Inborn errors of metabolism cause a wide spectrum of neurodevelopmental and neurodegenerative conditions [15]. A pivotal enzyme located at the intersection of the amino acid and folic acid metabolic pathways is SHMT2, the mitochondrial form of serine hydroxymethyltransferase. SHMT2 performs the first step in a series of reactions that provide one-carbon units covalently bound to folate species in mitochondria: it transfers one-carbon units from serine to tetrahydrofolate (THF), generating glycine and 5,10-methylene-THF [4, 11, 12].
Using whole exome sequencing (WES), we identified biallelic SHMT2 variants in five individuals from four different families. All identified variants were located in conserved residues, either absent or extremely rare in control databases (gnomAD, ExAC), and cosegregated based on a recessive mode of inheritance (pRec = 0.9918 for this gene) (Supplementary Figs. 1–3, Supplementary Table 1). In family F1, a homozygous missense variant present in two affected siblings was located in a region without heterozygosity (~ 10 Mb, the only region > 1 Mb shared by both siblings) in which no other candidate variants were found, providing a strong genetic evidence of causality for these variants. The missense/in-frame deletion nature of these variants, and the absence of loss-of-function homozygous individuals in control databases, combined with the fact that complete loss of SHMT2 is embryonic lethal in the mouse [18], suggested that these variants may cause hypomorphic effects. Using 3D molecular dynamics models of the SHMT2 protein, we concluded that these candidate variants probably alter the SHMT2 oligomerization process, and/or disrupt the conformation of the active site, thus inducing deleterious effects on SHMT2 enzymatic function (Supplementary Figs. 4–8, Supplementary Tables 2–3, Supplementary video) [8, 19].
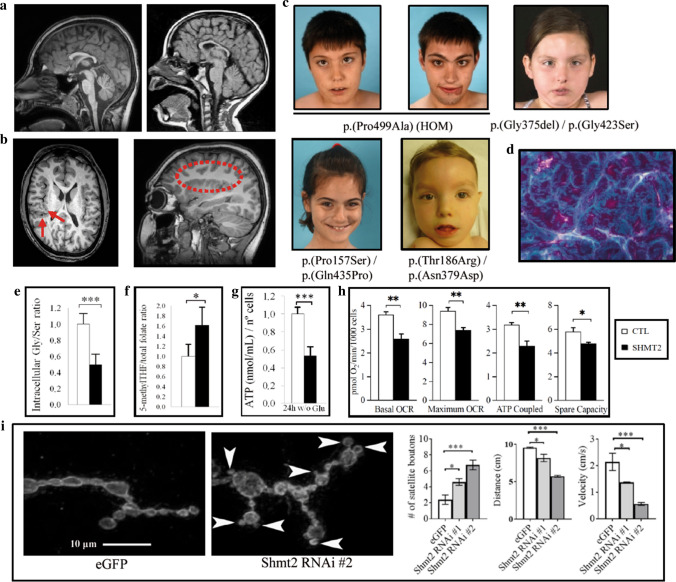
All patients presented a similar phenotype, characterized by dysmorphic features including long palpebral fissures, eversion of lateral third of lower eyelids, arched eyebrows, long eyelashes, thin upper lip, long philtrum, short fifth finger, fleshy pads at the tips of the fingers, mild 2–3 toe syndactyly and low-set thumbs. All patients exhibited intellectual disability and motor dysfunction, in the form of spastic paraparesis, ataxia, and/or peripheral neuropathy. Also, four out of five patients showed hypertrophic cardiomyopathy or atrial-septal defects, which tend to progress over time. All of the patients showed congenital microcephaly; MRI revealed corpus callosum abnormalities in all patients and perisylvian polymicrogyria-like pattern in patients P1–P4 (Fig. 1a–c, Supplementary Figs. 9–11, Supplementary Table 4). Quadriceps muscle and myocardium biopsies from Patient 4 showed myopathic changes, and myocardium biopsy showed the presence of “ragged red” fibers, suggestive of defective mitochondria (Fig. 1d, Supplementary Fig. 12).
Fig. 1.
