Abstract
Background
The effectiveness of screening for macrosomia is not well established. One of the critical elements of an effective screening program is the diagnostic accuracy of a test at predicting the condition. The objective of this study is to investigate the diagnostic effectiveness of universal ultrasonic fetal biometry in predicting the delivery of a macrosomic infant, shoulder dystocia, and associated neonatal morbidity in low- and mixed-risk populations.
Methods and findings
We conducted a predefined literature search in Medline, Excerpta Medica database (EMBASE), the Cochrane library and ClinicalTrials.gov from inception to May 2020. No language restrictions were applied. We included studies where the ultrasound was performed as part of universal screening and those that included low- and mixed-risk pregnancies and excluded studies confined to high risk pregnancies. We used the estimated fetal weight (EFW) (multiple formulas and thresholds) and the abdominal circumference (AC) to define suspected large for gestational age (LGA). Adverse perinatal outcomes included macrosomia (multiple thresholds), shoulder dystocia, and other markers of neonatal morbidity. The risk of bias was assessed using the Quality Assessment of Diagnostic Accuracy Studies (QUADAS-2) tool. Meta-analysis was carried out using the hierarchical summary receiver operating characteristic (ROC) and the bivariate logit-normal (Reitsma) models. We identified 41 studies that met our inclusion criteria involving 112,034 patients in total. These included 11 prospective cohort studies (N = 9986), one randomized controlled trial (RCT) (N = 367), and 29 retrospective cohort studies (N = 101,681). The quality of the studies was variable, and only three studies blinded the ultrasound findings to the clinicians. Both EFW >4,000 g (or 90th centile for the gestational age) and AC >36 cm (or 90th centile) had >50% sensitivity for predicting macrosomia (birthweight above 4,000 g or 90th centile) at birth with positive likelihood ratios (LRs) of 8.74 (95% confidence interval [CI] 6.84–11.17) and 7.56 (95% CI 5.85–9.77), respectively. There was significant heterogeneity at predicting macrosomia, which could reflect the different study designs, the characteristics of the included populations, and differences in the formulas used. An EFW >4,000 g (or 90th centile) had 22% sensitivity at predicting shoulder dystocia with a positive likelihood ratio of 2.12 (95% CI 1.34–3.35). There was insufficient data to analyze other markers of neonatal morbidity.
Conclusions
In this study, we found that suspected LGA is strongly predictive of the risk of delivering a large infant in low- and mixed-risk populations. However, it is only weakly (albeit statistically significantly) predictive of the risk of shoulder dystocia. There was insufficient data to analyze other markers of neonatal morbidity.
Gordon Smith and colleagues investigate the diagnostic effectiveness of universal ultrasonic fetal biometry in predicting infant macrosomia
Author summary
Why was this study done?
There is a debate regarding introducing universal third-trimester screening for macrosomia. An effective screening program requires two elements: an effective test at predicting a condition and an effective intervention.
There is evidence that early-term induction of labor (IOL) could reduce the rates of shoulder dystocia. However, there is no high-quality evidence regarding the diagnostic effectiveness of fetal biometry at predicting macrosomia and associated morbidity.
What did the researchers do and find?
We searched more than 10,000 titles and identified 41 studies including 112,034 patients that offered third-trimester ultrasounds for the prediction of macrosomia as part of universal ultrasound screening or were done in low- and mixed-risk populations. The quality of the studies was variable, and only three studies blinded the ultrasound findings to the clinicians.
We found that the two most common ultrasound markers, the estimated fetal weight (EFW) and the abdominal circumference (AC), could predict the majority of macrosomic infants at birth (sensitivity >50%) with high diagnostic performance (positive LRs between 7 and 10).
However, the EFW could only predict about 1 in 5 cases of shoulder dystocia (22% sensitivity) with low diagnostic performance (positive likelihood ratio of about 2). There was insufficient data to analyze other markers of neonatal morbidity.
What do these findings mean?
Universal third-trimester ultrasound screening will identify more pregnancies with macrosomia. However, it will not have a clinically significant effect at predicting shoulder dystocia. There is not enough evidence on the effect of ultrasound screening on neonatal morbidity.
We recommend caution prior to introducing universal third-trimester screening for macrosomia, as it would increase the rates of intervention, with potential iatrogenic harm, without clear evidence that it would reduce neonatal morbidity.
Introduction
Macrosomia is usually defined as birthweight >4,000 g or >90th centile for sex and gestational age. Macrosomic birth weight is associated with the risk of adverse outcomes, including perinatal death [1] and injuries related to traumatic delivery [2]. Ultrasonic estimated fetal weight (EFW) was first described in 1975 [3]. The equation for EFW that is in most widespread use was published by Hadlock and colleagues in 1985 [4], and the distribution of EFW in relation to week of gestation was published in 1991 [5]. Hence, the diagnostic tools to identify small for gestational age (SGA) and large for gestational age (LGA) fetuses have been available for many years. One of the main complications associated with macrosomia is shoulder dystocia, and a Cochrane review of four randomized controlled trials (RCTs) including 1,190 women demonstrated that routine induction of labor (IOL) for suspected LGA may prevent this outcome [6]. However, it remains unclear whether screening and intervention for suspected LGA results in better outcomes.
An RCT of IOL in women with an ultrasonically suspected LGA infant is in progress in the United Kingdom (The Big Baby trial, ISRCTN18229892). However, the women recruited to this trial will have been scanned because they were high risk for some reason, as the National Institute for Health and Care Excellence (NICE) has recommended that women should not be routinely scanned in late pregnancy [7]. Although the trial will confirm whether IOL is effective in high-risk women, it will not determine whether screening women without risk factors and intervening results in net benefit. It is often the case that screening and intervention programs that work well in high-risk groups do not work as well in low-risk populations, and one explanation for this can be that the screening test is less informative in low- and mixed-risk populations due to the lower prior risk of disease. In this study, we sought to quantify the diagnostic effectiveness of screening for fetal macrosomia and associated complications using universal ultrasonic fetal biometry in late pregnancy.
Methods
Sources
The protocol for this review was prospectively written and registered with PROSPERO (the International Prospective Register of Systematic Reviews), and the registration number was CRD42017064093. We searched the literature systematically using the Cochrane Database of Systematic Reviews (CDSR), Cochrane Central Register of Controlled Trials (CENTRAL), Medline, EMBASE, and ClinicalTrials.gov from inception to August 2019. An update search was done on May 28, 2020. We applied no restrictions on the language of the report or the location of the study. The studies were identified using a combination of words related to “ultrasound,” “pregnancy,” “estimated fetal weight,” “EFW,” “birthweight,” “macrosomia,” “large for gestational age,” “shoulder dystocia,” and “brachial plexus injury.” The exact search strategy is presented in S1 Text.
