Abstract
PURPOSE
The design of the implant-abutment complex is thought to be responsible for marginal bone loss (MBL) and might affect the condition of the peri-implant tissues. This the present study aimed to evaluate the influence of the implant-abutment complex on MBL and the peri-implant tissues in partially edentulous patients treated with dental implants and determine the most advantageous design.
MATERIALS AND METHODS
A total of ninety-one endosseous implants with different designs of implant-abutment complex [tissue level-TL (n = 30), platform switch-PS (n = 18), and platform match-PM (n = 43)] were reviewed for MBL, Probing Pocket Depth (PPD) and Bleeding on Probing (BoP). MBL was calculated for first year of the insertion and the following years.
RESULTS
The median MBL for the PM implants (2.66 ± 1.67 mm; n = 43) in the first year was significantly higher than those for the other types (P =.033). The lowest rate of MBL (0.61 ± 0.44 mm; n = 18) was observed with PS implants (P =.000). The position of the crown-abutment border showed a statisticallysignificant influence (P =.019) and a negative correlation (r=−0.395) on MBL. BoP was found significantly higher in PM implants (P =.006). The lowest BoP scores were detected in PS implants, but the difference was not significant (P =.523). The relation between PPD and connection type revealed no statistically significant influence (P >.05).
CONCLUSION
Within the limitations of the present study, it may be concluded that PS implants seem to show better peri-implant soft tissue conditions and cause less MBL.
Keywords: Marginal bone loss, Platform switching, Peri-implant, Biological width, Implant-abutment design
INTRODUCTION
Since the first implant treatment in the early 70s, implants have been routinely used in the treatment of missing teeth. After the placement of an implant, a remodeling process takes place in the bone around the implant.1 As a result of remodeling, a certain amount of marginal bone loss (MBL) is considered natural. In literature, the amount of MBL was reported to be 1.0 – 1.2 mm in the first year of implantation and 0.1 – 0.2 mm for each subsequent year.2,3 However, recent studies have shown that the MBL value with new implant designs and novel surface characteristics is considerably lower than previously stated.4,5,6
The collar region of the implant and the connection zone of the implant to the abutment seem to be important for the maintenance of the marginal bone levels. Similar to the crown margins in natural teeth, the biological width should not be violated. Many hypotheses have been proposed in order to bring an explanation, among which the implant-abutment complex (platform switch -PS- or platform matched -PM- implants as well as tissue level or bone level) had been mentioned as an important factor.7,8,9,10,11,12,13,14 Every manufacturer sticks to one of the philosophies and claims that the implants they produce have the most gentle design. In this manner, there are still implants of all possible designs of the implant abutment complex on the market and clinicians still need feedback about their impact on the marginal bone loss. The influence of platform switching on MBL is a popular discussion subject ever since.15,16,17,18,19,20 This effect was noticed coincidentally, when wide-diameter implants were introduced without matching wide-diameter prosthetic components. It is reported that due to such a mismatch of the implant-abutment connection, MBL around implants could be minimized.21 It was reported that altering the horizontal relationship between the outer edge of the implant and the attached, smaller diameter component could reduce or eliminate the expected postrestoration crestal bone remodeling that is typically observed around a two-piece implant.22
Nevertheless, the position of the crown-abutment margin might violate the biological width,11,14 and thus have influence on the resulting MBL.13
The aim of the present study was to evaluate the influence of the implant-abutment complex on marginal bone levels and on the condition of the peri-implant tissues. The null hypothesis was that platform-matched (PM) implants will have statistically significant MBL compared to tissue level and PS implants.
MATERIALS AND METHODS
This study was implemented as a retrospective study. Partially edentulous patients who had been treated with implant supported fix restorations and on a regular yearly maintenance visit were enrolled in this retrospective study. The information about the general and oral health of the patients and implant systems were provided from the patient registration system of the Istanbul University, Faculty of Dentistry, Istanbul, Turkey. A total of one hundred and fifty-three endosseous implants with cement-retained metal ceramic restorations were determined.
The main inclusion criteria were as follows: patient who have good general health (absence of uncontrolled systemic disease and conditions), who have received implant with length ≥ 8 mm and width ≥ 3.3 mm, who have implants at 3-year post loading at the time of the routine recall examination, and who have available intraoral periapical radiographies: at the date of loading with the final prosthesis (as baseline), and at yearly recalls after loading for 3 years.
