Abstract
Background
Medical education has observed numerous reforms in the last hundred years. While most of the reforms are applied to the undergraduate teaching, postgraduate education and training have lagged behind in keeping the pace. Anesthesiology curriculum has witnessed a few new methods inducted into practice like problem-based learning, flipped classroom etc. We introduced vertical integration with anatomy at our department and assessed its impact.
Methods
After a five-week schedule of integrated anatomy classes, a self-structured questionnaire was circulated amongst the 41 anesthesiology residents to know their perceptions and attitudes towards the classes. Their suggestions were also sought. The responses were analyzed with descriptive statistics (percentages).
Results
Thirty-six responses were received leading to a response rate of 87.8%. Fourteen residents (38.9%) believed that the integrated classes would be very helpful in their clinical practice, 20 (55.5%) residents believed them to be helpful while two (5.5%) residents believed that the classes would be little helpful in clinical practice. Hundred percent of the residents recommended the classes to be continued for the future batches. Half of the residents wanted the classes to be conducted twice in the three-year tenure (in the first and last semester) while 11 (30.5%) residents wanted the classes to be conducted every year. Seven (19.4%) residents thought that it's enough to conduct the classes once during the three-year tenure. Resident's suggested that they would like to have integrated classes with other departments like physiology, radiology, emergency medicine etc.
Conclusion
The integrated classes with anatomy were well perceived by the anesthesiology residents. Vertically integrated curriculum should be introduced in postgraduate training of various specialties for better education and hence, better patient care.
Keywords: Medical education, Anesthesiology training, Vertical integration, Basic sciences, Anesthesiology education
Introduction
In 1910, Abraham Flexner presented the concept of modern medical education emphasizing that students should first study the basic and biomedical subjects and the clinical subjects should follow next.1 However, this concept has frequently been criticized for dissociating basic sciences from clinical sciences.2 It is advocated that medical education should place basic science education well in the context of clinical practice.3,4 Medical education has seen major reforms in the recent decades using various methods like integration, problem-based learning, flipped classroom, unconventional learning etc.5, 6, 7 Integration in medical education is defined as “the organisation of teaching matter to interrelate or unify subjects frequently taught in separate academic courses or departments”.8 This organisation can occur across a wide spectrum of time period or depth of topics within a subject or amongst different subjects.9 Concepts of integration should be clear with the medical educators prior to its implementation in the curriculum.10 Integration in medical education is increasingly being adopted worldwide.
National Medical Commission (NMC) in India has advocated implementation of competency-based curriculum in undergraduate medical education which will be achieved in step-wise manner. As a part of Curriculum Implementation Support Program, a module on alignment and integration for undergraduate medical education program has been released in 2019 which details the goals and steps involved in implementation of integrated curriculum.11
Anesthesiology is a medical specialty the services of which are required in many areas of a clinical set up. The curriculum in anesthesiology has to fulfil the diverse requirements of the specialty ranging from procedural skills, maintaining the physiology, understanding the pathology of the patient to understanding the surgical challenges in the patient. Similar requirements are there in the intensive care units (ICU). Anaesthesia training and education broadly comprise clinical work under supervision, seminars and journal clubs along with conferences and workshops. While the literature on methodologies or reforms applied to undergraduate medical education is plenty, not many of these educational reforms have been applied to anaesthesia postgraduate training.12 Implementation of modern teaching methods in anesthesiology curriculum like problem or case-based learning and flipped classroom is evaluated by a few researchers who have stressed on their importance and a need to further the subject.13, 14, 15, 16
As the complexities of surgery increase, there is an increase in the procedural workload in anaesthesiology involving establishing airway with single or double lumen tubes, invasive vascular access, peripheral and neuraxial blocks and challenges in understanding and managing physiology. The postgraduate curriculum in anaesthesia as described by NMC, requires the residents to demonstrate knowledge in anatomy, physiology and biochemistry for various topics.17 No directives have been given regarding the means to achieve these competencies, though they have mentioned that Didactic lectures are of least importance and teaching should include seminars, journal clubs, symposia, tutorials, case discussions, and research presentations. Understanding the importance of basic sciences, we decided to integrate vertically with the basic sciences departments. Since, every procedural skill in anaesthesia requires thorough knowledge of anatomy, we initiated the vertical integration with the department of anatomy, aiming for a better training of anaesthesia residents.
