Abstract
Fluorosis is an endemic disease, prevailing in about 25 countries globally. Dental fluorosis is an acquired defect of enamel due to the exposure of an individual to excessive fluoride levels during tooth development. It could result in mild-to-severe discoloration of teeth, which might necessitate esthetic correction. Bleaching is one of the common treatment modalities used in the esthetic correction of such cases. In-office power bleaching is one of the techniques of tooth bleaching that involves clinical application and activation of the bleaching agent with light to accelerate the bleaching process. This case report describes the esthetic correction of severe dental fluorosis by power bleaching, without any need for invasive treatment. This report suggests that in-office power bleaching is an effective and conservative method for esthetic correction of tooth discoloration in severe dental fluorosis.
Keywords: Esthetics, bleaching, dental fluorosis, tooth discoloration, Esthétique, blanchiment, fluorose dentaire, décoloration des dents
Résumé
La fluorose est une maladie endémique, qui prévaut dans environ 25 pays dans le monde. La fluorose dentaire est un défaut acquis des l’émail dû à l’exposition d’un individu à des niveaux excessifs de fluor pendant de développement des dents. Cela pourrait aboutir à une décoloration légère à sévère des dents, qui nécessite une correction esthétique. Le blanchiment est l’une des modalités de traitement courantes utilisées dans la correction esthétique de ces cas. “In-office power” le blanchiment est l’une des techniques de blanchiment des dents qui implique l’application clinique et l’activation de l’agent de blanchiment avec de la lumière pour accélérer le processus de blanchiment. Ce rapport de cas décrit la correction esthétique de la fluorose dentaire sévère par blanchiment “power”, sans aucun besoin pour d’un traitement invasif. Ce rapport suggère que le blanchiment “In-office power” est une méthode efficace et conservatrice pour la correction esthétique de la décoloration dentaire dans la fluorose dentaire sévère.
INTRODUCTION
Fluorine is a critical element for the calcification of bones and teeth. Fluoride ions exert “anticariogenic (caries-inhibiting) effect” on teeth when consumed at optimum levels.[1] According to the World Health Organization guidelines, the optimum fluoride level of drinking water is “1.5 ppm.”[2] Fluoride consumed in excess than the optimum value may lead to dental and skeletal fluorosis. Various researchers have found a positive correlation between polymorphisms in collagen type 1 alpha 2, calcitonin receptor gene, estrogen receptor, and risk of dental fluorosis, indicating that genetic factors may influence the susceptibility of an individual to the disease when other factors like environmental or dietary fluoride exposure remain the same.[3]
Dental fluorosis is an acquired defect of dental enamel due to successive exposures to higher fluoride concentration during the tooth development.[4] It is induced by the presence of fluoride close to the developing tooth bud during the secretory and/or maturation phase of amelogenesis. Fluorosis is endemic in about 25 countries in the world.[5]
The resultant tooth discoloration with or without malformation could compromise the individual appearance, social integration, and quality of life.[6] Hence, the treatment of discolored teeth has gained prominence in the practice of esthetic dentistry. Bleaching is a conservative approach to esthetically alter the color of teeth. Bleaching of vital teeth can be done by in-office method, dentist-supervised home bleaching or self-bleaching using over-the-counter products.[7] An in-office bleaching, hydrogen peroxide (concentrations varying from 15% to 38%) is directly applied on the tooth surface. To accelerate the bleaching process, the bleaching agent may be “photo” activated using light-emitting diodes, plasma arc, quartz halogen, ultraviolet units, and lasers; referred to as “power bleaching.”[8] Application of light-activation method leads to a decrease in treatment time and reduction in adverse effects of bleaching materials.[7]
There is a paucity of reports of such treatment in our clime; therefore, the purpose of this report is to highlight the treatment of tooth discoloration due to dental fluorosis with in-office bleaching.
CASE REPORT
A 16-year-old male reported to the Department of Conservative Dentistry and Endodontics, with a complaint of discolored anterior teeth. The patient was unable to recollect the time since when the teeth were discolored. However, he reported that the teeth were discolored for many years, and discoloration has increased over time. The patient did not experience any kind of sensitivity or pain associated with the discolored teeth. The patient was questioned about the occurrence of such discolored teeth in his siblings or other residents of his native village. He informed that the teeth of his younger brother as well as other residents were also discolored in a similar manner.
