Abstract
The COVID-19 pandemic caused by SARS-CoV-2 has emerged as a global issue of concern for public health, environment and socio-economic setup. This review addresses several aspects of epidemiology, and pathogenesis, environmental resource quality (air quality, hazardous waste management, and wastewater surveillance issues), and socio-economic issues worldwide. The accelerated research activity in the development of diagnostic kits for SARS-CoV-2 is in progress for the rapid sequencing of various strains of SARS-CoV-2. A notable reduction in air pollutants (NO2 and PM2.5) has been observed worldwide, but high air polluted cities showed intense mortalities in COVID-19 affected areas. The use of health safety equipment halted transportation, and work-from-home policy drastically impacted the quantity of solid and hazardous wastes management services. Wastewater appeared as another mode of enteric transmission of SARS-CoV-2. Thus, wastewater-based surveillance could act as a mode of the data source to track the virus's community spread. The pandemic also had a substantial socio-economic impact (health budget, industrial manufacturing, job loss, and unemployment) and further aggravated the countries' economic burden.
Keywords: COVID-19, Air pollution, Socio-economic aspects, Wastewater surveillance, Solid waste management
Graphical abstract
Highlights
-
•
COVID-19 pandemic urge a molecular-level understanding of viruses like SARS-CoV-2.
-
•
Studies showed interrelationship of COVID-19 mortalities and air pollution.
-
•
Wastewater surveillance could gauge the success of precautionary measures.
-
•
COVID-19 drastically affected the global solid waste management sector.
-
•
COVID-19 had an adverse socio-economic impact by aggravated health burden of the community.
1. COVID-19: epidemiology and pathogenesis
Since the time of its detection in late December 2019 as a causative agent of a cluster of pneumonia cases in Hubei province, China, about 27.5 million cases have been reported till the end of August 2020 in 215 countries worldwide (Figure S1, Supplementary section) with about 0.89 million deaths (COVID-19, 2020). World Health Organization (WHO), on January 30, 2020, reconvened the Emergency Committee (EC) to declare the ‘2019-nCoV’ as an outbreak that constituted a Public Health Emergency of International Concern (PHEIC). On February 11, 2020, the International Committee on Taxonomy of Viruses (ICTV) provided a new name to the virus -severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and it has exhibited a closer genetic relatedness to the 2003 -SARS outbreak caused due to SARS-CoV (WHO, 2020; Adhikari et al., 2020; Zhu et al., 2020). The same day, WHO has provided the name-coronavirus disease (COVID-19) to the new disease caused by SARS-CoV-2 (WHO, 2020). By March 11, 2020, WHO declared COVID-19 a global pandemic (Cucinotta and Vanelli, 2020).
The first edition of WHO guidance (ref. no: WHO/2019-nCoV/IPC/2020.3) on infection prevention and control (IPC) relied on five key aspects; “i) ensuring triage, early recognition, and source control; ii) applying standard precautions for all patients; iii) implementing empiric additional precautions; iv) implementing administrative controls; v) using environmental and engineering controls” (adapted from WHO guidelines- COVID-19: Infection prevention and control/WASH) (WHO Global; WHO/2019-nCoV/IPC/2020.3.).
1.1. Molecular features and potential anti-viral interventions of SARS-CoV-2
SARS-CoV-2 virus's structural and functional proteins and genomic segments responsible for generating a functional viral particle is depicted in Fig. 1 . SARS-CoV-2 is a single-stranded RNA virus belonging to beta coronaviruses, which are classified under the genus beta coronaviruses and subfamily- Orthocoronaviridae. Known coronaviruses pathogenic to humans so far are SARS-CoV-2, HCoV-229 E, HCoV-OC43, SARS-CoV, HCoV-NL63, HCoV-HKU1 and MERS-CoV (K. Chen et al., 2020). A typical coronavirus genome encodes four major structural proteins, viz; the spike protein [S], the nucleocapsid protein [N], the membrane protein [M], and the envelope protein [E]. These structural proteins [the spike protein, S; the membrane protein, M; the nucleocapsid protein, N and the envelope proteins, E] create a functional viral particle (Schoeman and Fielding, 2019). The S-protein is crucial in viral attachment to the host receptor, fusion, and entry into the host cell and, as such, is a major target for antiviral therapeutics (Liu et al., 2004).
Fig. 1.
SARS-CoV-2 pictorial representation depicting structural and functional proteins (a) and genomic segments responsible for generation of a functional viral particle (b).
Angiotensin-converting enzyme 2 (ACE2), which is a metallopeptidase isolated from SARS-CoV permissive Vero E6 cells, was identified as the receptor for the S1 domain (Spike protein) of SARS-CoV strain (Li et al., 2003). Further, the X-ray crystallographic structural analysis of the receptor-binding domain (RBD) of the spike protein of SARS-CoV-2 strain in a molecular complex with ACE2 established a tight binding as compared to ACE2 binding with the strains of SARS-CoV or RaTG13 (a bat coronavirus) (Shang et al., 2020a, 2020b). Since ACE2 is downregulated after the SARS-CoV-2 infection, the AngII (angiotensin II) degradation is reduced, thereby increasing inflammatory responses leading to organ damage in the host (Q. Li et al., 2020a, 2020b). In MERS-CoV, the host receptor has been identified as dipeptidyl peptidase 4, DPP4, or CD26 revealing a divergent recognition pattern amongst coronaviruses (Raj et al., 2013). The human serine protease TMPRSS2 is required for S-protein priming on SARS-CoV-2 for cell entry through the ACE2 receptor. The serine protein inhibitor, camostate mesylate could inhibit the activity of TMPRSS2 and can be a potential antiviral intervention (Hoffmann et al., 2020).
Nanobodies are camelid-derived single-domain antibody fragments-the variable domain of heavy chain (VHH), which has been considered anti-tumour, auto-immune and anti-viral therapeutics (Demarest and Glaser, 2020). Through cryo-electron microscopy analysis, a 12.8 kDa nanobody has been identified to bind SARS-CoV-2 spike protein's receptor binding domain, RBD (complex structure resolved at 2.9 Å) with high specificity and affinity, thereby blocking the receptor binding to the viral particle (Hanke et al., 2020), that may become a potential anti-viral molecule after further studies. A recombinant RBD protein has been characterized by Tai et al. (2020) with a plausibility of candidate rRBD vaccine against SARS-CoV-2 to induce cross-reactive/cross-neutralizing antibodies in host cells.
1.2. Zoonotic origins
Significant outbreaks have emanated from coronaviruses earlier in 2002–2003 with ~800 deaths by SARS-CoV and ~850 deaths by MERS-CoV in 2012 (Du Toit, 2020). Isolation and detection of zoonotic SARS-CoV strain was based on studies performed between 2003 and 2005 on healthy Himalayan palm civets (Paguma larvata); ferret badgers (Melogale moschata), and raccoon dogs (Nyctereutes procyonoides) (Guangdong, China) (Wang et al., 2005); as well as ferrets (Mustela furo) and domestic cats (Felis domesticus) (Martina et al., 2003; Wong et al., 2020). In case of MERS- CoV, the common European bat (Pipistrellus kuhlii) acted as a natural host (Wong et al., 2020; Ithete et al., 2013) while the serological studies carried out on dromedary camels (DC) in the Kingdom of Saudi revealed the role of DC in the inter-species transmission of MERS- CoV to humans (Alagaili et al., 2014; Hemida et al., 2014).
Full-length genome analysis of beta coronaviruses isolated from the horseshoe bats, Rhinolophus sinicus and R. affinis, reveal 80% and 96% gene sequence identity with SARS-CoV-2, respectively (James et al., 2020; Zhou et al., 2020). Isolation of coronavirus strain from Malayan pangolin (Manis javanica) has revealed an amino acid identity of 100%, 98.2%, 96.7%, and 90.4% with the E (envelope), M (membrane), N (nucleocapsid), and S (spike) -proteins of SARS-CoV-2, respectively suggesting a plausible role of Malayan pangolin as an intermediate host (Xiao et al., 2020). The metagenomic sequencing of samples (lung, intestine, and blood) from Malayan pangolin by Lam et al. (2020) identifies it as a natural reservoir/intermediate host for SARS-CoV- 2 (HCoV-19). Further, it has been suggested that SARS-CoV-2 might have had its origins due to possible recombination between a Bat-CoV-RaTG13-like virus (Zhou et al., 2020) and a Pangolin-CoV-like virus (Wong et al., 2020; Xiao et al., 2020).
1.3. Transmission characteristics
The modes of transmission and precautionary measures, and survival times of SARS-CoV-2 on various surfaces are illustrated in Fig. 2 . The asymptomatic transmission has been extensively studied to understand the escalation in infection (Steffens, 2020). In this regard, the study on the outbreak on board of the cruise ship- Diamond Princess revealed that ~18% of total infections documented were asymptomatic (Mizumoto et al., 2020). Experimental studies on the viability of SARS-CoV-2 in aerosols (stable for ~3 h) and various surfaces (stable for ~72 h) indicated that aerosol and fomite transmission is credible (van Doremalen et al., 2020). Person-to-person transmission has been the primary mode for viral spread through nosocomial infections are of critical concern (Wang et al., 2020). Recently, though a case study by Gao et al. (2020) involving a singular patient revealed that asymptomatic transmissions might be weaker than projected rates, and further studies are required to verify the same.
Fig. 2.
SARS-CoV-2: Modes of transmission and precautionary measures along with survival on various surfaces (Sources: Nghiem et al., 2020a; Steffens, 2020).
As shown in Table 1 , SARS-CoV-2 exhibited a higher basic reproduction number (R 0) as compared to SARS-CoV or MERS- CoV (Chowell et al., 2004; Choi et al., 2018; Riou and Althaus, 2020; Steven et al., 2020). Riou and Althaus (2020) studied the initial pattern of human to human transmission of COVID-19 with an estimated R 0 value of ~2.2. An R 0 value above 1 is an indicator that there will be a sustained transmission chain with continuous human-to-human transmission. However, this R 0 value has been re-calibrated by the studies performed by Steven et al., (2020) to ~4.7 (yet to be published). The preventive measures so far for SARS-CoV-2 to arrest the spread have been the three-pronged mechanism involving (i) an early detection and isolation, (ii) contact tracing, and (iii) appropriate use of personal protective equipment (PPE).
Table 1.