Study selection
We set out to include cohort studies where an ultrasound scan was performed ≥24 weeks’ gestation (wkGA), excluding multiple pregnancies. We included studies of low-risk populations, universal screening, and mixed-risk populations (i.e., included both high-risk and low-risk pregnancies). Studies that included only high-risk women, such as patients with preexisting or gestational diabetes, and those in which the ultrasound was performed during labor were excluded. Studies were not selected on the basis of the definition of the index test, i.e., the formula and the threshold used. Finally, we included both blinded and unblinded studies.
Index tests and outcomes
For the purposes of the meta-analysis, we defined suspected LGA as a fetus with an EFW >4,000 g or >90th centile or with an abdominal circumference (AC) >36 cm or >90th centile. However, we have also documented other thresholds used. The outcomes studied included macrosomic birth weight (>4,000 g or >90th centile) and severe macrosomic birth weight (>4,500 g or >97th centile); shoulder dystocia; and perinatal morbidity (neonatal unit admission, 5-minute Apgar score of six or less, metabolic acidosis, neonatal hypoglycaemia, and neonatal jaundice).
Quality assessment
Two authors (AAM and NS) independently performed the literature search, using the software package Review Manager 5.3. Any differences were addressed in consultation with the senior author (GCS). The Quality Assessment of Diagnostic Accuracy Studies (QUADAS 2) tool was used to assess the risk of biases, following the Cochrane Handbook of Diagnostic Test Accuracy Studies [8]. The QUADAS 2 tool was employed to assess potential biases in patient selection, index test, reference standard, and flow and timing. In relation to flow and timing, we assessed the risk from the perspective of universal ultrasound screening near term (i.e., around 36 wkGA). Flow and timing are based on the timing of the ultrasound scan, the timing of delivery, and the length of the interval between scan and delivery. A standardized data extraction form was employed to obtain information on the characteristics of the study (publication year, location, setting, study design, blinding), the participants (inclusion and exclusion rules and number, including inclusion or exclusion of women with diabetes, either preexisting or gestational), the index test (range of wkGA when the scan was conducted, the EFW equation employed, and the threshold for screen positive), reference standard (outcome, wkGA at delivery, and the scan-to-delivery interval).
Data extraction and synthesis
Sensitivity, specificity, positive and negative likelihood ratios (LRs) [9] were calculated from standard two-by-two tables, which had been extracted for each study by tabulating each of the different definitions of screen positive with each of the different outcomes studied. The “hierarchical summary receiver–operating characteristics” (HSROC) model of Rutter and Gatsonis [10] was utilized for data synthesis. This method allows the results of studies to be combined despite variation between studies in the threshold employed for screen positive. The bivariate logit-normal (Reitsma) model [11] was used to calculate average estimates of sensitivity and specificity and respective variances, at a specific threshold, in analyses in which data were available from at least four studies. We also used meta-analysis to obtain a summary of the diagnostic odds ratios (DORs) [12]. Publication bias was assessed using the Deeks’ funnel plot asymmetry test when data was available from a sufficient number of studies. Significant asymmetry was assumed at P < 0.05 [13]. Statistical analyses were performed using STATA version 14 (StataCorp LP, College Station, Texas), specifically, its METANDI, METAN, and MIDAS packages. Analysis and reporting was performed using the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines (S1 PRISMA Checklist) [14].
Results
Study characteristics
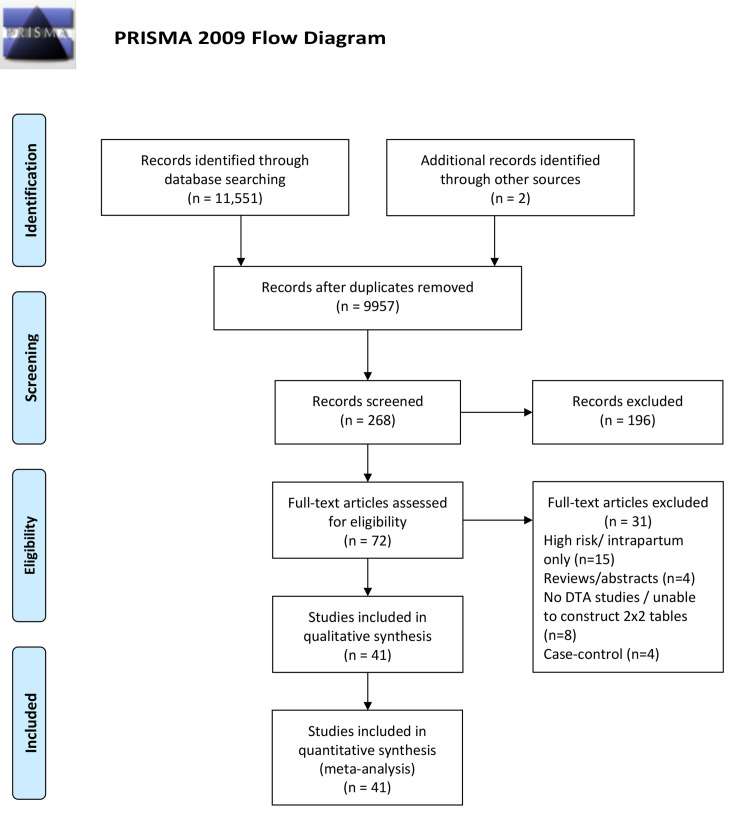
Fig 1 is the literature search PRISMA flowchart. Out of 9,811 unique titles and 72 full paper reviews, we identified 41 studies [15–55] fulfilling the inclusion criteria, including a total of 112,034 participants. The study characteristics are presented in S1 Table. Six studies [18,27,33,36,37,52] (N = 53,935) included unselected pregnancies, nine [23,29,31–33,35,43,45,53,54] (N = 6,436) were confined to low-risk pregnancies, and 26 [15–17, 9–22,24–26,28,30,34,38–42,44,46–51,55] (N = 51,663) recruited pregnancies at mixed risk. The list of the excluded studies and the reasons for the exclusion are presented in S2 Table.
