Abstract
Background
Difficulties related to eating are often reported in children born preterm. The objective of this study was to quantitatively synthesize available data on the prevalence of problematic feeding in children under 4 years of age who were born preterm.
Methods
Literature was identified from PubMed, CINAHL, and PsycInfo. The search was limited to English language and publication years 2000–2020. To be included in the meta-analysis, the article had to report the prevalence of problematic oral feeding within a population of children born prematurely (< 37 weeks’ gestation), and the child age at the time of study had to be between full-term corrected age and 48 months. For studies meeting inclusion criteria, the following data were extracted: sample size and subsamples by gestational age and/or child age at time of study; definition of problematic feeding; measures used for assessment of feeding; gestational age at time of birth of sample; child age at time of study; exclusion criteria for the study; and prevalence of problematic feeding. Random-effects meta-analyses were performed to estimate the prevalence of problematic feeding across all studies, by gestational age at birth, and by child age at time of study.
Results
There were 22 studies that met inclusion criteria. Overall prevalence of problematic feeding (N = 4381) was 42% (95% CI 33–51%). Prevalence was neither significantly different across categories of gestational age nor by child age at the time of study. Few studies used psychometrically-sound assessments of feeding.
Conclusion
Problematic feeding is highly prevalent in prematurely-born children in the first 4 years of life regardless of degree of prematurity. Healthcare providers of children born preterm should consider screening for problematic feeding throughout early childhood as a potential complication of preterm birth.
Systematic review registration number
Not applicable.
Supplementary Information
The online version contains supplementary material available at 10.1186/s12887-021-02574-7.
Keywords: Infant, premature; Child; Bottle feeding; Breast feeding; Feeding and eating disorders; Feeding behavior
Background
Feeding difficulties are a common complication experienced by preterm infants hospitalized in the neonatal intensive care unit [1]. Discharge from the hospital is often dependent on infants achieving sufficient oral feeding skills to accomplish appropriate growth, and feeding difficulties are a frequent reason for prolonged length of stay [1]. After discharge and through the first several years of life, infants and young children born preterm have been found to have more difficulties with feeding compared with their term-born peers [2–6].
Problematic feeding after neonatal discharge entails the child being unable or unwilling to safely eat and/or drink enough to obtain appropriate nutrition and hydration, despite the availability of food [7]. Specific symptoms of problematic feeding change over the first several years of life as children transition from a liquid-based diet (i.e., human milk or infant formula) [8, 9] to early complementary foods, and then to more complex foods [10]. As the skills required to successfully eat change, the symptoms of problems also change [7, 11]. Symptoms of problematic feeding may include behaviors such as refusing to eat appropriate volumes or developmentally-appropriate varieties of foods; symptoms of dysphagia or aspiration, such as coughing, choking, gagging, or respiratory compromise; problematic feeding behaviors, such as increased stress, crying, irritability or strict requirements for mealtime success; or delayed eating skills, such as difficulty chewing [8–11].
The prevalence of problematic feeding over the first several years of life in the population of children born preterm is not well understood. Understanding the prevalence of this problem and who is at greatest risk may help healthcare providers assess risk in preterm-born children and facilitate earlier interventions. Additionally, understanding the prevalence of this problem may guide the need for additional research to improve the care of these vulnerable children.
Methods
The primary purpose of this study was to quantitatively synthesize the prevalence of problematic feeding in children under 4 years of age who were born prematurely (< 37 weeks’ gestation). We hypothesized that problematic feeding would be more prevalent among infants born at earlier gestational ages compared to later gestational ages. We also hypothesized that prevalence of problematic feeding would be higher at younger ages and decrease in older children. The secondary aim of this study was to assess the risk of bias in measurement of problematic feeding within included studies by evaluating the psychometric properties of the feeding assessments used.
Data sources and study eligibility
PubMed, CINAHL, and PsycInfo were searched for literature reporting on the prevalence of problematic feeding in preterm-born infants (defined as < 37 weeks gestational age at birth) with the child age at the time of study being between full-term corrected age and 48 months old. Literature identification was conducted through an iterative process of multiple database searches and reference list reviews. Databases were searched for terms including: feeding or eating, difficult* or problem or dysfunction or disorder, and premature or preterm. Limitations were placed on the search including English language, humans, published after January 1, 2000, and full text. The literature search was conducted in May 2020.
Literature was limited to that published since 2000 because significant progress has been made in the medical treatment and neuroprotection of premature infants in the last 20 years, particularly with regards to management of chronic lung disease. Because feeding is highly tied to both respiratory status and neurodevelopment, we chose to only include studies reporting on the more recent era of neonatal care.
To be included in the meta-analysis, the article had to be written in English, have the full-text available through a comprehensive global inter-library loan network, report the prevalence of problematic oral feeding within a population of children who were born prematurely (defined as < 37 weeks’ gestation), and the child age at the time of study had to be between full-term corrected age and 48 months. Articles were excluded if they reported on samples collected from a feeding clinic, in which case the sample would be biased towards problematic feeding. Studies that compared feeding in infants born prematurely to those born full-term, but did not report a prevalence of problematic feeding within the premature sample, were also excluded. Until recently, there has been no accepted definition of problematic feeding [12]. For the purposes of this study, problematic feeding was broadly defined as any type of problematic oral feeding, such as dysphagia, aspiration, problematic feeding behaviors, feeding refusal, or delayed eating skills.
Data extraction
The following data were extracted from studies that met inclusion criteria: study author(s), year, and country of publication; sample size and subsamples by gestational age and/or child age at time of study; definition of problematic feeding; measures used for assessment of feeding; gestational age at time of birth of sample; child age at time of study; exclusion criteria for the study; and prevalence of problematic feeding. If problematic feeding was defined in more than one way and/or more than one prevalence was reported, the highest prevalence was used for the analysis. Data extraction was performed by the first author and validated by a second member of the research team (JY).
Statistical analysis
A random-effects meta-analysis of proportions approach was used to quantify the prevalence of problematic feeding in prematurely-born children in three ways. First, an overall prevalence was calculated across all studies. In several studies, the authors reported the prevalence for more than one subsample of infants, in which case each reported prevalence was entered into the analysis separately. The highest reported prevalence of problematic feeding in the first 4 years of life for each sample was entered into the analysis. Second, prevalence was calculated and compared across studies by gestational age at birth and by child age at the time of study. To evaluate the prevalence of problematic feeding by gestational age at birth, the studies were categorized into three categories based on the gestational ages at birth of the children included in the sample. The three categories were: extremely preterm (gestational age < 28 weeks), very preterm (gestational age 28–32 weeks), and moderate to late preterm (gestational age 33–37 weeks). Studies were categorized by the mean gestational age of the sample and the highest prevalence of problematic feeding reported in the study was used. For studies that did not report a mean gestational age and only reported range, they were placed in the category of the middle of the reported range. Data from studies that reported prevalence of a widely mixed gestational age sample were excluded from the analysis of problematic feeding by gestational age at birth.
Finally, to evaluate the prevalence of problematic feeding by child age at the time of study, the prevalence of problematic feeding was estimated and compared across studies based on four age categories: full-term – 5 months corrected gestational age, 6–11 months, 12–23 months, and 24–48 months. In longitudinal studies that reported prevalence of the same sample at multiple time points, all time points were used and the highest prevalence within each age category was entered into the analysis.
For all analyses, the random-effects model was chosen to incorporate both within- and between-study heterogeneity, which was appropriate given the lack of clear definition and poor measurement of problematic feeding. Weighted estimates, taking into account precision as a function of sample size, 95% confidence intervals (CI), z-tests (i.e., summary estimate divided by standard error of the summary estimate), and associated p-values were calculated. Additionally, dispersion in effect size across studies (Q) along with an associated p-value, and variation in observed estimates attributable to heterogeneity (I2) were calculated. Comparison of meta-analytic estimates of prevalence across categories of gestational age at birth and age at assessment was made using tests of heterogeneity among subgroups. An alpha of .05 was considered statistically significant for all tests; Stata v16 (College Station, TX) was used to perform all analyses.
