Abstract
Introduction
Erectile dysfunction (ED) is a highly common sexual dysfunction of men but often undertreated as patients experience high treatment barriers.
Aim
The aims of this study were to characterize patients with ED using an online prescription platforms (OPPs) and determine treatment barriers that might prevent patients from seeking care in conventional health care settings.
Methods
Data from a German OPP were retrospectively analyzed with focus on patients suffering from ED with at least one online prescription of phosphodiesterase-5 (PDE5) inhibitors between May 2019 and November 2019. In addition, a voluntary questionnaire was used to assess additional social features and prior treatment barriers.
Main Outcome Measure
The main outcome measures were the epidemiological data, prescription metadata, and follow-up questionnaires.
Results
A total of 11,456 male patients received prescriptions via the OPP (mean age: 49 years [95% CI 46.92–47.45]). Patients lived mainly in rural areas (69%) and frequently sought prescriptions outside the average office times of German urologists (49%). From all patients that responded to a follow-up questionnaire (n = 242), the majority were employed full-time (81%), married (50%), and native German (94%); 63.5% had not used PDE5 inhibitors before. From all repeat users, 41% had received them from unreliable sources. Reasons to seek treatment via the OPP were convenience (48%), shame (23%), and lack of discretion (13%).
Conclusion
In this first study, to epidemiologically characterize ED patients of an OPP, it was confirmed that inconvenience is a treatment barrier, along with shame and perceived lack of discretion. This is the first evidence that OPPs reduce treatment barriers and ease access for patients to the medical system.
Rodler S, von Büren J, Buchner A, et al. Epidemiology and Treatment Barriers of Patients With Erectile Dysfunction Using an Online Prescription Platform: A Cross-Sectional Study. Sex Med 2020;8:370–377.
Key Words: Erectile dysfunction, Online prescription platform, Telemedicine, Treatment barrier
Introduction
Erectile dysfunction (ED) is a multidimensional and highly common sexual dysfunction of men.1 Psychogenic, vasculogenic, neurologic, and endocrinologic changes, among others, are involved in this complex disease.2 Treatment includes lifestyle interventions, pharmacological treatment with phosphodiesterase-5 (PDE5) inhibitors, vacuum erection devices, intracavernosal injections, and surgical interventions.3 As ED is highly associated with metabolic syndrome and cardiovascular disease, incidence rates are high in western countries with 52% among patients between 40 and 70 years old and increasing with age.4 This high prevalence is confirmed in later studies where researchers noted a prevalence peak of ED at age 50–59 years.5 A desire for therapeutic intervention was expressed in 50% of men in their 60s.6
Conversely, data on patients treated for ED do not reflect this high prevalence.7 ED is commonly missed in patient evaluations, either due to a lack of consideration, false patient beliefs, or embarrassment of both clinician and patient.8,9 This lack of consideration is aggravated in at-risk populations as studies demonstrate high ED rates but no awareness of the actual disease in this patient group.10 Further treatment barriers are time and geographical11 issues that prevent patients from seeking treatment, especially in rural areas.
Direct-to-consumer health care platforms have gained interest, especially in highly focused indications with high treatment barriers.12 In 2006, online consultation was considered effective in the treatment of ED, especially for men who experience high embarrassment.13 Digital health care platforms have also been shown to improve the treatment of urologic patients by overcoming geographical barriers14 and to provide urgent care for urinary tract infections.15 At the time of this study, a comprehensive analysis of patients with ED using online prescription platforms (OPP) is lacking.
Objectives
The objective of this study was to describe the characteristics of a population that accesses an OPP for ED, including demographic factors, spatial distribution, and time-related use patterns, along with identifying potential treatment barriers.
Methods
Study Design
A cross-sectional study was conducted with anonymized data provided by Direct Health Services, the provider of “www.gospring.de/” a German OPP for men's health. The OPP is advertised on Internet search engines, digital media, and commercial spots. Patient data are collected via structured questionnaires. The patient is asked for frequency, situations, and duration of onset of ED. Contraindications for prescription included relevant preexisting diseases (eg, cardiovascular, hematological, hepatological, or renal), body mass index, excessive alcohol consumption, and allergies. To avoid drug-to-drug interactions, the system checks for comedication of nitrates (eg, glycerol trinitrate), riociguat, human immunodeficiency virus (HIV) medication (eg, ritonavir or indinavir), antifungal medication (ketoconazole, itraconazole), and alpha-antagonists such as doxazosin. All answers were checked by physicians before fulfilling a prescription. Therapeutic options included sildenafil and tadalafil. Tadalafil is available in a 5 mg daily dosing regimen or as on-demand medication (5 mg, 10 mg, 20 mg). Sildenafil is available as an on-demand medication (25 mg, 50 mg, 100 mg). For other treatment options or in case of contraindications, patients are directed to urologists or general practitioners. After prescribing, the medication can be ordered in an attached online pharmacy and is delivered to the patient's home within 48 hours. Inquiries on the drugs efficacy and the appearance of potential side effects as well as new diseases are made by default via e-mail to ensure patient safety. All research has been carried out in accordance with the Code of Ethics of the World Medical Association (Declaration of Helsinki) and its later amendments. Informed consent was received from all patients. Before initiation of the study, the local ethics authority (Ethikkommission der Ludwig-Maximilian-Universität München) revised the project design and waived approval (reference number: 19-718).
