This systematic review and network meta-analysis compares the 3 most common surgical techniques—endoscopic laser-assisted diverticulotomy, endoscopic stapler-assisted diverticulotomy, and transcervical diverticulectomy with cricopharyngeal myotomy—in adults with Zenker diverticulum.
Key Points
Question
Which surgical treatment for Zenker diverticulum is associated with the lowest incidence of postoperative persistent or recurrent dysphagia symptoms?
Findings
In this systematic review and network meta-analysis, open diverticulectomy with cricopharyngeal myotomy was associated with lowest incidence of persistent or recurrent symptoms compared with endoscopic stapler–assisted and CO2 laser diverticulotomy. There was no significant difference with the primary outcome measure when comparing the 2 endoscopic techniques.
Meaning
The open, transcervical approach appears to be superior to endoscopic techniques in avoiding persistent or recurrent symptoms postoperatively.
Abstract
Importance
Zenker diverticulum (ZD) can cause significant dysphagia, and symptoms can return or persist after surgery. This systematic review and network meta-analysis is the first to our knowledge to compare 3 common surgical techniques for ZD.
Objective
To compare the 3 most common surgical techniques—endoscopic laser-assisted diverticulotomy, endoscopic stapler-assisted diverticulotomy, and transcervical diverticulectomy with cricopharyngeal myotomy—in adult patients with ZD.
Data Sources
The published literature was searched using strategies designed by a medical librarian (search performed September 21, 2018). Strategies were established using a combination of controlled vocabulary terms and keywords and were executed in Ovid MEDLINE (1946 to September 21, 2018), Embase (1947 to September 21, 2018), Scopus (1823 to September 21, 2018), Cochrane Library, and ClinicalTrials.gov. Results were limited to English using database-supplied filters, which generated studies from 1997 to 2017.
Study Selection
Inclusion criteria were cohort studies or randomized clinical trials. Studies that included patients needing revision surgery or undergoing an alternative technique were excluded.
Data Extraction and Synthesis
The Preferred Reporting Items for Systematic Reviews and Meta-analyses–Network Meta-analyses (PRISMA-NMA) checklist was used to report the study findings. Two authors independently reviewed the studies.
Main Outcome and Measure
The primary outcome measure was the incidence of persistent or recurrent symptoms following surgery. The primary study outcome was planned before data collection began.
Results
The search generated 529 studies. After applying inclusion and exclusion criteria, 9 cohort studies remained, consisting of 903 patients treated with either laser-assisted diverticulotomy (n = 283), transcervical diverticulectomy (n = 150), or stapler-assisted diverticulotomy (n = 470). A network meta-analysis was performed. Between endoscopic laser-assisted diverticulotomy and open diverticulectomy, the open approach showed a statistically lower likelihood of persistent/recurrent symptoms following treatment (odds ratio [OR], 0.20; 95% CI, 0.04-0.91). Comparing laser-assisted diverticulotomy with the stapler-assisted technique, there was not a significant difference between the 2 techniques (OR, 0.83; 95% CI, 0.43-1.60). The consistency model for the network meta-analysis was supported (χ21 = 0.12; P = .73).
Conclusions and Relevance
This systematic review and meta-analysis compared 3 common techniques for treating ZD. The open approach showed a decreased likelihood of persistent or recurrent symptoms following surgery compared with the 2 other techniques.