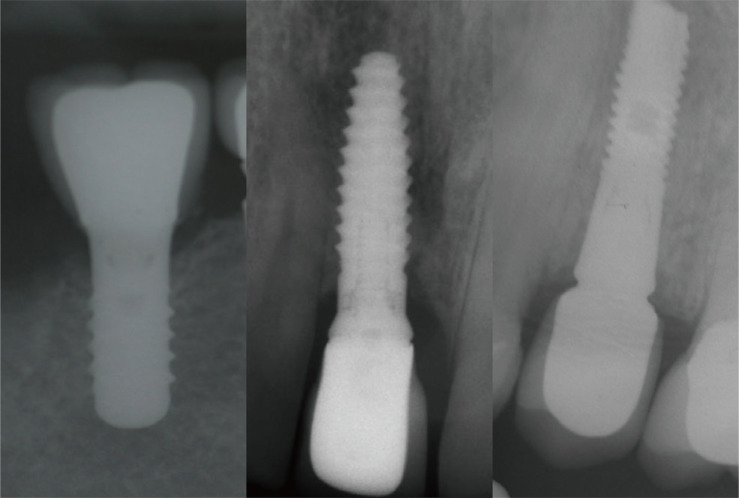
The main exclusion criteria were as follows: patients who have improper baseline/control radiographs, periimplantitis history, previous periodontitis history, uncontrolled systemic disease, cement overhangs, cigarette consummation (more than 10 cigarettes a day), and parafunctional habits such as bruxism, patients having received an implant supported fixed dental prosthesis with a cantilever, and implants that had undergone bone augmentation procedures during surgery. Additionally, patients not being compliant in terms of oral hygiene habits and routine recalls and having high plaque index scores and immediately inserted and/or loaded implants have been eliminated of the study group. Totally ninety-one endosseous implants were included in the study. Implants were classified as tissue level (Straumann, Basel, Switzerland; n = 30), platform switched (Astra Tech Implant System, Dentsply Sirona, York, PA, USA; n = 18), and platform match (BioHorizons, Birmingham, AL, USA; n = 43). The radiographic view of implant-abutment complex was shown in Fig. 1. Demographic information of patients is listed in Table 1.
Fig. 1. Radiographic view of the different implant-abutment complex.
Table 1. Demographic and general information about the study groups.
| Position of the implants | Restoration Type | Age range of the patients Mean ± SD | Sex |
|---|---|---|---|
| Anterior: 23 (n) | Bridge: 50 (n) | 51.17 ± 11.87 | 59 (female) |
| Premolar: 36 (n) | Crown: 41 (n) | 32 (male) | |
| Molar: 32 (n) |
n: number of implants in each subgroup
The current study has been conducted in full accordance with ethical principles, including the World Medical Association Declaration of Helsinki and it has been independently reviewed and approved by the Ethical Committee of the Health Research Authority of the Istanbul University (REC reference number 117-2). The current study was undertaken with the understanding and written consent of each patient and patients that accepted the invitation for reexamination were asked to sign an informed consent in accordance with guidelines approved by the Ethical Committee of the Health Research Authority of the university (REC reference number 117-2).
Peri-implant examination including Probing Pocket Depth (PPD), Bleeding on Probing (BoP), and Plaque Index were included to the evaluation for each implant. Peri-implant measurements were recorded at four sites (distal, mesial, buccal, palatinal) around all implants. The plaque accumulation was evaluated according to Sillness/Loe plaque index, whereby 0 = no plaque, 1 = nonvisible and scrapable plaque, 2 = moderate accumulation of plaque without interdental area and 3 = excessive plaque accumulation with interdental area. Probing depth was assessed to the nearest millimeter using a graded periodontal probe. The soft tissue condition based on probing was determined using the Implant Mucosal Index (IMI), whereby 0 = no bleeding, 1 = single-point bleeding, 2 = moderate point bleeding, 3 = suppuration (IMI ≥ 2, as an indication of mucositis).