A global summary of coronavirus outbreaks, epidemiological statistics, and clinical manifestations.
| Characteristic feature | SARS-CoV (Severe Acute Respiratory Syndrome -Coronavirus) (NCIRD, 2017; SARS, 2020) | MERS-CoV (Middle East Respiratory Syndrome- Coronavirus) (CDC, 2019a) | SARS-CoV-2 (Severe Acute Respiratory Syndrome -Coronavirus −2) (CDC, 2020; WHO, 2020b) | |
|---|---|---|---|---|
| Incidence and source | Disease | SARS | MERS | COVID-19 |
| Nature of the disease | Epidemic | Epidemic | Pandemic | |
| Origin | Bats, Palm Civets | Dromedary Camels | Bats | |
| Outbreak detected | February 2003 Guangdong, China | September 2012 Saudi Arabia | December 2019 Wuhan, China | |
| Transmission | Zoonotic, Nosocomial, Human to human | Zoonotic, Nosocomial, Human to Human | Zoonotic, Nosocomial, Human to Human | |
| Epidemiological statistics | Basic reproduction number (R0) | 0.19–1.08 (Chowell et al., 2004) | 2.0–5.0 (Choi et al., 2018) | 2.2–2.7 (Riou and Althaus, 2020), 4.7–6.6 (Steven et al., 2020) |
| Incubation time (in days) | 2–7 | 2–6 | 2–14 | |
| Laboratory confirmed cases | 8098 | 2494 | 7,805,148 | |
| No. of deaths reported (fatality rate -%) | 774 (9.55) | 858 (34.4) | 431192 (5.52) | |
| No. of countries affected | 26 | 27 | 216 | |
| Clinical manifestations | Target host cell receptor | Human angiotensin-converting enzyme 2 (ACE2) | Human dipeptidyl peptidase 4(DPP4 or CD26) | Human angiotensin-converting enzyme 2 (ACE2) |
| Common symptoms | Fever, malaise, myalgia, headache, diarrhea, and shivering (rigors) | Fever, chills/rigors, headache, non-productive cough, dyspnea, and myalgia | Fever, dry cough, and tiredness | |
| Other symptoms | Cough (initially dry), shortness of breath, and diarrhea | Sore throat, coryza, sputum production, nausea and vomiting, dizziness, diarrhea, and abdominal pain | Aches and pains, sore throat, diarrhea, conjunctivitis, headache, loss of taste or smell, a rash on the skin, or discoloration of fingers or toes | |
| Critical symptoms | Pneumonia and respiratory failure, heart, and liver failure. | Febrile upper respiratory tract illness leading to pneumonia. Acute respiratory distress syndrome (ARDS), refractory hypoxemia, and extrapulmonary complications. | Difficulty breathing or shortness of breath, chest pain or pressure, loss of speech or movement. Viral pneumonia and ARDS | |
| Comorbid conditions | Diabetes and Hepatitis | Diabetes, renal failure, chronic lung disease, immunocompromised persons | Diabetes, chronic lung disease, immunocompromised persons, severe obesity, renal and heart problems |
1.4. Clinical trials, diagnosis, and detection of SARS-CoV-2
The international clinical trials registry platform at https://www.who.int/emergencies/indicate that ~2800 trials are active as of May 21, 2020. The number of interventional clinical trials registered with https://clinicaltrials.gov/ct2 are 1052 by May 31, 2020, of which a representative list is comprising the completed trials (phases 2, 3, and 4) and active/recruiting trials for phase 1 (Table S1). Mechanisms involving antiviral/retroviral compound administration, mechanical ventilation support, steroidal treatment, and blood plasma transfusions are under varied phases in clinical trials worldwide. Increased mortality levels have been observed for infected individuals with acute respiratory distress syndrome (ARDS), arrhythmia, myalgia, cardiovascular shock, and heart attack.
Computed Tomography (CT) scans and nucleic acid testing has been the prominent modes of detection for COVID-19 (CDC, 2019b; Udugama et al., 2020). Three distinct highly conserved regions of the SARS-CoV-2 genome, viz; the genes RdRP (RNA dependent RNA polymerase), the E (envelope protein gene), and the N (nucleocapsid gene) has been identified by Corman et al. (2020) to develop and design primers for RT-PCR methods. Recent emphasis has been on developing the faster and robust technique of RT-LAMP (reverse transcriptase-loop-mediated isothermal amplification) using four to six primers against SARS-CoV-2 that could be performed well within 30 min (Lamb et al., 2020). SHERLOCK protocol (using Cas13a ribonuclease for RNA sensing) has been successfully utilized for the detection of SARS-CoV-2 (Hou et al., 2020).
The accelerated research activity in the development of diagnostic kits for SARS-CoV-2 is in progress for the rapid sequencing of various strains of SARS-CoV-2. It is to be noted that SARS-CoV-2 infection leads to the production of anti-viral protein antigens and antibodies in the host system, which can be utilized for diagnosing COVID-19. Serological testing mechanisms such as enzyme-linked immunosorbent assays (ELISA) utilizing SARS-CoV-2 Rp3 nucleocapsid protein (Zhang et al., 2020) or synthetic peptide antigens derived from the S and N proteins (Cai et al., 2020) has been used for the detection of COVID-19.
2. Environmental perspectives of COVID-19
2.1. COVID-19 pandemic and global air quality: some good news and some bad news
Air pollution is accountable for about 7 million premature deaths every year worldwide, and half of which is mainly due to outdoor air pollutants (mainly PM2.5, near-surface Ozone, NO2) (NASA, 2020a). Recent empirical studies indicate the direct impact of COVID-19 on the environment and vice versa. Studies suggested that climate, weather conditions, and even topography (latitude) directly correlate with COVID-19 (Baker et al., 2020; Carlson et al., 2020; Huang et al., 2020). Similarly, COVID-19 has directly impacted the environmental parameters such as municipal solid waste generation, water quality, outdoor and indoor, and air quality. The COVID-19 lockdown has improved the air quality in many parts of the world in terms of PM2.5, NOx, and SO2; however, there is some increase in pollutant like ground-level Ozone is also observed in some parts of the world due to atmospheric chemical process (Huang et al., 2020; Lam et al., 2020). Due to lockdown and social distancing, transportation and industrial activities have been stalled for the time being, which improved the air quality in urban areas. Human activities directly contribute to an increased level of PM2.5, aerosols, SOx, CO2, and NO2 in the atmosphere. Studies revealed the improvements in the level of NO2, PM2.5, and aerosols worldwide during this COVID-19 epidemic. NO2 is designated as a criteria pollutant due to its direct impact on nitrate aerosol and being a major component of PM2.5. Recent images by NASA's EOS-Aura satellite and European Space Agency's ERS-2 satellite indicate significant changes in global NO2 and aerosol concentration in the troposphere, below 10 km, which is the main area of human emissions due to transportation and industrial activities.
2.1.1. Global NO2 concentration during COVID-19 epidemic
NO2 emission is the indicator of industrial activities (mainly burning of gasoline, coal, diesel, etc.) and is considered as the human-made source in the troposphere. NASA's EOS-Aura satellite images were compared with the NO2 concentration (molec./cm2) in 2020 concerning baseline values (2015–2019) for the same period (month) (Fig. 3 ) for severely affected regions like Europe, Asia, and North America. The comparative study indicates the significant impact of COVID-19 lockdown on NO2 concentration in these regions (NASA, 2020b). The world's longest lockdown linked with the coronavirus's slow spread in India, China, and Europe. Studies by NASA and European Space Agency (ESA) indicates a significant reduction in air pollutants over China after shut down of transportation and industrial activities and NO2 level rebound to a nearly normal level for this time of the year (NASA, 2020b; Bauwens et al., 2020). In another image (Figure S2a, Supplementary section) by Tropospheric Monitoring Instrument (TROPOMI) on ESA's Sentinel-5 satellite and NASA's EOS-Aura satellite images indicts a dramatic drop in NO2 concentration over the widespread areas of China during industrial shutdown under COVID-19 lockdown. Maps show the slow level of NO2 during quarantine (10–January 25, 2020) and after the restriction was lifted (20–May 12, 2020). Figure S2b (Supplementary section) indicates that the NO2 trend was drastically lower (10–30%) in the COVID-19 period than the last five years' average (2015–2019) concentration (NASA, 2020b). The decline in NO2 concentration during the new year period (started in China during 25th January) is common in China when industrial activities are halted. New images from the Copernicus Sentinel-5P satellite of the European Union Copernicus programme indicates that in India, NO2 concentration dropped around 40–50% in major industrial cities Mumbai and Delhi as compared to the same time in the previous year (Figure S2b, Supplementary section) (ESA, 2020; NASA, 2020b) due to nationwide quarantine.
Fig. 3.
NO2 concentration comparison between five-year average (2015–2019) and year 2020 for same months (January 2020 and June 2020) in three severally affected parts of the world by COVID-19 (a) USA, (b) Europe, and (c) Asia. Source: Global Nitrogen Dioxide Program (Source: NASA, 2020b).
According to images provided by the Tropospheric Emission Monitoring Internet Service (TEMIS) program of ESA, the NO2 level in the USA was significantly lowered during the COVID-19 lockdown as compared to the images of January 2020 and June 2020 (Figure S2c, Supplementary section) (ESA, 2020). In Northern America, the NO2 concentration decreased significantly, up to 30%, during the lockdown period of 2020 as compared to the average NO2 level observed during the last five years (2015–2019) in the same month (NASA, 2020b). Recent reports based on Copernicus Sentinel-5P satellite images revealed that most industrial cities in Europe showed about 45–50% decline in NO2 level compared to the last year during this COVID-19 pandemic (ESA, 2020). Comparison of images taken between the period 13 March to April 13, 2020 and March–April 2019 suggested 45–54% decline in NO2 concentration at Paris, Madrid, Milan, and Rome cities of Europe (ESA, 2020) (Figure S2d, Supplementary section). A recent study published by Bauwens et al. (2020) revealed that Seoul and Daegu cities of South Korea showed about 43% and 24% reduction in NO2 columns during the first weeks of the health alert posted on February 23, 2020 and that significantly lower than the level reported in the previous year on the same period.
2.1.2. PM2.5, aerosols and overall air quality in major cities of the world during COVID-19
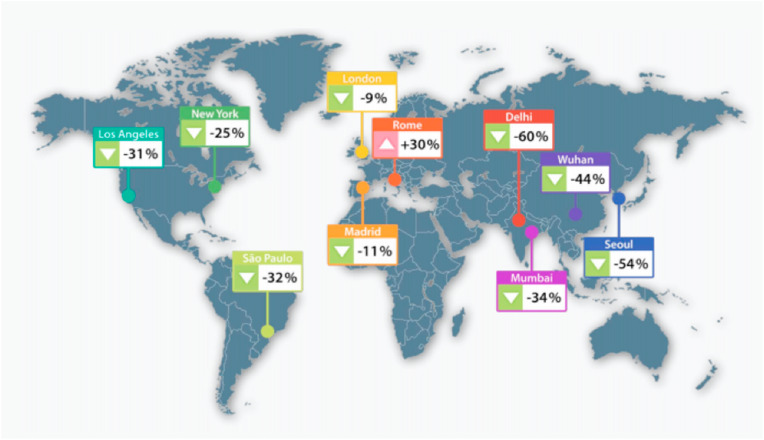
The level of air quality has improved in the majority of the global cities due to the halt in key air pollution source activities (i.e., transportation, industry, commercial activities) during the COVID-19 lockdown phase. Substantial reduction in outdoor PM2.5 concentration observed in the top five most polluted cities of the world, namely Ghaziabad (India); Gujranwala (Pakistan); Faisalabad (Pakistan); Delhi (India) Noida (India) during the strict lockdown periods. The level of PM2.5 and NOx have reduced about 20–60% during the COVID-19 lockdown as compared to the pre-COVID-19 time in most of the global cities, which followed the lockdown norms. The impact of the freezing economic activities due to COVID-19 lockdown on local air quality clearly noticed in major financial cities of the world (Fig. 4 ) (IQAir, 2020). Globally, the highest drop in outdoor PM2.5 concentration was detected in Delhi (−60%) followed by Seoul (−54%) and Wuhan (−44%) (Li et al., 2020a, 2020b; IQAir, 2020). Some of the United States cities have exhibited remarkable clean hours where the outdoor PM2.5 level has reached to almost 95% less than to World Health Organization (WHO) threshold guideline (<25 μg/m³-24-h mean). For example, in Los Angeles and New York, cities 90% and 98% hours between 7 and 28th of March, the PM2.5 level was below 1.3 μg/m³ (extremely rare) (IQAir, 2020).