Introduction
Zenker diverticulum (ZD) is an acquired pharyngeal outpouching in the hypopharynx between the inferior constrictor and the cricopharyngeus (CP) muscles.1 It most frequently occurs in the older adult population, typically after the seventh decade of life.2 Symptoms of ZD include dysphagia, regurgitation, weight loss, and recurrent aspiration.3,4 It is thought to develop secondary to CP muscle dysfunction, and the CP myotomy is considered fundamental in preventing recurrence.5,6 Although the incidence of ZD is reported to be fairly low in the general population,7 it is the most common type of pharyngoesophageal diverticulum.8
Surgery is the mainstay treatment for symptomatic ZD.9,10 Historically, ZD has been surgically excised using an open, transcervical approach.11 Open surgery techniques include diverticulectomy (excision of the pouch),12 diverticulopexy (suspension of the pouch),13 and cricopharyngeal myotomy. Unfortunately, transcervical excision has the potential to cause substantial complications,14 which is especially problematic in the older adult population. As a result, endoscopic diverticulotomy has become increasingly popular. The endoscopic approach is performed by transorally dividing the common wall between the diverticulum and the esophagus, thereby severing CP muscle fibers.15 Endoscopic diverticulotomy is also attractive because it avoids a neck incision, has a shorter intraoperative duration,16 and has a quicker recovery time.17
There is ongoing debate as to the comparative effectiveness of endoscopic and open techniques.18,19 Shah et al15 compared the size of the residual party wall following endoscopic and open surgical approaches. While the authors found that the endoscopic stapler technique tended to incompletely remove the common pouch wall compared with the open approach (postoperative median percentage of 44% and 0%, respectively), there was no significant difference in the degree of symptomatic improvement based on the Eating Assessment Tool (EAT-10)20 scores. Parker and Misono21 performed a systematic review and meta-analysis comparing 2 endoscopic techniques: CO2 laser and stapler-assisted diverticulotomy. The authors found no difference in the length of nothing-by-mouth duration, length of hospitalization, or rate of surgical revision, although the incidence of postoperative or recurrent dysphagia symptoms was not specifically investigated.
Despite previous studies, to our knowledge, no meta-analyses have examined the differences among all 3 major techniques in a single comparison. In this study, a systematic review and meta-analysis was performed to compare the 3 most common surgical techniques—endoscopic laser-assisted diverticulotomy, endoscopic stapler-assisted diverticulotomy, and transcervical diverticulectomy with cricopharyngeal myotomy—in adult patients with ZD. A network meta-analysis was conducted to simultaneously compare 3 treatment groups. The overall goal of the study was to compare the incidence of postoperative persistent and recurrent symptoms among the 3 aforementioned groups. We hypothesized that open, transcervical diverticulectomy would have relatively fewer number of patients with persistent or recurrent symptoms postoperatively.
Methods
This study was exempt from the Washington University Institutional Review Board owing to the use of previously published data. The Preferred Reporting Items for Systematic Reviews and Meta-analyses–Network Meta-analyses (PRISMA-NMA) checklist was used to report the study findings.22 This study was not registered to the PROSPERO database prior to data collection.
Systematic Review and Study Selection
The PICO (population, intervention, comparator, outcome) format was used prior to data collection to determine which studies were eligible for answering the main study question. The population of interest was adults 18 years and older with ZD. The intervention and comparator groups needed to be combined given 3 groups: (A) endoscopic laser-assisted diverticulotomy, (B) open diverticulectomy with cricopharyngeal myotomy, and (C) endoscopic stapler-assisted diverticulotomy. The outcome measure was the incidence of persistent or recurrent symptoms following surgical intervention.
The published literature was searched by a medical librarian for the concepts of laser therapy, endoscopic stapling, and open surgery for the treatment of ZD (date of search, September 21, 2018). These strategies were established using a combination of controlled vocabulary terms and keywords and were executed in Ovid MEDLINE (1946 to September 21, 2018), Embase (1947 to September 21, 2018), Scopus (1823 to September 21, 2018), Cochrane Library, and ClinicalTrials.gov. Results were limited to English using database-supplied filters. Results were exported to EndNote, and duplicate citations were removed. Full search strategies are provided in the eAppendix in the Supplement. The database search was supplemented with a hand search of relevant resources.
Two authors (N.K.B. and J.M.) independently reviewed research abstracts and studies using Microsoft Excel (Microsoft Corp). Studies were excluded if they were (1) not randomized clinical trials or cohort studies, (2) animal and cadaver studies, (3) investigating other pharyngeal/esophageal diverticula, or (4) not in English. At the full-text stage, studies were further excluded if they (1) used an endoscopic technique besides laser-assisted or stapler-assisted diverticulotomy, (2) used an open approach other than diverticulectomy with cricopharyngeal myotomy, (3) did not present the rate of persistent or recurrent symptoms, (4) included any cases of revision ZD, (5) studied any techniques using flexible endoscopes, or (6) presented results without any comparison or control (Figure 1).
Figure 1. Flow Diagram Outlining the Exclusion of Studies.
ZD indicates Zenker diverticulum.
