Abstract
Objective
The study aims to review the literature regarding abnormalities predisposing to Sudden Cardiac Death (SCD) in young Middle Eastern and African competitive athletes between the years 2009–2019 and aims to assess cardiac pre-participation screening methods.
Methods
A PubMed search was performed in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines. The search targeted articles that reported the prevalence of cardiac abnormalities found in Middle Eastern and African athletes, and it also focused on comparing cardiac screening methods for assessment of athletes.
Results
our studies fell within the inclusion criteria and were included in the study. Results identified a shortage in the literature regarding prevalence rates of SCD in the Middle East and Africa. Additionally, there seems to be a lack of ethnicity-specific cardiac pre-participation screening programs in the region. Nevertheless, the prevalence of SCD-related abnormalities (HCM, ARVC, etc …) ranged from 0.47 to 4.29%. Included studies conveyed only male athletes with no reports on the female athletic population.
Conclusion
The present study highlights a need to develop an efficient cardiac pre-participation screening program specific to Arab and African athletes due to their high false-positive rates in contrast to Caucasian athletes. Significant evidence proves that an adequate cardiac screening program can prevent SCD in young competitive athletes. Therefore, it is imperative that future studies highlight the prevalence of abnormalities directly related to SCD in order to create a valid screening program that can be implemented in the region to mitigate the risk of shocking events.
Keywords: Pre-participation cardiovascular screening, Sudden cardiac death, Sports cardiology, Arab athletes, African athletes
1. Introduction
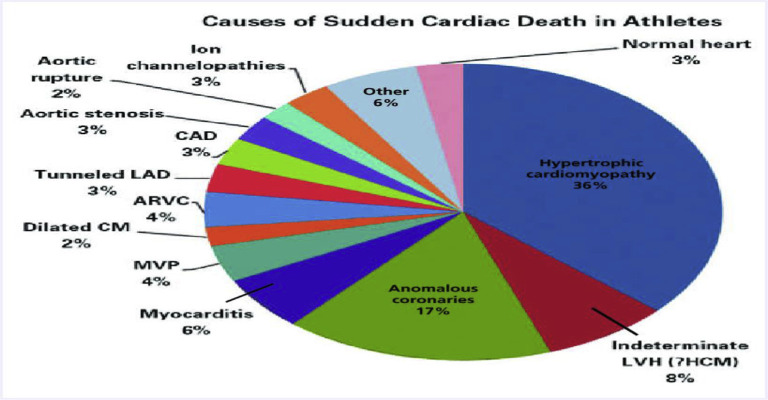
The heart of a competitive athlete is an intriguing phenomenon that portrays the enormous physiologic capabilities of the human heart. It is accompanied by complex structural, functional, and electrical remodelling which occur as a form of adaptation to help athletes improve their physical capabilities [1]. The resultant condition is referred to as the athletic heart syndrome (AHS). AHS is a benign condition that may not pose threats to the athlete, but it can give false reassurance in the sense that the athlete assumes he/she has the condition due to its familiarity in the sports world, but the athlete may actually suffer from an underlying condition that can be life-threatening. Refer to Illustration 1 [in appendix] for some of the most common causes of Sudden Cardiac Death (SCD) in competitive athletes [2].
Illustration 1.
Common causes of sudden cardiac death in athletes.2
Sudden Cardiac Death (SCD) is the most common cause of a non-traumatic death in young athletes. The incidence of SCD is estimated at 0.6/100,000 person-years in young competitive athletes in recent reports [3]. SCD in itself is a traumatic event, both for the athlete whose life has been terminated unexpectedly, and for the potential thousands of viewers who have been shocked by such an event. There is existing evidence that this outcome can be alleviated by adequate cardiac screening programs [4].
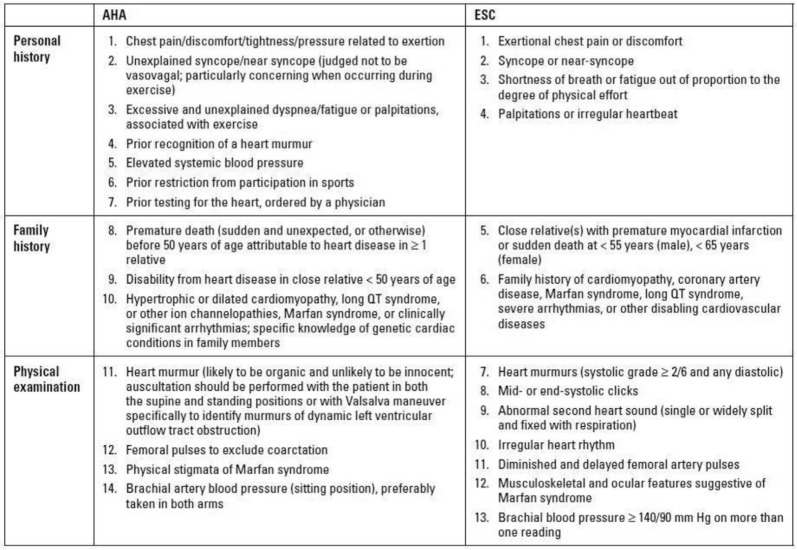
Most screening programs include a history and a physical examination, while other screening programs also include a resting 12-lead electrocardiogram (ECG). Many studies suggest the use of a 12-lead ECG as it is superior in the detection of disease associated with SCD [4]. The American Heart Association (AHA) and American College of Cardiology (ACC) guidelines recommend a 14-part evaluation checklist for young athletes that consists of questions regarding family and personal history, including heart-related symptoms such as fainting or feelings of chest discomfort. Another part of the checklist is the physical examination, including blood pressure measurement as well as auscultation for heart murmurs. Although this evaluation does not include electrocardiography, it is meant to stratify individuals that are at increased risk of SCD and require further evaluation [5]. In contrast to the recommendations in the United States; in 1982, Italy introduced a nationwide systematic pre-participation athletic screening. This pre-participation screening is essentially based on a 12-lead ECG, but also includes family and personal history, along with a physical examination [6]. Following the 25-year Italian experience, these recommendations later formed the basis for the European Society of Cardiology (ESC) consensus statement on pre-participation screening, in the hopes that they would eventually become adopted by the European health regulation system [7]. Refer to Illustration 2 [in appendix] to see the differences between the ESC recommendations and the AHA recommendations for cardiac pre-participation screening in competitive athletes [8].
