Abstract
Proximal humerus lesser tuberosity avulsions are uncommon injuries; however, when present, they can be debilitating for patients. As such, they pose a unique clinical challenge. These fractures were traditionally treated through an open approach to the proximal humerus; however, arthroscopic techniques continue to evolve and are increasingly used for these types of injuries. We describe our minimally invasive arthroscopic technique to repair lesser tuberosity avulsions using standard arthroscopic equipment. This method is safe, efficient, and applies basic shoulder arthroscopic techniques.
Compared with subscapularis tears, which are now known to be relatively common, lesser tuberosity avulsions are relatively rare.1,2 Typically seen in the adolescent population, surgical treatment of lesser tuberosity avulsions has undergone a marked evolution as more advanced techniques are developed and arthroscopic techniques have advanced.
The subscapularis origin lies in the anterior scapular fossa and inserts on the proximal humerus.3 Its insertion on the lesser tuberosity has been well described by Richards et al.4 to be trapezoidal in shape with mean width 18 mm superiorly and 3 mm inferiorly. The superior fibers of the subscapularis are most critical for load transmission, while also forming a sling for the biceps tendon.5, 6, 7 The primary function of the subscapularis is for internal rotation of the humerus, but also aids in shoulder stability acting as a restraint to anterior humeral head translation.8
The incidence of lesser tuberosity fractures is described in adults as 0.46 per 100,000 population years.9 There are numerous case reports of these injuries in adolescents.1,9, 10, 11, 12 Nondisplaced lesser tuberosity avulsions have been successfully treated nonoperatively with good results. However, displacement of 5 mm or angulation >45° have been described as a surgical indication because of risk for nonunion, malunion, and biceps subluxation.11
Identification of these injuries requires a thorough history, examination, and imaging. The injury mechanism classically involves traumatic forced abduction and external rotation of the affected shoulder. Examination will identify anterior shoulder pain, positive bear hug, “lift off,” and belly press tests. Imaging, particularly axillary radiographs (Fig 1) and magnetic resonance imaging (Fig 2), will confirm the diagnosis and degree of displacement of the fragment. This will help document amount of displacement, and, thus, the potential need for surgical intervention.13 Vavek et al.14 recommended a “high index of suspicion should be maintained in adolescent males with anterior shoulder pain and subscapularis weakness, especially after a fall.”
Fig 1.
Radiographic assessment of the left shoulder in a patient with exam concerning for subscapular avulsion fracture. (A) Grashey, (B) scapular Y, and (C) axillary views of the left shoulder. Axillary view best shows a proximal anterior radiodensity and associated bony defect in the humeral head, which is consistent with examination concerning for subscapular avulsion fracture.
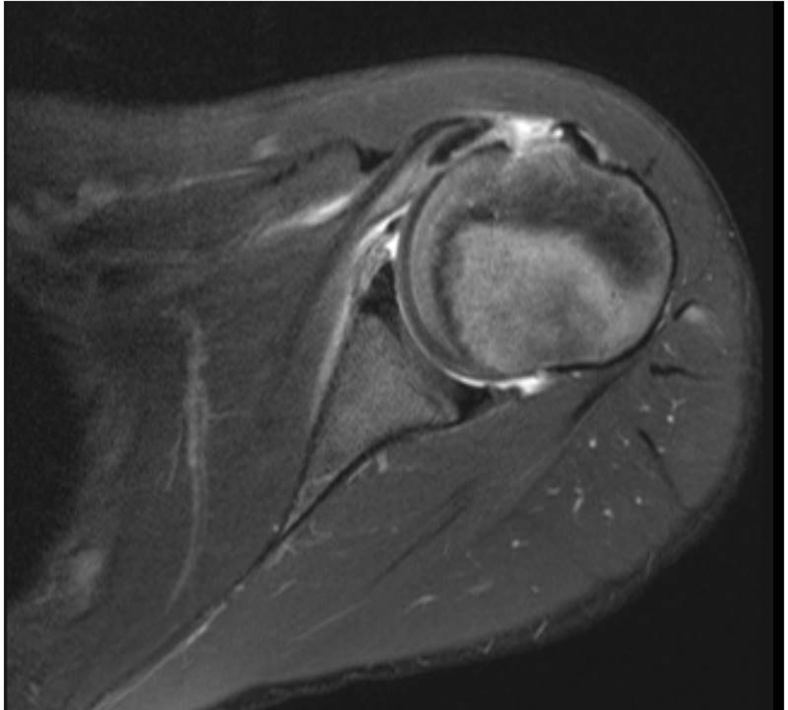
Fig 2.