Data Extraction
The primary outcome measure was the incidence of persistent or recurrent symptoms following ZD treatment. The study design, type of surgery, number of patients, length of follow-up, and location were collected. The Newcastle-Ottawa scale was selected to assess the quality of the included cohort studies.23 The Oxford quality scoring system was chosen to rate the quality of randomized control trials.24
Statistical Analysis
A network meta-analysis was performed to compare 3 techniques: endoscopic laser-assisted diverticulotomy (group A), open diverticulectomy with cricopharyngeal myotomy (group B), and endoscopic stapler-assisted diverticulotomy (group C). A network meta-analysis was designed to formulate direct and indirect comparisons to simultaneously evaluate multiple treatment modalities. Similarity between studies was qualitatively evaluated using the PICO technique. Odds ratios (ORs) for recurrent or persistent postoperative symptoms were calculated for each direct and pooled comparison using the network analysis (A vs B, A vs C, and B vs C), and CIs were calculated around the point estimate for each comparison.
The consistency assumption between direct and indirect comparisons within the network analysis was quantitatively assessed using the Wald test.25 Network geometry was generated to visually show the multiple comparisons. Data analysis was performed in Stata, version 15.1 (StataCorp).
Results
Systematic Review
The medical literature search consisting of computerized and manual searches generated 529 studies. After excluding duplicates, studies including other pharyngeal/esophageal pathology, and improper study design, 110 studies remained. The full texts of the remaining studies were reviewed. Studies that included alternate open/endoscopic techniques outside the study design, cases of revision ZD, or an inadequate comparison group were excluded. Following the exclusion, 9 studies were included in the meta-analysis (Figure 1).
Table 1 presents the studies include in the meta-analysis. All studies were retrospective cohort studies that compared 2 of the 3 study groups. The Newcastle-Ottawa scale (9-point scale) was used to measure the quality of the cohort studies. Five studies were rated as 9, while the remaining 4 studies were rated as 8 (mean, 8.56). Among the 4 studies with the 8-point rating, the point deduction occurred secondary to not specifying the average follow-up length.
Table 1. Studies Included in the Systematic Review.
| Sourcea | Patients in study, No. | Incidence of persistent/recurrent symptoms postsurgery | Pouch size, cm | Follow-up time | Type of laser | Type of stapler | Newcastle-Ottawa score (9-point scale) |
|---|---|---|---|---|---|---|---|
| Adam et al,3 2012 | A (n = 61) | A (n = 0) | Mean (SD): A = 3.3 (0.9) C = 3.5 (1.1) |
Minimum 6 mo | CO2 laser | Endo GIA 30 stapler | 9 |
| C (n = 67) | C (n = 7) | ||||||
| Bonavina et al,23 2007 | B (n = 116) | B (n = 2) | Median (range): B = 4.0 (1.0-9.0) C = 4.0 (2.5-8.0) |
Median: 27 mo (stapler-assisted); 48 mo (open) | NA | Ethicon ETS 35 stapler | 9 |
| C (n = 181) | C (n = 8) | ||||||
| Henry et al,24 2013 | B (n = 24) | B (n = 0) | Mean (SD): B = 4.1 (1.5) C = 5.3 (1.5) |
Mean: 33 mo (open); 28 mo (stapler-assisted) | NA | Ethicon 45 mm stapler | 9 |
| C (n = 12) | C (n = 4) | ||||||
| Keck et al,25 2010 | A (n = 4) | A (n = 1) | Not reported | Not reported | CO2 laser | NA | 8 |
| B (n = 10) | B (n = 1) | ||||||
| Leibowitz et al,26 2014 | A (n = 68) | A (n = 10) | Mean: A = 3.3 C = 3.8 |
Minimum 12 mo | CO2 laser | Not reported | 9 |
| C (n = 69) | C (n = 5) | ||||||
| Miller et al,27 2006 | A (n = 16) | A (n = 1) | Mean: A = 3.8 C = 4.4 |
Not reported | CO2 laser | Endo GIA 30 stapler | 8 |
| C (n = 19) | C (n = 0) | ||||||
| Murer et al,28 2015 | A (n = 29) | A (n = 5) | Mean: A = 2.6 C = 3.9 |
Mean (range): 4.7 (1.1-10.5) y | CO2 laser | Endo GIA 30 stapler | 8 |
| C (n = 45) | C (n = 3) | ||||||
| Verhaegen et al,29 2011 | A (n = 72) | A (n = 24) | Not reported | Median (range): 82.3 (7-222) mo [laser]; 19.2 (2-43) mo | CO2 laser | Endo GIA 30 stapler | 9 |
| C (n = 35) | C (n = 9) | ||||||
| Visser et al,30 2016 | A (n = 33) | A (n = 11) | Not reported | Not reported | CO2 laser | Endo GIA stapler | 8 |
| C (n = 42) | C (n = 19) |
Abbreviations: A, laser-assisted approach; B, open approach; C, stapler-assisted approach; NA, not applicable.