SHMT2-mutated patients: phenotype and functional evaluation in fibroblasts. a Sagital T1-weighted MRI planes showing corpus callosum hypoplasia in Patient P1 (left) and Patient P4 (right). b Axial T1-weighted MRI planes (left) in Patient P2 showing perisylvian polymicrogyria (PMG) visible around both Sylvian fissures and insulae (arrows) and right parasagittal T1-weighted MRI (dotted contour). Note the stippled gray-white boundary of the polymicrogyric cortex compared to the smooth gray-white boundary in normal cortical areas. c Dysmorphic features in Patients P1–P5. d Modified Gomori trichrome staining of Patient 4 myocardium biopsy sample showed the presence of “ragged red” fibers, consistent with a mitochondrial cytopathy. e Quantification of Gly/Ser ratio in fibroblasts from control individuals (CTL, n = 6) and patients (SHMT2, n = 5). f 5′-Methyl THF (tetrahydrofolate) normalized to total folate levels in fibroblasts from control individuals (CTL, n = 5) and patients (SHMT2, n = 5). g Measure of ATP concentration in control individuals (CTL, n = 6) and patients (SHMT2, n = 5) fibroblasts after 24-h incubation in a medium without glucose. Values were normalized by number of cells. Quantification depicted as fold change to control fibroblasts. h Quantification of mitochondrial oxygen consumption rates (OCR, pmol O2/min/1000 cells) in control individuals (CTL, n = 5) and patients (SHMT2, n = 4). i Shmt2 knockdown in motoneurons cause neuromuscular junction (NMJ) and motility defects in Drosophila. Left: immunofluorescence images of the neuromuscular junctions of muscle 4 segment A2–A3 stained with the presynaptic marker horseradish peroxidase (HRP, arrowhead). Right: quantification of the average number of satellite boutons, climbing distance and velocity in control (eGFP) and mutant (Shmt2 RNAi #1, #2) flies (n = 15-18 for boutons, n = 30 for distance and velocity). In e–h, values are expressed as mean ± SD, and two-tailed Student t tests were performed; in i, values are expressed as mean ± SEM, and one-way ANOVA with Tukey’s multiple comparisons test was performed (*p < 0.05, **p < 0.01, ***p < 0.001)
To assess the pathogenicity of SHMT2 variants, we pursued functional testing with patient-derived primary fibroblasts. SHMT2 protein levels in fibroblasts were not significantly altered (Supplementary Fig. 13). While all metabolites were in the normal range in plasma, fibroblasts from affected individuals showed a significant decrease in glycine/serine ratios compared to controls. Folate metabolism was also impaired: 5-methyltetrahydrofolate levels were increased in patients in relation to total folate (Fig. 1e, f). The substrate of SHMT2 tetrahydrofolate (THF) was undetectable in mitochondria-enriched control fibroblast samples, but low levels of this molecule were detectable in extracts from patient fibroblasts (Supplementary Table 5). These data support the impairment of SHMT2 enzymatic function in these patients. Because folate and serine are required for proper mitochondrial translation [11, 12], we verified levels of mitochondrial OXPHOS complexes, which did not vary (Supplemental Fig. 14).
Next we analyzed bioenergetic and mitochondrial function in patients’ fibroblasts, which were described to be impaired in knockout human cancer cell lines [11, 12]. ATP measurements, as well as extracellular flux analysis in a Seahorse device, under glucose restriction conditions, indicated an impaired oxidative capacity in patients’ cells relative to controls (Fig. 1g, h, Supplementary Fig. 15). Mitochondrial membrane potential was found to be altered, as well as ROS levels (both total and mitochondrial), supporting mitochondrial redox metabolism malfunction (Supplementary Fig. 16).