Axial T2-weighted magnetic resonance imaging (MRI) of the left shoulder in a patient with examination and initial radiographs concerning for subscapular avulsion fracture. Axial MRI sections demonstrate displaced osseocartilaginous fragment that maintains its attachment to the subscapularis tendon. This confirms the diagnosis of subscapularis avulsion fracture.
With the advancement of arthroscopic techniques, several methods have been described to address the displaced lesser tuberosity avulsion fracture. Classically, these injuries were managed by open reduction and internal fixation, which has fallen out of favor with the demonstrated success and decreased morbidity of arthroscopic techniques. There are currently 3 all-arthroscopic techniques described by Scheibel et al.,12 Heyworth et al.,15 and Cregar et al.,16 which have built upon one another to achieve maximum fracture healing area and secure fixation. The following technique is a natural advancement of these prior descriptions to achieve secure fixation in a streamlined fashion.
Technique
The patient is brought to the operating room, placed on a standard operative table, and undergoes general anesthesia. The patient is then positioned in the beach chair position, and the operative extremity is prepped and draped in the standard sterile fashion. We prefer a high beach chair (dinner table) position for shoulder arthroscopy; however, the procedure could also be performed in the lateral decubitus position based on surgeon preference.
The procedure begins with creating a standard high posterolateral viewing portal and performing a standard diagnostic shoulder arthroscopy examination with a 30° arthroscope (Video 1). An anterior working portal is created under direct visualization from outside-in. This portal should enter the joint immediately above the subscapularis tendon, midway between the glenoid and humerus. Using a needle and outside in technique increases accuracy. Without tension, the needle should sit in the center of the joint (Fig 3A). Next, an extensive rotator interval debridement is performed using shaver and radiofrequency ablation (Fig 3B). We rely predominantly on ablation given the vascular nature of this tissue (Fig 3C). The fracture fragment is identified, typically found retracted slightly medially.
Fig 3.
Intraoperative arthroscopic photos of the left shoulder from a standard posterior portal with the patient in the beach chair position. (A) The fracture is identified via anterior portal through rotator interval. (B and C) A thorough debridement of the rotator interval is completed. (D) A 70° arthroscope is inserted via the anterior portal and the fracture site is debrided to stimulate fracture healing.
After opening the rotator interval, the anterior portal can be switched to a larger portal (8.25 mm x 7 cm). This will allow passage of lassos, sutures, and anchors. A 70° camera is then placed through the posterior portal to view the lesser tuberosity avulsion site (Fig 3D). The arm is placed in flexion and internal rotation. This will allow an improved view of the lesser tuberosity donor site. A gentle posterior force on the humerus (lever push) will increase the amount of space available to work in the front of the shoulder, and can improve the view of the donor site. A shaver (Arthrex, Naples, FL) is then placed through the anterior portal and the avulsion site is debrided to bleeding bone for improved healing upon reduction and fixation.
After debriding the fracture site and the tuberosity fragment, the repair is completed. A 2.9-m PushLock (Arthrex) anchor is loaded with LabralTape (Arthrex) and introduced through the anterior portal and placed medial to the avulsion site, just at the articular cartilage junction (Fig 4 A and B). A suture lasso is then introduced and passed just medial to the avulsed fragment. Redundant lasso is passed into the joint, and the lasso is continually advanced as the lasso handle is withdrawn from the cannula. The lasso is then retrieved through the anterior portal. The 2 sutures from the medial anchor are then shuttled through the subscapularis medial to the fragment (Fig 4C).