All included studies in the network meta-analysis were retrospective cohort studies.
The total number of patients included in the analysis was 903 patients, with individual study enrollment ranging from 14 to 297 patients. There were 283 patients treated with endoscopic laser-assisted diverticulotomy (group A), 150 patients treated with open diverticulectomy with cricopharyngeal myotomy (group B), and 470 patients treated with endoscopic stapler-assisted diverticulotomy (group C).
Risk of Persistent or Recurrent Symptoms
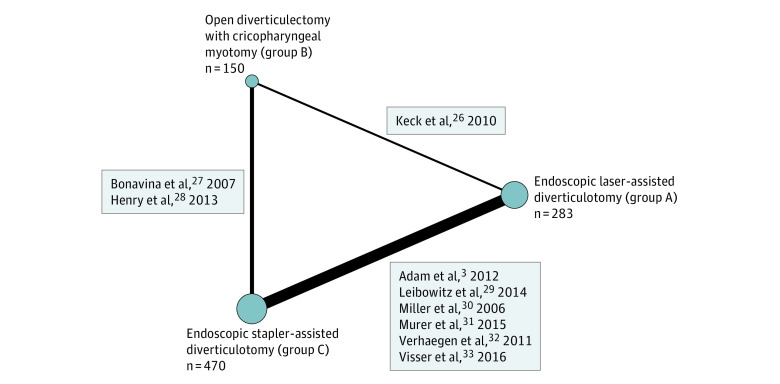
A geometric network was created among the 3 study groups (Figure 23,26,27,28,29,30,31,32,33). The OR for persistent or recurrent symptoms following surgery was calculated using pooled network comparisons. Between endoscopic laser-assisted diverticulotomy (group A) and open diverticulectomy with cricopharyngeal myotomy (group B), the open approach showed a statistically lower likelihood of persistent or recurrent symptoms following treatment (OR, 0.20; 95% CI, 0.04-0.91). Comparing laser-assisted diverticulotomy (group A) with the stapler-assisted technique (group C), the risk of persistent or recurrent symptoms slightly favored the stapler-assisted technique, but this finding was not statistically significant (OR, 0.83; 95% CI, 0.43-1.60). Finally, comparison between the open approach (group B) and stapler-assisted technique (group C) showed increased risk of persistent or recurrent symptoms with the stapler-assisted approach, although this was not statistically significant (OR, 4.10; 95% CI, 0.99-16.97).
Figure 2. Geometry of the Network Meta-analysis.
Nodes are sized proportionally to the cumulative number of patients who underwent each technique. The thickness of each line is proportional to the number of studies included in the comparison.
A forest plot was generated showing individual studies and group comparisons (Figure 33,26,27,28,29,30,31,32,33). Direct comparisons and a pooled network analysis were both performed. The network ORs and CIs are shown.
Figure 3. Forest Plot Comparing 3 Techniques Using Both Direct and Network Comparisons.
Top: The open technique was associated with a decreased likelihood of persistent or recurrent symptoms compared with the stapler-assisted technique (odds ratio [OR], 0.20; 95% CI, 0.04-0.91). Middle: There was no significant difference between the laser-assisted and stapler-assisted techniques (OR, 0.83; 95% CI, 0.43-1.60). Bottom: The stapler-assisted technique demonstrated increased likelihood of persistent or recurrent symptoms, but this was not statistically significant (OR, 4.10; 95% CI, 0.99-16.97).
Test for Consistency
The direct and pooled network ORs were qualitatively compared (Figure 3). In all 3 comparisons, the direct and pooled ORs appeared to be coherent (visually overlapping). Inconsistency tests between the differences in direct and indirect comparisons for each treatment comparison (A vs B, A vs C, and B vs C) were performed (Table 2). No local inconsistency was identified when comparing the direct and indirect estimates. The consistency assumption of the network analysis was quantitatively assessed globally. The null hypothesis was accepted (χ21 = 0.12, P = .73), and the consistency model was supported.
