Abstract
Background: Thalassemia is a chronic disease requiring lifelong treatment. The adherence to regular iron chelation therapy is important to ensure complication-free survival and good quality of life.
The study aim to assess the adherence to iron chelation therapy (ICT) in patients with transfusion-dependent thalassemia (TDT), evaluate various causes of non-adherence and study the impact of non-adherence on the prevalence of complications secondary to iron overload.
Materials and Methods: Patients with TDT on ICT for > 6 months were enrolled in the study. Hospital records were reviewed for demographic details, iron overload status, treatment details, and the prevalence of complications. A study questionnaire was used to collect information on adherence to ICT, knowledge of patients, and the possible reasons for non-adherence.
Results: A total of 215 patients with a mean age of 15.07+7.68 years and an M: F ratio of 2.2:1 were included in the study. Non-adherence to ICT was found in 10.7% of patients. Serum ferritin levels were significantly higher in the non-adherent group (3129.8+1573.2 µg/l) than the adherent population (2013.1+1277.1 µg/l). Cardiac as well as severe liver iron overload was higher in the non-adherent patients. No correlation was found between disease knowledge and adherence to ICT. Difficulties in drug administration and many medicines to be taken daily were statistically significant reasons for non-adherence. There was no difference in the co-morbidities arising due to the iron overload in the two groups.
Conclusion: Nearly 11% of patients with TDT were non-adherent to ICT. Non-adherence results in higher iron overload.
Key Words: Adherence, Iron chelation therapy, Iron overload, Transfusion-dependent thalassemia, Deferiprone, Deferasirox, Desferrioxamine
Introduction
Thalassemia is an inherited disorder characterized by a defect in the genes coding for the globin chain of hemoglobin1. Estimates reveal that there are about 1,00,000 patients with beta-thalassemia syndromes in India and nearly 8,000 to 10,000 new patients are added each year2,3. The only curative treatment for thalassemia currently is a bone marrow transplant. However, it is restricted to only a few patients due to the non-availability of an HLA-matched donor and high cost. Thus, most patients receive regular blood transfusions accompanied by iron chelation therapy (ICT) as the standard of care. The ideal management of a patient with transfusion-dependent thalassemia (TDT) requires a multidisciplinary therapeutic approach1,3,4. Despite these interventions, the patients of TDT have a very high rate of morbidity and mortality secondary to iron overload in the body. A study from the UK showed that about 50% of people with TDT died before the age of 35 primarily due to non-adherence to regular ICT4. Patients with high serum ferritin levels suffered from cardiac complications, liver dysfunction, various endocrinopathies as well as poor quality of life5. Serum ferritin levels maintained below 1000 µg/l were associated with normal life as documented earlier6. Thus, improving adherence to iron chelation is the most effective way to decrease the morbidity and mortality in patients with TDT. Adherence refers to the act of voluntary submission to some point of view7. Many psychological, social, and financial factors can result in non-adherence to ICT, thus affecting the quality of life of the patients. Data is scarce on adherence to ICT in developing countries like India. In a study from Jamshedpur, a compliance score was used to find adherence to ICT in patients of TDT8. Good compliance was found in only 33% patients using the tool.8 In this study, we used a Likert scale to assess adherence to ICT. The study also attempted to explore the relationship between disease knowledge and adherence as knowledge could have an impact on the patient’s beliefs and attitude towards ICT 9,10,11. Our study also explored the causes of non-adherence on an eleven-point questionnaire. The prevalence of various iron overload related complications was compared between the adherent and non-adherent populations.
MATERIALS AND METHODS
Primary objective:
• To assess the adherence to iron chelation therapy in patients with TDT.
Secondary objectives:
• To evaluate the relationship between disease knowledge and adherence to ICT.
• To discover the factors that influence adherence to iron chelation.
• To assess the relationship between adherence to ICT and complications secondary to iron overload.