Fig 1. PRISMA flow diagram.
Quality assessment
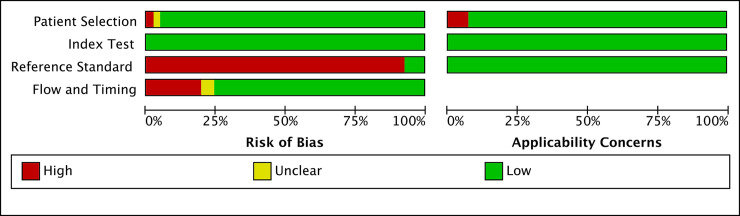
The risk of bias, as assessed by the QUADAS-2 tool, is summarized in Fig 2 and presented in detail in S1 Fig. The Galvin 2017 study [29] was published as an abstract; hence, we used a different study from the same cohort (GENESIS study) [56] to assess the risk of bias. Two of the included studies [51,52] have been authored by some of the coauthors of this paper. We used the same criteria for the quality assessment and analysis. Only three studies—Sovio 2018 [52] (Pregnancy Outcome Prediction study), Galvin 2017 [29] (GENESIS study), and Peregrine 2007 [47]—blinded the results to the clinicians. Hence, the large majority of studies were at risk of bias in relation to the reference standard. The second most common risk of bias was in relation to flow and timing, as six studies [19,24,36,39,47,55] performed the ultrasound either prior to IOL or less than 72 hours before delivery, resulting in a very short interval between the scan and delivery. Conversely, two studies [18,27] had a very long interval (ultrasound <33 wkGA). Two studies [17,20] did not present data on the gestational age at delivery. Finally, three studies [23,48,54] were confined to pregnancies progressing beyond 41 wkGA and were classified as having “high applicability concerns due to patient selection”.
Fig 2. Summary of bias assessment using the QUADAS-2 tool of the studies included in the meta-analysis.
QUADAS 2, Quality Assessment of Diagnostic Accuracy Studies.
Meta-analysis results
Full details of the summary diagnostic performance are presented in Table 1. In summary, both definitions of ultrasonically suspected macrosomia (i.e., either EFW >4,000 g or >90th percentile) had >50% sensitivity for predicting LGA at birth. Many associations were similar regardless of the formula employed, but the positive LRs for the Hadlock formulae (ranging between 7.5 and 12) tended to be higher than for the Shepard formula (around 5). The performance of definitions using just the AC was similar to using an ultrasonic EFW. The sensitivity for predicting severe macrosomia at birth of suspected LGA was around 70%. However, macrosomia (EFW >4,000 g or >90th centile) had a lower (22%) sensitivity for predicting shoulder dystocia, although the association was statistically significant and the positive LR was approximately 2.
Table 1. Summary diagnostic performance of suspected LGA to predict adverse perinatal outcome.
| Diagnostic test | Studies | Patients | Summary sensitivity | Summary specificity | Positive LR (95% CI) |
Negative LR (95% CI) |
|---|---|---|---|---|---|---|
| (95% CI) | (95% CI) | |||||
| Outcome: Birthweight >4,000 g (or 90th centile) | ||||||
| EFW (any) >4,000 g (or 90th centile) | 30 | 80,045 | 53.2% | 93.9% | 8.74 | 0.50 |
| (47.2%–59.1%) | (91.9%–95.5%) | (6.84–11.17) | (0.44–0.56) | |||
| EFW (Hadlock-AC/FL/HC/BPD) | 9 | 22,073 | 63.1% | 94.3% | 11.13 | 0.39 |
| (49.1%–75.2%) | (90.9%–96.5%) | (8.24–15.04) | (0.28–0.55) | |||
| EFW (Hadlock- AC/FL/BPD) | 10 | 17,110 | 55.1% | 92.9% | 7.77 | 0.48 |
| (44.1%–65.7%) | (89.7%–95.2%) | (5.55–10.89) | (0.38–0.61) | |||
| EFW (Hadlock- AC/FL/HC) | 7 | 60,648 | 55.2% | 94.9% | 11.84 | 0.47 |
| (45.7%–64.2%) | (92.4%–96.6%) | (7.46–15.74) | (0.39–0.58) | |||
| EFW (Hadlock- AC/FL) | 9 | 16,736 | 60.5% | 92.0% | 7.54 | 0.43 |
| (50.7%–69.5%) | (89.4%–93.7%) | (6.13–9.29) | (0.34–0.54) | |||
| EFW (Hadlock- AC/BPD) | 6 | 13,617 | 62.9% | 93.7% | 9.99 | 0.40 |
| (36.1%–83.5%) | (85.9%–97.3%) | (6.40–15.58) | (0.21–0.75) | |||
