Abstract
Chiari 1 Malformation in children is defined as 6 mm or more caudal extension of cerebellar tonsils below the foramen magnum. It is one of the deformities in the spectrum of craniovertebral junction anomalies. We report an unusual case of newborn girl with hypoplasia of bassiocciput of the clivus and extension of brainstem into the oropharynx, in addition to extension of cerebellar tonsils below the foramen magnum. Right anterior arch and right posterior arch of C1 vertebra are absent. Dens of C2 vertebra is asymmetric. Laryngoscope showed a membrane covering the brainstem in the oropharynx. Endotracheal and orogastric tubes were placed. A ventriculo-peritoneal shunt was placed for hydrocephalus. The patient was discharged home at 4.5 months of age with home Hospice care. To the best of our knowledge, this has not been described in the literature. The case illustrates a rare defect in the clivus and unusual protrusion of brainstem into oropharynx.
Keywords: Chiari 1 Malformation, Clivus hypoplasia, Craniocervical junction anomalies
Abbreviations: MRI, magnetic resonance imaging; CT, computed tomography; US, ultrasonography; CNS, central nervous system
Introduction
Chiari malformations are anomalies of craniocervical junction and posterior fossa with downward extension of cerebellar structures at the craniocervical junction [1]. Chiari malformations are associated with spinal cord abnormalities such as syringomyelia or in more severe cases with aqueductal stenosis, hydrocephalus, encephalocele, and lumbosacral meningomyelocele.
Chiari 1 malformations are typically due to short clivus, abnormal cervical vertebral segmentation, and/or a small or overcrowded posterior fossa [1] that leads to caudal extension of cerebellar tonsils. Sometimes medulla also extends down through the foramen magnum into the spinal canal [1]. In children, Chiari 1 malformation is defined as 6 mm or more caudal extension of cerebellar tonsils below the foramen magnum.
The unique feature of this case is that there is a defect in the inferior part of clivus with protrusion of brainstem into oropharynx. To the best of our knowledge, this has not been described in the literature.
Details of the case
The patient is a newborn African-America girl born prematurely at 33 weeks and 2 days of gestation. Prenatal ultrasound showed ventriculomegaly, polyhydramnios, intrauterine growth restriction, transverse lie, and left club foot. Prenatal Ultrasound did not identify the brainstem protrusion in the oropharynx. Clinical examination at birth verified macrocephaly and splayed sutures.
MRI of the brain performed at birth revealed hypoplasia of the basiocciput portion of the clivus (Fig. 1) and part of brainstem and cerebellar tissue extended anteriorly into the oropharynx (Fig. 2). There was marked hydrocephalus (Fig. 3). Cerebellum and brainstem extended below the foramen magnum.
Fig. 1.
Clival defect with brainstem extending into oropharynx: Midline sagittal T1- weighted (Fig. 1A) and T2-weighted (Fig. 1B) images demonstrate brainstem (green arrow) extending into oropharynx (blue asterisk) and hypoplasia of the basiocciput (blue arrow) portion of the clivus. Basisphenoid portion (green asterisk) and syndesmosis (yellow arrow) are also depicted.
Fig. 2.
Brainstem extending into oropharynx: Axial T2 weighted MRI image at the level of maxilla (yellow arrow) depict extension of brainstem (green arrow) into the oropharynx (blue asterisk).
Fig. 3.
Hydrocephalus: Axial T2 weighted MRI of the brain shows dilated lateral ventricles (yellow arrow).
These findings were further corroborated on CT scan with depiction of hypoplastic basiocciput part of the clivus (Fig. 4, Fig. 5, Fig. 6), absent right anterior arch of C1 and absent right posterior arch of C1 (Fig. 7). Additionally, there was abnormal alignment at the craniovertebral junction with levoconvex curvature of the upper cervical spine relative to the skull base. There was asymmetry of dens of C2. The right laminae of C2, C3, and C4 vertebrae were fused.
Fig. 4.