In previous works, Shmt2 knockout mice exhibited embryonic lethality, attributed to severe mitochondrial respiration defects in fetal liver, and ensuing inhibition of erythroblast differentiation resulting in anemia. Moreover, metabolic defects were not observed in brain tissue, possibly due to the preferential use of the glycine cleavage system to provide one-carbon units [17]. To investigate whether the patients’ neurological phenotype could be mediated by non-neuronal autonomous mechanisms, we knocked down Shmt2 specifically in Drosophila motor neurons (~ 65% knockdown of Shmt2 RNA as shown previously by qPCR) [3]. We analyzed the morphology of presynaptic terminals at neuromuscular junctions (NMJs), which reliably model excitatory synapses in the mammalian brain and spinal cord [2]. While no changes in the numbers of total boutons or mature boutons were observed in Shmt2-knockdown animals compared with eGFP controls, we found a significant increase in the numbers of satellite boutons, emerging from the main nerve terminal or budding excessively from primary boutons and forming clusters (Fig. 1i, Supplementary Fig. 17). Of note, previous studies have shown increased satellite boutons in Drosophila models for Amyotrophic Lateral Sclerosis and Spastic Paraplegia [7, 16]. Moreover, mutant flies showed reduced climbing distance and velocity compared to eGFP control animals (Fig. 1i). These results may reflect a role for human SHMT2 in the maintenance of presynaptic vesicles, and can be attributed to a selective decrease of Shmt2 in neurons, without any significant systemic interfering effects. Thus, these studies argue against non-cell autonomous mechanisms from the periphery causing neuronal malfunction in patients.
Interestingly, this novel rare disease entity corresponds faithfully to an intersection of diverse clinical manifestations associated with defects in metabolic pathways in which SHMT2 plays a crucial role, such as amino acid and folate metabolism and mitochondrial homeostasis [4, 11, 12]. SHMT2 impairment alters intracellular glycine/serine levels, which provides the main source of mitochondrial one-carbon units in proliferating cells, and thus probably contributes to microcephaly and polymicrogyria [9, 10, 13]. Microcephaly associated with hypomyelination is also seen in patients with loss of PYCR2, an enzyme of proline synthesis which interacts with SHMT2, causing hyperglycinemia, underscoring the impact of dysregulated glycine/serine levels on neurodevelopment [6]. SHMT2 malfunction also depletes a downstream product species, 5,10-methylTHF, required for nucleotide metabolism [1, 5]. Microcephaly, developmental delay/intellectual disability and cardiomyopathy have been extensively described in defects of folate metabolism [14]. In summary, we describe a novel neurodevelopmental, syndromic encephalopathy and movement disorder associated with cardiac defects. Despite a certain degree of variable severity, clinical manifestations were consistent in all individuals and thus establish a well-defined and recognizable clinical syndrome of defective folate and amino acid metabolism.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Acknowledgements
We are indebted to the families who participated in this study. We thank CERCA Program/Generalitat de Catalunya for institutional support. We thank Cristina Guilera and Juanjo Martínez for excellent technical assistance at Neurometabolic Diseases Lab. We thank the Mayo Clinic Mitochondrial Disease Center for excellent support. This study was supported by the Centre for Biomedical Research on Rare Diseases (CIBERER) [ACCI14-759], [ACCI19-26], the URDCat program (PERIS SLT002/16/00174), the Fondo de Investigación Sanitaria FIS PI17/00916 (ISCIII) (co-funded by European Regional Development Fund. ERDF, a way to build Europe), the Hesperia Foundation, and the Secretary for Universities and Research of the Ministry of Business and Knowledge of the Government of Catalonia [2017SGR1206] to AP. AGC and NJP were funded by Fondo de Investigación Sanitaria (FIS) P118/00111 (Instituto de Salud Carlos III: ISCIII and “Fondo Europeo de desarrollo regional” FEDER). RA was funded by FIS PI17/00109 (ISCIII). EV was funded by grants from the Ministerio de Economia, Industria y Competividad (Juan de la Cierva program FJCI-2016-28811) and Instituto de Salud Carlos III (Sara Borrell program, CD19/00221). SF was funded by the Instituto de Salud Carlos III [Miguel Servet program CPII16/00016, co-funded by European Social Fund. ESF investing in your future]. MR was funded by CIBERER. LPS and AJP were funded by predoctoral grants from the Instituto de Salud Carlos III (PFIS, FI18/00141 and FI18/00253). EK and MC were funded by the Center for Individualized Medicine at Mayo Clinic. ET and CF were funded by a grant from the NIH (HL121079), the Anne Dash Weinman Fund in Cardiovascular Research Honoring Steven J. Lester, and the Nasser Al-Rashid Fund for Research in Cardiovascular Diseases. AP and EWK are members of the Undiagnosed Diseases Network International (UDNI). We are indebted to the “Biobanc de l’Hospital Infantil Sant Joan de Déu per a la Investigació” integrated in the Spanish Biobank Network of ISCIII for the sample and data procurement of patient 3. MZ and ND were supported in part by The Linda T. and John A. Mellowes Endowed Innovation and Discovery Fund and the Genomic Sciences and Precision Medicine Center of Medical College of Wisconsin.