| EFW (Shepard) | 7 | 14,060 | 73.7% | 85.1% | 4.96 | 0.31 |
| (54.4%–86.9%) | (76.5%–90.9%) | (3.29–7.48) | (0.17–0.56) | |||
| AC >36cm (or 90th centile) | 5 | 10,543 | 57.8% | 92.3% | 7.56 | 0.46 |
| (39.6%–74.2%) | (88.7%–94.9%) | (5.85–9.77) | (0.30–0.68) | |||
| Outcome: Birthweight >4,500 g (or 97th centile) | ||||||
| EFW (any) >4,000 g (or 90th centile) | 5 | 51,686 | 67.5% | 89.7% | 6.58 | 0.36 |
| (47.8%–82.6%) | (79.1%–95.3%) | (2.78–15.58) | (0.20–0.65) | |||
| Outcome: Shoulder dystocia | ||||||
| EFW (any) >4,000 g (or 90th centile) | 6 | 26,264 | 22.0% | 89.6% | 2.12 | 0.87 |
| (9.9%–42.0%) | (80.8%–94.6%) | (1.34–3.35) | (0.74–1.02) |
Abbreviations: AC, abdominal circumference; BPD, Biparietal diameter; CI, confidence interval; EFW, estimated fetal weight; FL, femur length; HC, head circumference; LR, likelihood ratio
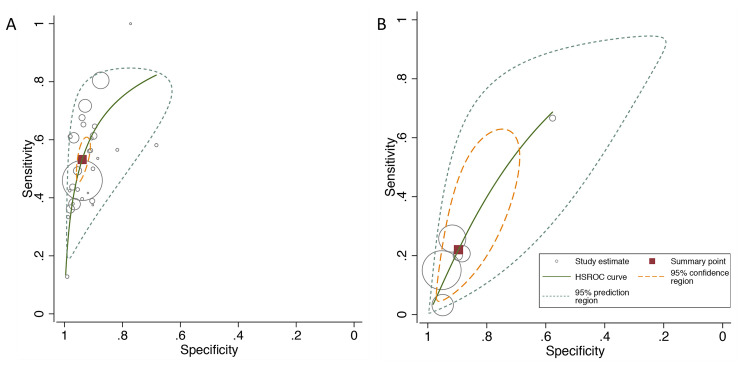
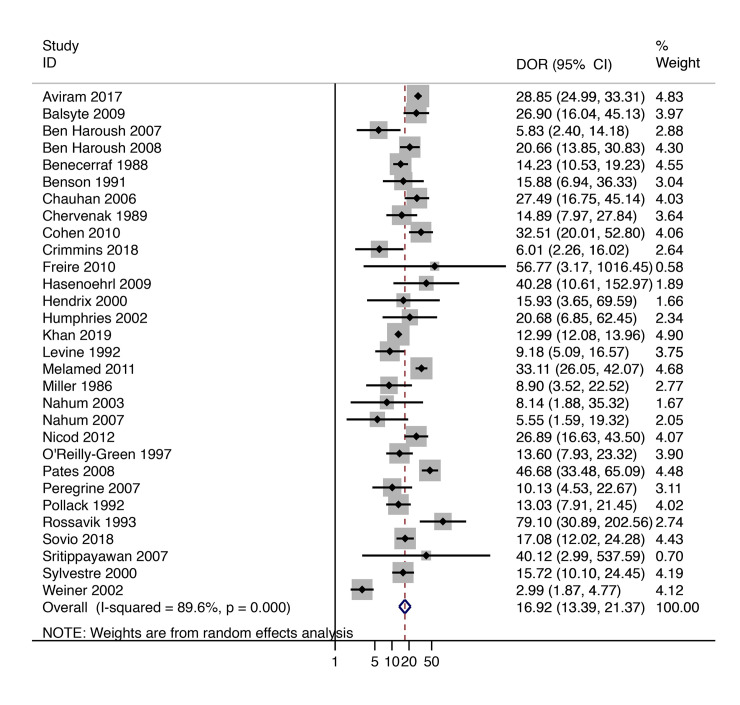
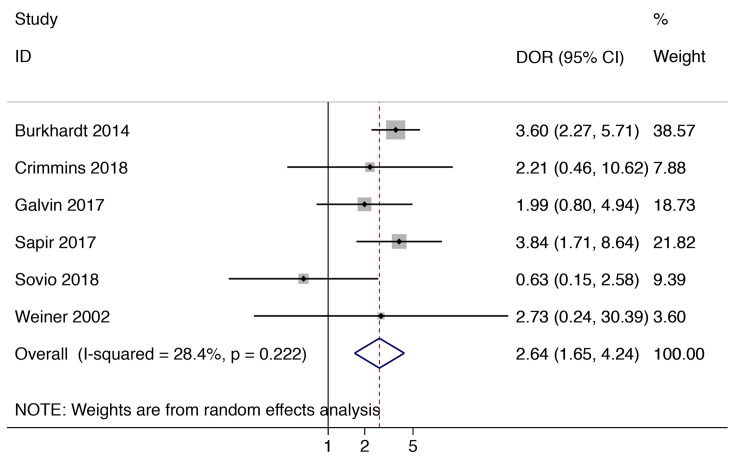
Fig 3 has summary ROC curves for shoulder dystocia and macrosomia. For the prediction of macrosomia at birth, most of the large studies were close to the point estimate, and only a few small studies were outside the prediction intervals. For shoulder dystocia, most studies reported sensitivities below 30%, and only one study [55] reported a sensitivity of >50%. However, in this study, the total number of shoulder dystocia cases was very small (n = 3). Fig 4 and Fig 5 present graphs of the pooling of DORs for macrosomia and shoulder dystocia, respectively. There was significant heterogeneity for the prediction of macrosomia but not for the prediction of shoulder dystocia.
Fig 3.
Summary ROC curves for the diagnostic performance of EFW >4,000 g (or 90th centile) at predicting (A) macrosomia at birth (birthweight above 4,000 g or above the 90th centile) and (B) shoulder dystocia. EFW, estimated fetal weight.
Fig 4. Diagnostic performance of EFW >4,000 g (or 90th centile) at predicting macrosomia at birth (birthweight above 4,000 g or above the 90th centile).
EFW, estimated fetal weight.
Fig 5. Diagnostic performance of EFW >4,000 g (or 90th centile) at predicting shoulder dystocia.
EFW, estimated fetal weight.
Only three studies—Crimmins 2018 [25], Galvin 2017 [29], and Sovio 2018 [52]—reported neonatal unit admission as an outcome, and a meta-analysis was not feasible. However, none of the studies reported statistically significant results with positive LRs of 0.73 (95% confidence interval [CI] 0.36–1.48), 1.39 (95% CI 0.97–2.00), and 1.33 (95% CI 0.80–2.22), respectively. Only the Sovio 2018 [52] study reported on 5-minute Apgar score of less than 7 and neonatal metabolic acidosis with positive LRs of 1.94 (95% CI 0.66–5.75) and 1.08 (95% CI 0.28–4.18), respectively. Moreover, the Sovio 2018 study was the only one that reported on neonatal hypoglycaemia and neonatal jaundice with positive LRs of 1.9 (95% CI 1.1–3.4) and 1.2 (95% CI 0.6–2.4), respectively.
The analysis demonstrated no significant evidence of publication bias (P = 0.57) when evaluated using Deeks’ funnel plot asymmetry test (S2 Fig).
Discussion
The main conclusion of this analysis is that an ultrasonic EFW indicating an increased risk of a large baby was strongly associated with delivering a macrosomic infant, but it was only weakly associated with the risk of shoulder dystocia. When the EFW was calculated using the widely employed Hadlock method, the positive LRs for macrosomia were in the region of 7 to 12, whereas they were approximately 2 in relation to the risk of shoulder dystocia.