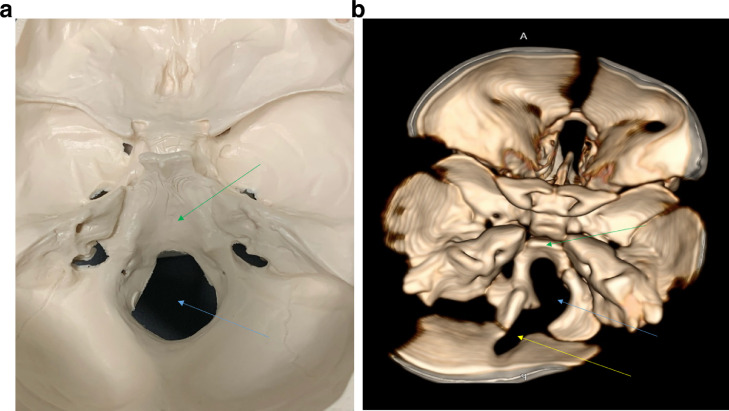
Superior view of foramen magnum: Photo of foramen magnum of a skeleton (Fig. 4A) and 3D rendered CT image of our case (Fig. 4B) show foramen magnum (blue arrow) and clivus (green arrow) as viewed from superior aspect. Figure 4B depicts the hypoplasia of the inferior part of the clivus and defect in the left side of the occipital bone (yellow arrow).
Fig. 5.
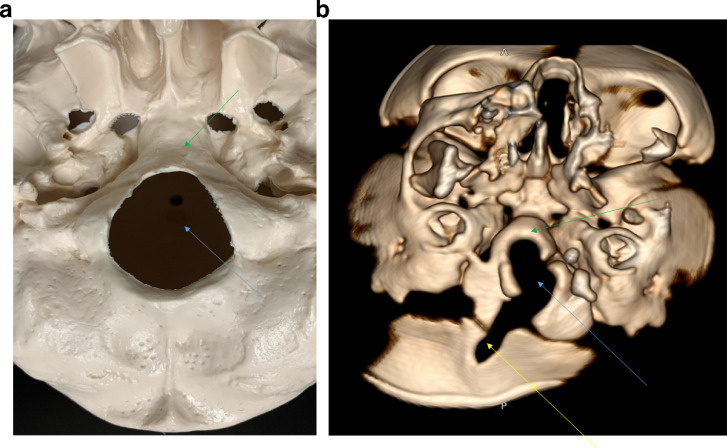
Inferior view of foramen magnum: Photo of foramen magnum of a skeleton (Fig. 5A) and 3D rendered CT image of our case (Fig. 5B) show foramen magnum (blue arrow) and clivus (green arrow) as viewed from inferior aspect. Figure 5B depicts the hypoplasia of the inferior part of the clivus and defect in the left side of the occipital bone (yellow arrow).
Fig. 6.
Bony defect and brainstem: Inferior view of the 3D rendered CT image of the case (Fig. 6A), axial T2-weighted MRI image (Fig. 6B) and superior view of the 3D rendered CT (Fig. 6C) that is flipped sideways to match Figure 6A and B depict foramen magnum (blue arrow), clivus (green arrow) and defect in the left side of the occipital bone (yellow arrow). Figure 6B depicts brainstem (purple arrow) extending into the oropharynx (blue asterisk). Defect in the left side of the occipital bone (yellow arrow) is also seen on MRI.
Fig. 7.
