Abstract
Background
As the more commonly used ilioinguinal approach is extensive and associated with complications arising from the dissection along the inguinal canal, we attempt to evaluate the efficacy of the modified Stoppa approach as an alternative in the operative management of acetabular fractures.
Methods
Twenty-three patients with acetabular fractures, were operated by the modified Stoppa approach. Fractures were classified; operative time and blood loss were recorded; the radiological and clinical outcomes were prospectively analysed. We analysed the radiological results according to the criteria of Matta and the clinical results by the Merle d’Aubigne and Postel score with a mean follow up of 15.13 months.
Results
The clinical outcomes were excellent or good in nineteen cases, fair and poor in two patients each. In eighteen of our cases the reduction was anatomic, imperfect in two cases, and poor in three cases. The mean pre-operative displacements on axial, sagittal and coronal NCCT sections were 3.8, 3.1 and 3.6 mm, respectively; and mean post-operative displacements were 0.2, 0.3 and 0.2 mm, respectively. The mean pre-operative and post-operative fracture gap were 12.8 mm and 1.1 mm respectively.
Conclusions
Minimizing perioperative morbidity and simultaneously allowing access for anatomical reduction are the major benefits of the approach. The modified Stoppa approach can substitute the ilioinguinal approach for the surgical fixation of acetabular fractures.
Keywords: Modified stoppa approach, Acetabular fractures, Anterior column, Acetabulum
1. Introduction
Various surgical approaches are in use for the operative management of acetabular fractures. These are classified as either limited or extensile based on the degree of exposure needed, or anterior and posterior depending on the requirement of exposure. The complications associated with these approaches adversely affect the functional outcome.1 Identifying the best possible approach for these fractures is a major orthopaedic challenge.
Ever since the original illustration by Letournel2 in 1961, the ilioinguinal approach has been preferred for anterior acetabular fracture fixation. In 1994, the Stoppa approach, an intra-pelvic approach used for inguinal hernia surgeries, was modified by Cole, Bolhofner3 and Hirvensalo et al.4 for the surgical management of pelvic and acetabular fractures. This was often used alongside the lateral window of the ilioinguinal approach.
As the ilioinguinal approach has been used more commonly, its outcomes have been extensively reported.2,5 Nowadays, the modified Stoppa approach is being used with great success for anterior acetabular fractures and its components. The proponents of the modified Stoppa approach claim an easier anatomic dissection and a better visualisation of the quadrilateral plate and pelvic brim.6,7 However, the reported evidence of the approach from our part of the world is still lacking.
The purpose of our study, therefore, was to evaluate the efficiency of the approach by analysing the clinical and radiological outcomes in patients undergoing internal fixation for acetabular fractures.
2. Methods and methodology
This study was conducted at an Indian tertiary care hospital with approval of the institutional ethical committee (Reference no: IECPG-692/January 19, 2017). We prospectively evaluated the patients clinically, functionally and radiologically, with a mean follow-up of 15.13 months (range: 6 months–24 months). A total of twenty-five consecutive cases with acetabular fractures meting the inclusion criteria were enrolled in the study from February 2017 to October 2018. Two cases were lost to follow up.
Patients aged between 18 and 65 years with (Judet and Letournel8) all simple and complex fracture types including anterior wall and anterior column fractures, transverse fractures, associated both-column fractures and anterior column with posterior hemi-transverse fractures) were included.
Exclusion criteria included acetabular fractures with isolated posterior wall or column involvement, posterior column with posterior wall fractures, T-type fractures with mainly posterior column and wall displacement, history of lower abdominal surgeries such as caesarean sections, bladder injury, open fractures and patients with fractures over 3 weeks old at the time of presentation.
Preoperatively, patients underwent anteroposterior (A.P), Judet (Iliac oblique and obturator oblique), and inlet and outlet radiographic views of the pelvis. All the patients underwent non-contrast CT scan on SOMATON Definition AS (64 detector row scanner, Siemens Medical, Forchheim, Germany) or SOMATOM Sensation scanner (40 detector row scanner, Siemens Medical, Forchheim, Germany) using following parameters: z-flying focal spot technology, 40 × 0.6 mm slices, images were reconstructed at slice thickness of 1.5 mm using smooth algorithm of karnel B30f. Images were analysed on Syngovia work stasion (Siemens Medical, Forchheim, Germany) to classify the fracture pattern, degree of fracture displacement, marginal impaction, intraarticular fragment and operative approach. The fractures were classified based on the Letournel and Judet Classification system.8
All patients were operated using the modified Stoppa approach.9 If an isolated approach was inadequate, a lateral window of the ilioinguinal approach was made, to aid in visualisation, reduction and fixation. The following parameters were tabulated during intra-operative period (Table 1). Fixation was achieved with 3.5 mm reconstruction plates and screws. In four patients, an additional spring plate was useful to buttress the quadrilateral surface.