Intraoral examination revealed brownish discoloration of enamel with all maxillary and mandibular incisors, canines, and premolars. The pattern of discoloration was bilateral and symmetrical. The surfaces of some of these teeth were pitted. Discoloration was more prominent on maxillary teeth as compared to mandibular teeth [Figure 1]. Pulp sensibility testing of discolored teeth was carried out using cold test and electric pulp testing. It indicated normal pulp with all these teeth. The medical history was noncontributory. Based on the clinical features and history, a diagnosis of “severe” form of “dental fluorosis” was made (according to the Dean's fluorosis index).[9]
Figure 1.
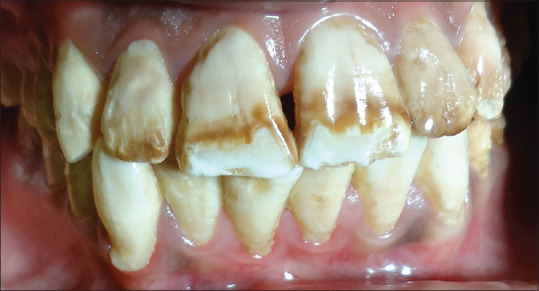
Preoperative photograph showing severe fluorosis
Various treatment options available were discussed with the patient, including in-office power bleaching, home bleaching, microabrasion, and composite veneers. The patient opted for “in-office power bleaching.” Informed consent was obtained from the patient. Tooth color was assessed using Vita shade guide, and pretreatment clinical photograph was taken. Maxillary and mandibular anterior teeth were polished with pumice and rubber cup. The rubber dam was applied to protect adjacent teeth and soft tissues. The patient was made to wear protective eyewear until the procedure was completed. Thirty-five percent of hydrogen peroxide gel was applied (Pola Office, SDI Limited, Australia) to the maxillary and mandibular anterior teeth. The bleaching gel was “photo” activated using a power bleaching unit (Bluedent 12 BL bleaching unit) for 15 min. The gel was removed with gauze, and the procedure was repeated for two more times. At the end of the procedure, all the applied gel was removed using suction, and teeth were rinsed with water. In the second visit after 1 week, the same procedure was repeated. At the end of the second visit, the patient was satisfied with the lightening of the shade of his teeth. Posttreatment tooth shade was recorded, and clinical photographs were taken at each visit [Figures 2 and 3].
Figure 2.
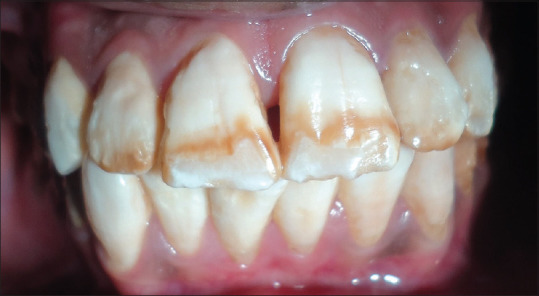
Post-bleaching photograph after the first bleaching session
Figure 3.
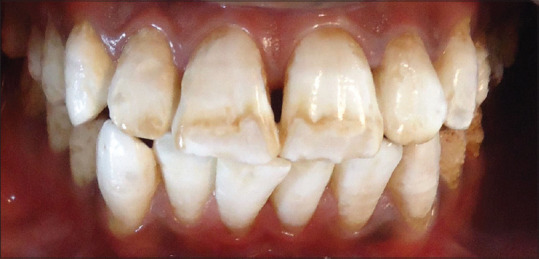
Post-bleaching photograph after the second bleaching session
After the completion of bleaching, it was suggested to the patient that further esthetic enhancement may be achieved by composite veneers. However, the patient was satisfied with the appearance of the teeth after bleaching and did not wish for the veneers. A desensitizing mouthwash was prescribed to the patient in view of possible post-bleaching sensitivity. The patient was followed up at 1, 3, and 6 months. There was no sensitivity, pain, or rebound effect associated with bleached teeth.