Assessment of risk of bias
To assess the risk of bias in measurement of problematic feeding within included studies, the quality of feeding assessments used were evaluated by their psychometric properties. A review of the literature was conducted in PubMed, CINAHL, and PyscInfo using the name of the feeding assessment measure. Data regarding the psychometric properties of the measure were extracted (RH) and verified by a second member of the team (BP). To assess the risk of bias in sampling, the exclusion criteria for each study was evaluated. Bias was assessed qualitatively.
Results
Included studies
There were 22 studies that met inclusion criteria [2–5, 13–30]. Additional file 1: Figure 1 presents a Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) [31] diagram of the results of study identification, screening, inclusion, and exclusion (with reasons). Table 1 presents data extracted from included studies.
Table 1.
Characteristics of Studies Included in Meta-Analysis
| First Author, Year of Publication, Country | Preterm Sample Size | Mean GA of Sample in weeks ± SD or (range) | Child Age at Time of Study | Exclusion Criteria | Feeding Assessment | Prevalence of Problematic Feeding |
|---|---|---|---|---|---|---|
| Adams-Chapman, 2013 [14], US | 1477 | 26 ± 2 | 18–22 mos CGA | Congenital infection or anomalies | Informal/Clinical Assessment | 13% |
| Adams-Chapman, 2015 [13], US | 467 | 26.2 ± 1.8 | 18 and 30 mos CGA | Congenital infection, major malformation, or congenital syndrome | Informal/Clinical Assessment |
18 mos: 47% 30 mos: 25% |
| Bilgin, 2016 [15], UK | 73 | 29.4 (25–33) | Term, 3, 6, and 18 mos CGA | None described | Informal/Clinical Assessment and Faddy Eating/Food Refusal Scale |
Term: 50.7% 3 mos: 20.5% 6 mos: 26% 18 mos: 57.5% |
| Buswell, 2009 [16], UK | 15 | 32 5/7 (24 4/7–36 6/7) | 10 mos CGA | Congenital problems, parenchymal hemorrhage, leukomalacia, visual impairment, aspiration precluding oral feeding, or significant social concerns | Schedule for Oral Motor Assessment | 20% |
| Cerro, 2002 [17], Australia | 95 | 29.2 ± 2.1 | 31 mos CGA (19–43 mos) | Neurological impairment | Informal/Clinical Assessment | 73% |
| Crapnell, 2013 [18], US | 80 | 26.6 ± 1.9 | 24 mos | Congenital anomalies | Infant – Toddler Social Emotional Assessment – Eating subscale | 23% |
| DeMauro, 2011 [19], US |
3 mos CGA - 220 Early PT /401 Late PT 6 mos CGA - 261 Early PT/ 398 Late PT 12 mos CGA - 244 Early PT / 451 Late PT |
Early PT: 25–33 6/7 Late PT: 34–36 6/7 |
3, 6, and 12 mos CGA | Congenital or chromosomal anomalies | Informal/Clinical Assessment |
3 mos CGA - Early PT: 33% Late PT: 29% 6 mos CGA - Early PT: 18% Late PT: 20% 12 mos CGA - Early PT: 14% Late PT: 12% |
| den Boer, 2013 [5], Netherlands | 47 | 30 ± 2 | 9.6 ± .7 mos CGA | None stated | Informal/Clinical Assessment | 47% |
| Dodrill, 2004 [20], Australia | 20 | 33.9 (32–36) | 13.5 mos CGA (11–16.4) | Medical comorbidities | Royal Children’s Hospital Oral Sensitivity Checklist | 100% |
| Enomoto, 2017 [21], Japan | 35 | 23.1–28.6 | Term CGA | Abnormal palate at birth | Informal/Clinical Assessment | 17.1% |
| Hawdon, 2000 [22], UK | 27 | 23–37 | Term CGA | NICU stay < 5 days and parents with “no fixed abode” | Neonatal Oral Motor Assessment Scale | 40.7% |
| Hoogewerf, 2017 [2], Netherlands |
EP: 38 VP: 118 MP: 95 |
EP: 27 (24–27) VP: 30 (28–31) MP: 34 (32–36) |
12–24 mos | NICU care < 4 days, chromosomal anomalies | Montreal Children’s Hospital Feeding Scale – Dutch version |
EP: 26.3% VP: 19.5% MP: 15.8% |
| Johnson, 2016 [4], UK | 597 | (32–36) | 24 mos CGA | Major structural or chromosomal congenital anomalies, cardiovascular malformations and neurosensory impairments | 17-item “Validated eating behavior questionnaire” | 14.9% |
| Jonsson, 2013 [23], Sweden | 27 | 31 ± 1.4 | < 6 mos | Presence of congenital anomalies or chronic illness not associated with prematurity. | Informal/Clinical Assessment | 48% |
| Kmita, 2011 [24], Poland |
Group 1: 22 Group 2: 18 |
Group 1: 26 (22–29) weeks Group 2: 31 (29–34 weeks) |
< 12 mos CGA | Teenage parents or congenital malformations/genetic syndromes | Informal/Clinical Assessment |
Group 1: 68.2% Group 2: 55.6% |
| Mathisen, 2000 [25], Australia | 20 | 27.3 ± 1.65 | 6–8 mos CGA | IVH, necrotizing enterocolitis, broncho-pulmonary dysplasia, chromosomal abnormality, SGA, receiving supplementary oxygen or tube feeds. | Schedule for Oral Motor Assessment | 80% |
| Nieuwenhuis, 2016 [26], Netherlands | 35 | 30 (26–32) | 3–3.9 years CGA | None stated | Montreal Children’s Hospital Feeding Scale – Dutch version | 11% |
| Pridham, 2007 [27], US | 41 | 26.4 ± 1.9 (23–30) | 1, 4, 8, and 12 mos corrected GA | Medical conditions that interfere with oral intake of nutrients or small for gestational age at birth | Child Feeding Skills Checklist |
1 mos: 28.7% 4 mos: 19.8% 8 mos: 34.5% 12 mos: 41.2% |
| Sanchez, 2016 [3], Australia | 90 | 27.9 (23.6–29.9) | 12 mos CGA | Infants with congenital abnormalities known to affect neurodevelopment | Schedule for Oral Motor Assessment | 38% |
| Sweet, 2003 [28], US | 21 | 24 (22–27) | 2 years | Birth weight > 600 g | Informal/Clinical Assessment | 62% |
| Torola, 2012 [29], Finland | 19 | 27 (23–30) | 0–5 mos CGA | Congenital or chromosomal anomaly | Neonatal Oral Motor Assessment Scale | 100% |
| Wood, 2003 [30], UK | 283 | 22 1/7–25 6/7 | 30 mos CGA | No exclusion criteria mentioned | Informal/Clinical Assessment | 33% |
Note. Additional information about definitions of problematic feeding can be found on Table 2 (Supplementary online content). EP Extremely preterm, CGA corrected gestational age, IVH intraventricular hemorrhage, mos months, MP moderately preterm, NICU neonatal intensive care unit, PMA post-menstrual age, PT preterm, SGA small for gestational age, VP very preterm
Meta-analysis of prevalence
Overall prevalence
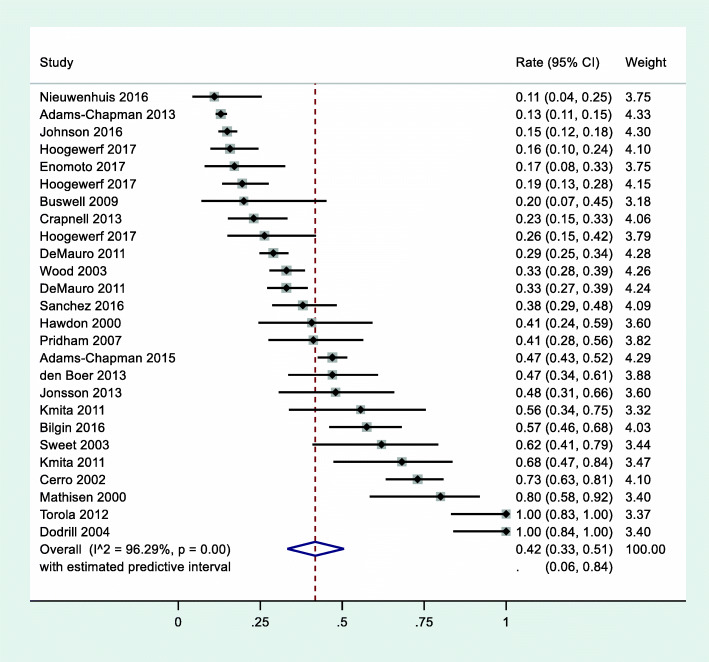
There were 22 studies that reported prevalence of problematic feeding, which collectively reported on 4381 infants and young children (Fig. 1). Across studies, the overall prevalence of problematic feeding was 42% (95% CI 33–51%; z = 14.32; p < .01). There was significant (Q = 673.94) and substantive (I2 = 96.29%) heterogeneity across studies reporting on the prevalence of problematic feeding. The estimated predictive interval for overall prevalence suggests that future studies, if conducted using similar assessment techniques as used in the included studies, may expect to find a prevalence between 6 and 84%.
