Abstract
Background
This randomized control study was designed to compare the clinical and radiological outcomes, including periprosthetic bone mineral density (BMD) changes, between the short and standard stems after using cementless hemiarthroplasty in elderly patients with femur neck fractures.
Materials and Methods
From January 2013 to May 2017, 151 patients (aged ≥ 65 years) underwent hemiarthroplasties due to femoral neck fractures. Patients were randomized into two groups; 77 patients in Group A implanting the short femoral stem and 74 patients in Group B implanting the standard femoral stem. Clinical and radiographic evaluations were performed in all patients.
Results
75 patients (40 patients in Group A and 35 patients in Group B) completed routine follow-up for a minimum of 2 years. The clinical outcomes, including ambulatory functions and thigh pain, were similar in both groups. All the femoral stems acquired radiologic stability. At postoperative one year, BMD values in Gruen zone (G) seven on the standard stem side were significantly lower than those on the short stem side (P = 0.038). At the second year of follow-up, the BMD values of Group A in G1, G3, G4, and G7 were significantly greater than those of Group B (P = 0.007, 0.032, 0.026, and P < 0.000, respectively).
Conclusions
Both the clinical outcomes and radiologic stability in both group demonstrated similar results in elderly patients with femoral neck fracture at the latest follow-up. In addition, the periprosthetic BMD of the short femoral stems demonstrated better periprosthetic bone preservation at a minimum of 2 years of follow-up.
Level of Evidences
Therapeutic Level II.
Keywords: Hemiarthroplasty, Short stem, Elderly, Femoral neck fracture, Periprosthetic bone preservation
Introduction
In elderly patients with femoral neck fracture, arthroplasty has been considered the better treatment option than internal fixation [1]. Although the clinical outcomes of total hip arthroplasty (THA) in elderly patients with femoral neck fracture were reported to be better than hemiarthroplasty, hemiarthroplasty was frequently recommended in cases where the patient has a low functional level and/or osteoporosis and high rates of postoperative dislocation of total hip arthroplasty [2]. Recently, the use of cementless hemiarthroplasties in elderly patients with femur neck fractures has increased [3]. Moreover, the clinical results of cementless stem procedures have been reported to be comparable with those of cemented stems for femoral neck fracture [4].
The standard cementless femoral stems in hip arthroplasty have excellent outcomes, and the survivorship ranges from 94 to 100% at up to 20 years’ follow-up. However, the disadvantages of cementless femoral stems include proximal–distal mismatch, non-ideal load transfer, bone loss, thigh pain, and periprosthetic fracture.
To overcome complications of standard femoral stems, shorter femoral stems have been increasingly utilized since 1989 [5, 6]. Theoretically, the short stem could preserve more of the native host bone around the prostheses than the standard femoral stem. Although there are numerous studies comparing the short stem and standard stem in THA [7–9], no study has compared the clinical and radiological outcomes between the standard and shorter stems using cementless hemiarthroplasty in elderly patients with femoral neck fractures.
Thus, this randomized control study was designed to compare the clinical and radiological outcomes, including periprosthetic bone mineral density (BMD) changes, between the short and standard stems after cementless hemiarthroplasty in elderly patients with femur neck fractures. We hypothesized that there is no significant difference in the clinical outcomes and periprosthetic bone preservation between the standard and short femoral stems.
Materials and Methods
The protocol of this prospective and randomized clinical study was approved by our institutional review board (IRB No. C2013200). Prior to the study, informed consent was obtained from all the included patients.
Patients
All patients aged ≥ 65 years who underwent hemiarthroplasties from January 2013 to May 2017 due to femoral neck fractures (Garden type [10] III or IV) were considered eligible (Fig. 1).
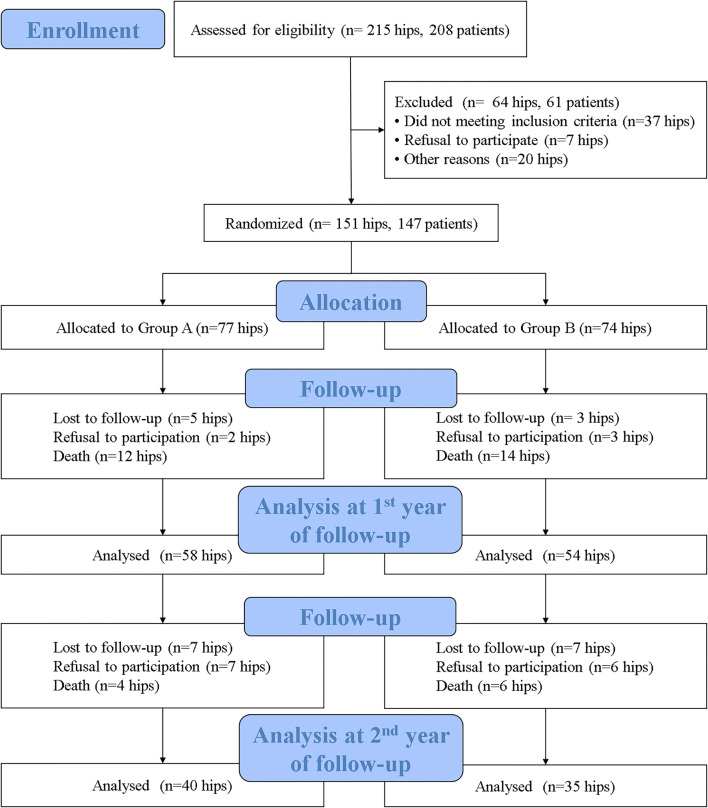
Fig. 1.
