Abstract
This study was aimed at investigating the phytochemical constituents, antifungal properties and antibiotic-modifying activity of the aqueous crude extract and fractions of Amburana cearensis seeds (CEFAC). The CEFAC were chemically characterized by LC–MS/MS–QTOF. In addition, the antifungal activity was assayed by the microdilution method against strains of Candida albicans. The phytochemical profile of CEFAC exhibited phenolic compounds, organic acids, and polyphenols. The results of the assessment of antifungal activity reveled an IC50 ranging from 45.6 to 2048 µg/mL. Interestingly, when CEFAC was associated with Fluconazole, we evidenced a decreased IC50 (1.81–11.9 µg/mL), suggesting a synergism with antibiotic. It was possible to identify in the crude extract and fractions several phenolic compounds, organic acids, and some polyphenols in positive ionization mode. These results suggest that CEFAC may present compounds with the ability to interact and act synergistically with antimicrobial drugs, highlighting its potential as an alternative source for the development of new antimicrobial agents.
Keywords: Amburana cearensis, Candida spp., Fungistatic, Fluconazole
Introduction
The fungi are part of the human microbiota (Siqueira and Sen 2004) and important etiological agents of human diseases, due to its ability to modulate the expression of virulence factors such as host cell adhesion, hyphae formation, phenotypic plasticity and production of hydrolytic enzymes. The genus Candida is the most widespread opportunistic fungal pathogen in the human body, causing mucosal and systemic infections, especially among immunosuppressed and hospitalized patients (Goulart et al. 2018). Due to the wide use of antifungal agents, drug resistance of Candida albicans is increasing, which poses a serious threat to antifungal therapy (Ksiezopolska and Gabaldõn 2018). Therefore, exploring new effective antifungal agents is urgently needed.
In this sense, natural products have been reported as sources of various bioactive molecules that may pave the way for novel antifungal agents (Ksouri et al. 2017; Zida et al. 2017). In addition, studies are carried out to promote the combination of antifungal drugs and natural products against resistant Candida strains (Calixto Jr. et al. 2015), which can be a strongly promise to face this challenge.
Amburana cearensis (Allemao) A. C. Sm., Fabaceae family (Papilionoideae, Leguminosae) is naturally widespread in Caatinga, northeastern Brazil (Bravo et al. 1999). The medicinal use of A. cearensis is common, especially in the treatment of headaches, muscle aches, constipation, and urinary tract infections (Leal et al. 2003; Agra et al. 2007; Lima et al. 2013). Several compounds with antioxidant and antimicrobial properties have been isolated from A. cearensis seeds, including coumarins, methyl esters, phytosterols (γ-sitosterol, stigmasterol, and campesterol) (Calixto Jr. et al. 2015; Pereira et al. 2017; Zida et al. 2017). Thus, the aqueous crude extract and fractions of A. cearensis seeds were subjected to chemical characterization and antifungal assessments to verify whether they present any potential to induce a synergistic effect when combined with Fluconazole against C. albicans.
Materials and methods
Plant material
Amburana cearensis seeds were identified and provided by Floresta Nacional de Nísia, a Conservation Unit managed by the Chico Mendes Institute for Biodiversity Conservation (ICMBio), located in the municipality of Nísia Floresta, state of the Rio Grande do Norte, Brazil, and the Caatinga Seed Network (UNIVASF).
Extraction and fractionation
The extraction was performed by homogenizing the seed powder of A. cearensis with 50 mM Tris–HCl solution, pH 7.5, ratio 1:10 (m/v), under constant agitation for 4 h at 4 °C and then centrifuged at 10,000×g for 30 min at the same temperature. The material was filtered, and the supernatant was identified as crude extract (CE). Then, CE was fractionated into three ammonium sulfate concentration ranges: 0–30% (FR-1), 30–60% (FR-2) and 60–90% (FR-3) of saturation. After each precipitation step, the sample was maintained at 4 °C for approximately 16 h and then centrifuged at 10,000×g for 30 min at 4 °C. The fractions were then resuspended and dialyzed for 20 h using distilled water. After dialysis, the fractions were lyophilized and stored at room temperature.
Identification of compounds by ultra-performance liquid chromatography-quadrupole\time-of-flight (UPLC–QTOF) system
The analysis was performed on ACQUITY UPLC (Waters), coupled to quadrupole/time-of-flight system (QTOF, Waters) by Brazilian Agricultural Research Corporation (EMBRAPA). The chromatographs were performed on a column Waters ACQUITY UPLC BEH (150 × 2.1 mm, 1.7 µm), fixed temperature of 40 °C, mobile water phases with 0.1% of formic acid (A) and acetonitrile with 0.1% formic acid (B), gradient ranging from 2 to 95% B (15 min), 0.4 mL/min flow and 5-µL injection volume. The ESI˗ mode was purchased in the 110–1180 Da, fixed source temperature at 120 °C, desolvation temperature at 350 °C, desolvation gas flow at 500 L/h, extraction cone of 0.5 V and 2.6 kV of capillary voltage. The ESI + mode was purchased in the 110–1180 Da, fixed source temperature at 120 °C, desolvation temperature at 350 °C, desolvation gas flow at 500 L/h and 3.2 kV of capillary voltage. Encephalin leucine was used as lock mass. The acquisition mode was MSE. The instrument was controlled by the software Masslynx 4.1 (Waters Corporation).
Antifungal assays
Strains and culture medium
The strains used in this study were standard type and isolated from Cultura Oswaldo Cruz (FIOCRUZ), Instituto Nacional de Controle de Qualidade em Saúde (INCQS), specifically CA INCQS 40006 and CA URM 4125, standard and isolated strain, respectively. The strains were inoculated on Sabouraud Dextrose Agar (SDA, KASVI) and incubated for 24 h at 37 °C. Subsequently, aliquots of the yeast were transported to test tubes, each containing 3 mL of sterile saline (0.9%). Inoculum concentration was standardized by comparison with the 0.5 McFarland scale (barium chloride) (NCCLS 2012). Sabouraud Dextrose (SD, HIMEDIA) in double concentration was used in the microdilution assay.
Chemicals and reagents
Dimethyl sulfoxide (DMSO, Merck, Germany) was used to fluidize the CE and fractions, while Fluconazole (Capsule—Prati Donaduzzi, Brazil) was diluted with distilled water and used as reference drug. The test solution was prepared by weighing 0.15 g of the CE and fractions and diluting with 1 mL of DMSO to obtain the desired concentration. Samples were diluted in sterile distilled water (16.384 μg/mL) such that DMSO had no activity on the tested cells (Stoppa et al. 2009).
IC50 and cell viability
To determine the concentration capable of inhibiting 50% of yeast growth (IC50), the CE and fractions isolated or combined with Fluconazole were tested by microdilution method in Sabouraud Dextrose broth in 96-well microplates with initial concentration of 16.384 μg/mL, and serially diluted to a final concentration of 8 μg/mL (Javadpour et al. 1996; Morais-Braga et al. 2016). Controls were also prepared for the diluents using 0.9% sodium chloride solution instead of inoculum. All tests were performed in quadruplicates. The plates were incubated at 37 °C for 24 h and then read on a spectrophotometer ELISA (Thermoplate®) at 630 nm.
Determination of minimum fungicidal concentration (MFC)
To verify the MFC, the tip of a sterile rod was inserted into each well of the previously tested plate. After inserting into the middle of each well, the rod was taken to a Petri dish containing SD with the aid of a guide plate attached to the bottom of the plate for yeast subculture and cell viability evaluation. After 24 h of incubation, the plates were analyzed for colony formation (Ernst et al. 1999). The concentration in which there was no growth of fungal colony was considered the MFC.
Evaluation of the modifying effect on Fluconazole action
First, the intrinsic action of CE, fractions and Fluconazole on yeast growth were verified. Then, it was evaluated if the antifungal action of Fluconazole was modulated by the CE and fractions. Therefore, CE and fractions were used at sub-inhibitory concentrations (MFC/16) according to Coutinho et al. (2008) with minor modifications from Morais-Braga et al. (2016). If the CE or fractions potentiates the action of the Fluconazole, the verified effect was considered synergic type. If it interfered with the action of the Fluconazole, the verified effect was considered antagonistic type. The plates were filled with 100 μL of medium + inoculum + sample followed by microdilution with 100 μL of Fluconazole at concentration of 8192 μg/mL. The mixture was added to the first well of the plate to be subjected to serial dilutions (1:1), ranging from 8192 to 8 μg/mL. The last well was used as control. The plates were incubated at 37 °C for 24 h. The reading was performed on an ELISA spectrophotometer (Thermoplate®).
Statistical analysis
GraphPad Prism software v.5.0 was used for statistical analysis. The data obtained were verified for their normal distribution using a two-way ANOVA (P < 0.05; *P < 0.1; ****P < 0.0001) and Bonferroni post hoc test. The IC50 values were obtained by nonlinear regression analysis with interpolation of the unknown standard curve obtained from fungal growth assays as a function of extract concentration and expressed in μg/mL.