Table 2. Inconsistency Test Between Direct and Indirect Treatment Comparisons Among Multiple Surgical Options.
| Comparisons | Coefficient (SE) | P value | ||
|---|---|---|---|---|
| Direct | Indirect | Difference | ||
| A vs B | −1.10 (1.65) | −1.76 (0.91) | 0.66 (1.89) | .73 |
| A vs C | −0.21 (0.37) | 0.46 (1.85) | −0.66 (1.89) | .73 |
| B vs C | 1.55 (0.84) | 0.89 (1.69) | 0.66 (1.89) | .73 |
Abbreviations: A, laser-assisted approach; B, open approach; C, stapler-assisted approach.
Discussion
This study compared 3 common treatments for ZD using a network meta-analysis. There were no randomized clinical trials included in the meta-analysis, only retrospective cohort studies. Overall, the results suggest that stapler-assisted and laser-assisted techniques have a similar likelihood of postoperative recurrent or persistent symptoms. The open technique was associated with decreased probability of recurrent or persistent symptoms compared with both laser-assisted and stapler-assisted techniques: OR, 0.20; 95% CI, 0.04-0.91; and OR, 0.23; 95% CI, 0.06-1.01; respectively. This translates to the open technique having approximately 20% the likelihood of recurrent or persistent symptoms, compared with the 2 endoscopic techniques. The CIs, however, are fairly wide for both comparisons, suggesting that the decreased odds observed with the open technique could be substantially more modest than the aforementioned effect size.
The principal advantage of performing a network meta-analysis is the ability to simultaneously compare multiple treatments through direct and indirect comparisons. In this study, groups A and C were directly compared using 6 studies. The groups were also indirectly compared using group B because it is a common point of comparison in other studies. Figure 2 establishes the structure of the network geometry. The consistency test helps to determine whether the indirect comparisons are making the same conclusions as the direct comparisons. It is possible for the indirect and direct comparisons to show the opposite direction of effect. This discrepancy may lead the investigator to reject the consistency model and the network analysis.25 In this meta-analysis, however, the consistency model was upheld, further supporting the validity of the network analysis.
There was only 1 study that directly compared the open and laser-assisted approaches.26 This individual study favored the open technique in the primary outcome measure, consistent with the network comparison. There were 2 studies that compared the open and stapler-assisted techniques.27,28 Both studies showed increased likelihood of persistent or recurrent symptoms with the stapler-assisted technique, which was also consistent with the network comparison. When looking at the comparison between stapler-assisted and laser-assisted techniques, the 6 individual studies appeared to be scattered between favoring 1 of the techniques.3,29,30,31,32,33
Among the 9 studies included in our primary meta-analysis, only 5 rated the severity of dysphagia or regurgitation.3,28,29,30,31 Of those, Miller et al,30 Leibowitz et al,29 and Adam et al3 reported both preoperative and postoperative dysphagia and regurgitation. All 3 studies used similar 4-point scales (absent, mild, moderate, severe); however, these scales were not standardized among the studies, making direct comparisons difficult. In addition, Adam et al3 used a previously validated Functional Oral Intake Scale for dysphagia, but the authors modified the scale—condensing it from 7 points to 4 points by combining all gastric-tube dependent or oral diet of single consistency states into 1 value.
Miller et al30 reported a 1.21-point mean reduction in their dysphagia score for the endoscopic stapler cohort and a 1.38-point mean reduction in CO2 laser cohort, but this difference was not statistically significant. Leibowitz et al29 reported similar outcomes to those from Miller et al, with reductions in dysphagia scores of 1.63 and 1.70 for the CO2 laser and endoscopic stapler groups, respectively. Adam et al3 reported a statistical superiority of dysphagia score reduction in the CO2 laser group compared with the stapler-assisted technique (1.97 vs 1.40, respectively). Direct comparisons using the aforementioned dysphagia scales are difficult because there is no uniform measure between the studies. Moving forward, it would be beneficial for future studies to use previously validated dysphagia scales and to report both preoperative and postoperative values.
Limitations
There are clear limitations to this meta-analysis. The decision whether to perform the laser-assisted, stapler-assisted, or open approach at the individual patient level can be influenced by many factors, including age, comorbidities,34 surgeon experience,35 the size of the pouch,36 and patient anatomy,37 but these factors are not consistently reported in each study. This allocation bias may affect the true frequency of recurrent or persistent symptoms following surgery. Studies with larger numbers of patients may have favored a particular technique, and the rates of postoperative recurrent or persistent symptoms may have been affected by studies in which surgeons are more experienced with a particular technique.