The CONSORT (Consolidated Standards of Reporting Trials) diagram of the study
The exclusion criteria were a history of hip surgery, pathologic fracture, and immunologic disorders such as rheumatoid arthritis, avascular necrosis of the femur head, Legg–Calvé–Perthes disease, and refusal to participate. The decision to enroll or exclude patients was made by an investigator who did not participate in the study.
In this randomized, single-blinded study, randomization into one of the two study groups was performed using Microsoft Excel (Microsoft, Redmond, Washington) to generate random numbers. Group allocations were made by a statistician, who did not otherwise participate in the study and were unknown to the investigators and patients. Information on group allocations was added to sealed envelopes. One day prior to surgery, the appropriately numbered envelope was opened to reveal the group allocation. The patients were divided into two groups as follows: Group A, patients who underwent hemiarthroplasty with a cementless short stem, and Group B, patients who underwent hemiarthroplasty with a cementless standard stem.
During the postoperative hospital admission period, all patients without end-stage renal disease in both groups received 5 mg of zoledronate (Aclasta; Novartis, Basel, Switzerland) intravenously annually and calcium and vitamin D supplements orally.
Surgical Procedure
All operations were performed using the posterolateral approach by a single experienced hip surgeon. The cementless femoral stem was inserted in a press-fit manner. The multimodal pain control cocktail injection was performed around the capsule. The posterior capsule and the short external rotators were tightly repaired using three drill holes in the trochanteric crest as described by Ji et al. [11]. The same postoperative protocol was used in both groups and consisted of immediate weight bearing with physiotherapy and mobilization.
Two different types of cementless femoral stems were used. In Group A, a Bencox M stem (Corentec®, Cheonan-si, South Korea) was used as a shorter femoral stem that has a proximal Ti-plasma spray microporous coating and a reduced size (length 95–119 mm). In this stem, the thin anterior–posterior width minimizes the amount of distal canal to be removed. The lateral part of the stem tip is removed to reduce the contact with the lateral cortical bone. In Group B, a Bencox ID stem (Corentec®, Cheonan-si, South Korea) was used as a standard femoral stem, which is a proximal Ti-plasma spray porous-coated standard metaphyseal fixation stem (length 137–177 mm). This stem has a patented trapezoidal neck design to allow wide angulation and protect impingement and dislocation, and the shaft of the stem has rectangular cross-sectional and longitudinal grooves that function to resist rotational motion.
Clinical Outcome Assessments
Clinical evaluation was performed using Koval's categories [12] for the activity level and reviewing the thigh pain at each follow-up. The activity levels were defined as follows: level I, independent community ambulator; level II, community ambulator with cane; level III, community ambulator with walker/crutches; level IV, independent household ambulator; level V, household ambulator with cane; level VI, household ambulator with walker/crutches; and level VII, nonfunctional ambulator [12]. Thigh pain was defined as pain perception in the anterior thigh below the inguinal area [13]. At each follow-up visit, the existence of thigh pain was evaluated and recorded, and the postoperative 6-week thigh pain score was set as the baseline value. Routine follow-up visits were scheduled at postoperative 6 weeks, 3, 6, 9, and 12 months, and every year thereafter. Patients who did not return for regular scheduled visits were contacted by telephone, and they were asked to send recent follow-up radiographs. Two nurses and one private locator identified the nonresponders and visited them.
Radiological Outcomes Assessments
Radiographic evaluation was performed by two orthopedic surgeons who did not participate in the index operation. A picture archiving and communication system (PACS; Maro View; Marotech, Seoul, Korea) was used.
Six-week anteroposterior and lateral radiographs of the pelvis were used for the baseline radiographic evaluation. Radiographic evaluation included an assessment of the initial fixation status, stability of the stem on follow-up, subsidence of the femoral stem, osteolysis and cortical porosis around the femoral stem, stress shielding grade, leg-length discrepancy, and heterotopic ossification. The grades of the initial fixation were classified according to Callaghan et al. [14, 15]. The stability of the femoral stem was evaluated by the method given by Engh et al. [16]. Subsidence of the femoral stem was defined as a change in the distance from the superolateral edge at the shoulder of the stem to the tip of the greater trochanter on the anteroposterior radiograph of the hip [17]; subsidence over 3 mm was defined as positive. Osteolytic lesions caused by stress shielding were defined by the criteria of Engh et al. [18], and the stress shielding grades were classified into four groups at the final follow-up as outlined previously by Engh et al. [19]; a classification of > grade 2 was determined to have clinical significance. Lesions were recorded according to the seven zones described by Gruen et al. [20]. Evidence of spot welding, pedestal formation, and reactive lines in each Gruen zone was also documented. Spot welds were defined as bone densification and trabecular streaming between the cortex and the implant [21]. Cortical porosis was considered as bone loss associated with normal aging, and was defined as a loss of endosteal definition and a decrease in bone mineralization resulting in a homogeneous but somewhat sparse (washed-out) appearance of the remaining cortex [22].To evaluate leg-length discrepancy, the distance between the interteardrop line and the lower margin of the lesser trochanter was measured on each leg. A difference > 2 cm was defined as a failure of leg-length equalization [23]. Heterotopic ossification was classified according to the system of Brooker et al. [24].
BMD Assessment
BMD was measured using dual-energy X-ray absorptiometry (DXA; Lunar Prodigy advance devices, GE Healthcare, Madison, WI, USA) on the admission day or before surgery and at the 12-month and 24-month postoperative follow-up. Patients were positioned supine with knee and foot support to ensure a neutral femur position. The Orthopaedic Software Package (GE Healthcare) was used to measure the BMD preoperatively in the femoral neck, and postoperatively in the seven Gruen zones [20].