Table 1.
Intra-operative measures.
| Total patients | 23 |
|---|---|
| Mean duration of surgery | 162.42 min |
| Mean duration of hospital stay | 14.95 days |
| Mean time interval between injury and surgery | 9.45 days |
| Mean blood loss | 695 mL (range, 375–1580 mL) |
| Intraoperative blood transfusions | 3 patients |
Immediate postoperative fracture reduction was evaluated using AP and Judet view radiographs of the pelvis and quantified by the criteria defined by Matta.5,8 Any loss in reduction and fracture union was evaluated at 6 weeks, 3 months and 6 months postoperatively, by AP and Judet radiographs of the pelvis with both hips. An immediate post-operative NCCT scan was performed to quantify reduction of fracture on the axial, sagittal and coronal sections. The NCCT scans of the pelvis were repeated at 6 months, to observe fracture union and any delayed fracture displacements.
The postoperative protocol was identical for all patients, with follow-ups at two weeks, six weeks, three months and six months. During their hospital stay, DVT prophylaxis in the form of mechanical pumps and compression stockings were given to all patients. LMW heparin (0.4 mL) was administered once a day, from the first postoperative day. Active and passive range of motion exercises were administered in the early post-operative period. Non-weight bearing mobilisation using walker/crutch was instructed for the initial six weeks, after which partial weight bearing was permitted. Full weight bearing was allowed after 3 months. The functional and radiological outcome was measured postoperatively after 6 months, by the Merle d’Aubigne and Postel scoring system10 and Matta radiological criteria.11,12 The cumulative scores were calculated.
Statistical analysis of the data was done using SPSS version 21.0. Quantitative variables were compared using ANOVA/Kruskal Wallis tests and Chi-Square test was used for qualitative variables. The normality of data was tested by Kolmogorov-Smirnov test.
3. Results
The modified Stoppa approach was utilised in twenty-five cases (See Fig. 1). Two cases were lost to follow-up. The mean age of the cohort, with eighteen males and five females, was 40.13 years (ranging from 20 to 65 years). Seventeen cases (73.91%) had road traffic accidents, which was the most common reason for injury. The only other mode of injury (6 cases) was fall from height (26.09%). The mean time interval between trauma and surgery was 9.45 days (range: 1–18 days). The concomitant and associated injuries that occurred are mentioned in Table 2. The major fracture pattern in our study was associated with both column fractures (9 cases) fractures, followed by transverse fractures (4 cases) (Table 3).
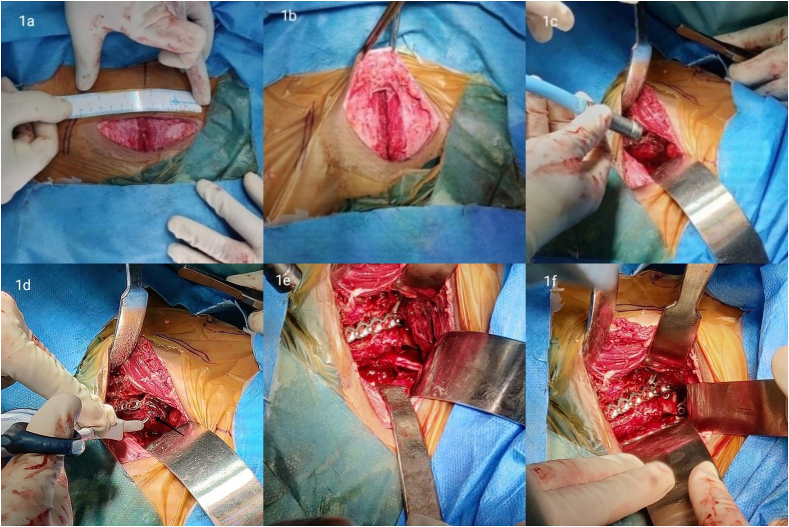
Fig. 1.
