Abstract
Percutaneous needle biopsy is minimally invasive and widely performed. Bleeding is an important complication of needle biopsy. Because the wound created by the needle is small, the recognition of bleeding in the body may be delayed, and this delay can lead to hemorrhagic shock and death. We report two cases of hemorrhagic shock in which the trauma triad of death developed after needle biopsy and the patients required resuscitation and damage control surgery. Needle biopsy is less invasive but cannot stop bleeding, and so surgery should be considered to ensure hemostasis in a compromised patient.
Keywords: Needle biopsy, Damage control surgery, Hemorrhagic shock, Deadly triad
Introduction
Percutaneous needle biopsy is a minimally invasive procedure, but it is associated with some complications [1,2]. Bleeding is common and sometimes leads to hemorrhagic shock and death. After needle biopsy, the wound is extremely small, and so it is easy to overlook bleeding; bleeding is often found after complications ensue. Prolonged hemorrhagic shock causes the trauma triad of death: metabolic acidosis, hypothermia, and coagulopathy [3,4]. Mortality depends on the pathology of bleeding, so it is important to stop bleeding and transfuse before cardiopulmonary arrest. Some patients with cancer already have coagulopathy resulting from the malignant tumor [5]. Therefore, physicians should perform biopsy with caution.
We report two cases of hemorrhagic shock that occurred after percutaneous needle biopsy and necessitated resuscitation. The first case involved shock caused by bleeding after needle biopsy of the liver, and second involved pleural bleeding.
Case 1
A 57-year-old man was admitted to our emergency department with cardiac arrest. The patient was resuscitated by advanced life support and underwent veno-arterial extracorporeal membrane oxygenation because we were suspected acute coronary syndrome at admission. At presentation, however, his hemoglobin level was 5.8 g/dL, and his fibrinogen level was 145 mg/dL; blood gas tests showed a pH 6.74 and a lactate level of 17.4 mmol/L. We were strongly suspected that the pathology of bleeding somewhere in his body caused cardiac arrest. Moreover, his body temperature was not abnormal, but lactate acidosis and coagulopathy had already occurred; thus, two components of the trauma deadly triad of death were present.
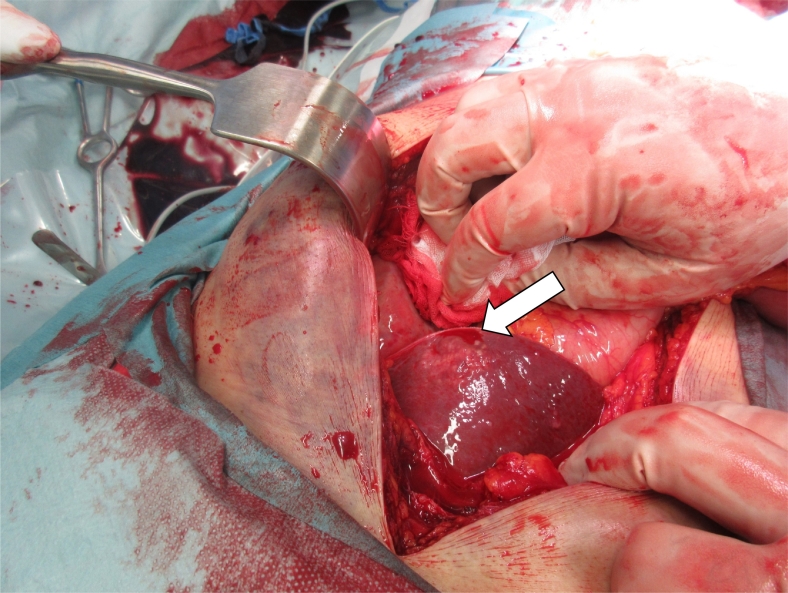
After resuscitation, from his family, we got his medical history that he had undergone needle biopsy of the liver to scrutinize cancer, the primary lesion of which was unknown, at another general hospital. Because the patient was examined at another hospital, information about him was sparse. We performed laparotomy to achieve hemostasis of the liver injury. The bleeding was in the lateral area of the liver (Fig. 1.). Hemostasis was achieved and gauze packing was performed; then we performed damage control surgery and open abdomen. Two days later, however, he could not be resuscitated.
Fig. 1.
Confirmed bleeding from the lateral portion of the liver. The bleeding site (white arrow) was closed with sutures and an electric device, but the closure was difficult because the patient had coagulopathy.
