Abstract
We present a case of a 28-year-old woman with a history of severe headaches and pituitary insufficiency. She was found to have a large, enhancing, sellar mass consistent with a pituitary adenoma. The patient's surgical care was delayed due to the coronavirus disease 2019 (COVID-19) pandemic, and follow-up imaging revealed spontaneous involution of the sellar mass. Spontaneous involution of pituitary masses has been described but not often encountered in clinical practice. This case highlights that follow-up imaging is necessary when scheduling elective surgeries during the COVID-19 pandemic.
Key words: COVID-19, Pituitary adenoma, Pituitary apoplexy
Abbreviations and Acronyms: COVID-19, Coronavirus disease 2019; CT, Computed tomography; MRI, Magnetic resonance imaging
Pituitary adenomas can undergo ischemic infarction or hemorrhagic transformation in pituitary apoplexy, a well-defined syndrome characterized by headache, vision loss, cranial nerve dysfunction, and pituitary hormone dysfunction.1 , 2 We present a case of a 28-year-old woman who presented to our outpatient clinic with severe headaches that began several months before our consultation. She presented with hypopituitarism that necessitated cortisol and thyroid supplementation. She never received high-dose glucocorticoid treatment. Vision was normal. Magnetic resonance imaging (MRI) demonstrated an enhancing mass within the pituitary sella measuring 1.9 × 1.8 × 2.7 cm (craniocaudad by anteroposterior by axial) with a Knosp 3A cavernous sinus invasion bilaterally (Figure 1A and B ).3 Imaging was most consistent with a pituitary adenoma with possible antecedent apoplexy. We recommended endonasal transsphenoidal resection; however, the surgery was delayed due to the novel coronavirus disease 2019 (COVID-19) outbreak.
Figure 1.
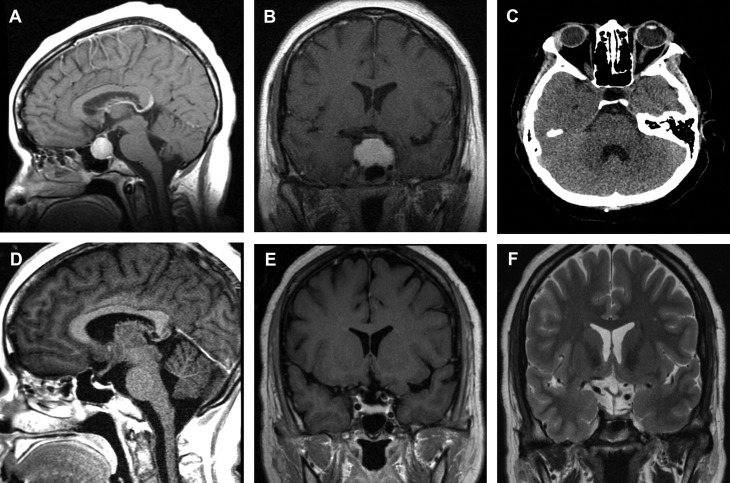
(A and B) Sagittal and coronal plane reformats of magnetic resonance imaging (MRI) brain T1 sequence with gadolinium contrast revealing a large enhancing mass in the sella turcica with Knosp 3A cavernous sinus invasion bilaterally. The mass is avidly enhancing and abuts the optic chiasm. The imaging is most consistent with a pituitary adenoma. (C) Computed tomography of the head without contrast reveals hypodensity within an enlarged sella turcica. The previously noted pituitary mass is no longer observed. (D and E) Sagittal and coronal plane reformats of MRI brain T1 sequence with gadolinium contrast reveals resolution of the previously noted pituitary adenoma. There is a thin rim of enhancing tissue in the sella consistent with residual pituitary gland or scant tumor. (F) Coronal plane reformat of MRI brain T2 sequence without contrast without contrast.
