Abstract
We investigated the cardiovascular complications and mortality rates of patients with diabetes in South Korea. The rates of hospitalization due to cardiovascular complications and mortality were analyzed using the Korean National Health Insurance Service-National Sample Cohort. From 2006 to 2015, the rates of hospitalization due to major cardiovascular complications decreased, while those due to heart failure (from 72 to 146 and 124 to 161 per 10,000 men and women, respectively) and peripheral artery disease (from 39 to 55 and 19 to 35 per 10,000 men and women, respectively) increased. In the period 2007 to 2015, the mortality rates for cancer, cerebrovascular disease, diabetes, heart disease, and hypertensive disease all decreased. However, the mortality rate for pneumonia increased. We observed a continuous reduction in cardiovascular complications and mortality in adults with diabetes. However, with the increase in some diabetes complications, more efforts are needed to prevent diabetes complications.
Keywords: Diabetes mellitus, Cardiovascular disease, Epidemiology, Mortality
Graphical abstract
INTRODUCTION
Diabetes is known to be associated with cardiovascular disease (CVD) morbidity and mortality [1]. Unlike the increased prevalence of diabetes itself, the incidence of CVD and CVD-related mortality among patients with diabetes have decreased significantly over the past two decades [2].
This study was aimed to investigate the rates of cardiovascular complications and mortality among Korean adults (aged ≥30 years) with diabetes by analyzing the data of the National Health Insurance Service-National Sample Cohort (NHIS-NSC).
METHODS
Data source and study design
The NHIS-NSC enrolled 1,021,208 individuals (2.2% of the total eligible Korean population in 2006) using a systematic sampling method. Detailed information on the NHIS-NSC can be found elsewhere [3]. The protocol of this study was approved by the Institutional Review Board of Ajou University Hospital, Suwon, Korea (approval No. AJIRB-MED-EXP-19-347) and the requirement for informed consent was waived.
For each calendar year, we identified individuals with diabetes aged 30 years or older. Diabetes was defined as diagnosed with E10–E14 codes of the 10th edition of the International Classification of Diseases (ICD-10) more than twice, or when a patient had a prescription for oral glucose-lowering medications (Anatomical Therapeutic Chemical [ATC] code A10B) for more than 30 days, or (in outpatients) a prescription for insulin (ATC code A10A).
Definitions of cardiovascular complications and mortality
We identified patients hospitalized due to six diabetes-related cardiovascular complications, namely ischemic heart disease, myocardial infarction, heart failure, hemorrhagic stroke, ischemic stroke, and peripheral artery disease (PAD), based on ICD-10 and procedure codes that contributes to clinically hospitalizations regardless of the principal reason for hospitalization (Supplementary Table 1). Information on the date and underlying cause of death was obtained from the National Death Registry using unique resident registration numbers. Causes of death were identified based on ICD-10 codes. There were six mutually exclusive cause of death categories (Supplementary Table 1).
Statistical analysis
We calculated the rates of hospitalization due to cardiovascular complications separately for each year by dividing the number of patients hospitalized for cardiovascular complications by the corresponding number of patients with diabetes for that year. For each calendar year, hospitalization rates were expressed as age-standardized rates per 10,000 individuals; mortality rates were expressed as age-standardized rates per 100,000 individuals, separately for men and women. The rates were age-standardized according to the weighted distribution of the 2011 population, across sexes and 5-year age groups from 30 to 34 years up to 85 years and above. All statistical analyses were performed using SAS software version 9.4 (SAS Institute Inc., Cary, NC, USA).
RESULTS
Hospitalization rate for cardiovascular complications
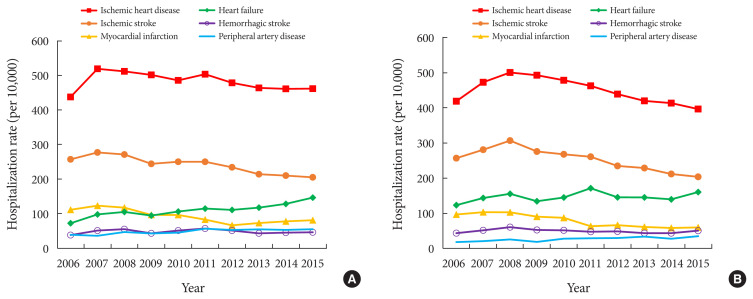
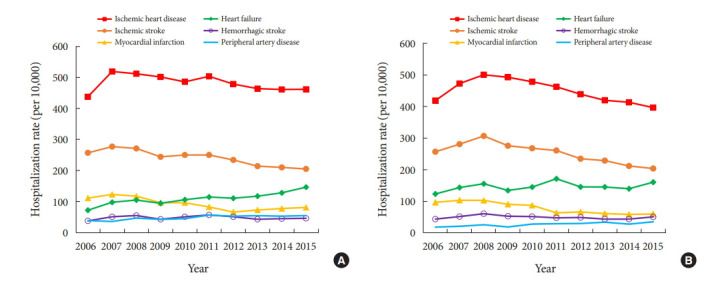
In the period 2006 to 2015, the hospitalization rates due to major cardiovascular complications (ischemic heart disease, ischemic stroke, and myocardial infarction) all decreased. There was a decreasing trend in ischemic heart disease rates (from 438 to 461 and 419 to 397 per 10,000 men and women with diabetes, respectively), ischemic stroke rates (from 257 to 205 and 257 to 204 per 10,000 men and women with diabetes, respectively), and myocardial infarction rates (from 111 to 81 and 97 to 60 per 10,000 men and women with diabetes, respectively). There was a slight increase in the hemorrhagic stroke rates (from 38 to 46 and 44 to 51 per 10,000 men and women with diabetes, respectively) (Fig. 1, Supplementary Table 2).