Results
Characterization of CE and fractions from A. cearensis seeds
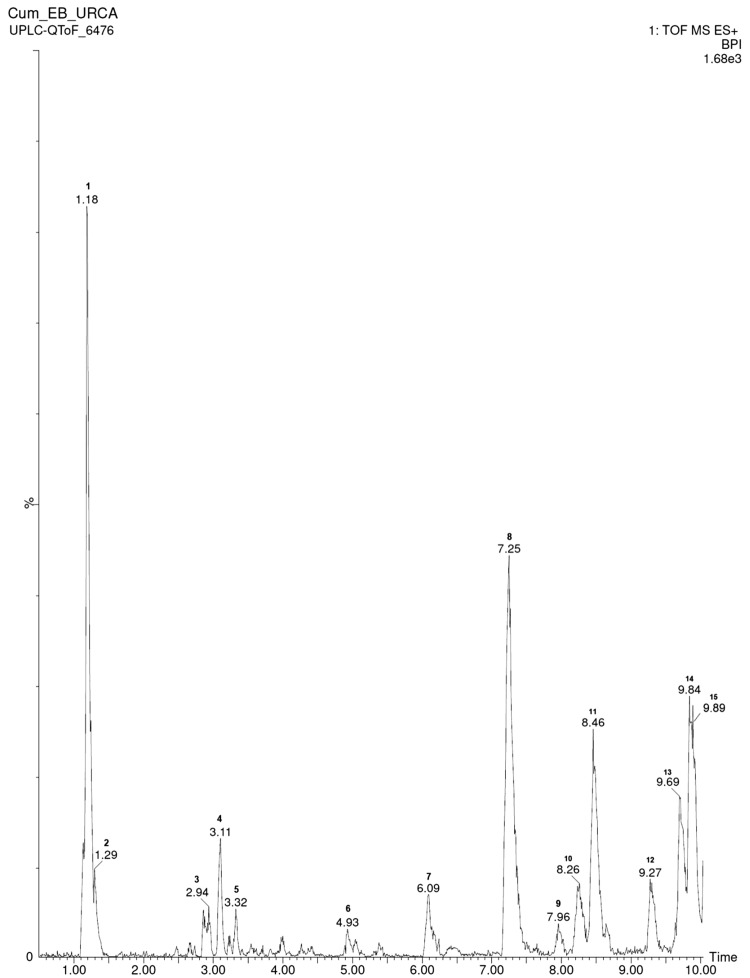
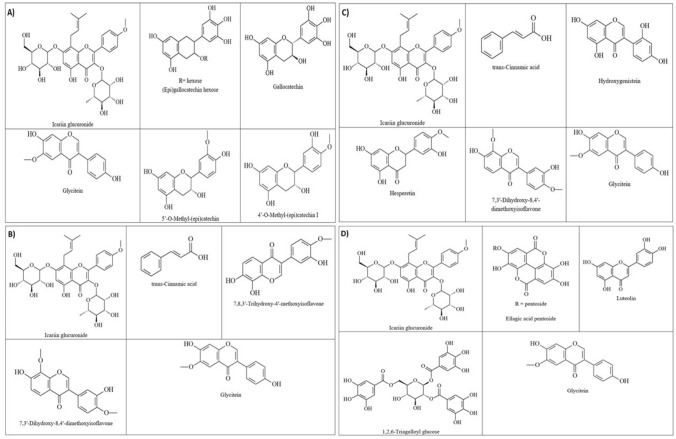
Figures 1, 2, 3 and 4 show the composition of the CE and fractions of A. cearensis seeds determined by LC–MS/MS–QTOF. The parameters analyzed were molecular weight, ionic mass, retention time, fragmentation pattern and compared with the available literature. In this study, we identified seven compounds in the CE (Table 1), six compounds in FR-1 (Table 2), eight compounds in FR-2 (Table 3) and five compounds in FR-3 (Table 4), varying from flavonoids, phenolic acids, flavan derivatives, organic acids and phenolic compounds. The chemical structures of the compounds are shown in Fig. 5.
Fig. 1.
Ultra-performance liquid chromatography with high-definition mass spectrometry (UPLC–MS) chromatography of CE from A. cearensis seeds
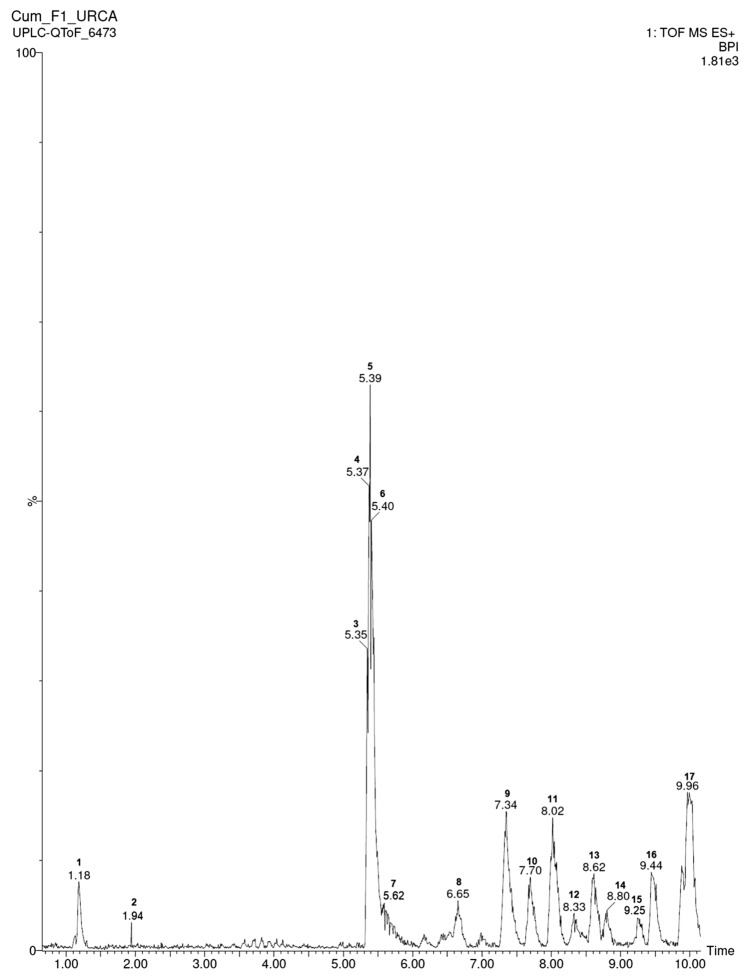
Fig. 2.
Ultra-performance liquid chromatography with high-definition mass spectrometry (UPLC–MS) chromatography of FR-1 from A. cearensis seeds
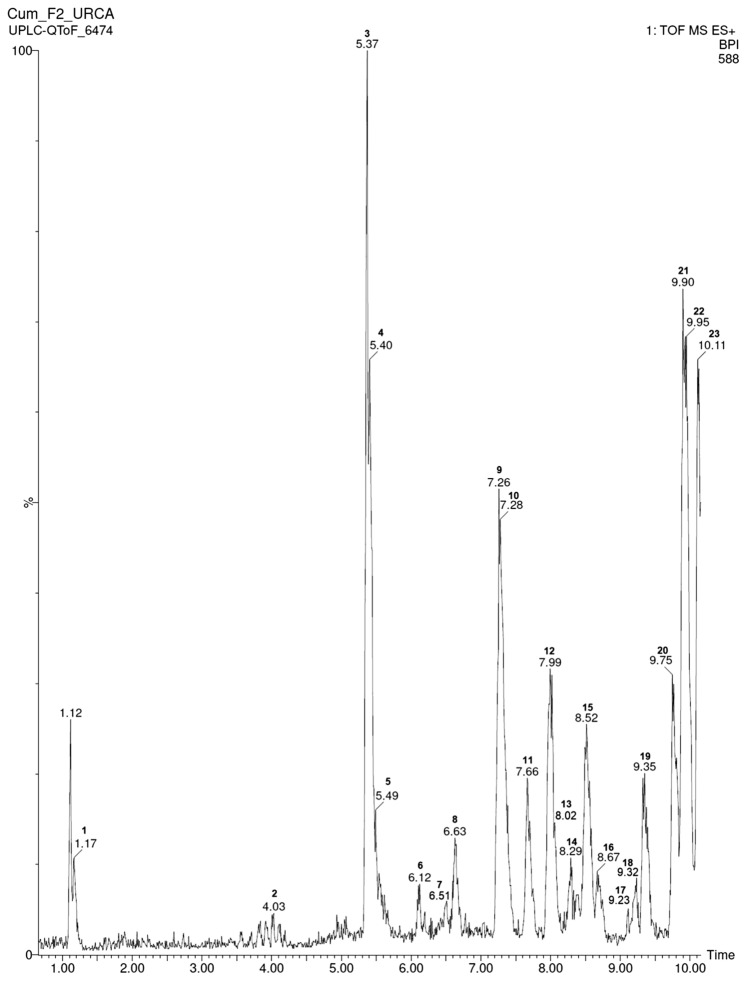
Fig. 3.