The length of follow-up was not uniformly reported. Some of the cohort studies reported lengthier follow-up periods (mean or median, >2 years),27,28,31 while other studies did not specify the length of follow-up.3,26,30 Studies with a shorter follow-up period may be underestimating the risk of recurrence. Some patients may have other pharyngeal or esophageal pathology that persisted even after successful surgery. Persistent dysphagia after surgery could be secondary to another condition, not addressed by the open or endoscopic surgery. Furthermore, the individual study definitions of persistent or recurrent symptoms postoperatively are likely variable.
Henry et al28 did not state specifically that revisions were not included, and attempts to reach out to the authors were unsuccessful. Given the study description, however, it is unlikely that revisions were included. Lastly, the size of the pouch could not be controlled, and some surgeons may have favored specific techniques based on the size of the pouch.3 Among the 6 studies that reported the pouch size, there did not appear to be a large difference in pouch size among the various surgical approaches (Table 1). Because all studies were cohort studies and subject to intrastudy comparison, many study-specific variations affected both arms of the cohort study and likely did not dramatically affect the overall OR.
Ultimately, the choice of surgical approach for treating ZD is based on multiple factors beyond the scope of this meta-analysis. A surgeon may still recommend an endoscopic approach—even with a potentially increased risk of recurrent or persistent symptoms—given a frail or older adult patient.14 This meta-analysis focuses on the likelihood of persistent or recurrent symptoms following surgery, which is an important consideration that should be factored when selecting the best treatment.
Conclusions
A network meta-analysis was developed to compare 3 common treatments for ZD: endoscopic laser-assisted diverticulotomy, open diverticulectomy with cricopharyngeal myotomy, and endoscopic stapler-assisted diverticulotomy. The open approach showed less likelihood of persistent or recurrent symptoms following surgery compared with both endoscopic laser-assisted and stapler-assisted diverticulotomy. The consistency model was supported in the meta-analysis, suggesting validity of the network.
eAppendix. Search strategies
References
- 1.van Overbeek JJ Meditation on the pathogenesis of hypopharyngeal (Zenker’s) diverticulum and a report of endoscopic treatment in 545 patients. Ann Otol Rhinol Laryngol. 1994;103(3):178-185. doi: 10.1177/000348949410300303 [DOI] [PubMed] [Google Scholar]
- 2.Crescenzo DG, Trastek VF, Allen MS, Deschamps C, Pairolero PC. Zenker’s diverticulum in the elderly: is operation justified? Ann Thorac Surg. 1998;66(2):347-350. doi: 10.1016/S0003-4975(98)00502-5 [DOI] [PubMed] [Google Scholar]
- 3.Adam SI, Paskhover B, Sasaki CT. Laser versus stapler: outcomes in endoscopic repair of Zenker diverticulum. Laryngoscope. 2012;122(9):1961-1966. doi: 10.1002/lary.23398 [DOI] [PubMed] [Google Scholar]
- 4.Feeley MA, Righi PD, Weisberger EC, et al. Zenker’s diverticulum: analysis of surgical complications from diverticulectomy and cricopharyngeal myotomy. Laryngoscope. 1999;109(6):858-861. doi: 10.1097/00005537-199906000-00003 [DOI] [PubMed] [Google Scholar]
- 5.Skinner KA, Zuckerbraun L. Recurrent Zenker’s diverticulum: treatment with crycopharyngeal myotomy. Am Surg. 1998;64(2):192-195. [PubMed] [Google Scholar]
- 6.Cook IJ, Blumbergs P, Cash K, Jamieson GG, Shearman DJ. Structural abnormalities of the cricopharyngeus muscle in patients with pharyngeal (Zenker’s) diverticulum. J Gastroenterol Hepatol. 1992;7(6):556-562. doi: 10.1111/j.1440-1746.1992.tb01485.x [DOI] [PubMed] [Google Scholar]
