Abstract
As the global COVID-19 pandemic has progressed, awareness of uncommon presentations and complications has increased. The actual incidence of spontaneous pneumothorax was found to be 0.66%, or six patients out of 902 who tested positive in recently published literature of 3368 patients (Zantah M, Dominguez Castillo E, Townsend R, Dikengil F, Criner GJ. Pneumothorax in COVID-19 disease-incidence and clinical characteristics. Respir Res. 2020 Sep 16; 21 (1):236.). Of those six patients, only two (0.22%) were not associated with mechanical ventilation barotrauma or comorbid lung disease such as COPD. Here, we present a spontaneous pneumothorax and pneumomediastinum in a patient four days after he had been discharged from hospitalization due to uncomplicated COVID-19 pneumonia.
Keywords: Case report, Spontaneous pneumothorax, Pneumomediastinum, COVID-19, Coronavirus, SARS-Cov-2, Complication, CT
1. Introduction
Since the first outbreak in Wuhan, China in December of 2019, coronavirus (COVID-19) due to the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has swept the globe causing a massive pandemic. Common symptoms that have been identified include fever, cough, dyspnea, headache, abdominal pain, nausea/vomiting, myalgia, diarrhea, pharyngitis, rhinorrhea, fatigue, and loss of smell and/or taste [2]; although some of those infected can be asymptomatic [3]. There have also been fairly common complications of COVID-19 pneumonia that have been recognized which include but are not limited to: respiratory failure/acute respiratory distress syndrome, pulmonary fibrosis, arrhythmias, acute cardiac injury, shock, thromboembolic events, and inflammatory complications [4]. Consequently, many COVID-19 patients have been treated with invasive ventilation. It is well established that mechanical ventilation can cause barotrauma and resultant pneumothorax or pneumomediastinum. Consequently, many mechanically ventilated COVID-19 infected patients have suffered from these complications. However, reports of spontaneous pneumothorax, tension pneumothorax, or pneumomediastinum as a result of COVID-19, in the absence of underlying lung disease or barotrauma due to mechanical ventilation are rare. Therefore, we describe a case of secondary spontaneous pneumothorax and pneumomediastinum in a patient with resolved, uncomplicated COVID-19 pneumonia.
2. Narrative
A 72-year-old male with a past medical history of coronary artery disease, coronary artery bypass graft surgery, hypertension, and prediabetes presented to the emergency room with seven days of progressively worsening malaise, fatigue, weakness, fever, sore throat, cough, and dyspnea. He was never a smoker and was never diagnosed with chronic lung disease. Chest x-ray (CXR) was significant for mild scattered patchy opacities bilaterally, and computed tomography (CT) was significant for patchy ground-glass opacities bilaterally (Fig. 1A and B). He was found to be COVID-19 positive but was stable with an oxygen saturation (O2 SAT) of 95% on room air. He was subsequently discharged home on standard COVID-19 precautions. Two days later, he returned to the emergency room with worsening dyspnea and cough, productive of whitish sputum; he was in acute hypoxic respiratory failure with an O2 SAT of 86% on room air. CXR was notable for passive atelectasis in the lung bases due to a poor inspiratory effort as well as foci of increased interstitial change in the right mid-lung zone and lateral left base which could also have been due to atelectasis or pneumonitis. The patient was admitted to the intermediate care unit with telemetry under COVID-19 precautions and started on supplemental oxygen, enoxaparin, intravenous (IV) dexamethasone as well as remdesivir. The following day, he was given two units of COVID-19 convalescent plasma and placed on 2 L oxygen (O2) to maintain an O2 SAT of 95%. However, the patient deteriorated over the next 24 hours requiring 35 L of high flow nasal cannula with fraction of inspired oxygen (FiO2) of 50% to maintain an O2 SAT of 86%. Awake prone positioning was initiated for as often as the patient could tolerate. Over the next nine days, the patient's status slowly improved, although CXR remained unchanged. By day 14 after admission, the patient was maintaining an O2 SAT above 90% on room air, was afebrile, stable, and subsequently discharged.
