To the Editor,
The spread of the coronavirus disease 2019 (COVID‐19) remains a worsening global health crisis. Although many studies have reported risk factors for severe COVID‐19, asthma characterization in COVID‐19 is still controversial, with different early reports from China and recent reports from Europe and the United States. 1 Prolonged viral shedding is a risk factor for poor outcome of COVID‐19 and may assist in inferring the immunological mechanism of virus elimination; however, no large‐scale studies have explored this subject. 2
Daegu Metropolitan City, the fourth largest city in the Republic of Korea with a population of 2.5 million, collected and shared a database of COVID‐19 patients hospitalized in 10 large general hospitals. This study used the database to evaluate the prevalence of asthma and clinical outcomes of COVID‐19 according to asthma in adult patients. The risk factors for delayed viral clearance were also evaluated.
A total of 2311 patients were registered in the database; 46 duplicated cases and 65 pediatric cases were excluded, leading to 2200 patients in the final analysis. The prevalence of asthma in patients with COVID‐19 was 3.2% which was similar to the prevalence of asthma in the Korea National Health and Nutrition Examination Survey (KNHANES) (Figure 1A and Table S1). The general pattern of the prevalence of asthma by age‐group in the KHANES was U‐shaped, and the prevalence in patients with COVID‐19 was similar but was lower in the 19‐29‐year age‐group (2.1%) (Figure 1B).
FIGURE 1.
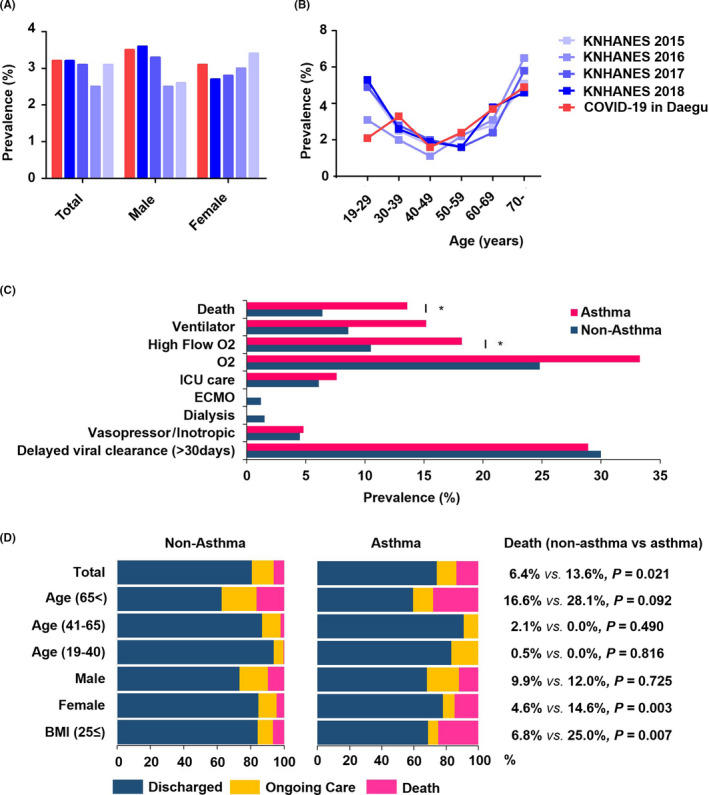
Characterization of asthma in adult COVID‐19 inpatients. (A) Prevalence of asthma in COVID‐19 and in the KNHANES. (B) Prevalence by age‐group in COVID‐19 and in the KNHANES. (C) Univariate analysis of clinical outcomes according to asthma. (D) Death and ongoing care according to the asthma subgroups. Abbreviations: KNHANES, Korea National Health and Nutrition Examination Survey; COVID‐19, coronavirus disease‐2019; ICU, intensive care unit; BMI, body mass index. *P < .05
Table S2 compares the characteristics between the asthma group and the nonasthma group. Older age (>65 years), overweight (BMI ≥25.0), and comorbidity of chronic obstructive pulmonary disease, and initially presented with dyspnea and nausea/vomiting were more common in the asthma group. Compared with the nonasthma group, the asthma group had a higher mortality rate (13.6% vs 6.4%, P = .02) and a greater need for high‐flow oxygen therapy (18.2% vs 10.5%, P = .048) (Figure 1C and Table S3). The higher mortality rate in asthma patients was particularly noticeable in older patients, overweight patients, and females. (Figure 1D). However, after adjusting for potential confounders, asthma had no significant association with clinical outcomes of COVID‐19 (Figure 2A and Table S4). Meanwhile, older age, male gender, and comorbid diseases including overweight, diabetes, chronic kidney disease, cancer, autoimmune disease, dementia, and other psychological disorder were significant risk factors for mortality (Tables S5 and S6).