The intra-operative pictures, of one among our patients demonstrating.
a) An arc-shaped transverse, Pfannenstiel skin incision of 5–6 inches/12–15 cm made about 2 cm proximal to the pubic symphysis.
b) Superficial exposure: subcutaneous tissues, rectus fascia, rectus abdominus muscle and transfersalis facia split over the symphysis pubis.
c) Deep exposure: insertion of the rectus abdominus muscle, the iliopectineal fascia and the iliopsoas muscle released and elevated for adequate exposure of the true pelvis by appropriate placement of retractors. Increased visualisation assisted by the light source from the arthroscopy unit.
d) Corona mortis clipped (arrows) to allow further access to the pelvic brim and the quadrilateral surface.
e) Isolation of the obturator neurovascular bundle, medial to the obturator internus, and then sheltered by a malleable retractor.
f) To retract the rectus musculature, a Hohmann retractor is placed on the pubic tubercle. A Deaver retractor is positioned under the iliopsoas muscle to protect the external iliac vascular bundles. A slender malleable retractor is positioned at the sciatic notch to protect the obturator neurovascular bundle.
Table 2.
Associated injuries.
| Site | Cases |
|---|---|
| Other Organ Injuries | |
| Head | 2 |
| Thorax | 3 |
| Genito-urinary | 4 |
| Associated Fractures | |
| Skull | 2 |
| Rib and sternum | 2 |
| Spine | – |
| Upper limbs | 4 |
| Lower limbs | 2 |
Table 3.
Fracture pattern.
| Type of fracture | Number of cases | Percentage |
|---|---|---|
| Anterior wall | 1 | 4.34 |
| Anterior column | 3 | 13.04 |
| Transverse | 4 | 17.39 |
| T Shaped | 3 | 13.04 |
| Transverse with Posterior wall | 0 | 0 |
| Anterior column with Posterior hemi transverse | 3 | 13.04 |
| Associated both column | 9 | 39.13 |
| Total | 23 | 100 |
The mean duration of surgery (considered from skin incision to closure) was 162 min (range, 108–254 min), and the mean blood loss was 695 mL (range, 375–1580 mL). A total of 3 patients needed blood transfusions (one unit each) during the intraoperative period. The duration of hospital stay ranged from 6 to 18 days (mean 14.95 days).
The corona mortis was visualised in 11 out of the 23 cases. Five of these were venous, four were arterial and the other two contained both arterial and venous anastomoses. All the anastomosis were found on the posterior aspect of the superior pubic ramus at a mean distance of 5.4 cm (range, 3.8–8.6 cm) from the symphysis pubis.
The mean pre-operative displacement in axial, sagittal and coronal sections were, 3.8, 3.1 and 3.6 mm respectively. The mean post-operative displacement in axial, sagittal and coronal sections were, 0.2, 0.3 mm and 0.2 mm, respectively. The mean pre-operative and post-operative gap was 12.8 mm and 1.1 mm respectively. (Table 4). In eighteen of our cases the reduction was anatomic, imperfect in two cases, and poor in three cases (as per criteria of Matta5,8) (Table 5). Radiographic evaluation demonstrated that fracture union occurred in up to 95.6% of patients by 3.2 ± 0.6 months (range, 2–6 months). The radiological outcome at 6 months11,12 (Table 6) was excellent in 16 cases (69.56%), good in 3 cases (13.04%), fair in 3 cases (13.04%) and poor in 1 case (4.34%). The clinical outcome was excellent in six, good in thirteen, fair and poor in 2 patients each, at 6 months of follow up (Table 7). The modified Stoppa approach alone was enough to achieve reduction in 10 cases (43.48%). The lateral window was used in 13 cases (56.52%).
Table 4.
Pre- and post-operative NCCT measurements.
| Measurement | Mean Preoperative (range) in mm | Mean Postoperative (range) in mm |
|---|---|---|
| Amount of Displacement | ||
| Axial section | 3.8 | 0.2 |
| Sagittal section | 3.1 | 0.3 |
| Coronal section | 3.6 | 0.2 |
| Gap distance | 12.8 | 1.1 |
Table 5.
