Abstract
Introduction
COVID-19 has had a significant impact on healthcare systems. We aim to quantify the impact of this outbreak on shoulder and elbow trauma in our institution.
Methods
We prospectively collected data on patients presenting to our hospital with shoulder and elbow injuries during COVID-19. This included the number of attendances to the emergency department, fracture clinic, inpatient admissions and operative treatments. This was compared to a pre-COVID-19 period. We also assessed the efficacy of telephone clinics.
Results
There has been a noticeable decrease in the number of emergency department and fracture clinic attendances with upper limb complaints. The number of in-person fracture clinic reviews also decreased, with a reciprocal exponential increase in telephone consultations. We recorded a decrease in the number of shoulder and elbow trauma procedures performed. There was a small increase in the proportion of injuries treated conservatively during COVID-19. Our telephone clinics yielded a diagnosis and management plan in many cases and patient perspective appeared favourable.
Conclusion
We have noted significant change in the upper limb caseload. Certain injuries have reduced, likely due to COVID-19 lockdown. Moreover, we consider several changes to current practices could be taken forward after the pandemic.
Keywords: COVID, response, shoulder, elbow, trauma
Introduction
COVID-19 has had a significant impact on the health services across the world since the outbreak was reported in Wuhan, China, in late December 2019.1 By April 2020, the United Kingdom government had introduced several public measures to try and restrict the spread of COVID-19.2 This was primarily based on social distancing and self-isolation.
The trauma and orthopaedic department had to make significant changes to the service to help deal with the large number of COVID-19 positive patients needing admission. Changes have been made based on the British Orthopaedic Association Standards for Trauma (BOAST) COVID-19 guidance3 and local consultant consensus.
Practice changes included:
Outpatients and fracture clinics:
Fracture clinics were conducted by telephone or video consults and only seeing patients face to face when necessary (e.g. plaster change, wound reviews). Where possible, patients had their radiographs on an outpatient basis in their local ‘COVID-19-clean’ sites and contacted the next day, either by phone or video consultation. The need for further follow-up within fracture clinic was also strictly rationalised. To reduce the need for attendance to hospital, patients were placed into a splint or brace in preference to plaster if possible.3
Inpatient services:
Elective lists were cancelled within a week of the measures being implemented, but trauma and emergency service provision continued uninterrupted.
The upper limb trauma was mainly ambulatory, and carried out at local independent hospital sites, as part of a national initiative to streamline workload.3 These patients were sent home from the emergency department or minor injuries unit after assessment and allocated to a separate list in a ‘COVID-19-clean’ site if a negative COVID-19 swab was produced. A small number of these patients were treated at the main site if they had complex medical needs, multiple injuries or tested positive for COVID-19.
Increase in the number of patients treated conservatively:
In line with the British Orthopaedic Association (BOA) guidance,3 it was anticipated that most upper limb injuries would be treated non-operatively, with a recognition that these may require reconstruction at a later date.
Surgical practice modifications:
Staff safety measures:
The use of power tools, diathermy and pulsatile lavage were identified as aerosol-generating-procedures,4 and their use was reduced as much as possible.
A report recently showed that there is no viral load detected in the blood of infected cases.5 Nevertheless, our Trust has recommended that all staff treat every patient as if they were COVID-19 positive (i.e.: using full personal protective equipment (PPE), including filtering facepiece 3 masks and minimising the number of staff members in theatre).
Efficiency and capacity measures:
In line with Public Health England guidance,2 all elective surgery for the upper limb was halted. New theatre practices were adopted which included the ‘donning and doffing’ of PPE, recovering patients in the same theatre, and deep cleaning of the operating theatre after every case. As expected, turnaround time was massively increased hence the number of cases performed daily decreased significantly. As a result, by the second week of implementation of these protocols, a second operating theatre was provided to alternate patients between them to improve efficiency without the need for additional personnel.
Aims
These changes had a significant impact on the working patterns of the department. This study aims to quantify the impact of this outbreak on the management of the upper limb trauma caseload and document the immediate response and change in practices of the department. We also aim to evaluate our use of telephone clinics within the upper limb subspecialty. To the best of our knowledge, this is the first study which specifically documents upper limb data.