Fig. 4.
PM2.5 reductions in 10 major cities worldwide during the period 23 March – 13 April 2020 of the COVID-19 (Source: IQAir, 2020).
Aerosols (solid and liquid particles suspended particles) from human sources cause unhealthy air with low visibility and can damage human health by affecting the functioning of vital organs like the lungs and heart (NASA, 2020b). A recent report by earth observatory of NASA based on Moderate Resolution Imaging Spectroradiometer (MODIS) on NASA's Terra satellite revealed that aerosol level was at 20-years’ lower in the Indio-Gangetic plain (NASA, 2020b) (Figure S2, supplementary section). Air quality in urban areas is also improved during COVID-19 lockdown. Central Pollution Control Board (CPCB) India revealed that during public lockdown the air quality in Indian cities (data of 103–115 cities) significantly improved, based on Air Quality Index (AQI), from 50 moderate (AQI, 101–200), 49 satisfactory (AQI 51–100), and 6 good (0–50) to 12, 61, and 30, respectively during the period 16 March to March 31, 2020 (CPCB, 2020).
Almost 2.9 billion people globally use solid biomass for daily cooking and heating needs, the primary source of household indoor air pollution. Every year more than four million people die prematurely globally due to the exposure to this high indoor air pollution. The COVID-19 lockdown stay home norms have reduced the outdoor air pollution extensively. However, it is difficult to say that people around the world have less exposure to air pollution, primarily those who use solid fuel for cooking. The indoor PM2.5 concentration in households using solid fuel for cooking ranges between 150 μg/m³ and 800 μg/m³, many times higher than the regular days' outdoor PM2.5 concentration. Regular days on average solid fuel users population spend 20% of their time outside the home where the PM2.5 level is less than the indoor level (NSSO, 1998). During COVID-19, lockdown stay home norms entire population have to remain inside the home, which indicates that in this solid fuel user households more exposed to higher air pollution as compared to pre-COVID-19 days.
2.1.3. Health burden due to air pollution and COVID-19
Formulation of well-informed policies by the health sector duly owes its success to numerous valuation studies that were performed globally in the past few decades. These valuation studies were aimed at quantifying the adverse impacts of environmental degradation on human health (Remoundou and Koundouri, 2009). The cause-specific disability-adjusted life year (DALY) has emerged in the global context as a new measure of the ‘burden of disease’ (Anand and Henson, 1998). As per the global estimates by WHO, air pollution is solely responsible for 6.7% of overall deaths and 7.6% of DALYs, respectively (Lim et al., 2012). The study conducted by Balakrishnan et al. (2019) revealed that air pollution impresses upon India a higher level of mortality rate and a huge disease burden. The relative risks for mortality are mostly observed for diseases like acute lower respiratory infections, chronic obstructive pulmonary disease, diabetes, ischemic heart diseases, lung cancer, and stroke, etc. due to ambient air and household exposure to PM2.5. A study by a researcher team from T.H. Chan School of Public Health, Harvard University, USA, based on 3080 counties data analysis, confirms that areas with high air pollution (especially PM2.5) would have high death rates in COVID-19 affected areas (Wu et al., 2020). They revealed that only 1 μg/m3 increase in PM2.5 would cause about an 8% increase in the COVID-19 death rate (95% confidence interval: 2%, 15%). In another study, Cui et al. (2003) found an interesting interrelationship between mortality rate and patient with SARS-CoV-2 in China. They found that the death rate in areas with low pollution levels was 4.08, while areas with moderate and high air pollution levels showed about 7.49 and 8.9% mortality during this COVID-19 pandemic in China. In contrary to these, few recent studies indicate the reduction in disease burden mainly due to NO2 and PM2·5, mainly by improved air qualities under this COVID-19 lockdown period. For example, Y. Chen et al. (2020) estimated the interrelationships between air pollutants (daily nitrogen dioxide, NO2; and PM2·5) and associated disease burden in Wuhan, Hubei, and other parts of China (367 Chinese cities) during this pandemic period using concentration-response functions (CRFs) modelled with attributable function method. Their study revealed that traffic-related air pollution burden substantially reduced in Chines cities (22·8 μg/m3 in Wuhan and 12·9 μg/m3 in China; PM2·5 1·4 μg/m3 in Wuhan and 18·9 μg/m3 in other parts of China) due to home quarantine and traffic bans, resulted in avoiding of 8911 and 3214 deaths related to the NO2 and PM2.5 in these cities. A study published by the Italian Society of Environmental Medicine suggested that the rapid contagion rate in some parts of Northern Italy could be due to atmospheric particulate pollutants that possibly acted as carriers and booster for coronavirus (Setti et al., 2020). Thus, few global fora suggested that it will be too early to prove a direct relationship between current air pollution scenarios and incidences of COVID-19. The high pollution could have increased the risk in the first level, but long-term monitoring is also needed to establish a correlation between urban air quality and death rate during COVID-19 outbreak.
2.2. Wastewater and COVID-19 pandemic
As per the WHO, SARS-CoV-2 does not easily outspread through the sewerage system. Nevertheless, unlike other microorganisms, non-contagious genetic remains of the virus can persist in wastewater systems in the localities of the infected population (Graham, 2020). Human excreta like faeces, sputum, and saliva could shed to both viable SARS-CoV-2 and viral RNA, which are consequently observed in wastewater. Even though the vital route of viral transmission is considered inhalation through human to human, via fomites and aerosols and hand contagion, existing data uncovers the prerequisite to understand the role of wastewater based epidemiology (WBE) and wastewater surveillance approach to forecast the transmission or re-emergence of viral infection among the communities (Kitajima et al., 2020). It has several advantages over the clinical investigation and may act as an efficient early warning system (EWS) for COVID-19 and future outbreaks (Fig. 5 )
Fig. 5.
Wastewater surveillance as an early warning system for COVID-19 (Randazzo et al., 2020a).
WBE is a new concept to understand the health of a population using “pooled samples.” These samples reflect the whole community as everyone contributes to it, say, sewage from a wastewater treatment plant (WWTP) or surface water sources (lakes, ponds, river stretch) in an area. From these samples, biological or chemical compounds can be extracted, analyzed, and interpreted to test a hypothesis. These compounds, often called biomarkers, can be chemicals like food toxicants and anthropogenic excretion products, like metabolites (Sims and Hordern, 2020). For example, WBE was successfully applied to find the pattern of illicit drug consumption in a community. Higher than expected concentration of illicit drugs was found in the sewage, which helps to reveal the types and rates of drug usage and to trace the hotspots of drug usage more precisely and possibly gauge the success of police countermeasures (Main et al., 2014).
2.2.1. Wastewater based epidemiology (WBE) and wastewater surveillance
Wastewater based epidemiology (WBE) and wastewater surveillance approach could be used as a non-invasive early-warning tool to alert the public to new COVID-19 infections (Mallapaty, 2020). Table 2 summarizes the findings of testing SARS-CoV-2 in wastewater at different WWTPs, sewerage systems, manholes, and surface waters during the year 2020. In a recent study in Australia (Ahmed et al., 2020), the researchers enumerated the SARS-CoV-2 RNA from wastewater using reverse transcriptase quantitative polymerase chain reaction (RT-qPCR). The Monte-Carlo simulation of estimated viral RNA copy numbers was used to evaluate the number of infected people (171–1090) in the catchment of WWTP. The findings revealed the significance of WBE for tracking contagious diseases like COVID-19 in populations having symptomatic and asymptomatic individuals. Hart and Halden (2020) conducted the computational analysis and modeling study to realize the practicability of examining SARS-CoV-2 in wastewater. They reported that one infected person hypothetically is traceable amongst 100 to 2,000,000 persons. The temperature and travel period in the sewerage network acutely affects the detection of the virus. Employing the proposed methodology, 2.1 billion people can be examined worldwide in 105,600 wastewater treatment plants. The implementation of WBE, in conjunction with clinical trials, could be time and cost-saving. Researchers from the Netherlands conducted a composite wastewater sampling at Schiphol Airport, Amsterdam, for COVID-19 virus analysis. The samples were analyzed using quantitative RT-PCR methodology and found positive for virus RNA, i.e., four days later, the first COVID-19 case surfaces in the Netherlands. The findings indicate that the virus released from potential symptomatic, asymptomatic, or pre-symptomatic persons transiting through the airport (Lodder and Husman, 2020). Moreover, wastewater samples were tested positive for the presence of COVID-19 virus RNA near Tilburg (Netherlands) within a week of first Dutch cases were reported. The above-discussed findings revealed that wastewater could serve as a subtle surveillance system and early warning tool (Lodder and Husman, 2020). Medema et al. (2020) reported the presence of SARS-CoV-2 virus RNA in the wastewater samples collected from seven cities and airports in The Netherlands. An increase in the RNA concertation in wastewater samples was positively correlated with the surge in the number of infections. The WBE could serve as an essential surveillance tool, as are clinical trials, mainly among asymptomatic and pre-symptomatic responses of many viral contagions and their misdiagnosis. Worldwide cases have been reported where the peoples get infected despite no travel history to COVID-19 impacted regions or not exposed to any infected individual. There is a possibility of enteric transmission in peoples who work with human waste and wastewater. At this juncture, access to safe water, sanitation, and hygiene conditions and safe disposal of human waste (specifically hospital waste and effluent) can serve as protective measures against any contagion, including COVID-19 (Lodder and Husman, 2020). Gormaley et al. (2020) suggested that the wastewater plumbing infrastructure (involving sewerage system) carrying a considerable viral load and aerosolization potential of virus (airborne spread) can be considered a potential transmission route of COVID-19 infection to communities. Particularly hospitals and health care premises are at high-risk. In the latest study, La Rosa et al. (2020b) concluded that SARS-CoV-2 has a poor survival rate in the water environment than non-enveloped viruses, and it is very sensitive to temperature (deactivate rapidly at 23 °C −25 °C than at 4 °C) and oxidants (chlorine). The virus RNA has been enumerated in water samples but not as a contagious virion (virus particle). No evidence has been reported so far about the presence of viruses in-ground or surface water or transmission through contaminated water. Future research should be focused on the development and optimization of reliable methodologies for virus detection.