A prospective single-arm study was conducted in the thalassemia day-care center (TDCC), Department of Pediatrics after obtaining approval from the Institutional Ethics Committee. Informed consent in the vernacular language was obtained from the patient/parent before enrolling them in the study. All patients with TDT on ICT for more than 6 months who consented for the study were included. The exclusion criteria were patients on ICT for less than 6 months, patients not consenting for the study and patients with other co-morbidities impairing their ability to adhere to ICT (e.g. stroke)
A study questionnaire (supplementary material) was used to collect the following data: a) demographic details of the patient such as age, sex, height, and weight of the patient b) treatment details of the patient as mentioned in their records i.e. the drug used for iron chelation, dose, frequency, route and number of tablets prescribed per day c) iron overload status including mean serum ferritin levels from the past 3 years, assessment of cardiac and hepatic iron overload by MRI T2* using standardized techniques12,13 d) Checking the presence or absence of co-morbidities secondary to iron overload from their records (Table 1).
Table 1.
Case definitions for the co-morbidities
| Co-morbidities | Eligibility (age group tested) | Definition |
|---|---|---|
| Liver dysfunction | Everyone | Elevated transaminases (more than 4 times above the baseline) or presence of cirrhosis/ fibrosis on Ultrasonography.1 |
| Cardiac failure/ Arrhythmias | >10 years | Echocardiography report showing ejection fraction <50% or arrhythmia. 1 |
| Short Stature and Retarded Growth |
Everyone | Height below the third centile for sex and age (based on WHO charts) 14 |
| Delayed Puberty and Hypogonadism |
|
a) Delayed Puberty: complete lack of pubertal development in girls by the age of 13 and in boys by the age of 14. b) Hypogonadism in boys: the absence of testicular enlargement. Hypogonadism in girls: the absence of breast development by the age of 16 with low LH and FSH in both males and females, and testosterone in males and estradiol in females. 14 |
| Hypothyroidism | >5 years | a) Sub-clinical hypothyroidism: high TSH with normal FT4 levels. B) Overt hypothyroidism: combination of high TSH with low FT4 levels. 14 |
| Diabetes Mellitus | >10 years | The diagnostic criteria for Glucose Tolerance and DM are as follows: 14 • GTT Serum Glucose at 2 hours >200mg/dl is diagnostic of DM. • GTT Serum Glucose at 2 hours > 140<2000mg/dl indicates glucose intolerance. |
| Hypoparathyroidism | >15 years | Low serum calcium and high phosphate levels, and low parathyroid hormone. 14 |
| Adrenal Insufficiency | >15 years | Cortisol levels are used for the assessment of adrenal insufficiency. 14 |
| Bone Disorders | >10 years | Z score on DEXA scan 14 • - 1 to - 2.5: osteopenia • < - 2.5: osteoporosis |
The adherence to ICT was assessed using Likert Scale where 1 represented “never missed a dose”, 2 represented “some of the time” (missed <25% of total doses), 3 represented “most of the time” (missed 25-50% of total doses) and 4 represented “all of the time” (missed >50% of total doses). Patients taking >75 % of the prescribed doses (score of 1 and 2) were considered to be adherent, whereas those with <75% (score 3 and 4) were considered non-adherent. The knowledge regarding thalassemia, transfusion, and ICT was analyzed using a 19-point questionnaire. This included open-ended questions so that all the concepts regarding thalassemia, transfusion, and ICT could be deciphered. The knowledge of the patients was then scored. A score of 1 was given for each correct response, a score of 0.5 was given when the patient was uncertain about the answer, and a score of 0 was given for each incorrect response. The knowledge regarding the disease and the prevalence of iron overload related complications were compared between the adherent and non-adherent groups.
Statistical analysis
Data was described in terms of range; mean ±standard deviation (± SD), frequencies (number of cases), and relative frequencies (percentages) as appropriate. For comparing categorical data, Chi-square (χ2) test was performed and the exact test was used when the expected frequency was less than 5. A probability value (p) less than 0.05 was considered statistically significant. All statistical calculations were done using SPSS (Statistical Package for the Social Science) SPSS 21 version statistical program for Microsoft Windows.