Fig. 1.
Overall prevalence of problematic feeding in children under 4 years old born preterm across all 22 studies (N = 4381)
Prevalence by gestational age at birth
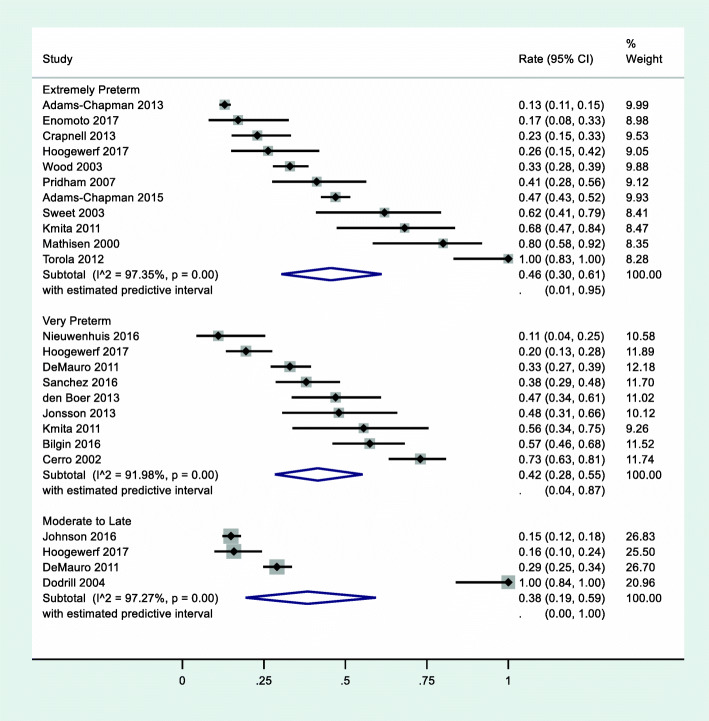
There were 20 studies that reported the prevalence of problematic feeding by gestational age at the time of birth, which collectively reported on 4339 infants (Fig. 2). No statistically significant difference was found in the prevalence of problematic feeding between infants by gestational age at birth (Q = .32, p = .85); heterogeneity remained high within each group of studies by gestational age at birth (all I2 > 91.98%).
Fig. 2.
Prevalence of problematic feeding by gestational age at time of birth. Extremely preterm = < 28 weeks gestation at birth (n = 2503); very preterm = 28–32 weeks gestation at birth (n = 723); moderate to late preterm = 32–37 weeks gestation at birth (n = 1113). Note that Buswell et al. [16] and Hawdon et al. [22] were excluded because they reported on infants across multiple gestational age categories at birth
Of the 20 studies included in this analysis, 11 reported on a sample of children born extremely preterm (< 28 weeks gestational age at birth). Among infants born extremely preterm (n = 2503), the prevalence of problematic feeding was 46% (95% CI 30–61%, z = 8.47; p < .01). There was significant (Q = 377.79) and substantive (I2 = 97.35%) heterogeneity across studies reporting prevalence of infants < 28 weeks’ gestation at birth.
There were nine studies that reported prevalence on a sample of infants born very preterm (28–32 weeks gestational age at birth) (n = 723). Among infants born very preterm, the prevalence of problematic feeding was 42% (95% CI 28–55%, z = 9.12; p < .01). Within these nine studies, there was significant (Q = 99.8) and substantive (I2 = 91.98%) heterogeneity across studies.
There were four studies that reported prevalence of problematic feeding in a sample of moderate to late preterm (gestational age 32–37 weeks) infants (n = 1113). The prevalence of problematic feeding in infants born 32–37 weeks’ gestation was 38% (95% CI 19–59%, z = 5.72; p < .01). Within these four studies, there was significant (Q = 109.78) and substantive (I2 = 97.27%) heterogeneity across studies.
Prevalence by child age at time of study
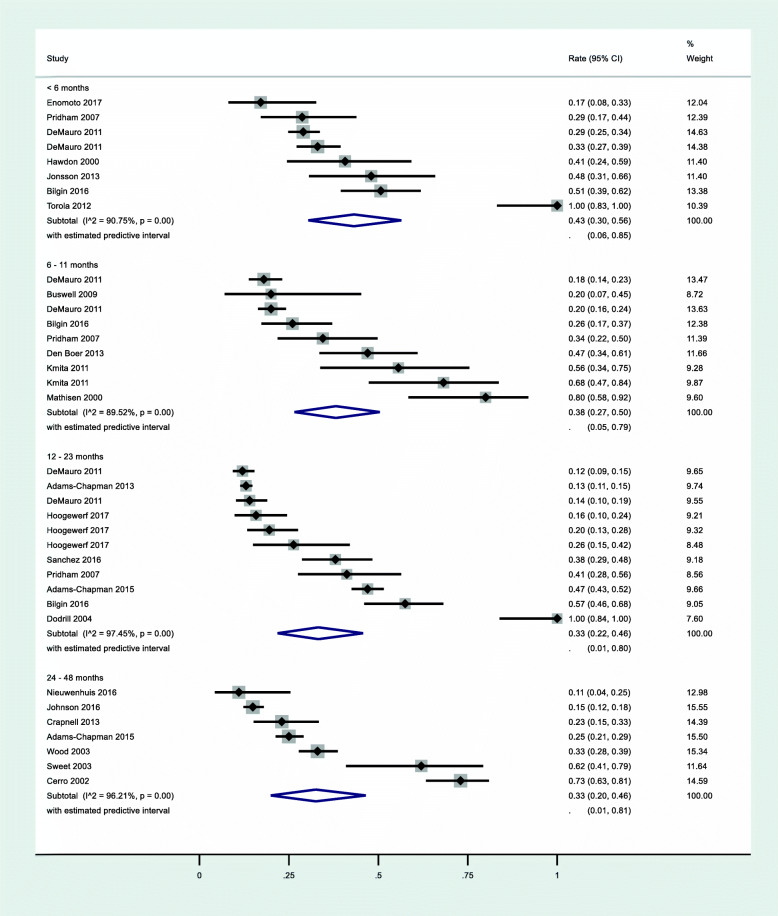
Within the 22 studies reporting on prevalence of problematic feeding in young children, seven studies reported prevalence in children aged 0–5 months at the time of study, seven studies reported on children aged 6–11 months at the time of study, 8 studies reported on children aged 12–23 months, and 7 studies reported on children 24–48 months. Several studies were longitudinal in nature and reported on problematic feeding of the same children at multiple ages, thus these samples were not entirely independent. There was no statistically significant difference found in prevalence of problematic feeding between young children of different ages at the time of study (Q = 1.73, p = .63) (Fig. 3); heterogeneity remained high within each group of studies by age at time of assessment (all I2 > 89.52%).
Fig. 3.