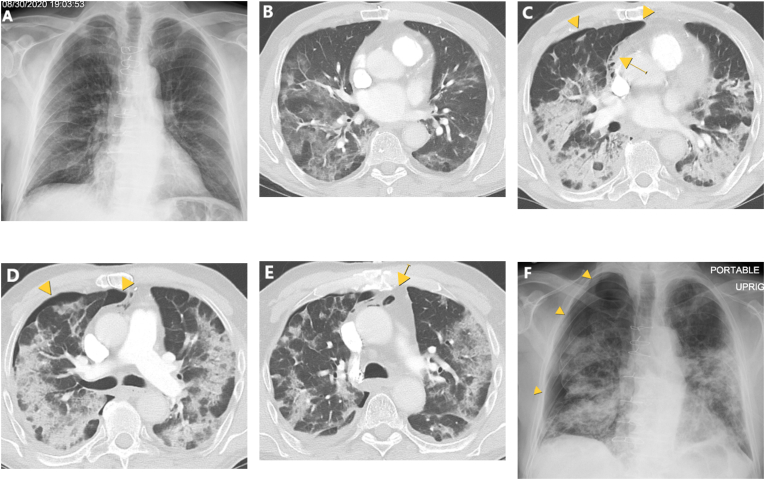
Fig. 1.
CXR (A) from first admission demonstrating mild scattered patchy opacity bilaterally and CT (B) with patchy ground-glass opacities bilaterally; no evidence of pneumothorax or pneumomediastinum. CT images (C,D,E) from the second admission date demonstrating anterior-lateral pneumothorax (yellow arrowheads) and small pneumomediastinum (yellow arrows). Portable CXR (F) prior to chest tube placement demonstrating the pneumothorax enlarged to approximately 30% (yellow arrowheads). (For interpretation of the references to colour in this figure legend, the reader is referred to the Web version of this article.)
Four days after discharge, the patient again returned to the emergency room with complaints of dyspnea, cough, and pleuritic type chest pain. He was hypoxic with an O2 SAT in the mid 80's on room air. He was otherwise hemodynamically stable and afebrile. Laboratory evaluation did not reveal any leukocytosis or significant derangements on his complete blood count (CBC) or basic metabolic panel (BMP). His procalcitonin and lactic acid were both normal at 0.09 ng/ml and 1.4 mmol/L respectively. However, his D-dimer, ferritin, and fibrinogen were each elevated at 0.93 mcg/mL, 515 ng/mL, and 520 mg/dL respectively. Additionally, C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) were both elevated. He was sent for a chest CT that did not show evidence of pulmonary embolism, although he continued to demonstrate ground-glass and consolidative opacities predominantly involving the mid to lower lung zones with scattered peripheral ground-glass opacities in the upper lobes bilaterally. Additionally, there was a small, 1 cm right anterior-lateral pneumothorax and small pneumomediastinum identified (Fig. 1C and D,E). The patient was once again admitted in order to monitor the pneumothorax, systemic inflammatory response syndrome, and to begin IV cefepime and azithromycin for possible superimposed bacterial pneumonia with recent COVID-19 infection. He was placed on 5 L nasal cannula supplemental oxygen and given breathing treatments of albuterol, metered-dose inhaler, as needed. Following infectious disease consultation, the patient's antibiotic regimen was changed from azithromycin to vancomycin. Over the course of the next five days, the pneumothorax progressively enlarged to approximately 30% (Fig. 1 F). At its largest size, the apical portion measured 3.7 cm from the upper chest wall and 3.1 cm from the lateral chest wall. General surgery was consulted for chest tube placement, and follow-up imaging demonstrated satisfactory position with near complete resolution of the pneumothorax. During the five days following the chest tube placement, the patient required 13 L of Optiflow and received dexamethasone and enoxaparin. He improved steadily until he became hemodynamically stable with an O2 SAT of 92% on 7 L of O2 by nasal cannula. The pneumothorax resolved, the chest tube was removed, and he was weaned down to 3 L of O2 by nasal cannula gradually over the course of the next two weeks. He was subsequently discharged home on hospital day 25 with supplemental oxygen.