The effect of the implant-abutment complex (tissue level, platform switching or platform match) was evaluated for marginal bone loss. Periapical radiographs, which were taken with the parallel technique, were included the study (Planmeca Prox, Planmeca OY, Helsinki, Finland). Measurements were analyzed at × 20 magnification using a software program (CorelDraw 11.0, Corel Corp. and Coral Ltd., Ottawa, Canada) by 2 blinded examiners. Marginal bone loss was evaluated from insertion to first year and from insertion to last control session. The rate of the marginal bone loss was calculated via periapical radiographs that were taken in annual-control sessions. Totally marginal bone loss was measured four times from insertion to last control session.
In order to determine the real height of the bone level and quantity of the marginal bone loss, distortion ratio was calculated for each radiograph. The known diameter of the implant at the collar region, obtained from the manufacturer's dimensions, was used as a reference point for each respective implant. The distance from the widest part of the implant supracrestally to the crestal bone level was measured on the magnified images (Fig. 2). To account for variability, the implant dimension (width) was measured and compared with the manufacturer-specified dimensions; ratios were calculated to adjust for distortion. Bone levels were determined by applying a distortion coefficient: true bone height is equal to true implant width multiplied by the bone height measured on the radiograph, which is then divided by the implant diameter measured on the radiograph.15
Fig. 2. Measurements on periapical radiography.
BW: Biologic width, IF: Implant fixture.
The position of the crown/abutment margin was determined radiographically. Then, the distance from the crown/abutment margin to alveolar bone crest was measured. Actual length of the crown/abutment margin (l-CAM) was calculated using the known length IF as follows: Actual l-CAM = Measured l-CAM / Measured length of IF × Actual length of the IF.
Mean and standard deviation were calculated for quantitative variables. All statistical analyses were performed by IBM SPSS Statistics 25 (IBM SPSS, Version 25.0, Armonk, New York, United States). The statistical evaluation included the Kolmogorov-Smirnova test to evaluate the normality of the distributions. Since the data were not normally distributed, non-parametric tests were used for all comparisons, including the Mann-Whitney U test and the Kruskal-Wallis rank test as appropriate. The level of significance was set at P = .05. The correlations between variables and marginal bone loss were analyzed using Spearman's test. The level of significance at 2-tailed correlation was set at r = 0.01 and 1-tailed r = 0.05. Post hoc power analysis was calculated using Gpower 3.1.9.7. Post hoc calculation was made with eta score 0.06, which represents a moderate effect of the variations onto the test groups.23 The effect size of the variations was 0.252 and it shows the small effect of the variations onto the test groups. The power of the result was 0.985 (= 0.05).
RESULTS
A total of 31 patients with 91 implants (aged 27.3 to 68.3 years, mean age 51.17 years) were evaluated. There were 30 tissue level (TL), 43 platform matching (PM), and 18 platform switched (PS) implants in total in the study group. 41 of all implants had been treated with single cemented crowns, whereas the remaining 50 implants supported cemented bridges (Table 1).
The median MBL rates were shown in Table 2. The median MBL for the PM implants in the first year was statistically significantly higher than the other types (P = .033). The slight difference in MBL between PS and TL implants in the first year was not significant (P = .231). The median MBL in PM implants after the first year was the highest among all groups (1.59 ± 1.06 mm). The average of the yearly MBL rates observed in the years following the first 12 months was statistically significantly different among the 3 groups (P = .000), where the lowest rate of MBL was observed with PS implants (0.14 ± 0.16 mm). Although TL implants showed a lower MBL rate than the PM implants, the difference was not statistically significant (P = .061).
Table 2. The mean MBL rates after first year and the average rate of the following years (Mean ± SD).
| Implant-abutment complex | ΔMBL_0-1 (Insertion to 1 year) | ΔMBL_rate_average (1 year to last session) | ΔMBL_T |
|---|---|---|---|
| PS (n = 18) | 0.42 ± 0.36 | 0.14 ± 0.16 | 0.61 ± 044 |
| PM (n = 43) | 1.84 ± 1.24 | 0.41 ± 0.27 | 2.66 ± 1.67 |
| TL (n = 30) | 0.53 ± 0.31 | 0.35 ± 0.37 | 1.30 ± 0.96 |
| P-value | .033a) | .000a) | .000a) |
a) Statistically significant difference compared among the groups according to Kruskal Wallis test.