Radiological reduction according to Matta’s Reduction Criteria.
| Reduction | Number of patients | Percentage |
|---|---|---|
| An atomic (0–1 mm) | 18 | 78.26 |
| Imperfect (1–3 mm) | 2 | 08.69 |
| Poor (>3 mm) | 3 | 13.04 |
Table 6.
Radiological outcome according to criteria of Matta.
| Grade | Number of patients | Percentage |
|---|---|---|
| Excellent | 16 | 69.56 |
| Good | 3 | 13.04 |
| Fair | 3 | 13.04 |
| Poor | 1 | 4.34 |
Table 7.
Merle d’Aubigne and Postel Clinical Grading System at 6 months.
| Clinical grade | No. of patients | Percentage |
|---|---|---|
| Excellent | 6 | 26.09 |
| Good | 13 | 56.52 |
| Fair | 2 | 8.69 |
| Poor | 2 | 8.69 |
4. Discussion
With minimally invasive surgery having become an everyday exercise, there is an extensive attempt to minimize morbidity and simultaneously achieve an anatomic reduction in acetabular fracture management. Although the ilioinguinal approach is more commonly used, there is a threat of injury to the contents of the inguinal canal and the femoral neurovascular bundles.13 With the introduction of the modified Stoppa approach, the ‘middle window’ is avoided, thus curtailing the threat of injury to the above structures. A vast majority of studies reporting good to excellent outcomes via this approach are from developed nations. Data with regard to its application for more challenging fracture types in the Indian setup is inadequate. The basis of our study, along with the preceding reports by Cole and Bolhofner,3 Hirvensalo et al.,4 and Sagi et al.,14 is to demonstrate that the approach is a less invasive and reduces patient morbidity, while permitting good to excellent clinico-radiological results.
As the ilioinguinal approach is more commonly used, the ability to attain acceptable reductions through it is well documented.15 In our study, anatomical reduction was achieved in eighteen (78.26%) cases and we reported good or excellent results in nineteen (82.60%) cases (Fig. 2 and 3). These results obtained in our study are comparable to similar studies done using the Stoppa approach. In a study done by Hirvensalo et al.4, anatomical reduction was achieved in 84% of patients in a case series of 164 acetabular fractures. They also reported Harris Hip Scores of greater than 80 in three-fourths of the cases. Sagi et al.14 in their study on 50 patients used Merle d’aubigne’s scale to assess functional outcome among their patients and concluded that 88% of cases had good or an excellent outcome. Up to 92% of their cases had good or excellent fracture reductions.Various other studies16,17 have emphasized that anatomical reductions and good clinical outcomes can be achieved by the modified Stoppa approach.
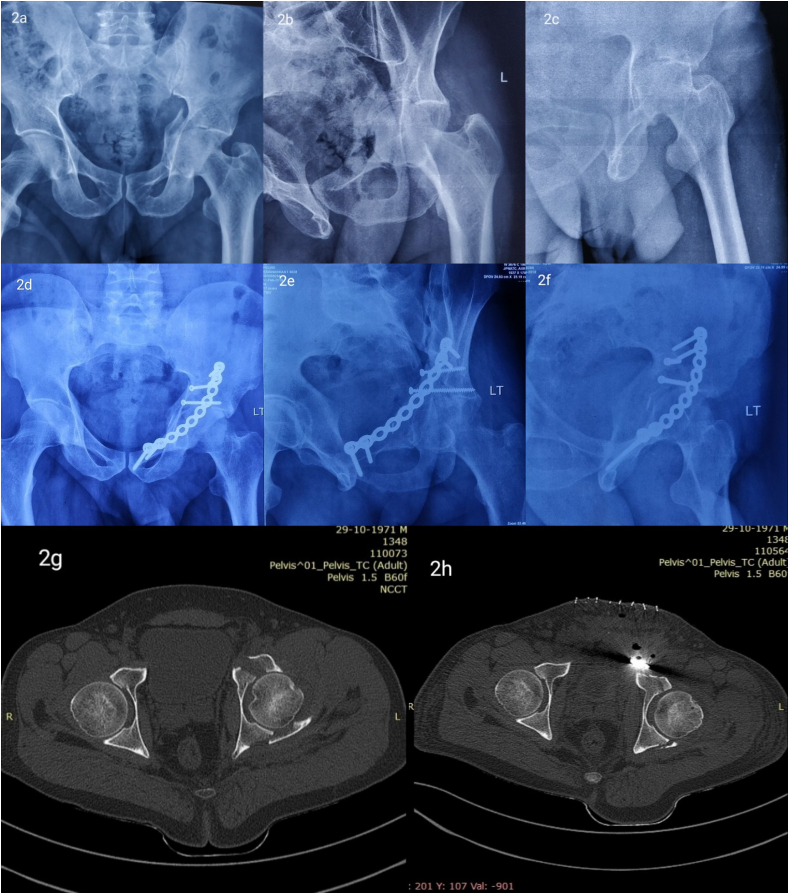
Fig. 2.