Illustration 2.
The differences between the ESC recommendations and the AHA recommendations for cardiac pre-participation screening in competitive athletes.7
The existing literature regarding SCD in Middle Eastern and African competitive athletes is not extensive enough to ascertain and highlight the prevalence of SCD-related abnormalities found during routine pre-participation cardiac screening.
Moreover, recent studies enable us to utilize ESC guidelines for the interpretation of ECGs in Middle Eastern athletes as there is no substantial difference in frequency of occurrence of “uncommon” and “ training-unrelated” ECG findings between Arab and Caucasian athletes [8].
1.1. Study Purpose/aim
This literature review will provide researchers and preventive medicine policy makers with up-to-date information concerning the prevalence of SCD and abnormalities linked to developing SCD. These can be detected during routine pre-participation cardiac screening in Middle Eastern and African competitive athletes. The study will help assess the different cardiac screening programs and their respective diagnostic results to aid in prevention. The paper will be a useful resource for future research papers and may serve as a recommendation for Middle Eastern and African sports regulating authorities with a gap in their literature where intervention can be possible.
2. Objectives
To highlight the significance of this topic by evaluating the existing literature on the prevalence of SCD and its related abnormalities.
To evaluate implications of cardiac screening and mitigations of the risk of SCD in young Middle Eastern and African athletes.
To determine the most appropriate cardiac screening test based on evidence.
To summarize the results and provide a basis of discussion for future research and possible interventions to prevent SCD in young Middle Eastern and African athletes.
2.1. Research question
Which cardiac screening methods can be implemented to mitigate the risk of sudden cardiac death in Middle Eastern and African competitive athletes?
3. Methods
3.1. Study Design
The study design is a Systematic Review of studies discussing cardiac screening in Middle Eastern and African competitive athletes. The review was performed according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines [9]. The literature was reviewed in March 2019 in a PUBMED search with the use of Medical Subject Headings (MeSH) terms. Development of the search strategy was performed with the aid of a cardiologist. The initial search strategy included 3 different databases, but due to restricted access, the search was limited to PubMed (MEDLINE) and Google Scholar only. Initially, publication titles and abstracts were screened followed by a full-text reading to determine whether the studies fit the inclusion criteria. The detailed search strategy can be found in the appendix.
3.2. Eligibility Criteria
The articles and studies must have examined Middle Eastern and African competitive athletes using any cardiac pre-participation method with summary results of findings. Papers with a study population of athletes originating from Middle Eastern or African countries were selected for review according to the following criteria:
Original published studies in peer-reviewed journals, in English or Arabic, involving pre-participation cardiac screening in Arab or African competitive athletes.
Study population not restricted to gender, or athletic level, but age restricted to less than 36 years of age.
Articles that involved no less than 100 participants as the sample size.
Articles that included Cardiac pre-participation screening programs and African or Middle Eastern Athletes.
Articles published between January 2009 and March 2019.
Studies were chosen from a ten year period to ensure inclusion of the latest knowledge in the field. The age criteria was set to an upper limit of 36 years of age to conform to the generic age of elite athlete populations in similar studies. The sample size of studies was restricted to no less than 100 athletes to yield more accurate results.
3.3. Exclusion Criteria
Books, Editorials, case reports and reviews.
Studies involving the non-athletic population.
Studies conducted outside the Middle East and Africa.
3.4. Variables
The variables that will be assessed in this research are: sample size, age group, gender, nationalities, different sports, study setting, guidelines used for pre-participation screening, and results yielded from each study respectively.
3.5. Title, Abstract and Article Selection
Publication titles retrieved through the search strategy were reviewed independently by the authors (YH, UB). All titles unquestionably irrelevant to this study were excluded (e.g. “Aspirin to Prevent Sudden Cardiac Death in Athletes with High Coronary Artery Calcium Scores.” and “Performance of the BMJ learning training modules for ECG interpretation in athletes.”) during the first step of the screening process.
Additionally, titles that were relevant (e.g. “Pre-participation musculoskeletal and cardiac screening of male athletes in the United Arab Emirates.”) or vague (e.g. “Screening athletes for cardiovascular disease in Africa: a challenging experience.”) were included at this point of the screening process.
Furthermore, abstracts and full texts were retrieved and assessed for suitability using the aforementioned eligibility and exclusion criteria.
Finally, all the data was collected from the studies that had been rigorously screened using the above methodology.