Results
The study was conducted at the TDCC of a tertiary care hospital in Punjab, India. A total of 240 TDT patients were registered in the unit. Twenty-five patients were excluded from the study, 17 were on ICT for less than 6 months and 8 did not consent for the study. Hence, 215 patients were included in the study. The baseline characteristics of the study population are mentioned in Table 2. The mean serum ferritin was 1458.4+489.1, 2119.6+877.7, 2146.7+1412.3 and 2296.3+1540.9µg/ml in the age groups of <5, 5-10, 10-18, >18 years, respectively. The mean serum ferritin in males was 1986.6+1154.7µg/ml which was significantly lower than the mean serum ferritin in females which was 2455.1+1676.1µg/ml(p=0.018). An MRI T2* to assess cardiac and liver iron overload was done in 149 patients (50 patients were younger than 10 years of age and 16 patients older than 10 years did not get an MRI done). Moderate to severe cardiac and hepatic iron overload was seen in 18.1% and 70.5% of patients, respectively.
Table 2.
Baseline characteristics of the study population
| Parameters |
Number of
patients |
Minimum | Maximum | Mean | Standard Deviation |
|---|---|---|---|---|---|
| Age (years) | 215 | 1.50 | 38.00 | 15.07 | 7.68 |
| Pre-transfusion HB (g/dl) | 215 | 4.20 | 11.60 | 9.20 | 0.86 |
| Yearly transfusion requirement*
(ml/kg/year) |
206 | 24.00 | 477.00 | 236.77 | 56.77 |
| Mean ferritin | 215 | 160.75 | 7594.00 | 2132.60 | 1352.65 |
| (ng/ml) |
denotes that only 206 patients out of 215 analyzed patients had been registered with the thalassemia day care center for more than 1 year. So, yearly transfusion requirement of 9 patients who were registered in the last one year could not be calculated.
Single iron chelator was being administered in 57.2% of patients (n=123) and a combination of two or more iron chelators was being used for 42.7% (n=92) patients. Deferasirox was the most commonly used iron chelator.
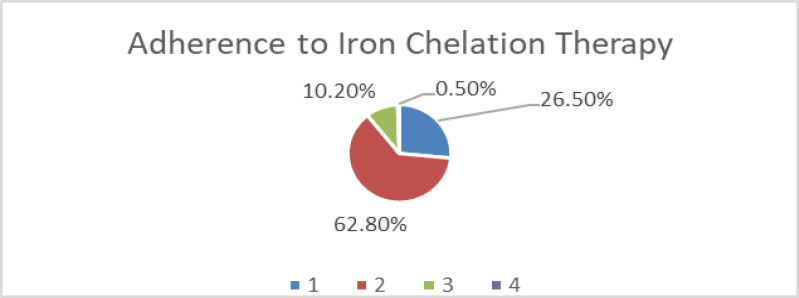
An adherence score of 1 was reported by 26.5% (n=57) of the study population, 62.8% (n=135) had the score of 2, 10.2% (n=22) had a score of 3 and 0.5% (n=1) had a score of 4. Thus, 10.7% of patients with TDT were non-adherent to the ICT.
The maximum adherence with ICT was found in the age group of 10-18 years (91.4%) and the adherence was lesser in the younger patients (p=0.848) (Figure 1). The adherence in males (90.5%) was found to be higher as compared to that in females (86.6%); however, the difference was not statistically significant (p=0.383). Amongst the currently available iron chelators, the adherence rate was highest with DFX (91.2%), followed by DFP (87.2%) and DFO (83.3%) (p=0.350). Amongst the patients on oral chelation regimen, the adherence rates were 88.3%, 90.6%, and 94.4% in patients who were on <5 tabs per day, 5-10 tabs per day and >10 tabs per day, respectively. (p=0.534). The adherence was highest among patients who were taking one dose of the drug per day (90.8%) and fell considerably if the number of doses was> 3/day (p=0.052). Patients on an oral chelation regimen reported better adherence (90.1%) as compared to those on a parenteral regimen (83.3%), although it could not achieve statistical significance (p=0.315). The mean serum ferritin in the adherent population was found to be significantly lower than the non-adherent population (2013.1+1277.1µg/ml vs 3129.8+1573.2µg/ml) (p=0.000). Cardiac iron overload was detected in 71.4% of the non-adherent patients as compared to 19.0% of the adherent patients (p=0.000). Liver iron overload was detected in a similar number of patients in both adherent and non-adherent groups (91.1% vs 92.9%); however, 78.6% of non-adherent patients had severe hepatic iron overload as compared to 36.3% of adherent patients (p=0.021).