In addition, a systematic literature review was conducted. We searched in title and abstract on MEDLINE for synonyms of ED as defined by a MeSH search (ie, Dysfunction, Erectile; Male Sexual Impotence; Impotence, Male Sexual; Sexual Impotence, Male; Male Impotence; Impotence, Male; Impotence) combined with either the MeSH synonyms for Telehealth (ie, Mobile Health; Health, Mobile; mHealth; Telehealth; eHealth; Remote Consultation) or the MeSH synonyms for shame (ie, shame; embarrassment). The complete set of MeSH terms was searched through http://www.nlm.nih.gov/mesh/. The search results were screened by 2 reviewers working independently and disagreements were resolved through consensus with a third reviewer. This manuscript was prepared according to the RECORD statement, a new extension of the STROBE statement.16
Setting
The service of the OPP is currently available in Germany only. Patient data were collected between May 2019 (service launch date) and November 2019. Between August 2019 and September 2019, a follow-up survey was conducted in this population (P2, Table 1). Participation in the follow-up survey was voluntary and had no impact on further treatment on the platform. Questionnaires with at least 90% of questions answered were included.
Table 1.
Patient characteristics
| Parameter | All prescriptions ED (P1) |
Follow-up survey (P2) |
Previously treated for ED (P3) |
P value (3 groups) | |||
|---|---|---|---|---|---|---|---|
| (n = 11,456) |
(n = 242) |
(n = 92) |
|||||
| % | n | % | x | % | n | ||
| Age | <.001 | ||||||
| Median | 49 | 52 | 52 | ||||
| 95% CI | 46.92–47.45 | 50.6–53.4 | 50.84–53.16 | ||||
| Range | 18–91 | 20–78 | 26-78 | ||||
| Age group | 100% | 10,680∗ | 100% | 237∗ | 100% | 84∗ | <0.001 |
| 18-25 | 6% | 685 | 3% | 6 | 0% | 0 | |
| 26-30 | 7% | 794 | 4% | 9 | 4% | 3 | |
| 31-40 | 19% | 2,045 | 11% | 27 | 14% | 12 | |
| 41-50 | 25% | 2,665 | 26% | 62 | 21% | 18 | |
| 51-60 | 30% | 3,232 | 41% | 98 | 44% | 37 | |
| 61-70 | 12% | 1,259 | 15% | 35 | 17% | 14 | |
| PDE5 | 100% | 9,351∗ | 100% | 233∗ | 100% | 84∗ | 0.005 |
| Sildenafil | 77% | 7,154 | 71% | 166 | 68% | 57 | |
| Viagra | 3% | 285 | 7% | 16 | 1% | 1 | |
| Tadalafil | 18% | 1,696 | 20% | 47 | 27% | 23 | |
| Cialis | 2% | 216 | 2% | 4 | 4% | 3 | |
| Location | 100% | 11,456 | 100% | 242 | 100% | 88 | 0.09 |
| Rural | 69% | 7,937 | 67% | 162 | 59% | 52 | |
| Urban | 31% | 3,519 | 33% | 80 | 41% | 36 | |
| Day time | 100% | 11,456 | 100% | 242 | 100% | 88 | 0.216 |
| Office time | 51% | 5,657 | 53% | 128 | 57% | 50 | |
| Out of office time | 49% | 5,799 | 47% | 114 | 43% | 38 | |
| Weekday | 100% | 11,456 | 100% | 242 | 100% | 88 | 0.84 |
| Monday to Friday | 73% | 8,318 | 71% | 173 | 70% | 62 | |
| Weekend | 27% | 3,138 | 29% | 69 | 30% | 26 | |
Numbers are lower than the respective population due to changes in the structured questionnaires in the first month of the service.
Participants
Male patients who received prescriptions for ED via the OPP were included in this study. Patients aged 18 years old or older with self-assessed ED were eligible for prescription evaluation. ED was confirmed by physicians' prior prescription, including only patients experiencing ED problems regularly.17 Patients living in cities with more than 100,000 inhabitants were classified as “urban” while all others were considered “rural.”18
Statistical Analysis
A chi-square test was used for statistical analysis, and P-values smaller than 0.05 were regarded as statistically significant. All calculations were conducted by MedCalc 19 (MedCalc, Ostend, Belgium) software.