Ultra-performance liquid chromatography with high-definition mass spectrometry (UPLC–MS) chromatography of FR-2 from A. cearensis seeds
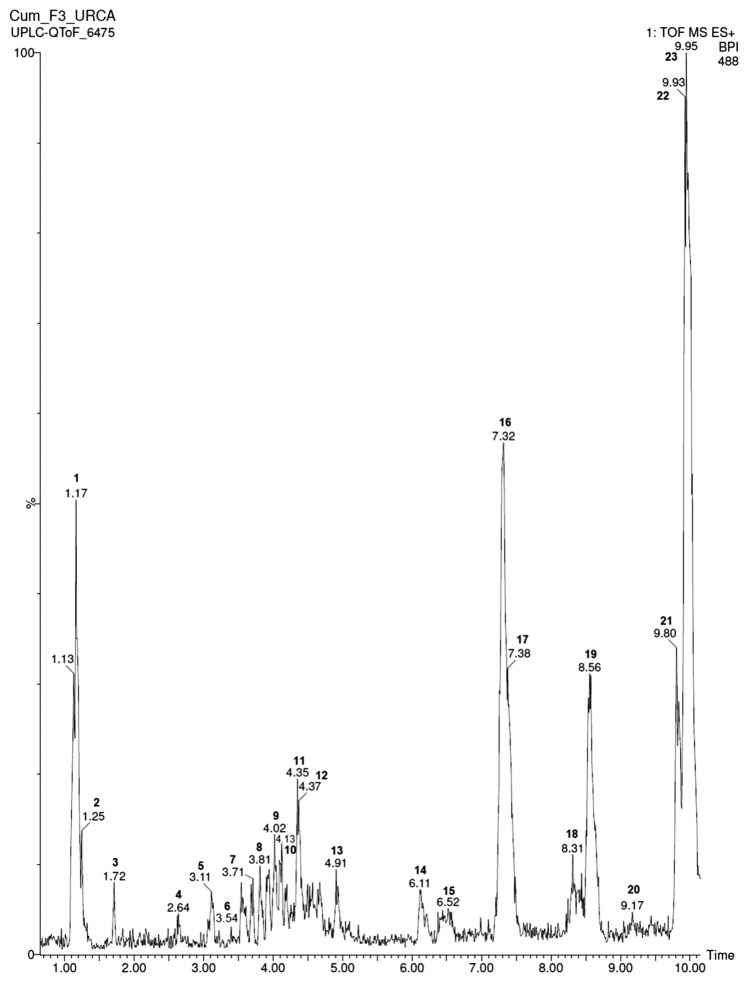
Fig. 4.
Ultra-performance liquid chromatography with high-definition mass spectrometry (UPLC–MS) chromatography of FR-3 from A. cearensis seeds
Table 1.
Compounds identified by UPLC-ESI-TOFMS/MS in positive mode in the CE of A. cearensis seeds
| Peak no. | Retention time (min) | [M-H]− observed | [M-H]− calculated | Product ions (MS/MS) | Empirical formula | Parts per million (error) | Putative name | References |
|---|---|---|---|---|---|---|---|---|
| 1 | 1.18 | 689.2051 | 689.2082 | 689.2087, 367.1008, 352.8637 | C33H37O16 | 4.5 | Icariin glucuronide | Shunjun et al. (2017) |
| 2 | 1.29 | 527.1564 | 527.1553 | 202.1848, 184.9314, 178.0209 | C27H27O11 | 2.1 | QQCA (quinicquinic-caffeic acid ester) | Plazonić et al. (2009) |
| 3 | 2.94 | 467.1732 | 467.1706 | 329.0866, 261.0790, 179.0338, 137.0256 | C21H23O12 | 2.2 | (Epi)gallocatechin hexose II | Ibrahim et al. 2014 |
| 4 | 3.11 | 305.0735 | 305.0720 | 179.0339, 167.0341, 137.0252, 125.0241 | C15H13O7 | 4.9 | Gallocatechin | Ibrahim et al. (2014) |
| 5 | 3.32 | 172.0376 | 172.0372 | 242.9876, 144.0423, 116.0501 | C6H2N7 | 2.3 | No identified | – |
| 6 | 4.93 | 218.2143 | 218.2120 | 177.0513, 145. 0170, 225.9959 | C12H28NO2 | 10.5 | No identified | – |
| 7 | 6.09 | 246.2422 | 246.2433 | 258.8799, 184.0619, 156.0619 | C14H32NO2 | 4.5 | No identified | – |
| 8 | 7.25 | 247.2733 | 247.2746 | 275.2783, 256.2661, 230.2536 | C16H36NO2 | 4.7 | No identified | – |
| 9 | 7.96 | 283.1002 | 283.1029 | 295.0207, 240.0207, 133.0802 | C16H12O5 | 9.5 | Dihydroxymethoxyisoflavone | Oliveira et al. (2017) |
| 10 | 8.26 | 119.0829 | 119.0821 | 437.2041, 185.1608, 120.0852 | C4H11N2O2 | 6.7 | No identified | – |
| 11 | 8.46 | 303.0885 | 303.0874 | 137.0244 | C16H15O6 | 3.6 | 4′- or 5′-O-Methyl-(epi)catechin I | Ibrahim et al. (2014) |
| 12 | 9.27 | 393.3636 | 393.3639 | 334.3075, 249.1913,133.0866 | C13H41N14 | 0.8 | No identified | – |
| 13 | 9.69 | 332.3412 | 332.28 | 330.3311, 270.9351, 150.7104 | 1.0 | Gallic-caffeic acid ester | Plazonić et al. (2009) | |
| 14 | 9.84 | 457.2762 | 457.2743 | 155.0720, 458.2881 | C31H37O3 | 4.2 | No identified | – |
| 15 | 9.89 | 457.2829 | 457.2801 | 155.0675, 458.2868 | C24H41O8 | 6.1 | No identified | – |
Table 2.
Compounds identified by UPLC–ESI–TOFMS/MS in positive mode in the FR-1 of A. cearensis seeds
| Peak no. | Retention time (min) | [M-H]− observed | [M-H]− calculated | Product ions (MS/MS) | Empirical formula | Parts per million (error) | Putative name | References |
|---|---|---|---|---|---|---|---|---|
| 1 | 1.18 | 689.2130 | 689.2117 | 689.2087, 367.1008, 352.8637 | C33H37O16 | 4.5 | Icariin glucuronide | Shunjun et al. (2017) |
| 2 | 1.94 | 453.7779 | 453.7796 | 454.7751, 451.7924, 449.7784 | C6NO11S6 | 3.7 | No identified | – |
| 3 | 5.35 | 147.0405 | 147.0446 | 147.0417, 62.1057 | C9H8O2 | − 27.0 | Trans-cinnamic acid | Ibrahim et al. (2014) |
| 4 | 5.37 | 147.0408 | 147.0446 | 147.0417, 62.1057 | C9H8O2 | − 25.0 | Possible isomer trans-cinnamic acid | Ibrahim et al. (2014) |
| 5 | 5.39 | 147.0407 | 147.0446 | 147.0417, 62.1057 | C9H8O2 | Possible isomer trans-cinnamic acid | Ibrahim et al. (2014) | |
| 6 | 5.40 | 147.0417 | 147.0446 | 147.0417, 62.1057 | C9H8O2 | − 19.0 | Possible isomer trans-cinnamic acid | Ibrahim et al. (2014) |
| 7 | 5.62 | 147.0417 | 147.0446 | 147.0417, 62.1057 | C9H8O2 | − 19.0 | Possible isomer trans-cinnamic acid | Ibrahim et al. (2014) |
| 8 | 6.65 | 299.0892 | 299.0919 | 284.0323,256.0673,184.0652 | C17H15O5 | 9.0 | 7,8,3′-Trihydroxy-4′-methoxyisoflavone | Oliveira et al. (2017) |
| 9 | 7.34 | 274.2764 | 274.2746 | 318.3075, 274.2844, 256.2657 | C16H36NO2 | 6.6 | No identified | – |
| 10 | 7.70 | 313.1020 | 313.1017 | 269.0793, 252.0761, 184.0693 | C18H17O5 | 1.0 | 7,3′-Dihydroxy-8,4′-dimethoxyisoflavone | Oliveira et al. (2017) |
| 11 | 8.02 | 283.0938 | 283.0970 | 240.0811, 211.0820, 197.0556 | C17H15O4 | 11.3 | Dihydroxymethoxyisoflavone | Oliveira et al. (2017) |
| 12 | 8.33 | 119.0855 | 119.0861 | 113.0861, 117.1045 | C9H11 | − 5.0 | No identified | – |
| 13 | 8.62 | 302.3014 | 302.3059 | 184.0782, 177.1111, 113.0846 | C18H40NO2 | − 6.0 | No identified | – |
| 14 | 8.80 | 391.3424 | 391.3424 | 331.2966, 177.1157, 133.0889 | C22H47O5 | 0.0 | No identified | – |
| 15 | 9.25 | 323.2748 | 323.2797 | 373.1831, 339.2472,133.0887 | C17H39O5 | − 15.2 | No identified | – |
| 16 | 9.44 | 393.3588 | 393.3588 | 393.3560, 334.3107, 177.1114 | C22H49O5 | 2.0 | No identified | – |
| 17 | 9.96 | 330.3365 | 330.3372 | 258.0484, 312.3296, 331.3336 | C20H44NO2 | − 2.1 | No identified | – |
Table 3.