This is the largest systematic review on the prediction of macrosomia and the only study that was focused on low- and mixed-risk populations from the perspective of using third-trimester ultrasound as routine screening in all pregnancies. We reported on multiple ultrasound markers and formulas. Moreover, we also reported on the prediction of shoulder dystocia, which is a major perinatal complication, the prevention of which would be a major aim of the routine ultrasound screening. The main limitation of this study is that there was significant heterogeneity between the studies in the ability to predict a macrosomic infant, as the forest plot of DORs indicates. The source of this heterogeneity is unclear, but it could relate to differences in the quality of the performance of the diagnostic test, such as the quality of the imaging equipment, the skill and training of sonographers, and the characteristics of the population. Finally, despite the large amount of studies included, only three studies [25, 29, 52] reported any outcomes of neonatal morbidity, and a meta-analysis was not feasible.
In the current study, we incorporated previously published data from the POP study (Sovio 2018) [52], which included nulliparous women who had a research scan at 36 wkGA, which was blinded in most cases to the clinicians. We found that the DOR (95% CI) from the POP study was very similar to the summary DOR derived from all of the other studies, which suggests that the results from the POP study are likely to be generalizable. The POP study was one of only a few identified that blinded the ultrasound result. Another blinded study, conducted in seven centers across Ireland between 2012 and 2015, the GENESIS study (Galvin 2017) [29], was a prospective cohort study of 2,772 nulliparous pregnant women. The results of the GENESIS study have only been published in conference proceedings [29] and include the outcome of shoulder dystocia but not macrosomia. Interestingly, neither the POP study nor the GENESIS study observed a statistically significant association between ultrasonic LGA and shoulder dystocia. When blinded and unblinded studies were combined, the meta-analysis demonstrated that ultrasound may be predictive of shoulder dystocia, albeit weakly. However, the associations observed in the other studies may be due to ascertainment bias. Specifically, if the fetus is suspected to be large on the basis of the EFW, the staff attending the delivery may have a lower threshold for using maneuvers for shoulder dystocia in the event of any delay. They may also be more likely to document a given delay as being due to shoulder dystocia. Hence, unblinded studies could result in stronger associations with shoulder dystocia through ascertainment bias. The fact that ultrasonic EFW is relatively poor as a predictor of shoulder dystocia is not unexpected, given that the actual birth weight of the baby is also not strongly predictive of the outcome: the majority of cases of shoulder dystocia involve a normal birth weight infant [57].
Finally, ultrasonic suspicion of a large baby is a clinical situation where there is evidence that knowledge of the scan result may itself cause complications. Multiple studies have demonstrated that women who have a false positive diagnosis of fetal macrosomia based on EFW are more likely to be delivered by emergency caesarean section [58,59]. This finding underlines the potential for harm caused by screening low-risk women. Research studies in which the results of the scan are revealed could lead to associations with adverse outcomes that were caused by an iatrogenic harm from a false positive result. Conversely, analysis of studies in which the scan was revealed may fail to show true associations with adverse outcome as knowledge of the scan result led to interventions that mitigated the risk.
We conclude that ultrasonically suspected LGA in the general population has quite good diagnostic effectiveness for macrosomic birth weight. However, it is not strongly predictive of the risk of associated complications, such as shoulder dystocia. Similar observations have been made in relation to ultrasonically suspected SGA [60, 61]. That study indicated that reduced fetal abdominal growth velocity helped discriminate between healthy SGA babies and those that were at increased risk of complications. Interestingly, the analogous finding is also true in LGA babies, in whom the combination of LGA and accelerated abdominal growth velocity was associated with the risk of neonatal morbidity [52]. We believe that future studies should address the other factors which help differentiate those suspected LGA fetuses which are at the greatest risk of complications.
Supporting information
(DOC)
(DOCX)
(DOCX)
(DOCX)
QUADAS 2, Quality Assessment of Diagnostic Accuracy Studies
(TIFF)
(TIFF)
Acknowledgments
The views expressed here are those of the authors and not necessarily those of the NHS, the NIHR, or the Department of Health.
Abbreviations
- AC
abdominal circumference
- BPD
Biparietal diameter
- CDSR
Cochrane Database of Systematic Reviews
- CENTRAL
Cochrane Central Register of Controlled Trials
- CI
confidence interval
- DOR
diagnostic odds ratio
- EFW
estimated fetal weight
- EMBASE
Excerpta Medica database
- FL
femur length
- HC
head circumference
- HSROC
hierarchical summary receiver–operating characteristics
- IOL
induction of labor
- LGA
large for gestational age
- LR
likelihood ratio
- NICE
National Institute for Health and Care Excellence
- PRISMA
Preferred Reporting Items for Systematic Reviews and Meta-Analyses
- QUADAS 2
Quality Assessment of Diagnostic Accuracy Studies
- RCT
randomized controlled trial
- ROC
receiver operating characteristic
- SGA
small for gestational age
- wkGA
weeks’ gestation
Data Availability
All relevant data are within the manuscript and its Supporting Information files. All the studies included in the meta-analysis are publicly available.