3. Discussion
COVID-19 infection has been shown to rarely cause spontaneous pneumothorax, with an incidence of <1% although this may be underreported [5]. Additionally, these patients are often treated with invasive ventilation leading to barotrauma or have multiple pre-existing cardiopulmonary comorbidities [6]. However, we report a patient who had no prior lung injury, was never a smoker, and did not receive invasive ventilation. While the mechanism of spontaneous pneumothorax is frequently secondary to complications of cystic lung lesions, the mechanism in COVID-19 infection is less well understood. Known risk factors for spontaneous pneumothorax include male sex, thin and tall body habitus, smoking, trauma, and infection [7]. In COVID-19 infections, it is thought that the inflammatory response and ischemic damage within the lung parenchyma predisposes to cell adhesion between type I and type II pneumocytes, alveolar damage, and subsequent rupture [8]. Finally, the severity of associated symptoms in COVID-19 infection may lead to increased respiratory effort and cough due to the resulting ventilation/perfusion mismatch and contribute to alveolar cystic rupture [8].
While the risk of spontaneous pneumothorax in COVID-19 infection is uncertain, it is reasonable to predict that patients receiving invasive ventilation, or other predispositions to spontaneous pneumothorax may have an increased risk. However, the associated severity and prognosis of spontaneous pneumothorax concomitantly in COVID-19 infection has yet to be established [9]. Interestingly, in our case study and others, pneumothorax occurred days to weeks after onset of symptoms [[1], [2], [3], [4], [5], [6],[9], [10], [11], [12], [13], [14], [15], [16], [17], [18], [19], [20], [21], [22], [23], [24], [25], [26], [27], [28], [29], [30], [31], [32], [33], [34], [35]]. Even though our patient did not present with evidence of cysts or bullae on initial CXR or CT, the delayed time frame to onset of pneumothorax could have given rise to pulmonary changes which predisposed him to pneumothorax. Thus, initial inflammatory insult and resulting increased respiratory effort due to COVID-19 may inflict micro-lesions within the tissue which predispose patients to spontaneous pneumothorax, but require weeks for adequate cystic lesions to develop, thus enabling pneumothorax to occur [3].
Review of the current literature reveals 32 case reports of spontaneous pneumothorax or pneumomediastinum in 58 COVID-19 pneumonia infections, of which 14 patients expired and 43 underwent chest tube placement (Table 1). Thus, spontaneous pneumothorax is a known complication of COVID-19 infection, although with an undetermined prevalence and long-term risk.
Table 1.
Literature review of COVID-19-associated pneumothorax in patients without history of mechanical ventilation or prior lung disease.
| Serial Number | Author/published Year/country |
Number of relevant cases/total cases | Age (years) | Gender | Comorbidities | Diagnosis | Treatment/Intervention | Outcome |
|---|---|---|---|---|---|---|---|---|
| 1. | Sun R et al. [21], March 2020, Wuhan, China |
1 | 38 | Male | Nil | Left pneumothorax | Conservative | Recovered |
| 2. | Wang W et al. [25], August 2020, Zhejiang, China |
1 | 62 | Male | Nil | Right pneumothorax, pneumomediastinum, subcutaneous emphysema | Conservative | Recovered |