FIGURE 2.
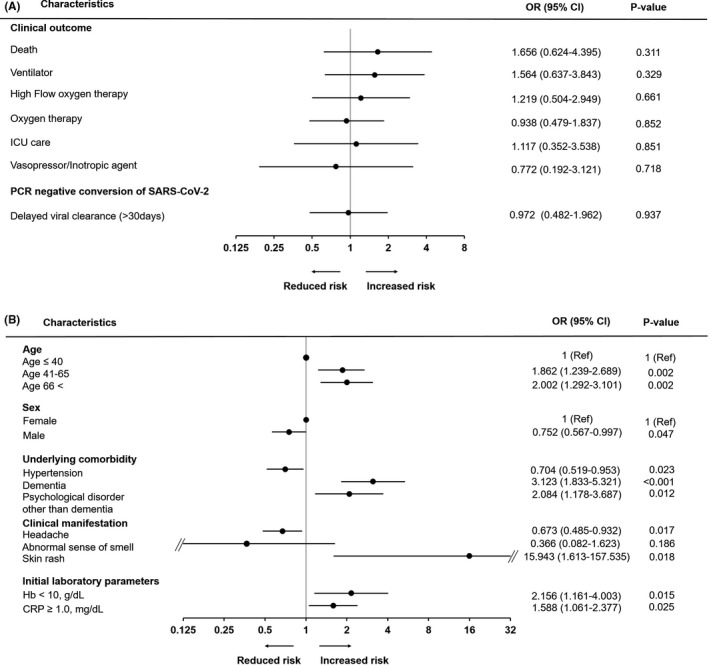
(A) Forest plot showing odds ratios (ORs) of asthma for the clinical outcomes. (B) Forest plot showing odds ratios (ORs) for risk factors for delayed viral clearance (>30 d) of total patients (N = 1321; the nondelayed viral clearance group = 906, the delayed viral clearance group = 415). ORs are adjusted for age, sex, body mass index, smoking history, underlying comorbidity, and medication for COVID‐19 by multivariate logistic regression model. Abbreviations: PCR, polymerase chain reaction; SARS‐CoV‐2, severe acute respiratory syndrome coronavirus 2; COVID‐19, coronavirus disease 2019; Hb, hemoglobin; CRP, C‐reactive protein
In multivariate analysis, asthma was not a risk factor for death. However, asthma, a heterogeneous disease, may affect COVID‐19 differently depending on asthma phenotype. Early‐onset allergic asthma is often accompanied by type 2 inflammation, while asthma in obesity and elderly is more frequently accompanied by non–type 2 inflammation. 3 Recent studies have reported higher expression of angiotensin‐converting enzyme 2 (ACE2) and transmembrane protease, serine 2 (TMPRSS2) in respiratory samples of neutrophilic inflammation compared to eosinophilic inflammation asthma. 4 The low prevalence of COVID‐19 infection in those younger than 30 years old and a relatively high mortality rate in patients who were female, overweight, and elderly in our study suggest that neutrophilic asthma may be a risk factor for infection and poor prognosis of COVID‐19. 5
In order to analyze the risk factors of delayed viral clearance, patients were divided into two groups. The nondelayed viral clearance group was defined as patients with two consecutive negative real‐time RT‐PCR results at intervals of ≥24 hours within 30 days since diagnosis. The delayed viral clearance group was defined as patients with a positive real‐time RT‐PCR test after 30 days, without two consecutive negative RT‐PCR results. So, 906 patients were included in the nondelayed viral clearance group and 415 patients in the delayed viral clearance group. After adjusting for potential confounders, delayed viral clearance was not significantly associated with asthma (Figure 1E and Table S4). Older age, underlying dementia and psychological disorders other than dementia, initial symptom of skin rash, and initial laboratory abnormalities of hemoglobin <10 g/dL and C‐reactive protein (CRP) ≥1.0 mg/dL were significant risk factors for delayed viral clearance. On the other hand, male sex, hypertension, and initial symptom of headache reduced the risk for delayed viral clearance (Figure 2B and Table S7). When limited to patients with no activity limitation (mild COVID‐19 group), older age, dementia, initial symptoms of skin rash and headache, and initial hemoglobin < 10 g/dL still showed significant differences (Table S8).