Results
General Patient Characteristics
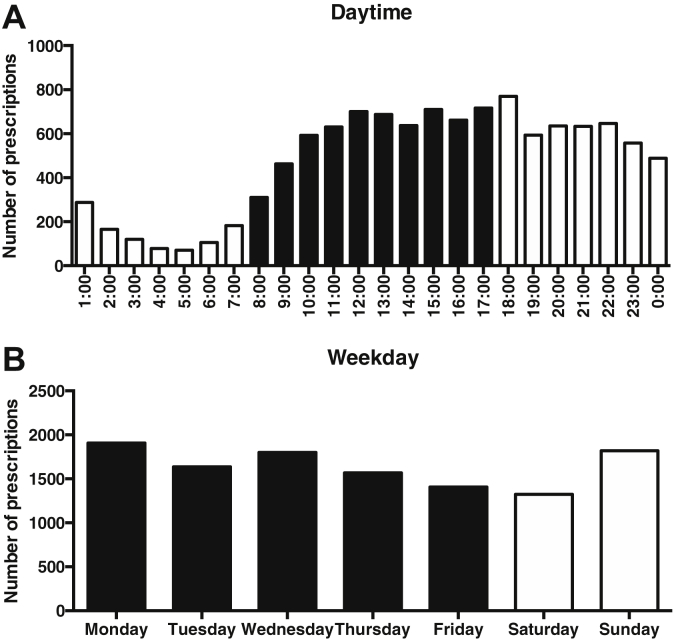
The cohort consisted of 11,456 patients (P1) diagnosed with ED on the OPP between May 2019 and November 2019. Mean age at the time of prescription was 49 years (95% CI 46.92–47.45; range 18–91, Table 1). Approximately 80% were treated with the active substance sildenafil, and 20% of patients received the active substance tadalafil. 69 percent reported living in a rural area, whereas 31% lived in urban areas. Approximately half of treatment requests (51%) occurred between 7 am and 5 pm during the average working hours of a urologist, whereas 49% occurred between 9 pm and 7 am (Figure 1A). The number of prescriptions was independent of the weekday. 27 percent of prescriptions were written on the weekend and 73% from Monday to Friday. The days with the highest number of treatment requests were Sunday and Monday (Figure 1B).
Figure 1.
Prescription volume by daytime and weekday. (A) The average prescription volume (n = 11,465) was analyzed by hours. Daytime was defined as the time between 8 and 17 (black), approximating the opening hours of urologists and pharmacies. (B) Prescription volumes (n = 11,465) were analyzed by weekday. Monday to Friday were defined as weekdays (black), referring to the opening days of urologists in Germany.
Analysis was conducted for a subset of 242 patients (P2) that responded to the follow-up questionnaire completely. The P2 group differed significantly in terms of age with an average age of 52 years (95% CI 50.6–53.4; range 20–78; P < .001). This age difference also appeared with the subgroup of patients who had previously been treated with PDE5 inhibitors (P3: n = 92) with a mean age of 52 (95% CI 50.84–53.16; range 26–78; P < .001). Other treatment characteristics like active substance used, location, time of day, and day of the week revealed no significant differences between the 3 groups.
Additional Social Features of Patients
Through a voluntary follow-up questionnaire, further patient characteristics were investigated (Table 2). Mid-range earners were the largest subgroup of those seeking help, represented by 35% with a monthly gross income between 2,001 and 3,000 euros and 30% between 3,001 and 5,000 euros. 50 percent of respondents had a master's or bachelor's degree, 18% had completed vocational training, and 32% had a high school degree as their highest education level. 50 percent of respondents stated they were married, 26% were in a relationship, and 19% were single. In terms of sexual orientation, 88% of patients identified themselves as heterosexual, 4% as homosexual, and 5% as bisexual. Concerning employment status, 81% of respondents were employed full-time, 4% part-time, and 10% were retired. Regarding ethnicity, 94% considered themselves native German, while 6% identified as immigrants.
Table 2.