Table 2.
Findings of testing SARS-CoV-2 in Wastewater at Different WWTP during the year 2020.
| Country | Sampling |
Outcomes | Reference | ||
|---|---|---|---|---|---|
| Location | Sample Type | Duration | |||
| Australia |
|
|
7 days (February–April) |
|
Ahmed et al. (2020a) |
| France |
|
|
2 months (March–April) |
|
Wurtzer et al. (2020) |
| Israel |
|
|
10 days (March–April) |
|
Or et al. (2020) |
| Italy |
|
|
8 days (February–April) |
|
La Rosa et al. (2020a) |
|
|
2 days (April) |
|
Rimoldi et al. (2020) | |
| Netherlands |
|
|
March: Before the outbreak, Outbreak started, Outbreak spread |
|
Medema et al. (2020) |
| Spain |
|
|
March–April |
|
Randazzo et al. (2020a) |
|
|
February–April |
|
Randazzo et al. (2020b) | |
| Turkey |
|
|
April |
|
Kocamemi et al. (2020a) |
|
|
May |
|
Kocamemi et al. (2020b) | |
| USA |
|
|
March |
|
Wu et al. (2020) |
|
|
March–April |
|
Nemudryi et al. (2020) | |
2.2.2. Methods of virus detection in wastewater
Recently, a group from Cranfield Water Science Institute developed a small portable paper-based device to detect SARS-CoV-2 on-site in wastewater and track disease carriers in the community (Mao et al., 2020). The paper device is used to filter the viral genome fragments from wastewater samples. The presence of SARS-CoV-2 RNA is confirmed by a visible green or blue-coloured ring representing a positive or negative result. This paper-based testing method is less expensive and labour-intensive than PCR based detection. Such paper-based analytical devices enable on-site screening of COVID-19 carriers in real-time in the case of asymptomatic infections in the community. The science of quantitative microbial risk assessment (QMRA) has been used for more than 40 years (Haas et al., 1999). It has proved beneficial both with the severe acute respiratory syndrome (SARS) (Watanabe et al., 2010) and the Middle East respiratory syndrome (MERS) (Adhikari et al., 2020) outbreak. QMRA helps in studying, identifying, and evaluating different aspects of disease outbreak such as potential risks, ventilation rate at the workplace, social distance protective enough, surface disinfection targets (e.g., UV light), determining wastewater treatment disinfection targets, etc. (Kitajima et al., 2020). Modeling-based approach may prove to be a beneficial tool in tackling the COVID-19 impact. Nemudryi et al. (2020) applied two different sampling methods to investigate the SARS-CoV-2 in wastewater. They reported that the sampling method is crucial and that composite samples could provide a more reliable viral concentration in wastewater over time. Murukami et al. (2020) suggested that there is a necessity to develop the essential techniques to detect the SARS-CoV-2 RNA in wastewater samples. In the meantime, wastewater samples could be preserved for future verification of the methods and rebuilding the progression trend of the contagion.
2.2.3. Operationalizing wastewater surveillance
It has been recognized as an essential tool to detect an infectious disease outbreak previously (WHO, 2013) for other viral diseases. Many countries like Australia, Israel, China, and many European countries have made a strategic investment into WBE nationally (Hart and Halden, 2020). As evident in current scenario, diseases can spread across borders very quickly. Hence, there is a compelling case to operationalize it internationally, especially as it is it is much faster and cheaper than clinical surveillance. For this, the researchers, industry, and government decision-makers must work together. Figure S3 is a simplified process flow diagram to implement WBE using samples from sewerage network and currently available analytical tools. The sample should be collected regularly (for instance, every third day, when there is no outbreak) from WWTPs and other critical locations in the sewer network. Using RT-qPCR and genome sequencing, viral RNA fragments can be quantified, and correlated with the population served by the WWTP to estimate the number of infected persons. And based on this, effective response measures like lockdown and increased surveillance can be implemented. If no viral strains are detected, the WBE can be administered routinely. It will help to curb the current pandemic and its second wave or a new viral outbreak in the future.
WBE is dependent on various natural and anthropogenic factors like ambient temperature, precipitation, water supply and sewerage network. Its application in developing countries will be difficult due poor sewerage network and adverse climatic conditions for the virus. However, studies from India (Kumar et al., 2020; Arora et al., 2020), Pakistan (Sharif et al., 2020) and Brazil (Fongaro et al., 2020) indicate that it can be implemented, albeit with greater challenges. Also, SARS-CoV-2 viral genome was detected in wastewater at ambient temperature as high as 40–50 °C (Arora et al., 2020), thus making a compelling case for worldwide implementation of WBE.
2.2.4. Wastewater sector: future challenges
Wastewater is a complex matrix having many DNA/RNA fragments and other impurities. Thus, concentrating a sample and detecting a specific strain of the virus is difficult. Though WBE prevents individual stigmatization, it can lead to collective stigmatization. For example, wastewater surveillance studies suggest that if viral load is detected at the WWTP influent, then sampling should be done at major sewer interceptors to identify the exact location(s) of the outbreak. It will lead to community-based stigmatization. Predicting the number of infected persons based on viral load in the wastewater is difficult. The viral shedding in the human excretion products varies among the individuals and as well also during infection in a single individual.
Sewage temperature and flow rate can influence viral concentration. Thus, data has to be normalized for spatial-temporal comparison and predicting infected persons. Poor sanitation infrastructure presents its challenges. No standard protocol is available to conduct wastewater based epidemiology research. More studies and data are necessary for the occurrence and persistence of SARS-CoV-2 in the wastewater system to understand the transmission pathways of the virus thoroughly. It could help to take essential risk prevention measures to protect public health. The research also required potential aerosol spread of COVID-19 considering the trends of previous outbreaks (Nghiem et al., 2020b). Wastewater surveillance needs to be further investigated concerning direct public health response, mainly where clinical testing is limited (Randazzo et al., 2020a).
2.3. Solid and hazardous waste management under COVID-19 epidemic
About 7.6 billion population of the world produce about 2.01 billion of tonnes of municipal solid waste (MSW) per year, of which, 33% is not managed in an environmentally safer manner (Kaza et al., 2018). Solid hazardous waste particularly generated from households, community centres, hospitals, treatment facilities and, other industrial operations (pharmaceutical manufacturing units, chemical industry, medical incinerations, packing industries) has been increased substantially after the outbreak of COVID-19 (ISWA , 2020). Sudden rise in medical waste generation worldwide has put extra pressure on its safe storage and further treatment as waste operators were not ready for this alarming episode.
2.3.1. Municipal solid waste management: some key issues
Household waste is an important part of MSW and it contributes about 40–60% of the total waste generated in urban settlements in the developing countries. More than 6 billion population started to bear mask under this pandemic attack but safe disposal of used masks at the household level is poorly disposed especially in Asia, Africa, and Latin American countries where enforcement of SWM rules and public participation in sanitation practices is not adequate (UNEP, 2020a). The millions of tons used masks, produced by households every day, is being disposed with MSW in developing states (Nzediegwu and Chang, 2020). The lockdown and work from the stay-at-home policy have risen the organic waste quantity substantially in MSW stream, which requires immediate disposals to avoid onsite decay of it. The limited transportation due to social distancing issues, led to piling up of MSW in urban areas in illegal dump sites. The volume of paper and plastic waste in MSW stream has risen suddenly due to excess purchasing of food and retailer items during this lockdown period and that possibly would cause extra burden on recycling practicesin urban centres. The organic waste content also increased enormously in MSW due to halted transportation, cuts in agriculture goods transports and exports, and excess storage of food items by consumers. The high organic load in MSW and its further disposal at landfill sites would substantially increase greenhouse gases (GHGs) emission worldwide. Single use plastic in MSW has been increased recently due to health concerns and that will impact existing schemes and programs started to reduce the volume of plastic reaching to oceans.
2.3.2. Biomedical waste generation and management
Unprepared urban managers are facing a major challenge of biomedical waste management that has been increased enormously during this COVID-19 pandemic. Used personal protective equipment (PPE) and other biomedical waste articles (googles, plastic coverall, hazmat suits, surgical items, N95 masks, shoe-caps, head covers, nitrile gloves, splash-proof apron, non-plastic and plastic coverall, etc.), generated from quarantine centres, hospitals, and diagnostic labs, have increased 5–6 times than pre-Covid-19 period. A report published in South China Monitoring Post revealed that more than 240 tonnes of biomedical waste was produced daily during the peak of the COVID-19 outbreak in 20 cities across the mainland of China, about 6-times higher before the epidemic occurred (SCMP, 2020), has been and to manage this the biomedical waste treatment facility was upgraded from 50 tonnes per day to 263 tonnes per day this pandemic period. The medical institutions in the US produces about 5 million tonnes biomedical wastes per year but under COVID-19 outbreak, the medical waste quantity would be about 2.5 million tonnes per month, about 6-times higher than the annual generation rate Cutler (2020), India with 4.1 million corona cases (15.58% of the global number) in 1.37 billion population showing relatively low infection rate as compared to other highly populated countries in the world due to proactive measures taken by the governments. But inadequate facilities, for example, 198 common bio-medical waste treatment facilities (CBMWTFs) and 225 incinerations units for 1.37 billion population indicate the inadequacy to hand biomedical waste generated during this epidemic outbreak. Data of national pollution control agency (Central Pollution Control Board, CPCB) revealed that during 2017 only 78% of the total biomedical waste generated was treated at CBMWTFs and rest was buried at landfill sites or disposed to unknown places. According to a post published by SUEZ, an international firm associated with medical waste incineration business, indicates that biomedical waste being treated has risen by 50% and 40% in France, and Netherlands during this COVID-19 pandemic (SUEZ, 2020). The COVID-19 pandemic affected the waste management industry drastically in terms of capital investment, working forces, and circular economy breakdowns.