Statistical Analysis
The sample size for the prospective study was based on an existing comparable study. The difference between the preoperative and postoperative outcome measures was analyzed using the Wilcoxon signed rank test or paired t test for continuous outcome measures, and Chi-square test or Fisher’s exact test for categorical outcome measures. The t test or Mann–Whitney U test was used for the comparison of independent variables between the two groups.
For analysis, the patients’ activity levels according to Koval’s categories were dichotomized into ambulatory outdoors (Koval’s categories of 1, 2, and 3) and housebound (Koval’s categories of 4, 5, 6, and 7).
The Statistical Package for Social Sciences (SPSS; version 22.0; SPSS Inc., Chicago, IL, USA) program was used for all analyses, and significance was defined as a P value of < 0.05. The distribution of variables is given as the mean and standard deviation (SD).
Results
Patients
We performed a prospective analysis of 151 hips (147 patients) with fracture of the femoral neck treated with bipolar hemiarthroplasty via either a short stem or a standard stem. In total, 77 hips (Group A) underwent bipolar hemiarthroplasties with short stems, and 74 hips (group B) underwent bipolar hemiarthroplasties with standard stems. During the study period, eight hips (5.3%) were lost to follow-up, five hips (3.3%) were excluded due to refusal to participate in the study, and 26 hips (17.2%) were excluded due to death of the patient within 1 year. In addition, 14 hips (9.3%) were lost to follow-up, 13 hips (8.6%) were excluded due to refusal to participate, and 10 hips (6.6%) were excluded due to death of the patient within the subsequent 1 year (Fig. 1).
The mean age at the time of the operation was 81.2 ± 5.6 years in Group A and 80.8 ± 6.4 years in group B. The mean follow-up period was 24.7 ± 16.5 months in Group A and 22.0 ± 3.1 months in group B. Most patients in both groups were assessed as ASA grade III (62 patients in group A, 69 patients in group B), and there was no significant between-group difference (P = 0.752). Every included patient underwent BMD preoperatively, and there was no statistically significant difference between groups. Furthermore, there was no significant difference between groups in terms of the demographic data (Table 1).
Table 1.
Demographic data
| Variable | Group A | Group B | P value |
|---|---|---|---|
| No. of patients | 77 | 74 | |
| Age (year) (mean ± SD) | 81.2 ± 5.6 | 80.8 ± 6.4 | 0.645 |
| Sex (M/F) | 18/59 | 17/57 | N/A |
| Height (cm) (mean ± SD) | 156.6 ± 7.4 | 157.9 ± 8.7 | 0.318 |
| Weight (kg) (mean ± SD) | 55.4 ± 9.0 | 54.8 ± 9.2 | 0.663 |
| Body mass index (kg/m2) (mean ± SD) | 22.7 ± 3.7 | 22.0 ± 3.1 | 0.209 |
| Surgical side (right/Left) | 37/40 | 38/36 | 0.746 |
| Mean f/u period (months) | 24.8 ± 16.5 | 26.7 ± 20.7 | 0.520 |
| Preoperative ambulation status Koval’s categories (1/2/3/4/5/6/7) | 41/15/2/5/12/2/0 | 43/8/5/4/8/6/0 | 0.277 |
| ASA grade (II/III/IV) | 7/62/8 | 5/59/10 | 0.752 |
| Radiological findings | |||
| Garden type (3/ 4) | 13/63 | 16/58 | 0.751 |
| Dorr type (A/B/C) | 1/73/3 | 3/64/7 | 0.209 |
| Preoperative BMD | |||
| L-spine BMD (L1–4) (mean ± SD) | 0.90 ± 0.19 | 0.86 ± 0.20 | 0.907 |
| Femur neck BMD (mean ± SD) | 0.61 ± 0.10 | 0.59 ± 0.12 | 0.394 |
| Femur Total BMD (mean ± SD) | 0.66 ± 0.12 | 0.64 ± 0.16 | 0.420 |
| Osteoporosis (T-score ≤ -2.5) | 54 (76.1%) | 58 (84.1%) | 0.292 |
SD standard deviation, BMD bone mineral density
Clinical Outcomes
Among the total 151 patients, 75 patients were available for follow-up over the 2 years, and 36 patients (23.9%) died during the follow-up period.
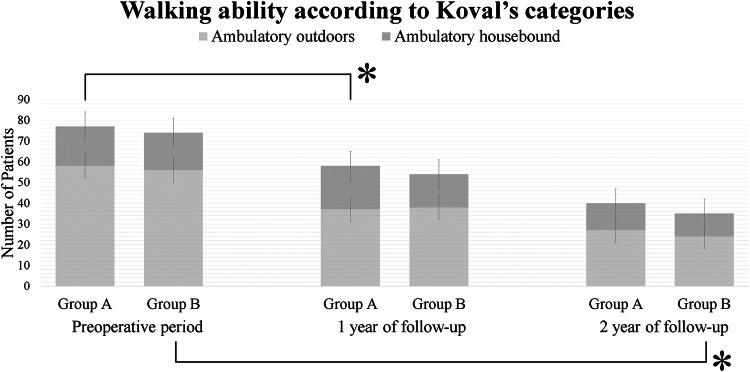
There was no significant difference in terms of ambulatory functions according to Koval’s categories between the two groups in the preoperative period, and at the 1st- and 2nd-year follow-ups. However, in both groups, the walking abilities became significantly worse than the preoperative walking abilities (Table 2, Fig. 2).
Table 2.