Social characteristics
| Parameter | Follow-up survey (P2) |
|
|---|---|---|
| (n = 242) | ||
| % | n | |
| Income | 100% | 242 |
| <1,000 | 5% | 11 |
| 1,001-2,000 | 19% | 46 |
| 2,001-3,000 | 35% | 84 |
| 3,001-5,000 | 30% | 73 |
| >5,000 | 12% | 28 |
| Education | 100% | 242 |
| University degree | 50% | 120 |
| Training | 18% | 43 |
| School | 32% | 79 |
| Relationship status | 100% | 242 |
| Single | 19% | 47 |
| Relationship | 26% | 64 |
| Married | 50% | 120 |
| Other | 5% | 11 |
| Sexual orientation | 100% | 242 |
| Heterosexual | 88% | 214 |
| Homosexual | 4% | 10 |
| Bisexual | 5% | 12 |
| Other | 2% | 6 |
| Employment status | 100% | 252∗ |
| Full time | 81% | 203 |
| Part time | 3% | 8 |
| Unemployed | 1% | 2 |
| Retired | 10% | 25 |
| Student | 2% | 4 |
| Other | 3% | 10 |
| Migration background | 100% | 242 |
| German | 94% | 227 |
| Non-German | 6% | 15 |
Multiple answers of 242 respondents.
Previous Usage of Phosphodiesterase-5 (PDE5) Inhibitors
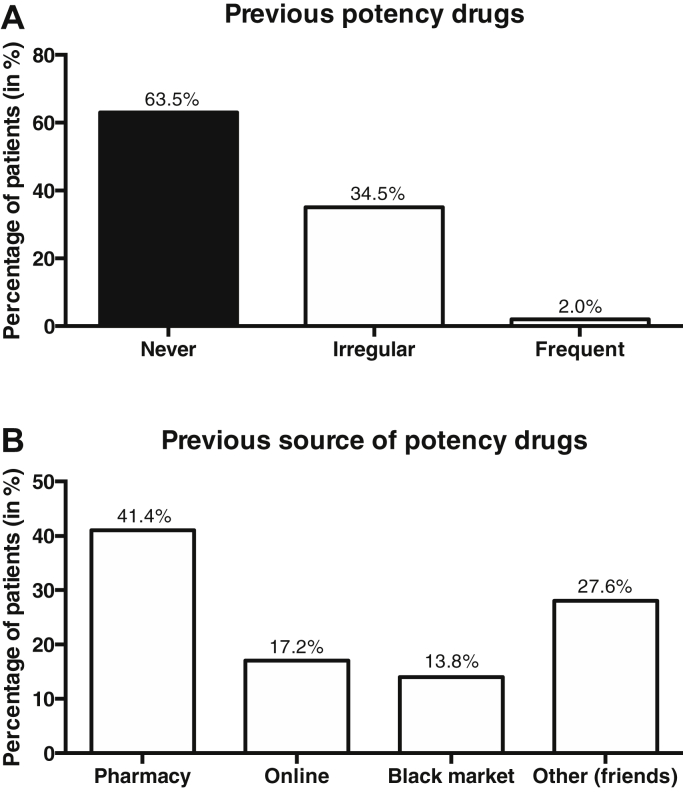
Patients who agreed to answer the follow-up questionnaire (n = 242) were asked for their previous treatment with PDE5 inhibitors. No previous usage was reported by 63.5% of patients (Figure 2A). Of the patients who had used potency drugs previously (n = 92), 41% reported purchasing the medication at a pharmacy, 17% via online sources, 14% via the black market, and 28% via other sources, such as through a friend (Figure 2B).
Figure 2.
Previous prescription and source of potency drugs. (A) Patients who agreed to answer the follow-up questionnaire (n = 242) were asked for their previous usage of potency drugs. Answer options were limited to either “never” (black) or previous use (white). When patients stated previous use, they could choose between “irregular” or “frequent” use. (B) All patients who have used potency drugs before (n = 92) were selected and asked for the primary source of their prior potency drug prescription.
Rationale for Online Prescription and Source of Referral
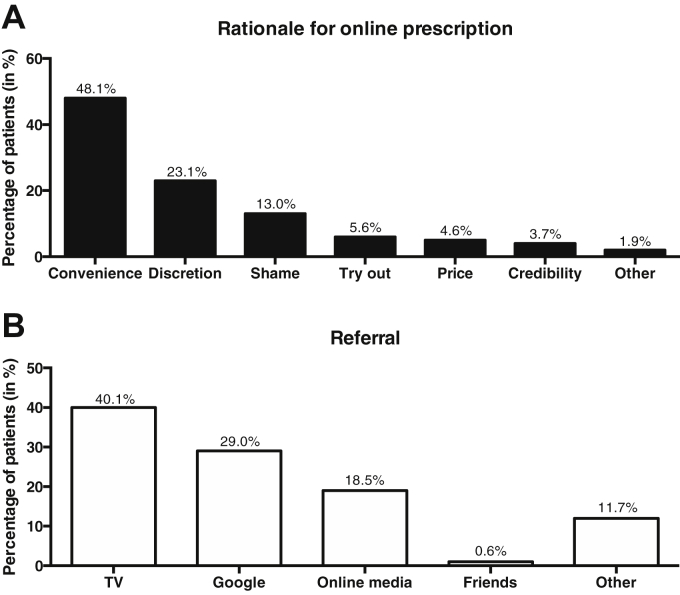
Patients were asked for their primary motivation to use an OPP to identify potential treatment barriers in conventional prescription settings. The question was included in the follow-up questionnaire (P2) with a time lag. Patients (n = 152) were allowed to choose multiple options. 48 percent of respondents stated convenience was one of the main reasons for using an OPP, 23% for discretion, and 13% for shame (Figure 3A). Patients were referred to the OPP via TV advertising (40%), Google search engine advertising (29%), online media focusing on ED (19%), friends (1%), and other sources (12%, Figure 3B).