PS: platform switched implants; PM: platform-matched implants; TL: tissue level implants; ΔMBL: marginal bone loss; ΔMBL_0-1: marginal bone loss for insertion of the implants to 1 year; ΔMBL_rate_average: marginal bone loss rates after first year and the average rate of the following years; ΔMBL_T: marginal bone loss for 1st year to last control session.
The relation of marginal bone loss with the position of the crown-abutment margin, probing pocket depth, and bleeding on probing was shown in Table 3. The position of the crown-abutment margin showed a statistically significant influence (P = .028; P = .031; P = .019) and a negative correlation (r = −0.387; r = −0.347; r = −0.395) on MBL. With decreased distance of the crown-abutment margin to the alveolar bone crest, the MBL became statistically significantly greater. On the other hand, there was no significant relation and correlation between PPD and MBL. There was a positive correlation (r = 0.231) and a significant relation (P = .045) between BoP and the MBL on the mesial, whereas no significant relation could be observed on the distal and the total average MBL (P > .05).
Table 3. The correlation of the peri-implant scores, position of the crown-abutment margin and MBL.
| ΔM | ΔD | ΔT | |
|---|---|---|---|
| Position of the crown-abutment margin | -0.387b) | -0.347b) | -0.395b) |
| 0.028a) | 0.031a) | 0.019a) | |
| PPD (mean) | 0.085 | 0.096 | 0.098 |
| 0.421 | 0.366 | 0.355 | |
| BoP | 0.231c) | 0.196 | 0.212 |
| P-value | 0.045a) | 0.089 | 0.066 |
a) Statistically significant difference compared among the groups according to Kruskal Wallis test. b) Statistically significant and 2-tailed correlation among the groups according to Spearmen's rho correlation test. c) Statistically significant and 1-tailed correlation among the groups according to Spearmen's rho correlation test.
PPD: probing pocket depth; BoP: bleeding on probing; ΔM: marginal bone loss for mesial side of the implant; ΔD: marginal bone loss for distal side of the implant; ΔT: average marginal bone loss for mesial and distal side of the implant.
The influence of the implant-abutment complex to BoP and PPD was shown in Table 4. BoP was found significantly higher in PM implants compared to the other two types (P = .006). The lowest BoP scores were detected in PS implants, although the difference between PS and TL implants was statistically not significant (P = .523). The evaluation of the relation between PPD and connection type revealed no statistically significant influence (P > .05).
Table 4. Comparison of PPD and BoP values with implant abutment complex (Mean ± SD).
| Implant-abutment complex | Peri-implant scores | |
|---|---|---|
| PPD | BoP | |
| PS (n = 18) | 2.26 ± 0.82 | 1.28 ± 0.45 |
| PM (n = 43) | 2.42 ± 0.86 | 1.81 ± 0.79 |
| TL (n = 30) | 2.11 ± 0.5 | 1.37 ± 0.48 |
| P-value | .162 | .006a) |
a) Statistically significant difference compared among the groups according to Kruskal Wallis test.
PS: platform switched implants; PM: platform-matched implants; TL: tissue level implants; PPD: probing pocket depth; BoP: bleeding on probing.
DISCUSSION
The main purpose of the present study was to analyze the influence of the implant-abutment complex on the MBL as well as on the condition of the peri-implant tissues. This retrospective clinical study was conducted in order to compare 3 different implant types placed by the same surgeon and restored with prostheses by the same team with the same prosthodontic vision. Significant differences among the three evaluated implant collar designs could be observed. While the PM implants showed the highest MBL rate in the first year and also in the following years, the measured data were even higher (Table 2) than the data reported in literature.3,4 Traditionally, 1.0 – 1.2 mm after the first year of loading and 0.2 mm in the following had been considered physiological although recent studies have reported that the MBL rate could be less than previously mentioned values.5,6,7,11,14,24,25 The reason why the highest MBL within the physiological limits happens in the first year after implant placement is because of the physiological remodeling process. PS implants on the other hand showed a much lower MBL rate in the first year where the highest MBL takes place (Table 2), but the following years were comparable with the numbers from the literature. Parallel to the results here, a recent review had pointed out that PS implants show less MBL than PM implants and an average of 0.45 mm difference between implant and abutment diameter would be very efficient in decreasing MBL.10
Radiographs are the most reliable measurement tools for following marginal bone level changes and important parameters in routine clinical practice.26 The measurements were accomplished on radiographs, which were taken following installation of the prostheses, thus serving as a reliable baseline reference, and each year during the recall sessions.