- 7.van Overbeek JJM Pathogenesis and methods of treatment of Zenker’s diverticulum. Ann Otol Rhinol Laryngol. 2003;112(7):583-593. doi: 10.1177/000348940311200703 [DOI] [PubMed] [Google Scholar]
- 8.Little RE, Bock JM. Pharyngoesophageal diverticuli: diagnosis, incidence and management. Curr Opin Otolaryngol Head Neck Surg. 2016;24(6):500-504. doi: 10.1097/MOO.0000000000000309 [DOI] [PubMed] [Google Scholar]
- 9.Bergeron JL, Chhetri DK. Indications and outcomes of endoscopic CO2 laser cricopharyngeal myotomy. Laryngoscope. 2014;124(4):950-954. doi: 10.1002/lary.24415 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Koch M, Mantsopoulos K, Velegrakis S, Iro H, Zenk J. Endoscopic laser-assisted diverticulotomy versus open surgical approach in the treatment of Zenker’s diverticulum. Laryngoscope. 2011;121(10):2090-2094. doi: 10.1002/lary.22152 [DOI] [PubMed] [Google Scholar]
- 11.Stewart K, Sen P. Pharyngeal pouch management: an historical review. J Laryngol Otol. 2016;130(2):116-120. doi: 10.1017/S0022215115002285 [DOI] [PubMed] [Google Scholar]
- 12.Witterick IJ, Gullane PJ, Yeung E. Outcome analysis of Zenker’s diverticulectomy and cricopharyngeal myotomy. Head Neck. 1995;17(5):382-388. doi: 10.1002/hed.2880170504 [DOI] [PubMed] [Google Scholar]
- 13.Vannucci J, Matricardi A, Scarnecchia E, et al. Is myotomy plus diverticulopexy suitable for symptomatic Zenker’s diverticula? Dysphagia. 2019;34(2):240-247. doi: 10.1007/s00455-018-9936-1 [DOI] [PubMed] [Google Scholar]
- 14.Verdonck J, Morton RP. Systematic review on treatment of Zenker’s diverticulum. Eur Arch Otorhinolaryngol. 2015;272(11):3095-3107. doi: 10.1007/s00405-014-3267-0 [DOI] [PubMed] [Google Scholar]
- 15.Shah RN, Slaughter KA, Fedore LW, Huang BY, Deal AM, Buckmire RA. Does residual wall size or technique matter in the treatment of Zenker’s diverticulum? Laryngoscope. 2016;126(11):2475-2479. doi: 10.1002/lary.25975 [DOI] [PubMed] [Google Scholar]
- 16.Smith SR, Genden EM, Urken ML. Endoscopic stapling technique for the treatment of Zenker diverticulum vs standard open-neck technique: a direct comparison and charge analysis. Arch Otolaryngol Head Neck Surg. 2002;128(2):141-144. doi: 10.1001/archotol.128.2.141 [DOI] [PubMed] [Google Scholar]
- 17.Adams J, Sheppard B, Andersen P, et al. Zenker’s diverticulostomy with cricopharyngeal myotomy: the endoscopic approach. Surg Endosc. 2001;15(1):34-37. doi: 10.1007/s004640000323 [DOI] [PubMed] [Google Scholar]
- 18.Johnson CM, Postma GN. Zenker diverticulum—which surgical approach is superior? JAMA Otolaryngol Head Neck Surg. 2016;142(4):401-403. doi: 10.1001/jamaoto.2015.3892 [DOI] [PubMed] [Google Scholar]
- 19.Chan DSY, Foliaki A, Lewis WG, Clark GWB, Blackshaw GRJC. Systematic review and meta-analysis of surgical treatment of non-Zenker’s oesophageal diverticula. J Gastrointest Surg. 2017;21(6):1067-1075. doi: 10.1007/s11605-017-3368-3 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Belafsky PC, Mouadeb DA, Rees CJ, et al. Validity and reliability of the Eating Assessment Tool (EAT-10). Ann Otol Rhinol Laryngol. 2008;117(12):919-924. doi: 10.1177/000348940811701210 [DOI] [PubMed] [Google Scholar]
- 21.Parker NP, Misono S. Carbon dioxide laser versus stapler-assisted endoscopic Zenker’s diverticulotomy: a systematic review and meta-analysis. Otolaryngol Head Neck Surg. 2014;150(5):750-753. doi: 10.1177/0194599814521554 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Hutton B, Catalá-López F, Moher D. La extensión de la declaración PRISMA para revisiones sistemáticas que incorporan metaanálisis en red: PRISMA-NMA. Article in Spanish. Med Clin (Barc). 2016;147(6):262-266. doi: 10.1016/j.medcli.2016.02.025 [DOI] [PubMed] [Google Scholar]