Figure 1.
Adherence to iron chelation therapy. Adherence score of 1-4.
The knowledge of patients regarding thalassemia, blood transfusion, and ICT was analyzed based on a 19-point questionnaire. The mean knowledge score of the adherent group was 15.8+2.0 and the non-adherent group was 16.0+2.4(p=0.662).
The study attempted to find the causes of non-adherence based on an 11-point questionnaire. The various beliefs of the patients regarding ICT are shown in Table 3. A higher proportion of non-adherent patients felt there were too many medications and found it difficult to consume the medications. Other beliefs like medicines do not show immediate results and busy schedules lead to missing doses were also documented to be higher in the non-adherent population though it could not reach statistical significance. Nearly half (47.8%) of the non-adherent patients also felt that nothing happens if they miss their dose. About 82.3% of the adherent population and 73.9% of the non-adherent patients agreed to have experienced cost constraints while purchasing the medicines.
Table 3.
Beliefs regarding ICT in the two groups of adherent and non-adherent population
| Reasons |
Adherent population (n=192)
|
Non- adherent population (n=23)
|
p | ||||
|---|---|---|---|---|---|---|---|
| Disagree(%) | Uncertain(%) | Agree(%) | Disagree(%) | Uncertain(%) | Agree(%) | ||
| I don’t believe that medicines are of any help |
87.0 | 3.6 | 9.4 | 82.6 | 8.7 | 8.7 | 0.520 |
| My ferritin levels are not high enough for me to be on regular iron chelation |
84.4 | 10.4 | 5.2 | 82.6 | 13.0 | 4.4 | 0.919 |
| Medicines don’t show immediate results |
23.4 | 8.9 | 67.7 | 13.0 | 0.0 | 87.0 | 0.127 |
| Nothing will happen if I miss my doses |
51.0 | 9.4 | 39.6 | 47.8 | 4.4 | 47.8 | 0.614 |
|
Too many
medicines to be taken everyday |
46.4 | 2.6 | 51.0 | 17.4 | 4.3 | 78.3 | 0.030 |
| I keep very busy during the day and forget my dose |
59.9 | 3.6 | 36.5 | 47.8 | 0.0 | 52.2 | 0.262 |
| It is easier to take medicine after meal than empty stomach |
67.7 | 1.6 | 30.7 | 65.2 | 0.0 | 34.8 | 0.784 |
|
Route of
administering medicines is difficult for me |
89.6 | 2.1 | 8.3 | 69.6 | 0.0 | 30.4 | 0.005 |
| Feel shy to take medicines in front of others |
94.3 | 2.1 | 3.6 | 91.3 | 0.0 | 8.7 | 0.417 |
| Cost of medicines is too high |
14.6 | 3.1 | 82.3 | 17.4 | 8.7 | 73.9 | 0.368 |
| There are too many side effects |
82.8 | 6.3 | 10.9 | 91.3 | 0.0 | 8.7 | 0.425 |
An analysis was done to compare the prevalence of various iron overload related complications in the adherent and non-adherent groups (Table 4). No statistical difference was found between the prevalence of complications in the two groups.
Table 4.