Ambulatory functions according to dichotomized Koval’s categories (ambulatory outdoors: 1, 2, 3; ambulatory housebound: 4, 5, 6, 7)
| Follow-up period | Group | Ambulatory outdoors | Ambulatory housebound | P valuea | P valueb | P valuec |
|---|---|---|---|---|---|---|
| Preoperative period (n = 151) | Group A | 58 (75.3%) | 19 (26.7%) | N/A | ||
| Group B | 56 (76.7%) | 18 (24.3%) | ||||
| 1st year-follow-up (n = 112) | Group A | 37 (63.8%) | 21 (36.2%) | 0.548 | 0.018 | |
| Group B | 38 (70.4%) | 16 (29.6%) | 0.133 | |||
| 2nd year-follow-up (n = 75) | Group A | 27 (67.5%) | 13 (32.5%) | N/A | 0.323 | 0.183 |
| Group B | 24 (68.6%) | 11 (31.4%) | 0.160 | 0.032 |
aComparison at each follow-up between the two groups
bComparison with previous year in each group
cComparison between the preoperative period and the 2nd year-follow-up in each group
Fig. 2.
Graph showing dichotomized walking ability according to Koval’s categories during the follow-up (the thick black lines and asterisks represent statistically significant differences)
With regard to thigh pain, 23/77 (29.9%) patients in Group A and 18/74 (24.3%) patients in Group B had thigh pain at the postoperative 6th week; this decreased to 2/38 (5.0%) patients and 2/33 (5.7%) patients at the latest follow-up. However, there were no differences between the groups in terms of the prevalence of thigh pain at each follow-up (P = 0.469, 1.000, and 1.000, respectively) (Table 3).
Table 3.
Thigh pain at the 1st year and 2nd year-follow-up
| Follow-up period | Group | Without pain | With pain | P valuea | P valueb |
|---|---|---|---|---|---|
| Postoperative 6th week | Group A (n = 77) | 54 (70.1%) | 23 (29.9%) | 0.469 | |
| Group B (n = 74) | 56 (75.7%) | 18 (24.3%) | |||
| 1st year-follow-up | Group A (n = 58) | 54 (93.1%) | 4 (6.9%) | 1.000 | 0.002 |
| Group B (n = 54) | 51 (94.4%) | 3 (5.6%) | 0.013 | ||
| 2nd year-follow-up | Group A (n = 40) | 38 (95.0%) | 2 (5.0%) | 1.000 | 1.000 |
| Group B (n = 35) | 33 (94.3%) | 2 (5.7%) | 1.000 |
aComparison at each follow-up between the two groups
bComparison with the previous year in each group
Radiologic Outcomes
All the femoral stems in both groups had radiographic evidence of bone ingrowth at the time of the last follow-up. Although axial subsidence, stem stability, leg length discrepancy, and periprosthetic osteolysis were not significantly different between the two groups at the latest follow-up, cortical porosis was more common in Group B at the 1st- and 2nd-year follow-ups (P = 0.034 and 0.010, respectively) (Table 4).
Table 4.
Radiologic assessment at each follow-up year
| Parameters | 1st follow-up year (n = 112) | 2nd follow-up year (n = 75) | P valuea | P valueb | P valuec | P valued | ||
|---|---|---|---|---|---|---|---|---|
| Group A (n = 58) | Group B (n = 54) | Group A (n = 40) | Group B (n = 35) | |||||
| Axial subsidence (mm) | 0.2 ± 0.6 | 0.3 ± 0.6 | 0.0 ± 0.2 | 0.0 ± 0.3 | 0.394 | 0.986 | 0.180 | 0.109 |
| Periprosthetic osteolytic lesion (Yes/No) | 8/50 | 9/45 | 3/37 | 6/29 | 0.794 | 0.289 | N/A | 0.711 |