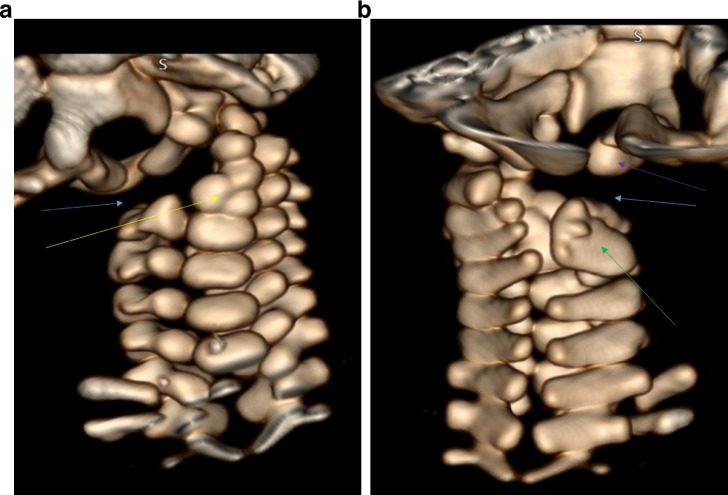
Anomalies of upper cervical spine: Anterior view (Fig. 7A) and posterior view (Fig. 7B) from the 3D rendered CT show absent anterior and posterior arch of C1 on the right side (blue arrow), fused right laminae (green arrow) of C2, C3 and C4 vertebrae as well as asymmetric dens of C2 (yellow arrow). Right occipital condyle (purple arrow) does not articulate with any bony structure.
Laryngoscope showed a membrane covering the brainstem in the oropharynx. Endotracheal and orogastric tubes were placed carefully. The infant was shunted for hydrocephalus. The patient was discharged home at 4.5 months of age with home Hospice care.
Discussion
John Cleland and Hans Chiari described anomalies of craniocervical junction in late 19th century. The 3 types of hindbrain extension into upper cervical spinal canal are categorized as Chiari malformation types 1-3 [2], [3], [4]–5]. The posterior section of the middle skull base is called clivus that is formed by the basisphenoid superiorly and by basiocciput inferiorly which are derived from the neural crest and mesoderm respectively [6], [7], [8], [9]–10]. Embryonic development of the base of the skull occurs by mesenchymal condensation, chondrification and ossification. In the case of Chiari 1 malformation, skull base anatomical anomaly may occur due to segmental defect or underdevelopment of the occipital bone due to mesodermal insufficiency [6].
Congenital Chiari 1 malformations are typically asymptomatic during childhood, but as children grow into adulthood, they may experience headache, dizziness, or other cerebellar symptoms. Some of these patients develop syringomyelia which is a cystic cavity formed in the spinal cord due to an obstruction of cerebrospinal fluid within the central canal of the spinal cord secondary to the mass effect of cerebellar tonsillar herniation. A moderately large syringomyelia can damage the spinothalamic tract crossing fibres within the anterior white commissure [11]. Patients with Chiari 1 malformation and syringomyelia are most often treated by surgical decompression of the crowded foramen magnum.
Moore and Moore have described a complex variant of Chiari 1 malformation with a more severe clinical phenotype that may require more extensive surgical decompression [12]. In this variant, along with caudal tonsillar herniation there is inferior brainstem herniation through the foramen magnum, sometimes referred to as Chiari 1.5 malformation.
The Chiari II malformation is characterized by the downward displacement of the cerebellar vermis and tonsils through the foramen magnum often with small fourth ventricle leading to hydrocephalus. Chiari II malformations typically have a coexisting meningomyelocele which is a herniation of the spinal cord meninges and neural tissue through the vertebral body. This may lead to a paralysis or sensory loss at and below the level of the lesion [13].
The Chiari III malformation is rare. It is characterized by inferior displacement of the medulla into the spinal canal with cervical or occipital encephalocele, typically with ectopia of cerebellar structures into the encephalocele [14].
The Chiari IV malformation is not a true malformation, but rather describes hypoplasia of the cerebellum [1]. This may be associated with Dandy-Walker syndrome which is hypoplasia of the cerebellar vermis leading to cystic enlargement of 4th ventricle that fills the enlarged posterior fossa and is associated with noncommunicating hydrocephalus and spina bifida.
Management for Chiari malformation is based on the extent of neurologic defect and other anatomical abnormalities typically with decompressive surgery of the craniocervical junction to restore CSF flow for those with significant occipital headaches, cranial nerve palsies, syringomyelia, or other cerebellar symptoms [13]. Posterior decompression by suboccipital craniectomy sometimes with accompanying duraplasty is most common. Treatment for Chiari II malformation includes closure of neural tube defects and shunt placement to decompress hydrocephalus [1]. Asymptomatic patients without syringomyelia or meningomyelocele may be managed conservatively with annual clinical assessment and magnetic resonance imagining studies.