Methods
The data for the study were collected prospectively and compared to similar data for a period prior to the pandemic. We collected and analysed data of patients attending Accident and Emergency (A&E) departments and minor injuries units across the Trust with an upper limb complaint, as well as the number of patients reviewed in fracture clinics with an upper limb complaint (both in person and by telephone) and the number of shoulder and elbow trauma operations performed. Data were collected from 1st April 2019 to 15th March 2020 (to ascertain an average of ‘normal’ practice pre-COVID-19) and data from 1st April 2020 to 15th May 2020 (during COVID-19 measures) for A&E and fracture clinic attendances. Data were collected from 1st February 2020 to 15th March 2020 as pre-COVID-19 and from the 1st April 2020 to 15th May 2020 as the COVID-19 period for surgical trauma procedures.
In addition, we evaluated the use of telephone clinics to establish whether a diagnosis could be made over the phone, the role of imaging and investigations, the creation of a management plan and patient views regarding the use of a telephone consultation. Clinic letters of patients with upper limb complaints were studied by an independent observer. These were a mix of new referrals, follow-ups and post-operative patients. There were no second opinion referrals in this cohort.
Inclusion criteria: Closed fractures of the scapula, clavicle, proximal humerus, humeral diaphysis, distal humerus, olecranon and proximal radius and ulna.
Exclusion criteria: Fractures of the midshaft and distal radius and ulna; open fractures.
Outpatient data collected:
Total number of upper limb complaint attendances to A&E and minor injuries units across the Trust.
Number of injuries to the clavicle, humerus and elbow.
Comparison of trends in upper limb to injuries of lower limb.
Numbers of patients reviewed in the fracture clinic with an upper limb complaint.
Numbers of patients who were consulted via telephone versus face-to-face consultations in the fracture clinic with an upper limb complaint.
Rate of operative treatment of shoulder & elbow injuries in the pre-COVID-19 period versus during COVID-19.
Inpatient data collected:
Inpatient admissions with upper limb injury.
Operative data
Number of shoulder and elbow trauma operations performed.
Results
Upper limb complaints declined significantly during COVID-19 measures, compared to pre-COVID. According to A&E diagnosis codes, ‘Injuries of shoulder/arm/elbow/wrist/hand’ decreased from average 1146 per month pre-COVID-19 to 325 per month during COVID-19.
Similarly, ‘Pain in shoulder/arm/elbow/wrist/hand’ complaints decreased from 257 per month pre-COVID-19 to 100 per month during COVID-19 measures (Figure 1).
Figure 1.

Showing presentations to Accident and Emergency and minor injury departments across the trust with an upper limb complaint.
Average weekly upper limb presentations decreased more significantly during COVID-19 when compared to lower limb presentations (Figure 2).
Figure 2.

Comparison of decline in upper limb injuries to lower limb injuries.
Admissions to orthopaedic wards with upper limb injuries declined from 16.5 to 9.5 per month during COVID-19.
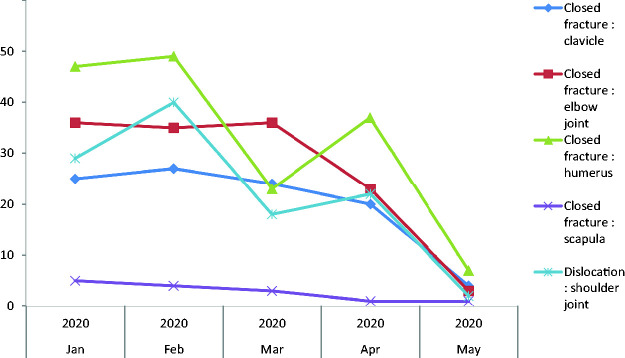
The rates of closed fracture of the clavicle declined from average 25 to 12 per month, closed fracture of the scapula from 4 to 1, dislocation of the shoulder from 29 to 15 per month and closed fracture of the humerus from 40 to 22. Similarly, the closed fracture of the elbow joint declined from 36 to 13 per month (Figure 3).