4. Results
4.1. The Literature Search
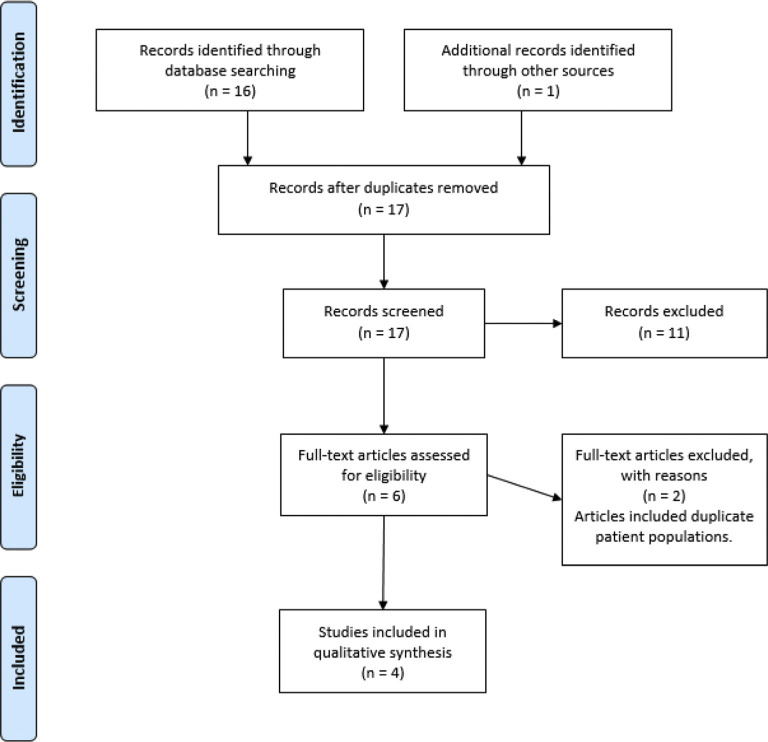
The PubMed Search strategy yielded a total of 16 titles. 1 paper was identified through Google Scholar. Consequently, after title and abstract screening, the total number of papers was reduced to 6. Finally, after a full text screening for eligibility, 4 original articles met the selection criteria. A detailed overview of the screening process is presented in Fig. 1 in appendix. 2 articles were excluded from the review as they contained duplicate patient populations.
Figure 1:
The PRISMA flow diagram describe the literature searching process.
4.2. Search Summary
Four studies met the eligibility criteria and were included in the review. No studies meeting the inclusion criteria have been published between 2009 and 2010 or 2016–2019. Table 1 summarizes all the included studies published over a 10-year interval between 2009 and 2019. Studies are listed in chronological order. 2 Studies were conducted in Qatar, 1 study was conducted in the United Arab Emirates (UAE) and 1 study was conducted in Gabon [10–13]. Both studies conducted in Qatar identified athletes from many different nationalities, whereas the studies conducted in Gabon and the UAE outlined athletes from a local nationality respectively. Guidelines used to interpret ECG findings are included in Table 1.
Table 1.
Overview of studies assessing competitive athletes who have undergone cardiac pre-participation screening in Middle Eastern, and African countries 2011–2018. Studies are grouped by country and are listed in chronological order.
| Author (year) | Country | Study Setting | Sample Size | (Age -Group) Mean Age (Years) | Gender Distribution | Sample Population Nationalities | Sports included in the study | Guidelines used for pre-participation screening of competitive athletes | SCD-associated abnormality (WPW, ARVC, HCM, DCM, long QT syndrome) |
|---|---|---|---|---|---|---|---|---|---|
| Wilson MG et al. (2011)10 | Qatar | Sports Hospital | 1100 (West Asian & African) | (12–35) 22.6 ± 6 years | 100% ♂ | Gulf States (QAT, BHR, OM, AE, KWT, YEM, SA) Middle Eastern Countries (EGY, PSE, SYR, JO, LBN, IRQ) African Countries (SDN, SOM, GHA, NGA, CMR, SEN, ET) Others (USA, CAN, AUS) | 17 sporting disciplines (Football, Basketball, Tennis, Handball, & Volleyball) | 2010 European Society of Cardiology (ESC) Recommendations | 7 athletes [0.64%] - (95% CI (0.31% –1.31%)) WPW (n = 2, 1 WA & 1 B), ARVC (n = 1, B), long QT (n = 1, WA), HCM (n = 3, 2 WA & 1 B) |
| Schmied C et al. (2013)11 | Gabon | Organized Screening program | 210 | (18–22) 18.6 years | 100% ♂ | Gabon | Football | 2010 European Society of Cardiology (ESC) Recommendations | 9 athletes [4.29%] - (95% CI (2.27% –7.95%)) Long QT (n = 5), WPW (n = 3), HCM (n = 1) All African |
| Maffulli N et al. (2014)12 | UAE | Sports Club | 230 | (14–35) 20.68 ± 5.22 years | 100% ♂ | United Arab Emirates | Football, Swimming, Cycling, Handball, Basketball | Lausanne Recommendations 2010 European Society of | 5 athletes [2.17%] – (95% CI (0.93% –4.98%)) WPW (n = 2), A- FIB (n = 1), long QT (n = 1), ARVC (n = 1) All Arab |
| Riding NR et al. (2015)13 | Qatar | Sports Hospital | 2115 (West Asian & African) | (NR) 23.23 ± 5.26 years | 100% ♂ | Gulf States (QAT, BHR, OM, AE, KWT, YEM, SA) Middle Eastern Countries (EGY, MAR, TUN, DZA, PSE, JO, LBN) African Countries (SDN, SOM, GHA, NGA, CMR, SEN, ET, TCD, CIV) Caribbean Countries (TTO, JAM, CUB) Others (BRA, COL, ECU, URY, North America, South America, Mainland Europe, AUS) | Football, Handball, Volleyball, Basketball | 2010 European Society of Cardiology (ESC) Recommendations Seattle Criteria Refined Criteria | 10 athletes [0.47%] - (95% CI (0.26% –0.86%)) HCM (n = 7, 5 B & 2 WA), WPW (n = 3, WA) |
Notes. ♂ = males, NR = Not Reported.