| 3. | Wang J et al. [10], March 2020, Guangzhou, China | 1 | 36 | Male | Nil | Pneumomediastinum | Conservative | Expired |
| 4. | Rohailla S et al. [11], May 2020, Toronto, Canada | 1 | 26 | Male | Nil | Right pneumothorax | Chest tube | Recovered and discharged |
| 5. | Ucpinar BA et al. [12], May 2020, Istanbul, Turkey | 1 | 82 | Female | Nil | Left pneumothorax, pneumomediastinum, subcutaneous emphysema (neck, post. thoracic wall) | Chest tube | Recovered and discharged |
| 6. | Quincho-Lopez A et al. [13], July 2020, Lima, Peru | 1/2 | 31 | Male | Chronic gastritis, hypercholesterolemia | Pneumomediastinum | Conservative | Recovered and discharged |
| 7. | Lopez Vega JM et al. [14], June 2020, Madrid, Spain | 3 |
84 67 73 |
Female Male Male |
Hypertension, prosthetic heart valve, chronic kidney disease, and congestive cardiac failure Not reported Basal cell epithelioma, OSA, depression |
Right hydropneumothorax Bilateral pneumothorax, pneumomediastinum Pneumomediastinum |
Conservative Chest tube CPAP |
Expired Expired Expired |
| 8. | Hollingshead C et al. [15]., June 2020, Ohio, USA | 1 | 50 | Male | Nil | Right posterior pneumothorax | Chest tube | Not reported |
| 9. | Eperiesiova B et al. [16], July 2020, Michigan, USA | 4/7 | 54 Not Reported Not Reported Not Reported |
Female Not Reported Not Reported Not Reported |
Hypertension Not Reported Not Reported Not Reported |
Pneumomediastinum, subcutaneous emphysema Left pneumothorax, Pneumomediastinum Right pneumothorax Right pneumothorax |
Conservative Chest Tube Chest Tube Chest Tube |
Recovered and discharged Not Reported Not Reported Not Reported |
| 10. | Mallick T et al. [17], July 2020, New York, USA | 3/3 | 40 68 58 |
Male Male Female |
Smoker Nil Hypertension |
Right pneumothorax Bilateral pneumothorax, pneumomediastinum, subcutaneous emphysema Right pneumothorax, Pneumomediastinum, subcutaneous emphysema |
Chest tube Chest tubes Pleural cavity decompression |
Expired Recovered and discharged Recovered and discharged |
| 11. | Ferreira JG et al. [18], August 2020, Rio de Janiero, Brazil | 1 | 45 | Male | Nil | Left tension pneumothorax | Chest tube | Recovered and discharged |
| 12. | Spiro JE et al. [2], June 2020, Munich, Germany | 1 | 47 | Male | Nil | Right tension pneumothorax | Chest tube | Recovered and discharged |
| 13. | Khurram R et al. [19], August 2020, London, United Kingdom | 1 | 64 | Male | Nil | Right tension pneumothorax | Chest tube | Recovered and discharged |
| 14. | Martinelli AW et al. [20], September 2020, Cambridge, United Kingdom | 18/62 | Variesa | Variesa | Variesa | Variesa | Variesa | Variesa |
| 15. | Chen X et al. [5], September 2020, Wuhan, China | 1 | 66 | Male | Nil | Left pneumothorax | Chest tube | Recovered and discharged |
| 16. | Fan Q et al. [22], September 2020, Wuhan, China | 1 | 32 | Male | Nil | Left pneumothorax, subpleural bulla | Chest tube | Recovered and discharged |
| 17. | Alhakeem A et al. [3], July 2020, Doha, Qatar | 1 | 49 | Male | Nil | Bilateral pneumothorax | Chest tubes | Stable |
| 18. | Borghesi A et al. [23], July 2020, Brescia, Italy | 1 | 73 | Female | Breast cancer | Left pneumothorax | Conservative | Recovered and discharged |
| 19. | Gurkan O et al. [24], June 2020, Istanbul, Turkey | 1 | 24 | Male | Nil | Left pneumothorax | Conservative | Recovered and discharged |
| 20. | Zantah M et al. [1], September 2020, Pennsylvania, USA | 2/6 | 49 81 |