According to Tubbs, Lyerly MJ, Loukas M, et al., currently, there is no consensus on either the exact pathogenesis or treatment for any of the Chiari malformations. Although the Chiari classification is helpful in categorizing most patients, this scheme most likely does not represent a precise continuum of the same disease process [15]. Nevertheless, surgical decompression is most often the treatment of course for those with significant symptoms.
In Ingraham and Swan's survey of over 500 cases of spina bifida and cranium bifidum, they report that while meningoceles are most commonly congenital malformations of the central nervous system located in the lumbar region, they may be present at any point along the neuraxis including in the occipital, nasal, nasopharyngeal, frontal, basal and parietal locations [16]. Ingraham and Swan's survey did not report any transclival meningocele.
In 1980, Lockwood, Quencer and Page were the first researchers to report a case of a meningocele that protruded through the clivus [17]. Using computerized tomographic cisternography, these researchers investigated the case of a 63-year-old woman with a 10-year history of spontaneous cerebrospinal fluid rhinorrhea. Ultimately these researchers were able to surgically repair the clival defect using Gelfoam, dried dura and a bone plug with resolution of the rhinorrhea [17].
Akyuz, Arslan, Gurkanlar, et al describe a case of a 36-year-old female with intermittent spontaneous cerebrospinal fluid rhinorrhea who was found to have a transclival meningocele diagnosed by MRI and CT. It was surgically corrected via transsphenoidal approach with fascia graft and bio-glue [18]. They claimed that theirs was the third case in the literature of a transclival meningocele producing rhinorrhea in an adult [19]. A transclival meningocele is an extremely rare lesion [18].
What is described above may well be a novel case. To the best of our knowledge, no case of transclival protrusion of brainstem into oropharynx in a pediatric patient exists in the literature.
Conclusion
Severe clival defects and brainstem protrusion in the oropharynx can be a rare manifestation of Chiari 1 malformation and understanding these craniocervical junction anomalies can be prudent for neuroradiology teaching and better clinical outcome. Important lesson is that the brainstem that protrudes in the oropharynx is at risk for damage and needs careful intubation and orogastric tube placement for survival.
References
- 1.Sarnat HB. Disorders of segmentation of the neural tube: chiari malformations. Handbook of Clin Neurol. 2008;87:89. doi: 10.1016/S0072-9752(07)87006-0. [DOI] [PubMed] [Google Scholar]
- 2.Carmel PW, Markesbery WR. Early descriptions of the Arnold-Chiari malformation. The contribution of John Cleland. J Neurosurg. 1972;37:543. doi: 10.3171/jns.1972.37.5.0543. [DOI] [PubMed] [Google Scholar]
- 3.Poretti A, Boltshauser E, Huisman TAGM. Chiari Malformations and Syringohydromyelia in Children. Seminars in Ultrasound, CT and MRI. 2016;37(2):129–142. doi: 10.1053/j.sult.2015.12.001. [DOI] [PubMed] [Google Scholar]
- 4.Schijman E. History, anatomic forms, and pathogenesis of Chiari I malformations. Childs Nerv Syst. 2004;20:323. doi: 10.1007/s00381-003-0878-y. [DOI] [PubMed] [Google Scholar]