Compounds identified by UPLC–ESI–TOFMS/MS in positive mode in the FR-2 of A. cearensis seeds
| Peak no | Retention time (min) | [M-H]− observed | [M-H]− calculated | Product ions (MS/MS) | Empirical formula | Parts per million (error) | Putative name | References |
|---|---|---|---|---|---|---|---|---|
| 1 | 1.17 | 689.2051 | 689.2082 | 689.2087, 367.1008, 352.8637 | C33H37O16 | 4.5 | Icariin glucuronide | Shunjun et al. (2017) |
| 2 | 4.03 | 591.3693 | 591.3686 | 401.1527, 172.8673, 133.0836 | C37H51O6 | 1.2 | No identified | – |
| 3 | 5.37 | 147.0419 | 147.0446 | 147.0422, 62.2985 | C9H7O2 | − 18.4 | Trans-cinnamic acid | Ibrahim et al. (2014) |
| 4 | 5.40 | 147.0412 | 147.0446 | 147.0422, 62.2985 | C9H7O2 | − 23.1 | Possible isomer trans-cinnamic acid | Ibrahim et al. (2014) |
| 5 | 5.49 | 147.0408 | 147.0446 | 147.0422, 62.2985 | C9H7O2 | − 23.1 | Possible isomer trans-cinnamic acid | Ibrahim et al. (2014) |
| 6 | 6.12 | 246.2432 | 246.2433 | 247.4212, 184.0706, 156.0435 | C14H32NO2 | − 0.4 | No identified | Ibrahim et al. (2014) |
| 7 | 6.51 | 285.2693 | 285.2700 | 269.7, 163.8, 150.5 | C15H10O6 | − 2.5 | Hydroxygenistein | Schmeda-Hirschmann et al. (2019) |
| 8 | 6.63 | 299.0910 | 299.0919 | 283.7, 230.7 | C17H15O5 | − 3.0 | Methoxy trihydroxy flavanone | Schmeda-Hirschmann et al. (2019) |
| 9 | 7.26 | 274.2721 | 274.2719 | 275.2858, 256.2728, 184.0647 | C12H32N7 | 0.7 | No identified | – |
| 10 | 7.28 | 274.2730 | 274.2719 | 275.2858, 256.2728, 184.0647 | C12H32N7 | 4.0 | No identified | – |
| 11 | 7.66 | 313.1066 | 313.1076 | 269.0793, 252.0761, 184.0693 | C18H17O5 | − 3.2 | 7,3′-Dihydroxy-8,4′-dimethoxyisoflavone | Oliveira et al. (2017) |
| 12 | 7.99 | 283.0953 | 283.0970 | 240.0811, 211.0820, 197.0556 | C17H15O4 | − 6.0 | Dihydroxymethoxyisoflavone | Oliveira et al. (2017) |
| 13 | 8.02 | 283.0921 | 283.0970 | 240.0811, 211.0820, 197.0556 | C17H15O4 | − 17.3 | Dihydroxymethoxyisoflavone possible isomer | Oliveira et al. (2017) |
| 14 | 8.29 | 119.0850 | 119.0861 | 113.0861, 117.1045 | C9H11 | − 9.2 | No identified | – |
| 15 | 8.52 | 302.3076 | 302.3059 | 184.0782, 177.1111, 113.0846 | C18H40NO2 | 5.6 | No identified | – |
| 16 | 8.67 | 391.3500 | 391.3509 | 184.0709, 177.1171 | C17H43N8O2 | − 2.3 | No identified | – |
| 17 | 9.23 | 323.2783 | 323.2797 | 373.1831, 339.2472,133.0887 | C17H39O5 | − 4.3 | No identified | – |
| 18 | 9.32 | 393.3557 | 393.3580 | 393.3560, 334.3107, 177.1114 | C22H49O5 | − 5.8 | No identified | – |
| 19 | 9.35 | 393.3589 | 393.3580 | 393.3560, 334.3107, 177.1114 | C22H49O5 | 2.3 | No identified | – |
| 20 | 9.75 | 330.3365 | 330.3372 | 258.0484, 312.3296, 331.3336 | C20H44NO2 | − 2.1 | No identified | – |
| 21 | 9.90 | 457.2744 | 457.2743 | 155.0720, 458.2881 | C31H37O3 | 0.2 | No identified | – |
| 22 | 9.95 | 457.2778 | 457.2743 | 155.0720, 458.2881 | C31H37O3 | 7.7 | No identified | – |
| 23 | 10.11 | 395.3740 | 395.3750 | 335.3429, 184.0704, 133.0864 | C23H47N4O | − 2.5 | No identified | – |
Table 4.
Compounds identified by UPLC–ESI–TOFMS/MS in positive mode in the FR-3 of A. cearensis seeds
| Peak no | Retention time (min) | [M-H]− observed | [M-H]− calculated | Product ions (MS/MS) | Empirical formula | Parts per million (error) | Putative name | References |
|---|---|---|---|---|---|---|---|---|
| 1 | 1.17 | 689.2147 | 689.2140 | 689.2087, 367.1008, 352.8637 | C33H37O16 | 1.0 | Icariin glucuronide | Shunjun et al. (2017) |
| 2 | 1.25 | 136.0607 | 136.0610 | 152.0563, 136.0607 | C4H10NO4 | − 2.2 | No identified | – |
| 3 | 1.72 | 136.0612 | 136.0610 | 152.0563, 136.0607 | C4H10NO4 | 1.5 | No identified | – |
| 4 | 2.64 | 172.0363 | 172.0372 | 242.9876, 144.0423, 116.0501 | C6H2N7 | − 5.2 | No identified | – |
| 5 | 3.11 | 433.1133 | 433.1135 | 300.9686 | C21H21O10 | − 0.5 | Ellagic acid pentoside 1 | Schmeda-Hirschmann et al. (2019) |
| 6 | 3.54 | 287.0533 | 287.0556 | 287.0538, 241.0332, 175.0282 | C15H11O6 | 8.0 | Luteolin | Ibrahim et al. (2014) |
| 7 | 3.71 | 133.0901 | 133.0865 | 207.0626, 151.0330, 133.0813 | C6H13O3 | 2.7 | No identified | – |
| 8 | 3.81 | 133.0860 | 133.0865 | 207.0626, 151.0330, 133.0813 | C6H13O3 | − 3.5 | No identified | – |
| 9 | 4.02 | 591.3591 | 591.3592 | 207,0608, 151.0291 133.0836 | C26H55O14 | − 0.2 | No identified | – |
| 10 | 4.13 | 635.3927 | 635.3927 | 465.0265 | C39H55O7 | − 3.3 | Trigalloyl hexoside | Schmeda-Hirschmann et al. (2019) |
| 11 | 4.35 | 207.0683 | 207.0657 | 369.1195, 207.0621, 175.0858 | C11H11O4 | 12.6 | No identified | – |
| 12 | 4.37 | 207.0658 | 207.0657 | 369.1195, 207.0621, 175.0858 | C11H11O4 | 0.5 | No identified | – |
| 13 | 4.91 | 207.0661 | 207.0657 | 240.0811, 211.0820, 197.0556 | C11H11O4 | 1.9 | No identified | – |
| 14 | 6.11 | 246.2453 | 246.2433 | 258.8799, 184.0619, 156.0619 | C14H32NO2 | 8.1 | No identified | – |
| 15 | 6.52 | 283.0364 | 283.1029 | 295.0207, 240.0207, 133.0802 | C16H12O5 | 9.5 | Dihydroxymethoxyisoflavone | Oliveira et al. (2017) |
| 16 | 7.32 | 274.2742 | 274.2746 | 318.3075, 274.2844, 256.2657 | C16H36NO2 | − 1.5 | No identified | – |
| 17 | 7.38 | 318.2995 | 318.2981 | 274.2706. 256.2648 | C14H36N7O | 4.4 | No identified | – |
| 18 | 8.31 | 119.0870 | 119.0821 | 437.2041, 185.1608, 120.0852 | C4H11N2O2 | 6.7 | No identified | – |
| 19 | 8.56 | 302.3055 | 302.3059 | 184.0782, 177.1111, 113.0846 | C18H40NO2 | − 1.3 | No identified | – |
| 20 | 9.17 | 304.3001 | 304.3004 | 212.2469, 133.0871 | C21H38N | − 1.0 | No identified | – |
| 21 | 9.80 | 330.3346 | 330.3372 | 258.0484, 312.3296, 331.3336 | C20H44NO2 | − 2.1 | No identified | – |
| 22 | 9.93 | 457.2736 | 457.2743 | 155.0720, 458.2881 | C31H37O3 | − 1.5 | No identified | – |
| 23 | 9.95 | 457.2711 | 457.2743 | 155.0720, 458.2881 | C31H37O3 | − 7.0 | No identified |
Fig. 5.
Main compounds identified in CE, FR-1, FR-2 and FR-3 of A. cearensis seeds. a aqueous crude extract; b fraction 1; c fraction 2; and d fraction 3
In addition, it was possible to identify the presence of some organic acids such as cinnamic acid and some possible trans-isomers in FR-1 and FR-2 (Tables 2 and 3, respectively). We evidenced the presence of some polyphenols as 4′- or 5′-O-methyl-(epi)catechin I in CE, and a polyphenol monomer trigalloyl hexoside in FR-3. The presence of the flavonoid icariin glucuronide was observed in all samples, as well as dihydroxymethoxyisoflavone, 7,8,3′-trihydroxy-4′-methoxyisoflavone and trihydroxyflavanone.