Male Female |
Nil Not reported |
Left pneumothorax Bilateral pneumothorax |
Chest tube Chest tubes |
Expired Expired |
| 21. | Ahluwalia AS et al. [26], September 2020, New York, USA | 1 | 31 | Male | Nil | Left tension pneumothorax, right pneumothorax, pneumomediastinum, pneumopericardium | Chest tube | Recovered and discharged |
| 22. | Janssen ML et al. [27], August 2020, Rotterdam, the Netherlands | 1/3 | 63 | Male | Nil | Right pneumothorax | Chest tube | Recovered and discharged |
| 23. | Gonzalez-Pacheco et al. [9], July 2020, Mexico City, Mexico | 1 | 45 | Male | Nil | Bilateral pneumothorax | Chest tubes | Recovered and discharged |
| 24. | Al-Shokri SD et al. [28], July 2020, Doha, Qatar | 1/3 | 50 | Male | Not reported | Right tension pneumothorax | Chest tube | Recovered and transferred |
| 25. | Sahu KK et al. [29], August 2020, Massachusetts, USA | 1 | 61 | Male | Hypertension | Pneumomediastinum, pneumopericardium, subcutaneous emphysema | Intubation | Expired |
| 26. | Yasukawa K et al. [30], July 2020, Washington DC, USA | 1 | 37 | Male | Nil | Right tension pneumothorax, right bulla | Chest tube | Recovered and discharged |
| 27. | Carvalho do Lago VC et al. [6], July 2020, Sao Paulo, Brazil | 2 | 34 62 |
Male Male |
Nil Ex-smoker |
Left pneumothorax Right pneumothorax |
Chest tube Chest tube |
Stable Stable |
| 28. | Lei P et al. [31], April 2020, Guiyang, China | 1 | 64 | Male | Nil | Pneumomediastinum | Conservative | Recovered |
| 29. | Zhou et al. [32], April 2020, Hangzhou, Zhejiang, China | 1 | 38 | Male | Not reported | Pneumomediastinum, subcutaneous emphysema | Conservative | Recovered and discharged |
| 30. | Correa Neto et al. [33], May 2020, Sao Paulo, Brazil | 1 | 80 | Female | Hypertension, CAD | Pneumothorax, pneumoperitoneum | Intubation, chest tube, exploratory laparotomy | Expired |
| 31. | Kolani et al. [34], May 2020, Fez, Morocco | 1 | 23 | Female | Nil | Pneumomediastinum | Conservative | Recovered and discharged |
| 32. | Lacroix M et al. [35], May 2020, Paris, France | 1 | 57 | Male | Not reported | Pneumomediastinum, subcutaneous emphysema | Intubation | Not reported |
Data for each case varies. To be conscientious of space, these were not individually reported.
4. Conclusion
Spontaneous pneumothorax in COVID-19 infection is a rare, emergent, but treatable complication and may present days to weeks after apparent resolution of initial COVID-19 symptoms. Clinicians should consider spontaneous pneumothorax in patients with acute dyspnea and chest pain, particularly if they have a recent history of COVID-19 pneumonia. Additionally, the hypothesized underlying mechanism may increase a patient's risk for pneumothorax even weeks after recovery from COVID-19 infection, due to lung insult and subsequent increased respiratory effort. However further research is needed in this area.
Funding
No funding was provided or needed for this study.
Credit author statement
Jennifer Dennison: Writing-Original draft preparation, Investigation, Visualization: Samuel Carlson: Writing-Original draft preparation: Shannon Faehling: Writing-Review and Editing: Margaret Lieb: Writing-Review and Editing: Ateeq Mubarik: Writing-Review and Editing, Supervision.
Declaration of competing interest
All named authors declare that they have no conflict of interests, financial or otherwise.