2.3.3. COVID-19 pandemic stalls the waste recycling industry
Reuse and recycling practices have been recommended as key initiatives for solid waste management programme worldwide to reduce the volume of waste reaching to landfill sites and to increase the life of natural resource under sustainable development programmes. Global recycling market valued about 265 billion US dollars in 2017 and that is expected to increase by 377 billion US dollars in the year 2024 (EPA, 2017). MSW contains several articles (plastic, polythene, newspaper, cardboard, glass, rubber, e-waste, metal, textiles, etc.), which are recycled by informal sectors particularly in developing countries for livelihood earning (Suthar et al., 2016) and by formal sectors in developed countries as state policies of natural resource conservation. A study by Kaza et al. (2018) found that globally MSW contains about 42% recyclable fractions (17%, paper and cardboard; plastic, 12%; wood, 5%; metal, 4%; rubber, 2%; glass, 2%), which can be used efficiently as secondry source of raw materials for remanufacturing in industrial sector. Now plastic trading has become a global business and China alone receives 56% (by weight) of the global imported waste plastic. Entirely Europe recycles about 46% of its waste and that contains about 12% plastic (3.4 Mt) (Velis, 2014). Plastic bottles (PET) gained much attention in the recycling business due to their high recycling values and therefore; some countries like Germany alone recycles > 97% of total PET plastic produced while the US just 29.9% (EPA, 2017). But due to strict regulation on the use of recycled plastic and halted segregation process (formal and informal), during this COVID-19 epidemic, has badly impacted plastic recycling operations worldwide. The limited operation, low collection rates, social distancing, comparatively high cost of recycled plastic than virgin plastic, etc. have been appeared as key drivers of financial distress in recycling industries worldwide. At this crucial time when the world is struggling to make plastic-free oceans, the single-use plastic quantity would be the biggest rollback for hard-won environmental commitments to reduce ocean plastic pollution (Tenenbaum, 2020).
Rag pickers, which are considered as major drivers of circular economy business in developing countries, are at major risks due to loss of business and livelihood under this COVID-19 lockdown. In India, 1.5–4.0 million rag pickers are under extreme social pressure due to limited excess to waste disposal points and their illegal waste picking practices could be a possible cause of wide speared of COVID-19 pandemic in slum areas through a chain of contaminations (Fig. 6 ). Waste articles also carry the active stain of SARS-CoV-2 as found in recent scientific investigations. A recent report by The New England Journal of Medicine revealed that SARS- SARS-CoV-2 could survive more than 72 h on the surface of the plastic and stainless and other solid surfaces (paper, cardboard, copper, etc.) (Fig. 2) also showed survival of SARS-CoV-2 for a significant period, efficient to cause new infections (van Doremalen et al., 2020). Another study by Casanova et al. (2010) found that virus can survive on steel surface for 28 d at 4 °C and its further survival depends on relative humidity and temperature in the surrounding environment. Further studies are required to see the possible role of ambient environmental conditions on survival and transmission of SARS-CoV-2 through waste handling processes. The survival of SARS-CoV-2 on some recyclable waste articles could be a health risk for waste pickers, households, waste managers who are involved in segregation, transportation and waste (recyclable) trading. Although, Government institutions, NGOs, and other agencies are providing safety equipment to such workforces that are again limited to some restricted sites.
Fig. 6.
MSW collection in urban areas of developing countries and its possible role in COVID-19 dispersal.
2.3.4. Upgradation in MSW management policy to address issues in COVID-19 pandemic
After COVID-19 episode, the national and international agencies are working on a framework of new guidelines and policies to handle the household and biomedical waste generated from different sectors of the society. WHO issued a notification on water, sanitation and waste management with major emphasis on proper using of PPE during waste handling, transportation and management operations. Few international initiatives are described as follow: (i) WHO: Waste should be stored offsite in safe bags and could be disinfected by appropriate modes like a 10% lime slurry. Biomedical waste should be treated (autoclaving and high-temperature incineration), preferably onsite, then disposed of safely (WHO, 2020c); (ii) United Nations Environmental Programme (UNEP): Household waste, which may contain PPE mixed with other household garbage, should be treated as hazardous waste and PPE should be separated and treated as the guideline of the Basel Convention. The recent draft indicates that ‘other wastes’ could be included as a separate category where contaminated household waste and incineration ash can be included (UNEP, 2020); (iii) European Union (EU) member states urged to follow the directives issued by European Centre for Diseases Prevention and Control (ECDC) about the solid waste generated from household, hospitals, and public ventures, which mainly comply with the recommendation made by WHO and Basel recommendations. Recycling of waste is an important part of the European waste management system therefore, the separate collection is recommended to ensure the safety of workers at recycling centres and product quality as per standards (EC, 2020).
Some severely affected Asian countries like China and India has issued some new direction in their existing waste management legal frameworks. For example, China issued a new guideline to manage solid waste particularly biomedical wastes. Department of Ecology and Environment of provinces, autonomous regions, and municipalities are empowered to ensure the proper collection, transportation and management of biomedical wastes. The areas those are not having centralized disposal facilities could have in-situ waste treatment facilities mainly provided with mobile incinerators. CBCB, India has issued a notification in addition to existing Biomedical Waste Management Rule 2016 for quarantine camps, households, healthcare facilities, testing centres, and waste collection points. New direction suggested: quarantine wards would collect waste in two double-layered bags (yellow colour) separately from household waste items; such waste would be handed over to the authorized waste staff of CBWTF; the inner and outer surface of temporary waste collecting bins and containers should be sanitized 1% sodium hypochlorite solutions; the dedicated vehicle for waste collection from infected areas; record and hygiene maintenance by waste workers.
2.4. Socio-economic perspectives of COVID-19 pandemic: some recent observations
2.4.1. Impact of the global economy, livelihood and health costs
The impact of COVID-19 has spread all over the globe and has impacted around 5.61 million people across the globe. As per an estimation by the Asian Development Bank (ADB) the economic impact of COVID-19 would be around 5.8 to 8.8 trillion UD $ (6.4–9.7% of the global GDP), excluding the impact of policy measures (ADB, 2020). The adverse health burden leads to a severe economic crisis and recession. Social distancing, lockdown had impacted the workforce and job cuts. ADB (2020) have predicted that there will be a drop in employment in Asia of an amount of 109 million-167 million jobs. It had adversely impacted the vulnerable section of the community. As per World Bank, “The COVID-19 recession has seen the fastest, steepest downgrades in consensus growth projections among all global recessions since 1990” (World Bank, 2020). ADB (2020) have predicted that there will be a drop in employment in Asia of an amount of 109–167 million jobs. It had adversely impacted the vulnerable section of the community. A recent report by International Labour Organization (ILO) estimated (as of April 22, 2020), that would be a significant impact on 1.6 billion informal sector workers accounting around 76% of informal employment (ILO, 2020). Their estimates suggest that the income losses associated with them will be enormous (around 82% in lower-middle and low-income countries and 76% in high-income countries). Countries predominantly relying on the service sector, higher levels of informality and fragile safeguards against the termination of employment experienced higher job losses (ILO, 2020).
Developed and developing economies addressing the extra health burden arising from COVID-19. Health-related interventions have been estimated to be 82 to 115 billion US $ for Asia specific (ADB, 2020). A recent study by Roberton et al. (2020) quantified the impact of the COVID-19 pandemic and control efforts on reproductive, maternal, new-born, and child health in 118 low-income and middle-income countries (LMICs) using the Lives Saved Tool and concluded that a significant increase in maternal and child death would occur during this pandemic. Another study by McCartney et al. (2020), in the context of the UK, estimated that fully mitigating COVID 19 can prevent a loss of 5.63 years of life expectancy of its citizens.
India is amongst the fourth-worst hit nation by the COVID-19 pandemic after the US, Brazil, and Russia (https://www.worldometers.info/coronavirus/). As per Ministry of Health and Family Welfare (MHFW), India, 10 per cent of India's population are accountable for 50% of India's COVID-19 linked deaths while 73% of COVID-19 deaths are due to co-morbidities. To perceive the demographic characteristics of the COVID-19 affected population, we attempted to group the COVID-19 cases using K-means based on their age, gender, and several active cases using Python 2.7.16 (Fig. 7 ). Five datasets have been merged starting from January 30, 2020 to May 26, 2020 have been taken from COVID-19-India Association of Physicians (API, 2020). Prevalence of infection was observed in most of the adult population both for males and females from around 30 years. A cross-validation of the exercise was also conducted with STATA 14. It was observed that 76% of the COVID-19 infected people belong to the age category of 26–44 years while 8.5% belong to the age category >60 years. Predominantly most of the COVID-19 affected population are males (around 27%) compared to females (14%). 59% of the gender remain unassigned in the COVID-19 data (Table S2, S3, Supplementary section).
Fig. 7.
Pseudo 3D plot.
These observations are in line with recorded calculations by Raifmann et al. (2020) who observed 43% of adults were at higher risk to SARS-CoV-2 infections. Also, the study concluded that low-income households are at higher risk of SARS-CoV-2 infections as compared to high-income households. Similarly, Ray et al. (2020) have also identified the vulnerable subgroups who are at potentially high risk of COVID-19 in the context of India. Uninsured, adult population with diabetes, the proportion of the population has the provision of access to inpatient and outpatient facilities in hospitals are being categorised as some who are at high risk.
The impact of the COVID-19 pandemic also had an impact on the environment. The urban air quality significantly improved due to no vehicular emission as well as other closure of coal-based thermal power plants. Helm (2020) concluded that the intergenerational equity will be worse where the future generations will be overburdened with- ‘appreciable debt to support consumption levels now over national incomes. The debt associated with new fiscal stimuli to address the negative economic consequences of the current pandemic; specific debt to fund investments designed to reduce future pollution’.
2.4.2. Policy implications and future challenges
The combined impact of health and economic crisis had a serious threat to economies and human lives and have triggered rapid and remarkable policy action around the world (IMF, 2020). The COVID-19 pandemic had further aggravated the health and social inequality prevailing in the developing countries. Also, social distancing has impacted the economy, incomes, employment, social isolation, physical activity and isolation (McCartney et al., 2020). A pro-active government intervention should aim in reducing income and wealth inequalities and providing a safety net for the poor. Shang et al. [114] have emphasized on strengthening the existing social protection programmes by expanding the coverage and increasing the benefits. Liquidity support in the form of direct lending, loan guarantees, capital injection and deferral of utility and rent payments can be facilitated. The post-COVID-19 pandemic period should focus on rebuilding the society and the economy with local employment generation for the low-income categories, better health infrastructure, provision of coverage of health insurance. Countries with an effective poverty –oriented programme and fiscal space, universal (or near-universal) benefits can utilize it to enhance income support for households beyond the vulnerable and stimulate aggregate demand (Shang et al., 2020a, 2020b). As put forward by Ray et al. (2020) to deal with the crisis it requires a strong integration of the government, scientific community, health care professionals and the global community. Policy responses targeting the impact on the environment due to COVID-19 crisis as suggested by IMF (2020) may involve facilitating public green investment projects, introducing a carbon tax, green financing, financial support from the high-income countries to the vulnerable ones which can assist them in cutting their emission level and recharge their disaster funds which have been already utilized to deal with COVID-19 pandemic.