Prevalence of problematic feeding by child age at time of study
Problematic feeding occurred with a prevalence rate of 43% (95% CI 30–56%, z = 9.69; p < .01) in infants aged 0–5 months (n = 843). Within the seven studies reporting on eight different groups of infants in this age group, there was significant (Q = 75.66) and substantive (I2 = 90.75%) heterogeneity across studies.
In infants aged 6–11 months (n = 895) born prematurely, the prevalence of problematic feeding was 38% (95% CI 27–50%, z = 9.49; p < .01). Within the seven studies reporting on nine different groups of infants in this age group, there was significant (Q = 76.31) and substantive (I2 = 89.52%) heterogeneity across studies.
The prevalence of problematic feeding among toddlers aged 12–23 months (n = 3114) was 33% (95% CI 22–46%, z = 8.66; p < .01). Within the eight studies reporting on 11 different groups of toddlers in this age group, there was significant (Q = 392.73) and substantive (I2 = 97.45%) heterogeneity across studies.
Finally, among children 24–48 months old (n = 1578), the prevalence of problematic feeding was 33% (95% CI 20–46%, z = 7.61; p < .01). Among the seven studies reporting on seven groups of children in this age group, there was significant (Q = 158.42) and substantive (I2 = 96.21%) heterogeneity across studies.
Assessment of Bias of included studies
Quality of feeding assessment
Of the 22 studies included in this meta-analysis, only five utilized a formal assessment of feeding with evidence of strong psychometric properties [2, 3, 16, 25, 26]. Three studies used the Schedule for Oral Motor Assessment (SOMA) [3, 16, 25], an assessment conducted from a video recording of a structured feeding session. In the context of the SOMA, children are offered a series of food challenges with varying textures and degrees of difficulty to evaluate oral-motor function. The SOMA has evidence of strong psychometric properties, including acceptable test-retest reliability [32, 33], predictive validity [34], criterion validity [34], and intra-rater and inter-rater reliability [33, 35, 36].
Two studies used the Montreal Children’s Hospital Feeding Scale (MCHFS) - Dutch version [2, 26]. The MCHFS is a 14-item parent-report tool that assesses multiple constructs, including oral motor, oral sensory, appetite, maternal concerns about feeding, mealtime behaviors, maternal strategies, and family reactions to the child’s feeding [37]. Of the 14 items on the MCHFS, only nine items relate to the child’s behavior or skill during feeding. The original bilingual version (in English and French) has evidence of known-groups validity and test-retest reliability [37], as well as internal consistency reliability (Cronbach’s α = .9) and construct validity with related measures [38]. The Dutch version of the MCHFS, called the Screeninglijst Eetgedrag Peuters, also has evidence of acceptable internal consistency reliability (Cronbach’s α = .75–.84) [39] and concurrent validity with clinical assessment in both children born premature [40] and with Down Syndrome [41].
Five of the 22 studies included in the meta-analysis assessed feeding using a formalized assessment with inconsistent evidence of psychometric properties or limited psychometric testing. Two of these five studies [22, 29] used the Neonatal Oral Motor Assessment Scale (NOMAS) [42], which is a 28-item clinician-report assessment of jaw and tongue movement and function. The psychometric properties of the NOMAS have been tested in multiple research studies, but with inconsistent results with regards to inter-rater and test-retest reliability [43–47], as well as poor evidence of construct validity [46, 47]. Psychometric properties of the NOMAS improved after a change was made to the scoring system in 2016 [48], but both of the studies included in this meta-analysis were conducted prior to this change.
Crapnell and colleagues [18] used the 9-item Infant-Toddler Social Emotional Assessment (ITSEA) – Eating subscale [49], which assessed gagging and choking, eating refusal, spitting of food, picky eating, and holding food in the cheek. The ITSEA – Eating subscale has reported acceptable internal consistency reliability (Cronbach’s α = .78–.82) [18, 49]. The full ITSEA scale has reported acceptable test-retest reliability, interrater reliability, and evidence of criterion validity [49], however these data have not been reported specifically for the ITSEA – Eating subscale.
Johnson and colleagues [4] used a 17-item eating behavior questionnaire [50] that assessed four domains of eating difficulties, including refusal/picky eating, oral motor problems, oral hypersensitivity, and eating behavior problems. This questionnaire had documented acceptable internal consistency reliability for the full measure (Cronbach’s α = .83–.88) [4, 50], as well as for three of the four subscales (Cronbach’s α = .79–.9) [50]. The 4-item subscale on eating behavior problems had a reported internal consistency reliability (Cronbach’s α = .55) [50] that was below the generally accepted threshold of .7 [51]. No other psychometric testing of validity or reliability has been published. Finally, Bilgin and Wolke used a 7-item scale they created to assess “faddy eating” (i.e., picky eating) and food refusal [15] and included items related to eating too little, having a poor appetite, eating slowly, being sensitive to textures, and picky eating. No information was provided on the development of these items, but internal consistency reliability was reported as acceptable (Cronbach’s α = .74–.81) [15].
Two of the 22 studies included in the meta-analysis used formalized feeding assessments but with no published psychometric properties. Pridham and colleagues [27] used the Child Feeding Skills Checklist, which is an observational tool. For the purposes of this meta-analysis, we utilized information reported on observed oral-motor skills. Additionally, Dodrill and colleagues [20] reported on oral sensitivity using the Royal Children’s Hospital Oral Sensitivity Checklist. While this is a more formalized assessment of facial defensiveness and sensitivity to oral stimulation, there are no published psychometrics on this measure.
Of the 22 included studies, 10 used an informal or clinical assessment of feeding with no psychometric testing. The ways in which these 10 studies defined problematic feeding varied widely. The specific definitions of problematic feeding used in these 10 studies are provided on Table 2. For example, Adams-Chapman and colleagues [14] defined dysfunctional feeding as a physician order not to ingest feedings by mouth, any need for gastrostomy or tube feedings, gagging, choking, or coughing with oral feeding, documented history of aspiration, excessive drooling during feeding, or difficulty swallowing. Enomoto [21], on the other hand, considered feeding to be a problem if the infant required a milk-thickening agent, but they did not describe the process for determining the need for a milk-thickening agent. Other informal assessments included questions about appetite, oral-motor dysfunction, avoidant feeding behaviors, choking, gagging, excessive spit-up, and difficulties during feeding observed by the provider.
Table 2.