Abbreviations: QAT = Qatar, BHR= Bahrain, OM= Oman, AE = United Arab Emirates, KWT= Kuwait, YEM= Yemen, SA= Kingdom of Saudi Arabia, EGY = Egypt, PSE= Palestine, SYR= Syria, JO = Jordan, LBN = Lebanon, IRQ= Iraq, SDN= Sudan, SOM= Somalia, GHA = Ghana, NGA= Nigeria, CMR= Cameroon, SEN= Senegal, ET = Ethiopia, USA= United States of America, CAN= Canada, AUS = Australia, MAR = Morocco, TUN = Tunisia, DZA = Algeria, TCD = Chad, CIV= Ivory Coast, TTO = Trinidad and Tobago, JAM = Jamaica, CUB= Cuba, BRA= Brazil, COL= Columbia, ECU = Ecuador, URY= Uruguay, WA=West Asian (Arab), B= Blac
4.3. Sample Characteristics (Age and Gender)
Although it was not part of the exclusion criteria, none of the studies reported any information on the female population. Therefore, all four studies reported data in males only (100%). The trend in age selection ranged from 12 to 35 years across all studies. One study only had data on a younger population ranging from 18 to 22 years. All four papers mentioned the mean age and age group, except one paper which did not report the age range of the sample.
4.4. Sample Size and Population
The range of sample sizes was between 210 and 2491 across all studies. Two studies presented data from smaller sample sizes comprising of 210 and 230 athletes, whereas the other two studies presented data from larger sample sizes involving 1220 and 2491 athletes respectively. The two studies with smaller sample sizes took place in Gabon and UAE, and included athletes originating from the country where the study took place [11],[12]. Meanwhile, the two studies with larger sample sizes took place in Qatar, and included athletes of diverse origin from countries within the Gulf States, the Middle East, Africa, Caribbean countries, and others [10],[13]. The rate of positive findings of a SCD-related abnormality varied between 0.47% and 4.29% amongst all studies.
4.5. Study Setting and Focus
Two (50%) of the studies included were conducted in Qatar, one (25%) in Gabon and one (25%) in the UAE. One study was limited to 1 sport (Football). The remaining three studies presented samples from various sports including but not limited to Football, Basketball, Handball, and Volleyball. Three studies took place in athletic settings (sports hospital or sports club) [10],[12],[13]. One study ran within an organized screening program with the aid of local physicians [11].
4.6. Data Collection
4.6.1. Guidelines for Screening
All the studies included assessed the results of the cardiovascular screening using the 2010 European Society of Cardiology (ESC) recommendations (100%). In addition, two of the four studies referred to additional recommendations for interpretation. One study by Maffulli et al. added the Lausanne recommendations for interpretation of UAE National athletes and exhibited false-positive rates at (20.4%) [12].
On the other hand, the other study by Riding et al. highlighted the importance of using the 2014 refined criteria when screening to reduce the number of false-positives to 3.6% in Arab athletes (vs 19.1% using ESC guidelines and 9.7% using Seattle criteria) and 10% in African athletes (vs 29.9% using ESC guidelines and 16.6% using Seattle Criteria) [13].
4.6.2. Support in Assessment
The study done in the UAE by Maffulli et al. provided questionnaires in the Arabic language, and the interpretation was approved by the respective local health authority [12]. The two studies based in Qatar had athletes completing questionnaires with the assistance of French-speaking, Arabic-speaking, and English-speaking cardiac nurses [10],[13]. The study based in Gabon by Schmied et al. ensured the completion of the questionnaires with the aid of local physicians [11].
4.7. Prevalence
4.7.1. Cardiac Family History of SCD
Prevalence rates of SCD in a young relative were reported in three studies. Interestingly, Maffulli et al. indicated that 2 Arab athletes had a positive family history of SCD in a relative before the age of 35 years [12]. However, another study by Wilson et al. presented 17 west Asian and 14 black athletes with a positive family history of SCD in a young first-degree family relative [10]. Finally, the study by Schmied et al. points to 36 (17%) African athletes with a family history of sudden or unexplained death [11].
4.7.2. History of Syncope or Chest Discomfort
Prevalence rates of a positive history of syncope or chest discomfort were reported in three studies. The study by Schmied et al. indicated that 19 (9%) African athletes had atypical chest discomfort that was not specifically related to exercise, and none of the athletes reported any history of syncope [11]. Notably, the study by Maffulli et al. showed a positive history of syncope in 6 (2.6%) Arab athletes, and a history of some sort of chest discomfort (palpitations, shortness of breath, or chest pain) in 8 (3.8%) Arab athletes [12]. The study by Wilson et al. reported that 8 (0.66%) athletes had some sort of cardiovascular symptoms at rest or during physical activity. Although this study did not report any rates of a history of syncope, it did indicate that one football player of West Asian origin had a positive history of impact syncope during exercise [10].
4.7.3. SCD-associated Abnormality Rates
All four studies included in the review reported rates of conditions commonly known to be associated with Sudden Cardiac death including: Wolff-Parkinson-White syndrome (WPW), arrhythmogenic right ventricular cardiomyopathy (ARVC), hypertrophic cardiomyopathy (HCM), etc.