After the initial COVID-19 surge in the United States, we rescheduled the patient's surgery. Notably, the patient did not become pregnant, nor did she develop a sudden headache or altered mental status to suggest apoplexy before our rescheduled surgery date. Before the surgery, we obtained a computed tomography (CT) without contrast with thin cuts through the skull base for approach planning purposes (Figure 1C). The CT was completed 6 months after the previous MRI. The CT revealed hypodensity within the previously-enlarged sella turcica consistent with an “empty sella.” There was no mass within the sella turcica. A repeat MRI was obtained that revealed resolution of the bulk of the pituitary adenoma with a thin rim of enhancing tissue at the caudad portion of the sella consistent with pituitary gland or scant residual tumor (Figure 1D, E, and F). We cancelled the patient's surgery and have elected to obtain a repeat MRI in 6 months to inspect for recurrence of the pituitary adenoma.
While pituitary apoplexy can present as a neurosurgical emergency, it can also cause involution of a pituitary adenoma.4, 5, 6 This event is not often observed in clinical setting, as most symptomatic pituitary apoplexies warrant neurosurgical intervention.2 In addition, resolution of pituitary masses due to hypophysitis has been described after the administration of high-dose glucocorticoids, but this patient only received physiological cortisol replacement before the procedure.7 This case was delayed due to the COVID-19 pandemic, which emphasizes the need for routine imaging surveillance if there is delay in surgical management of a pituitary mass. In the cases of mildly symptomatic pituitary apoplexy, resolution of the pituitary adenoma can obviate the need for surgical intervention.
Footnotes
Conflict of interest statement: Dr. David P. Bray is partially supported by the Nell W. and William S. Elkin Research Fellowship in Oncology, Winship Cancer Institute, Emory University Hospital, Atlanta, Georgia, USA.
References
- 1.Bailey P. Pathological report of a case of acromegaly, with special reference to the lesions in the hypophysis cerebri and in the thyroid gland, and a case of hemorrhage into the pituitary. Phila Med J. 1898;1:789–792. [Google Scholar]
- 2.Verrees M., Arafah B.M., Selman W.R. Pituitary tumor apoplexy: characteristics, treatment, and outcomes. Neurosurg Focus. 2004;16:1–7. doi: 10.3171/foc.2004.16.4.7. [DOI] [PubMed] [Google Scholar]
- 3.Micko A.S.G., Wöhrer A., Wolfsberger S., Knosp E. Invasion of the cavernous sinus space in pituitary adenomas: endoscopic verification and its correlation with an MRI-based classification. J Neurosurg. 2015;122:803–811. doi: 10.3171/2014.12.JNS141083. [DOI] [PubMed] [Google Scholar]
- 4.Villar-Taibo R., Ballesteros-Pomar M.D., Vidal-Casariego A., Álvarez-San Martín R.M., Kyriakos G., Cano-Rodríguez I. Spontaneous remission of acromegaly: apoplexy mimicking meningitis or meningitis as a cause of apoplexy? Arq Bras Endocrinol Metabol. 2014;58:76–80. doi: 10.1590/0004-2730000002701. [DOI] [PubMed] [Google Scholar]
- 5.Robinson D.B., Michaels R.D. Empty sella resulting from the spontaneous resolution of a pituitary macroadenoma. Arch Intern Med. 1992;152:1920–1923. [PubMed] [Google Scholar]
- 6.Fraser L.A., Lee D., Cooper P., Van Uum S. Remission of acromegaly after pituitary apoplexy: case report and review of literature. Endocr Pract. 2009;15:725–731. doi: 10.4158/EP09126.CRR. [DOI] [PubMed] [Google Scholar]
- 7.Park S.M., Bae J.C., Joung J.Y., et al. Clinical characteristics, management, and outcome of 22 cases of primary hypophysitis. Endocrinol Metab. 2014;29:470–478. doi: 10.3803/EnM.2014.29.4.470. [DOI] [PMC free article] [PubMed] [Google Scholar]