Preoperative (Fig. 2 a, b, c) and postoperative (Fig. 2 d, e, f) radiographs demonstrating a fixation of a transverse acetabular fracture using the modified Stoppas’ approach with indirect reduction using posterior column screws from the anterior side Pre- and postoperative (Fig. 2 g, h) NCCT scans of the same patient..
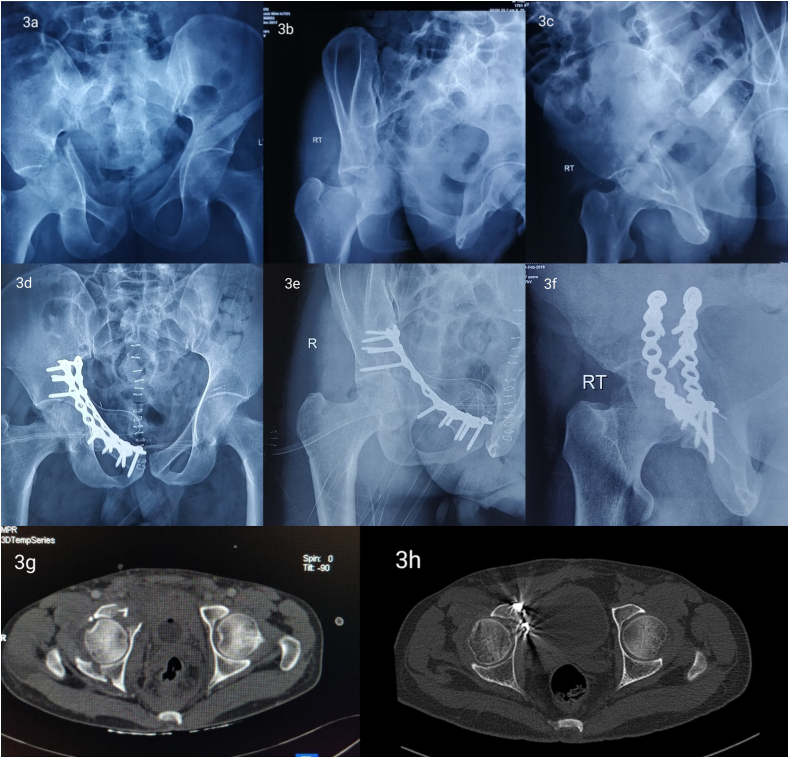
Fig. 3.
Preoperative (Fig. 3 a, b, c) and postoperative (Fig. 3 d, e, f) radiographs representing the reduction by double plating technique; one each, on the pelvic brim and the quadrilateral plate. Pre- and post-operative (Fig. 3 g, h) NCCT scans of the same patient.
In our study we had two cases in whom the functional outcomes were poor, and three cases with poor radiological reductions. Two of the three patients with poor reductions presented with an associated both column type and an anterior column with posterior hemi transverse type of fracture, in the 3rd week post-trauma (18th and 15th day respectively). Due to the late presentation and complex fracture type, there was difficulty in intraoperative fracture mobilization, subsequent reduction and an unsatisfactory outcome. The third patient had a superior dome impaction, and the challenging nature of fracture type led to poor results.