Prevalence ranged between 0.47% and 4.29% across all four studies. The first study by Wilson et al. highlighted seven (0.63%) athletes (4 West Asian and 3 Black) with an SCD-associated abnormality. One Arab athlete and one African athlete had WPW syndrome. Two Arab athletes and One African Athlete with HCM. One African athlete with ARVC and one Arab athlete with Long QT syndrome [10]. Remarkably, the second study by Schmied et al. indicated that nine (4.29%) African athletes were found to have an SCD-related abnormality, five of which had Long QT syndrome, three of which had WPW syndrome, and one was diagnosed with HCM upon echocardiography [11]. The third study by Maffulli et al. pointed out that five (2.17%) Arab athletes had an SCD-related abnormality. Two of the athletes had WPW, one athlete had Atrial Fibrillation (A-FIB), one athlete with Long QT syndrome and one athlete with ARVC [12]. The final study by Riding et al. reported ten (0.47%) athletes with an SCD-related abnormality. Five black and two Arab athletes were diagnosed with HCM, and three Arab athletes were diagnosed with WPW syndrome [13]. Refer to Table 1 [in appendix] for an overview on the results of this paper.
5. Discussion
Sudden Cardiac Death (SCD) in young competitive athletes is mainly due to congenital heart diseases, mainly Hypertrophic Cardiomyopathy [14]. Therefore, it is crucial to highlight any conditions that may predispose to developing an SCD event in order to increase prevention.
The present scientific evidence has established that pre-participation screening including a history, a physical examination, and an electrocardiography comprises the ideal screening method that can help in reducing the risk of SCD in young athletes. ECGs greatly improve the sensitivity of the pre-participation examination (PPE) with reasonable specificity and excellent negative predictive values [15].
5.1. Interpretation of Major Findings
This paper systematically reviewed the literature on the prevalence of cardiac abnormalities detected during cardiac pre-participation screening of Middle Eastern and African athletes. The paper also assessed the efficacy of different guidelines that could be implemented to mitigate the risk of sudden cardiac death (SCD) in young competitive athletes.
Findings were consistent across all four studies assessed in regards to study design (cross-sectional studies with ECG interpretations on pathological abnormalities), gender distributions, sampled populations, as well as age ranges (male competitive athletes below the age of 35). However, the results exhibited slight variations in regards to prevalence rates of SCD-related pathological abnormalities ranging from 0.47% to 4.29%.
Both studies conducted in Qatar occurred in the same setting, however there were big differences in sample size as well as the guidelines used to interpret findings. The first study in Qatar by Wilson et al. [10] examined 1220 competitive athletes (800 West Asian, 300 black, and 120 Caucasian) with 135 West Asian (Arab) controls. This study observed high levels of false-positives in the black population (31%) vs. the West Asian population (17%), and these results were extracted by utilizing the 2010 ESC Recommendations for screening. The study also highlighted that having a black/African heritage is an independent predictor to discovering uncommon ECG findings, particularly when compared to West Asians (2.6 times greater in Africans) and 3.5 times greater in Africans when compared to Caucasians. The prevalence of SCD-related abnormalities in Arab and African athletes in this study was 0.63% with 4 West Asian athletes and 3 Black athletes, and this study suggests that the prevalence of a cardiac disease in black athletes was two times higher than that of West Asian athletes (1% vs 0.5%).
The other study performed in Qatar by Riding et al. [13] observed 2491 competitive athletes (1367 Arab, 748 Black, and 376 Caucasian). This study managed to reduce the rate of false-positives after comparing three different sets of guidelines to interpret ECG's in their diverse sample population. The false-positive rates (FPR) when using the ESC recommendations in the Arab athletes were at 18.8%, compared to 29.1% in Black athletes and 18.6% in Caucasians. On the contrary, the FPR with the use of the Seattle Criteria were reduced to 9.4% in Arab athletes, 15.8% in Black athletes and 8.5% in Caucasians. Finally, the FPR when using the Refined Criteria indicated further reduction in the Arab athletes to 3.3%, compared to 9.2% in Black athletes, and 2.1% in Caucasians. These results indicate that ECG interpretations by the 2014 Refined Criteria are superior to both the 2013 Seattle Criteria as well as the 2010 ESC Recommendations. This was made evident by the fact that the 2014 Refined Criteria managed to significantly decrease the number of false-positives in a cohort of Arab and African athletes all whilst being 100% sensitive in SCD-related cardiac pathology discovery. The prevalence of SCD-related abnormalities in Arab and African athletes identified in this study was 0.47% with 5 West Asian athletes and 5 African athletes. This study suggests that the prevalence of HCM in black athletes is almost five times greater than in Arab athletes (0.9% vs 0.2%) [13]. This is relevant as HCM has been recognized to be the leading cause of SCD in young competitive athletes suggesting that Black athletes are at a higher risk of developing SCD [14],[16].
In another study by Schmied et al., [11] 210 Male Gabonian Football players were assessed. The sample population from this study was different than the previous two studies in terms of the size and nationality of players, as this study only considered a relatively small amount of Gabonian nationals. In contrast to other studies, this study included routine echocardiography assessment of all the athletes participating. This study interpreted ECGs with the use of the 2010 ESC Recommendations and emphasized that abnormal ECG patterns unrelated to training were twice as high in African athletes in comparison to Caucasian athletes in two studies (12% vs 5–7%). These results confirm that ECG interpretations require a better understanding of race-related ECG differences when screening large multi-ethnic populations in comparison to homogenous Caucasian populations [17],[18]. The prevalence of SCD-related abnormalities in these African athletes was estimated at 4.29% with 5 identified cases of Long QT syndrome, 3 known cases of WPW, and 1 case of HCM [11].