Figure 3.
Rationale and referral for online prescription of PDE5 inhibitors. (A) Patients (n = 242) were asked where they have heard about the analyzed online prescription platform for the first time. Response options included TV advertising (TV), Google search engine advertisement (Google), online articles about, for example, erectile dysfunction treatment (Online media) and friends as well as other sources. (B) Patients (n = 152) were asked for their primary reason to use an online prescription platform to identify potential treatment barriers in conventional prescription settings.
Discussion
In this study of patients with ED using a German OPP for prescription of PDE5 inhibitors, most patients were between 40 and 60 years old, married, and living in a rural area. Convenience, discretion, and shame were major reasons to use this OPP to buy PDE5 inhibitors. For most patients, it was the first prescription of PDE5 inhibitors, while previously treated patients showed considerable use from potentially illegal sources.
The average male in Germany is 43.1 years old19 with the largest birth group being 55 years old.20 The incidence of ED increases over time with rates of 28% at age 50 years and 64% at age 70 years.5 According to those studies, the ED rate in Germany for 45-year-old patients is reported to be 25.2%.21 The average age of patients using the OPP was 49 years with 50% of users being between 37 and 56 years old. As we were expecting higher ED rates in the older age groups, the population using the OPP seems to be left-shifted compared with the expected overall prevalence in the respective age groups.
In 2017, 20.9 million or 62% of men above 18 years were in relationships, of which 84% were married.22 In the analyzed cohort, the percentage of people in relationships was 76% higher than the previously mentioned study. Data on sexual orientation in Germany are limited to a few studies, revealing 87% of the German population as heterosexual and around 1% as homosexual.23 Patients using the OPP presented with a rate of 4% as homosexual, reflecting either a higher engagement of homosexuals with their sexuality or higher rates of homosexual men detected by real-world surveys.24
The average net income in Germany is 3,132 €25—comparable to the study cohort. The distribution across the various income categories confirms this finding and reveals similar percentages in Germany and this study.26 The employment rate in Germany for men is 79.6% with 6–12% of men working part-time, depending on age.27 Rates were higher in the study cohort, with a higher percentage in full-time jobs.
24 percent of males in Germany have a migratory background compared to 6% of OPP users.28 Patients with migration background might be underrepresented as they are either not attracted by the advertising strategy of the OPP or they have higher treatment barriers than the average population. As this is the first study to characterize a patient cohort using an OPP for ED, it has been revealed that patients were on average younger than expected, were mostly in full-time employment, were less likely to have a migratory background, and were more likely to be in a relationship or married than the overall German population.
ED is commonly associated with high treatment barriers. Embarrassment, either to talk to a doctor or for the doctor to ask, is frequently reported in the literature.1 13 percent of patients from P2 reported shame and 23% reported discretion as the leading reason to use an OPP, revealing that both aspects related to embarrassment are important. Although many studies focus on shame, the distance to a specialist center is also reported to be a concern.29 In the study cohort, the majority (69%) was from rural areas, compared to 62% in the overall German population.18 People in these areas might have less access or have to make greater efforts to reach a specialist.
The analysis of the prescription request times revealed that 49% of prescriptions were written outside the estimated standard office times of a German urologist. Surprisingly, 48% of the study cohort stated convenience as the major reason to use an OPP. Convenience might therefore apply to both geographical and time-related treatment barriers. Interestingly, from a patient perspective, the traditional treatment barriers of shame and discretion are outweighed by convenience. The data suggest that primarily full-time employed, married patients aged between 40 and 60 years use the OPP to get accelerated access to the medical system and thereby avoid time or distance-related treatment barriers. These findings are highlighted by the fact that for most patients, it is the first prescription of a PDE5 inhibitor.