Funding Statement
This study was funded by the National Institute for Health Research (NIHR) Health Technology Assessment programme, grant number 15/105/01. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
References
- 1.Moraitis AA, Wood AM, Fleming M, Smith GC. Birth weight percentile and the risk of term perinatal death. Obstetrics and gynecology. 2014;124(2 Pt 1):274–83. Epub 2014/07/09. 10.1097/aog.0000000000000388 . [DOI] [PubMed] [Google Scholar]
- 2.Esakoff TF, Cheng YW, Sparks TN, Caughey AB. The association between birthweight 4000 g or greater and perinatal outcomes in patients with and without gestational diabetes mellitus. American journal of obstetrics and gynecology. 2009;200(6):672.e1–4. Epub 2009/04/21. 10.1016/j.ajog.2009.02.035 . [DOI] [PubMed] [Google Scholar]
- 3.Campbell S, Wilkin D. Ultrasonic measurement of fetal abdomen circumference in the estimation of fetal weight. British journal of obstetrics and gynaecology. 1975;82(9):689–97. Epub 1975/09/01. 10.1111/j.1471-0528.1975.tb00708.x . [DOI] [PubMed] [Google Scholar]
- 4.Hadlock FP, Harrist RB, Sharman RS, Deter RL, Park SK. Estimation of fetal weight with the use of head, body, and femur measurements—a prospective study. American journal of obstetrics and gynecology. 1985;151(3):333–7. Epub 1985/02/01. 10.1016/0002-9378(85)90298-4 . [DOI] [PubMed] [Google Scholar]
- 5.Hadlock FP, Harrist RB, Martinez-Poyer J. In utero analysis of fetal growth: a sonographic weight standard. Radiology. 1991;181(1):129–33. Epub 1991/10/01. 10.1148/radiology.181.1.1887021 . [DOI] [PubMed] [Google Scholar]
- 6.Boulvain M, Irion O, Dowswell T, Thornton JG. Induction of labour at or near term for suspected fetal macrosomia. Cochrane Database Syst Rev. 2016;(5):Cd000938 Epub 2016/05/23. 10.1002/14651858.CD000938.pub2 . [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.National Collaborating Centre for Ws, Children's H. National Institute for Health and Clinical Excellence: Guidance. Antenatal Care: Routine Care for the Healthy Pregnant Woman. London: RCOG Press National Collaborating Centre for Women's and Children's Health; 2008. [Google Scholar]
- 8.Whiting PF, Rutjes AW, Westwood ME, Mallett S, Deeks JJ, Reitsma JB, et al. QUADAS-2: a revised tool for the quality assessment of diagnostic accuracy studies. Annals of internal medicine. 2011;155(8):529–36. Epub 2011/10/19. 10.7326/0003-4819-155-8-201110180-00009 . [DOI] [PubMed] [Google Scholar]
- 9.Simel DL, Samsa GP, Matchar DB. Likelihood ratios with confidence: sample size estimation for diagnostic test studies. J Clin Epidemiol. 1991;44(8):763–70. Epub 1991/01/01. 10.1016/0895-4356(91)90128-v . [DOI] [PubMed] [Google Scholar]
- 10.Rutter CM, Gatsonis CA. A hierarchical regression approach to meta-analysis of diagnostic test accuracy evaluations. Statistics in medicine. 2001;20(19):2865–84. Epub 2001/09/25. 10.1002/sim.942 . [DOI] [PubMed] [Google Scholar]
- 11.Reitsma JB, Glas AS, Rutjes AW, Scholten RJ, Bossuyt PM, Zwinderman AH. Bivariate analysis of sensitivity and specificity produces informative summary measures in diagnostic reviews. J Clin Epidemiol. 2005;58(10):982–90. Epub 2005/09/20. 10.1016/j.jclinepi.2005.02.022 . [DOI] [PubMed] [Google Scholar]
- 12.Deeks JJ. Systematic reviews in health care: Systematic reviews of evaluations of diagnostic and screening tests. BMJ (Clinical research ed). 2001;323(7305):157–62. Epub 2001/07/21. 10.1136/bmj.323.7305.157 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Deeks JJ, Macaskill P, Irwig L. The performance of tests of publication bias and other sample size effects in systematic reviews of diagnostic test accuracy was assessed. J Clin Epidemiol. 2005;58(9):882–93. Epub 2005/08/09. 10.1016/j.jclinepi.2005.01.016 . [DOI] [PubMed] [Google Scholar]
- 14.Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7):e1000097 Epub 2009/07/22. 10.1371/journal.pmed.1000097 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Aviram A, Yogev Y, Ashwal E, Hiersch L, Hadar E, Gabbay-Benziv R. Prediction of large for gestational age by various sonographic fetal weight estimation formulas-which should we use? Journal of Perinatology. 2017;37(5):513–7. 10.1038/jp.2017.5 . [DOI] [PubMed] [Google Scholar]
- 16.Balsyte D, Schaffer L, Burkhardt T, Wisser J, Kurmanavicius J. Sonographic prediction of macrosomia cannot be improved by combination with pregnancy-specific characteristics. Ultrasound in Obstetrics & Gynecology. 2009;33(4):453–8. 10.1002/uog.6282 . [DOI] [PubMed] [Google Scholar]
- 17.Benacerraf BR, Gelman R, Frigoletto FD Jr. Sonographically estimated fetal weight: Accuracy and limitation. American Journal of Obstetrics and Gynecology. 1988;159(5):1118–21. 10.1016/0002-9378(88)90425-5 . [DOI] [PubMed] [Google Scholar]
- 18.Ben-Haroush A, Yogev Y, Hod M, Bar J. Predictive value of a single early fetal weight estimate in normal pregnancies. European Journal of Obstetrics Gynecology and Reproductive Biology. 2007;130(2):187–92. . [DOI] [PubMed] [Google Scholar]
- 19.Ben-Haroush A, Melamed N, Mashiach R, Meizner I, Yogev Y. Use of the amniotic fluid index combined with estimated fetal weight within 10 days of delivery for prediction of macrosomia at birth. Journal of Ultrasound in Medicine. 2008;27(7):1029–32. 10.7863/jum.2008.27.7.1029 . [DOI] [PubMed] [Google Scholar]
- 20.Benson CB, Coughlin BF, Doubilet PM. Amniotic fluid volume in large-for-gestational-age fetuses of nondiabetic mothers. Journal of Ultrasound in Medicine. 1991;10(3):149–51. 10.7863/jum.1991.10.3.149 . [DOI] [PubMed] [Google Scholar]
- 21.Burkhardt T, Schmidt M, Kurmanavicius J, Zimmermann R, Schaffer L. Evaluation of fetal anthropometric measures to predict the risk for shoulder dystocia. Ultrasound in obstetrics & gynecology: the official journal of the International Society of Ultrasound in Obstetrics and Gynecology. 2014;43(1):77–82. . [DOI] [PubMed] [Google Scholar]