DISCUSSION
Dental fluorosis leads to the creation of an unsatisfactory “self-image” in the individual's mind and a sense of discontent, which depends on the severity of fluorosis.[10,11] Discoloration of teeth is the most common reason for which patients seek treatment. The various treatment modalities used for esthetic correction of such teeth include bleaching, resin infiltration, microabrasion, veneers, and full crowns. The choice of treatment depends on the severity of fluorosis.[12]
Conservative treatment modality like power bleaching may provide the dramatic esthetic enhancement of discolored teeth to the extent that no subsequent treatment is needed. However, if satisfactory esthetic correction is not achieved with bleaching, direct or indirect restorative procedures such as composite veneers or resin infiltration may be undertaken, which are invasive, destructive of natural tooth tissue, expensive, and time-consuming.[13] Thus, power bleaching may lead to an acceptable treatment result or reduce the amount of enamel and dentin removal for composite veneers.[14] Jarad et al. showed that bleaching before direct composite veneer placement had a significant effect on the final shade of the veneer, which was also dependent on the thickness or shade of the restoration.[15] In our case, composite veneers could have been placed on maxillary anterior teeth after power bleaching. However, the patient was not ready for the same, as he was satisfied with the result of bleaching.
More recently, resin infiltration has been applied in the management of dental fluorosis as an effective and conservative technique. It involves the penetration of low-viscosity resin into the fluorotic opacities after conditioning with hydrochloric acid. Schoppmeier et al. showed that prior in-office power bleaching improved the “masking effect” of resin infiltration on fluorotic opacities. In this way, power bleaching may be used as a pretreatment regimen for achieving better esthetic results with resin infiltration.[16]
One of the concerns about light-activated in-office vital bleaching is the increase in the surface and intra-pulpal temperature associated with the use of bleaching lamps. Sulieman et al. reported that increase in intra-pulpal temperature with the use of various lamps (plasma arc lamp, xenon-halogen lamp, and standard halogen lamp) was below the critical threshold of 5.5°C, except for the laser-based lamp.[17]
Post-bleaching sensitivity is a common side effect of bleaching, which results because of the percolation of peroxide to the pulp through dentin. Moghadam et al. reported that 42.9% of patients experienced sensitivity after home bleaching, whereas 57.1% of patients following power bleaching.[18] Kabil et al. studied the effect of “descending light intensity protocol (high intensity, followed by moderate and finally low intensity)” on post-bleaching sensitivity and found lower sensitivity with this protocol as compared to conventional “high light intensity protocol.”[19] Desensitizing agents may be used after bleaching to reduce post-bleaching sensitivity.[20]
CONCLUSION
The findings of this case report suggest that in-office bleaching is an effective, simple, and noninvasive method for esthetic correction of discolored teeth with severe dental fluorosis. It might also be used as a pretreatment regimen for direct or indirect esthetic restoration and resin infiltration in such cases.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient and his parents have given their consent for his images and other clinical information to be reported in the journal. The patient understands that his names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
REFERENCES
- 1.Priyadharsini N, Malathi N, Tamizhchelvan H, Dineshkumar T. Dental fluorosis: A histological study using light and confocal microscopy. Indian J Dent Res. 2015;26:248–51. doi: 10.4103/0970-9290.162896. [DOI] [PubMed] [Google Scholar]
- 2.Goyal A, Verma M, Toteja GS, Gauba K, Mohanty V, Mohanty U, et al. Validation of ICMR index for identification of dental fluorosis in epidemiological studies. Indian J Med Res. 2016;144:52–7. doi: 10.4103/0971-5916.193283. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Pramanik S, Saha D. The genetic influence in fluorosis. Environ Toxicol Pharmacol. 2017;56:157–62. doi: 10.1016/j.etap.2017.09.008. [DOI] [PubMed] [Google Scholar]