Assessment of resident's perceptions regarding the new teaching-learning methods (vertical integration with anatomy, in this case) is important for further development and restructuring. Hence, a questionnaire-based study (cross-sectional) was planned to assess the same. This study design was selected as a first step in analyzing this new teaching-learning method in anaesthesia postgraduate curriculum. We hypothesized that the vertical integration was clinically beneficial and the residents were receptive for the new education method.
Materials and methods
This questionnaire based descriptive, cross-sectional study was conducted after approval from the Institutional Ethics Committee. The vertical integration was planned after discussion with anatomists and a schedule for anatomy classes was chalked out for the anaesthesiology residents (Table 1). It included anatomy pertaining to airway, neuraxis, peripheral nerve blocks, and vascular access.
Table 1.
The five-week schedule of the integrated classes with Anatomy.
| Class –I | Naso Pharynx |
| Oro Pharynx | |
| Larynx & Trachea IX, X- superior & recurrent Laryngeal Nerve | |
| Class –II | Arterial & Venous Cannulation- Entire course of Veins - Internal Jugular Vein, Subclavian, Cubital fossa veins -cephalic, basilica, Median cubital |
| Arteries - Radial, ulnar, brachial, dorsalis pedis, posterior tibial | |
| Cerebral circulation- Circle of Willis | |
| Class –III | Nerve Anatomy- |
| Nerve Blocks- Brachial plexus: interscalene, supraclavicular, axillary, musculocutaneous | |
| Wrist block, ankle block | |
| Femoral nerve block, Sciatic & Obturator nerve block | |
| Class -IV | Field Blocks - Pectoral I & II Block, Paravertebral, Erector spinae block, Transversus Abdominis Plane block, Quadratus lumborum block, Rectus sheath block, ilioinguinal block, Facia iliaca |
| Class -V | Spinal canal anatomy |
| Caudal space anatomy | |
| Intercostal space and pleural space (Block and drain placement) |
The schedule spanned over five weeks and each class was of 2 h duration. For the ease of conduct without interrupting the ongoing operating room lists, a total of 41 residents in the department at that time were divided into two batches, such that each batch had one integrated class every week.
In each class, the residents had an interactive session with anatomy and anesthesiology faculty. In the beginning of each session, there was an introductory presentation to give an overview about the topic for the day. This was followed by demonstration of the anatomy on a dissected cadaver and thereafter hands-on time was given on the cadaver to visualize the anatomy related to the topic for the day and its relations. At the end, demonstration on a virtual dissection table (SECTRA Medicals, Sweden) was followed by hands-on practice for the visualization of anatomy including its relations. For example, if brachial plexus anatomy was the topic for the day, after a short introductory presentation, brachial plexus anatomy was demonstrated on a dissected cadaver and on the virtual dissection table by explaining in detail about the anatomic relations with the surrounding structures. Thereafter, residents were given time to visualize the anatomy on their own, being supervised by the faculty. This ‘hands-on’ time was given for both, the cadaver and the virtual dissection table.
After completion of the whole schedule (five classes per batch of residents), a self-structured questionnaire was shared with all the residents as Google Forms to assess their perception regarding the class (Fig. 1). The participation was voluntary and the responses were anonymous. Descriptive statistics were applied to the responses received and were presented as percentages.
Fig. 1.
Questionnaire circulated to the residents as Google Forms.
Results
Thirty-six responses were received from a total of 41 residents leading to a response rate of 87.8%. The response for individual question is presented in Table 2.
Table 2.