- 5.Barkovich AJ, Wippold FJ, Sherman JL, Citrin CM. Significance of cerebellar tonsillar position onMR. AJNR Am J Neuroradiol. 1986;7(5):795–799. [PMC free article] [PubMed] [Google Scholar]
- 6.Poretti A., Ashmawy R., Garzon-Muvdi T., Jallo G., Huisman T., Raybaud C. Chiari Type 1 deformity in children: pathogenic, clinical, neuroimaging, and management aspects. Neuropediatrics. 2016;46:293–307. doi: 10.1055/s-0036-1584563. [DOI] [PubMed] [Google Scholar]
- 7.Nwotchouang BST, Eppelheimer MS, Bishop P, Biswas D, Andronowski JM, Frim D. Three-dimensional CT morphometric image analysis of the clivus and sphenoid sinus in Chiari Malformation Type I. Ann Biomed Eng. 2019;47(11):2284–2295. doi: 10.1007/s10439-019-02301-5. [DOI] [PubMed] [Google Scholar]
- 8.Milhorat T.H., Chou M.W., Trinidad E.M., Kula R.W., Mandell M., Wolpert C. Chiari I malformation redefined: clinical and radiographic findings for 364 symptomatic patients. Neurosurgery. 1999;44(5):1005–1017. doi: 10.1097/00006123-199905000-00042. [DOI] [PubMed] [Google Scholar]
- 9.Arens R., McDonough J.M., Costarino A, Mahboubi S, Tayag-Kier CE, Maislin G. Magnetic resonance imaging of the upper airway structure of children with obstructive sleep apnea syndrome. Am J Respir Crit Care Med. 2001;164:6998. doi: 10.1164/ajrccm.164.4.2101127. [DOI] [PubMed] [Google Scholar]
- 10.Deza E.S.M, Santamarta A., Ayala S, Murias E., Vega Valdes P, Pendas L, Oviedo E. The Clivus Lesions: Crossroads Of Skull Base. European Society of Radiology. ECR. 2014 doi: 10.1594/ecr2014/C-1617. [DOI] [Google Scholar]
- 11.Menezes AH. Chiari I malformations and hydromyelia–complications. Pediatric Neurosurg. 1991;17:146. doi: 10.1159/000120586. 1992. [DOI] [PubMed] [Google Scholar]
- 12.Moore HE, Moore KR. Magnetic resonance imaging features of complex Chiari malformation variant of Chiari 1 malformation. Pediatr Radiol. 2014;44(11):1403–1411. doi: 10.1007/s00247-014-3021-1. [DOI] [PubMed] [Google Scholar]
- 13.McLone DG, Dias MS. The Chiari II malformation: Cause and impact. Childs Nerv Syst. 2003;19(7-8):540–550. doi: 10.1007/s00381-003-0792-3. [DOI] [PubMed] [Google Scholar]
- 14.Caldarelli M, Rea G, Cincu R, Di Rocco C. Chiari type III malformation. Childs Nerv Syst. 2002;18:207. doi: 10.1007/s00381-002-0579-y. [DOI] [PubMed] [Google Scholar]
- 15.Tubbs RS, Lyerly MJ, Loukas M, Shoja MM, Oakes WJ. The pediatric Chiari I malformation: a review. Childs Nerv Syst. 2007;23(11):1239–1250. doi: 10.1007/s00381-007-0428-0. [DOI] [PubMed] [Google Scholar]
- 16.Ingraham FD, Swan H. Spina bifida and cranium bifidum. I. A survey of five hundred forty-six cases. N Engl J Med. 1943;228:559–563. [Google Scholar]
- 17.Lockwood Alan H., Quencer Robert M, Pake Larry K. CSF rhinorrhea from a tranclival meningocele demonstrated with metrizamide CT cisternography. J. Neurosurg. 1980;53:553–555. doi: 10.3171/jns.1980.53.4.0553. [DOI] [PubMed] [Google Scholar]
- 18.Akyuz M., Arslan G., Gurkanlar D, Tuncer R. CSF Rhinorrhea from a Transclival Meningocele: A Case Report. J. Neuroimaging. 2008;18:191–193. doi: 10.1111/j.1552-6569.2007.00187.x. [DOI] [PubMed] [Google Scholar]
- 19.Novegno F, Caldarelli M, Massa A. The natural history of the Chiari Type I anomaly. J Neurosurg Pediatr. 2008;2:179. doi: 10.3171/PED/2008/2/9/179. [DOI] [PubMed] [Google Scholar]