| Gruen zone 1 | 7 | 6 | 3 | 4 | ||||
| Gruen zone 7 | 3 | 5 | 1 | 5 | ||||
| Cortical porosis (yes/no) | 10/48 | 19/35 | 6/34 | 15/20 | 0.034 | 0.010 | 0.660 | 0.183 |
| Leg length discrepancy (mm) | 1.2 ± 5.0 | 2.1 ± 5.0 | 1.8 ± 2.1 | 2.8 ± 7.9 | 0.075 | 0.104 | 0.317 | 0.317 |
| Stem stability | All bony stability during follow-up periods | |||||||
aComparison between the two groups at the 1st year-follow-up
bComparison between the two groups at the 2nd year-follow-up
cComparison in group A between the 1st and 2nd year-follow-up
dComparison in group B between the 1st and 2nd year-follow-up
BMD Assessment of Periprosthetic Femoral Bone Using the Seven Gruen Zones
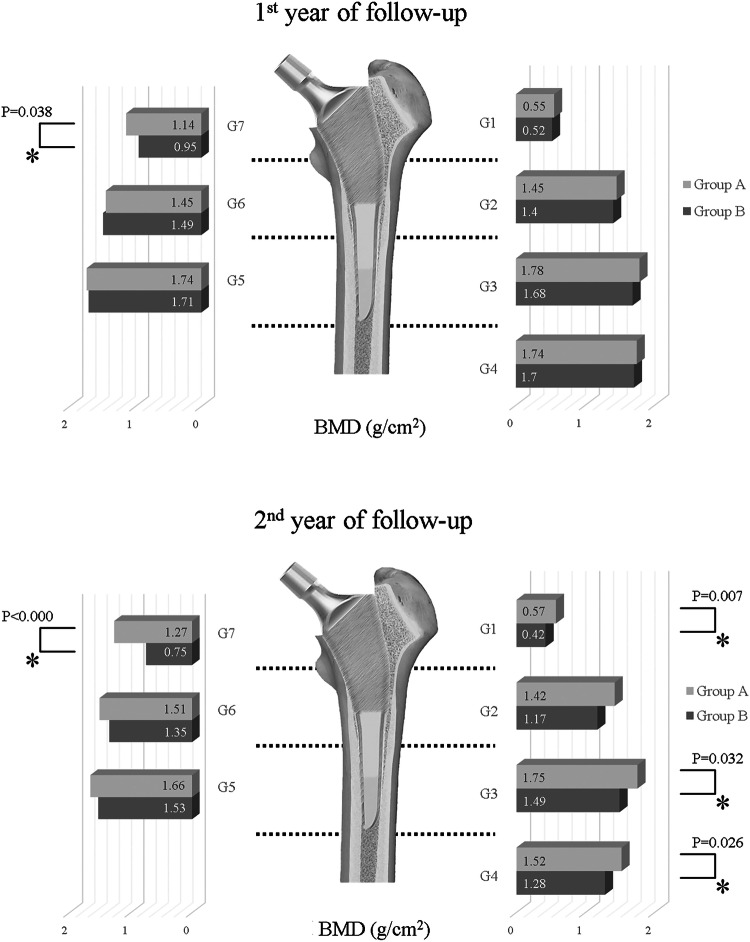
The mean BMD values and standard deviations (g/cm2) in each of the Gruen zones are summarized in Table 3. At the 1st postoperative year, the BMD values in Gruen zone (G) seven on the standard stem side were significantly lower than those on the short stem side (P = 0.038). Moreover, at the 2nd-year follow-up, the BMD values in G1, G3, G4, and G7 were significantly greater on the short stem side than the standard stem side (P = 0.007, 0.032, 0.026, and < 0.000, respectively). During the follow-up, although the periprosthetic BMDs of the short femoral stem were shown to maintaining trends, those of the standard femoral stems demonstrated a decreasing trend when comparing 1- and 2-year periprosthetic BMD (Table 5, Figs. 3, 4, and 5).
Table 5.
Bone mineral density (BMD) in each zone at 1st and 2nd years of follow-up (g/cm2)
| Zone | 1st year-follow-up (n = 112) | 2nd year-follow-up (n = 75) | P valuea | P valueb | P valuec | P valued | ||
|---|---|---|---|---|---|---|---|---|
| Group A (n = 58) | Group B (n = 54) | Group A (n = 40) | Group B (n = 35) | |||||
| G1 | 0.55 ± 0.17 | 0.52 ± 0.18 | 0.57 ± 0.16 | 0.42 ± 0.12 | 0.369 | 0.007 | 0.675 | 0.063 |
| G2 | 1.45 ± 0.23 | 1.40 ± 0.34 | 1.42 ± 0.24 | 1.17 ± 0.29 | 0.610 | 0.096 | 0.701 | 0.064 |
| G3 | 1.78 ± 0.22 | 1.68 ± 0.30 | 1.75 ± 0.24 | 1.49 ± 0.30 | 0.163 | 0.032 | 0.080 | 0.052 |
| G4 | 1.74 ± 0.20 | 1.70 ± 0.30 | 1.52 ± 0.19 | 1.28 ± 0.27 | 0.211 | 0.026 | 0.328 | 0.045 |
| G5 | 1.74 ± 0.20 | 1.71 ± 0.30 | 1.66 ± 0.25 | 1.53 ± 0.28 | 0.723 | 0.341 | 0.386 | 0.057 |
| G6 | 1.45 ± 0.27 | 1.49 ± 0.29 | 1.51 ± 0.17 | 1.35 ± 0.32 | 0.465 | 0.084 | 0.507 | 0.099 |
| G7 | 1.14 ± 0.34 | 0.95 ± 0.32 | 1.27 ± 0.29 | 0.75 ± 0.23 | 0.038 | 0.000 | 0.067 | 0.041 |
G Gruen zone
aComparision of BMD between the two groups at the 1st year-follow-up
bComparision of BMD between the two groups at the 2nd year-follow-up
cComparision in group A between the BMD at the 1st and 2nd year-follow-up
dComparision in group B between the BMD at the 1st and 2nd year-follow-up
Fig. 3.
a At the 1st year, in Gruen zone 7, the BMD of Group A was statistically better. b At the 2nd year, in Gruen zones 1, 3, 4, and 7, the statistical differences had become apparent
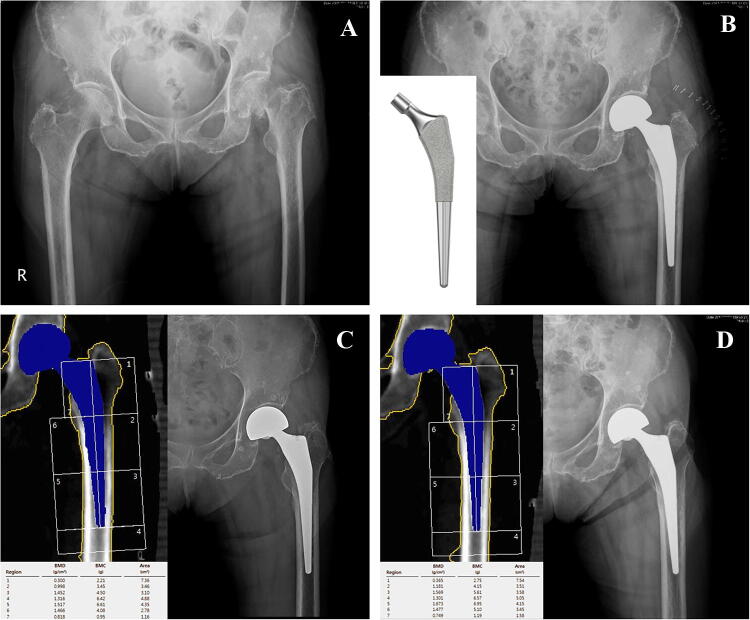
Fig. 4.