The implant-abutment complex type seems to be very effective on the MBL in the first year and in the following years. The present study confirmed that less MBL could be attained if PS implants are preferred in clinical practice.
In the present study, the position of the crown-abutment margin was evaluated in relation to MBL, too. The evaluation revealed a statistically significant and negative correlation (Table 4). The rate of MBL increased when the distance of the crown-abutment margin to alveolar bone crest decreased. It can be explained by the secure distance of the implant-abutment connection from the crestal bone neighboring the implant. Similar with present study result, it had been reported that if the crown/abutment border is located closer to bone level, the rate of MBL increases.27 Besides a slight movement that occurs at the implant-abutment interface,14 it was pointed out to the fact that microbial infiltration could occur if the implant-abutment junction is not in a safe distance to the crest, which then could increase the rate of MBL.28 The position of the crown-abutment margin seems to be closely related with the marginal bone stability for all types of implants. However, the shift in the PS implants seems to better respect the biological width than the other implant-abutment complex types.10,13,14,27 Similar to the PS implants, the crown-abutment margin in TL implants is in a secure distance to the marginal bone and shows better peri-implant conditions than PM implants.
Immediately after implant insertion, a marginal bone remodeling commences. It is a dynamic process and its rate is not constant. The rate is proposed to be a part of the implant success index.29 The time of prosthetic loading is considered to be a common reference point for measuring the MBL, as we did in the present study. Many opinions about thresholds for MBL are published, but a few of them were adopted. One of the most widely accepted thresholds is the 0.1 – 0.2 mm of bone loss per year.30 Other commonly used thresholds are loss of 2 mm after the first year of loading31 or 2.5 mm bone loss after 5 years.32 The MBL rates in the present study were comparable with the widely accepted thresholds.
Several case definitions were reported for peri-implantitis in the latest consensus report.33 In the present study, the consensus case definition used for peri-implantitis diagnosis was BoP and/or ≥ 6 mm probing depth together with bone loss ≥ 3 mm. If one of these findings was not evident, the implant was included in the study group and only implants with a peri-implantitis diagnosis were excluded, similar to very recent studies.34
Changes in condition of the peri-implant tissues were analyzed in terms of PPD and BoP values for different implant-abutment complexes in this study. Basically, it was noted that the type had influenced the BoP values whereas PPD values were not affected (Table 3). PS and TL implant-abutment complex showed lower BoP values than the PM implants (1.28 ± 0.45 and 1.37 ± 0.48) and the differences were significant (P = .006). PPD values were not significantly affected by the design (Table 3) and PPD had no statistically significant relation with MBL. On the other hand, latest studies report that changes in PPD over time may be regarded as an indicator of soft tissue inflammation,13,35 but it could be stated that PPD values alone are not sufficient to predict future bone loss.36 PPD values were not related with MBL in the present study, in accordance with previous studies.37,38,39
The relationship between MBL and BoP was analyzed in the present study and a weak-positive correlation was found (Table 3). As stated in the latest definitions33, BoP could be a precursor of an inflammation, which definitely is important of excessive MBL. Similar with the current study result, Acharya et al . had reported that BoP could be observed in case of MBL and these two parameters positively correlated with each other.34
The major limitations of this study originate from its retrospective nature and the limited number of analyzed implants. Multiple factors could affect the result of the current study, such as the position of the implants and the type of the restorations. In order to minimize variables, only implants with fixed cemented restorations have been included in the study and patients with removable dentures or screw-retained fixed prostheses were excluded. Without a doubt, in a long-term follow-up period, many drop-outs appear and thus the number of patients to be included in the study is always confined. In order to exclude deceptive marginal bone loss due to gingival inflammation, only patients with good oral hygiene and attending regular recalls were included in the study, which was also a limiting factor.
Nevertheless, it can be concluded the implant-abutment complex is an important factor for marginal bone loss as well as peri-implant health. The implants respecting the biological width around the marginal bone area, especially the implants with the platform switching property, seem to cause less marginal bone loss. Further prospective studies with larger number of patients and implants are needed to be able to draw concrete conclusions.
CONCLUSION
Within the limitations of the study, implants with a platform switching abutment-implant complex design seem to show better peri-implant soft and hard tissue conditions and cause less marginal bone loss. Further studies with more participants would be necessary to validate the present results.