Many studies have compared the surgical blood loss betweens the ilioinguinal and the modified Stoppa approach.7,14,18,19 Elmadag et al.7 stated that the mean loss of blood between the two approaches was similar and statistically insignificant (1110 mL and 1170 mL for the Stoppa and ilioinguinal approach, respectively). In an RCT comparing the two approaches, Ma et al.19 concluded that there was less peri-operative haemorrhage and fewer requirements for transfusions with the modified Stoppa approach, mainly due to its less extensive dissection, reduced wound drainage and briefer operative period. In our study, the mean surgical loss of blood was 695 mL (range, 375–1580 mL) which is similar and even lesser as compared to other studies.14,17
The corona mortis, i.e. the anastomosis between the obturator and external iliac vessels, was present in 11 out of the 23 cases (47.82%). Five of these were venous and 4 were arterial and two were of the mixed variety. All the anastomosis were on the posterior aspect of the superior pubic ramus at a mean distance of 5.4 cm from the pubic symphysis. In our study, no accidental damage or uncontrolled bleeding occurred from the corona mortis. Such vascular injuries are frequently reported. Darmanis et al.20, have reported a case of an accidental injury to the corona mortis resulting in uncontrolled bleeding and the patient required 12 units of blood. Ma et al.19 have also reported a case with an accidental injury to the corona mortis, however, the patient remained stable and recovered well. During dissection, precaution has to be practiced to identify the anastomosis, and blunt-ended deep retractors ought to be used to prevent any inadvertent injury to the structure.
4.1. Complications
The operative management of acetabular fractures is frequently associated with complications. The lateral femoral cutaneous nerve is the most commonly injured nerve with the ilioinguinal approach13. The damage to this nerve is owing to the extreme retraction while exposing the middle window. This nerve is less commonly injured during the Stoppa approach and damage to the lateral cutaneous nerve occurred in none of our patients. In the modified Stoppa approach, other nerve injuries are frequently reported. Sagi et al.,14 have reported post-operative obturator nerve palsies in 26% of their patients. All their patients, except for one, recovered within six months. Similarly, Ma et al.19 reported two (6.7%) obturator nerve palsies. There were no obturator nerve injuries in any of our 23 cases. Great care is to be applied to minimize retraction of the obturator neurovascular bundles and no sharp-edged retractors should be inserted into the floor of the pelvis. While dissecting the obturator bundle, iatrogenic injury can be prevented by covering it with a wet sponge.
Post-traumatic arthritis following these fractures is relatively common and has been reported to range from 17%2 to 57%.21 Nearly 50% of patients developed arthrosis with an anatomical reduction in ten to twenty-five years, whereas 80% of patients with imperfect reductions develop arthrosis in less than ten years.2,4 As ours is a relatively short-term follow-up study, we did not have any incidence of post-traumatic arthritis. A longer follow up is required to appreciate such changes and is, therefore, a limitation of our study.
The modified Stoppa approach is being increasingly used in the fixation of anterior acetabular fractures and related components of complex acetabular fractures6,7. Certain studies have also shown that this approach is particularly effective in the reduction of the quadrilateral plate.16,18,22, 23, 24 As no muscle is excised from its attachments, the morbidity rate with this approach is substantially less.
As a substitute for the ilioinguinal approach, the modified Stoppa approach provides better access to the quadrilateral surface. There is better visual access to the whole pelvic brim from the pubic body to the frontal aspect of the sacral ala, and also to the posterior column, from the greater sciatic notch to the ischial spine. In our experience, the approach to the above structures was comfortable. We also accessed the superior part of the iliac bone and crest via an additional lateral window. Shazar et al.6 have emphasized the possibility of reduction in posterior column fractures and the application of a buttress plate from the posterior column up to the pelvic brim. In the current study, the surgeries were performed by an orthopaedic surgeon with more than 13 years of experience in pelvi-acetabular trauma. There is a steep learning curve for approaching the fractures of the acetabulum6. However, once the ilioinguinal approach is mastered, the modified Stoppa approach is less demanding, as the approach is not as extensive and avoids dissection along the inguinal canal.
This approach mandates fragile dissection, in patients having undergone previous revision surgeries, i.e Implant removals or Lower Segment Cesarian Sections, due to the formation of intra-pelvic adhesions. Kacra et al.25 suggested that the obturator and iliolumbar vessels are primarily at risk during the approach. Nevertheless, it is comparatively safe, to execute this approach in cases with a lean physique. Severe obesity and previous pelvic operative procedures are the relative contra-indications.17
4.2. Limitations
A small number of patients and a relatively brief duration of follow up were the major limitations of our study. We did not analyse our results against a comparable group. Ideally, a multicentric, randomized study with a large sample size would help confirm our results. However, our short-term results are encouraging for the practice of the Stoppa approach in the surgical fixation of acetabular fractures.