In the past, treatment barriers have led to high rates of illicit PDE5 inhibitor use as patients bypass the medical system. A Swiss study revealed that the overall prevalence of men using PDE5 inhibitors without prior professional health care interaction was 3.0% and that 32.3% of patients buying PDE5 inhibitors bought them without prior professional health care interaction.30 In the OPP group, a large percentage had obtained PDE5 inhibitors either directly from illegal sources or via friends. PDE5 inhibitors from illegal sources put patients at risk of wrong dosing or active ingredient.31 In addition, relevant contraindications and conditions where ED is an early warning symptom of other diseases1 might be overlooked, such as diseases caused by cardiovascular risk factors, like diabetes mellitus, hypertension, dyslipidemia, and sleep apnea.32, 33, 34, 35 In this setting, health care platforms can grant access for patients confronted by treatment barriers to the medical system and achieve not just an improved quality of life but also treat the underlying disease and treat it effectively. Therefore, OPPs have the potential to reduce illegal substance use and promote the health of men.
OPPs seem to be an important addition to the treatment options of patients. Besides the OPP in this study, health platforms can be applied to other diseases and conditions where specialists are either spatially or temporarily not available,36 where high treatment barriers exist,37 or where access to medical care has to be facilitated.38 Quick scalability in predefined indications and thereby access of a large population to specialized care are of great potential, but equivalence in standard of care to in-person visits has still to be demonstrated.12 OPPs have the potential to provide a high standard of care as treatment algorithms are standardized. High-quality OPPs might focus on structured follow-up to evaluate safety and efficacy of the prescribed drugs besides the initial indication. Through structured follow-up of underlying diseases and prevention, a higher standard than routine outpatient care might be provided. Furthermore, high-risk patients could be referred earlier to a specialist—either in-person or online. Thereby, OPPs can, in selected indications, close an important care gap and add to adherence and pharmacovigilance. As there are limited data on safety and efficacy of such platforms, further research is warranted to assess OPPs prospectively.
This study is limited by the cross-sectional design, as causative connections and developments over time cannot be analyzed. Response to the additional follow-up survey was voluntary. Despite a high response rate of 35.5%, sample bias might apply, as P2 and P3 were significantly older than P1. Nevertheless, important treatment barriers, such as location, time of day, and day of the week, are equally distributed throughout all groups. As certain parts of the questionnaire include sensitive questions, some patients might have answered inaccurately. The validity of the study is limited by the OPP design and advertising channels, such as TV commercials potentially attracting more elderly people. Therefore, conclusions about treatment barriers in the overall German population might not be represented and would require further evaluation, especially in underrepresented subgroups.
Conclusion
As the first study to epidemiologically characterize ED patients using an OPP, most patients were found to be full-time employed, married, native German, and living in a rural area. Patients using the OPP reported convenience, shame, and discretion as treatment barriers and searched for solutions to surpass them. OPPs can fill this demand and prevent patients from purchasing PDE5 inhibitors outside the medical system. Through the deployment of interdisciplinary follow-up of associated diseases and the potential to provide an access point to the medical system, OPPs might be beneficial beyond their primary focus. Further research is warranted to verify positive effects on medical care and to determine the safety and efficacy of OPPs prospectively.
Statement of authorship
Category 1
-
(a)Conception and Design
- Severin Rodler; Sven Jungmann; Christian Wülfing
-
(b)Acquisition of Data
- Katja Elkhanova; Johannes von Büren
-
(c)Analysis and Interpretation of Data
- Severin Rodler; Sven Jungmann; Alexander Buchner
Category 2
-
(a)Drafting the Article
- Severin Rodler; Sven Jungmann; Johannes von Büren; Christian Wülfing
-
(b)Revising It for Intellectual Content
- Christian Wülfing; Sven Jungmann; Christian Stief; Severin Rodler
Category 3
-
(a)Final Approval of the Completed Article
- Severin Rodler; Christian Wülfing; Sven Jungmann
Footnotes
Ethics Committee Approval: Before initiation of the study, the local ethics authority (Ethikkommission der Ludwig-Maximilian-Universität München) revised the project design and waived approval (reference number: 19-718).
Funding: This study was supported and anonymized data provided by Direct Health Services.
Conflict of Interest: S.R., C.W., and S.J. serve on the medical advisory board of Direct Health Services, the provider of www.gospring.de. J.v.B. and K.E. are employees of Direct Health Services GmbH. C.W. owns shares of Direct Health services GmbH.