Fig 4.
Intraoperative arthroscopic photos of the left shoulder using a 70° arthroscope from standard posterior portal with the patient in the beach chair position. (A and B) The first anchor is placed medial to the fracture. (C) Labral tape is pulled deep to superficial through subscapularis tendon medial to avulsion fragment. (D) The second anchor site is defined lateral to the avulsion site.
The LabralTape is then loaded into a second PushLock anchor. The second anchor is placed through the anterior portal and inserted lateral to the avulsion site (Fig 4D, Fig 5A). This reduces the fragment into the avulsion site via knotless technique with all anchors outside the fracture site (Fig 5 B and C). It allows excellent, low profile compression of the fragment.
Fig 5.
Intraoperative arthroscopic photos of the left shoulder using 70° arthroscope from standard posterior portal with the patient in the beach chair position. (A) Place second anchor lateral to humeral avulsion site. (B) Tension the subscapularis in place. (C) Final construct.
The arm is immobilized in a sling for 6 weeks. At 2 weeks, passive range of motion of the shoulder is begun, limiting external rotation to neutral for the first 6 weeks. At 6 weeks, the sling is discontinued, and additional passive stretching exercises are completed (without restriction). Strengthening is initiated at 3 months.
Discussion
Lesser tuberosity avulsion fractures are rare injuries that are frequently missed because of diagnostic examination and imaging challenges. This can lead to delays in management.10,17 Delays in management have been associated with worse outcomes, including pain, weakness, loss of motion, nonunion, and associated biceps pathology.10,18,19
Although these injuries can be managed through open techniques, equivalent outcomes were demonstrated by open or arthroscopic techniques in a metanalysis by Vavken et al.14 Given the decreased morbidity and equivalent outcomes of arthroscopic techniques, it is now accepted and our preference to perform these repairs through an all arthroscopic technique.
Currently, multiple all arthroscopic techniques have been described (Table 1). These techniques have progressed from knotted to knotless suture technique, anchor fixation within the defect to adjacent bone, and, finally, multiple portal sites to a single viewing and single working portal. This technique uses previous advancements of knotless technique to create a low profile construct and anchors outside of the fracture site to maximize bone-to-bone healing potential.16 It goes beyond prior techniques to use only 1 anterior working portal for a more efficient surgical technique and uses the beach chair position (Table 2). The surgery is accomplished through only 2 total portals through a wide rotator interval debridement and use of a 70° camera to visualize the anterior humerus from a posterior portal (Table 3).
Table 1.
Comparison of Published Arthroscopic Subscapularis Avulsion Fracture Repair Techniques
| Scheibel et al.12 | Heyworth et al.15 | Cregar et al.16 | Barlow et al. | |
|---|---|---|---|---|
| Position | Beach chair | Not specified | Lateral | Beach chair |
| Knots | Mattress stich, single stitch | Horizontal mattress | Luggage loop, knotless | Knotless |
| Anchor position | Inside fracture | Inside fracture | Outside fracture | Outside fracture |
| No. of portals | 3 | 3 | 4 | 2 |
Table 2.
Key Points for Completing Knotless Single Anterior Portal Subscapularis Avulsion Fracture Repair
|
Table 3.
Equipment Required
DePuy Synthes.
Arthrex.
Smith and Nephew.
Cregar et al.16 previously described a similar all arthroscopic technique. The authors described using primarily a lateral viewing portal along with a subacromial bursectomy. They also used an accessory biceps portal in addition to an anterior working portal. The current technique differs in using a traditional posterior viewing portal and 70° camera to achieve adequate visualization of the avulsion site, saving time and preserving adjacent structures. To aid in visualization of the subscapularis footprint, the arm is placed in elevation and internal rotation. This is similar to the technique described by Denard and Burkhart to “see around the corner” for articular-sided subscapularis repairs.20 The limitations to the technique include surgeon comfort with the 70° camera and size of avulsion fragment. The technique may not be appropriate for larger avulsions that require more than 2 anchors to provide sufficient stability (Table 4).