References
- 1.Pikner SS, Gröndahl K. Radiographic analyses of “advanced” marginal bone loss around Brånemark dental implants. Clin Implant Dent Relat Res. 2009;11:120–133. doi: 10.1111/j.1708-8208.2008.00098.x. [DOI] [PubMed] [Google Scholar]
- 2.Albrektsson T, Buser D, Sennerby L. On crestal/marginal bone loss around dental implants. Int J Prosthodont. 2012;25:320–322. [PubMed] [Google Scholar]
- 3.Goiato MC, Pellizzer EP, da Silva EV, Bonatto Lda R, dos Santos DM. Is the internal connection more efficient than external connection in mechanical, biological, and esthetical point of views? a systematic review. Oral Maxillofac Surg. 2015;19:229–242. doi: 10.1007/s10006-015-0494-5. [DOI] [PubMed] [Google Scholar]
- 4.Lombardi T, Berton F, Salgarello S, Barbalonga E, Rapani A, Piovesana F, Gregorio C, Barbati G, Di Lenarda R, Stacchi C. Factors influencing early marginal bone loss around dental implants positioned subcrestally: a multicenter prospective clinical study. J Clin Med. 2019;8:1168–1181. doi: 10.3390/jcm8081168. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Pan YH, Lin HK, Lin JC, Hsu YS, Wu YF, Salamanca E, Chang WJ. Evaluation of the peri-implant bone level around platform-switched dental implants: a retrospective 3-year radiographic study. Int J Environ Res Public Health. 2019;16:2570–2582. doi: 10.3390/ijerph16142570. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Rana V, Dhakne VM, Jadhawar S, Kadam I, Mishra K, Patil P. Bone level measurements around platform switched and platform matched implants: a comparative study. Niger J Surg. 2019;25:9–13. doi: 10.4103/njs.NJS_19_18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Schwarz F, Alcoforado G, Nelson K, Schaer A, Taylor T, Beuer F, Strietzel FP. Impact of implant-abutment connection, positioning of the machined collar/microgap, and platform switching on crestal bone level changes. Camlog Foundation Consensus Report. Clin Oral Implants Res. 2014;25:1301–1303. doi: 10.1111/clr.12269. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Pieri F, Aldini NN, Marchetti C, Corinaldesi G. Influence of implant-abutment interface design on bone and soft tissue levels around immediately placed and restored single-tooth implants: a randomized controlled clinical trial. Int J Oral Maxillofac Implants. 2011;26:169–178. [PubMed] [Google Scholar]
- 9.Koo KT, Lee EJ, Kim JY, Seol YJ, Han JS, Kim TI, Lee YM, Ku Y, Wikesjö UM, Rhyu IC. The effect of internal versus external abutment connection modes on crestal bone changes around dental implants: a radiographic analysis. J Periodontol. 2012;83:1104–1109. doi: 10.1902/jop.2011.110456. [DOI] [PubMed] [Google Scholar]
- 10.DI Girolamo M, Calcaterra R, DI Gianfilippo R, Arcuri C, Baggi L. Bone level changes around platform switching and platform matching implants: a systematic review with meta-analysis. Oral Implantol (Rome) 2016;9:1–10. doi: 10.11138/orl/2016.9.1.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Wallace SS. Significance of the ‘biologic width’ with respect to root-form implants. Dent Implantol Update. 1994;5:25–29. [PubMed] [Google Scholar]
- 12.Tarnow D, Elian N, Fletcher P, Froum S, Magner A, Cho SC, Salama M, Salama H, Garber DA. Vertical distance from the crest of bone to the height of the interproximal papilla between adjacent implants. J Periodontol. 2003;74:1785–1788. doi: 10.1902/jop.2003.74.12.1785. [DOI] [PubMed] [Google Scholar]
- 13.Lee BA, Kim BH, Kweon HHI, Kim YT. The prosthetic abutment height can affect marginal bone loss around dental implants. Clin Implant Dent Relat Res. 2018;20:799–805. doi: 10.1111/cid.12648. [DOI] [PubMed] [Google Scholar]