a Preoperative X-ray of an 80-year-old woman (Group A; short stem group). b Immediate postoperative image after hemiarthroplasty with Bencox M stem (Corentec®, South Korea). c, d Follow-up X-ray and Dual-energy X-ray absorptiometry images at postoperative 1st and 2nd years
Fig. 5.
a Preoperative X-ray of an 82-year-old woman (Group B; standard stem group). b Immediate postoperative image after hemiarthroplasty with Bencox ID stem (Corentec®, South Korea). c, d Follow-up X-ray and Dual-energy X-ray absorptiometry images at postoperative 1st and 2nd years
Complications
Dislocation occurred in two patients (one from each group) within 3 months postoperatively; both cases were treated with closed reduction and abduction bracing for 3 months, and there was no recurrence of dislocation until the latest follow-up. There were also two periprosthetic fractures (Vancouver type B1) in each group; they were treated by open reduction and internal fixation with a plate. In Group B, one hip had a thromboembolic episode and was successfully treated with antithrombotic drugs. No aseptic loosening, infection, or heterotrophic ossification were observed in either groups at the latest follow-up.
Discussion
To the best of our knowledge, this is the first study to compare the use of the short and standard stems in bipolar hemiarthroplasty for elderly fractured patients. This prospective randomized control study demonstrates that cementless bipolar hemiarthroplasty using short and standard stems improves clinical outcomes comparably and leads to the acquisition of radiologic stability at the latest follow-up. However, the BMD values in G1, G3, G4, and G7 were significantly greater on the short stem side than on the standard stem side (P = 0.007, 0.042, 0.026, and < 0.000, respectively).
Previous comparison studies between short and standard cementless stems in patients with total hip arthroplasty have reported better clinical outcomes, including those regarding thigh pain and preservation of proximal periprosthetic cortical bones [6, 25, 26]. Yu et al. [6] preformed a comparison study in patients aged ≥ 70 years with total hip arthroplasty comprising 55 hips with a short femoral cementless stem and 58 hips with a standard femoral cementless stem. They reported that although the Harris hip score and radiologic fixation were not significantly different between the two groups, the short stem showed less thigh pain and intra-operative femoral fracture rate at a mean follow-up of 40 months [6]. A prospective randomized control study in patients undergoing cementless total hip arthroplasty was performed to determine the stability of short femoral stem in 20 patients compared to that of a standard femoral stem in 18 patients. The authors reported that the stability of the short stem was better than that of the standard stem, and that the dynamically inducible micromotion, rate of complications, and functional outcome were not significantly different between the two groups at a minimum of 2 years of follow-up [26].
These findings are in agreement with those of the current study in that similar clinical outcomes and radiologic stabilities were observed in both groups at the minimum 2-year follow-up. However, it is difficult to directly compare the current study with previous studies given the use of different surgical indications, such as femoral neck fracture, type of surgery, and different patient demographics. Nevertheless, the clinical outcomes and the radiologic stabilities are similar to those observed in previous comparison studies.
Currently, femoral implant designs for THA are known to influence periprosthetic BMD; however, evidence for a change in periprosthetic BMD remains controversial. Yan et al. performed a meta-analysis using seven studies involving 910 patients and five short femoral stem designs. The authors reported no significant differences in the percentage of BMD changes in all Gruen zones, and short stems with lateral flare revealed a moderate- to low-quality evidence for superiority over the standard THA [27]. According to a recent update, a systematic review and meta-analysis using 12 randomized controlled trials comparing the short stem to the standard cementless stem demonstrated that the short stem resulted in less BMD changes in G7 at 1 and 2 years postoperatively [mean difference (MD) = 5.11; 95% CI 1.61, 8.61; P = 0.30; and MD = 4.90; 95% CI 1.01, 8.79; P = 0.17, respectively] [28]. In this study, the BMD values in G7 on the standard stem side were significantly lower than those on the short stem side at postoperative 1 year (P = 0.038). These differences in periprosthetic BMD progressed in G1, G3, and G4, and were more prominent in G7 at the 2-year follow-up (P = 0.007, 0.042, 0.026, and < 0.000, respectively). In addition, when comparing the outcomes at the 1- and 2-year follow-up assessments, the periprosthetic BMDs of the standard femoral stems demonstrated a decreasing trend, and those of the short femoral stems were maintained. Our findings indicate that stem designs are important factors that influence the periprosthetic BMD of the femoral stems [29]. Although the fixation method and alloy also influence load transfer to the surrounding bone, changes to the periprosthetic BMD in the short stem areas showed better bone preservation in this study.
This study has several limitations. First, many patients were lost to follow-up or refused to participate in this study; among the 151 hips, 22 (14.6%) were lost to follow-up. Although we tried to follow-up these patients, many had relocated or were otherwise unreachable. Although 18 hips of participants who initially agreed to participate were examined, several participants did not present for regular follow-up appointments, including radiographic examinations and repeat BMD measurements. Second, we also observed a high rate of mortality (36/151 hips (23.9%)) at 2 years postoperatively. However, most patients in both groups were assessed as ASA grade III (62 patients in group A, 69 patients in group B). According to Nkanang et al. [30], increased age is associated with an increased risk of perioperative mortality for patients who are ASA grade 3 and above. Therefore, older age and the presence of severe comorbidities might be related to the high mortality observed in this study. Third, although we tried to assess the cause of death in 36 patients who died during the study period, we were often unable to confirm the cause or date of death for patients who died at other hospitals or at their homes. Fourth, in terms of comparing the changes in BMD from the preoperative period to the postoperative assessment, the BMD of the opposite side femoral neck was used as the preoperative BMD; this was in line with the methods used in previous studies [31, 32]. Finally, the comparison of the short and standard stems for cementless hemiarthroplasty in elderly patients with femur neck fracture has not yet been studied. Our results were compared with the outcomes in patients who underwent total hip arthroplasty; thus, the results of this direct comparison have a potential limitation in terms of generalization.
