Abstract
Purpose
We reported one patient infected with acute respiratory syndrome coronavirus-2 (SARS-CoV-2) presented with sleep disorders; insomnia and restless leg syndrome.
Methods
Patient data were obtained from medical records from Al-Raghy Isolation Hospital in Assuit University.
Results
A 49-year-old female patient presented with insomnia and restless leg syndrome associated with anosmia, ageusia. Three days before, she had developed a cough, malaise and athenia, headache, arthralgia, myalgia affecting mainly upper limbs, diarrhea and a fever followed by tachypnea. The naso-oropharyngeal swab test for coronavirus disease 2019 (COVID-19) by qualitative real-time reverse-transcriptase–polymerase-chain-reaction assay was positive. The patient was treated with Oseltamivir 75mg and clarithromycin 500 mg (12 hourly for each respectively) for 10 days with paracetamol. Two weeks later, the patient made a complete neurological and respiratory recovery.
Conclusion
Our case highlighted the rare occurrence of restless leg syndrome and insomnia during the COVID-19 pandemic. The era of sleep disorders spectrum in patients with COVID-19 remains to be characterized suggesting a frightening scientific association between COVID-19 and neuropsychiatric illness.
Keywords: Sleep disorders, COVID-19
1. Background
The coronavirus disease 2019 (COVID-19) is critically affecting not only the physical health but also mental health globally (Hossain et al., 2020; Rajkumar, 2020; Sultana et al., 2020). The spectrum of the coronavirus disease 2019 (COVID-19) ranges from asymptomatic infection to severe respiratory failure. Gastrointestinal (e.g., diarrhea) or even neurological manifestations (e.g., headache) have also been reported as other features of COVID-19. In addition, other neurological symptoms such as anosmia and ageusia are presented by many patients (Gutiérrez-Ortiz et al., 2020). There is a scarcity of evidence on the magnitude of sleep disorders among individuals affected by this pandemic. In humans infected with influenza virus, sleep duration decreases during incubation and increases during the symptomatic phase. A recent review of randomized control trials of oseltamivir versus placebo in adults and adolescents with influenza showed a significantly faster return to baseline sleep durations with treatment, supporting the notion that it was the virus that caused increased sleep (Das et al., 2020). Interestingly, We describe a case of COVID-19-associated sleep disorders as presenting symptoms.
2. Case presentation
On May 12, 2020, a 49-year-old healthcare worker woman known to have hypertension, diabetes mellitus and ischemic heart disease with paroxysmal atrial fibrillation (AF); was admitted to isolation emergency department of Assuit University Hospitals for fever, dry cough, tachypnoea, watery diarrhea, lassitude, arthralgia and myalgia. One week before, while the patient was in Aswan Univeristy Hospitals developed fever (38.5–39 °C), dry cough with burning sensation in the nasopharynx and sore throat. This was associated with severe agonizing pain allover the body especially joints and muscles of upper limbs. At this time, she was treated with antibiotic, antipyretic and antitussive medications. Within 2 days, she developed bleeding per nose, infrequent blood tinged sputum, severe anorexia and loss of taste and smell. Meanwhile, she experienced sleep disturbances; insomnia, poor sleep quality, and abnormal events that occur during sleep as strong urge to move her legs over the nigh that improved somewhat by moving them (restless leg syndrome). Therefore, the patient was transferred to Assuit University Hospitals for admission by her will. On admission at Al-Raghy isolation Hospital of Assuit University Hospitals, the patient was alert, tachypneic with elevated body temperature (39 °C). No evidence of clinical abnormalities or neurological deficits. Computed Tomography (CT) scan of the chest was positive for bilateral interstitial alveolar pneumonitis scattered in the periphery “subpleural” of both lungs namely at the posterior segment of the right upper lung lobe, apical, medial posterior basal and lateral segments of right lower lung lobe, anterior segment of left upper lung lobe and apical segment of left lower lung lobe characteristic for atypical pneumonia/viral infection from COVID-19 (Fig. 1). Laboratory analysis revealed normal complete blood count except for reduced hemoglobin level (10.0 g/dl) with mildly elevated erythrocytic sedimentation rate (ESR). However, the levels of ferritin, D-dimer and c-reactive protein (CRP) were normal. Her oxygen saturation 97%. No arrhythmias were noted during the hospitalization. EEG and polysomnography were ruled out to prevent further exposure with the COVID-19 patient. During hospitalization, she received oseltamivir 75mg, zinc vitamin and vitamin C 5oomg (12 hourly for each) for 10 days with repeated PCR every 48 hours and her sleep restored normal on the fourth days of treatment. 5 days later, she was discharged with complete clinical improvement and two successive negative PCR results (48 hours apart).