Descriptive analysis of questions from the questionnaire.
| S No | Question | Options provided | Response n (%) |
|---|---|---|---|
| 1. | How satisfied were you with the classes in terms of topics covered? | More topics need to be covered | 6 (16.7) |
| Covered mostly all the topics required | 30 (83.3) | ||
| Few topics need to be omitted | 0 (0) | ||
| 2. | How was the duration of the class? | Too Long | 0 (0) |
| Long | 5 (13.9) | ||
| Just Appropriate | 30 (83.3) | ||
| Short | 1 (2.8) | ||
| 3. | Do you believe the classes would be helpful in clinical practice? | Very Helpful | 14 (38.9) |
| Helpful | 20 (55.6) | ||
| Little Helpful | 2 (5.5) | ||
| Not Helpful | 0 (0) | ||
| 4. | What is the best alternate option for revising the anatomy for clinical application? | Textbooks/Atlas | 12 (33.3) |
| Mobile based application | 9 (25) | ||
| You tube | 15 (41.7) | ||
| 5. | What would be the best timing for these classes during the tenure of the residency? | Once (in first/second semester) | 7 (19.4) |
| Twice (in first semester and in last semester) | 18 (50) | ||
| Every year | 11 (30.6) | ||
| 6. | Overall Satisfaction | Extremely Satisfied | 0 (0) |
| Very much Satisfied | 5 (13.9) | ||
| Satisfied | 30 (83.3) | ||
| Not much Satisfied | 1 (2.8) | ||
| Extremely Unsatisfied | 0 (0) |
Most of the residents [30 (83.3%)] responded that the schedule covered all the topics required and the duration of each class was appropriate. Three out of these six residents wanted the inclusion of sonoanatomy in the topics since the applications of ultrasonography are increasing in the perioperative period as well as in the ICU.
Thirty-four (94.5%) believed that the integrated classes would be either very helpful or helpful in their clinical practice. The best alternative to these integrated anatomy classes was YouTube.
Twenty-nine (80.5%) residents wanted the classes to be conducted either twice in the three-year tenure (in the first and last semester) or every year.
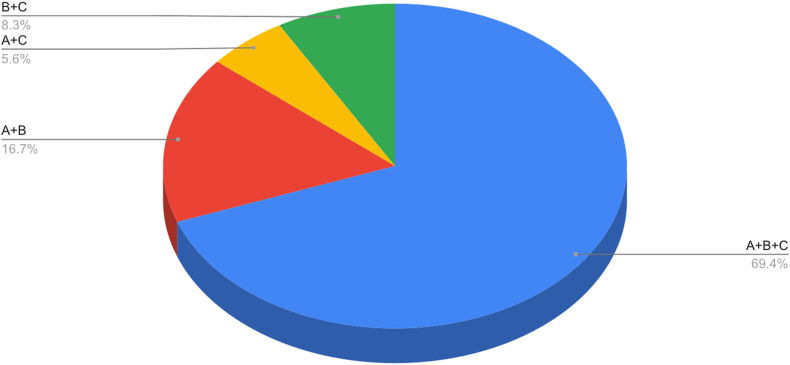
The resident's preference regarding the constitution of class is depicted in Fig. 2 wherein the majority (69.4%) favored all the three components of the class viz. introductory lecture in the beginning, Hands on/Demonstration on the cadaver and SECTRA Virtual Dissection Table.
Fig. 2.
Pie chart depicting resident's preference for constitution of integrated class. (A- Introductory lecture in the beginning; B- Hands on/Demonstration on the cadaver; C- Hands-on/Demonstration on the SECTRA Virtual Dissection Table).