Case 2
A 57-year-old man was admitted to our emergency department with right massive hemothorax that developed in another hospital. The patient had undergone needle biopsy of the pleura to examine bilateral pleural effusion of uncommon cause. Shortly after his arrival at our hospital, cardiac arrest occurred, and the patient needed advanced life support. We performed right thoracotomy and confirmed a bleeding point from right dorsal fifth intercostal artery (Fig. 2, Fig. 3). At surgery, his hemoglobin level was 4.6 g/dL, and his fibrinogen level was 83 mg/dL; blood gas tests showed a pH of 7.04 and a lactate level of 17.4 mmol/L. In addition, body temperature was 32.1 °C; thus, he already had all the components of the trauma deadly triad. Due to unstable condition, we decided to perform damage control surgery and gauze packing at the bleeding point and temporarily close the chest wall.
Fig. 2.
Right thoracotomy was performed because of posterior pleural bleeding. A large amount of blood and many clots were observed.
Fig. 3.
Confirmed bleeding from the posterior pleura. The bleeding site was closed with sutures, and the bleeding was stopped. In this photograph, the tip of the suction is at the bleeding point.
After 2 days, we verified hemostasis and closed the patient's chest. He survived, and a month after admission to our hospital, he was transferred to the previous hospital.
Discussion
Percutaneous needle biopsy is less invasive than surgical biopsy, and some of its complications, such as bleeding, infection, peritonitis, pleural injury, and pain, are more likely to be overlooked [[6], [7], [8]]. The most dangerous complication in liver biopsy is bleeding. The previous reports showed that the rate of bleeding complications was 1%–6% in cases of mild liver disease without transfusion and 0%–5% in cases of moderate to severe liver disease with transfusion or intervention, and the mortality rate was approximately 0.5% or less [6]. On the other hand, common and serious complications of thoracic needle biopsy include not only bleeding but also pneumothorax. Pneumothorax was the most common complication according to two reports, occurring in 35% of patients who underwent thoracic needle biopsy [8,9]. The mortality rate was between 0.02% and 0.15% [8,9]. Biopsy is performed in order to examine in detail malignant diseases that have caused coagulopathy [5]. With coagulation disorders, even small amounts of bleeding, such as that caused by needle biopsy, do not cease spontaneously and are difficult to stop, and they can cause hemorrhagic shock and death.
In patients with liver tumor or hepatitis, needle biopsy carries a high risk of certain complications [6,7]. In case 1, biopsy of the lateral hepatic segment, which is anatomically anchored loosely and contains less liver parenchyma, increases the risk of bleeding (Fig. 4). In such cases at risk, procedures other than needle biopsy should be considered, such as endoscopic ultrasound-guided biopsy and laparoscopy [[10], [11], [12]]. The latest report showed that endoscopic ultrasound-guided biopsy by using 22-gauge needly was safety method and good inspection accuracy [12]. Surgery such as laparoscopy and sufficient hemostasis are especially important for patients with bleeding tendencies. We think that understanding of the patient's general condition and careful consideration of the most suitable examination method will help reduce rates of complications and mortality.
Fig. 4.
Abdominal computed tomographic image, which was ordered from another hospital at a later date, showed a mass in the lateral portion of the liver. Cancer was diagnosed; the primary neoplasm was unknown. In the other hospital, percutaneous needle biopsy had been performed to determine the primary cancer.
The life-threatening complication of percutaneous transthoracic biopsy is hemothorax, as occurs with intercoastal artery damage [[7], [8], [9]]. In case 2, the biopsy was performed from posterior fifth intercostal space, which resulted in vascular injury. Because lateral perforators arise from the posterior intercostal arteries in approximately 30% of people [13], the biopsy from posterior positions involves the risk of artery damage. In addition, because the risk of complications of biopsy is high, physicians should consider performing it in tertiary care hospitals, in which bleeding can be stopped quickly by emergency surgery or transcatheter arterial embolization.
In our two patients, the discovery of bleeding was delayed because the bleeding points were in the abdomen and the thorax. As a result of lengthy continuous bleeding, the trauma deadly triad had appeared in these patients. Our strategy of damage control surgery and intensive care saved the patient in case 2 but not the patient in case 1. The patient in case 1 had cancer of unknown primary. Cancer is sometimes complicated by the occurrence of disseminated intravascular coagulation (DIC) [14]. Due to exhaustion of platelets and coagulation factors in gradual proceeding DIC, the patient in case 1 probably led to have coagulopathy. Even in the presence of excessive coagulopathy, a patient could be saved if hemostasis is reliably obtained in the proper biopsy method. In both cases, biopsy and treatment for primary disease was performed at other hospitals, and our report have major limitation since there were no detailed medical records, blood examinations, and pathological biopsy results.