Antifungal activity of CE and fractions of A. cearensis seeds
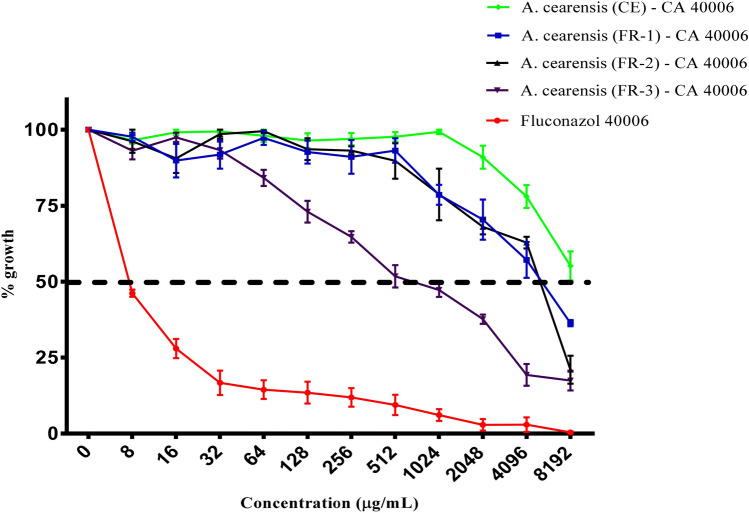
All samples used alone induced inhibition growth of C. albicans strains (Figs. 6, 7, 8, 9), and FR-3 of A. cearensis seeds showed the lowest IC50 (123.5 µg/mL) against INCQS 40.006 (Table 5). However, Fluconazole + FR-2 showed the lowest IC50 (2.10 and 1.81 µg/mL), indicating that the combination of antifungal drug and FR-2 has synergistic effect against C. albicans (Table 5). Similar effects have been evidenced for the CE and FR-1 combined with Fluconazole against URM 4127 strain. On the other hand, we evidenced antagonistic effect when CE, FR-1 and FR-3 were combined with Fluconazole (Table 5).
Fig. 6.
Antifungal effects (μg/mL) of aqueous crude extract and fractions of A. cearensis seeds against C. albicans 40006. Fluconazole was used as a control against C. albicans
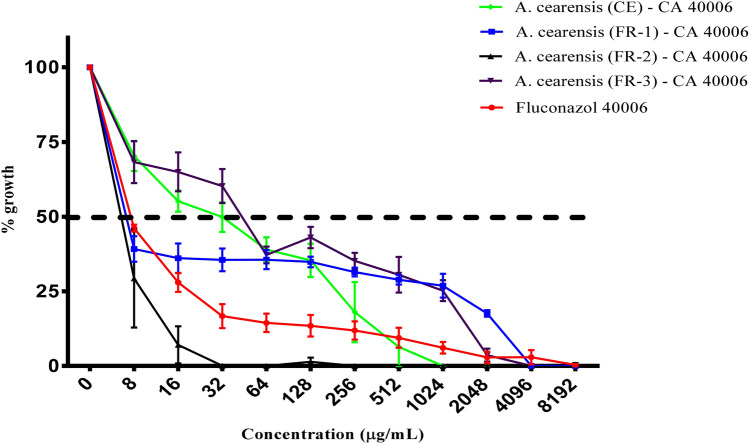
Fig. 7.
Antifungal effects (μg/mL) of aqueous crude extract and fractions of A. cearensis seeds combined with fluconazole against C. albicans 40006. Fluconazole was also used as a control against C. albicans
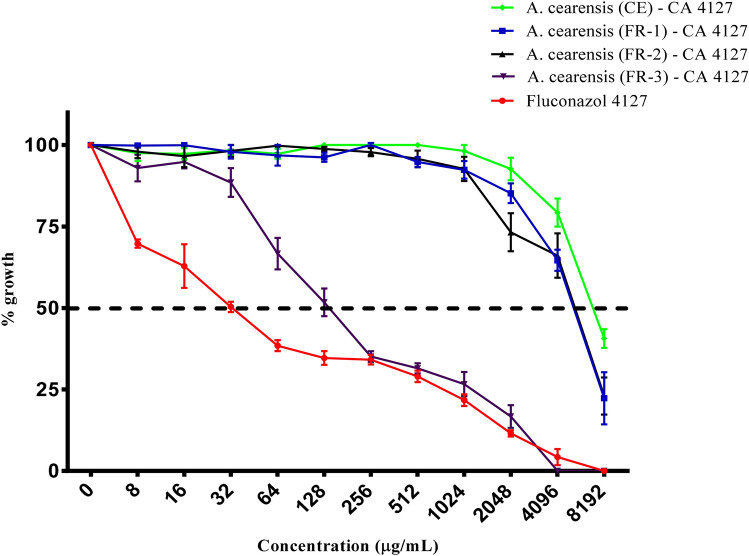
Fig. 8.
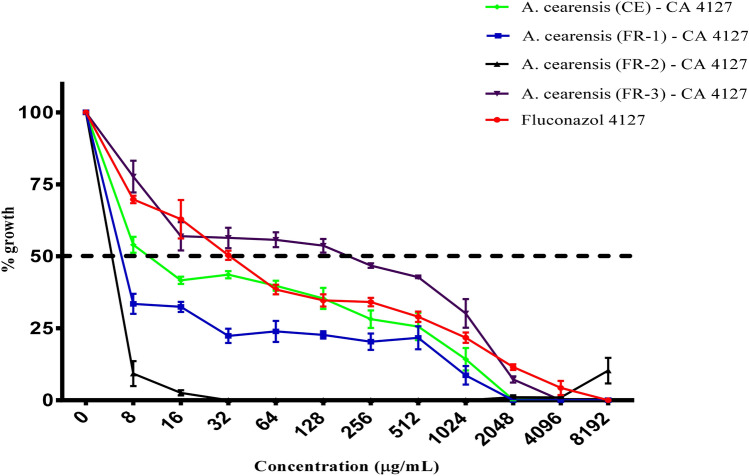
Antifungal effects (μg/mL) of aqueous crude extract and fractions of A. cearensis seeds against C. albicans 4127. Fluconazole was used as a control against C. albicans
Fig. 9.
Antifungal effects (μg/mL) of aqueous crude extract and fractions of A. cearensis seeds combined with fluconazole against C. albicans 4127. Fluconazole was also used as a control against C. albicans
Table 5.
IC50 (µg/mL) of CE and fractions from A. cearensis seeds against C. albicans strains
| Evaluated combination | CA INCQS 40006 | CA URM 4127 |
|---|---|---|
| FCZ | 2.4 ± 1.2 | 7.68 ± 4.8 |
| CE—A. cearensis | > 2048 ± 3.6 | > 2048 ± 3.2 |
| FR-1—A. cearensis | 1968.6 ± 9.5 | 1138.4 ± 4.8 |
| FR-2—A. cearensis | 1173.3 ± 8.1 | 1273.3 ± 6.3 |
| FR-3—A. cearensis | 123.5 ± 5.5 | 45.6 ± 6.1 |
| CE—A. cearensis + FCZ | 9.54 ± 4.0 | 3.14 ± 2.0 |
| FR-1—A. cearensis + FCZ | 3.51 ± 2.5 | 2.41 ± 1.8 |
| FR-2—A. cearensis + FCZ | 2.1 ± 0.99 | 1.81 ± 0.8 |
| FR-3—A. cearensis + FCZ | 11.9 ± 8.7 | 18.8 ± 7.4 |
CA Candida albicans, FCZ fluconazole, CE aqueous crude extract, FR-1 fraction 1, FR-2 fraction 2, FR-3 fraction 3, MIC minimum inhibitory concentration, INCQS National Institute of Health Control, URM University Recife Mycology—P ≤ 0.05 in relation to FCZ control
Fungicidal activity
The MFC for all samples tested alone was ≥ 16.384 µg/mL for INCQS 40.006. However, fluconazole + FR-2 showed the lowest MFC (128 µg/mL) against URM 4127 strain (Table 6), which indicated a synergic effect of antifungal drug and FR-2. Conversely, CE and FR-1 combined with antifungal drug showed antagonistic effect against URM 4127 strain (Table 6).
Table 6.
Minimal fungicidal concentrations (MFC) in µg/mL to fluconazole (FCZ) alone and combined with CE and fractions from A. cearensis seeds
| CA URM 4127 | |
|---|---|
| Fluconazole | 2048 |
| A. cearensis CE + FCZ | 2048 |
| A. cearensis FR-1 + FCZ | 8192 |
| A. cearensis FR-2 + FCZ | 128 |
| A. cearensis FR-3 + FCZ | 8192 |
Discussion
Amburana cearensis characterization
Polyphenols are secondary metabolites ubiquitously distributed among plants. They are divided in phenolic compounds, phenolic acids (cinnamic acid derivatives) and glycosidic phenylpropanoid esters (Ferreira et al. 2010). Phenolic compounds were previously reported as having antimicrobial and anti-inflammatory activities (Klančnik et al. 2010).
In addition, they exhibit antioxidant properties (Moure et al. 2001; Giada 2013; Flores et al. 2013), due to hydroxyls attached to aromatic rings. These molecules include flavonoids, phenolic acids, tannins, and tocopherols (Soares 2002; Angelo and Jorge 2007) that act as effective scavengers of reactive oxygen species, and chelating Fe3+ that catalyze lipid peroxidation (Andrade et al. 2007).
On the other hand, flavonoids represent a group of plant pigments abundantly distributed in nature. Its presence in plants may have a relationship with defensive ability, such as protection against UV radiation, antifungal and antibacterial actions, as well as attracting pollinators (Lavola 1998). These compounds have two aromatic rings connected by a bridge of three carbon atoms (C6C3C6) (Simões et al. 2007).