Figure 3.
Trends of upper limb presentations pre-COVID-19 measures and during COVID-19 measures.
The average number of patients reviewed in fracture clinics with an upper limb complaint declined significantly from an average of 42 per week pre-COVID measures to an average total of 27 per week during COVID-19 measures. Of these, the majority of patients were reviewed by telephone or video consultation. A small minority were still seen face to face in fracture clinic (Figure 4).
Figure 4.
Number of patients reviewed in the fracture clinic with an upper limb complaint.
The number of shoulder and elbow surgical trauma cases decreased by roughly half, from 23 performed across the trust in a six-week period pre-COVID-19 to 12 in a six-week period during COVID-19.
Ninety-eight shoulder and elbow injuries were recorded at the main site in April and May 2020 (during COVID-19) of which 70% of injuries were treated conservatively. This is in comparison to 125 injuries recorded in April and May 2019 (pre-COVID-19), of which 67% were treated conservatively.
When evaluating our use of telephone clinics for upper limb patients; 93% of telephone consultations resulted in a clear diagnosis. Twenty-seven per cent of telephone consultations were conducted with the required imaging and investigations fully available, with 67% of consultations resulting in a clear action plan with regard to future imaging and investigations. All consultations resulted in a management plan for the patient going forward. Most (93%) telephone consultations resulted in patient satisfaction, as documented in the clinic letter.
Discussion
Our department is the main trauma site in a large trust which serves over 700,000 people. The trust encompasses two acute hospitals and four peripheral minor injuries units. Across all sites, our data show that the total number of patients with shoulder and elbow trauma reduced significantly, as a result of lockdown measures.
It is interesting to note that the decline in the upper limb injuries was more precipitous compared to lower limb injuries. Upper limb injuries reduced by 48% when compared to pre-COVID times, in comparison to a fall of only 23% for lower limb injuries. There are few possible reasons for this trend, including a moderate surge of neck of femur fractures, which are a significant constituent of lower limb injuries.6
We believe that the reduction in social mobility due to lockdown is the main reason behind the decreased number of upper limb injuries.
As the upper limb injury referrals dropped by almost half, the number of operations performed for shoulder and elbow trauma also expectedly decreased by a similar proportion. These included proximal and distal humerus fixation procedures, paediatric supracondylar fracture fixation procedures and olecranon fixation. This is directly related to the BOA COVID-19 guidance3 which recommended the conservative management of these injuries when reasonable to do so.
The percentage of patients treated non-operatively however was similar to pre-COVID times due to a lower total number of injuries sustained during COVID-19. We did also note a significant discrepancy between April 2020 (40 injuries) and May 2020 (58 injuries) and we postulate that the government easing of lockdown in May 2020, to include increased return to work and outdoor exercise could have contributed to this.7
The protocols for the running of the fracture clinic were also amended to suit social distancing measures and reduce the number of hospital visits. A risk-stratification protocol (Figure 5) was initiated, and hospital sites were marked as ‘clean’ and ‘COVID-19’. Fracture patients requiring a follow-up radiograph or plaster change attended a ‘Clean’ site, local to their home address. These were often located at the peripheral minor injuries unit. The radiographs were then assessed by a clinician remotely and a telephone consult was offered. The use of splints and braces rather than casts wherever possible was encouraged, as per BOA guidance.3 In addition, a video consultation system, ‘AccuRX’ (AccuRx, London, UK) was used by some clinicians to review wounds or adequacy of splints and braces, and this is demonstrated in Figure 5. The feedback from patients for telemedicine consults is encouraging to date, and we are currently reviewing the objective efficacy of telemedicine as we believe it would be an excellent tool for certain indications in the future.
Figure 5.
Risk stratification algorithm for treatment of fractures and other injuries to minimise hospital exposure.