Table 4.
Strengths and Limitations of Single Anterior Portal Repair
| Strengths | Limitations |
|---|---|
|
|
Although displaced lesser tuberosity avulsion fractures are a rare injury, precise surgical management is critical to return patients to full function. This technique facilitates a safe, predictable, effective repair using standard arthroscopy equipment and skills.
Footnotes
The authors report that they have no conflicts of interest in the authorship and publication of this article. Full ICMJE author disclosure forms are available for this article online, as supplementary material.
Supplementary Data
Intraoperative video of knotless arthroscopic repair of subscapularis avulsion fracture of the left shoulder using 2 single anterior portals with the patient in the beach chair position. The procedure begins viewed from a standard posterior portal with identification of the fragment and a generous rotator interval debridement. After switching to the 70° camera through the posterior portal, the fragment can be well visualized and the fracture site debrided to promote healing. Anchors are placed in a horizontal mattress fashion outside of the fracture site beginning with the medial anchor. The construct is then tightened and evaluated for stability. Postoperative the patient is immobilized for 6 weeks in a sling to allow for fracture healing. Then the sling is discontinued and the patient is progressed through 6 weeks of passive range of motion protocol while limiting external rotation, and finally the patient completes 6 weeks of active strengthening rehabilitation.
References
- 1.Kunkel S.S., Monesmith E.A. Isolated avulsion fracture of the lesser tuberosity of the humerus: A case report. J Shoulder Elbow Surg. 1993;2:43–46. doi: 10.1016/S1058-2746(09)80137-7. [DOI] [PubMed] [Google Scholar]
- 2.LaMont L.E., Green D.W., Altchek D.W., Warren R.F., Wickiewicz T.L. Subscapularis tears and lesser tuberosity avulsion fractures in the pediatric patient. Sports Health. 2015;7:110–114. doi: 10.1177/1941738114533657. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.D'Addesi L.L., Anbari A., Reish M.W., Brahmabhatt S., Kelly J.D. The subscapularis footprint: An anatomic study of the subscapularis tendon insertion. Arthroscopy. 2006;22:937–940. doi: 10.1016/j.arthro.2006.04.101. [DOI] [PubMed] [Google Scholar]
- 4.Richards D.P., Burkhart S.S., Tehrany A.M., Wirth M.A. The subscapularis footprint: An anatomic description of its insertion site. Arthroscopy. 2007;23:251–254. doi: 10.1016/j.arthro.2006.11.023. [DOI] [PubMed] [Google Scholar]
- 5.Arai R., Sugaya H., Mochizuki T., Nimura A., Moriishi J., Akita K. Subscapularis tendon tear: An anatomic and clinical investigation. Arthroscopy. 2008;24:997–1004. doi: 10.1016/j.arthro.2008.04.076. [DOI] [PubMed] [Google Scholar]
- 6.Clark J.M., Harryman D.T., 2nd Tendons, ligaments, and capsule of the rotator cuff. Gross and microscopic anatomy. J Bone Joint Surg Am. 1992;74:713–725. [PubMed] [Google Scholar]
- 7.Halder A., Zobitz M.E., Schultz E., An K.N. Structural properties of the subscapularis tendon. J Orthop Res. 2000;18:829–834. doi: 10.1002/jor.1100180522. [DOI] [PubMed] [Google Scholar]
- 8.Perry J. Anatomy and biomechanics of the shoulder in throwing, swimming, gymnastics, and tennis. Clin Sports Med. 1983;2:247–270. [PubMed] [Google Scholar]
- 9.Robinson C.M., Teoh K.H., Baker A., Bell L. Fractures of the lesser tuberosity of the humerus. J Bone Joint Surg Am. 2009;91:512–520. doi: 10.2106/JBJS.H.00409. [DOI] [PubMed] [Google Scholar]