Frequency of complications related to iron overload in two groups
| Complication | Total no. of patients with the complication |
% of total Adherent patients with complication |
% of total non-adherent patients with complication |
p |
|---|---|---|---|---|
|
Liver dysfunction
Present Present(drug related) Cirrhosis |
11 | 4.7 | 8.7 | 0.294 |
| 7 | 2.6 | 8.7 | ||
| 5 | 2.6 | 0.0 | ||
| Cardiac dysfunction | 2 | 1.4 | 0.0 | 0.742 |
| Short stature | 65 | 28.6 | 43.5 | 0.143 |
| Delayed puberty | 54 | 49.5 | 54.5 | 0.925 |
| Hypothyroidism | 63 | 33.7 | 25.0 | 0.687 |
|
Glucose tolerance
Impaired GTT Diabetes mellitus |
10 | 7.2 | 0.0 | 0.257 |
| 3 | 1.4 | 7.2 | ||
| Hypoparathyroidism | 6 | 6.3 | 0.0 | 0.691 |
| Adrenal insufficiency | 9 | 8.5 | 10.0 | 0.874 |
|
Bone disorders
Osteopenia Osteoporosis |
97 | 63.4 | 46.7 | 0.407 |
| 38 | 22.5 | 40.0 |
Discussion
In a cohort of 215 TDT patients with a mean age of 15.07 years, 89.3% were found to be adherent to ICT. The non-adherent population had a higher body iron content as compared to the adherent patients. These results are comparable to the study done by Trachtenberg F et al. that reported more than 90% adherence towards the two common chelators, DFO (n=79) and DFX (n=186). The mean age of the population in their study was 22 years. In previous studies, adherence, when compared to the age of the patients, was found to be higher in children as compared to adults 15,16. However, we found a lower degree of adherence in children < 10 years as compared to adolescents and adults (p=0.848). These may be linked to the onset of complications in the age group of 10-18 years, following which the patients get repetitive counselling on the importance of adherence to ICT. In the case of children <5 years, the practice of taking the chelator empty stomach in the morning lead to skipped doses as reported by the parents. They also reported difficulty in administering DFX early morning as it has to be dispersed in 50-100 ml of water. Film-coated tablets are not widely used in our country due to cost restraints and only one patient in our cohort was using the film-coated tablet.
The serum ferritin level in males was significantly lower than the females (p=0.018). The self-reported adherence in the male population (90.5%) was more than that reported in females (86.6%), though it was not statistically significant (p=0.383). This could be because adolescent boys, compared to girls, were more likely to receive the drug under parental supervision. This; however, is a general observation and not systematically studied.
The adherence with DFX was found to be better than that with DFP and DFO. These results are in concurrence with many of the earlier studies reported in the literature15,17,18,19,20. Rashid et al. found that the most commonly cited reason for non-adherence with DFO was pain at the site of injection16. We did not find any significant difference in adherence between oral and parenteral regimen (p =0.315). This may be due to a selection bias in our study population that had a very small number of patients on a parenteral regimen as compared to those on oral chelation regimen. Moreover, the patients who are currently on DFO have been advised the same due to severe iron overload and have chosen DFO over other chelation regimens after multiple counselling sessions.
The adherence was maximum amongst patients taking one dose per day and decreased as the number of doses per day increased (p=0.052). The patients are likely to miss some of their doses when they are on multiple doses per day. The analysis with the total number of tablets of drug consumed per day showed that the adherence increases as the number of tablets increases (p =0.534). This corroborates with better adherence amongst older individuals as compared the younger patients.
A good adherence with ICT is likely to be associated with a lower level of iron accumulation in the body. The mean serum ferritin was significantly lower in the patients’ adherence to ICT compared to non-adherent patients (p=0.000). Similar results were reported by a study done by Trachtenberg et al.9 However, Lee et al. reported that there was no correlation between self-reported adherence with serum ferritin levels21. This may be because their study reported adherence only for patients on DFO alone with about 69% non-adherent and 19% severely non-adherent population (taking < 50% of their prescribed ICT).
We could not find any statistically significant difference between the knowledge regarding thalassemia/blood transfusion or ICT and adherence in patients. Education and counselling of the patients impacted adherence to ICT in various previous studies9,10,11. Similar to our study, Al‐Kloub MI et al. showed that disease knowledge had no relation with adherence to ICT in adolescent patients22.
Too many medicines to be taken daily and difficulties in drug administration were the important reasons cited by the non-adherent patients. Various other authors have also shown the role of situational psychological factors, busy work schedule, and social stigma as reasons for non-adherence to ICT23.
Various authors have elucidated the role of lower family income, poor family support as well as side effects of the chelators as the possible reasons for poor adherence in patients21,24,25. All these results suggest a complex interplay of physical, social as well as psychological factors leading to non-adherence to ICT.