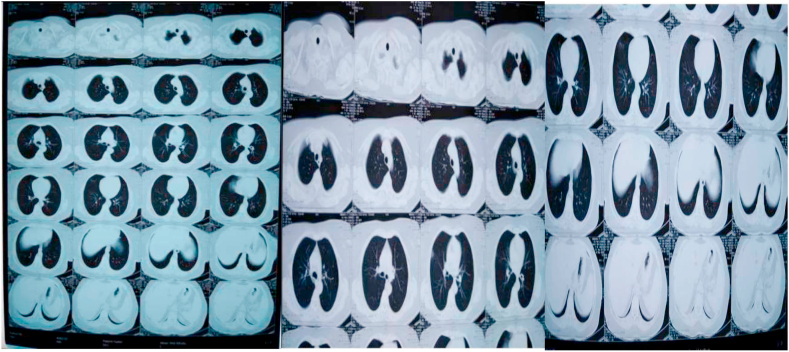
Fig. 1.
Chest CT of the patient. Bilateral scattered interstitial alveolar pneumonitis, viral etiology is suggested.
3. Discussion and conclusion
To our knowledge, the interaction between sleep disorders and COVID-19 pandemic is not yet elucidated. In this study, we expressed a case with PCR confirmed COVID-19 infection presented with sleep disorders. Sleep is a fundamental CNS phenomenon that is regulated by complex interactions between neurotransmitters, immunologically active peptides, and hormones (Besedovsky et al., 2019).
In our PCR positive COVID-19 case, the main presenting sleep disorders were insomnia and restless leg syndrome. This could be directly related to the infection per se or related to hypoxia. Notably, Sleep and the immune system are bidirectionally related. However, the mechanisms of these changes have not been determined entirely. This hypothesis was in agreement with Ibarra-Coronado et al. (2015) who suggested that altered sleep during infection is a component of the acute phase response, promoting recovery during illness, likely through mechanisms that involve cytokines and interleukins and their receptors, as well as receptors of the innate immune system. The consequent secretion of these immunological mediators is accompanied by responses by the endocrine and nervous systems, such as the secretion of cortisol and epinephrine. These substances can cross the blood-brain barrier to reach their receptors in various neural structures or may have a vagal input to modulate the responses that maintain homeostasis.
Moreover, Das et al. (2020), stated that no single cytokine is consistently associated with sleep, and this may explain why different infections are associated with different patterns of sleep disruption. Cytokine storm, which is a well known immune reaction of this particular viral infection, may lead to inflammation and injury of the central nervous system tissue. Furthermore, Wan et al. (2020), stated that interleukin (IL)-6, an important member of the cytokine storm, was associated with the severity of COVID-19 symptoms. Interestingly, Lasselin et al. (2019), reported that poor sleep quality and longer sleep latency which are central symptoms in insomnia, were observed during acute respiratory infection, suggested that immune processes could possibly contribute to pathological states of sleep disturbances. Moreover, respiratory infections affected both objective and subjective sleep in a number of ways: when sick, people spent objectively longer time in bed and slept longer, but also suffered from more awakenings, at least during the first days when symptoms were high. During sickness, people also reported having worse sleep quality, increased difficulties falling asleep, more restless sleep and less deep sleep. Asif (Asif et al., 2017), reported that Sleep and stress are also associated. While sleep inhibits the activity of the hypothalamic-pituitary- adrenal gland (HPA) axis, which mediates several facets of the response to most stressors, several stressors inhibit sleep and increase waking time and brain cortical arousal.