3. Conclusion and future perspectives
The preventive measures adopted so far to contain the spread of SARS-CoV-2 have been the three-pronged mechanism involving (i) an early detection and isolation, (ii) contact tracing, and (iii) appropriate use of personal protective equipment (PPE). Pandemics like COVID-19 have to be tackled as a socio-economic initiative comprising proper sanitation measures, maintenance of health and personal hygiene, prioritizing clean air, water, and soil environments. The improvement in outdoor air quality has been reported due to the COVID-19 lockdown. On the other hand, longer exposure to indoor air pollution will increase the chances of COVID-19 mortalities. The data of past studies and COVID-19 air quality would help identify the pollution causing sources that require attention but were not accounted for earlier. Using the wastewater surveillance tool to confirm the spread of the virus in the communities required more water samplings and testing data. Wastewater surveillance could gauge the success of precautionary measures, including lockdowns and social distancing, as timely analysis can decrease the contagion's magnitude. The survival of CoV-2 on some recyclable waste articles could be a health risk for waste pickers, households, and waste managers involved in segregation, transportation, and waste (recyclable) trading. Social protection to the vulnerable communities can be enhanced by widening the coverage and benefits of the existing programs and implementing new schemes. Cash transfers to the targeted groups can be facilitated who have been adversely affected by the pandemic. Countries like India have witnessed reverse migration and public works, and green jobs can be an alternative source of employment.
Author’s contribution
Surinder Suthar: COVID-19 pandemic and global air quality: Some good news and some bad news, Solid and hazardous waste management under COVID-19 epidemic. Sukanya Das: Socio-economic perspectives of COVID-19 pandemic: Some recent observations. Ajay Nagpure: COVID-19 pandemic and global air quality: Some good news and some bad news. Chaithanya Madhurantakam: COVID-19: Epidemiology and pathogenesis. Satya Brat Tiwari: Wastewater and COVID-19 epidemic. Pallavi Gahlot: Wastewater and COVID-19 epidemic. Vinay Kumar Tyagi: Wastewater and COVID-19 epidemic
Declaration of competing interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Acknowledgements
Authors are thankful to Department of Biotechnology -GoI (GrantNo. BT/RLF/Re-entry/12/2016) for financial support to this research. The author would like to thank Dr Nilotpal Ghosh for analysis involved in figures used in Socio-economic section.
Footnotes
Supplementary data to this article can be found online at https://doi.org/10.1016/j.jenvman.2020.111700.
Appendix A. Supplementary data
The following is the Supplementary data to this article:
References
- ADB . ADB briefs; 2020. An Updated Assessment of the Economic Impact of COVID-19. No 133. [DOI] [Google Scholar]
- Adhikari S.P., Meng S., Wu Y.J., Mao Y.P., Ye R.X., Wang Q.Z., Sun C.S. Epidemiology, causes, clinical manifestation and diagnosis, prevention, and control of coronavirus disease (COVID-19) during the early outbreak period: a scoping review. Infect Dis Poverty. 2020;9(29) doi: 10.1186/s40249-020-00646-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ahmed W., Angel M., Edson J., Bibby K., Bivins A. First confirmed detection of SARS-CoV-2 in untreated wastewater in Australia: a proof of concept for the wastewater surveillance of COVID-19 in the community. Sci. Total Environ. 2020;728:138764. doi: 10.1016/j.scitotenv.2020.138764. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Alagaili A.N., Briese T., Mishra N., Kapoor V., Sameroff S.C. Middle East respiratory syndrome coronavirus infection in dromedary camels in Saudi Arabia. mBio. 2014;5(2) doi: 10.1128/mBio.00884-14. e00884-14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Anand S., Hanson K. DALYs: efficiency versus equity. World Dev. 1998;26(2):307–310. [Google Scholar]
- API 2020. https://api.covid19india.org/csv/ Accessed on 28th May 2020.
- Arora S., Nag A., Sethi J., Rajvanshi J., Saxena S., Shrivastava S.K., Gupta A.B. 2020. Sewage Surveillance for the Presence of SARS-CoV-2 Genome as a Useful Wastewater Based Epidemiology (WBE) Tracking Tool in India. medRxiv. [DOI] [PubMed] [Google Scholar]
- Balakrishnan K., Dey S., Gupta T., Dhaliwal R.S., Brauer M., Cohen A.J. The impact of air pollution on deaths, disease burden, and life expectancy across the states of India: the Global Burden of Disease Study 2017. Lancet Planet Health. 2019;3:e26–39. doi: 10.1016/S2542-5196(18)30261-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bauwens M., Compernolle S., Stavrakou T., Müller J.F., van Gent J. Impact of coronavirus outbreak on NO2 pollution assessed using TROPOMI and OMI observations. Geophys. Res. Lett. 2020 doi: 10.1029/2020GL087978. https://10.1029/2020GL087978 e2020GL087978. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cai X.F., Chen J., Hu J.L., Long Q.X., Deng H.J. 2020. A Peptide-Based Magnetic Chemiluminescence Enzyme Immunoassay for Serological Diagnosis of Corona Virus Disease 2019 (COVID-19)https://10.1101/2020.02.22.20026617 medRxiv. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Casanova L.M., William S.J., David A.R., Weber J., Sobsey M.D. Effects of air temperature and relative humidity on coronavirus survival on surfaces. Appl. Environ. Microbiol. 2010;76:2712–2717. doi: 10.1128/AEM.02291-09. [DOI] [PMC free article] [PubMed] [Google Scholar]
- CDC . U.S. Centre for Disease Control and Prevention; Atlanta, GA: 2019. Middle East Respiratory Syndrome. 2 August 2019. National Center for Immunization and Respiratory Diseases (NCIRD), Division of Viral Diseases.https://www.cdc.gov/coronavirus/mers/clinical-features.html [Google Scholar]
- CDC . Division of Viral Diseases, U.S. Centers for Disease Control and Prevention; Atlanta, GA: 2019. Novel Coronavirus (2019-nCoV) Real-Time RT-PCR Diagnostic Panel. 2020. [Google Scholar]
- CDC . U.S. Centers for Disease Control and Prevention; Atlanta, GA: 2020. U.S. Centres for Disease Control and Prevention, U.S. Department of Health & Human Services: Coronavirus (COVID-19)https://www.cdc.gov/coronavirus/2019-ncov/ [Google Scholar]
- Chen K., Wang M., Huang C., Kinney P.L., Anastas P.T. Air pollution reduction and mortality benefit during the COVID-19 outbreak in China. The Lancet Planetar. Healt. 2020;4(6):E210–E212. doi: 10.1016/S2542-5196(20)30107-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Chen Y., Liu Q., Guo D. Emerging coronaviruses: genome structure, replication, and pathogenesis. J. Med. Virol. 2020;92(4):418‐423. doi: 10.1002/jmv.25681. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Choi S., Jung E., Choi B.Y., Hur Y.J., Ki M. High reproduction number of Middle East respiratory syndrome coronavirus in nosocomial outbreaks: mathematical modelling in Saudi Arabia and South Korea. J. Hosp. Infect. 2018;99(2):162‐168. doi: 10.1016/j.jhin.2017.09.017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Chowell G., Castillo-Chavez C., Fenimore P.W., Kribs-Zaleta C.M., Arriola L., Hyman J.M. Model parameters and outbreak control for SARS. Emerg. Infect. Dis. 2004;10(7):1258‐1263. doi: 10.3201/eid1007.030647. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Corman V.M., Landt O., Kaiser M., Molenkamp R., Meijer A., Chu D.K., Bleicker T., Brünink S. Detection of 2019 novel coronavirus (2019-nCoV) by real-time RT-PCR. Euro Surveill. 2020;25(3):2000045. doi: 10.2807/1560-7917.ES.2020.25.3.2000045. [DOI] [PMC free article] [PubMed] [Google Scholar]
- COVID-19 . 2020. Coronavirus Disease Pandemic.https://www.worldometers.info/coronavirus/ [Google Scholar]
- Cpcb . Central Pollution Control Board (CPCB); New Delhi, India: 2020. Impact of Janta Curfew and Lockdown on Air Quality.https://www.cpcb.nic.in/ Report publication date: 31st march, 2020. [Google Scholar]
- Cucinotta D., Vanelli M. WHO declares COVID-19 a pandemic. Acta Biomed. 2020;1:157‐160. doi: 10.23750/abm.v91i1.9397. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cui Y., Zhang Z.F., Froines J., Zhao J., Wang H., Yu S.Z., Detels R. Air pollution and case fatality of SARS in the People's Republic of China: an ecologic study. Environ. Health. 2003;2(1):15. doi: 10.1186/1476-069X-2-15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cutler S. 2020. Mounting Medical Waste from COVID-19 Emphasizes the Need for a Sustainable Waste Management Strategy.https://ww2.frost.com/frost-perspectives/managing-the-growing-threat-of-covid-19-generated-medical-waste/ [Google Scholar]
- Demarest S.J., Glaser S.M. Antibody therapeutics, antibody engineering, and the merits of protein stability. Curr. Opin. Drug Discov. Dev. 2008;11(5):675‐687. [PubMed] [Google Scholar]
- Du Toit A. Outbreak of a novel coronavirus. Nat. Rev. Microbiol. 2020;18(3):123. doi: 10.1038/s41579-020-0332-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- EPA . United States Environmental Protection Agency; 2017. Facts and Figures about Materials, Waste and Recycling. Plastics: Material-specific Data.https://www.epa.gov/facts-and-figures-about-materials-waste-and-recycling/plastics-material-specific-data [Google Scholar]
- ESA European space agency. 2020. https://www.esa.int/Applications/Observing_the_Earth/Copernicus/Sentinel-5P