- 14.Hermann JS, Buser D, Schenk RK, Cochran DL. Crestal bone changes around titanium implants. A histometric evaluation of unloaded non-submerged and submerged implants in the canine mandible. J Periodontol. 2000;71:1412–1424. doi: 10.1902/jop.2000.71.9.1412. [DOI] [PubMed] [Google Scholar]
- 15.de Oliveira RR, Novaes AB, Jr, Taba M, Jr, Papalexiou V, Muglia VA. Bone remodeling adjacent to Morse cone-connection implants with platform switch: a fluorescence study in the dog mandible. Int J Oral Maxillofac Implants. 2009;24:257–266. [PubMed] [Google Scholar]
- 16.Kwon HJ, Lee DW, Park KH, Kim CK, Moon IS. Influence of the tooth- and implant-side marginal bone level on the interproximal papilla dimension in a single implant with a microthread, conical seal, and platform-switched design. J Periodontol. 2009;80:1541–1547. doi: 10.1902/jop.2009.080558. [DOI] [PubMed] [Google Scholar]
- 17.Hürzeler M, Fickl S, Zuhr O, Wachtel HC. Peri-implant bone level around implants with platform-switched abutments: preliminary data from a prospective study. J Oral Maxillofac Surg. 2007;65:33–39. doi: 10.1016/j.joms.2007.03.024. [DOI] [PubMed] [Google Scholar]
- 18.Degidi M, Iezzi G, Scarano A, Piattelli A. Immediately loaded titanium implant with a tissue-stabilizing/maintaining design (‘beyond platform switch’) retrieved from man after 4 weeks: a histological and histomorphometrical evaluation. A case report. Clin Oral Implants Res. 2008;19:276–282. doi: 10.1111/j.1600-0501.2007.01449.x. [DOI] [PubMed] [Google Scholar]
- 19.Novaes AB, Jr, de Oliveira RR, Muglia VA, Papalexiou V, Taba M. The effects of interimplant distances on papilla formation and crestal resorption in implants with a morse cone connection and a platform switch: a histomorphometric study in dogs. J Periodontol. 2006;77:1839–1849. doi: 10.1902/jop.2006.060162. [DOI] [PubMed] [Google Scholar]
- 20.López-Marí L, Calvo-Guirado JL, Martín-Castellote B, Gomez-Moreno G, López-Marí M. Implant platform switching concept: an updated review. Med Oral Patol Oral Cir Bucal. 2009;14:e450–e454. [PubMed] [Google Scholar]
- 21.Becker J, Ferrari D, Herten M, Kirsch A, Schaer A, Schwarz F. Influence of platform switching on crestal bone changes at non-submerged titanium implants: a histomorphometrical study in dogs. J Clin Periodontol. 2007;34:1089–1096. doi: 10.1111/j.1600-051X.2007.01155.x. [DOI] [PubMed] [Google Scholar]
- 22.Lazzara RJ, Porter SS. Platform switching: a new concept in implant dentistry for controlling postrestorative crestal bone levels. Int J Periodontics Restorative Dent. 2006;26:9–17. [PubMed] [Google Scholar]
- 23.Cohen J. A power primer. Psychol Bull. 1992;112:155–159. doi: 10.1037//0033-2909.112.1.155. [DOI] [PubMed] [Google Scholar]
- 24.Gupta S, Sabharwal R, Nazeer J, Taneja L, Choudhury BK, Sahu S. Platform switching technique and crestal bone loss around the dental implants: a systematic review. Ann Afr Med. 2019;18:1–6. doi: 10.4103/aam.aam_15_18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Spinato S, Galindo-Moreno P, Bernardello F, Zaffe D. Minimum abutment height to eliminate bone loss: influence of implant neck design and platform switching. Int J Oral Maxillofac Implants. 2018;33:405–411. doi: 10.11607/jomi.5604. [DOI] [PubMed] [Google Scholar]
- 26.Chaytor DV, Zarb GA, Schmitt A, Lewis DW. The longitudinal effectiveness of osseointegrated dental implants. The Toronto study: bone level changes. Int J Periodont Restor Dent. 1991;11:112–125. [PubMed] [Google Scholar]