Icariin glucuronide is categorized as a flavonol, one of the subclasses of flavonoid, which have ability to induce bone tissue repair (Wei et al. 2011), human stem cell proliferation (Fan et al. 2011), immunoregulation (Kim et al. 2001), increases of cGMP in smooth cavernous muscle cells (Ning et al. 2006), increases of nitric oxide (Bin and Huang 2007), and mimics testosterone’s effects (Zhang and Yang 2006).
Cinnamic acid is a naturally occurring aromatic carboxylic acid whose molecular structure is usually presented in trans-form. It is part of the auxin group, plant hormones that regulate cell growth and differentiation, and some of its derivatives play an important role in plant defense against pest attack (Niero 2010). It should be noted that its derivatives exhibit antioxidant (Hussain et al. 2014), antibacterial (Chiriac et al. 2005), anticancer (Ekmekcioglu et al. 1998), antifungal (Sadeghi et al. 2013), antitumor (Lee et al. 2003) and phytotoxic effects (Nishikawa et al. 2013).
Coumarins are derived from phenylalanine metabolism, being one of the early precursors of p-hydroxycinnamic acid (p-coumaric acid), which is hydroxylated at the C-2′ (ortho-hydroxylation). The ortho-hydroxylated derivative undergoes a photocatalyzed double-bond (EZ) isomerization. The Z isomer spontaneously lactonizes, producing umbelliferone. Prenylation of the benzene ring at positions 6 or 8 of the 7-hydroxy coumarin derivative is the first step in furan- and pyranocoumarin biogenesis. Cyclization of 6- or 8-isoprenylcoumarin derivatives occurs by nucleophilic attack of the C-7 hydroxyl group to the epoxide formed by oxidation of the double bond of the isopentenyl residue. Based on the orientation of the nucleophilic attack, the product will be hydroxyisopropyl dihydrofuranocoumarin or hydroxy dimethyl dihydropyranocoumarin (Bourgaud et al. 2006).
Most coumarins are biogenetically derived from the shikimic acid pathway, but a significant number of them appear to derive from a mixed pathway (shikimic acid and acetate) such as phenylcoumarin. 4-n-Propylcoumarin, e.g., are entirely derived from the acetate pathway (Strack 1997). Coumarin synthesis can be induced by a response to biotic and abiotic stress, nutritional deficiency, chemical messengers such as plant hormones and other external metabolites (Cabello-Hurtado et al. 1998; Dewick 2009; Bosqueiro 1996; Haida et al. 2007). Coumarins have a variety of pharmacological properties, especially anti-inflammatory, antioxidant, antibacterial, antiviral, antithrombotic, antimutagenic and antihypertensive activities (Hoult and Payá 1996).
Characterization studies performed on stem bark extracts of A. cearensis, evidenced coumarin (Carvalho 1994), responsible for its characteristic odor, isokaempferide (Maia 2004), kaempferol and afrormosin, amburoside A (Leal et al. 1997) and B (Leal et al. 2003), vanillic acid (Bravo et al. 1999) and protocatechuic acid (Canuto et al. 2004), and large amount of sucrose. In addition, other studies show that coumarin (Carvalho 1994), isokaempferide (Maia 2004) and amburoside A (Leal et al. 1997) have anti-inflammatory, antioxidant, and bronchodilator effects (Leal et al. 2008). Of which some coincide with precursors of those found in our study. However, it should be noted that some identified compounds in this study are not yet reported for its biological activity.
Antifungal, fungicidal, and modulating antifungal activity
It is noteworthy that the indiscriminate and increasing use of azole antifungal drugs, both to prevent and treat active infections, has increased the prevalence of Fluconazole-resistant strains of Candida (Day et al. 2013). In United States, an annual increase of > 3400 cases of antifungal resistance were identified, as reported by the Center for Disease Control and Prevention, thus making fluconazole-resistant Candida a serious threat (Gajdács 2019).
Fluconazole acts by preventing the biosynthesis pathway of the main constituent of the fungal cell membrane, ergosterol. It inhibits the enzyme lanosterol 14-α demethylase in the fungal cytochrome P-450 enzyme system, which is encoded by the ERG11 gene. Thus, lanosterol cannot be converted to ergosterol and consequently the accumulation of precursors occurs causing fungal membrane instability (Carrillo-Muñoz et al. 2006; Menozzi et al. 2017).
Alternatives for treating Candida infections are considered limited and many existing antifungal drugs have undesirable side effects such as high toxicity, especially in immunosuppressed individuals (Fica 2004). For these patients, antifungal therapies are a challenging situation, which represent an urgent need to research and develop novel antifungal drugs more effective and less toxic (Calabrese et al. 2013).
Bravo et al. (1999) already shown that the main component of A. cearensis was coumarin, mainly responsible for bronchodilator activity. It also highlights the presence of phenolic glycosides that presented antimalarial, antiprotozoal, antifungal, and antibacterial activity in vitro. In addition, Salas et al. (2011) using natural and enzymatically modified flavonoids from plants against Penicillium, Aspergillus and Fusarium species evidenced antifungal activity. However, Steiner et al. (2008) showed that antifungal activity induced by isoflavone, especially genistein, demonstrated a better effect, but without a clear mechanism of action.
The combined use of drugs that can achieve synergistic results, showing increased of therapeutic effect, decreased minimal inhibitory concentration, regression of antibiotic resistance development, and a decrease in host toxicity has become increasingly studied as an alternative for the treatment of infections (Silva et al. 2015).
Some phenolic compounds such as gallic acid, catechin, luteolin and quercetin demonstrated in vitro antifungal activity against different Candida species, including C. albicans and C. tropicalis (Alves et al. 2014), corroborating with this study. In addition, Silva et al. (2014) evaluated the flavonoid combined with Fluconazole in in vitro microdilution against Fluconazole-resistant C. tropicalis, and observed a considerable synergistic effect, reducing the MICs of the flavonoids from 64 to 0.25 μg/mL, similar to our results against C. albicans.
Conclusion
CE, FR-1, FR-2 and FR-3 of A. cearensis seeds presented phenolic compounds, organic acids, and polyphenols, that contributed to its antifungal capacity and synergistic effects. Our results show that A. cearensis seeds can be considered as promising source of antifungal agents and modulators of antifungal activity. However, further studies are needed to identify the active compounds and to prove their efficacy, safety, and mechanism of action.
Acknowledgements
The autthors are grateful to the Brazilian research agencies FUNCAP, CAPES, CNPq and FINEP for the support of this work.
Author contributions
Methodology—antimicrobial assays (MTAO; MVOBA and GMMM); methodology—chemical analysis (PRVR; ESB and EOS); methodology—statistical analysis (IRAM; JCA and EAS); supervision o f work—(HDMC and AFU); resources (VPAL and JIOC).
Compliance with ethical standards
Ethical statements
This article is according to the international, national and institutional rules considering biodiversity rights.