SHMT2 Working Group: Alfonso Oyarzábal, Inés Medina, Aida Ormazábal, Jordi Muchart, Juan Manuel Carretero, Cristina Jou, Mireia del Toro, Andrés Nascimento, Abraham J. Paredes, Delia Yubero, Roser Colomé. Neurometabolic Unit and Synaptic Metabolism Lab, Neurology Department, Institut Pediàtric de Recerca, Hospital Sant Joan de Déu, and MetabERN, 08950, Barcelona, Catalonia, Spain: AlOy, IM, AiOr, JM, JMC, RC. Centre for Biomedical Research on Rare Diseases (CIBERER), Instituto de Salud Carlos III, 28029, Madrid, Spain: AlOy, AiOr, CJ, AJP, DY, RC. Pathology Department, Institut de Recerca Sant Joan de Déu, and MetabERN, 08950, Barcelona, Catalonia, Spain: CJ. Pediatric Neurology Department, Vall d’Hebron University Hospital, Universitat Autònoma de Barcelona, 08916, Barcelona, Spain: MdT. Neuromuscular Unit, Neurology Department, Institut Pediàtric de Recerca, Hospital Sant Joan de Déu, 08950, Barcelona, Catalonia, Spain: AN. Clinical Biochemistry and Genetics Departments, Institut de Recerca Sant Joan de Déu, and MetabERN, 08950, Barcelona, Catalonia, Spain: AJP, DY.
Author contributions
Conceptualization: AGC, EV, MAC, and AP. Funding acquisition: AGC, SB, EWK, SF, UP, RA, MAC, and AP. Performed research and experiments: AGC, EV, NJP, ENA, LG, ET, NRD, AS, RU, LPS, JMT, RHG, SWG, MR, SF, ARP, BC, TB, MV, CF, MTZ, UP, and RA. Supervision: AGC, RA, MAC, and AP. Writing of the original draft: AGC, EVP, MAC, and AP. All authors contributed to revising the manuscript.
Compliance with ethical standards
Conflict of interest
The authors have declared that no conflict of interest exists.
Footnotes
The members of SHMT2 Working Group are listed in the Acknowledgements section.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Àngels García-Cazorla and Edgard Verdura contributed equally to this study.
Margot A. Cousin and Aurora Pujol contributed equally to this study.
Contributor Information
Àngels García-Cazorla, Email: agarcia@sjdhospitalbarcelona.org.
Aurora Pujol, Email: apujol@idibell.cat.
SHMT2 Working Group:
Alfonso Oyarzábal, Inés Medina, Aida Ormazábal, Jordi Muchart, Juan Manuel Carretero, Cristina Jou, Mireia del Toro, Andrés Nascimento, Abraham J. Paredes, Delia Yubero, and Roser Colomé
References
- 1.Acuna-Hidalgo R, Schanze D, Kariminejad A, Nordgren A, Kariminejad MH, Conner P, et al. Neu-Laxova syndrome is a heterogeneous metabolic disorder caused by defects in enzymes of the l-serine biosynthesis pathway. Am J Hum Genet. 2014;95:285–293. doi: 10.1016/j.ajhg.2014.07.012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Budnik V. Synapse maturation and structural plasticity at Drosophila neuromuscular junctions. Curr Opin Neurobiol. 1996;6:858–867. doi: 10.1016/s0959-4388(96)80038-9. [DOI] [PubMed] [Google Scholar]
- 3.Celardo I, Lehmann S, Costa AC, Loh SH, Martins LM. DATF4 regulation of mitochondrial folate-mediated one-carbon metabolism is neuroprotective. Cell Death Differ. 2017;24:638–648. doi: 10.1038/cdd.2016.158. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Ducker GS, Rabinowitz JD. One-carbon metabolism in health and disease. Cell Metab. 2017;25:27–42. doi: 10.1016/j.cmet.2016.08.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.El-Hattab AW. Serine biosynthesis and transport defects. Mol Genet Metab. 2016;118:153–159. doi: 10.1016/j.ymgme.2016.04.010. [DOI] [PubMed] [Google Scholar]