Our study could not find out any statistically significant difference in the occurrence of iron overload related complications between the adherent and non-adherent patients. This could be because our population has predominately younger individuals who need to be followed up for some time for the development of any complications later in life18,26,27.
CONCLUSION
The study revealed that there is a statistically significant relationship between self-reported adherence and iron overload status. This may be reflected in terms of better clinical outcomes in patients with TDT in the future. ICT is more likely to be successful if initiated and tailored according to the needs and daily routine of the patients.
References
- 1.Cappellini MD, Cohen A, Porter J, Taher A, Viprakasit V ed. Guidelines for the Management of Transfusion Dependent Thalassaemia. 3rd Edition. Nicosia, Cyprus: Thalassemia International Federation; 2014. [PubMed] [Google Scholar]
- 2.Colah R, Italia K, Gorakshakar A. Burden of thalassemia in India: The road map for control. J Pediatr Hematol Oncol. 2017;4(2):79–84. [Google Scholar]
- 3.Mathew A, Sobti PC. The burden of thalassemia in Punjab: A roadmap forward. J Pediatr Hematol Oncol. 2017;4(2):85–7. [Google Scholar]
- 4.Modell B, Khan M, Darlison M. Survival in β-thalassemia major in the UK: data from the UK Thalassaemia Register. Lancet. 2000;355(9220):2051–2. doi: 10.1016/S0140-6736(00)02357-6. [DOI] [PubMed] [Google Scholar]
- 5.Abetz L, Baladi JF, Jones P, et al. The impact of iron overload and its treatment on quality of life: results from a literature review. Health Qual Life Outcomes. 2006;4:73. doi: 10.1186/1477-7525-4-73. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Belhoul KM, Bakir ML, Saned MS, et al. Serum ferritin levels and endocrinopathy in medically treated patients with β thalassemia major. Ann Hematol. 2012;91(7):1107–14. doi: 10.1007/s00277-012-1412-7. [DOI] [PubMed] [Google Scholar]
- 7.Porter JB, Evangeli M, El-Beshlawy A. Challenges of adherence and persistence with ICT. Int J Hematol. 2011;94(5):453–60. doi: 10.1007/s12185-011-0927-3. [DOI] [PubMed] [Google Scholar]
- 8.Kannan S, Singh A. Compliance score as a monitoring tool to promote treatment adherence in children with thalassemia for improved physical growth. Asian J Transfus Sci. 2017;11(2):108–114. doi: 10.4103/ajts.AJTS_61_16. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Trachtenberg FL, Mednick L, Kwiatkowski JL, et al. Beliefs about chelation among thalassemia patients. Health Qual Life Outcomes. 2012;10:148. doi: 10.1186/1477-7525-10-148. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Jeesh A, Aser Adnan Y, Al-Haboub MA. The Effects of Patients' and Care-Givers' Knowledge, Attitude, & Practice (KAP) on Quality of Life Among Thalassemia Major Patients' in the Damascus-Syrian Arab Republic. Eur Sci J . 2018;14(12):308. [Google Scholar]
- 11.Lee YL, Lin DT, Tsai SF. Disease knowledge and treatment adherence among patients with thalassemia major and their mothers in Taiwan. J Clin Nurs. 2009 Feb;18(4):529–38. doi: 10.1111/j.1365-2702.2007.02150.x. [DOI] [PubMed] [Google Scholar]