Maffulli et al. [12] inspected 230 Male athletes, and all the athletes were of Arab origin. The study used the Lausanne recommendations for presenting the results of pre-participation screening in which a personal and family history are obtained, as well as a physical examination and a 12-lead electrocardiogram [19]. ECG interpretations came according to the 2010 ESC recommendations and the false positive rate of ECGs was 18.3%. This study highlighted that their findings were comparable to findings in a study by Baggish et al. [20] which assessed collegiate athletes with an electrocardiography false-positive rate of 16.9% and an overall false-positive rate of 20.4%. The prevalence of SCD-related abnormalities in these Arab athletes was approximately 2.17% with 5 athletes recognized being at risk, 2 of them were identified with WPW, 1 case of Long QT syndrome, 1 case of Atrial Fibrillation (A-FIB) and 1 case of ARVC. This study implied that the use of the Lausanne recommendations in the respective country where the study took place would favour ECG implementation. It also recommended that some improvements must be made in order to decrease the rate of false-positives [12].
One study by Williams et al. [21] indicated that the use of ECG for cardiovascular pre-participation screening outperformed the AHA 14-point evaluation in high school athletes, and this study suggests that the consensus-derived questionnaires on history are not adequate to be the primary tool in cardiovascular screening. Interestingly another study by Rao et al. pointed out that the approach in American pre-participation screening is ineffective in detecting and preventing the risk of SCD [22]. Refer to Table 2 [in appendix] for an overview of the False-Positive Rates ranging across the studies.
Table 2.
False Positive Rates.
| Study | False-Positive Rates in each population with guidelines used for ECG interpretations | |||
|---|---|---|---|---|
| Arabs | Africans | Other | Guidelines used
|
|
| Wilson MG et al. (2011)10 | 17% | 31% | 2010 ESC Recommendations | |
| Schmied C et al. (2013)11 | 2010 ESC Recommendations | |||
| Maffulli N et al. (2014)12 | 18.3% | 2010 ESC Recommendations | ||
| Riding NR et al. (2015)13 | 18.8% | 29.1% | 18.6% in Caucasians | 2010 ESC Recommendations |
| 9.4% | 15.8% | 8.5% in Caucasians | 2013 Seattle Criteria | |
| 3.3% | 9.2% | 2.1% in Caucasians | 2014 Refined Criteria | |
5.2. Factors for Development of Sudden Cardiac Death
As mentioned in the introduction, there are many predisposing causes to SCD in young competitive athletes. The most common causes in each of the studies discussed were highlighted with their corresponding prevalence rates. A retrospective study by Maron et al. [23] judged that the greatest proportion of SCD events in athletes were due to cardiovascular causes. HCM was the most common in their study with a 36% occurrence. ARVC, Long QT syndrome, WPW and DCM were also amongst the common factors, all of which could have been identified through routine pre-participation cardiovascular screening.
The Demographics in this study indicated that the three main sports with highest prevalence rates of SCD were American Football, followed by Basketball, and then Soccer. These rates however could not be generalized to all populations due to variations with regards to native sports in different countries. A study by Borjesson et al. [24] highlighted that Cardiovascular SCD in male athletes was estimated to be 2.4 times higher among African Americans when compared to White (Caucasian) athletes. The Qatari Experience focused on Football as it is the most popular sport in the region, therefore distinctions between studies must be made in terms of sport played in order to correctly assess the prevalence of SCD associated with each individual sport [10].
Although not evident in the papers examined in this study, the incidence of SCD is estimated to be higher in male athletes when compared to female athletes after taking into account ethnicity and choice of sport played [23–25].
5.3. Implications for Public Health Practitioners/ Researchers
The current review aimed to provide researchers and sports medicine policy makers with the prevalence rates of abnormalities detected during pre-participation screening. The abnormalities looked at in these studies are ones that have been directly associated with developing Sudden Cardiac Death. Recommendations for future research would be to create new original data in different countries in Middle Eastern and African regions, this would allow discussions to be more specific to Arab and African populations. Hopefully, researchers will also begin to include the female population as a part of their studies since the female sports world is on the rise and because there appears to be a shortage of data regarding females in these regions especially.
Furthermore, since SCD is a traumatic event that can affect thousands of athletes in the Middle East and Africa as well as millions of observers and sports fans, measures must be taken by public health professionals and sectors to develop the most efficacious screening program for these athletes. Based on this study, the 2014 Refined Criteria seems to be the most efficient guide in identifying all athletes with cardiac pathology. These criteria seem to have the best results in Arab and Black athletes when compared to other criteria used in other studies [13].
5.4. Strengths, Limitations, & Generalisability
This is the first study in the Arab region to review the literature on the prevalence of abnormalities directly linked to SCD in Middle Eastern and African young competitive athletes. One of the strengths of this study is that it comprised of studies from different regions in the Arab world that included different populations, thus giving an idea on individual differences between countries within similar geographical areas. The main limitation of this study is the access to only two databases (MEDLINE & Google Scholar) which might have possibly decreased the number of yielded searches, hence not detecting some articles which may fall under the inclusion criteria. Another limitation is the fact that only four studies fell under the eligibility criteria, thus reducing potential for generalizability. This clearly depicts the gap in the literature regarding pre-participation screening in athletes in this region, and even though the paucity of the literature complicates the ability to draw significant conclusions, this enables the review to portray the necessity of in-depth studies evaluating pre-participation screening in Middle Eastern and African athletes; as this will provide enough information to draw significant conclusions as those drawn in other major studies (e.g. Corrado D et al. [5]), and be able to apply these measures on young athletes in the region. Furthermore, the review can serve as a reference point of the current situation, from which we can build further necessary investigations targeting major deficiencies in the literature in this region, the first being the evaluation of female athletes, which were not analyzed in the studies included in this review.
