An 80-year-old male diabetic patient with end-stage renal disease was evaluated for decreasing access flow and difficult cannulation of his established percutaneous arteriovenous fistula (pAVF), created 6 months ago with the Ellipsys vascular access system (Avenu Medical, San Juan Capistrano, Calif).1, 2, 3 The patient's ipsilateral hand was cool without distal pulses. Percutaneous transluminal angioplasty of the pAVF anastomosis had only modestly improved access flow because of significant diffuse arterial calcifications. Bilateral distal arterial occlusions were present and the pAVF remained dysfunctional. Further and more aggressive attempts with percutaneous transluminal angioplasty were thought likely to result in severe hand ischemia (steal syndrome); therefore, arterial inflow proximalization was established using a 4- to 7-mm graft (W. L. Gore & Associates, Flagstaff, Ariz) with a lateral axillary artery anastomosis and an end-to-end outflow anastomosis to the mature cephalic vein, ligating the distal pAVF inflow site.
An excellent thrill was recovered immediately over the entire length of the cephalic vein in the arm. Distal circulation improved substantially.
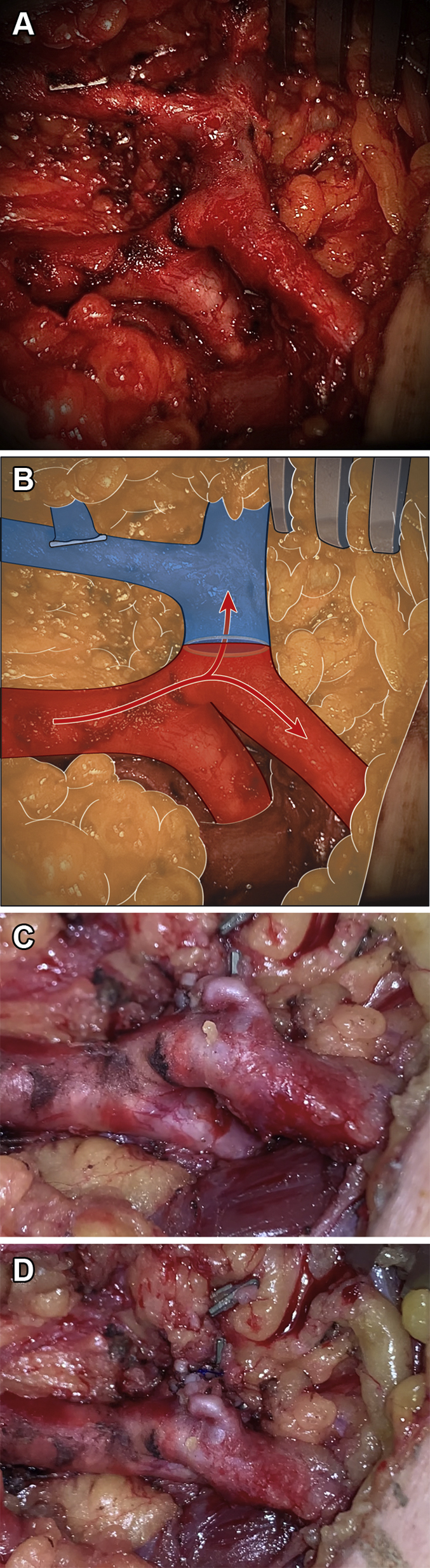
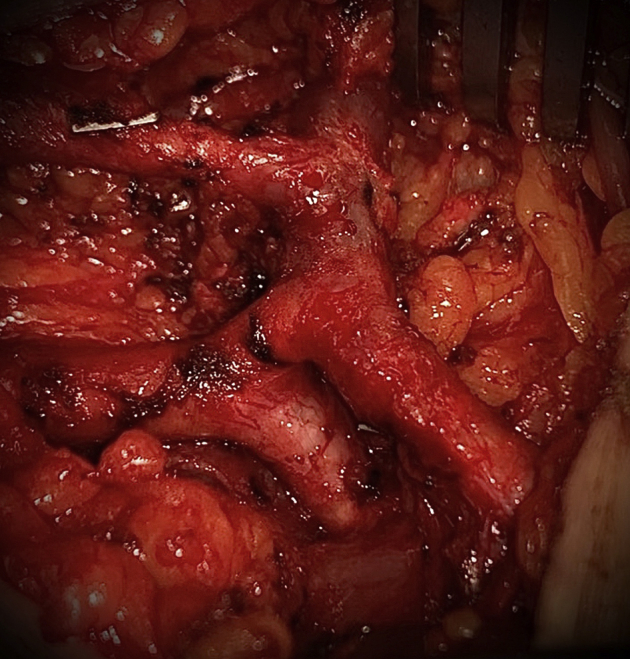
A/Cover, B, and Video 1 show a perioperative view of the percutaneously created Ellipsys anastomosis between the proximal radial artery and perforating vein of the elbow. To our knowledge, this is the first direct visualization of an Ellipsys pAVF anastomosis in a human. The anatomic configuration and natural course of the pAVF are apparent along with the absence of suture or fibrosis, yielding a shape similar to surgical proximal radial artery AVFs described by Jennings et al.4 C (medial view), D (anterior view), and Video 2 show the ligated pAVF anastomosis.
Need for ligation of a pAVF has been a concern of some critics because of the multiple venous branches. This report demonstrates that in the rare case in which ligation is necessary, an Ellipsys pAVF may be easily ligated without consequence or technical challenges. The patient's informed consent was obtained before submission of this manuscript.
Footnotes
Author conflict of interest: A.M. has been paid a consulting fee by Avenu Medical and is on the speakers bureau. A.M. and W.C.J. have shares in Avenu Medical.
The editors and reviewers of this article have no relevant financial relationships to disclose per the Journal policy that requires reviewers to decline review of any manuscript for which they may have a conflict of interest.
Supplementary data
Perioperative view of the percutaneously created Ellipsys anastomosis between the proximal radial artery and perforating vein of the elbow.
Ligated percutaneous arteriovenous fistula anastomosis.
Cover Image.
References
- 1.Mallios A., Jennings W.C., Boura B., Costanzo A., Bourquelot P., Combes M. Early results of percutaneous arteriovenous fistula creation with the Ellipsys Vascular Access System. J Vasc Surg. 2018;68:1150–1156. doi: 10.1016/j.jvs.2018.01.036. [DOI] [PubMed] [Google Scholar]
- 2.Mallios A., Fonkoua H., Allouache M., Boura B. Percutaneous arteriovenous dialysis fistula. J Vasc Surg. 2020;71:1395. doi: 10.1016/j.jvs.2020.01.034. [DOI] [PubMed] [Google Scholar]
- 3.Mallios A., Bourquelot P., Franco G., Fonkoua H., Allouache M., Boura B. Mid-term results of percutaneous arteriovenous fistula creation with the Ellipsys vascular access system, technical recommendations and an algorithm for maintenance. J Vasc Surg. 2020 Apr 7 doi: 10.1016/j.jvs.2020.02.048. [Online ahead of print] [DOI] [PubMed] [Google Scholar]
- 4.Jennings W., Mallios A., Mushtaq Proximal radial artery arteriovenous fistula for hemodialysis vascular access. J Vasc Surg. 2018;67:244–253. doi: 10.1016/j.jvs.2017.06.114. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Perioperative view of the percutaneously created Ellipsys anastomosis between the proximal radial artery and perforating vein of the elbow.
Ligated percutaneous arteriovenous fistula anastomosis.