Fig. 1.
Rates of hospitalization due to cardiovascular complications among men (A) and women (B) with diabetes in South Korea (2006 to 2015).
However, increasing rates of heart failure (from 72 to 146 and 124 to 161 per 10,000 men and women with diabetes, respectively) and PAD (from 39 to 55 and 19 to 35 per 10,000 men and women with diabetes, respectively) were seen (Fig. 1, Supplementary Table 2). The hospitalization rates for revascularization slightly decreased or remained the same (percutaneous coronary intervention, from 97 to 95 and 56 to 50 per 10,000 men and women with diabetes, respectively; coronary artery bypass surgery from 11 to 7 and 4 to 4 per 10,000 men and women with diabetes, respectively) (Supplementary Table 2).
Mortality rate and cause of death in patients with diabetes
In 2007 to 2015, the mortality rate decreased in both men and women (from 2,599 to 2,010 and 1,939 to 1,662 per 100,000 adults with diabetes, respectively) (Supplementary Table 3). The mortality rates for cancer, cerebrovascular disease, diabetes, heart disease, and hypertensive disease decreased in both men and women. However, the mortality rates due to pneumonia increased in both men and women (from 22 to 93 and 34 to 79 per 100,000 adults with diabetes, respectively) (Fig. 2, Supplementary Table 3).
Fig. 2.
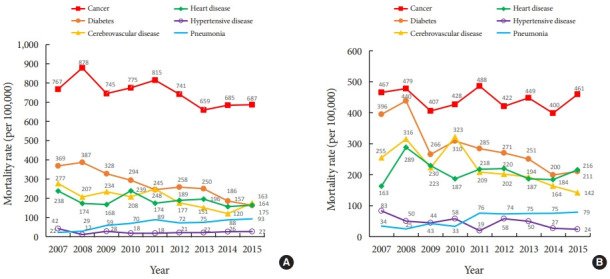
Mortality rates among men (A) and women (B) with diabetes in South Korea (2007 to 2015).
"Updated on 25 March 2021"
In 2015, the six leading causes of death accounted for 66.7% of all deaths in Korean adults with diabetes (cancer, 30.3%; diabetes, 10.5%; heart disease, 10.5%; cerebrovascular disease, 8.9%; pneumonia, 5.0%; and hypertensive disease, 1.5%) (Supplementary Fig. 1). The five most common causes of cancer deaths were lung, liver, colorectal, pancreas, and stomach cancer (Supplementary Table 4).
DISCUSSION
The rates of hospitalization due to major cardiovascular complications and deaths caused by vascular disease and cancer decreased among adult (aged ≥30 years) with diabetes in Korea. These findings are consistent with previous study in Korea [4]. In patients with diabetes, the proportion of patients with good glycemic control remains less than half of them, while the proportion of patients with extremely poor glycemic control is dramatically decreasing [5]. In addition, the overall improvement of cardiovascular risk factors management such as blood pressure, smoking, and lipid level and proper treatment of cardiovascular events and the regular national cancer screening program in Korea is related with the decrease in mortality in patients with diabetes [6–9].
The hospitalization rate for heart failure increased. Better preventive treatments of cardiovascular risk factors may also have contributed to the reduced risk of developing heart failure [10]. However, paradoxically, due to ageing and the development of treatments that allow increased survival after acute heart insults or with chronic cardiac abnormalities, number of patients with heart failure increased [11]. In Korea, appropriate treatment by the certification system for cardiovascular intervention institute/specialist since 2011, efforts to improve awareness of early symptoms, decreasing of the proportion of ST-elevation myocardial infarction led to a decrease in the case-fatality in hospitalized acute myocardial infarction patients from 2007 to 2016 [12]. Also, according to the Korean hospitalized heart failure registry, the development of cardiovascular treatment has increased the survival rate of acute coronary syndrome, as a result, ischemic heart disease is a major cause of hospitalized for heart failure [13]. In addition, the prevalence of heart failure increased with age, and the proportion of patients with diabetes has increased [13,14].