5. Conclusion
Despite certain limitations, our study demonstrates that good to excellent outcomes are achieved by utilising the modified Stoppa approach for the fixation of acetabular fractures. Curtailing perioperative morbidity and simultaneously making way for anatomical reduction are the major benefits of the approach. Our study provides, an alternative to the widely used ilioinguinal approach for the operative management of transverse and anterior acetabular fractures, associated both column and anterior-column with posterior hemi-transverse fractures.
Contributor Information
Tushar Nayak, Email: orthodrtushar@gmail.com.
Samarth Mittal, Email: samarthmittal@gmail.com.
Vivek Trikha, Email: vivektrikha@gmail.com.
Kamran Farooque, Email: Kamran.farooque@gmail.com.
Shivanand Gamanagatti, Email: shiv223@gmail.com.
Vijay Sharma, Email: drvijaysharmapelviacetabulum@gmail.com.
References
- 1.Küper M.A., Konrads C., Trulson A., Bahrs C., Stöckle U., Stuby F.M. Complications of surgical approaches for osteosynthetic treatment of acetabular fractures: analysis of pitfalls and how to avoid them. Injury. 2020 Feb 21 doi: 10.1016/j.injury.2020.02.100. [DOI] [PubMed] [Google Scholar]
- 2.Letournel E.M. The treatment of acetabular fractures through the ilioinguinal approach. Clin Orthop Relat Res. 1993 Jul;(292):62–76. [PubMed] [Google Scholar]
- 3.Cole J.D., Bolhofner B.R. Acetabular fracture fixation via a modified Stoppa limited intrapelvic approach. Description of operative technique and preliminary treatment results. Clin Orthop Relat Res. 1994 Aug;(305):112–123. [PubMed] [Google Scholar]
- 4.Hirvensalo E., Lindahl J., Kiljunen V. Modified and new approaches for pelvic and acetabular surgery. Injury. 2007 Apr 1;38(4):431–441. doi: 10.1016/j.injury.2007.01.020. [DOI] [PubMed] [Google Scholar]
- 5.Matta J.M. Operative treatment of acetabular fractures through the ilioinguinal approach: a 10-year perspective. J Orthop Trauma. 2006 Jan 1;20(1):S20–S29. [PubMed] [Google Scholar]
- 6.Shazar N., Eshed I., Ackshota N., Hershkovich O., Khazanov A., Herman A. Comparison of acetabular fracture reduction quality by the ilioinguinal or the anterior intrapelvic (modified rives–stoppa) surgical approaches. J Orthop Trauma. 2014 Jun;28(6):313–319. doi: 10.1097/01.bot.0000435627.56658.53. [DOI] [PubMed] [Google Scholar]
- 7.Elmadag M., Guzel Y., Acar M.A., Uzer G., Arazi M. The Stoppa approach versus the ilioinguinal approach for anterior acetabular fractures: a case control study assessing blood loss complications and function outcomes. Orthop Traumatol Surg Res. 2014;100(6):675–680. doi: 10.1016/j.otsr.2014.05.020. [DOI] [PubMed] [Google Scholar]
- 8.Matta J.M. Fracture of the acetabulum: accuracy of reduction and clinical results in patients managed operatively within three weeks after the injury. Orthop Trauma Dir. 2011 Mar;9:31–36. 02. [PubMed] [Google Scholar]
- 9.Archdeacon M.T., Kazemi N., Guy P., Sagi H.C. The modified Stoppa approach for acetabular fracture. JAAOS-Journal of the American Academy of Orthopaedic Surgeons. 2011;19(3):170–175. doi: 10.5435/00124635-201103000-00006. [DOI] [PubMed] [Google Scholar]
- 10.D’Aubigné R.M., Postel M. Functional results of hip arthroplasty with acrylic prosthesis. JBJS. 1954 jun;36(3):451–475. [PubMed] [Google Scholar]
- 11.Matta J.M., Anderson L.M., Epstein H.C., Hendricks P. Fractures of the acetabulum. A retrospective analysis. Clin Orthop Relat Res. 1986;(205):230–240. [PubMed] [Google Scholar]