Conclusions
In conclusion, the clinical outcomes and radiologic stability of the short stem in cementless bipolar hemiarthroplasty are similar to that of the standard femoral stem in elderly patients with femoral neck fracture at the latest follow-up. In addition, the periprosthetic BMD of the short femoral stems is better in G1, G3, G4, and G7 at a minimum of 2 years of follow-up.
Acknowledgements
No benefits in any form have been received or will be received from any commercial party related directly or indirectly to the subject of this article.
Funding
None.
Compliance with Ethical Standards
Conflict of interest
No benefits in any form have been received or will be received from a commercial party related directly or indirectly to the subject of this article. Each author certifies that he or she has no commercial associations (e.g., consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Jiang J, Yang CH, Lin Q, Yun XD, Xia YY. Does arthroplasty provide better outcomes than internal fixation at mid- and long-term followup? A Meta-analysis. Clinical Orthopaedics and Related Research. 2015;473:2672–2679. doi: 10.1007/s11999-015-4345-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Burgers PT, Van Geene AR, Van den Bekerom MP, et al. Total hip arthroplasty versus hemiarthroplasty for displaced femoral neck fractures in the healthy elderly: a meta-analysis and systematic review of randomized trials. International Orthopaedics. 2012;36:1549–1560. doi: 10.1007/s00264-012-1569-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Luo X, He S, Li Z, Huang D. Systematic review of cemented versus uncemented hemiarthroplasty for displaced femoral neck fractures in older patients. Archives of Orthopaedic and Trauma Surgery. 2012;132:455–463. doi: 10.1007/s00402-011-1436-9. [DOI] [PubMed] [Google Scholar]
- 4.Taylor F, Wright M, Zhu M. Hemiarthroplasty of the hip with and without cement: a randomized clinical trial. Journal of Bone and Joint Surgery. 2012;94:577–583. doi: 10.2106/JBJS.K.00006. [DOI] [PubMed] [Google Scholar]
- 5.Morrey BF. Short-stemmed uncemented femoral component for primary hip arthroplasty. Clinical Orthopaedics and Related Research. 1989;249:169–175. [PubMed] [Google Scholar]
- 6.Yu H, Liu H, Jia M, Hu Y, Zhang Y. A comparison of a short versus a conventional femoral cementless stem in total hip arthroplasty in patients 70 years and older. Journal of Orthopaedic Surgery and Research. 2016;11:33. doi: 10.1186/s13018-016-0367-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Salemyr M, Muren O, Ahl T, et al. Lower periprosthetic bone loss and good fixation of an ultra-short stem compared to a conventional stem in uncemented total hip arthroplasty. Acta Orthopaedica. 2015;86:659–666. doi: 10.3109/17453674.2015.1067087. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Sluimer JC, Hoefnagels NH, Emans PJ, Kuijer R, Geesink RG. Comparison of two hydroxyapatite-coated femoral stems: clinical, functional, and bone densitometry evaluation of patients randomized to a regular or modified hydroxyapatite-coated stem aimed at proximal fixation. Journal of Arthroplasty. 2006;21:344–352. doi: 10.1016/j.arth.2005.06.015. [DOI] [PubMed] [Google Scholar]
- 9.Koyano G, Jinno T, Koga D, Yamauchi Y, Muneta T, Okawa A. Comparison of bone remodeling between an anatomic short stem and a straight stem in 1-stage bilateral total hip arthroplasty. Journal of Arthroplasty. 2017;32:594–600. doi: 10.1016/j.arth.2016.07.016. [DOI] [PubMed] [Google Scholar]
- 10.Garden RS. Stability and union in subcapital fractures of the femur. Journal of Bone and Joint Surgery. British Volume. 1964;46:630–647. doi: 10.1302/0301-620X.46B4.630. [DOI] [PubMed] [Google Scholar]
- 11.Ji HM, Kim KC, Lee YK, Ha YC, Koo KH. Dislocation after total hip arthroplasty: a randomized clinical trial of a posterior approach and a modified lateral approach. Journal of Arthroplasty. 2012;27:378–385. doi: 10.1016/j.arth.2011.06.007. [DOI] [PubMed] [Google Scholar]
- 12.Koval KJ, Skovron ML, Aharonoff GB, Meadows SE, Zuckerman JD. Ambulatory ability after hip fracture. A prospective study in geriatric patients. Clinical Orthopaedics and Related Research. 1995;310:150–159. [PubMed] [Google Scholar]
- 13.Barrack RL, Paprosky W, Butler RA, Palafox A, Szuszczewicz E, Myers L. Patients' perception of pain after total hip arthroplasty. Journal of Arthroplasty. 2000;15:590–596. doi: 10.1054/arth.2000.6634. [DOI] [PubMed] [Google Scholar]
- 14.Heekin RD, Callaghan JJ, Hopkinson WJ, Savory CG, Xenos JS. The porous-coated anatomic total hip prosthesis, inserted without cement. Results after five to seven years in a prospective study. The Journal of Bone and Joint Surgery. 1993;75:77–91. doi: 10.2106/00004623-199301000-00011. [DOI] [PubMed] [Google Scholar]