- 22.Chauhan SP, Parker D, Shields D, Sanderson M, Cole JH, Scardo JA. Sonographic estimate of birth weight among high-risk patients: feasibility and factors influencing accuracy. American journal of obstetrics and gynecology. 2006;195(2):601–6. Epub 2006/06/27. 10.1016/j.ajog.2006.04.012 . [DOI] [PubMed] [Google Scholar]
- 23.Chervenak JL, Divon MY, Hirsch J, Girz BA, Langer O. Macrosomia in the postdate pregnancy: Is routine ultrasonographic screening indicated? American Journal of Obstetrics and Gynecology. 1989;161(3):753–6. 10.1016/0002-9378(89)90395-5 . [DOI] [PubMed] [Google Scholar]
- 24.Cohen JM, Hutcheon JA, Kramer MS, Joseph KS, Abenhaim H, Platt RW. Influence of ultrasound-to-delivery interval and maternal-fetal characteristics on validity of estimated fetal weight. Ultrasound in obstetrics & gynecology: the official journal of the International Society of Ultrasound in Obstetrics and Gynecology. 2010;35(4):434–41. . [DOI] [PubMed] [Google Scholar]
- 25.Crimmins S, Mo C, Nassar Y, Kopelman JN, Turan OM. Polyhydramnios or Excessive Fetal Growth Are Markers for Abnormal Perinatal Outcome in Euglycemic Pregnancies. American Journal of Perinatology. 2018;35(2):140–5. 10.1055/s-0037-1606186 . [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Cromi A, Ghezzi F, Di Naro E, Siesto G, Bergamini V, Raio L. Large cross-sectional area of the umbilical cord as a predictor of fetal macrosomia. Ultrasound in Obstetrics & Gynecology. 2007;30(6):861–6. 10.1002/uog.5183 . [DOI] [PubMed] [Google Scholar]
- 27.De Reu PAOM, Smits LJM, Oosterbaan HP, Nijhuis JG. Value of a single early third trimester fetal biometry for the prediction of birth weight deviations in a low risk population. Journal of Perinatal Medicine. 2008;36(4):324–9. 10.1515/JPM.2008.057 [DOI] [PubMed] [Google Scholar]
- 28.Freire DMC, Cecatti JG, Paiva CSM. Correlation between estimated fetal weight by ultrasound and neonatal weight. [Portuguese]. Revista Brasileira de Ginecologia e Obstetricia. 2010;32(1):4–10. 10.1590/s0100-72032010000100002 . [DOI] [PubMed] [Google Scholar]
- 29.Galvin DM, Burke N, Burke G, Breathnach F, McAuliffe F, Morrison J, et al. 94: Accuracy of prenatal detection of macrosomia >4,000g and outcomes in the absence of intervention: results of the prospective multicenter genesis study. American Journal of Obstetrics and Gynecology. 2017;216(1, Supplement):S68 10.1016/j.ajog.2016.11.983. [DOI] [Google Scholar]
- 30.Gilby JR, Williams MC, Spellacy WN. Fetal abdominal circumference measurements of 35 and 38 cm as predictors of macrosomia. A risk factor for shoulder dystocia. Journal of Reproductive Medicine. 2000;45(11):936–8. . [PubMed] [Google Scholar]
- 31.Hasenoehrl G, Pohlhammer A, Gruber R, Staudach A, Steiner H. Fetal weight estimation by 2D and 3D ultrasound: Comparison of six formulas. Ultraschall in der Medizin. 2009;30(6):585–90. 10.1055/s-0028-1109185 . [DOI] [PubMed] [Google Scholar]
- 32.Hendrix NW, Grady CS, Chauhan SP. Clinical vs. sonographic estimate of birth weight in term parturients. A randomized clinical trial. Journal of Reproductive Medicine. 2000;45(4):317–22. . [PubMed] [Google Scholar]
- 33.Henrichs C, Magann EF, Brantley KL, Crews JH, Sanderson M, Chauhan SP. Detecting fetal macrosomia with abdominal circumference alone. Journal of Reproductive Medicine. 2003;48(5):339–42. . [PubMed] [Google Scholar]
- 34.Humphries J, Reynolds D, Bell-Scarbrough L, Lynn N, Scardo JA, Chauhan SP. Sonographic estimate of birth weight: relative accuracy of sonographers versus maternal-fetal medicine specialists. Journal of Maternal-Fetal & Neonatal Medicine. 2002;11(2):108–12. 10.1080/jmf.11.2.108.112 . [DOI] [PubMed] [Google Scholar]
- 35.Kayem G, Grange G, Breart G, Goffinet F. Comparison of fundal height measurement and sonographically measured fetal abdominal circumference in the prediction of high and low birth weight at term. Ultrasound in obstetrics & gynecology: the official journal of the International Society of Ultrasound in Obstetrics and Gynecology. 2009;34(5):566–71. Epub 2009/07/08. 10.1002/uog.6378 . [DOI] [PubMed] [Google Scholar]
- 36.Kehl S, Brade J, Schmidt U, Berlit S, Bohlmann MK, Sutterlin M, et al. Role of fetal abdominal circumference as a prognostic parameter of perinatal complications. Archives of Gynecology & Obstetrics. 2011;284(6):1345–9. 10.1007/s00404-011-1888-8 . [DOI] [PubMed] [Google Scholar]
- 37.Khan N, Ciobanu A, Karampitsakos T, Akolekar R, Nicolaides KH. Prediction of large for gestational age neonates by routine third trimester ultrasound. Ultrasound in obstetrics & gynecology: the official journal of the International Society of Ultrasound in Obstetrics and Gynecology. 2019;25 . [DOI] [PubMed] [Google Scholar]
- 38.Levine AB, Lockwood CJ, Brown B, Lapinski R, Berkowitz RL. Sonographic diagnosis of the large for gestational age fetus at term: does it make a difference? Obstetrics & Gynecology. 1992;79(1):55–8. . [PubMed] [Google Scholar]
- 39.Melamed N, Yogev Y, Meizner I, Mashiach R, Pardo J, Ben-Haroush A. Prediction of fetal macrosomia: effect of sonographic fetal weight-estimation model and threshold used. Ultrasound in obstetrics & gynecology: the official journal of the International Society of Ultrasound in Obstetrics and Gynecology. 2011;38(1):74–81. . [DOI] [PubMed] [Google Scholar]
- 40.Miller JM Jr., Korndorffer FA 3rd, Gabert HA. Fetal weight estimates in late pregnancy with emphasis on macrosomia. Journal of Clinical Ultrasound. 1986;14(6):437–42. 10.1002/jcu.1870140606 . [DOI] [PubMed] [Google Scholar]
- 41.Miller JM Jr, Brown HL, Khawli OF, Pastorek IJG, Gabert HA. Ultrasonographic identification of the macrosomic fetus. American Journal of Obstetrics and Gynecology. 1988;159(5):1110–4. 10.1016/0002-9378(88)90423-1 . [DOI] [PubMed] [Google Scholar]