- European Commission . 2020. Waste Management in the Context of the Coronavirus Crisis.https://ec.europa.eu/info/sites/info/files/waste_management_guidance_dg-env.pdf 14 April 2020. [Google Scholar]
- Fongaro G., Stoco P.H., Souza D.S.M., Grisard E.C., Magri M.E., Rogovski P. 2020. SARS-CoV-2 in Human Sewage in Santa Catalina, Brazil, November 2019. medRxiv. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gao M., Yang L., Chen X., Deng Y., Yang S., Xu H., Chen Z., Gao X. A study on infectivity of asymptomatic SARS-CoV-2 carriers. Respir. Med. 2020;169:106026. doi: 10.1016/j.rmed.2020.106026. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gormley M., Aspray T.J., Kelly D.A. COVID-19: mitigating transmission via wastewater plumbing systems. Lancet. 2020;8:643. doi: 10.1016/S2214-109X(20)30112-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Graham D. 2020. Sewage Monitoring Could Provide an Early Warning of COVID-19 Outbreaks.https://www.ncl.ac.uk/press/articles/latest/2020/04/covid19sewage/ [Google Scholar]
- Haas C.N., Rose J.B., Gerba C.P. John Wiley & Sons. United States of America; 1999. Quantitative Microbial Risk Assessment. [Google Scholar]
- Hanke L., Perez L.V., Sheward D.J., Das H., Schultz T. 2020. An Alpaca Nanobody Neutralizes SARS-CoV-2 by Blocking Receptor Interaction. bioRxiv 2020.06.02.130161. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hart O.E., Halden R.U. Computational analysis of SARS-CoV-2/COVID-19 surveillance by wastewater-based epidemiology locally and globally: feasibility, economy, opportunities and challenges. Sci. Total Environ. 2020;730:138875. doi: 10.1016/j.scitotenv.2020.138875. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Helm D. The environmental impacts of the coronavirus. Environ. Resour. Econ. 2020;1(May 7):1–18. doi: 10.1007/s10640-020-00426-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hemida M.G., Chu D.K., Poon L.L., Perera R.A., Alhammadi M.A., Ng H.Y. MERS coronavirus in dromedary camel herd, Saudi Arabia. Emerg. Infect. Dis. 2014;20(7):1231‐1234. doi: 10.3201/eid2007.140571. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hoffmann M., Kleine-Weber H., Schroeder S., Krüger N., Herrler T. SARS-CoV-2 cell entry depends on ACE2 and TMPRSS2 and is blocked by a clinically proven protease inhibitor. Cell. 2020;181(2):271–280. doi: 10.1016/j.cell.2020.02.052. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hou T., Zeng W., Yang M., Chen W., Ren L. 2020. Development and Evaluation of A CRISPR-Based Diagnostic for 2019-Novel Coronavirus. medRxiv. [DOI] [Google Scholar]
- ILO 2020. https://www.ilo.org/wcmsp5/groups/public/---dgreports/---dcomm/documents/briefingnote/wcms_743146.pdf
- IMF (International Monetary Fund) 2020. Greening the Recovery, Special Series on Fiscal Policies to Respond to COVID-19.https://www.imf.org/en/Publications/SPROLLs/covid19-special-notes April 20. [Google Scholar]
- IQAir . 2020. COVID-19 Air Quality Report.https://www2.iqair.com/ Publication date: Apr. 22, 2020. [Google Scholar]
- ISWA (International Solid Waste Association) 2020. Waste Management during the COVID-19 Pandemic ISWA's Recommendations.https://www.iswa.org/fileadmin/galleries/0001_COVID/ISWA_Waste_Management_During_COVID-19.pdf [Google Scholar]
- Ithete N.L., Stoffberg S., Corman V.M., Cottontail V.M., Richards L.R. Close relative of human Middle East respiratory syndrome coronavirus in bat, South Africa. Emerg. Infect. Dis. 2013;19(10):1697‐1699. doi: 10.3201/eid1910.130946. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jaimes J.A., André N.M., Chappie J.S., Millet J.K., Whittaker G.R. Phylogenetic analysis and structural modeling of SARS-CoV-2 spike protein reveals an evolutionary distinct and proteolytically sensitive activation loop. J. Mol. Biol. 2020;432(10) doi: 10.1016/j.jmb.2020.04.009. (2020) 3309‐3325. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kaza S., Yao L., Bhada-Tata P., Van Woerden F., Ionkova K., Morton J., Poveda R.A., Sarraf M., Malkawi F., Harinath A.S., Banna F., An G., Imoto H., Levine D. International Bank for Reconstruction and Development/The World Bank 1818 H Street NW; Washington, DC 20433: 2018. What a Waste 2.0: A Global Snapshot of Solid Waste Management to 2050. [Google Scholar]
- Kitajima M., Ahmed W., Bibby K., Carducci A., Gerba C.P., Hamilton K.A., Haramoto E., Rose J.B. SARS-CoV-2 in wastewater: state of the knowledge and research needs. Sci. Total Environ. 2020;739:139076. doi: 10.1016/j.scitotenv.2020.139076. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kocamemi B.A., Kurt H., Sait A., Sarac F., Saatci A.M., Pakdemirli B. 2020. SARS-CoV-2 Detection in Istanbul Wastewater Treatment Plant Sludges. medRxiv. [DOI] [Google Scholar]
- Kocamemi B.A., Kurt H., Hacioglu S., Yarali C., Saatci A.M., Pakdemirli B. 2020. First Data-Set on SARS-CoV-2 Detection for Istanbul Wastewaters in Turkey. medRxiv. [DOI] [Google Scholar]
- Kumar M., Patel A.K., Shah A.V., Raval J., Rajpara N., Joshi M., Joshi C.G. First proof of the capability of wastewater surveillance for COVID-19 in India through detection of genetic material of SARS-CoV-2. Sci. Total Environ. 2020:141326. doi: 10.1016/j.scitotenv.2020.141326. [DOI] [PMC free article] [PubMed] [Google Scholar]
- La Rosa G., Iaconelli M., Mancini P., Ferraro G.B., Veneri C., Bonadonna L., Lucentini L. 2020. First Detection of SARS-COV-2 in Untreated Wastewaters in Italy. medRxiv. [DOI] [PMC free article] [PubMed] [Google Scholar]
- La Rosa G., Bonadonna L., Lucentini L., Kenmoe S., Suffredini E. Coronavirus in water environments: occurrence, persistence and concentration methods - a scoping review. Water Res. 2020;179:115899. doi: 10.1016/j.watres.2020.115899. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lam T.T., Jia N., Zhang Y.W., Shum M.H., Jiang J.F. Identifying SARS-CoV-2 related coronaviruses in Malayan pangolins. Nature. 2020 doi: 10.1038/s41586-020-2169-0. [DOI] [PubMed] [Google Scholar]
- Li W., Moore M.J., Vasilieva N., Sui J., Wong S.K. Farzan, Angiotensin-converting enzyme 2 is a functional receptor for the SARS coronavirus. Nature. 2003;426(6965):450‐454. doi: 10.1038/nature02145. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Li Q., Guan X., Wu P., Wang X., Zhou L. Early transmission dynamics in wuhan, China, of novel coronavirus-infected pneumonia. N. Engl. J. Med. 2020;382(13):1199–1207. doi: 10.1056/NEJMoa2001316. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Li S.R., Tang Z.J., Li Z.H., Liu X. Searching therapeutic strategy of new coronavirus pneumonia from angiotensin-converting enzyme 2: the target of COVID-19 and SARS-CoV. Eur. J. Clin. Microbiol. Infect. Dis. 2020;39(6):1021‐1026. doi: 10.1007/s10096-020-03883-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lim S.S., Vos T., Flaxman A.D., Danaei G., Shibuya K. A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012;380(9859):2224–2260. doi: 10.1016/S0140-6736(12)61766-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Liu S., Xiao G., Chen Y., He Y., Niu J. Interaction between heptad repeat 1 and 2 regions in spike protein of SARS-associated coronavirus: implications for virus fusogenic mechanism and identification of fusion inhibitors. Lancet. 2004;363(9413):938‐947. doi: 10.1016/S0140-6736(04)15788-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lodder W., de Roda Husman A.M. SARS-CoV-2 in wastewater: potential health risk, but also data source. Lancet Gastroenterol Hepatol. 2020;5(6):533–534. doi: 10.1016/S2468-1253(20)30087-X. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Main D. 2014. Real-Time Wastewater Analysis Shows what Drugs Are Being Used where.https://www.popsci.com/article/science/real-time-wastewater-analysis-shows-what-drugs-are-being-used-where/ (accesses in June 1, 2020) [Google Scholar]
- Mallapaty S. How sewage could reveal true scale of coronavirus outbreak. Nature. 2020;580:176–177. doi: 10.1038/d41586-020-00973-x. [DOI] [PubMed] [Google Scholar]
- Mao K., Zhang H., Yang Z. Can a paper-based device trace COVID-19 sources with wastewater-based epidemiology? Environ. Sci. Technol. 2020;54(7):3733–3735. doi: 10.1021/acs.est.0c01174. [DOI] [PubMed] [Google Scholar]
- Martina B.E., Haagmans B.L., Kuiken T., Fouchier R.A., Rimmelzwaan G.F. Virology: SARS virus infection of cats and ferrets. Nature. 2003;425(6961):915. doi: 10.1038/425915a. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McCartney G., Leyland A., Walsh D., Dundas R. Scaling COVID-19 against inequalities: should the policy response consistently match the mortality challenge? medRxiv. 2020. [DOI] [PMC free article] [PubMed]
- Medema G., Heijnen L., Elsinga G., Italiaander R., Brouwer A. Presence of SARS-Coronavirus-2 in sewage. MedRxiv. 2020 doi: 10.1101/2020.03.29.20045880. [DOI] [PubMed] [Google Scholar]
- Mizumoto K., Kagaya K., Zarebski A., Chowell G. Estimating the asymptomatic proportion of coronavirus disease 2019 (COVID-19) cases on board the Diamond Princess cruise ship, Yokohama, Japan, 2020. Euro Surveill. 2020;25(10):2000180. doi: 10.2807/1560-7917.ES.2020.25.10.2000180. [DOI] [PMC free article] [PubMed] [Google Scholar]
- NASA . 2020. Global Nitrogen Dioxide Monitoring News.https://so2.gsfc.nasa.go 15th July 2020. [Google Scholar]
- NASA 2020. https://earthobservatory.nasa.gov/images 15th July 2020.