Our patient had restless leg syndrome (RLS).This could be attributed by COVID19-induced cytokine storm syndrome which led to cytokine IL-6 production that can stimulate up-regulation of hepcidin production in the choroid plexus. This hepcidin bound to choroid plexus-associated ferroportin, leading to decrease availability of iron for the CNS in RLS. Moreover, the microcytic hypo chromic anemia due to low serum iron level in our case could be considered as another factor behind the occurrence of RLS. These findings were in consistent with Weinstock et al. (2011), who stated that Inflammation can lead to systemic iron deficiency that could trigger CNS iron deficiency and subsequent RLS symptoms. Another explanation for the occurrence of RLS is that our patient had known to be diabetic and so, she could had a subclinical, otherwise asymptomatic diabetic peripheral neuropathy which exacerbate with viral infection.
Fortunately, our case restored normal sleep pattern on the fourth day of admission after receiving treatment with combination therapy of oseltamivir and azithromycin with improvement of her general condition. This could be attributed to the fact of oseltamivir could reduce the cellular and cytokine inflammatory response, block the viral replication and thus it could prevent triggering dysregulation of immune response. Our results were in concordance with Chokalingam et al. (Chockalingam et al., 2016), who reported the oseltamivir was able to inhibit the viral release and thereby inhibit viral replication during the initial infection period. Moreover, Bettis et al. (2006), who showed a significantly faster return to baseline sleep durations with treatment with oseltamivir versus placebo in adults and adolescents with influenza. Interestingly Ishaqui et al. (2020), reported that the combination therapy of oseltamivir and azithromycin, like in our case, significantly reduced numerous proinflammatory cytokines and there was a trend towards faster symptoms resolution compared with oseltamivir alone.
We recognize that the main limitations of the case were the absence of electroencephalography and polysomnography studies as well as magnetic resonance imaging of brain. The reason for this was the extreme circumstances in our hospitals at the peak of this pandemic.
In conclusion, we described a patient with confirmed PCR COVID-19 infection who presented by fever, asthenia, insomnia and restless leg syndrome with good outcome. Neurological manifestations might occur because of an aberrant immune response to COVID-19. At present, the full clinical spectrum of patients with COVID-19 with sleep disorders remains to be characterized. Further studies would be urgently needed for a comprehensive understanding of the neurological pathology of COVID-19 and its effects on the nervous system. Improving our understanding of the neurobiology of corona viruses could augment our knowledge of sleep disorders with potential viral association.
4. Ethics approval and consent to participate
The current study was approved by the Institutional Ethics Committee, Faculty of Medicine, our University. The patient was provided with complete information about the study objectives, methods, and risk/benefit assessment. A written consent was obtained from the patient upon acceptance to take part in the study. The study was conducted in accordance with the principles of Declaration of Helsinki. Approval for the study was obtained from the IRB committee of our Medical Faculty.
5. Consent for publication
A written consent was obtained from the patient upon acceptance to take part in the study.
6. Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Competing interests
The authors declare that they have no competing interests.
Funding
Non declared.
Authors' contributions
*T A.: contributing to the conception and design, or analyzing and interpreting data;
*T E: drafting the article or revising it critically for important intellectual content; and approving the final version to be published.
*B S.: analyzing and interpreting data;
*M A. and *E A.: performing laboratory analysis supporting the study and collecting data.
Declaration of competing interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Acknowledgements
Not applicable.