- 23.Stang A Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol. 2010;25(9):603-605. doi: 10.1007/s10654-010-9491-z [DOI] [PubMed] [Google Scholar]
- 24.Jadad AR, Moore RA, Carroll D, et al. Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials. 1996;17(1):1-12. doi: 10.1016/0197-2456(95)00134-4 [DOI] [PubMed] [Google Scholar]
- 25.Shim S, Yoon B-H, Shin I-S, Bae J-M. Network meta-analysis: application and practice using Stata. Epidemiol Health. 2017;39:e2017047. doi: 10.4178/epih.e2017047 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Keck T, Rozsasi A, Grün PM. Surgical treatment of hypopharyngeal diverticulum (Zenker’s diverticulum). Eur Arch Otorhinolaryngol. 2010;267(4):587-592. doi: 10.1007/s00405-009-1079-4 [DOI] [PubMed] [Google Scholar]
- 27.Bonavina L, Bona D, Abraham M, Saino G, Abate E. Long-term results of endosurgical and open surgical approach for Zenker diverticulum. World J Gastroenterol. 2007;13(18):2586-2589. doi: 10.3748/wjg.v13.i18.2586 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Henry MAC, Lerco MM, Tagliarini JV, Castilho EC, Novaes FT, Lamonica VC. Pharyngoesophageal diverticulum: evaluation of treatment results. Rev Col Bras Cir. 2013;40(2):104-109. doi: 10.1590/S0100-69912013000200004 [DOI] [PubMed] [Google Scholar]
- 29.Leibowitz JM, Fundakowski CE, Abouyared M, et al. Surgical techniques for Zenker’s diverticulum: a comparative analysis. Otolaryngol Head Neck Surg. 2014;151(1):52-58. doi: 10.1177/0194599814529405 [DOI] [PubMed] [Google Scholar]
- 30.Miller FR, Bartley J, Otto RA. The endoscopic management of Zenker diverticulum: CO2 laser versus endoscopic stapling. Laryngoscope. 2006;116(9):1608-1611. doi: 10.1097/01.mlg.0000233508.06499.41 [DOI] [PubMed] [Google Scholar]
- 31.Murer K, Soyka MB, Broglie MA, Huber GF, Stoeckli SJ. Zenker’s diverticulum: outcome of endoscopic surgery is dependent on the intraoperative exposure. Eur Arch Otorhinolaryngol. 2015;272(1):167-173. doi: 10.1007/s00405-014-2959-9 [DOI] [PubMed] [Google Scholar]
- 32.Verhaegen VJO, Feuth T, van den Hoogen FJA, Marres HAM, Takes RP. Endoscopic carbon dioxide laser diverticulostomy versus endoscopic staple-assisted diverticulostomy to treat Zenker’s diverticulum. Head Neck. 2011;33(2):154-159. doi: 10.1002/hed.21413 [DOI] [PubMed] [Google Scholar]
- 33.Visser LJ, Hardillo JAU, Monserez DA, Wieringa MH, Baatenburg de Jong RJ. Zenker’s diverticulum: Rotterdam experience. Eur Arch Otorhinolaryngol. 2016;273(9):2755-2763. doi: 10.1007/s00405-015-3825-0 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Van Abel KM, Tombers NM, Krein KA, et al. Short-term quality-of-life outcomes following transoral diverticulotomy for Zenker’s diverticulum: a prospective single-group study. Otolaryngol Head Neck Surg. 2016;154(2):322-327. doi: 10.1177/0194599815616078 [DOI] [PubMed] [Google Scholar]
- 35.McLean TR, Haller CC. Stapled diverticulectomy and myotomy for symptomatic Zenker’s diverticulum. Am J Surg. 2006;192(5):e28-e31. doi: 10.1016/j.amjsurg.2006.08.009 [DOI] [PubMed] [Google Scholar]
- 36.Aiolfi A, Scolari F, Saino G, Bonavina L. Current status of minimally invasive endoscopic management for Zenker diverticulum. World J Gastrointest Endosc. 2015;7(2):87-93. doi: 10.4253/wjge.v7.i2.87 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Zbären P, Schär P, Tschopp L, Becker M, Häusler R. Surgical treatment of Zenker’s diverticulum: transcutaneous diverticulectomy versus microendoscopic myotomy of the cricopharyngeal muscle with CO2 laser. Otolaryngol Head Neck Surg. 1999;121(4):482-487. doi: 10.1016/S0194-5998(99)70242-1 [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
eAppendix. Search strategies