Conclusion
Our two patients suffered bleeding shock after percutaneous needle biopsy and required damage control surgery. Needle biopsy is minimally invasive, but sometimes it causes bleeding, and surgery may be necessary to achieve hemostasis, depending on the condition of the patient.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Declaration of competing interest
None.
References
- 1.Boyum J.H., Atwell T.D., Schmit G.D. Incidence and risk factors for adverse events related to image-guided liver biopsy. Mayo Clin. Proc. 2016;91:329–335. doi: 10.1016/j.mayocp.2015.11.015. [DOI] [PubMed] [Google Scholar]
- 2.Mueller M., Kratzer W., Oeztuerk S. Percutaneous ultrasonographically guided liver punctures: an analysis of 1961 patients over a period of ten years. BMC Gastroenterol. 2012;12:173. doi: 10.1186/1471-230X-12-173. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Davis J.W., Mackersie R.C., Holbrook T.L., Hoyt D.B. Base deficit as an indicator of significant abdominal injury. Ann. Emerg. Med. 1991 Aug;20(8):842–844. doi: 10.1016/s0196-0644(05)81423-4. [DOI] [PubMed] [Google Scholar]
- 4.Ferrara A., MacArthur J.D., Wright H.K., Modlin I.M., McMillen M.A. Hypothermia and acidosis worsen coagulopathy in the patient requiring massive transfusion. Am. J. Surg. 1990 Nov;160(5):515–518. doi: 10.1016/s0002-9610(05)81018-9. [DOI] [PubMed] [Google Scholar]
- 5.Patel H.K., Khorana A.A. Anticoagulation in cancer patients: a summary of pitfalls to avoid. Curr. Oncol. Rep. 2019;21(2):18. doi: 10.1007/s11912-019-0767-5. [DOI] [PubMed] [Google Scholar]
- 6.Rockey D., Caldwell S., Goodman Z. Liver biopsy. Hepatology. 2009;49:1017–1044. doi: 10.1002/hep.22742. [DOI] [PubMed] [Google Scholar]
- 7.Veltri A., Bargellini I., Giorgi L. CIRSE guidelines on percutaneous needle biopsy (PNB) Cardio Vascular and Interventional Radiology. 2017;40(10):1501–1513. doi: 10.1007/s00270-017-1658-5. [DOI] [PubMed] [Google Scholar]
- 8.Guo Z., Shi H., Li W. Chinese multidisciplinary expert consensus: guidelines on percutaneous transthoracic needle biopsy. Thoracic Cancer. 2018;9(11):1530–1543. doi: 10.1111/1759-7714.12849. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Tomiyama N., Yasuhara Y., Nakajima Y. CT-guided needle biopsy of lung lesions: a survey of severe complication based on 9783 biopsies in Japan. Eur. J. Radiol. 2006;59(1):60–64. doi: 10.1016/j.ejrad.2006.02.001. [DOI] [PubMed] [Google Scholar]
- 10.Diehl D., Johal A., Khara H. Endoscopic ultrasound-guided liver biopsy: a multicenter experience. Endoscopy International Open. 2015;3(03):E210–E215. doi: 10.1055/s-0034-1391412. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Denzer U. Liver assessment and biopsy in patients with marked coagulopathy: value of mini-laparoscopy and control of bleeding. Am. J. Gastroenterol. 2003;98(4):893–900. doi: 10.1111/j.1572-0241.2003.07342.x. [DOI] [PubMed] [Google Scholar]
- 12.Hasan M.K., Kadkhodayan K., Idrisov E., Ali S., Rafiq E., Ben-Ami Shor D., Abdel-Jalil A., Navaneethan U., Bang J., Varadarajulu S., Hawes R., Pernicone P. Endoscopic ultrasound-guided liver biopsy using a 22-G fine needle biopsy needle: a prospective study. Endoscopy. 2019;51(9):818–824. doi: 10.1055/a-0967-3640. [DOI] [PubMed] [Google Scholar]
- 13.Jeon E.Y., Cho Y.K., Yoon D.Y. Angiographic analysis of the lateral intercostal artery perforator of the posterior intercostal artery: anatomic variation and clinical significance. Diagn. Interv. Radiol. 2015;21(5):415–418. doi: 10.5152/dir.2015.15096. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Levi M. Management of cancer-associated disseminated intravascular coagulation. Thromb. Res. 2016;140:S66–S70. doi: 10.1016/S0049-3848(16)30101-3. [DOI] [PubMed] [Google Scholar]