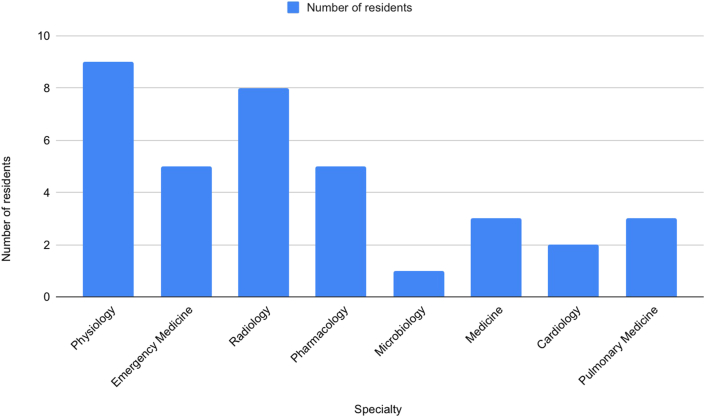
Hundred percent of the residents recommended the classes to be continued for the future batches. Resident's suggestions regarding the other departments they would like to have integrated classes with are depicted in Fig. 3.
Fig. 3.
Number of residents plotted against the choice of specialty they wish to have integrated classes with in addition to Anatomy.
Additional feedback and suggestions section received interesting responses which are summarized in Table 3. Most of the residents 35 (97.2%) were either very much satisfied or satisfied with the integrated classes.
Table 3.
Feedback by the residents.
| We should have one SECTRA virtual dissection table in department so that we can revise and clear our doubt as and when we face any problem |
| Conduct of short tests, MCQs and intra-departmental quiz |
| If we could have a hands-on ultrasound guided demonstration of the structures regarding a particular topic along with the cadaveric and SECTRA virtual dissection, it would be great |
| It was really good for us for our future practice and knowledge. I think this type of class should be organized frequently for our practice. |
| A small booklet with images and handmade notes would make a great difference, and will be easy to recall the topic |
| Anatomy Professors should have some anaesthesia/pain orientation so that they know where to give stress and why |
| If it could be conducted in the morning rather than post lunch |
| Nice effort by our department, academic activity is very good |
| A test can be conducted after the class |
| More emphasis on cadaver training |
| Repeat once in third semester |
Discussion
We received a positive feedback from the residents regarding the integrated classes. The purpose of our study was to assess the perception of anesthesiology residents towards integrated classes with the department of anatomy. The assessment was based on a questionnaire comprising ten questions. The fact that cent percent of the residents who responded want the integrated classes to be continued for the subsequent batches testifies that the residents benefitted from them. However, rather than getting complacent, it's important that the feedback and suggestions are acknowledged, discussed and acted upon.
Medical education has undergone various reforms since the time of Flexner who defined the medical curriculum into a form where basic sciences are taught first and followed by the clinical subjects.1 This subject or discipline-based curriculum has been followed worldwide and is challenged by the integrated curriculum.
An integrated curriculum as defined by Shoemaker is a curriculum wherein various aspects are brought into a meaningful association with the intent of better focus on the matter of discussion.18 So the integration helps put medical teaching into context. Three types of integration have been defined: vertical, horizontal and spiral. Horizontal integration occurs across subjects within a defined time. It's an integration among subjects taught in the same professional year of undergraduate curriculum e.g., Anatomy, Physiology and biochemistry. Vertical integration occurs across time and overcomes the conventional divide between the basic sciences and clinical subjects; e.g., integration between anatomy, pathology, medicine and surgery. Spiral integration happens across time and subjects. It combines both horizontal and vertical integration.19
All the reforms are inducted into the medical curriculum to help put education into context, to catch up with the current issues and to adapt to the changing times and changing needs. All the reforms, especially in India, have been applied to undergraduate teaching while the postgraduate curriculum has largely remained unchanged over several decades.20
We tried to introduce vertical integration into the curriculum of our residents as the new teaching-learning method. We initiated the integration with anatomy, developed a schedule and implemented the same. The assessment of the new methodology with inputs from the stakeholders was sought with the help of a questionnaire. The response rate was good and the majority (83.3%) of students were satisfied with the topics covered while a few (8.4%) wanted sonoanatomy to be included in the integrated classes. Knowledge of sonoanatomy is important in the current anaesthesia practice and will be included in subsequent integrated classes with either anatomy or radiology. About 80% of the residents want the integrated classes to be conducted more than once during their tenure of three years and the logistics for the same are being worked out.