- 4.Abanto Alvarez J, Rezende KM, Marocho SM, Alves FB, Celiberti P, Ciamponi AL. Dental fluorosis: Exposure, prevention and management. Med Oral Patol Oral Cir Bucal. 2009;14:E103–7. [PubMed] [Google Scholar]
- 5.Kumar S, Gopal K. A review on fluorosis and its preventive strategies. Indian J Environ Protection. 2000;20:430–40. [Google Scholar]
- 6.Meireles SS, Goettems ML, Dantas RV, Bona ÁD, Santos IS, Demarco FF. Changes in oral health related quality of life after dental bleaching in a double-blind randomized clinical trial. J Dent. 2014;42:114–21. doi: 10.1016/j.jdent.2013.11.022. [DOI] [PubMed] [Google Scholar]
- 7.Alqahtani MQ. Tooth-bleaching procedures and their controversial effects: A literature review. Saudi Dent J. 2014;26:33–46. doi: 10.1016/j.sdentj.2014.02.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Sulieman M. An overview of bleaching techniques: 3. In-surgery or power bleaching. Dent Update. 2005;32:101. doi: 10.12968/denu.2005.32.2.101. [DOI] [PubMed] [Google Scholar]
- 9.Moulton FR. The Investigation of Physiologic Effects by Epidemiological Method: Fluorine and Dental Health. Washington, DC: American Association for the Advancement of Science; 1942. pp. 23–31. [Google Scholar]
- 10.de Castilho LS, e Ferreira EF, Perini E. Perceptions of adolescents and young people regarding endemic dental fluorosis in a rural area of Brazil: Psychosocial suffering. Health Soc Care Community. 2009;17:557–63. doi: 10.1111/j.1365-2524.2009.00859.x. [DOI] [PubMed] [Google Scholar]
- 11.Alkhatib MN, Holt R, Bedi R. Aesthetically objectionable fluorosis in the United Kingdom. Br Dent J. 2004;197:325–8. doi: 10.1038/sj.bdj.4811651. [DOI] [PubMed] [Google Scholar]
- 12.Ermis RB, Ugurlu M. A case report on fluorosed teeth whitening without microabrasion – Is it possible? J Res Dent. 2015;3:83–7. [Google Scholar]
- 13.Deliperi S, Congiu MD, Bardwell DN. Integration of composite and ceramic restorations in tetracycline-bleached teeth: A case report. J Esthet Restor Dent. 2006;18:126–34. doi: 10.1111/j.1708-8240.2006.00011.x. [DOI] [PubMed] [Google Scholar]
- 14.Ng F, Manton DJ. Aesthetic management of severely fluorosed incisors in an adolescent female. Aust Dent J. 2007;52:243–8. doi: 10.1111/j.1834-7819.2007.tb00495.x. [DOI] [PubMed] [Google Scholar]
- 15.Jarad FD, Griffiths CE, Jaffri M, Adeyemi AA, Youngson CC. The effect of bleaching, varying the shade or thickness of composite veneers on final colour: An in vitro study. J Dent. 2008;36:554–9. doi: 10.1016/j.jdent.2008.04.004. [DOI] [PubMed] [Google Scholar]
- 16.Schoppmeier CM, Derman SH, Noack MJ, Wicht MJ. Power bleaching enhances resin infiltration masking effect of dental fluorosis. A randomized clinical trial. J Dent. 2018;79:77–84. doi: 10.1016/j.jdent.2018.10.005. [DOI] [PubMed] [Google Scholar]
- 17.Sulieman M, Addy M, Rees JS. Surface and intra-pulpal temperature rises during tooth bleaching: An in vitro study. Br Dent J. 2005;199:37–40. doi: 10.1038/sj.bdj.4812558. [DOI] [PubMed] [Google Scholar]
- 18.Moghadam FV, Majidinia S, Chasteen J, Ghavamnasiri M. The degree of color change, rebound effect and sensitivity of bleached teeth associated with at-home and power bleaching techniques: A randomized clinical trial. Eur J Dent. 2013;7:405–11. doi: 10.4103/1305-7456.120655. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Kabil SH, Haridy MF, Farid MR. Effect of high light intensity bleaching protocol versus descending light intensities bleaching protocol on post bleaching teeth sensitivity: A randomized clinical trial. Open Access Maced J Med Sci. 2019;7:2173–81. doi: 10.3889/oamjms.2019.588. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Nanjundasetty JK, Ashrafulla M. Efficacy of desensitizing agents on postoperative sensitivity following an in-office vital tooth bleaching: A randomized controlled clinical trial. J Conserv Dent. 2016;19:207–11. doi: 10.4103/0972-0707.181927. [DOI] [PMC free article] [PubMed] [Google Scholar]


