Learning points for clinicians
This case report highlights that severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can be detected in pleural effusions by RT-PCR. In this case, the SARS-CoV-2-related pneumonia was associated with a lymphocytic, exudative, complicated pleural effusion.
Patient presentation
A 71-year-old African American man presented with a 3-week history of fever, productive cough and progressively worsening shortness of breath to the emergency department. An RT-PCR COVID-19 test (Xpert Xpress SARS-CoV-2, Cepheid, Sunnyvale, CA, USA) was performed via nasopharyngeal swab on arrival to the emergency department, and the patient was found to be positive. The patient had a rapidly deteriorating course with increased work of breathing and oxygen requirement and, therefore, was transferred to the intensive care unit. On presentation to the intensive care unit, his physical exam showed: temperature 102.6°F; heart rate 92 b.p.m.; respiratory rate of 30 breaths per minute; blood pressure 157/95 mmHg; and SpO2 of 95% on 2 l nasal cannula. He was in mild respiratory distress. Chest examination showed decreased breath sounds and dullness to percussion on the posterior aspect of the left chest. Chest X-ray showed a left-sided, alveolar consolidation with air bronchograms consistent with pneumonia and a large left-sided pleural fluid collection concerning for a parapneumonic effusion. The pertinent laboratory tests were as follows: (i) white blood cell count of 10.3 × /µl (4.0–10.5 × /µl); (ii) lactate dehydrogenase 363 U/l (94–200 U/l); (iii) ferritin 343.2 ng/ml (22.9–336.2 ng/ml); (iv) fibrinogen 798 mg/dl (200–393 mg/dl); (v) D-dimer 1144 ng/ml (≤500 ng/ml); and (vi) procalcitonin 0.16 ng/ml (0.00–0.50 ng/ml). Chest computed tomography demonstrated a large left pleural effusion and mediastinal lymphadenopathy.
A therapeutic thoracentesis with ultrasound was performed with complete drainage and removal of 1200 ml of serosanguinous fluid. Pleural fluid culture and cytology were negative. The fluid met criteria for exudative plueral fluid and the total nucleated cell count was 993 (/mm3) with 89% lymphocytes. An RT-PCR (Xpert® Xpress SARS-CoV-2, Cepheid, Sunnyvale, CA, USA) was performed on the pleural fluid and was positive for severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Sputum and blood cultures were negative. He was treated supportively for acute respiratory distress syndrome with high flow nasal cannula, dexamethasone and hydroxychloroquine. There was no reccurrence of the pleural effusion during his hospital course.
Discussion
To our knowledge, this is a novel description of COVID-19 related pleural effusion describing the pleural fluid analysis of virus detection confirmed by RT-PCR and behaving as a complicated parapneumonic effusion. There is a paucity of data describing the pleural complications in relation to the viral infections in general. A prior study by Cohen and Sahn,1 reported an 8% incidence of pleural effusions in patients with acute viral infection, while using lateral decubitus chest X-rays incidence is reported to be 18%. However, the true incidence of viral related pleural effusion may be even higher if pleural ultrasonography is used as a screening tool for pleural fluid presence. In a review by Nestor et al., 2 the pleural fluid analysis in viral related pleural effusion is variable and typically exudative. Pleural fluid appearance can range from serous, serosanguineous, to hemorrhagic.
With respect to the SARS-CoV-2 pneumonia, review of literature reveals the prevalence of pleural effusion can be as high as 14% in patients.3–5 In one of the largest trials, Li et al.3 described intrathoracic lymph node enlargement in 67% of cases and pleural effusion in 14% of cases. Patients with more severe cases have a higher prevalence of both lymphadenopathy and pleural effusions.3–5
Pleural fluid analysis in this case showed an exudative effusion with high lymphocyte count. Even though pleural fluid analysis is rarely diagnostic in isolation, the differential diagnosis of a lymphocytic, exudative pleural effusion is broad and would include viral related pleural effusions. In our case, SARS-CoV-2 RNA was detected using RT-PCR, which is consistent with the diagnosis of a complicated parapneumonic effusion from SARS-CoV-2 related pneumonia.
Conflict of interest. None declared.
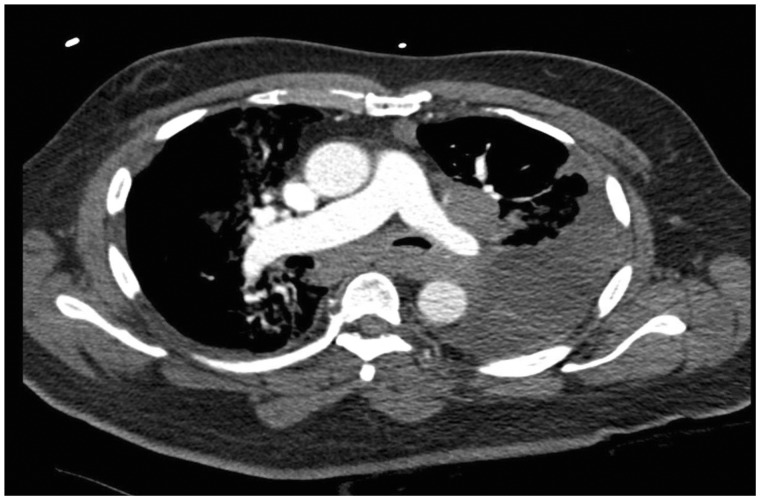
Figure 1.
An axial image of a contrasted chest computed tomography (CT) at the level of the bifurcation of the main pulmonary artery and at the level of the hilum. The chest CT demonstrates a large, left-sided, non-complex pleural effusion. There are pathologically enlarged lymph nodes, defined by >1 cm in short axis, located in the sub-carinal and hilar regions.
References
- 1. Cohen M, Sahn SA. Resolution of pleural effusion. Chest 2001; 119:1547–62. [DOI] [PubMed] [Google Scholar]
- 2. Nestor J, Huggins JT, Kummerfeldt C, DiVietro M, Walters K, Sahn SA. Viral diseases affecting the pleura. J Clin Virol 2013; 58:367–73. [DOI] [PubMed] [Google Scholar]
- 3. Li X, Fang X, Bian Y, Lu J. Comparison of chest CT findings between COVID-19 pneumonia and other types of viral pneumonia: a two-center retrospective study. Eur Radiol 2020;30:5470–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Liu KC, Xu P, Lv WF, Qiu XH, Yao JL, Gu JF, et al. CT manifestations of coronavirus disease-2019: a retrospective analysis of 73 cases by disease severity. Eur Radiol 2020;126:108941. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Li K, Wu J, Wu F, Guo D, Chen L, Fang Z, et al. The clinical and chest CT features associated with severe and critical COVID-19 pneumonia. Invest Radiol 2020;55:327–31. [DOI] [PMC free article] [PubMed] [Google Scholar]