Problematic Feeding Definitions and Prevalence Calculations
| First Author, Year of Publication | Feeding Assessment | Definition of Problematic Feeding | Prevalence Calculation |
|---|---|---|---|
| Adams-Chapman, 2013 [14] | Informal/Clinical Assessment | Dysfunctional feeding defined as: 1) medical order not to ingest feedings by mouth, 2) need for gastrostomy or tube feedings, 3) gags/chokes or coughs with feeds, 4) documented aspiration, 5) excessive drooling during feeds, or 6) difficulty swallowing. | 13% of the sample were reported to have dysfunctional feeding per the definition at left. |
| Adams-Chapman, 2015 [13] | Informal/Clinical Assessment | Abnormal feeding defined as: unable to tolerate foods by mouth, requiring tube feeds for > 50% of nutritional intake, or choking, gagging, coughing, or gasping with solids. Drooling continuously or having documented history of dysphagia or aspiration were also considered abnormal. | 47% had abnormal feeding at 18 months. 25% had abnormal feeding at 30 months. |
| Bilgin, 2016 [15] | Informal/Clinical Assessment and Faddy Eating/Food Refusal Scale |
Problems in oral motor functioning were measured with the following items: (1) stopping after a few sucks, (2) excessive dribbling/difficulty swallowing, and (3) gagging/choking during the feed. Participants who endorsed 2 or 3 items were determined to have an oral-motor function problem. Faddy eating/food refusal: At term, 3, and 6 months, endorsement of the following item was deemed faddy eating/food refusal: fighting against the bottle/breast. At 18 months, a faddy eating/food refusal scale included the following variables: Eats too little, leaves most of the food offered, poor appetite, picky eater, slow eater, refuses to eat lumpy food, or refuses to eat pureed food. Participants who endorsed 5 or more problems were determined to have faddy eating/food refusal. |
Feeding problems were defined as having an oral-motor function problem and/or faddy eating/food refusal (per definitions at left). These authors found the following prevalence of feeding problems at each age: Term – 50.7%; 3 months – 20.5%; 6 months – 26%; and 18 months – 57.5%. |
| Buswell, 2009 [16] | Schedule for Oral Motor Assessment (SOMA) | Infants who scored on or above the threshold on the SOMA were determined to have oral motor dysfunction. | 20% of the sample were found to have oral-motor dysfunction. |
| Cerro, 2002 [17] | Informal/Clinical Assessment | Parents’ perceptions of their child’s eating behavior were explored using an unpublished 48-item questionnaire developed in consultation with various experts and consideration of current literature. The questionnaire involved closed questions, Likert scales and specified lists. | 73% of the sample was reported to have at least one feeding problem. |
| Crapnell, 2013 [18] | Infant – Toddler Social Emotional Assessment – Eating subscale | Children were determined to have a feeding problem if their score exceeded the ≥10th percentile of the normative sample. | 23% of the sample met criteria for a feeding problem. |
| DeMauro, 2011 [19] | Informal/Clinical Assessment | A feeding behavior questionnaire was used that included 4 questions about oromotor dysfunction and 7 questions about avoidant feeding behavior. Participant scores were categorized as normal/low if no items were endorsed, borderline/medium if 1 item was endorsed, and high if 2 or more of the items were endorsed. | At 3 months, 33% of early preterm infants and 29% of late preterm infants had medium or high avoidant behavior. At 6 months, 18% of early preterm infants and 20% of late preterm infants had medium or high avoidant behavior. At 12 months, 14% of early preterm infants and 12% of late preterm infants had medium or high avoidant behavior. |
| den Boer, 2013 [5] | Informal/Clinical Assessment | Eating and drinking observed by a speech and language therapist. The feeding was then rated for: choking while drinking, choking while eating, and gagging. | 40% of the sample was found to have choking while drinking. 46% of the sample was found to have choking while eating. 55% of the sample was found to have gagging during a meal. For the meta-analysis, we used an average of these problems for a prevalence of 47% of the preterm sample having feeding-related problem. |
| Dodrill, 2004 [20] | Royal Children’s Hospital Oral Sensitivity Checklist | A subset of questions on the Royal Children’s Hospital Oral Sensitivity Checklist evaluates the child’s response to stimulation of the oral region. Abnormal sensitivity was defined as any behavior suggesting abnormal sensitivity, included behaviors such as head turning, gagging, and vomiting with oral stimulation. | 100% of the sample displayed behaviors suggestive of abnormal oral sensitivity. |
| Enomoto, 2017 [21] | Informal/Clinical Assessment | A feeding problem was defined as oral feeding difficulty requiring a milk-thickening agent. | 17.1% of the sample required a milk-thickening agent. |
| Hawdon, 2000 [22] | Neonatal Oral Motor Assessment Scale (NOMAS) | Feeding pattern was categorized according to the NOMAS as normal, disorganized, or dysfunctional. | Of the 27 preterm infants in the sample, 11(i.e., 40.7%) were found to have either disorganized or dysfunctional feeding. |
| Hoogewerf, 2017 [2] | Montreal Children’s Hospital Feeding Scale (MCHFS)– Dutch version | Children were categorized as having a feeding problem if their score on the MCHFS was > 1 standard deviation from the mean score of the reference population. | Of the children born extremely preterm, 26.3% of the sample were found to have a feeding problem. 19.5% of the children born very preterm were found to have a feeding problem, while 15.8% of children born moderately preterm were found to have a feeding problem. |
| Johnson, 2016 [4] | 17-item “Validated eating behavior questionnaire” | Total eating difficulties score was calculated for the 17-item questionnaire. A score > 90th percentile of the term, control group was considered significant eating difficulties. | 14.9% of the late- and moderately-preterm group were found to have significant eating difficulties. |
| Jonsson, 2013 [23] | Informal/Clinical Assessment | Questionnaire developed by authors - Symptoms measured included vomiting, eating reluctance, poor weight gain, long feeding time, or other symptoms. | 48% of the preterm group were reported to have had some form of difficulty with feeding at the time of being discharged from the hospital. |
| Kmita, 2011 [24] | Informal/Clinical Assessment | Parental descriptions of feeding behavior were explored through exploratory analysis of semi structured interviews and daily diaries. | Parents reported no problems with feeding in 31.8% of group 1 and 44.4% of group 2. We then calculated that 68.2% of group 1 and 55.6% of group 2 had some problematic feeding behavior. |
| Mathisen, 2000 [25] | Schedule for Oral Motor Assessment (SOMA) | Scores on or above the threshold of the SOMA met criteria for oral motor dysfunction. | 80% of the extremely low birth weight infants were reported to have feeding problems. |
| Nieuwenhuis, 2016 [26] | Montreal Children’s Hospital Feeding Scale (MCHFS) – Dutch version | Scores on the MCHFS – Dutch version >84th percentile met criteria for a feeding problem. | 11% of the preterm sample was found to have a score on the MCHFS – Dutch version that met criteria for a feeding problem. |
| Pridham, 2007 [27] | Child Feeding Skills Checklist | Preterm-born children were observed using the Child Feeding Skills Checklist to assess feeding skills that would be expected at 1, 4, 8, and 12 months corrected gestational age. | Pridham and colleagues reported the percent of the sample that was able to perform the oral-motor skills expected at each time of measure. From this, we calculated the average percent of the sample at each time of measure that was not able to perform the expected oral-motor skill, and therefore determined to have some degree or problematic feeding. At 1 month, an average of 28.7% were not able to perform the expected oral-motor skills. At 4 months, an average of 19.8% were not able to perform expected skills. At 8 months, an average of 34.5% were not able to perform expected skills. At 12 months, an average of 41.2% were not able to perform expected skills. |
| Sanchez, 2016 [3] | Schedule for Oral Motor Assessment (SOMA) | Oral motor feeding impairment was defined as failing ≥1 SOMA challenge. | 38% of the sample of preterm children failed ≥1 SOMA challenge. |
| Sweet, 2003 [28] | Informal/Clinical Assessment | “Feeding problems” observed during neonatal follow-up clinic visit. | 13 of the 21 infants (i.e., 62%) who returned for the 2 year follow-up were found to have feeding problems. |
| Torola, 2012 [29] | Neonatal Oral Motor Assessment Scale (NOMAS) | The NOMAS categorizes the sucking pattern into normal, disorganized or dysfunctional. | None of the preterm infants had a normal sucking pattern. 84.2% had disorganized sucking while 15.8% had a dysfunctional sucking pattern. |
| Wood, 2003 [30] | Informal/Clinical Assessment | Feeding history obtained using a semi-structured interview. | Parents of 33% of children reported feeding difficulties at 30 months corrected gestational age. |
MCHFS Montreal Children’s Hospital Feeding Scale (MCHFS), NOMAS Neonatal Oral Motor Assessment Scale, SOMA Schedule for Oral Motor Assessment
Sampling Bias of included studies
Exclusion criteria for each study are presented on Table 1. The most common exclusion criteria from the 22 included studies were congenital anomalies/malformations (41%) and congenital syndromes/genetic disorders/chromosomal anomalies (36%). Five studies (23%) excluded infants with neurological abnormalities, including acquired conditions related to prematurity, and four studies (18%) did not define or report their exclusion criteria. Less common reasons from exclusion from the sample were social concerns (14%), congenital infections (9%), short stays in the neonatal intensive care unit (NICU; 9%) and small for gestational age at birth (9%). Rare reasons were exclusion included visual impairment, aspiration precluding oral feeding, medical comorbidities, abnormal palate, chronic illness not associated with prematurity, necrotizing enterocolitis, bronchopulmonary dysplasia, requiring supplemental oxygen or tube feedings, and medical conditions that interfere with oral intake of nutrients.