References
- Agra MF, Baracho GS, Nurit K, Basílio IJLD, Coelho VPM. Medicinal and poisonous diversity of the flora of “Cariri Paraibano”, Brazil. J Ethnopharmacol. 2007;111:383–395. doi: 10.1016/j.jep.2006.12.007. [DOI] [PubMed] [Google Scholar]
- Alves CT, Ferreira ICFR, Barros L, Silva S, Azeredo J, Henriques M. Antifungal activity of phenolic compounds identified in flowers from North Eastern Portugal against Candida species. Future Microbiol. 2014;9:139–146. doi: 10.2217/fmb.13.147. [DOI] [PubMed] [Google Scholar]
- Andrade CA, Costa CK, Bora K, Miguel MD, Miguel OG, Kerber VA. Determination of the phenolic content and evaluation of the antioxidant activity of Acacia podalyriifolia A. Cunn. ex G. Don, Leguminosae-mimosoideae. Revista Brasileira de Farmacognosia. 2007;17:231–235. doi: 10.1590/s0102-695x2007000200017. [DOI] [Google Scholar]
- Angelo PM, Jorge N. Phenolic compounds in foods—a brief review. Rev Inst Adolfo Lutz. 2007;66:1–9. [Google Scholar]
- Bin XuH, Huang ZQ. Icariin enhances endothelial nitric-oxide synthase expression on human endothelial cells in vitro. Vascul Pharmacol. 2007;47:18–24. doi: 10.1016/j.vph.2007.03.002. [DOI] [PubMed] [Google Scholar]
- Bosqueiro ALD. Plantas como fonte de fitofármaco. Ciência Educação. 1996;02:91–96. [Google Scholar]
- Bourgaud F, Hehn A, Larbat R, Doerper S, Gontier E, Kellner S, Matern U. Biosynthesis of coumarins in plants: a major pathway still to be unravelled for cytochrome P450 enzymes. Phytochem Rev. 2006;5:293–308. doi: 10.1007/s11101-006-9040-2. [DOI] [Google Scholar]
- Bravo JAB, Sauvain M, Gimenez AT, Muñoz VO, Callapa J, Le Men-Olivier L, Massiot G, Lavaud C. Bioactive phenolic glycosides from Amburana cearensis. Phytochemistry. 1999;50:71–74. doi: 10.1016/S0031-9422(98)00497-X. [DOI] [Google Scholar]
- Cabello-Hurtado F, Durst F, Jorrín JV, Werck-Reichhart D. Coumarins in Helianthus tuberosus: characterization, induced accumulation and biosynthesis. Phytochemistry. 1998;49:1029–1036. doi: 10.1016/S0031-9422(97)01036-4. [DOI] [Google Scholar]
- Calabrese EC, Castellano S, Santoriello M, Sgherri C, Quartacci MF, Calucci L, Warrilow AGS, Lamb DC, Kelly SL, Milite C, Granata I, Sbardella G, Stefancich G, Maresca B, Porta A. Antifungal activity of azole compounds CPA18 and CPA109 against azole-susceptible and -resistant strains of Candida albicans. J Antimicrob Chemother. 2013;68:1111–1119. doi: 10.1093/jac/dks506. [DOI] [PubMed] [Google Scholar]
- Calixto Júnior JT, Morais SM, Martins CG, Vieira LG, Morais-Braga MFB, Carneiro JNP, Machado AJP, Menezes IRA, Tintino SR, Coutinho HDM. Phytochemical analysis and modulation of antibiotic activity by Luehea paniculata Mart. & Zucc. (Malvaceae) in multiresistant clinical isolates of Candida Spp. BioMed Research International. 2015;2015:1–10. doi: 10.1155/2015/807670. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Canuto KM, Leal LKAM, Viana GSB, Bezerra AME, Silveira E (2004) Aspectos químicos do estudo interdisciplinar (química, agronomia e farmacologia) de A. cearensis. In: XVIII Simpósio de Plantas Medicinais Do Brasil
- Carrillo-Muñoz AJ, Giusiano G, Ezkurra PA, Quindós G. Antifungal agents: mode of action in yeast cells. Rev Esp Quimioterap. 2006;19:130–139. [PubMed] [Google Scholar]
- Carvalho P (1994) Espécies Florestais Brasileiras : recomendações silviculturais, potencialidades e uso da madeira. EMBRAPA
- Chiriac CI, Tanasa F, Onciu M. A novel approach in cinnamic acid synthesis: direct synthesis of cinnamic acids from aromatic aldehydes and aliphatic carboxylic acids in the presence of boron tribromide. Molecules. 2005;10:481–487. doi: 10.3390/10020481. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Coutinho HDM, Costa JGM, Siqueira-Júnior JP, Lima EO. In vitro anti-staphylococcal activity of Hyptis martiusii Benth against methicillin-resistant Staphylococcus aureus-MRSA strains. Braz J Pharmacogn. 2008;18:670–675. doi: 10.1590/S0102-695X2008000500005. [DOI] [Google Scholar]
- Day JN, Chau TTH, Wolbers M, Mai PP, Dung NT, Mai NH, Phu NH, Nghia HD, Phong ND, Thai CQ, Thai LH, Chuong LV, Sinh DX, Duong VA, Hoang TN, Diep PT, Campbell JI, Sieu TPM, Baker SG, Chau NVV, Hien TT, Lalloo DG, Farrar JJ. Combination antifungal therapy for cryptococcal meningitis. N Engl J Med. 2013;368:1291–1302. doi: 10.1056/NEJMoa1110404. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Dewick PM (2009) Medicinal natural products: a biosynthetic approach, 3rd edn. Wiley
- Ekmekcioglu C, Feyertag J, Marktl W. Cinnamic acid inhibits proliferation and modulates brush border membrane enzyme activities in Caco-2 cells. Cancer Lett. 1998;128:137–144. doi: 10.1016/S0304-3835(98)00073-1. [DOI] [PubMed] [Google Scholar]
- Ernst EJ, Klepser ME, Ernst ME, Messer SA, Pfaller MA. In vitro pharmacodynamic properties of MK-0991 determined by time-kill methods. Diagn Microbiol Infect Dis. 1999;33:75–80. doi: 10.1016/S0732-8893(98)00130-8. [DOI] [PubMed] [Google Scholar]
- Fan JJ, Cao LG, Wu T, Wang DX, Jin D, Jiang S, Zhang ZY, Bi L, Pei GX. The dose-effect of icariin on the proliferation and osteogenic differentiation of human bone mesenchymal stem cells. Molecules. 2011;16:10123–10133. doi: 10.3390/molecules161210123. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ferreira JFS, Luthria DL, Sasaki T, Heyerick A. Flavonoids from Artemisia annua L. As antioxidants and their potential synergism with artemisinin against malaria and cancer. Molecules. 2010;15:3135–3170. doi: 10.3390/molecules15053135. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Fica CA. Tratamiento de infecciones fúngicas sistémicas Primera parte: fluconazol, itraconazol y voriconazol. Revista Chilena de Infectología. 2004;21:26–38. doi: 10.4067/s0716-10182004000100004. [DOI] [Google Scholar]
- Flores G, Dastmachi K, Wu SB, Whalen K. Phenolic-rich extract from the Costa Rican guava (Psidium friedrichsthalianum) pulp with antioxidant and anti-inflammatory activity. Potential for COPD therapy. Food Chem. 2013;141:889–895. doi: 10.1016/j.physbeh.2017.03.040. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gajdács M. The concept of an ideal antibiotic: implications for drug design. Molecules. 2019 doi: 10.3390/molecules24050892. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Giada MLR. Food phenolic compounds: main classes, sources and their antioxidant power. Croatia: InTech; 2013. [Google Scholar]
- Goulart LS, de Souza WWR, Vieira CA, de Lima JS, de Olinda RA, de Araújo C. Oral colonization by Candida species in HIV-positive patients: association and antifungal susceptibility study. Sao Paulo: Einstein; 2018. p. 16. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Haida K, Parzianello L, Werner S, Garcia D. Avaliação in vitro da atividade antimicrobiana de oito espécies de plantas medicinais. Arq Cienc Saude Unipar. 2007;11:185–192. [Google Scholar]
- Hoult JRS, Payá M. Pharmacological and biochemical actions of simple coumarins: natural products with therapeutic potential. Gen Pharmacol. 1996;27:713–722. doi: 10.1016/0306-3623(95)02112-4. [DOI] [PubMed] [Google Scholar]
- Hussain SH, Latif A, Cox RJ, Simpson TJ, Ali M, Arfan M, Uddin G. Phytochemicals from the aerial parts of Ligularia thomsonii and their radical scavenging activity. Phytochem Lett. 2014;7:6–10. doi: 10.1016/j.phytol.2013.09.002. [DOI] [Google Scholar]
- Ibrahim M, Abu-Reidah A, Contreras M, Arraez-Roman D, Fernandez-Gutierrez A, Segura-Carretero A. UHPLC-ESI–QTOF–MS-based metabolic profiling of Vicia faba L. (Fabaceae) seeds as a key strategy for characterization in foodomics. Electrophoresis. 2014;35:1571–1581. doi: 10.1002/elps.201300646. [DOI] [PubMed] [Google Scholar]
- Javadpour MM, Juban MM, Lo WCJ, Bishop SM, Alberty JB, Cowell SM, Becker CL, McLaughlin ML. De novo antimicrobial peptides with low mammalian cell toxicity. J Med Chem. 1996;39:3107–3113. doi: 10.1021/jm9509410. [DOI] [PubMed] [Google Scholar]
- Kim JH, Mun YJ, Im SJ, Han JH, Lee HS, Woo WH. Effects of the aqueous extract of Epimedii Herba on the antibody responses in mice. Int Immunopharmacol. 2001;1:935–944. doi: 10.1016/S1567-5769(01)00030-3. [DOI] [PubMed] [Google Scholar]
- Klančnik A, Piskernik S, Jeršek B, Možina SS. Evaluation of diffusion and dilution methods to determine the antibacterial activity of plant extracts. J Microbiol Methods. 2010;81:121–126. doi: 10.1016/j.mimet.2010.02.004. [DOI] [PubMed] [Google Scholar]