- 10.Ogawa K., Takahashi M. Long-term outcome of isolated lesser tuberosity fractures of the humerus. J Trauma. 1997;42:955–959. doi: 10.1097/00005373-199705000-00029. [DOI] [PubMed] [Google Scholar]
- 11.Levine B., Pereira D., Rosen J. Avulsion fractures of the lesser tuberosity of the humerus in adolescents: Review of the literature and case report. J Orthop Trauma. 2005;19:349–352. [PubMed] [Google Scholar]
- 12.Scheibel M., Martinek V., Imhoff A.B. Arthroscopic reconstruction of an isolated avulsion fracture of the lesser tuberosity. Arthroscopy. 2005;21:487–494. doi: 10.1016/j.arthro.2004.11.012. [DOI] [PubMed] [Google Scholar]
- 13.Mizrahi D.J., Averill L.W., Blumer S.L., Meyers A.B. Chronic lesser tuberosity avulsion in an adolescent with an associated biceps pulley injury. Pediatr Radiol. 2018;48:749–753. doi: 10.1007/s00247-017-4016-5. [DOI] [PubMed] [Google Scholar]
- 14.Vavken P., Bae D.S., Waters P.M., Flutie B., Kramer D.E. Treating subscapularis and lesser tuberosity avulsion injuries in skeletally immature patients: A systematic review. Arthroscopy. 2016;32:919–928. doi: 10.1016/j.arthro.2015.10.022. [DOI] [PubMed] [Google Scholar]
- 15.Heyworth B.E., Dodson C.C., Altchek D.W. Arthroscopic repair of isolated subscapularis avulsion injuries in adolescent athletes. Clin J Sport Med. 2008;18:461–463. doi: 10.1097/JSM.0b013e318188b1a5. [DOI] [PubMed] [Google Scholar]
- 16.Cregar W.M., MacLean I.S., Verma N.N., Trenhaile S.W. Lesser tuberosity avulsion fracture repair using knotless arthroscopic fixation. Arthrosc Techniques. 2018;7:e899–e905. doi: 10.1016/j.eats.2018.04.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Provance A.J., Polousky J.D. Isolated avulsion fracture of the subscapularis tendon with medial dislocation and tear of biceps tendon in a skeletally immature athlete: A case report. Curr Opin Pediatr. 2010;22:366–368. doi: 10.1097/MOP.0b013e328337fea5. [DOI] [PubMed] [Google Scholar]
- 18.Neogi D.S., Bejjanki N., Ahrens P.M. The consequences of delayed presentation of lesser tuberosity avulsion fractures in adolescents after repetitive injury. J Shoulder Elbow Surg. 2013;22:e1–e5. doi: 10.1016/j.jse.2012.12.004. [DOI] [PubMed] [Google Scholar]
- 19.Paxinos O., Karavasili A., Manolarakis M., Paxinos T., Papavasiliou A. Neglected lesser tuberosity avulsion in an adolescent elite gymnast. Shoulder Elbow. 2014;6:178–181. doi: 10.1177/1758573214531413. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Denard P.J., Burkhart S.S. A new method for knotless fixation of an upper subscapularis tear. Arthroscopy. 2011;27:861–866. doi: 10.1016/j.arthro.2010.11.010. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Intraoperative video of knotless arthroscopic repair of subscapularis avulsion fracture of the left shoulder using 2 single anterior portals with the patient in the beach chair position. The procedure begins viewed from a standard posterior portal with identification of the fragment and a generous rotator interval debridement. After switching to the 70° camera through the posterior portal, the fragment can be well visualized and the fracture site debrided to promote healing. Anchors are placed in a horizontal mattress fashion outside of the fracture site beginning with the medial anchor. The construct is then tightened and evaluated for stability. Postoperative the patient is immobilized for 6 weeks in a sling to allow for fracture healing. Then the sling is discontinued and the patient is progressed through 6 weeks of passive range of motion protocol while limiting external rotation, and finally the patient completes 6 weeks of active strengthening rehabilitation.