References
- 1.Yafi F.A., Jenkins L., Albersen M. Erectile dysfunction. Nat Rev Dis primers. 2016;2:16003. doi: 10.1038/nrdp.2016.3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Pastuszak A.W. Current diagnosis and Management of erectile dysfunction. Curr Sex Health Rep. 2014;6:164–176. doi: 10.1007/s11930-014-0023-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Mobley D.F., Khera M., Baum N. Recent advances in the treatment of erectile dysfunction. Postgrad Med J. 2017;93:679–685. doi: 10.1136/postgradmedj-2016-134073. [DOI] [PubMed] [Google Scholar]
- 4.Feldman H.A., Goldstein I., Hatzichristou D.G. Impotence and its medical and psychosocial correlates: results of the Massachusetts Male Aging Study. J Urol. 1994;151:54–61. doi: 10.1016/s0022-5347(17)34871-1. [DOI] [PubMed] [Google Scholar]
- 5.Corona G., Lee D.M., Forti G. Age-related changes in general and sexual health in middle-aged and older men: results from the European Male Ageing Study (EMAS) J Sex Med. 2010;7:1362–1380. doi: 10.1111/j.1743-6109.2009.01601.x. [DOI] [PubMed] [Google Scholar]
- 6.Bacon C.G., Mittleman M.A., Kawachi I. Sexual function in men older than 50 years of age: results from the health professionals follow-up study. Ann Intern Med. 2003;139:161–168. doi: 10.7326/0003-4819-139-3-200308050-00005. [DOI] [PubMed] [Google Scholar]
- 7.Mulhall J.P., Luo X., Zou K.H. Relationship between age and erectile dysfunction diagnosis or treatment using real-world observational data in the USA. Int J Clin Pract. 2016;70:1012–1018. doi: 10.1111/ijcp.12908. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Shabsigh R., Perelman M.A., Laumann E.O. Drivers and barriers to seeking treatment for erectile dysfunction: a comparison of six countries. BJU Int. 2004;94:1055–1065. doi: 10.1111/j.1464-410X.2004.05104.x. [DOI] [PubMed] [Google Scholar]
- 9.Almigbal T.H., Schattner P. The willingness of Saudi men with type 2 diabetes to discuss erectile dysfunction with their physicians and the factors that influence this. PloS one. 2018;13:e0201105. doi: 10.1371/journal.pone.0201105. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Shabsigh R., Kaufman J., Magee M. Lack of awareness of erectile dysfunction in many men with risk factors for erectile dysfunction. BMC Urol. 2010;10:18. doi: 10.1186/1471-2490-10-18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Uhlman M.A., Gruca T.S., Tracy R. Improving access to urologic care for rural populations through outreach clinics. Urology. 2013;82:1272–1276. doi: 10.1016/j.urology.2013.08.053. [DOI] [PubMed] [Google Scholar]
- 12.Jain T., Lu R.J., Mehrotra A. Prescriptions on demand: the growth of direct-to-consumer telemedicine Companies. JAMA. 2019 doi: 10.1001/jama.2019.9889. [DOI] [PubMed] [Google Scholar]
- 13.Leusink P.M., Aarts E. Treating erectile dysfunction through electronic consultation: a pilot study. J Sex Marital Ther. 2006;32:401–407. doi: 10.1080/00926230600835361. [DOI] [PubMed] [Google Scholar]
- 14.Witherspoon L., Liddy C., Afkham A. Improving access to urologists through an electronic consultation service. Can Urol Assoc J. 2017;11:270–274. doi: 10.5489/cuaj.4314. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Rastogi R., Martinez K.A., Gupta N. Management of urinary tract Infections in direct to consumer telemedicine. J Gen Intern Med. 2019;35:643–648. doi: 10.1007/s11606-019-05415-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Benchimol E.I., Smeeth L., Guttmann A. The REporting of studies Conducted using Observational Routinely-collected health Data (RECORD) statement. PLoS Med. 2015;12:e1001885. doi: 10.1371/journal.pmed.1001885. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.O'Donnell A.B., Araujo A.B., Goldstein I. The validity of a single-question self-report of erectile dysfunction. Results from the Massachusetts Male Aging Study. J Gen Intern Med. 2005;20:515–519. doi: 10.1111/j.1525-1497.2005.0076.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Statistisches Bundesamt Gemeindeverzeichnis-Informationssystem GV-ISys. www.destatis.de/DE/Themen/Laender-Regionen/Regionales/Gemeindeverzeichnis/_inhalt.html Available at:
- 19.Statistisches Bundesamt Bevölkerungsstand. https://www.destatis.de/DE/Themen/Gesellschaft-Umwelt/Bevoelkerung/Bevoelkerungsstand/Tabellen/durchschnittsalter-zensus.html;jsessionid=D0F8DDE9C65C9F9241547BD97A68D19E.internet731 Available at:
- 20.Statistisches Bundesamt Bevölkerung in deutschland. https://service.destatis.de/bevoelkerungspyramide/#! Available at:
- 21.Hallanzy J., Kron M., Goethe V.E. Erectile dysfunction in 45-year-old heterosexual German men and associated lifestyle risk factors and Comorbidities: results from the German male sex study. Sex Med. 2019;7:26–34. doi: 10.1016/j.esxm.2018.11.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Statistisches Bundesamt Bevölkerung. www.destatis.de/DE/Themen/Gesellschaft-Umwelt/Bevoelkerung/Haushalte-Familien/Publikationen/Downloads-Haushalte/lebenssituation-maenner-5122204179004.pdf?__blob=publicationFile Available at:
- 23.Haversath J., Garttner K.M., Kliem S. Sexual Behavior in Germany. Dtsch Arztebl Int. 2017;114:545–550. doi: 10.3238/arztebl.2017.0545. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Dalia Research Counting the LGBT population: 6% of Europeans identify as LGBT. www.daliaresearch.com/blog/counting-the-lgbt-population-6-of-europeans-identify-as-lgbt Available at:
- 25.Statistisches Bundesamt Einkommen, Einnahmen, Ausgaben. www.destatis.de/DE/Themen/Gesellschaft-Umwelt/Einkommen-Konsum-Lebensbedingungen/Einkommen-Einnahmen-Ausgaben/Tabellen/liste-gebietsstaende.html Available at:
- 26.Statistisches Bundesamt Wirtschaftsrechnung. www.destatis.de/DE/Themen/Gesellschaft-Umwelt/Einkommen-Konsum-Lebensbedingungen/Einkommen-Einnahmen-Ausgaben/Publikationen/Downloads-Einkommen/einkommensverteilung-2152606139004.pdf?__blob=publicationFile Available at:
- 27.Statistisches Bundesamt Bevölkerung und Erwerbstätigkeit. www.destatis.de/DE/Themen/Arbeit/Arbeitsmarkt/Erwerbstaetigkeit/Publikationen/Downloads-Erwerbstaetigkeit/erwerbsbeteiligung-bevoelkung-2010410187004.pdf?__blob=publicationFile Available at:
- 28.Statistisches Bundesamt Bevölkerung und Erwerbstätigkeit. https://www.destatis.de/DE/Themen/Gesellschaft-Umwelt/Bevoelkerung/Migration-Integration/Publikationen/Downloads-Migration/migrationshintergrund-2010220177004.pdf?__blob=publicationFile&v=4 Available at:
- 29.Ball M., Nelson C.J., Shuk E. Men's experience with sexual dysfunction post-rectal cancer treatment: a qualitative study. J Cancer Educ. 2013;28:494–502. doi: 10.1007/s13187-013-0492-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Schnetzler G., Banks I., Kirby M. Characteristics, behaviors, and attitudes of men bypassing the healthcare system when obtaining phosphodiesterase type 5 inhibitors. J Sex Med. 2010;7:1237–1246. doi: 10.1111/j.1743-6109.2009.01674.x. [DOI] [PubMed] [Google Scholar]
- 31.Keizers P.H.J., Wiegard A., Venhuis B.J. The quality of sildenafil active substance of illegal source. J Pharm Biomed Anal. 2016;131:133–139. doi: 10.1016/j.jpba.2016.08.027. [DOI] [PubMed] [Google Scholar]
- 32.Fung M.M., Bettencourt R., Barrett-Connor E. Heart disease risk factors predict erectile dysfunction 25 years later: the Rancho Bernardo Study. J Am Coll Cardiol. 2004;43:1405–1411. doi: 10.1016/j.jacc.2003.11.041. [DOI] [PubMed] [Google Scholar]
- 33.Chiurlia E., D'Amico R., Ratti C. Subclinical coronary artery atherosclerosis in patients with erectile dysfunction. J Am Coll Cardiol. 2005;46:1503–1506. doi: 10.1016/j.jacc.2005.06.068. [DOI] [PubMed] [Google Scholar]
- 34.Saigal C.S., Wessells H., Pace J. Predictors and prevalence of erectile dysfunction in a racially diverse population. Arch Intern Med. 2006;166:207–212. doi: 10.1001/archinte.166.2.207. [DOI] [PubMed] [Google Scholar]
- 35.Budweiser S., Enderlein S., Jorres R.A. Sleep apnea is an independent correlate of erectile and sexual dysfunction. J Sex Med. 2009;6:3147–3157. doi: 10.1111/j.1743-6109.2009.01372.x. [DOI] [PubMed] [Google Scholar]
- 36.Fogel A.L., Sarin K.Y. A survey of direct-to-consumer teledermatology services available to US patients: Explosive growth, opportunities and controversy. J Telemed Telecare. 2017;23:19–25. doi: 10.1177/1357633X15624044. [DOI] [PubMed] [Google Scholar]
- 37.Orizio G., Merla A., Schulz P.J. Quality of online pharmacies and websites selling prescription drugs: a systematic review. J Med Internet Res. 2011;13:e74. doi: 10.2196/jmir.1795. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Jain T., Schwarz E.B., Mehrotra A. A Study of Telecontraception. New Engl J Med. 2019;381:1287–1288. doi: 10.1056/NEJMc1907545. [DOI] [PubMed] [Google Scholar]