- NCIRD . U.S. Department of Health & Human Services; 2017. National Centre for Immunization and Respiratory Diseases, Division of Viral Diseases.https://www.cdc.gov/sars/about/fs-sars.html Severe Acute Respiratory syndrome (SARS). (6th December 2017) [Google Scholar]
- Nemudryi A., Nemudraia A., Surya K., Wiegand T., Buyukyoruk M., Wilkinson R., Wiedenheft B. 2020. Temporal Detection and Phylogenetic Assessment of SARS-CoV-2 in Municipal Wastewater. medRxiv. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Nghiem L.D., Morgan B., Donner E., Short M.D. The COVID-19 pandemic: considerations for the waste and wastewater services sector. Case Stu. Chem. Environ. Eng. 2020;1:100006. doi: 10.1016/j.cscee.2020.100006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Nghiem L.D., Morgan B., Donner E., Short M.D. The COVID-19 pandemic: considerations for the waste and wastewater services sector. Case Stud. Chem. Environ. Eng. 2020;1:100006. doi: 10.1016/j.cscee.2020.100006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Nzediegwu C., Chang S.X. Improper solid waste management increases potential for COVID-19 spread in developing countries. Resour. Conserv. Recycl. 2020;161:104947. doi: 10.1016/j.resconrec.2020.104947. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Or I.B., Yaniv K., Shagan M., Ozer E., Erster O., Mendelson E., Mannasse B., Shirazi R., Kramarsky-Winter E., Nir O., Abu-Ali H. 2020. Regressing SARS-CoV-2 Sewage Measurements onto COVID-19 Burden in the Population: a Proof-Of-Concept for Quantitative Environmental Surveillance. medRxiv. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Raifman M., Raifman J. Disparities in the population at risk of severe illness from covid-19 by race/ethnicity and income. Am. J. Prev. Med. 2020;59(10):137–139. doi: 10.1016/j.amepre.2020.04.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Raj V.S., Mou H., Smits S.L., Dekkers D.H., Müller M.A. Dipeptidyl peptidase 4 is a functional receptor for the emerging human coronavirus-EMC. Nature. 2013;495(7440):251‐254. doi: 10.1038/nature12005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Randazzo W., Truchado P., Cuevas-Ferrando E., Simon P., Allende A., Sanchez G. SARS-CoV-2 RNA in wastewater anticipated COVID-19 occurrence in a low prevalence area. Water Res. 2020;181:115942. doi: 10.1016/j.watres.2020.115942. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Randazzo W., Cuevas-Ferrando E., Sanjuan R., Domingo-Calap P., Sanchez G. 2020. Metropolitan Wastewater Analysis for COVID-19 Epidemiological Surveillance. medRxiv. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ray D., Bhattacharyya R., Wang L., Salvatore M., Mohammed S. 2020. Predictions and Role of Interventions for COVID-19 Outbreak in India.https://medium.com/@covind_19/predictions-and-role-of-interventions-for-covid-19-outbreak-in-india-52903e2544e6 (Accessed on 1st June 2020) [DOI] [PMC free article] [PubMed] [Google Scholar]
- Remoundou K., Koundouri P. Environmental effects on public health: an economic perspective. Int. J. Environ. Res. Publ. Health. 2009;6(8):2160–2178. doi: 10.3390/ijerph6082160. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rimoldi S.G., Stefani F., Gigantiello A., Polesello S., Comandatore F. 2020. Presence and Vitality of SARS-CoV-2 Virus in Wastewaters and Rivers. medRxiv. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Riou J., Althaus C.L. Pattern of early human-to-human transmission of Wuhan 2019 novel coronavirus (2019-nCoV), December 2019 to January 2020. Euro Surveill. 2020;25(4):2000058. doi: 10.2807/1560-7917.ES.2020.25.4.2000058. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Roberton T., Carter E.D., Chou V.B., Stegmuller A.R., Jackson B.D., Tam Y., Lewis T.S., Walker N. Early estimates of the indirect effects of the COVID-19 pandemic on maternal and child mortality in low-income and middle-income countries: a modelling study. The Lancet Global Health. 2020;8(7):e901–908. doi: 10.1016/S2214-109X(20)30229-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- SARS . 2020. Severe Acute Respiratory Syndrome (SARS). 1998-2020 Mayo Foundation for Medical Education and Research (MFMER)https://www.mayoclinic.org/diseases-conditions/sars/symptoms-causes/syc-20351765 (Accessed on June 20, 2020) [Google Scholar]
- Schoeman D., Fielding B.C. Coronavirus envelope protein: current knowledge. Virol. J. 2019;16(1):69. doi: 10.1186/s12985-019-1182-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- SCMP . South China Monitoring Post; 2020. Coronavirus Leaves China with Mountains of Medical Waste.https://www.scmp.com/news/china/society/article/3074722/coronavirus-leaves-china-mountains-medical-waste [Google Scholar]
- Setti L., Passarini F., de Gennaro G., Gilio A.D., Palmisani J. 2020. Relazione circa l’effetto dell’inquinamento da particolato atmosferico e la diffusione di virus nella popolazione.http://www.simaonlus.it/wpsima/wp-content/uploads/2020/03/COVID19_Position-Paper_Relazione-circa-l%E2%80%99effetto-dell%E2%80%99inquinamento-da-particolato-atmosferico-e-la-diffusione-di-virus-nella-popolazione.pdf [Google Scholar]
- Shang B., Evans B., An Z. 2020. Expenditure Policies in Support of Firms and Households, IMF Special Series on Fiscal Policies to Respond to COVID-19.https://www.imf.org/en/Publications/SPROLLs/covid19-special-notes April 20. [Google Scholar]
- Shang J., Ye G., Shi K., Wan Y., Luo C. Structural basis of receptor recognition by SARS-CoV-2. Nature. 2020;581(7807):221–224. doi: 10.1038/s41586-020-2179-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sharif S., Ikram A., Khurshid A., Salman M., Mehmood N., Arshad Y., Ahmad J. 2020. Detection of SARS-Coronavirus-2 in Wastewater, Using the Existing Environmental Surveillance Network: an Epidemiological Gateway to an Early Warning for COVID-19 in Communities. medRxiv. [DOI] [Google Scholar]
- Sims N., Hordern B.K. Future perspectives of wastewater-based epidemiology: monitoring infectious disease spread and resistance to the community level. Environ. Int. 2020;139:105689. doi: 10.1016/j.envint.2020.105689. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Steffens I.A. A hundred days into the coronavirus disease (COVID-19) pandemic. Euro Surveill. 2020;25(14):2000550. doi: 10.2807/1560-7917.ES.2020.25.14.2000550. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Steven S., Yen T.L., Chonggang X., Ethan R.S., Nick H., Ruian K. 2020. The Novel Coronavirus, 2019-nCoV, Is Highly Contagious and More Infectious than Initially Estimated. medRxiv, 2020.02.07.20021154. [DOI] [Google Scholar]
- SUEZ . 2020. COVID-19: SUEZ Mobilised to Treat Infectious Biomedical Waste.https://www.suez.com/en/news/covid-19-suez-mobilised-to-treat-infectious-biomedical-waste [Google Scholar]
- Suthar S., Rayal P., Ahada C.P.S. Role of different stakeholders in trading of reusable/recyclable urban solid waste materials: a case study. Sustainab. Cities Societ. 2016;22:104–115. [Google Scholar]
- Tai W., He L., Zhang X., Pu J., Voronin D., Jiang S., Zhou Y., Du L. Characterization of the receptor-binding domain (RBD) of 2019 novel coronavirus: implication for development of RBD protein as a viral attachment inhibitor and vaccine. Cell. Mol. Immunol. 2020;17(6):613‐620. doi: 10.1038/s41423-020-0400-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tenenbaum L. 2020. The Amount of Plastic Waste Is Surging Because of the Coronavirus Pandemic.https://www.forbes.com/sites/lauratenenbaum/2020/04/25/plastic-waste-during-the-time-of-covid-19/ [Google Scholar]
- Udugama B., Kadhiresan P., Kozlowski H.N., Malekjahani A., Osborne M., Li V.Y.C., Chen H., Mubareka S., Chan J.B. Diagnosing COVID-19: the disease and tools for detection. ACS Nano. 2020;14(4):3822–3835. doi: 10.1021/acsnano.0c02624. [DOI] [PubMed] [Google Scholar]
- UNEP . 2020. Waste Management an Essential Public Service in the Fight to Beat COVID-19.https://www.unenvironment.org/news-and-stories/press-release/waste-management-essential-public-service-fight-beat-covid-19 [Google Scholar]
- van Doremalen N., Bushmaker T., Morris D.H., Holbrook M.G., Gamble A. Aerosol and surface stability of SARS-CoV-2 as compared with SARS-CoV-1. N. Engl. J. Med. 2020;382(16):1564‐1567. doi: 10.1056/NEJMc2004973. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Velis C.A. ISWA; Vienna: 2014. Global Recycling Markets - Plastic Waste: A Story for One Player – China. Report Prepared by FUELogy and Formatted by D-Waste on Behalf of International Solid Waste Association - Globalisation and Waste Management Task Force. September 2014. [Google Scholar]
- Wang M., Yan M., Xu H., Liang W., Kan B. SARS-CoV infection in a restaurant from palm civet. Emerg. Infect. Dis. 2005;11(12):1860–1865. doi: 10.3201/eid1112.041293. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wang Y., Wang Y., Chen Y., Qin Q. Unique epidemiological and clinical features of the emerging 2019 novel coronavirus pneumonia (COVID-19) implicate special control measures. J. Med. Virol. 2020;10 doi: 10.1002/jmv.25748. 1002/jmv.25748. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Watanabe T., Bartrand T.A., Weir M.H., Omura T., Haas C.N. Development of a dose‐response model for SARS coronavirus. Risk Anal.: Int. J. 2010;30(7):1129–1138. doi: 10.1111/j.1539-6924.2010.01427.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Who . WHO; 2013. World Health Organization (WHO), Poliovirus Detected from Environmental Samples in Israel and West Bank and Gaza Strip.https://www.who.int/csr/don/2013_09_20_polio/en/ (2013) [Online; accessed on 21-May-2020] [Google Scholar]
- WHO (World Health Organisation) Water, sanitation, hygiene, and waste management for the COVID-19 virus. Interim guidance. 2020 23 April 2020. [Google Scholar]
- Who . Department of Communications; 2020. Interim Guidance. 19 March 2020 | COVID-19: Infection Prevention and Control/WASH; Infection Prevention and Control during Health Care when Novel Coronavirus (nCoV) Infection Is Suspected.https://www.who.int/emergencies/diseases/novel-coronavirus-2019/ WHO Global; WHO/2019-nCoV/IPC/2020.3. [Google Scholar]
- Who . 2020. Coronavirus Disease (COVID-19) Dashboard.https://covid19.who.int/ (data as of 11:52 AM CEST, 15th June 2020) [Google Scholar]
- Wong G., Bi Y.H., Wang Q.H., Chen X.W., Zhang Z.G., Yao Y.G. Zoonotic origins of human coronavirus 2019 (HCoV-19/SARS-CoV-2): why is this work important? Zool. Res. 2020;41(3):213‐219. doi: 10.24272/j.issn.2095-8137.2020.031. [DOI] [PMC free article] [PubMed] [Google Scholar]
- World Bank 2020. https://www.worldbank.org/en/news/feature/2020/06/08/the-global-economic-outlook-during-the-covid-19-pandemic-a-changed-world (Accessed on 11th June 2020)
- Wu X., Nethery R.C., Sabath B.M., Braun D., Dominici F. 2020. Exposure to Air Pollution and COVID-19 Mortality in the United States. medRxiv, 2020.04.05.20054502. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wurtzer S., Marechal V., Mouchel J.M., Moulin L. 2020. Time Course Quantitative Detection of SARS-CoV-2 in Parisian Wastewaters Correlates with COVID-19 Confirmed Cases. medRxiv. [DOI] [Google Scholar]
- Xiao K., Zhai J., Feng Y., Zhou N., Zhang X., Zou J.J., Li N. Isolation of SARS-CoV-2-related coronavirus from Malayan pangolins. Nature. 2020 doi: 10.1038/s41586-020-2313-x. [DOI] [PubMed] [Google Scholar]
- Zhang W., Du R.H., Li B., Zheng X.S., Yang X.L. Molecular and serological investigation of 2019-nCoV infected patients: implication of multiple shedding routes. Emerg. Microb. Infect. 2020;9(1):386–389. doi: 10.1080/22221751.2020.1729071. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zhou P., Yang X.L., Wang X.G., Hu B., Zhang L. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature. 2020;579(7798):270‐273. doi: 10.1038/s41586-020-2012-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zhu N., Zhang D., Wang W., Li X., Yang B., Song J., Zhao X. China novel Coronavirus investigating and research team. A novel Coronavirus from patients with Pneumonia in China, 2019. N. Engl. J. Med. 2020;382(8):727‐733. doi: 10.1056/NEJMoa2001017. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.