PAD also increased slightly. Recent meta-analysis reported that the prevalence of PAD increased from 2000 to 2010 in high-income countries due to an ageing population [15]. However, in this study, the outcome events were ascertained from health insurance claims data, and diagnoses were not adjudicated by medical records. In addition, using diagnoses code will tend to result in higher observed incidence and prevalence. Thus, to increase accuracy of diagnoses in claim database, we restricted patients undergoing PAD-related procedures and surgery.
Recently, the advance of new technology of peripheral angiography has led to an increase of PAD-related procedures and surgery. Thus, the increase of PAD is partly due to the diagnosis of hidden patients with PAD. In Korea, using the database of the NHIS, amputation involving diabetic foot based on vascular interventions for PAD steadily increased from 2011 to 2016, particularly in minor amputations [16]. During the study period from 2004 to 2013, endovascular revascularization including balloon angioplasty, stent placement, and percutaneous atherectomy increased, while open revascularization such as bypass with artificial graft and autologous vein decreased. This study suggested that the endovascular revascularization for PAD treatment expanded by ageing, increasing number of patients with diabetes and chronic kidney disease on hemodialysis—risk factors for the development of PAD, and repeated interventions for maintaining reasonable clinical outcomes [17].
Deaths from pneumonia also increased. The increased risk of intensive care unit hospitalization and death due to pneumonia in diabetes patients have been reported [18]. In diabetes, impaired immune response is associated with hyperglycemia, and hospitalization for hyperglycemia has been shown to increase the risk of pneumonia-related mortality [19,20].
In conclusion, the present study revealed a decrease in the rates of cardiovascular complications and mortality, among Korean adults with diabetes, which may reflect advances in diabetes care. However, the hospitalization rates for heart failure and PAD and the mortality rates for pneumonia increased. Thus, more efforts are needed to prevent diabetes complications.
Acknowledgments
This study used NHIS data (NHIS-2020-2-110) made by National Health Insurance Service (NHIS). The authors declare no conflict of interest with NHIS. The authors declare no conflict of interest with NHIS.
Some of the data was released in October 2019 in the form of ‘Diabetes & Complications in Korea’ from the Korean Diabetes Association. We would like to thank the Committee of Public Relation, Korean Diabetes Association for helping with the work.
Footnotes
CONFLICTS OF INTEREST
No potential conflict of interest relevant to this article was reported.
AUTHOR CONTRIBUTIONS
Conception or design: B.Y.K., J.H.L., D.J.K.
Acquisition, analysis, or interpretation of data: J.H.P., K.H.H., D.J.K.
Drafting the work or revising: J.H.P., K.H.H., B.Y.K., J.H.L., D.J.K.
Final approval of the manuscript: J.H.P., K.H.H., D.J.K.
FUNDING
None
SUPPLEMENTARY MATERIALS
Supplementary materials related to this article can be found online at https://doi.org/10.4093/dmj.2020.0175.
Codes of diagnoses and procedures
Rates of hospitalization due to cardiovascular complications per 10,000 adults with diabetes
Mortality rates per 100,000 adults with diabetes
Most common causes of death as a proportion of all deaths among patients with diabetes in 2015
Most common causes of death as a proportion of all deaths among patients with diabetes in 2015.