Discussion
This meta-analysis of currently available data found that problematic feeding was highly prevalent (42%) in children under 4 years of age who were born prematurely (< 37 weeks’ gestation). The main limitation of the data included in these analyses was that few of the studies used formalized assessments of feeding with evidence of adequate psychometric properties. Our finding of significant and substantive heterogeneity across studies likely reflects this issue of poor measurement of the problem, as well as variation in the samples studied and true variation of problematic feeding in infants with varying degrees of medical complexity. Across studies, the definition of problematic feeding varied widely and, in many cases, only captured those with feeding difficulties on the more severe end of the spectrum.
Even in the studies that did use a psychometrically-sound formalized assessment of feeding, there were limitations of the assessments used. The SOMA, which was used by three studies and had the most evidence of psychometric integrity, is a measure focused specifically on oral-motor function. While oral-motor function is a critical component of feeding, comprehensive assessment of feeding also includes evaluation of physiologic stability, behavioral responses to feeding, swallowing, gastrointestinal tract function, and ability to regulate satiety and hunger. Evaluation of problematic feeding by SOMA alone is likely to underestimate the true prevalence of feeding problems.
The MCHFS, utilized by two of the studies included in this meta-analysis, is a more inclusive assessment than the SOMA and includes evaluation of oral-motor function, oral sensory function, appetite, and mealtime behaviors. However, with only nine items directly related to the child’s eating, it is not a comprehensive assessment. The MCHFS also mixes in constructs related to maternal concerns about feeding, maternal strategies, and family reactions to the child’s feeding. While these are important factors in an overall assessment of the family and can be highly related to problematic feeding in the child, these are complex constructs that should be evaluated separately from an assessment of the child’s ability and willingness to eat. When these constructs are mixed within the same assessment, it is unclear whether abnormal score reflects a problem related to the child’s ability or willingness to eat or whether the score reflects difficulty in family functioning, family stress, maternal coping, or education about feeding.
In addition to the poor measurement of problematic feeding, many of the studies included in this meta-analysis excluded children who were at highest risk for developing problematic feeding. Many studies excluded infants with congenital infections and anomalies, as well as those with neurologic impairment, a common comorbidity associated with premature birth. For example, Mathisen and colleagues [25] reported 80% of their sample of very preterm infants had problematic feeding using the SOMA, even when excluding those with common complications of prematurity that are likely to increase risk of feeding difficulties, including intraventricular hemorrhage, necrotizing enterocolitis, bronchopulmonary dysplasia, and need for supplementary oxygen or tube feedings. Given that those premature infants with highest risk for problematic feeding were excluded from many studies, it may be that the overall prevalence of 42% identified from this meta-analysis is an underestimate of the true prevalence of problematic feeding in all children born premature. This also means that problematic feeding is a complication of premature birth in approximately 42% of children who may otherwise be considered lower risk because they do not have other major comorbidities.
When we explored the prevalence of problematic feeding by gestational age at birth, our analyses found no statistically significant difference. This finding is consistent with that of Hoogewerf and colleagues [2], included in this meta-analysis, who used the MCHFS and found no difference in prevalence of problematic feeding by gestational age. However, this finding is not consistent with other literature. In a study of 256 children born premature, Park and colleagues [6] found that children born very preterm had significantly more feeding problems than children born moderate to late preterm. This inconsistency in the literature is likely a reflection of the measurement of feeding problems. Park and colleagues [6] used the Pediatric Eating Assessment Tool, which is a comprehensive measure of feeding with strong evidence of psychometric properties that only measures symptoms of problematic feeding and does not mix constructs of feeding strategies or family concerns [10, 52, 53]. Of note, the study by Park and colleagues was not included in this meta-analysis because the prevalence of problematic feeding within the sample was not reported.
Our analyses also found no difference in prevalence of problematic feeding by the child’s age at the time of study. This finding was also not consistent with the findings of Park and colleagues [6], who found that preterm-born children aged 6–15 months had significantly more feeding problems than those aged 15 months to 2.5 years. This inconsistency is likely a result of better measurement in the Park [6] study and/or differences in the categorization of child ages.
Limitations
As discussed, the main limitations at the study and outcome level were related to few studies using psychometrically-sound assessments of feeding and exclusion of children with highest risk for problematic feeding. At the review level, the data used for this meta-analysis was limited to studies found by searching PubMed, CINAHL, and PsycInfo and available in English language through the global inter-library loan network available to the first author. It is possible that additional research studies reporting on prevalence of problematic feeding in children born prematurely are available outside of these databases, in other languages, or through other networks.
Conclusions
Problematic feeding occurs in approximately 42% of children under 4 years of age who were born prematurely (< 37 weeks’ gestation). To date, the study of problematic feeding in children has been limited by a lack of definition of the problem [12] and lack of valid and reliable measures. In 2019, Goday and colleagues proposed a consensus definition of Pediatric Feeding Disorder - impaired oral intake that is not age-appropriate, and is associated with medical, nutritional, feeding skill, and/or psychosocial dysfunction [12]. This improved definition of the problem, along with newly-developed, psychometrically-sound measures of feeding [7–11, 52–59] can be used to improve upon the research and care of problematic feeding in children born preterm and with other medical conditions. A large epidemiological study using a comprehensive and psychometrically-sound assessment of feeding is needed to determine the true prevalence of problematic feeding in children born preterm.
Supplementary Information
Additional file 1: Figure 1. Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) diagram of study source identification, screening, inclusion, and exclusion (with reasons).
Acknowledgements
Not applicable.
Abbreviations
- CGA
Corrected gestational age
- EP
Extremely preterm
- ITSEA
Infant-Toddler Social Emotional Assessment
- IVH
Intraventricular hemorrhage
- MCHFS
Montreal Children’s Hospital Feeding Scale
- Mos
Months
- MP
Moderately preterm
- NICU
Neonatal intensive care unit
- NOMAS
Neonatal Oral Motor Assessment Scale
- PMA
Post-menstrual age
- PRISMA
Preferred Reporting Items for Systematic Reviews and Meta-Analyses
- PT
Preterm
- SGA
Small for gestational age
- SOMA
Schedule for Oral Motor Assessment
- VP
Very preterm
Authors’ contributions
BP made substantial contributions to the conception and design, acquisition and interpretation of data, and drafted the manuscript. RH made substantial contributions to the acquisition of data and revised the manuscript critically for important intellectual content. JY made substantial contributions to the acquisition of data and revised the manuscript critically for important intellectual content. JL made substantial contributions to the interpretation of data and revised the manuscript critically for important intellectual content. CL made substantial contributions to the analysis and interpretation of data and revised the manuscript for important intellectual content. All authors approved of the final manuscript as submitted and agree to be accountable for all aspects of the work and to ensure that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Funding
Not applicable.