- 42.Nahum GG, Pham KQ, McHugh JP. Ultrasonic prediction of term birth weight in Hispanic women. Accuracy in an outpatient clinic. Journal of Reproductive Medicine. 2003;48(1):13–22. . [PubMed] [Google Scholar]
- 43.Nahum GG, Stanislaw H. A computerized method for accurately predicting fetal macrosomia up to 11 weeks before delivery. European Journal of Obstetrics, Gynecology, & Reproductive Biology. 2007;133(2):148–56. 10.1016/j.ejogrb.2006.08.011 . [DOI] [PubMed] [Google Scholar]
- 44.Nicod AC, Hohlfeld P, Vial Y. Performance of ultrasound estimation of fetal weight in fetuses weighing < = 2000 g and more than 4000 g. [French]. Revue Medicale Suisse. 2012;8(359):2022–7. . [PubMed] [Google Scholar]
- 45.O'Reilly-Green CP, Divon MY. Receiver operating characteristic curves of sonographic estimated fetal weight for prediction of macrosomia in prolonged pregnancies. Ultrasound in obstetrics & gynecology: the official journal of the International Society of Ultrasound in Obstetrics and Gynecology. 1997;9(6):403–8. Epub 1997/06/01. 10.1046/j.1469-0705.1997.09060403.x . [DOI] [PubMed] [Google Scholar]
- 46.Pates JA, McIntire DD, Casey BM, Leveno KJ. Predicting macrosomia. Journal of Ultrasound in Medicine. 2008;27(1):39–43. 10.7863/jum.2008.27.1.39 . [DOI] [PubMed] [Google Scholar]
- 47.Peregrine E, O'Brien P, Jauniaux E. Clinical and ultrasound estimation of birth weight prior to induction of labor at term. Ultrasound in Obstetrics & Gynecology. 2007;29(3):304–9. 10.1002/uog.3949 . [DOI] [PubMed] [Google Scholar]
- 48.Pollack RN, Hauer-Pollack G, Divon MY. Macrosomia in postdates pregnancies: the accuracy of routine ultrasonographic screening. American Journal of Obstetrics & Gynecology. 1992;167(1):7–11. 10.1016/s0002-9378(11)91615-9 . [DOI] [PubMed] [Google Scholar]
- 49.Rossavik IK, Joslin GL. Macrosomatia and ultrasonography: what is the problem? Southern Medical Journal. 1993;86(10):1129–32. 10.1097/00007611-199310000-00010 . [DOI] [PubMed] [Google Scholar]
- 50.Sapir A, Khayyat I, Drukker L, Rabinowitz R, Samueloff A, Sela HY. Ultrasound predication of shoulder dystocia in low risk term singleton deliveries. American Journal of Obstetrics and Gynecology. 2017;216 (1 Supplement 1):S221 . [Google Scholar]
- 51.Smith GC, Smith MF, McNay MB, Fleming JE. The relation between fetal abdominal circumference and birthweight: findings in 3512 pregnancies. British journal of obstetrics and gynaecology. 1997;104(2):186–90. Epub 1997/02/01. 10.1111/j.1471-0528.1997.tb11042.x . [DOI] [PubMed] [Google Scholar]
- 52.Sovio U, Moraitis AA, Wong HS, Smith GCS. Universal vs selective ultrasonography to screen for large-for-gestational-age infants and associated morbidity. Ultrasound in obstetrics & gynecology: the official journal of the International Society of Ultrasound in Obstetrics and Gynecology. 2018;51(6):783–91. Epub 2017/04/21. 10.1002/uog.17491 . [DOI] [PubMed] [Google Scholar]
- 53.Sritippayawan S, Anansakunwat W, Suthantikorn C. The accuracy of gestation-adjusted projection method in estimating birth weight by sonographic fetal measurements in the third trimester. Journal of the Medical Association of Thailand. 2007;90(6):1058–67. . [PubMed] [Google Scholar]
- 54.Sylvestre G, Divon MY, Onyeije C, Fisher M. Diagnosis of macrosomia in the postdates population: combining sonographic estimates of fetal weight with glucose challenge testing. Journal of Maternal-Fetal Medicine. 2000;9(5):287–90. 10.1002/1520-6661(200009/10)9:5<287::AID-MFM6>3.0.CO;2-1 . [DOI] [PubMed] [Google Scholar]
- 55.Weiner Z, Ben-Shlomo I, Beck-Fruchter R, Goldberg Y, Shalev E. Clinical and ultrasonographic weight estimation in large for gestational age fetus. European Journal of Obstetrics, Gynecology, & Reproductive Biology. 2002;105(1):20–4. 10.1016/s0301-2115(02)00140-9 . [DOI] [PubMed] [Google Scholar]
- 56.Burke N, Burke G, Breathnach F, McAuliffe F, Morrison JJ, Turner M, et al. Prediction of cesarean delivery in the term nulliparous woman: results from the prospective, multicenter Genesis study. American journal of obstetrics and gynecology. 2017;216(6):598.e1–.e11. Epub 2017/02/19. 10.1016/j.ajog.2017.02.017 . [DOI] [PubMed] [Google Scholar]
- 57.Ouzounian JG. Shoulder Dystocia: Incidence and Risk Factors. Clin Obstet Gynecol. 2016;59(4):791–4. Epub 2016/10/21. 10.1097/GRF.0000000000000227 . [DOI] [PubMed] [Google Scholar]
- 58.Little SE, Edlow AG, Thomas AM, Smith NA. Estimated fetal weight by ultrasound: a modifiable risk factor for cesarean delivery? American journal of obstetrics and gynecology. 2012;207(4):309.e1–6. Epub 2012/08/21. 10.1016/j.ajog.2012.06.065 . [DOI] [PubMed] [Google Scholar]
- 59.Blackwell SC, Refuerzo J, Chadha R, Carreno CA. Overestimation of fetal weight by ultrasound: does it influence the likelihood of cesarean delivery for labor arrest? American journal of obstetrics and gynecology. 2009;200(3):340.e1–3. Epub 2009/03/04. 10.1016/j.ajog.2008.12.043 . [DOI] [PubMed] [Google Scholar]
- 60.Sovio U, White IR, Dacey A, Pasupathy D, Smith GCS. Screening for fetal growth restriction with universal third trimester ultrasonography in nulliparous women in the Pregnancy Outcome Prediction (POP) study: a prospective cohort study. Lancet (London, England). 2015;386(10008):2089–97. Epub 2015/09/12. 10.1016/s0140-6736(15)00131-2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Heazell AE, Hayes DJ, Whitworth M, Takwoingi Y, Bayliss SE, Davenport C. Biochemical tests of placental function versus ultrasound assessment of fetal size for stillbirth and small-for-gestational-age infants. Cochrane Database Syst Rev. 2019;5:Cd012245 Epub 2019/05/16. 10.1002/14651858.CD012245.pub2 [DOI] [PMC free article] [PubMed] [Google Scholar]