- 12.Carpenter JP, He T, Kirk P, et al. On T2* magnetic resonance and cardiac iron. Circulation. 2011;123(14):1519–28. doi: 10.1161/CIRCULATIONAHA.110.007641. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Garbowski MW, Carpenter JP, Smith G, et al. Biopsy-based calibration of T2* magnetic resonance for estimation of liver iron concentration and comparison with R2 Ferriscan. J Cardiovasc Magn Reson. 2014;16(1):40. doi: 10.1186/1532-429X-16-40. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.De Sanctis V, Soliman AT, Elsedfy H, et al. Growth and endocrine disorders in thalassemia: The international network on endocrine complications in thalassemia (I-CET) position statement and guidelines. Indian J Endocrinol Metab. 2013;17(1):8–18. doi: 10.4103/2230-8210.107808. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Trachtenberg F, Vichinsky E, Haines D, et al. Iron chelation adherence to deferoxamine and deferasirox in thalassemia. Am J Hematol. 2011;86(5):433–6. doi: 10.1002/ajh.21993. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Rashid M, Karimi M. Compliance of deferoxamine injection in beta-thalassemia major patients in Iran. Transfus Med. 2012;22(2):104–7. doi: 10.1111/j.1365-3148.2011.01130.x. [DOI] [PubMed] [Google Scholar]
- 17.Goulas V, Kourakli-Symeonidis A, Camoutsis C. Comparative effects of three iron chelation therapies on the quality of life of Greek patients with homozygous transfusion-dependent Beta-thalassemia. ISRN Hematol. 2012;2012:139862. doi: 10.5402/2012/139862. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Delea TE, Edelsberg J, Sofrygin O, et al. Consequences and costs of noncompliance with ICT in patients with transfusion‐dependent thalassemia: a literature review. Transfusion. 2007;47(10):1919–29. doi: 10.1111/j.1537-2995.2007.01416.x. [DOI] [PubMed] [Google Scholar]
- 19.Haghpanah S, Zarei T, Zahedi Z, et al. Compliance, and satisfaction with deferasirox (Exjade®) compared with deferoxamine in patients with transfusion-dependent beta-thalassemia. Hematology. 2014;19(4):187–91. doi: 10.1179/1607845413Y.0000000121. [DOI] [PubMed] [Google Scholar]
- 20.Porter J, Bowden DK, Economou M, et al. Health-related quality of life, treatment satisfaction, adherence, and persistence in β-thalassemia and myelodysplastic syndrome patients with iron overload receiving deferasirox: results from the EPIC clinical trial. Anemia. 2012;2012:297641. doi: 10.1155/2012/297641. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Lee WS, Toh TH, Chai PF, et al. Self‐reported level of and factors influencing the compliance to desferrioxamine therapy in multi transfused thalassaemias. J Paediatr Child Health. 2011;47(8):535–40. doi: 10.1111/j.1440-1754.2011.02017.x. [DOI] [PubMed] [Google Scholar]
- 22.Al‐Kloub MI, Nayel Salameh T, Froelicher ES. Impact of psychosocial status and disease knowledge on deferoxamine adherence among thalassemia major adolescents. Int J Nurs Pract. 2014;20(3):265–74. doi: 10.1111/ijn.12143. [DOI] [PubMed] [Google Scholar]
- 23.Vosper J, Evangeli M, Porter JB, et al. Psychological Factors Associated with Episodic Chelation Adherence in Thalassemia. Hemoglobin. 2018;42(1):30–36. doi: 10.1080/03630269.2018.1433686. [DOI] [PubMed] [Google Scholar]
- 24.Trachtenberg FL, Gerstenberger E, Xu Y, et al. Relationship among chelator adherence, change in chelators, and quality of life in thalassemia. Qual Life Res. 2014;23(8):2277–88. doi: 10.1007/s11136-014-0671-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Rofail D, Abetz L, Viala M, et al. Satisfaction and adherence in patients with iron overload receiving ICT as assessed by a newly developed patient instrument. Value Health. 2009;12(1):109–17. doi: 10.1111/j.1524-4733.2008.00390.x. [DOI] [PubMed] [Google Scholar]
- 26.Gabutti V, Piga A. Results of long-term iron-chelating therapy. Acta Haematol. 1996;95(1):26–36. doi: 10.1159/000203853. [DOI] [PubMed] [Google Scholar]
- 27.Soliman A, Yassin M, Al Yafei F, et al. Longitudinal study on liver functions in patients with thalassemia major before and after deferasirox (DFX) therapy. Mediterr J Hematol Infect Dis. 2014;6(1):e2014025. doi: 10.4084/MJHID.2014.025. [DOI] [PMC free article] [PubMed] [Google Scholar]