REFERENCES
- 1.Matheus AS, Tannus LR, Cobas RA, Palma CC, Negrato CA, Gomes MB. Impact of diabetes on cardiovascular disease: an update. Int J Hypertens. 2013;2013 doi: 10.1155/2013/653789. 653789. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Rawshani A, Rawshani A, Franzen S, Eliasson B, Svensson AM, Miftaraj M, et al. Mortality and cardiovascular disease in type 1 and type 2 diabetes. N Engl J Med. 2017;376:1407–18. doi: 10.1056/NEJMoa1608664. [DOI] [PubMed] [Google Scholar]
- 3.Lee J, Lee JS, Park SH, Shin SA, Kim K. Cohort profile: the National Health Insurance Service-National Sample Cohort (NHIS-NSC), South Korea. Int J Epidemiol. 2017;46:e15. doi: 10.1093/ije/dyv319. [DOI] [PubMed] [Google Scholar]
- 4.Jung CH, Chung JO, Han K, Ko SH, Ko KS, Park JY, et al. Improved trends in cardiovascular complications among subjects with type 2 diabetes in Korea: a nationwide study (2006–2013) Cardiovasc Diabetol. 2017;16:1. doi: 10.1186/s12933-016-0482-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Ha KH, Kim DJ. Current status of managing diabetes mellitus in Korea. Korean J Intern Med. 2016;31:845–50. doi: 10.3904/kjim.2016.253. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.OECD. Cardiovascular disease and diabetes: policies for better health and quality of care. Available from: https://www.oecd.org/publications/cardiovascular-disease-and-diabetes-policies-for-better-health-and-quality-of-care-9789264233010-en.htm(cited 2020 Oct 26)
- 7.Chang Y, Kang HY, Lim D, Cho HJ, Khang YH. Long-term trends in smoking prevalence and its socioeconomic inequalities in Korea, 1992–2016. Int J Equity Health. 2019;18:148. doi: 10.1186/s12939-019-1051-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Kang SH, Kim SH, Cho JH, Yoon CH, Hwang SS, Lee HY, et al. Prevalence, awareness, treatment, and control of hypertension in Korea. Sci Rep. 2019;9:10970. doi: 10.1038/s41598-019-46965-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Son M, Yun JW. Cancer mortality projections in Korea up to 2032. J Korean Med Sci. 2016;31:892–901. doi: 10.3346/jkms.2016.31.6.892. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Canto JG, Kiefe CI, Rogers WJ, Peterson ED, Frederick PD, French WJ, et al. Number of coronary heart disease risk factors and mortality in patients with first myocardial infarction. JAMA. 2011;306:2120–7. doi: 10.1001/jama.2011.1654. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Chen J, Normand SL, Wang Y, Krumholz HM. National and regional trends in heart failure hospitalization and mortality rates for Medicare beneficiaries, 1998–2008. JAMA. 2011;306:1669–78. doi: 10.1001/jama.2011.1474. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Kim RB, Kim HS, Kang DR, Choi JY, Choi NC, Hwang S, et al. The trend in incidence and case-fatality of hospitalized acute myocardial infarction patients in Korea, 2007 to 2016. J Korean Med Sci. 2019;34:e322. doi: 10.3346/jkms.2019.34.e322. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Youn JC, Han S, Ryu KH. Temporal trends of hospitalized patients with heart failure in Korea. Korean Circ J. 2017;47:16–24. doi: 10.4070/kcj.2016.0429. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Lee JH, Lim NK, Cho MC, Park HY. Epidemiology of heart failure in Korea: present and future. Korean Circ J. 2016;46:658–64. doi: 10.4070/kcj.2016.46.5.658. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Song P, Rudan D, Zhu Y, Fowkes FJI, Rahimi K, Fowkes FGR, et al. Global, regional, and national prevalence and risk factors for peripheral artery disease in 2015: an updated systematic review and analysis. Lancet Glob Health. 2019;7:e1020–30. doi: 10.1016/S2214-109X(19)30255-4. [DOI] [PubMed] [Google Scholar]
- 16.Kim J, Chun DI, Kim S, Yang HJ, Kim JH, Cho JH, et al. Trends in lower limb amputation in patients with diabetic foot based on vascular intervention of peripheral arterial disease in Korea: a population-based nationwide study. J Korean Med Sci. 2019;34:e178. doi: 10.3346/jkms.2019.34.e178. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Park YY, Joh JH, Han SA, Kim SH, Cho S, Park HC, et al. National trends for the treatment of peripheral arterial disease in Korea between 2004 and 2013. Ann Surg Treat Res. 2015;89:319–24. doi: 10.4174/astr.2015.89.6.319. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Kim EJ, Ha KH, Kim DJ, Choi YH. Diabetes and the risk of infection: a national cohort study. Diabetes Metab J. 2019;43:804–14. doi: 10.4093/dmj.2019.0071. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Koh GC, Peacock SJ, van der Poll T, Wiersinga WJ. The impact of diabetes on the pathogenesis of sepsis. Eur J Clin Microbiol Infect Dis. 2012;31:379–88. doi: 10.1007/s10096-011-1337-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.van Vught LA, Wiewel MA, Klein Klouwenberg PM, Hoogendijk AJ, Scicluna BP, Ong DS, et al. Admission hyperglycemia in critically ill sepsis patients: association with outcome and host response. Crit Care Med. 2016;44:1338–46. doi: 10.1097/CCM.0000000000001650. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Codes of diagnoses and procedures
Rates of hospitalization due to cardiovascular complications per 10,000 adults with diabetes
Mortality rates per 100,000 adults with diabetes
Most common causes of death as a proportion of all deaths among patients with diabetes in 2015
Most common causes of death as a proportion of all deaths among patients with diabetes in 2015.