.hub.arcgis.com/datasets/dd4580c810204019a7b8eb3e0b329dd6_0?selectedAttribute=AnzahlTodesfall [Google Scholar]
- 15.DAX aktuell heute realtime . 2020. DAX Chart - boerse.de.https://www.boerse.de/indizes/Dax/DE0008469008 [Google Scholar]
- 16.Bäuerle A., Skoda E.-M., Dörrie N. Psychological support in times of COVID-19: the Essen community-based CoPE concept. J Public Health. 2020;382:727. doi: 10.1093/pubmed/fdaa053. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Bäuerle A., Graf J., Jansen C. An e-mental health intervention to support burdened people in times of the COVID-19 pandemic: CoPE it. J Public Health. 2020;395:912. doi: 10.1093/pubmed/fdaa058. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Thombs B.D., Kwakkenbos L., Carrier M.-E. Protocol for a partially nested randomised controlled trial to evaluate the effectiveness of the scleroderma patient-centered intervention network COVID-19 home-isolation activities together (SPIN-CHAT) program to reduce anxiety among at-risk scleroderma patients. J Psychosom Res. 2020;135:110132. doi: 10.1016/j.jpsychores.2020.110132. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Multimedia component 1