Availability of data and materials
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
Declarations
Ethics approval and consent to participate
This was an analysis of existing literature and did not involve human or animal research subjects, so ethics approval and consent were not necessary.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Lau C, Bhat K, Potak D, Schanler RJ. Oral Feeding Assessment Predicts Length of Hospital Stay in Late Preterm Infants. J Pediatr Mother Care. 2015;1(1):102. [PMC free article] [PubMed] [Google Scholar]
- 2.Hoogewerf M, Ter Horst HJ, Groen H, Nieuwenhuis T, Bos AF, van Dijk MWG. The prevalence of feeding problems in children formerly treated in a neonatal intensive care unit. J Perinatol. 2017;37(5):578–584. doi: 10.1038/jp.2016.256. [DOI] [PubMed] [Google Scholar]
- 3.Sanchez K, Spittle AJ, Slattery JM, Morgan AT. Oromotor feeding in children born before 30 Weeks' gestation and term-born peers at 12 Months' corrected age. J Pediatr. 2016;178:113–118. doi: 10.1016/j.jpeds.2016.07.044. [DOI] [PubMed] [Google Scholar]
- 4.Johnson S, Matthews R, Draper ES, et al. Eating difficulties in children born late and moderately preterm at 2 y of age: a prospective population-based cohort study. Am J Clin Nutr. 2016;103(2):406–414. doi: 10.3945/ajcn.115.121061. [DOI] [PubMed] [Google Scholar]
- 5.den Boer SL, Schipper JA. Feeding and drinking skills in preterm and low birth weight infants compared to full term infants at a corrected age of nine months. Early Hum Dev. 2013;89(6):445–447. doi: 10.1016/j.earlhumdev.2012.12.004. [DOI] [PubMed] [Google Scholar]
- 6.Park J, Thoyre SM, Pados BF, Gregas M. Symptoms of feeding problems in preterm-born children at 6 months to 7 years old. J Pediatr Gastroenterol Nutr. 2019;68(3):416–421. doi: 10.1097/MPG.0000000000002229. [DOI] [PubMed] [Google Scholar]
- 7.Pados BF, Thoyre SM, Park J, Estrem HH, McComish C. Development and content validation of the child Oral and motor proficiency scale (ChOMPS) J Early Interv. 2019;41(3):220–232. doi: 10.1177/1053815119841091. [DOI] [Google Scholar]
- 8.Pados BF, Thoyre SM, Estrem HH, Park J, McComish C. Factor structure and psychometric properties of the neonatal eating assessment tool-bottle-feeding (NeoEAT-bottle-feeding) Adv Neonatal Care. 2018;18(3):232–242. doi: 10.1097/ANC.0000000000000494. [DOI] [PubMed] [Google Scholar]
- 9.Pados BF, Thoyre SM, Estrem HH, Park J, McComish C. Factor structure and psychometric properties of the neonatal eating assessment tool-breastfeeding. J Obstet Gynecol Neonatal Nurs. 2018;47(3):396–414. doi: 10.1016/j.jogn.2018.02.014. [DOI] [PubMed] [Google Scholar]
- 10.Thoyre SM, Pados BF, Park J, Estrem H, McComish C, Hodges EA. The pediatric eating assessment tool: factor structure and psychometric properties. J Pediatr Gastroenterol Nutr. 2018;66(2):299–305. doi: 10.1097/MPG.0000000000001765. [DOI] [PubMed] [Google Scholar]
- 11.Park J, Pados BF, Thoyre SM, Estrem HH, McComish C. Factor structure and psychometric properties of the child Oral and motor proficiency scale. J Early Interv. 2019;41(4):283–299. doi: 10.1177/1053815119841092. [DOI] [Google Scholar]
- 12.Goday PS, Huh SY, Silverman A, et al. Pediatric feeding disorder: consensus definition and conceptual framework. J Pediatr Gastroenterol Nutr. 2019;68(1):124–129. doi: 10.1097/MPG.0000000000002188. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Adams-Chapman I, Bann C, Carter SL, Stoll BJ, Network NNR. Language outcomes among ELBW infants in early childhood. Early Hum Dev. 2015;91(6):373–379. doi: 10.1016/j.earlhumdev.2015.03.011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Adams-Chapman I, Bann CM, Vaucher YE, Stoll BJ, Eunice Kennedy Shriver National Institute of Child H, Human Development Neonatal Research N Association between feeding difficulties and language delay in preterm infants using Bayley Scales of Infant Development-Third Edition. J Pediatr. 2013;163(3):680–685. doi: 10.1016/j.jpeds.2013.03.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Bilgin A, Wolke D. Regulatory problems in very preterm and full-term infants over the first 18 months. J Dev Behav Pediatr. 2016;37(4):298–305. doi: 10.1097/DBP.0000000000000297. [DOI] [PubMed] [Google Scholar]
- 16.Buswell CA, Leslie P, Embleton ND, Drinnan MJ. Oral-motor dysfunction at 10 months corrected gestational age in infants born less than 37 weeks preterm. Dysphagia. 2009;24(1):20–25. doi: 10.1007/s00455-008-9161-4. [DOI] [PubMed] [Google Scholar]
- 17.Cerro N, Zeunert S, Simmer KN, Daniels LA. Eating behaviour of children 1.5-3.5 years born preterm: parents' perceptions. J Paediatr Child Health. 2002;38(1):72–78. doi: 10.1046/j.1440-1754.2002.00728.x. [DOI] [PubMed] [Google Scholar]
- 18.Crapnell TL, Rogers CE, Neil JJ, Inder TE, Woodward LJ, Pineda RG. Factors associated with feeding difficulties in the very preterm infant. Acta Paediatr. 2013;102(12):e539–e545. doi: 10.1111/apa.12393. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.DeMauro SB, Patel PR, Medoff-Cooper B, Posencheg M, Abbasi S. Postdischarge feeding patterns in early- and late-preterm infants. Clin Pediatr. 2011;50(10):957–962. doi: 10.1177/0009922811409028. [DOI] [PubMed] [Google Scholar]
- 20.Dodrill P, McMahon S, Ward E, Weir K, Donovan T, Riddle B. Long-term oral sensitivity and feeding skills of low-risk pre-term infants. Early Hum Dev. 2004;76(1):23–37. doi: 10.1016/j.earlhumdev.2003.10.001. [DOI] [PubMed] [Google Scholar]
- 21.Enomoto M, Sezaki H, Muranishi R, et al. Acquired palatal groove and delayed oral feeding in preterm infants. Pediatr Int. 2017;59(2):171–175. doi: 10.1111/ped.13113. [DOI] [PubMed] [Google Scholar]
- 22.Hawdon JM, Beauregard N, Slattery J, Kennedy G. Identification of neonates at risk of developing feeding problems in infancy. Dev Med Child Neurol. 2000;42(4):235–239. doi: 10.1017/S0012162200000402. [DOI] [PubMed] [Google Scholar]
- 23.Jonsson M, van Doorn J, van den Berg J. Parents' perceptions of eating skills of pre-term vs full-term infants from birth to 3 years. Int J Speech Lang Pathol. 2013;15(6):604–612. doi: 10.3109/17549507.2013.808699. [DOI] [PubMed] [Google Scholar]
- 24.Kmita G, Urmanska W, Kiepura E, Polak K. Feeding behaivour problems in infants born preterm: a psychological perspective. Preliminary report. Med Wieku Rozwoj. 2011;15(3):216–223. [PubMed] [Google Scholar]
- 25.Mathisen B, Worrall L, O'Callaghan M, Wall C, Shepherd RW. Feeding problems and dysphagia in six-month-old extremly low birth weight infants. Adv Speech-Language Pathol. 2000;2(1):9–17. doi: 10.3109/14417040008996782. [DOI] [Google Scholar]
- 26.Nieuwenhuis T, Verhagen EA, Bos AF, van Dijk MW. Children born preterm and full term have similar rates of feeding problems at three years of age. Acta Paediatr. 2016;105(10):e452–e457. doi: 10.1111/apa.13467. [DOI] [PubMed] [Google Scholar]
- 27.Pridham K, Steward D, Thoyre S, Brown R, Brown L. Feeding skill performance in premature infants during the first year. Early Hum Dev. 2007;83(5):293–305. doi: 10.1016/j.earlhumdev.2006.06.004. [DOI] [PubMed] [Google Scholar]
- 28.Sweet MP, Hodgman JE, Pena I, Barton L, Pavlova Z, Ramanathan R. Two-year outcome of infants weighing 600 grams or less at birth and born 1994 through 1998. Obstet Gynecol. 2003;101(1):18–23. doi: 10.1016/s0029-7844(02)02451-1. [DOI] [PubMed] [Google Scholar]
- 29.Torola H, Lehtihalmes M, Yliherva A, Olsen P. Feeding skill milestones of preterm infants born with extremely low birth weight (ELBW) Infant Behav Dev. 2012;35(2):187–194. doi: 10.1016/j.infbeh.2012.01.005. [DOI] [PubMed] [Google Scholar]