6. Conclusion
Accurate measurements of prevalence rates of these SCD-related abnormalities are essential for planning the most useful screening program for Middle Eastern and African athletes and this has been demonstrated to be efficacious in countries with a rigorous pre-participation screening program. There is a vital need to improve the methodology on reporting prevalence rates of SCD-related abnormalities so that there can be comparisons between studies in different countries within the region. As there appears to be a paucity in the literature surrounding this topic in the region, further research is required in order to better understand the extent of SCD-related abnormalities in the Middle East and Africa with the hopes of preventing traumatic experiences. Through this, the authors are aiming to elucidate the importance of pre-participation screening in middle-eastern athletes, which until now hasn't been prioritized, as a measure to safeguard our numerous young athletes; and while the yield of saving lives may not be as high compared to other public health measures, it provides a solid safety net for athletes in our region.
Key messages.
What is already known about this subject?
Individual prevalence rates of cardiac abnormalities linked to Sudden Cardiac Death (SCD) in Middle Eastern and African competitive athletes.
Pre-participation cardiac screening reduces the risk of developing SCD.
What does this study add?
First literature review regarding prevalence rates of abnormalities related to SCD detected during cardiac pre-participation screening in the Middle East and Africa.
Summarizing the literature on the most efficacious cardiac pre-participation screening method on West Asian and African athletes.
How might this impact on public health practice?
The paper provides current data on literature of the prevalence of cardiac abnormalities discovered during screening that are major risk factors to developing SCD in Middle Eastern and African competitive athletes.
The paper fills the current gaps in the literature by recommending the ideal method of cardiac screening, which may help to prevent SCD in competitive athletes in the Middle East and Africa, as well as serving as a useful resource for future research papers in the region.
Acknowledgments
Dr. Osama Hallak for critically reviewing the study manuscript.
Abbreviations
- SCD
Sudden Cardiac Death
- WPW
Wolff-Parkinson-White syndrome
- ARVC
Arrhythmogenic right ventricular cardiomyopathy
- HCM
Hypertrophic Cardiomyopathy
- DCM
Dilated Cardiomyopathy
- A-FIB
Atrial Fibrillation
- FPR
False Positive Rates
- PPE
Pre-Participation Examination
- AHS
Athletic Heart Syndrome
- ECG
Electrocardiogram
- AHA
American Heart Association
- ACC
American College of Cardiology
- ESC
European Society of Cardiology
- UAE
United Arab Emirates
Appendix
Search Strategy
(((“sudden cardiac death”[Mesh]) AND “screening”[Mesh]) AND “athletes”[Mesh]) AND (“Africa”[Mesh] OR “middle east”[Mesh] OR “
UAE”[Mesh] OR “Saudi Arabia”[Mesh] OR “Bah-rain”[Mesh] OR “Kuwait”[Mesh] OR “Qatar”[Mesh] OR “Oman”[Mesh] OR “Syria”[Mesh] OR “Pales-tine”[Mesh] OR “Jordan”[Mesh] OR “IRAQ”[Mesh] OR “SUDAN”[Mesh] OR “Libya”[Mesh] OR “Tunisia”[Mesh] OR “Lebanon”[Mesh]).
Disclosure of funding
For this type of study, funding is not required.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Ethical clearance
The institutional ethical committee (IRB) had approved the study.
Declaration of Competing Interest
The authors declare that they have no conflict of interest.
References
- 1.Prior DL, La Gerche A. The athlete's heart. Heart. 2012;98(12):947–55. doi: 10.1136/heartjnl-2011-301329. [Internet].Available from: https://heart.bmj.com/content/98/12/947. [DOI] [PubMed] [Google Scholar]
- 2.Saqib Ghani, Sanjay Sharma, Maron BJ, Doerer JJ, Haas TS, Tierney DM, et al. Preparticipation cardiovascular screening in athletes: when and how?. Cardiovascular Medicine. 15. 7-13. 2012;119(8):1085–92. Sudden Deaths in Young Competitive Athletes. Circulation. [Google Scholar]
- 3.Harmon KG, Zigman M, Drezner JA. The effectiveness of screening history, physical exam, and ECG to detect potentially lethal cardiac disorders in athletes: a systematic review/ meta-analysis. J Electrocardiol [Internet] 2015;48(3):329–38. doi: 10.1016/j.jelectrocard.2015.02.001. [DOI] [PubMed] [Google Scholar]
- 4.Screening young athletes for heart disease [Internet] 2015 Available from: www.heart.org. https://www.heart.org/en/news/2018/05/01/screening-young-athletes-for-heart-disease.