References
- 1.Zantah M., Dominguez Castillo E., Townsend R., Dikengil F., Criner G.J. Pneumothorax in COVID-19 disease- incidence and clinical characteristics. Respir. Res. 2020 Sep 16;21(1):236. doi: 10.1186/s12931-020-01504-y. PMID: 32938445; PMCID: PMC7492794. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Spiro J.E., Sisovic S., Ockert B., Böcker W., Siebenbürger G. Secondary tension pneumothorax in a COVID-19 pneumonia patient: a case report. Infection. 2020 Jun 18:1–4. doi: 10.1007/s15010-020-01457-w. Epub ahead of print. PMID: 32557347; PMCID: PMC7301769. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Alhakeem A., Khan M.M., Al Soub H., Yousaf Z. Case report: COVID-19-Associated bilateral spontaneous pneumothorax-A literature review. Am. J. Trop. Med. Hyg. 2020 Sep;103(3):1162–1165. doi: 10.4269/ajtmh.20-0680. PMID: 32666917; PMCID: PMC7470558. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Abushahin A., Degliuomini J., Aronow W.S., Newman T. A case of spontaneous pneumothorax 21 Days after diagnosis of coronavirus disease 2019 (COVID-19) pneumonia. Am J Case Rep. 2020 Aug 15:21. doi: 10.12659/AJCR.925787. e925787. PMID: 32798215; PMCID: PMC7447295. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Chen X., Zhang G., Tang Y., Peng Z., Pan H. The coronavirus diseases 2019 (COVID-19) pneumonia with spontaneous pneumothorax: a case report. BMC Infect. Dis. 2020 Sep 9;20(1):662. doi: 10.1186/s12879-020-05384-x. PMID: 32907540; PMCID: PMC7479294. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.do Lago V.C., Cezare T.J., Fortaleza C.M.C.B., Okoshi M.P., Baldi B.G., Tanni S.E. Does COVID-19 increase the risk for spontaneous pneumothorax? Am. J. Med. Sci. 2020 Jul 16 doi: 10.1016/j.amjms.2020.07.024. S0002-9629(20)30320-7. Epub ahead of print. PMID: 32819707; PMCID: PMC7365097. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Gupta D., Hansell A., Nichols T., Duong T., Ayres J.G., Strachan D. Epidemiology of pneumothorax in england. Thorax. 2000 Aug;55(8):666–671. doi: 10.1136/thorax.55.8.666. PMID: 10899243; PMCID: PMC1745823. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Liu K., Zeng Y., Xie P., Ye X., Xu G., Liu J., Wang H., Qian J. COVID-19 with cystic features on computed tomography: a case report. Medicine (Baltim.) 2020 May;99(18) doi: 10.1097/MD.0000000000020175. PMID: 32358406; PMCID: PMC7440163. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.González-Pacheco H., Gopar-Nieto R., Jiménez-Rodríguez G.M., Manzur-Sandoval D., Sandoval J., Arias-Mendoza A. Bilateral spontaneous pneumothorax in SARS-CoV-2 infection: a very rare, life-threatening complication. Am. J. Emerg. Med. 2020 Jul 12 doi: 10.1016/j.ajem.2020.07.018. S0735-6757(20)30610-0. Epub ahead of print. PMID: 32712235; PMCID: PMC7354379. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Wang J., Su X., Zhang T., Zheng C. Spontaneous pneumomediastinum: a probable unusual complication of coronavirus disease 2019 (COVID-19) pneumonia. Korean J. Radiol. 2020 May;21(5):627–628. doi: 10.3348/kjr.2020.0281. PMID: 32323507; PMCID: PMC7183829. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Rohailla S., Ahmed N., Gough K. SARS-CoV-2 infection associated with spontaneous pneumothorax. CMAJ (Can. Med. Assoc. J.) 2020 May 11;192(19):E510. doi: 10.1503/cmaj.200609. Epub 2020 Apr 21. PMID: 32317275; PMCID: PMC7234273. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Ucpinar B.A., Sahin C., Yanc U. Spontaneous pneumothorax and subcutaneous emphysema in COVID-19 patient: case report. J Infect Public Health. 