Our measures described above resulted in a decline in the number of patients reviewed in fracture clinics with an upper limb complaint. Furthermore, the declining inpatient admissions and upper limb clinic referrals could be due to the hesitancy of patients to seek clinical intervention for fear of visiting the hospital. However, there is no evidence in the literature to support this. Patients with upper limb injuries, especially those with ligament sprains and tendon injuries, tended to be ambulatory. Therefore, it is conceivable that they would defer treatment until the pandemic has passed.
Consequently, we may see a surge in these cases once the effects of lockdown and the COVID-19 pandemic have eased and services should be prepared for such a phenomenon.
In 93% of the patients, a clear working diagnosis was established and in the remaining 7%, a face-to-face review was deemed necessary to make a diagnosis. This was due to difficulty in establishing the region of injury sufficiently, or due to inability to highlight the pathology without examination.
In more than two-thirds of patients, the need for further imaging was identified. We believe that this highlights the value of the virtual consultation. The patient then visited the hospital only once for examination with all the required investigations available to the clinician, reducing unnecessary exposure. These patients subsequently had their diagnosis confirmed when they visited face to face and were examined during their next appointment. A clear working plan for the next appointment could be made based on the consultation and most patients were happy with the outcome of the consultation.
Our assessment includes only telephone consultations. We acknowledge that the cohort was assessed by a single observer only and the inter-observer reliability could not be assessed.
Nevertheless, this study highlights the importance of the availability of required imaging or investigations before a definitive plan can be made. The telephone consultations could successfully identify these patients and reduce unnecessary visits to hospital, something which is of great value whilst the risk of COVID-19 looms. Although the role of clinical examination is critical in the process of treating upper limb injuries, our data show that significant and useful information could be gleaned from a telephone consultation and we believe there is a role for it in the times ahead.
Conclusion
The COVID-19 pandemic has made a significant impact on healthcare resources, public health systems and the way healthcare services are delivered. On a positive note, however, we have had an opportunity to explore and innovate with certain clinical tools such as telemedicine, risk stratification algorithms and video-conferencing. We believe that the method of delivery of healthcare is expected to change drastically in the times ahead and hence quantitative and qualitative assessment of the measures as described will be extremely useful in assessing their viability going forward.
Footnotes
Declaration of Conflicting Interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: The author(s) received no financial support for the research, authorship, and/or publication of this article.
Guarantor: JR.
Contributorship: GF designed the majority of the manuscript and data was collected by SV, MS, PVR and GKR with review of the manuscript and critique provided by BD and JR.
ORCID iDs
Giles Faria https://orcid.org/0000-0002-9167-7521
Siddharth Virani https://orcid.org/0000-0001-6275-0286
References
- 1.Chang Liang Z, Wang W, Murphy D, et al. Novel coronavirus and orthopaedic surgery: early experiences from Singapore. J Bone Joint Surg Am 2020; 102: 745–749. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.https://www.gov.uk/government/publications/wuhan-novel-coronavirus-infection-prevention-and-control/reducing-the-risk-of-transmission-of-covid-19-in-the-hospital-setting 2020 (accessed 14 June 2020).
- 3.https://www.boa.ac.uk/uploads/assets/ee39d8a8-9457-4533-9774e973c835246d/4e3170c2-d85f-4162-a32500f54b1e3b1f/COVID-19-BOASTs-Combined-FINAL.pdf 2020 (accessed 14th June 2020).
- 4.Yeh HC, Turner RS, Jones RK, et al. Characterization of aerosols produced during surgical procedures in hospitals. Aerosol Sci Technol 1995; 22: 151–161. [Google Scholar]
- 5.Wölfel R, Corman VM, Guggemos W, et al. Virological assessment of hospitalized patients with COVID-2019. Nature 2020; 581: 465–469. [DOI] [PubMed] [Google Scholar]
- 6.Malik-Tabassum K, Crooks M, Robertson A, et al. Management of hip fractures during the COVID-19 pandemic at a high-volume hip fracture unit in the United Kingdom. J Orthop 2020; 20: 332–337. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.https://www.gov.uk/government/speeches/pm-address-to-the-nation-on-coronavirus-10-May-2020 (14 June 2020).