While there are no studies or literature on vertical integration with anatomy (or any other basic science) in postgraduate anaesthesia training to compare our results with; studies regarding perception of integrated classes in undergraduate medical students are available. Kolhe et al conducted a cross sectional study to know the perception of 62 first year undergraduate medical students regarding integrated teaching of Anatomy and Physiology.20 According to them, 3% students agreed that integrated teaching method is an average level practice, 71% of students agreed that integrated teaching method is a good practice and 26% students approved that it is the best technique of teaching. Ninety-five percent students felt that there is a need of integrated teaching in anatomy and physiology. Almost 89% enjoyed the integrated teaching lecture than the regular didactic method. Their findings were in agreement with other studies assessing the perception of undergraduate medical students.21, 22, 23
The residents also want the integration (both horizontal and vertical) to be made with other departments like physiology, radiology, pharmacology etc. This means that the integrated classes that might seem to increase academic burden, are actually favored by the residents and they want more. More residents wanted integration with basic sciences and para-clinical departments rather than clinical departments like pulmonary medicine, cardiology, medicine etc. We also received constructive feedback on the classes implying that the stakeholders (residents) should actually partner in the curriculum design to meet the interests of teachers and students alike.
The integrated curriculum can be applied to all the specialties with the goal of better learning experience ultimately translating into better patient care.
The limitations to the study are the ones inherent to questionnaire -based studies like low response rate due to survey fatigue, the possibility of dishonest answers and unanswered questions. However, we received a good response rate and making all the questions compulsory and answers anonymous must have overcome a few other limitations. Another limitation is that we just assessed the resident's perception of the integrated classes and did not assess the knowledge or changes in clinical practice at the completion of the schedule. In future, studies can be designed to include multiple centers, include a pre-/post-test for knowledge and assess the clinical benefit of integrated classes.
To conclude, vertical integration with basic sciences is well perceived by the residents and should be considered for inclusion in the curriculum of postgraduate training in all the medical specialties.
Disclosure of competing interest
The authors have none to declare.
References
- 1.Barzansky B. Abraham Flexner and the era of medical education reform. Acad Med. 2010;85(9suppl l):S19–S25. doi: 10.1097/ACM.0b013e3181f12bd1. [DOI] [PubMed] [Google Scholar]
- 2.Quintero G.A., Vergel J., Arredondo M., Ariza M.C., Gómez P., Pinzon-Barrios A.M. Integrated medical curriculum: advantages and disadvantages. J Med Educ Curric Dev. 2016;3:S18920. doi: 10.4137/JMECD.S18920. JMECD. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Cooke M., Irby D.M., Sullivan W., Ludmerer K.M. American medical education 100 years after the Flexner report. N Engl J Med. 2006;355(13):1339–1344. doi: 10.1056/NEJMra055445. [DOI] [PubMed] [Google Scholar]
- 4.Catrambone R., Holyoak K.J. Overcoming contextual limitations on problem-solving transfer. J Exp Psychol Learn Mem Cogn. 1989;15(6):1147–1156. [Google Scholar]
- 5.Irby D.M., Cooke M., O'Brien B.C. Calls for reform of medical education by the carnegie foundation for the advancement of teaching: 1910 and 2010. Acad Med. 2010;85(2):220–227. doi: 10.1097/ACM.0b013e3181c88449. [DOI] [PubMed] [Google Scholar]
- 6.Bland C.J., Starnaman S., Wersal L., Moorehead-Rosenberg L., Zonia S., Henry R. Curricular change in medical schools: how to succeed. Acad Med. 2000;75(6):575–594. doi: 10.1097/00001888-200006000-00006. [DOI] [PubMed] [Google Scholar]
- 7.Hurtubise L., Hall E., Sheridan L., Han H. The flipped classroom in medical education: engaging students to build competency. J Med Educ Curricul Dev. 2015;2:35–43. doi: 10.4137/JMECD.S23895. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Harden R.M., Sowden S., Dunn W.R. Educational strategies in curriculum development: the SPICES model. Med Educ. 1984;18(4):284–297. doi: 10.1111/j.1365-2923.1984.tb01024.x. [DOI] [PubMed] [Google Scholar]
- 9.Brauer D.G., Ferguson K.J. The integrated curriculum in medical education: AMEE Guide No. 96. Med Teach. 2015;37(4):312–322. doi: 10.3109/0142159X.2014.970998. [DOI] [PubMed] [Google Scholar]
- 10.Loftus S. Understanding integration in medical education. Med Sci Educ. 2015;25(3):357–360. [Google Scholar]
- 11.Board of Governors in supersession of Medical Council of India. Curriculum Implementation Support Program, Module – 4. Alignment and integration. https://www.nmc.org.in/wp-content/uploads/2020/08/Alignment-and-Integration_03.10.2019.pdf [Accessed on 25 December, 2020].