- 27.Hermann JS, Schoolfield JD, Schenk RK, Buser D, Cochran DL. Influence of the size of the microgap on crestal bone changes around titanium implants. A histometric evaluation of unloaded non-submerged implants in the canine mandible. J Periodontol. 2001;72:1372–1383. doi: 10.1902/jop.2001.72.10.1372. [DOI] [PubMed] [Google Scholar]
- 28.Lee CT, Huang YW, Zhu L, Weltman R. Prevalences of peri-implantitis and peri-implant mucositis: systematic review and meta-analysis. J Dent. 2017;62:1–12. doi: 10.1016/j.jdent.2017.04.011. [DOI] [PubMed] [Google Scholar]
- 29.Hasegawa M, Hotta Y, Hoshino T, Ito K, Komatsu S, Saito T. Long-term radiographic evaluation of risk factors related to implant treatment: suggestion for alternative statistical analysis of marginal bone loss. Clin Oral Implants Res. 2016;27:1283–1289. doi: 10.1111/clr.12734. [DOI] [PubMed] [Google Scholar]
- 30.Albrektsson T, Zarb G, Worthington P, Eriksson AR. The long-term efficacy of currently used dental implants: a review and proposed criteria of success. Int J Oral Maxillofac Implants. 1986;1:11–25. [PubMed] [Google Scholar]
- 31.Misch CE, Perel ML, Wang HL, Sammartino G, Galindo-Moreno P, Trisi P, Steigmann M, Rebaudi A, Palti A, Pikos MA, Schwartz-Arad D, Choukroun J, Gutierrez-Perez JL, Marenzi G, Valavanis DK. Implant success, survival, and failure: the International Congress of Oral Implantologists (ICOI) Pisa Consensus Conference. Implant Dent. 2008;17:5–15. doi: 10.1097/ID.0b013e3181676059. [DOI] [PubMed] [Google Scholar]
- 32.Berglundh T, Persson L, Klinge B. A systematic review of the incidence of biological and technical complications in implant dentistry reported in prospective longitudinal studies of at least 5 years. J Clin Periodontol. 2002;29:197–212. doi: 10.1034/j.1600-051x.29.s3.12.x. [DOI] [PubMed] [Google Scholar]
- 33.Renvert S, Persson GR, Pirih FQ, Camargo PM. Peri-implant health, peri-implant mucositis, and peri-implantitis: Case definitions and diagnostic considerations. J Periodontol. 2018;89:S304–S312. doi: 10.1002/JPER.17-0588. [DOI] [PubMed] [Google Scholar]
- 34.Acharya A, Leung MCT, Ng KT, Fan MHM, Fokas G, Mattheos N. Peri-implant marginal bone loss rate preand post-loading: An exploratory analysis of associated factors. Clin Oral Implants Res. 2019;30:410–419. doi: 10.1111/clr.13424. [DOI] [PubMed] [Google Scholar]
- 35.Roos-Jansåker AM, Lindahl C, Renvert H, Renvert S. Nine- to fourteen-year follow-up of implant treatment. Part II: presence of peri-implant lesions. J Clin Periodontol. 2006;33:290–295. doi: 10.1111/j.1600-051X.2006.00906.x. [DOI] [PubMed] [Google Scholar]
- 36.Meloni SM, Jovanovic SA, Lolli FM, Pisano M, De Riu G, De Riu N, Lugliè PF, Tullio A. Platform switching vs regular platform implants: nine-month post-loading results from a randomised controlled trial. Eur J Oral Implantol. 2014;7:257–265. [PubMed] [Google Scholar]
- 37.Doornewaard R, Jacquet W, Cosyn J, De Bruyn H. How do peri-implant biologic parameters correspond with implant survival and peri-implantitis? A critical review. Clin Oral Implants Res. 2018;29:100–123. doi: 10.1111/clr.13264. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Bergenblock S, Andersson B, Fürst B, Jemt T. Long-term follow-up of CeraOne™ single-implant restorations: an 18-year follow-up study based on a prospective patient cohort. Clin Implant Dent Relat Res. 2012;14:471–479. doi: 10.1111/j.1708-8208.2010.00290.x. [DOI] [PubMed] [Google Scholar]
- 39.Dierens M, Vandeweghe S, Kisch J, Nilner K, De Bruyn H. Long-term follow-up of turned single implants placed in periodontally healthy patients after 16-22 years: radiographic and peri-implant outcome. Clin Oral Implants Res. 2012;23:197–204. doi: 10.1111/j.1600-0501.2011.02212.x. [DOI] [PubMed] [Google Scholar]