- Ksiezopolska E, Gabaldón T. Evolutionary emergence of drug resistance in Candida opportunistic pathogens. Genes. 2018;9:461–486. doi: 10.3390/genes9090461. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ksouri S, Djebir S, Bentorki AA, Gouri A, Hadef Y, Benakhla A. Antifungal activity of essential oils extract from Origanum floribundum Munby, Rosmarinus officinalis L. and Thymus ciliatus Desf. againstCandida albicans isolated from bovine clinical mastitis. J Mycol Med. 2017;27:245–249. doi: 10.1016/j.mycmed.2017.03.004. [DOI] [PubMed] [Google Scholar]
- Lavola A. Accumulation of flavonoids and related compounds in birch induced by UV-B irradiance. Tree Physiol. 1998;18:53–58. doi: 10.1093/treephys/18.1.53. [DOI] [PubMed] [Google Scholar]
- Leal LKAM, Matos ME, Matos FJA, Ribeiro RA, Ferreira FV, Viana GSB. Antinociceptive and antiedematogenic effects of the hydroalcoholic extract and coumarin from Torresea cearensis Fr. All. Phytomedicine. 1997;4:221–227. doi: 10.1016/S0944-7113(97)80071-2. [DOI] [PubMed] [Google Scholar]
- Leal LKAM, Nechio M, Silveira ER, Canuto KM, Fontenele JB, Ribeiro RA, Viana GSB. Anti-inflammatory and smooth muscle relaxant activities of the hydroalcoholic extract and chemical constituents from Amburana cearensis A. C. Smith. Phytother Res. 2003;17:335–340. doi: 10.1002/ptr.1139. [DOI] [PubMed] [Google Scholar]
- Leal LKAM, Fonseca FN, Pereira FA, Canuto KM, Felipe CFB, Fontenele JB, Pitombeira MV, Silveira ER, Viana GSB. Protective effects of amburoside A, a phenol glucoside from Amburana cearensis, against CCl4-induced hepatotoxicity in rats. Planta Med. 2008;74:497–502. doi: 10.1055/s-2008-1074501. [DOI] [PubMed] [Google Scholar]
- Lee YJ, Kuo HC, Chu CY, Wang CJ, Lin WC, Tseng TH. Involvement of tumor suppressor protein p53 and p38 MAPK in caffeic acid phenethyl ester-induced apoptosis of C6 glioma cells. Biochem Pharmacol. 2003;66:2281–2289. doi: 10.1016/j.bcp.2003.07.014. [DOI] [PubMed] [Google Scholar]
- Lima LR, Cavalcante RRL, Martins MCC, Parente DM, Cavalcante AAMCC. Avaliação da atividade antiedematogênica, antimicrobiana e mutagênica das sementes de Amburana cearensis (A. C. Smith) (Imburana-de-cheiro) Revista Brasileira de Plantas Medicinais. 2013;15:415–422. doi: 10.1590/S1516-05722013000300015. [DOI] [Google Scholar]
- Maia GN. Caatinga: Árvores e Arbustos e Suas Utilidades. Fortaleza: Printcolor gráfica e Editora; 2004. [Google Scholar]
- Menozzi CAC, Castelo-Branco FS, França RRF, Domingos JLO, Boechat N. Optimization of fluconazol synthesis: an important azole antifungal drug. Revista Virtual de Quimica. 2017;9:1216–1234. doi: 10.21577/1984-6835.20170071. [DOI] [Google Scholar]
- Morais-Braga MFB, Carneiro JNP, Machado AJT, dos Santos ATL, Sales DL, Lima LF, Figueredo FG, Coutinho HDM. Psidium guajava L., from ethnobiology to scientific evaluation: Elucidating bioactivity against pathogenic microorganisms. J Ethnopharmacol. 2016;194:1140–1152. doi: 10.1016/j.jep.2016.11.017. [DOI] [PubMed] [Google Scholar]
- Moure A, Cruz JM, Franco D, Manuel Domínguez J, Sineiro J, Domínguez H, Núñez MJ, Carlos Parajó J. Natural antioxidants from residual sources. Food Chem. 2001;72:145–171. doi: 10.1016/S0308-8146(00)00223-5. [DOI] [Google Scholar]
- NCCLS (2012) Método de Referência para Testes de Diluição em Caldo para Determinação da Sensibilidade de Leveduras à Terapia Antifúngica : Norma Aprovada-Segunda Edição
- Niero ELO. Efeitos de ácido cinâmico sobre melanócitos e células derivadas de melanoma humanos: avaliação do seu potencial antitumoral e de proteção contra danos celulares causados por radiação ultravioleta. Tese de doutorado. 2010 doi: 10.11606/T.42.2010.tde-28092010-111234. [DOI] [Google Scholar]
- Ning H, Xin ZC, Lin G, Banie L, Lue TF, Lin CS. Effects of icariin on phosphodiesterase-5 activity in vitro and cyclic guanosine monophosphate level in cavernous smooth muscle cells. Urology. 2006;68:1350–1354. doi: 10.1016/j.urology.2006.09.031. [DOI] [PubMed] [Google Scholar]
- Nishikawa K, Fukuda H, Abe M, Nakanishi K, Taniguchi T, Nomura T, Yamaguchi C, Hiradate S, Fujii Y, Okuda K, Shindo M. Substituent effects of cis-cinnamic acid analogues as plant growh inhibitors. Phytochemistry. 2013;96:132–147. doi: 10.1016/j.phytochem.2013.08.013. [DOI] [PubMed] [Google Scholar]
- Oliveira GP, Silva TMG, Camara CA, Santana ALBD, Moreira MSA, Silva TMS. Isolation and structure elucidation of flavonoids from Amburana cearensis resin and identification of human DNA topoisomerase II-α inhibitors. Phytochem Lett. 2017;22:61–70. doi: 10.1016/j.phytol.2017.09.006. [DOI] [Google Scholar]
- Pereira EPL, Braga-De-Souza S, Santos CC, Santos LO, Cerqueira MD, Ribeiro PR, Fernandez LG, Silva VDA, Costa SL. Amburana cearensis seed extracts protect PC-12 cells against toxicity induced by glutamate. Braz J Pharmacogn. 2017;27:199–205. doi: 10.1016/j.bjp.2016.08.010. [DOI] [Google Scholar]
- Plazonić A, Bucar F, Maleš Z, Mornar A, Nigović B, Kujundžić N. Identification and quantification of flavonoids and phenolic acids in Burr Parsley (Caucalis platycarpos L.), using high-performance liquid chromatography with diode array detection and electrospray ionization mass spectrometry. Molecules. 2009;14:2466–2490. doi: 10.3390/molecules14072466. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sadeghi M, Zolfaghari B, Senatore M, Lanzotti V. Antifungal cinnamic acid derivatives from Persian leek (Allium ampeloprasum Subsp. Persicum) Phytochem Lett. 2013;6:360–363. doi: 10.1016/j.phytol.2013.04.007. [DOI] [Google Scholar]
- Salas MP, Céliz G, Geronazzo H, Daz M, Resnik SL. Antifungal activity of natural and enzymatically-modified flavonoids isolated from citrus species. Food Chem. 2011;124:1411–1415. doi: 10.1016/j.foodchem.2010.07.100. [DOI] [Google Scholar]
- Schmeda-Hirschmann G, Burgos-Edwards A, Theoduloz C, Jiménez-Aspee F, Vargas-Arana G. Male sexual enhancers from the Peruvian Amazon. J Ethnopharmacol. 2019;229:167–179. doi: 10.1016/j.jep.2018.10.007. [DOI] [PubMed] [Google Scholar]
- Shunjun X, Yu J, Zhan J, Yang L, Guo L, Xu Y. Pharmacokinetics, tissue distribution, and metabolism study of icariin in rat. Biomed Res Int. 2017;2017:1–17. doi: 10.1155/2017/4684962. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Silva CR, De Andrade NJB, De Sousa CR, Figueiredo NS, Sampaio LS, Magalhães HIF, Cavalcanti BC, Gaspar DM, De Andrade GM, Lima ISP, De Barros VGS, De Moraes MO, Lobo MDP, Grangeiro TB, Nobre HV. Synergistic effect of the flavonoid catechin, quercetin, or epigallocatechin gallate with fluconazole induces apoptosis in Candida tropicalis resistant to fluconazole. Antimicrob Agents Chemother. 2014;58:1468–1478. doi: 10.1128/AAC.00651-13. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Silva KMA, Chaves TP, Santos RL, Brandão DO, Fernandes FHA, de Ramos JFJL, Medeiros ACD, dos Santos VL, Felismino DC. Modulation of the erythromycin resistance in Staphylococcus aureus by ethanolic extracts of Ximenia americana L and Schinopsis brasiliensis Engl. Bol Latinoam Caribe Plant Med Aromat. 2015;14:92–98. [Google Scholar]
- Simões C, Schenkel E, Gosman G (2007) Farmacognosia: da planta ao medicamento. Editora UFRGS 5
- Siqueira JF, Sen BH. Fungi in endodontic infections. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2004;97:632–641. doi: 10.1016/j.tripleo.2003.12.022. [DOI] [PubMed] [Google Scholar]
- Soares SE. Phenolic acids as antioxidants. Revista de Nutricao. 2002;15:71–81. doi: 10.1590/s1415-52732002000100008. [DOI] [Google Scholar]
- Steiner C, Arnould S, Scalbert A, Manach C. Isoflavones and the prevention of breast and prostate cancer: new perspectives opened by nutrigenomics. Br J Nutr. 2008 doi: 10.1017/S0007114508965788. [DOI] [PubMed] [Google Scholar]
- Stoppa MA, Casemiro LA, Vinholis AHC, Cunha WR, Andrade ML, Silva E, Martins CHG, Furtado NAJC. Comparative study of the recommended methodologies by Clsi and Eucast for activity evaluation antifungal. Quim Nova. 2009;32:498–502. doi: 10.1590/S0100-40422009000200038. [DOI] [Google Scholar]
- Strack D (1997) Phenolic metabolism. In: Dey P, Harborne J (eds) Plant biochemistry. Elsevier, pp 387–416
- Wei H, Zili L, Yuanlu C, Biao Y, Cheng L, Xiaoxia W, Yang L, Xing W. Effect of icariin on bone formation during distraction osteogenesis in the rabbit mandible. Int J Oral Maxillofac Surg. 2011;40:413–418. doi: 10.1016/j.ijom.2010.10.015. [DOI] [PubMed] [Google Scholar]
- Zhang ZB, Yang QT. The testosterone mimetic properties of icariin. Asian J Androl. 2006;8:601–605. doi: 10.1111/j.1745-7262.2006.00197.x. [DOI] [PubMed] [Google Scholar]
- Zida A, Bamba S, Yacouba A, Ouedraogo-Traore R, Guiguemdé RT. Substances naturelles actives sur Candida albicans, sources de nouveaux médicaments antifongiques: revue de la littérature. J Mycol Med. 2017;27:1–19. doi: 10.1016/j.mycmed.2016.10.002. [DOI] [PubMed] [Google Scholar]