Dementia and older age are identified as important risk factors for delayed viral clearance, while nervous system symptoms such as headaches and an abnormal sense of smell reduced the risk for delayed viral clearance. Previous studies have shown that coronavirus can initially invade the peripheral nerves and enter the central nervous system. 6 The immunological function of the brain is altered and dysregulated in neurodegenerative diseases, 7 and it has also been reported that local neurological symptoms such as headache and olfactory symptoms may be a biomarker of the magnitude of a host's innate immune response to virus. 8 It can be hypothesized that the immunological mechanism of detecting and removing viruses that have infiltrated the central nervous system in COVID‐19 is important for virus clearance. Anemia and skin rash, which was associated with increased risk, may also be related to the mechanism of virus clearing, and further research on the mechanism is needed. Since male sex, hypertension, and elevated CRP did not show a significant difference in the mild COVID‐19 group, they may be more closely associated with severity of disease rather than viral clearance.
These data did not include asymptomatic or minimal symptomatic patients who did not require hospitalization. However, our study covered almost all hospitalized patients diagnosed with COVID‐19 in Daegu from February 2020 to May 2020, minimizing selection bias. 9 In addition, because most hospitals, following the guidance from the Korea Centers for Disease Control & Prevention, employed similar protocols for discharge from quarantine and RT‐PCR follow‐up testing, we were able to analyze the risk factors for viral clearance in a relatively large number of patients.
In summary, despite the differences depending on phenotypes, the prevalence of asthma was not significantly different in patients with COVID‐19, and asthma did not affect the outcomes of COVID‐19 in multivariate analysis. Dementia, older age, and initial presentation of skin rash and anemia were independently associated with delayed viral clearance. On the other hand, in patients with headache initially, the viral clearance time was shortened.
CONFLICTS OF INTEREST
The authors declare no competing financial interest.
Supporting information
Tab S1‐S7
App S1
ACKNOWLEDGMENTS
This work was supported by the Research Program of Medicity Daegu Council funded by Daegu Metropolitan City (fund code COVID19_DM05).
Kim and Jung these authors contributed equally to this work
Contributor Information
Hyun Jung Jin, Email: jhj0619@yu.ac.kr.
Han‐Ki Park, Email: haan33@gmail.com.
REFERENCES
- 1. Johnston SL. Asthma and COVID‐19: is asthma a risk factor for severe outcomes? Allergy. 2020;75:1543‐1545. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Yan D, Liu X‐Y, Zhu Y‐N, et al. Factors associated with prolonged viral shedding and impact of Lopinavir/Ritonavir treatment in hospitalised non‐critically ill patients with SARS‐CoV‐2 infection. Eur Respir J. 2020;56(1):2000799. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Wenzel SE. Asthma phenotypes: the evolution from clinical to molecular approaches. Nat Med. 2012;18(5):716‐725. [DOI] [PubMed] [Google Scholar]
- 4. Bradding P, Richardson M, Hinks TS, et al. ACE2, TMPRSS2 and furin gene expression in the airways of people with asthma–implications for COVID‐19. J Allergy Clin Immunol. 2020;146:208‐211. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Jesenak M, Banovcin P, Diamant Z. COVID‐19, chronic inflammatory respiratory diseases and eosinophils–Observations from reported clinical case series. Allergy. 2020;75(7):1819‐1822. [DOI] [PubMed] [Google Scholar]
- 6. Narasaraju T, Tang BM, Herrmann M, et al. Neutrophilia and NETopathy as key pathologic drivers of progressive lung impairment in patients with COVID‐19. Front Pharmacol. 2020;11:870. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Vellingiri B, Jayaramayya K, Iyer M, et al. COVID‐19: a promising cure for the global panic. Sci Total Environ. 2020;725:138277. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. Ejlerskov P, Hultberg JG, Wang J, et al. Lack of neuronal IFN‐β‐IFNAR causes Lewy body‐and Parkinson's disease‐like dementia. Cell. 2015;163(2):324‐339. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Eliezer M, Hautefort C, Harmel AL, et al. Sudden and complete olfactory loss function as a possible symptom of COVID‐19. JAMA Otolaryngol Head Neck Surg. 2020;146(7):674‐675. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Tab S1‐S7
App S1