2020 Jun;13(6):887–889. doi: 10.1016/j.jiph.2020.05.012. Epub 2020 May 26. PMID: 32475804; PMCID: PMC7247978. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Quincho-López A., Quincho-Lopez D.L., Hurtado-Medina F.D. Case report: pneumothorax and pneumomediastinum as uncommon complications of COVID-19 pneumonia-literature review. Am. J. Trop. Med. Hyg. 2020 Sep;103(3):1170–1176. doi: 10.4269/ajtmh.20-0815. PMID: 32705978; PMCID: PMC7470555. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.López Vega J.M., Parra Gordo M.L., Diez Tascón A., Ossaba Vélez S. Pneumomediastinum and spontaneous pneumothorax as an extrapulmonary complication of COVID-19 disease. Emerg. Radiol. 2020 Jun 11:1–4. doi: 10.1007/s10140-020-01806-0. Epub ahead of print. PMID: 32524296; PMCID: PMC7286744. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Hollingshead C., Hanrahan J. Spontaneous pneumothorax following COVID-19 pneumonia. IDCases. 2020 Jun 17;21 doi: 10.1016/j.idcr.2020.e00868. PMID: 32596131; PMCID: PMC7306487. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Eperjesiova B., Hart E., Shokr M., Sinha P., Ferguson G.T. Spontaneous pneumomediastinum/pneumothorax in patients with COVID-19. Cureus. 2020 Jul 3;12(7) doi: 10.7759/cureus.8996. PMID: 32642391; PMCID: PMC7336633. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Mallick T., Dinesh A., Engdahl R., Sabado M. COVID-19 complicated by spontaneous pneumothorax. Cureus. 2020 Jul 9;12(7) doi: 10.7759/cureus.9104. PMID: 32789049; PMCID: PMC7417091. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Ferreira J.G., Rapparini C., Gomes B.M., Pinto L.A.C., Freire M.S.D.S.E. Pneumothorax as a late complication of COVID-19. Rev. Inst. Med. Trop. Sao Paulo. 2020;62:e61. doi: 10.1590/s1678-9946202062061. Epub 2020 Aug 31. PMID: 32876299; PMCID: PMC7458073. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Khurram R., Johnson F.T.F., Naran R., Hare S. Spontaneous tension pneumothorax and acute pulmonary emboli in a patient with COVID-19 infection. BMJ Case Rep. 2020 Aug 11;13(8) doi: 10.1136/bcr-2020-237475. PMID: 32784238; PMCID: PMC7418853. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Martinelli A.W., Ingle T., Newman J., Nadeem I., Jackson K., Lane N.D., Melhorn J., Davies H.E., Rostron A.J., Adeni A., Conroy K., Woznitza N., Matson M., Brill S.E., Murray J., Shah A., Naran R., Hare S.S., Collas O., Bigham S., Spiro M., Huang M.M., Iqbal B., Trenfield S., Ledot S., Desai S., Standing L., Babar J., Mahroof R., Smith I., Lee K., Tchrakian N., Uys S., Ricketts W., Patel A.R.C., Aujayeb A., Kokosi M., Wilkinson A.J.K., Marciniak S.J. COVID-19 and pneumothorax: a multicentre retrospective case series. Eur. Respir. J. 2020 Sep 9:2002697. doi: 10.1183/13993003.02697-2020. Epub ahead of print. PMID: 32907891; PMCID: PMC7487269. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Sun R., Liu H., Wang X. Mediastinal emphysema, giant Bulla, and pneumothorax developed during the course of COVID-19 pneumonia. Korean J. Radiol. 2020 May;21(5):541–544. doi: 10.3348/kjr.2020.0180. Epub 2020 Mar 20. PMID: 32207255; PMCID: PMC7183834. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Fan Q., Pan F., Yang L. Spontaneous pneumothorax and subpleural bullae in a patient with COVID-19: a 92-day observation. Eur. J. Cardio. Thorac. Surg. 2020 Oct 1;58(4):858–860. doi: 10.1093/ejcts/ezaa305. PMID: 32951046. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Borghesi A., Aggiusti C., Farina D., Maroldi R., Muiesan M.L. COVID-19 pneumonia: three thoracic complications in the same patient. Diagnostics. 2020 Jul 20;10(7):498. doi: 10.3390/diagnostics10070498. PMID: 32698424; PMCID: PMC7399854. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Gurkan O., Yilmaz A., Cengel F., Altunok E.S., Ekin E.E. COVID-19 pulmonary infection with pneumothorax in a young patient. J Coll Physicians Surg Pak. 2020 Jun;30(6):43–45. doi: 10.29271/jcpsp.2020.Supp1.S43. PMID: 32723448. [DOI] [PubMed] [Google Scholar]