- 30.Wood NS, Costeloe K, Gibson AT, et al. The EPICure study: growth and associated problems in children born at 25 weeks of gestational age or less. Arch Dis Child Fetal Neonatal Ed. 2003;88(6):F492–F500. doi: 10.1136/fn.88.6.F492. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Moher D, Liberati A, Tetzlaff J, Altman DG, the PRISMA Group Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. PLoS Med. 2009;6(7):e1000097. doi: 10.1371/journal.pmed1000097. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Reilly S, Skuse D, Mathisen B, Wolke D. The objective rating of oral-motor functions during feeding. Dysphagia. 1995;10(3):177–191. doi: 10.1007/BF00260975. [DOI] [PubMed] [Google Scholar]
- 33.Abadi MZM, Yadegari F, Mehdizade M, Bakhshi E. Test-retest and inter-rater reliability study of the schedule for Oral-motor assessment in Persian children. Iran Rehabil J. 2018;16(1):45–53. doi: 10.29252/nrip.irj.16.1.45. [DOI] [Google Scholar]
- 34.Skuse D, Stevenson J, Reilly S, Mathisen B. Schedule for oral-motor assessment (SOMA): methods of validation. Dysphagia. 1995;10(3):192–202. doi: 10.1007/BF00260976. [DOI] [PubMed] [Google Scholar]
- 35.Benfer KA, Weir KA, Bell KL, Ware RS, Davies PS, Boyd RN. Oropharyngeal dysphagia and gross motor skills in children with cerebral palsy. Pediatrics. 2013;131(5):e1553–e1562. doi: 10.1542/peds.2012-3093. [DOI] [PubMed] [Google Scholar]
- 36.Benfer KA, Weir KA, Bell KL, Ware RS, Davies PS, Boyd RN. Oropharyngeal dysphagia in preschool children with cerebral palsy: oral phase impairments. Res Dev Disabil. 2014;35(12):3469–3481. doi: 10.1016/j.ridd.2014.08.029. [DOI] [PubMed] [Google Scholar]
- 37.Ramsay M, Martel C, Porporino M, Zygmuntowicz C. The Montreal Children's hospital feeding scale: a brief bilingual screening tool for identifying feeding problems. Paediatr Child Health. 2011;16(3):147–e17. doi: 10.1093/pch/16.3.147. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Rogers S, Ramsay M, Blissett J. The Montreal Children's hospital feeding scale: relationships with parental report of child eating behaviours and observed feeding interactions. Appetite. 2018;125:201–209. doi: 10.1016/j.appet.2018.02.007. [DOI] [PubMed] [Google Scholar]
- 39.Van Dijk MWG, Timmerman ME, Martel C, Ramsay M. Towards the development of a Dutch screening instrument for the detection of feeidng problems in young children. Neth J Psychol. 2011;66:112–119. [Google Scholar]
- 40.Van Dijk M, Bruinsma E, Hauser MP. The relation between child feeding problems as measured by parental report and mealtime behavior observation: a pilot study. Appetite. 2016;99:262–267. doi: 10.1016/j.appet.2016.01.026. [DOI] [PubMed] [Google Scholar]
- 41.Van Dijk M, Lipke-Steenbeek W. Measuring feeding difficulties in toddlers with Down syndrome. Appetite. 2018;126:61–65. doi: 10.1016/j.appet.2018.03.018. [DOI] [PubMed] [Google Scholar]
- 42.Palmer MM, Crawley K, Blanco IA. Neonatal Oral-motor assessment scale: a reliability study. J Perinatol. 1993;13(1):28–35. [PubMed] [Google Scholar]
- 43.Case-Smith J. An efficacy study of occupational therapy with high-risk neonates. Am J Occup Ther. 1988;42(8):499–506. doi: 10.5014/ajot.42.8.499. [DOI] [PubMed] [Google Scholar]
- 44.Case-Smith J, Cooper P, Scala V. Feeding efficiency of premature neonates. Am J Occup Ther. 1989;43(4):245–250. doi: 10.5014/ajot.43.4.245. [DOI] [PubMed] [Google Scholar]
- 45.da Costa SP, van der Schans CP. The reliability of the neonatal Oral-motor assessment scale. Acta Paediatr. 2008;97(1):21–26. doi: 10.1111/j.1651-2227.2007.00577.x. [DOI] [PubMed] [Google Scholar]
- 46.Zarem C, Kidokoro H, Neil J, Wallendorf M, Inder T, Pineda R. Psychometrics of the neonatal oral motor assessment scale. Dev Med Child Neurol. 2013;55(12):1115–1120. doi: 10.1111/dmcn.12202. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Bingham PM, Ashikaga T, Abbasi S. Relationship of neonatal Oral motor assessment scale to feeding performance of premature infants. J Neonatal Nurs. 2012;18(1):30–36. doi: 10.1016/j.jnn.2010.09.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.da Costa SP, Hubl N, Kaufman N, Bos AF. New scoring system improves inter-rater reliability of the neonatal Oral-motor assessment scale. Acta Paediatr. 2016;105(8):e339–e344. doi: 10.1111/apa.13461. [DOI] [PubMed] [Google Scholar]
- 49.Carter AS, Briggs-Gowan MJ, Jones SM, Little TD. The infant-toddler social and emotional assessment (ITSEA): factor structure, reliability, and validity. J Abnorm Child Psychol. 2003;31(5):495–514. doi: 10.1023/a:1025449031360. [DOI] [PubMed] [Google Scholar]
- 50.Samara M, Johnson S, Lamberts K, Marlow N, Wolke D. Eating problems at age 6 years in a whole population sample of extremely preterm children. Dev Med Child Neurol. 2010;52(2):e16–e22. doi: 10.1111/j.1469-8749.2009.03512.x. [DOI] [PubMed] [Google Scholar]
- 51.Salter K, Jutai JW, Teasell R, Foley NC, Bitensky J. Issues for selection of outcome measures in stroke rehabilitation: ICF body functions. Disabil Rehabil. 2005;27(4):191–207. doi: 10.1080/09638280400008537. [DOI] [PubMed] [Google Scholar]
- 52.Thoyre SM, Pados BF, Park J, et al. Development and content validation of the pediatric eating assessment tool (Pedi-EAT) Am J Speech Lang Pathol. 2014;23(1):46–59. doi: 10.1044/1058-0360(2013/12-0069). [DOI] [PubMed] [Google Scholar]
- 53.Pados BF, Thoyre SM, Park J. Age-based norm-reference values for the pediatric eating assessment tool. Pediatr Res. 2018;84(2):233–239. doi: 10.1038/s41390-018-0067-z. [DOI] [PubMed] [Google Scholar]
- 54.Pados BF, Thoyre SM, Galer K. Neonatal eating assessment tool - mixed breastfeeding and bottle-feeding (NeoEAT - mixed feeding): factor analysis and psychometric properties. Matern Health Neonatol Perinatol. 2019;5:12. doi: 10.1186/s40748-019-0107-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Pados BF, Estrem HH, Thoyre SM, Park J, McComish C. The neonatal eating assessment tool: development and content validation. Neonatal Network. 2017;36(6):359–367. doi: 10.1891/0730-0832.36.6.359. [DOI] [PubMed] [Google Scholar]
- 56.Pados BF, Thoyre SM, Park J. Age-based norm-reference values for the child Oral and motor proficiency scale. Acta Paediatr. 2018;107(8):1427–1432. doi: 10.1111/apa.14299. [DOI] [PubMed] [Google Scholar]
- 57.Pados BF, Park J, Thoyre SM. Neonatal eating assessment tool-bottle-feeding: norm-reference values for infants less than 7 months old. Clin Pediatr. 2019;58(8):857–863. doi: 10.1177/0009922819839234. [DOI] [PubMed] [Google Scholar]
- 58.Pados BF, Park J, Thoyre SM. Neonatal eating assessment tool-breastfeeding: reference values for infants less than 7 months old. J Hum Lact. 2019;36(2):236–244. doi: 10.1177/0890334419869598. [DOI] [PubMed] [Google Scholar]
- 59.Pados BF, Johnson J, Nelson M. Neonatal eating assessment tool – mixed breastfeeding and bottle-feeding: reference values and factors associated with problematic feeding symptoms in healthy, full-term infants. J Am Assoc Nurse Pract. Online ahead of print. 10.1097/JXX.0000000000000476. [DOI] [PubMed]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Additional file 1: Figure 1. Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) diagram of study source identification, screening, inclusion, and exclusion (with reasons).
Data Availability Statement
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.