- 12.Matta J.M., Mehne D.K., Roffi R. Fractures of the acetabulum. Early results of a prospective study. Clin Orthop Relat Res. 1986 Apr;(205):241–250. [PubMed] [Google Scholar]
- 13.Tosounidis T.H., Giannoudis V.P., Kanakaris N.K., Giannoudis P.V. The Ilioinguinal approach: state of the art. JBJS essential surgical techniques. 2018;8(2) doi: 10.2106/JBJS.ST.16.00101. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Sagi H.C., Afsari A., Dziadosz D. The anterior intra-pelvic (modified rives-stoppa) approach for fixation of acetabular fractures. J Orthop Trauma. 2010 May 1;24(5):263–270. doi: 10.1097/BOT.0b013e3181dd0b84. [DOI] [PubMed] [Google Scholar]
- 15.Letournel E. The treatment of acetabular fractures through the ilioinguinal approach. Clin Orthop Relat Res. 1993;(292):62–76. [PubMed] [Google Scholar]
- 16.Isaacson M.J., Taylor B.C., French B.G., Poka A. Treatment of acetabulum fractures through the modified Stoppa approach: strategies and outcomes. Clin Orthop Relat Res. 2014;472(11):3345–3352. doi: 10.1007/s11999-014-3460-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Kilinc C.Y., Acan A.E., Gultac E., Kilinc R.M., Hapa O., Aydogan N.H. Treatment results for acetabulum fractures using the modified Stoppa approach. Acta Orthop Traumatol Turcica. 2019;53(1):6–14. doi: 10.1016/j.aott.2018.11.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Fan L., Jin Y.J., He L., Lü Z., Fan H.H. Modified Stoppa approach in treatment of pelvic and acetabular fractures. Zhongguo gu shang= China journal of orthopaedics and traumatology. 2012;25(10):810–812. [PubMed] [Google Scholar]
- 19.Ma K., Luan F., Wang X. Randomized, controlled trial of the modified Stoppa versus the ilioinguinal approach for acetabular fractures. Orthopedics. 2013 Oct 1;36(10):e1307–e1315. doi: 10.3928/01477447-20130920-25. [DOI] [PubMed] [Google Scholar]
- 20.Darmanis S., Lewis A., Mansoor A., Bircher M. Corona mortis: an anatomical study with clinical implications in approaches to the pelvis and acetabulum. Clin Anat: The Official Journal of the American Association of Clinical Anatomists and the British Association of Clinical Anatomists. 2007;20(4):433–439. doi: 10.1002/ca.20390. [DOI] [PubMed] [Google Scholar]
- 21.Giannoudis P.V., Grotz M.R., Papakostidis C., Dinopoulos H. Operative treatment of displaced fractures of the acetabulum: a meta-analysis. The Journal of bone and joint surgery. British volume. 2005 Jan;87(1):2–9. [PubMed] [Google Scholar]
- 22.Andersen R.C., O’Toole R.V., Nascone J.W., Sciadini M.F., Frisch H.M., Turen C.W. Modified stoppa approach for acetabular fractures with anterior and posterior column displacement: quantification of radiographic reduction and analysis of interobserver variability. J Orthop Trauma. 2010;24(5):271–278. doi: 10.1097/BOT.0b013e3181b2b4ca. [DOI] [PubMed] [Google Scholar]
- 23.Keel M., Bastian J.D., Büchler L., Siebenrock K.-A. Anterior approaches to the acetabulum. Unfallchirurg. 2013;116(3):213–220. doi: 10.1007/s00113-012-2332-7. [DOI] [PubMed] [Google Scholar]
- 24.Khoury A., Weill Y., Mosheiff R. The Stoppa approach for acetabular fracture. Operat Orthop Traumatol. 2012;24(4–5):439–448. doi: 10.1007/s00064-011-0093-z. [DOI] [PubMed] [Google Scholar]
- 25.Kacra B.K., Arazi M., Cicekcibasi A.E., Büyükmumcu M., Demirci S. Modified medial Stoppa approach for acetabular fractures: an anatomic study. Journal of Trauma and Acute Care Surgery. 2011;71(5):1340–1344. doi: 10.1097/TA.0b013e3182092e8b. [DOI] [PubMed] [Google Scholar]