- 25.Wang W., Gao R., Zheng Y., Jiang L. COVID-19 with spontaneous pneumothorax, pneumomediastinum and subcutaneous emphysema. J. Trav. Med. 2020 Aug 20;27(5) doi: 10.1093/jtm/taaa062. taaa062. PMID: 32330274; PMCID: PMC7188125. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Ahluwalia A.S., Qarni T., Narula N., Sadiq W., Chalhoub M.N. Bilateral pneumothorax as possible atypical presentation of coronavirus disease 2019 (COVID-19) Respir Med Case Rep. 2020;31:101217. doi: 10.1016/j.rmcr.2020.101217. Epub 2020 Sep 11. PMID: 32934903; PMCID: PMC7483079. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Janssen M.L., van Manen M.J.G., Cretier S.E., Braunstahl G.J. Pneumothorax in patients with prior or current COVID-19 pneumonia. Respir Med Case Rep. 2020;31:101187. doi: 10.1016/j.rmcr.2020.101187. Epub 2020 Aug 13. PMID: 32837901; PMCID: PMC7425767. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Al-Shokri S.D., Ahmed A.O.E., Saleh A.O., AbouKamar M., Ahmed K., Mohamed M.F.H. Case report: COVID-19-Related pneumothorax-case series highlighting a significant complication. Am. J. Trop. Med. Hyg. 2020 Sep;103(3):1166–1169. doi: 10.4269/ajtmh.20-0713. PMID: 32662394; PMCID: PMC7470563. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Sahu K.K., Mishra A.K., Goldman Y. A rare case of Pneumopericardium secondary to COVID-19. Heart Lung. 2020 Aug 21;49(6):679–680. doi: 10.1016/j.hrtlng.2020.08.017. Epub ahead of print. PMID: 32861883; PMCID: PMC7441933. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Yasukawa K., Vamadevan A., Rollins R. Bulla formation and tension pneumothorax in a patient with COVID-19. Am. J. Trop. Med. Hyg. 2020 Sep;103(3):943–944. doi: 10.4269/ajtmh.20-0736. PMID: 32662395; PMCID: PMC7470585. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Lei P., Mao J., Wang P. Spontaneous pneumomediastinum in a patient with coronavirus disease 2019 pneumonia and the possible underlying mechanism. Korean J. Radiol. 2020 Jul;21(7):929–930. doi: 10.3348/kjr.2020.0426. PMID: 32524794; PMCID: PMC7289698. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Zhou C., Gao C., Xie Y., Xu M. COVID-19 with spontaneous pneumomediastinum. Lancet Infect. Dis. 2020 Apr;20(4):510. doi: 10.1016/S1473-3099(20)30156-0. Epub 2020 Mar 9. PMID: 32164830; PMCID: PMC7128610. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Corrêa Neto I.J.F., Viana K.F., Silva M.B.S.D., Silva L.M.D., Oliveira G.D., Cecchini A.R.D.S. Perforated acute abdomen in a patient with COVID-19: an atypical manifestation of the disease. J. Coloproctol. 2020;40(3):269–272. [Google Scholar]
- 34.Kolani S., Houari N., Haloua M., Alaoui Lamrani Y., Boubbou M., Serraj M., Aamara B., Maaroufi M., Alami B. Spontaneous pneumomediastinum occurring in the SARS-COV-2 infection. IDCases. 2020 May 11;21 doi: 10.1016/j.idcr.2020.e00806. PMID: 32395425; PMCID: PMC7212974. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Lacroix M., Graiess F., Monnier-Cholley L., Arrivé L. SARS-CoV-2 pulmonary infection revealed by subcutaneous emphysema and pneumomediastinum. Intensive Care Med. 2020 Aug;46(8):1620–1621. doi: 10.1007/s00134-020-06078-3. Epub 2020 May 19. PMID: 32430514; PMCID: PMC7235431. [DOI] [PMC free article] [PubMed] [Google Scholar]