References
- Asif N., Iqbal R., Nazir C.F. Human immune system during sleep. Am. J. Clin. Exp. Immunol. 2017;6(6):92–96. [PMC free article] [PubMed] [Google Scholar]
- Besedovsky L., Lange T., Haack M. The sleep-immune crosstalk in health and disease. Physiol. Rev. 2019;99:1325–1380. doi: 10.1152/physrev.00010.2018. Mar 27. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bettis R., Iacuzio D., Jung T. Impact of influenza treatment with oseltamivir on health, sleep and daily activities of otherwise healthy adults and adolescents. Clin. Drug Invest. 2006;26:329–340. doi: 10.2165/00044011-200626060-00004. 2006. [DOI] [PubMed] [Google Scholar]
- Chockalingam A., Hamed S., Goodwin D.G., Rosenzweig B.A., Pang E., BoyneII M.T., Patel V. The effect of oseltamivir on the disease progression of lethal influenza A virus infection: plasma cytokine and miRNA responses in a mouse model. Dis. Markers. 2016:12. doi: 10.1155/2016/9296457. 9296457. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Das G., Mukherjee N., Ghosh S. Neurological insights of COVID-19 pandemic. ACS Chem. Neurosci. 2020;11:1206–1209. doi: 10.1021/acschemneuro.0c00201. [DOI] [PubMed] [Google Scholar]
- Gutiérrez-Ortiz C., Méndez A., Rodrigo-Rey S., Pedro-Murillo E.S., Bermejo-Guerrero L., Gordo-Mañas R., De Aragón-Gómez F., Benito-León J. Miller Fisher Syndrome and polyneuritis cranialis in COVID-19. Neurology. Aug 4, 2020;95:e601–e605. doi: 10.1212/WNL.0000000000009619. April 17. [DOI] [PubMed] [Google Scholar]
- Hossain M.M., Sultana A., Purohit N. Mental health outcomes of quarantine and isolation for infection prevention: a systematic umbrella review of the global evidence. SSRN Elec. J. 2020 doi: 10.4178/epih.e2020038. e2020038 page 1-page 11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ibarra-Coronado E.G., Pantaleón-Martínez A.M., Velazquéz-Moctezuma J., Prospéro-García O., Méndez-Díaz M., Pérez-Tapia M., Pavón L., Morales-Montor J. The bidirectional relationship between sleep and immunity against infections. J. Immunol. Res. Aug 31, 2015;2015 doi: 10.1155/2015/678164. 678164 page 1-page 14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ishaqui A.A., Khan A.H., Sulaiman S.A.S., Alsultan M.T., Khan I., Naqvi A.A. Assessment of efficacy of OseltamivirAzithromycin combination therapy in prevention of Influenza-A (H1N1) pdm09 infection complications and rapidity of symptoms relief. Expet Rev. Respir. Med. 2020;14(5):533–541. doi: 10.1080/17476348.2020.1730180. [DOI] [PubMed] [Google Scholar]
- Lasselin J., Ingreb M., Regenbogenb C., Olssonb M.J., Garkeb M., Bryttinge M., Edgarf R., Lekandera M., Axelssona J. Sleep during naturally occurring respiratory infections: a pilot study. Brain Behav. Immun. 2019;79(2019):236–243. doi: 10.1016/j.bbi.2019.02.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rajkumar R.P. COVID-19 and mental health: a review of the existing literature. Asi. J. Psychiatr. 2020;52 doi: 10.1016/j.ajp.2020.102066. 102066–page 6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sultana A., Sharma R., Hossain M. Burnout among healthcare providers during COVID-19 Pandemic : challenges and evidence-based interventions. SocArXiv Pap. july 4, 2020 doi: 10.31235/osf.io/4hxga. [DOI] [PubMed] [Google Scholar]
- Wan S., Yi Q., Fan S., Lv J., Zhang X., Guo L. Characteristics of lymphocyte subsets and cytokines in peripheral blood of 123 hospitalized patients with 2019 novel coronavirus pneumonia (NCP) medRxiv. 2020, june doi: 10.1101/2020.02.10.20021832. [DOI] [Google Scholar]
- Weinstock L.B., Walters A.S., Paueksakon P. Restless legs syndrome – theoretical roles of inflammatory and immune mechanisms. Sleep Med. Rev. 2011 aug;16(4):341–354. doi: 10.1016/j.smrv.2011.09.003. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.