- 15.Callaghan JJ, Dysart SH, Savory CG. The uncemented porous-coated anatomic total hip prosthesis. Two-year results of a prospective consecutive series. The Journal of Bone and Joint Surgery. 1988;70:337–346. doi: 10.2106/00004623-198870030-00004. [DOI] [PubMed] [Google Scholar]
- 16.Engh CA, Glassman AH, Suthers KE. The case for porous-coated hip implants. The femoral side. Clinical Orthopaedics and Related Research. 1990;261:63–81. [PubMed] [Google Scholar]
- 17.Meijerink, H.J., Gardeniers, J.W., Buma, P., Lemmens, J.A., Schreurs, B.W. (2004) Hydroxyapatite does not improve the outcome of a bipolar hemiarthroplasty. Clinical Orthopaedics and Related Research, 143–150. [DOI] [PubMed]
- 18.Engh CA, Bobyn JD, Glassman AH. Porous-coated hip replacement. The factors governing bone ingrowth, stress shielding, and clinical results. The Journal of Bone and Joint Surgery. 1987;69:45–55. doi: 10.1302/0301-620X.69B1.3818732. [DOI] [PubMed] [Google Scholar]
- 19.Engh, C.A., Bobyn, J.D. (1988). The influence of stem size and extent of porous coating on femoral bone resorption after primary cementless hip arthroplasty. Clinical Orthopaedics and Related Research, 231, 7–28. [PubMed]
- 20.Gruen, T.A., McNeice, G.M., Amstutz, H.C. (1979). "Modes of failure" of cemented stem-type femoral components: a radiographic analysis of loosening. Clinical Orthopaedics and Related Research, 17–27. [PubMed]
- 21.Kido K, Fujioka M, Takahashi K, Ueshima K, Goto T, Kubo T. Short-term results of the S-ROM-A femoral prosthesis operative strategies for Asian patients with osteoarthritis. Journal of Arthroplasty. 2009;24:1193–1199. doi: 10.1016/j.arth.2009.03.009. [DOI] [PubMed] [Google Scholar]
- 22.Capello WN, D'Antonio JA, Geesink RG, Feinberg JR, Naughton M. Late remodeling around a proximally HA-coated tapered titanium femoral component. Clinical Orthopaedics and Related Research. 2009;467:155–165. doi: 10.1007/s11999-008-0550-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Woolson ST, Hartford JM, Sawyer A. Results of a method of leg-length equalization for patients undergoing primary total hip replacement. Journal of Arthroplasty. 1999;14:159–164. doi: 10.1016/S0883-5403(99)90119-5. [DOI] [PubMed] [Google Scholar]
- 24.Brooker AF, Bowerman JW, Robinson RA, Riley LH., Jr Ectopic ossification following total hip replacement. Incidence and a method of classification. Journal of Bone and Joint Surgery. 1973;55:1629–1632. doi: 10.2106/00004623-197355080-00006. [DOI] [PubMed] [Google Scholar]
- 25.Lee SJ, Yoon KS. favorable functional recovery and stem stability after hip arthroplasty with a short metaphyseal stem in elderly patients with osteoporotic femoral neck fractures. Hip & Pelvis. 2019;31:11–17. doi: 10.5371/hp.2019.31.1.11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Ferguson RJ, Broomfield JA, Malak TT, et al. Primary stability of a short bone-conserving femoral stem: a two-year randomized controlled trial using radiostereometric analysis. The Bone & Joint Journal. 2018;100-B:1148–1156. doi: 10.1302/0301-620X.100B9.BJJ-2017-1403.R1. [DOI] [PubMed] [Google Scholar]
- 27.Yan SG, Li D, Yin S, Hua X, Tang J, Schmidutz F. Periprosthetic bone remodeling of short cementless femoral stems in primary total hip arthroplasty: A systematic review and meta-analysis of randomized-controlled trials. Medicine (Baltimore). 2017;96:e8806. doi: 10.1097/MD.0000000000008806. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Liang HD, Yang WY, Pan JK, et al. Are short-stem prostheses superior to conventional stem prostheses in primary total hip arthroplasty? A systematic review and meta-analysis of randomised controlled trials. British Medical Journal Open. 2018;8:e021649. doi: 10.1136/bmjopen-2018-021649. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Knutsen AR, Lau N, Longjohn DB, Ebramzadeh E, Sangiorgio SN. Periprosthetic femoral bone loss in total hip arthroplasty: systematic analysis of the effect of stem design. Hip International. 2017;27:26–34. doi: 10.5301/hipint.5000413. [DOI] [PubMed] [Google Scholar]
- 30.Nkanang B, Parker M, Parker E, Griffiths R. Perioperative mortality for patients with a hip fracture. Injury. 2017;48:2180–2183. doi: 10.1016/j.injury.2017.07.007. [DOI] [PubMed] [Google Scholar]
- 31.Tran P, Zhang BX, Lade JA, Pianta RM, Unni RP, Haw CS. Periprosthetic bone remodeling after novel short-stem neck-sparing total hip arthroplasty. Journal of Arthroplasty. 2016;31:2530–2535. doi: 10.1016/j.arth.2016.04.023. [DOI] [PubMed] [Google Scholar]
- 32.Wixson RL, Stulberg SD, Van Flandern GJ, Puri L. Maintenance of proximal bone mass with an uncemented femoral stem analysis with dual-energy X-ray absorptiometry. Journal of Arthroplasty. 1997;12:365–372. doi: 10.1016/S0883-5403(97)90191-1. [DOI] [PubMed] [Google Scholar]