- 6.Escande-Beillard N, Loh A, Saleem SN, Kanata K, Hashimoto Y, Altunoglu U, et al. Loss of PYCR2 causes neurodegeneration by increasing cerebral glycine levels via SHMT2. Neuron. 2020;107:82–94.e6. doi: 10.1016/j.neuron.2020.03.028. [DOI] [PubMed] [Google Scholar]
- 7.Estes PS, Boehringer A, Zwick R, Tang JE, Grigsby B, Zarnescu DC. Wild-type and A315T mutant TDP-43 exert differential neurotoxicity in a Drosophila model of ALS. Hum Mol Genet. 2011;20:2308–2321. doi: 10.1093/hmg/ddr124. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Giardina G, Brunotti P, Fiascarelli A, Cicalini A, Costa MG, Buckle AM, et al. How pyridoxal 5’-phosphate differentially regulates human cytosolic and mitochondrial serine hydroxymethyltransferase oligomeric state. FEBS J. 2015;282:1225–1241. doi: 10.1111/febs.13211. [DOI] [PubMed] [Google Scholar]
- 9.De Koning TJ, Duran M, Dorland L, Gooskens R, Van Schaftingen E, Jaeken J, et al. Beneficial effects of l-serine and glycine in the management of seizures in 3-phosphoglycerate dehydrogenase deficiency. Ann Neurol. 1998;44:261–265. doi: 10.1002/ana.410440219. [DOI] [PubMed] [Google Scholar]
- 10.De Koning TJ, Klomp LWJ. Serine-deficiency syndromes. Curr Opin Neurol. 2004;17:197–204. doi: 10.1097/00019052-200404000-00019. [DOI] [PubMed] [Google Scholar]
- 11.Minton DR, Nam M, McLaughlin DJ, Shin J, Bayraktar EC, Alvarez SW, et al. Serine Catabolism by SHMT2 Is Required for Proper Mitochondrial Translation Initiation and Maintenance of Formylmethionyl-tRNAs. Mol Cell. 2018;69:610.e5–621.e5. doi: 10.1016/j.molcel.2018.01.024. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Morscher RJ, Ducker GS, Li SH, Mayer JA, Gitai Z, Sperl W, Rabinowitz JD. Mitochondrial translation requires folate-dependent tRNA methylation. Nature. 2018;554:128–132. doi: 10.1038/nature25460. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Murtas G, Marcone GL, Sacchi S, Pollegioni L. l-serine synthesis via the phosphorylated pathway in humans. Cell Mol Life Sci. 2020 doi: 10.1007/s00018-020-03574-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Pope S, Artuch R, Heales S, Rahman S. Cerebral folate deficiency: analytical tests and differential diagnosis. J Inherit Metab Dis. 2019;42:655–672. doi: 10.1002/jimd.12092. [DOI] [PubMed] [Google Scholar]
- 15.Saudubray J-M, Baumgartner M, Walter J. Inborn metabolic diseases, diagnosis and treatment. 2016. New York: Springer; 2016. [Google Scholar]
- 16.Sherwood NT, Sun Q, Xue M, Zhang B, Zinn K. Drosophila spastin regulates synaptic microtubule networks and is required for normal motor function. PLoS Biol. 2004 doi: 10.1371/journal.pbio.0020429. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Tani H, Mito T, Velagapudi V, Ishikawa K, Umehara M, Nakada K, et al. Disruption of the mouse Shmt2 gene confers embryonic anaemia via foetal liver-specific metabolomic disorders. Sci Rep. 2019;9:16054. doi: 10.1038/s41598-019-52372-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Tani H, Ohnishi S, Shitara H, Mito T, Yamaguchi M, Yonekawa H, et al. Mice deficient in the Shmt2 gene have mitochondrial respiration defects and are embryonic lethal. Sci Rep. 2018;8:425. doi: 10.1038/s41598-017-18828-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Walden M, Tian L, Ross RL, Sykora UM, Byrne DP, Hesketh EL, et al. Metabolic control of BRISC–SHMT2 assembly regulates immune signalling. Nature. 2019;570:194–199. doi: 10.1038/s41586-019-1232-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.