In the last 40 years, self–blood glucose monitoring (BGM) has revolutionized the treatment of type 1 diabetes mellitus (T1DM). Glaser et al1 reported that lack of understanding of and/or frustration with complexity of insulin dose calculations may contribute to poor adherence to insulin regimes and consequently suboptimal metabolic control in T1DM.
At a general practice level we found that there is a variation in BGM strip analytical performance.2 Furthermore, we recently showed a link between blood glucose meter accuracy and an established qualitative error grid (Parkes’ Grid), highlighting the potential impact of BGM strip precision on clinical decision making/glycemic outcomes.3,4
In this study, we collected patient views about their experience of self-BGM, including confidence in the equipment, and how this relates to the day-to-day experience of managing T1DM.
In an online survey, we asked people with T1DM about their experience of BGM day-to-day and how this influences decisions around insulin dosing. We also examined how patients feel/behave in relation to this.
Patients agreed to take part through our “Research for the Future” program. In total, 116 individuals completed the survey (29% response rate).
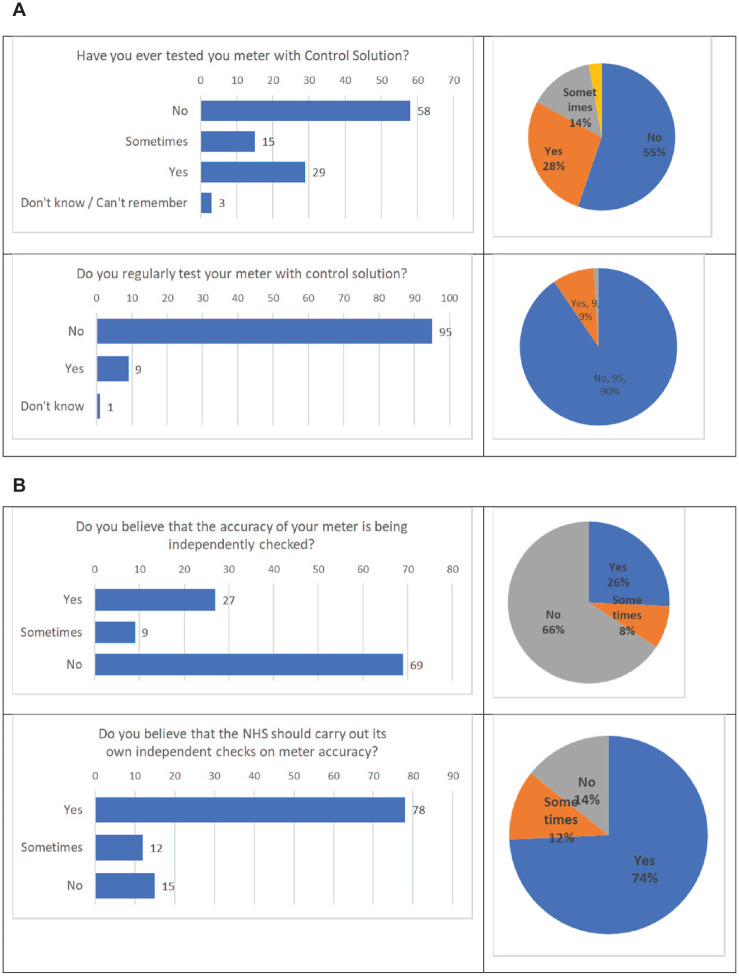
Of those who responded, 42% did not remember being trained on their meter. Fifty-five percent had not ever checked meter performance using control solution (Figure 1a) and 90% did not regularly use control solution. Eight-five percent were unaware of international accuracy standards (International Standards Organization).5 A minority of respondents (20%) said they had discussed accuracy with other people with diabetes or healthcare professionals. Sixty-three percent of patients reported glycosylated hemoglobin results ≤64 mmol/mol.
Figure 1.
BGM meter accuracy: patient views on (a) use of control solution and (b) BGM meter performance checking in the United Kingdom. BGM, blood glucose monitoring.
As many as 34% of people believed that the accuracy of their meter was being independently checked by an external agency and 86% said that the National Health Service should conduct independent checks on meter accuracy (Figure 1b).
The study sample comprised long-term engaged people who have better glycemic control than national average, but even within this group there was significant variation in behavior/understanding, including (a) awareness of the long-term risks of not calibrating the BG meter and (b) confidence in external agencies ensuring optimal BG meter performance.
Our survey revealed under appreciation of the importance of meter precision and an unfounded level of confidence that processes underpinning BGM device precision/accuracy are robust. There was lack of understanding of the need to perform control checks. In contrast, there was strong belief that the health system should protect people with T1DM, including ensuring that the key equipment for BGM is fit for purpose.
In T1DM, in situ blood glucose monitors, such as the FreeStyle Libre flash monitor,6 are increasingly being utilized by people with insulin treated diabetes. Nevertheless traditional BGM will continue to be the way that most people who take insulin monitor their diabetes.
Our survey highlights lack of understanding, even among the most engaged people, and shows areas where changes in education/support regarding BGM meters might benefit all people with T1DM.
Footnotes
Declaration of Conflicting Interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: The author(s) received no financial support for the research, authorship, and/or publication of this article.
ORCID iDs: Stephen Brown  https://orcid.org/0000-0003-3715-580X
https://orcid.org/0000-0003-3715-580X
Adrian H. Heald  https://orcid.org/0000-0002-9537-4050
https://orcid.org/0000-0002-9537-4050
References
- 1. Glaser NS, Iden SB, Green-Burgeson D, et al. Benefits of an insulin dosage calculation device for adolescents with type 1 diabetes mellitus. J Pediatr Endocrinol Metab. 2004;17:1641-1651. [DOI] [PubMed] [Google Scholar]
- 2. Heald AH, Livingston M, Fryer A, et al. Real-world practice level data analysis confirms link between variability within Blood Glucose Monitoring Strip (BGMS) and glycosylated haemoglobin (HbA1c) in Type 1 Diabetes. Int J Clin Pract. 2018;72:e13252. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Stedman M, Rea R, Duff CJ, et al. Applying Parkes Grid method to evaluate impact of variation in Blood Glucose Monitoring (BGM) Strip accuracy performance in Type 1 Dia-betes highlights the potential for amplification of imprecision with less accurate BGM strips. J Diabetes Sci Technol. 2021;15:76-81. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Heald AH, Livingston M, Fryer A, et al. Route to improving Type 1 diabetes mellitus glycaemic outcomes: real-world evidence taken from the National Diabetes Audit. Diabet Med. 2018;35:63-71. [DOI] [PubMed] [Google Scholar]
- 5. International Organization for Standardization 15197. In vitro Diagnostic Test Systems – Requirements for Blood-Glucose Monitoring Systems for Self-testing in Managing Diabetes Mellitus. Geneva, Switzerland: International Organization for Standardization; 2013. [Google Scholar]
- 6. Kalra S, Gupta Y. Ambulatory glucose profile: flash glucose monitoring. J Pak Med Assoc. 2015;65:1360-1362. [PubMed] [Google Scholar]