- 5.Corrado D, Basso C, Pavei A, Michieli P, Schiavon M, Thiene G. Trends in sudden cardiovascular death in young competitive athletes after implementation of a pre-participation screening program. JAMA [Internet] 2006;296(13):1593. doi: 10.1001/jama.296.13.1593. [DOI] [PubMed] [Google Scholar]
- 6.Corrado D, Pelliccia A, Bjørnstad HH, Vanhees L, Biffi A, Borjesson M, et al. Cardiovascular pre-participation screening of young competitive athletes for prevention of sudden death: proposal for a common European protocol. Eur Heart J. 2005;26(5):516–24. doi: 10.1093/eurheartj/ehi108. [DOI] [PubMed] [Google Scholar]
- 7.Lithwick DJ, Fordyce CB, Morrison BN, Nazzari H, Krikler G, Isserow S, et al. Pre-participation screening in the young competitive athlete: international recommendations and a Canadian perspective. Br Columbia Med J. 2016;58(3):145–51. Available from: https://www.bcmj.org/articles/pre-participation-screening-young-competitive-athlete-international-recommendations-and#a8. [Google Scholar]
- 8.Riding NR, Salah O, Sharma S, Carr e F, George KP, Farooq A, et al. ECG and morphologic adaptations in Arabic athletes: are the European Society of Cardiology's recommendations for the interpretation of the 12-lead ECG appropriate for this ethnicity? Br J Sports Med. 2014;48(15):1138–43. doi: 10.1136/bjsports-2012-091871. Internet. [DOI] [PubMed] [Google Scholar]
- 9.Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting Items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7):e1000097. doi: 10.1371/journal.pmed.1000097. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Wilson MG, Chatard JC, Carre F, Hamilton B, Whyte GP, Sharma S, et al. Prevalence of electrocardiographic abnormalities in West-Asian and African male athletes. Br J Sports Med. 2012;46(5):341–7. doi: 10.1136/bjsm.2010.082743. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Schmied C, Di Paolo FM, Zerguini AY, Dvorak J, Pelliccia A. Screening athletes for cardiovascular disease in Africa: a challenging experience. Br J Sports Med. 2013;47(9):579–84. doi: 10.1136/bjsports-2012-091803. [DOI] [PubMed] [Google Scholar]
- 12.Alattar A, Ghani S, Mahdy N, Hussain H, Maffulli N. Pre-participation musculoskeletal and cardiac screening of male athletes in the United Arab Emirates. Translat Med @ UniSa. 2014;9:43–9. Available from: https://www.ncbi.nlm.nih.gov/pubmed/24809035. [PMC free article] [PubMed] [Google Scholar]
- 13.Riding NR, Sheikh N, Adamuz C, Watt V, Farooq A, Whyte GP, et al. Comparison of three current sets of electrocardiographic interpretation criteria for use in screening athletes. Heart. 2015;101(5):384–90. doi: 10.1136/heartjnl-2014-306437. Heart (British Cardiac Society). BMJ Publishing Group. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Maron BJ, Epstein SE, Roberts WC. Causes of sudden death in competitive athletes. J Am Coll Cardiol. 1986;7(1):204–14. doi: 10.1016/s0735-1097(86)80283-2. [DOI] [PubMed] [Google Scholar]
- 15.Alattar A, Maffulli N. The validity of adding ECG to the preparticipation screening of athletes an evidence based literature review. Translat Med @ UniSa. 2015;11:2–13. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4309649/#b9-tm-11-02. [PMC free article] [PubMed] [Google Scholar]
- 16.Maron BJ, Shirani J, Poliac LC, Mathenge R, Roberts WC, Mueller FO. Sudden death in young competitive athletes. Clinical, demographic, and pathological profiles. J Am Med Assoc. 1996;276(3):199–204. [PubMed] [Google Scholar]
- 17.Corrado D, Basso C, Schiavon M, Thiene G. Screening for hypertrophic cardiomyopathy in young athletes. N Engl J Med. 1998;339(6):364–9. doi: 10.1056/NEJM199808063390602. [DOI] [PubMed] [Google Scholar]
- 18.Pelliccia A, Culasso F, Di Paolo FM, Accettura D, Cantore R, Castagna W, et al. Prevalence of abnormal electrocardiograms in a large, unselected population undergoing pre-participation cardiovascular screening. Eur Heart J. 2007;28(16):2006–10. doi: 10.1093/eurheartj/ehm219. [DOI] [PubMed] [Google Scholar]
- 19.Bille K, Figueiras D, Schamasch P, Kappenberger L, Brenner JI, Meijboom FJ, et al. Sudden cardiac death in athletes: the Lausanne recommendations. Eur J Cardiovasc Prev Rehabil. 2006;13(6):859–75. doi: 10.1097/01.hjr.0000238397.50341.4a. [DOI] [PubMed] [Google Scholar]
- 20.Baggish AL, Hutter AM, Wang F, Yared K, Weiner RB, Kupperman E, et al. Cardiovascular screening in college athletes with and without electrocardiography: a cross-sectional study. Ann Intern Med. 2010;152(5):269–75. doi: 10.7326/0003-4819-152-5-201003020-00004. [DOI] [PubMed] [Google Scholar]
- 21.Williams EA, Pelto HF, Toresdahl BG, Prutkin JM, Owens DS, Salerno JC, et al. Performance of the American heart association (AHA) 14-point evaluation versus electrocardiography for the cardiovascular screening of high school athletes: a prospective study. J Am Heart Asso. 2019;16.8(14) doi: 10.1161/JAHA.119.012235. Available from: https://www.ahajournals.org/doi/10.1161/JAHA.119.012235. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Rao AL, Standaert CJ, Drezner JA, Herring SA. Expert opinion and controversies in musculoskeletal and sports medicine: preventing sudden cardiac death in young athletes. Arch Phys Med Rehabil. 2010;91(6):958–62. doi: 10.1016/j.apmr.2010.02.006. [DOI] [PubMed] [Google Scholar]
- 23.Maron BJ, Haas TS, Ahluwalia A, Murphy CJ, Garberich RF. Demographics and epidemiology of sudden deaths in young competitive athletes: from the United States national registry. Am J Med. 2016;129(11):1170–7. doi: 10.1016/j.amjmed.2016.02.031. [DOI] [PubMed] [Google Scholar]
- 24.Borjesson M, Pelliccia A. Incidence and aetiology of sudden cardiac death in young athletes: an international perspective. Br J Sports Med. 2009;43(9):644–8. doi: 10.1136/bjsm.2008.054718. [DOI] [PubMed] [Google Scholar]
- 25.Harmon KG, Asif IM, Klossner D, Drezner JA. Incidence of sudden cardiac death in national collegiate athletic association athletes. 2011;123(15):1594–600. doi: 10.1161/CIRCULATIONAHA.110.004622. [DOI] [PubMed] [Google Scholar]