- 12.Bould M.D., Naik V.N., Hamstra S.J. Review article: new directions in medical education related to anesthesiology and perioperative medicine. Can J Anesth. 2012;59:136–150. doi: 10.1007/s12630-011-9633-0. [DOI] [PubMed] [Google Scholar]
- 13.de Oliveira Filho G.R., Schonhorst L. Problem-based learning implementation in an intensive course of anaesthesiology: a preliminary report on residents' cognitive performance and perceptions of the educational environment. Med Teach. 2005;27:382–384. doi: 10.1080/01421590500151021. [DOI] [PubMed] [Google Scholar]
- 14.Yazigi A., Madi-Jebara S., Richa F., Yazbeck P. Case/problem-based learning discussion for teaching ethics to anaesthesiology residents. Eur J Anaesthesiol. 2008;25:689. doi: 10.1017/S0265021508003864. [DOI] [PubMed] [Google Scholar]
- 15.Chilkoti G., Wadhwa R., Kumar A. Status of problem based learning in postgraduate anesthesia teaching: a cross-sectional survey. Saudi J Anaesth. 2015;9(1):64–70. doi: 10.4103/1658-354X.146316. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Kurup V., Sendlewski G. The feasibility of incorporating a flipped classroom model in an anesthesia residency curriculum-pilot study. Yale J Biol Med. 2020 Aug 31;93(3):411–417. [PMC free article] [PubMed] [Google Scholar]
- 17.National Medical Commission. PG Curricula. https://www.nmc.org.in/information-desk/for-colleges/pg-curricula-2 [Accessed on 25 October, 2020].
- 18.Shoemaker B.J.E. Integrative education: a curriculum for the twenty-first century. OSSC Bullet. 1989;33(2):n2. [Google Scholar]
- 19.Husain M., Khan S., Badyal D. Integration in medical education. Indian Pediatr. 2020;57:842–847. [PubMed] [Google Scholar]
- 20.Kolhe S.K., Kadam S.S., Narkhede J.P., Kulkarni V. Perception of medical teachers about integrated teaching in medical curriculum. Soc Med Sci. 2018;21(31):1–10. [Google Scholar]
- 21.Stalin P., Bazroy J., Singh Z. Evaluation of correlated integrated teaching programme among undergraduate medical students. J Res Med Educ Ethics. 2014;4:60–64. [Google Scholar]
- 22.Lohitshwa Renu, Narendra S.S., Mufti Mehak. Evaluation of impact of integrated teaching over didactic lecture on student learning. J Educ Res Med Teach. 2014;2(2):14–16. [Google Scholar]
- 23.Muller J.H., Jain S., Loeser H., Irby D.M. Lessons which have to be learned about integrating a medical school curriculum and the perceptions of students, the faculty and the curriculum leaders. Med Educ. 2008;42:778–785. doi: 10.1111/j.1365-2923.2008.03110.x. [DOI] [PubMed] [Google Scholar]